18: The Lymphatic System
- Page ID
- 12538
Skills to Develop
- Describe the structure of the lymphatic tissue (lymph fluid, vessels, ducts, and organs)
- Describe the structure of the primary and secondary lymphatic organs
The lymphatic system is the system of vessels, cells, and organs that carries excess fluids to the bloodstream and filters pathogens from the blood. The swelling of lymph nodes during an infection and the transport of lymphocytes via the lymphatic vessels are but two examples of the many connections between these critical organ systems.
Structure of the Lymphatic System
The lymphatic vessels begin as open-ended capillaries, which feed into larger and larger lymphatic vessels, and eventually empty into the bloodstream by a series of ducts. Along the way, the lymph travels through the lymph nodes, which are commonly found near the groin, armpits, neck, chest, and abdomen. Humans have about 500– 600 lymph nodes throughout the body (Figure 18.1).
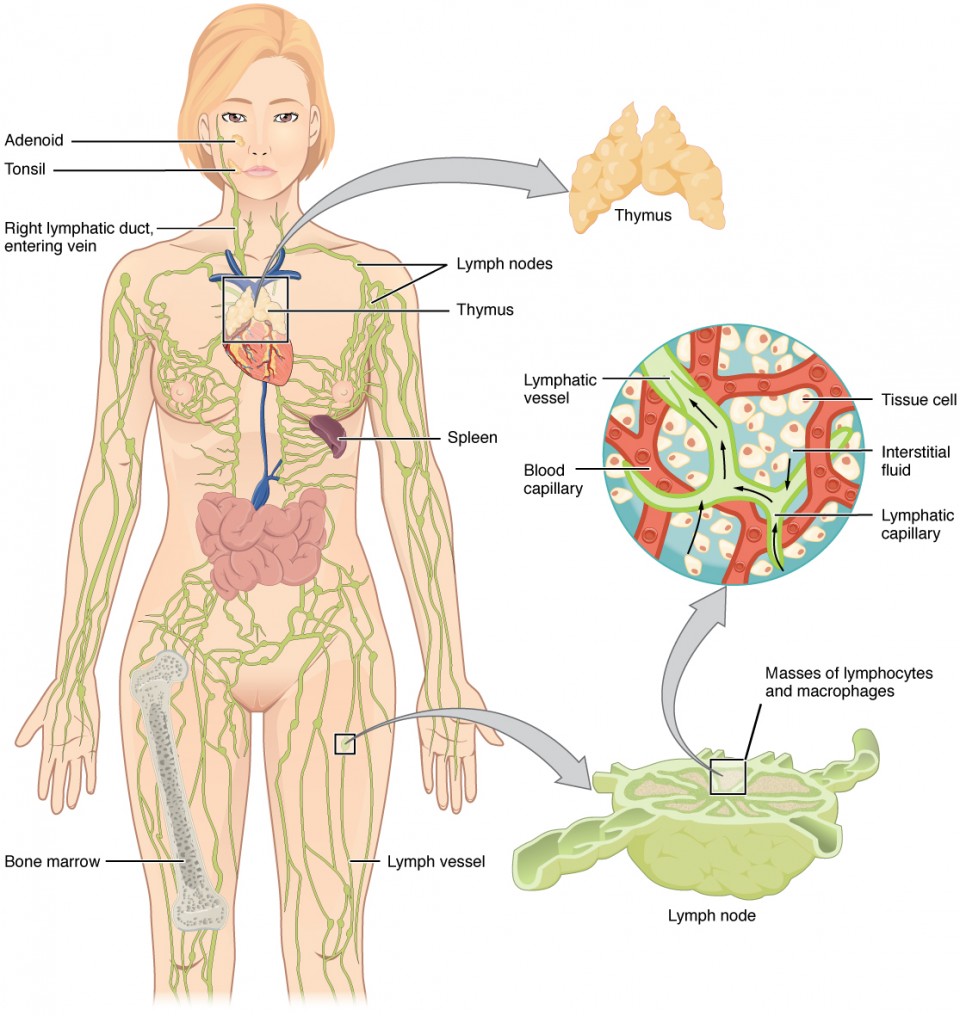
Figure 18.1 Anatomy of the Lymphatic System Lymphatic vessels in the arms and legs convey lymph to the larger lymphatic vessels in the torso.
Lymphatic Capillaries
Lymphatic capillaries, also called the terminal lymphatics, are vessels where interstitial fluid enters the lymphatic system to become lymph fluid. Located in almost every tissue in the body, these vessels are interlaced among the arterioles and venules of the circulatory system in the soft connective tissues of the body (Figure 18.2).
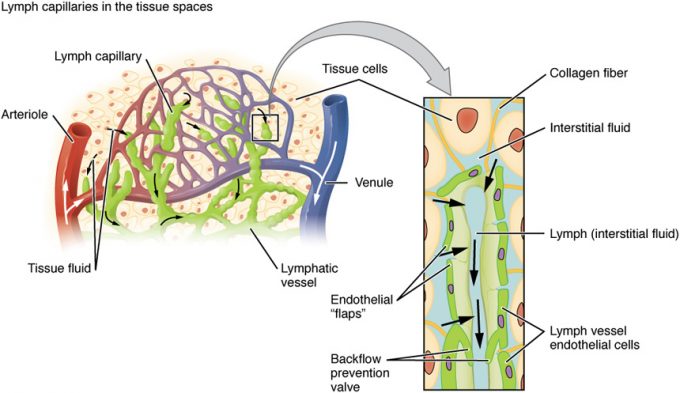
Figure 18.2 Lymphatic Capillaries Lymphatic capillaries are interlaced with the arterioles and venules of the cardiovascular system. Collagen fibers anchor a lymphatic capillary in the tissue (inset). Interstitial fluid slips through spaces between the overlapping endothelial cells that compose the lymphatic capillary.
Larger Lymphatic Vessels, Trunks, and Ducts
The lymphatic capillaries empty into larger lymphatic vessels, which are similar to veins in terms of their three- tunic structure and the presence of valves. These one-way valves are located fairly close to one another, and each one causes a bulge in the lymphatic vessel, giving the vessels a beaded appearance (see Figure 18.2).
The superficial and deep lymphatics eventually merge to form larger lymphatic vessels known as lymphatic trunks. On the right side of the body, the right sides of the head, thorax, and right upper limb drain lymph fluid into the right subclavian vein via the right lymphatic duct (Figure 18.3). On the left side of the body, the remaining portions of the body drain into the larger thoracic duct, which drains into the left subclavian vein. The thoracic duct itself begins just beneath the diaphragm in the cisterna chyli, a sac-like chamber that receives lymph from the lower abdomen, pelvis, and lower limbs by way of the left and right lumbar trunks and the intestinal trunk.
The overall drainage system of the body is asymmetrical (see Figure 18.3). The right lymphatic duct receives lymph from only the upper right side of the body. The lymph from the rest of the body enters the bloodstream through the thoracic duct via all the remaining lymphatic trunks. In general, lymphatic vessels of the subcutaneous tissues of the skin, that is, the superficial lymphatics, follow the same routes as veins, whereas the deep lymphatic vessels of the viscera generally follow the paths of arteries.
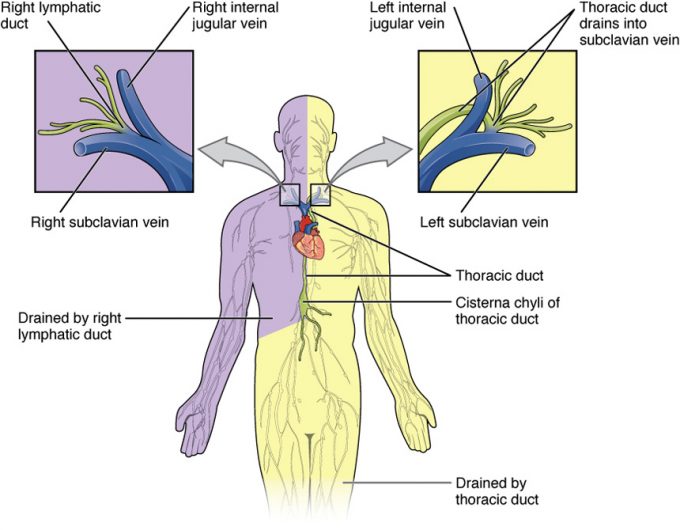
Figure 18.3 Major Trunks and Ducts of the Lymphatic System The thoracic duct drains a much larger portion of the body than does the right lymphatic duct.
Lymphoid Organs
Thymus
The thymus gland is a bilobed organ found in the space between the sternum and the aorta of the heart (Figure 18.4). Connective tissue holds the lobes closely together but also separates them and forms a capsule. The connective tissue capsule further divides the thymus into lobules via extensions called trabeculae. The outer region of the organ is known as the cortex and contains large numbers of thymocytes with some epithelial cells, macrophages, and dendritic cells (two types of phagocytic cells that are derived from monocytes). The cortex is densely packed so it stains more intensely than the rest of the thymus (see Figure 18.4). The medulla, where thymocytes migrate before leaving the thymus, contains a less dense collection of thymocytes, epithelial cells, and dendritic cells.
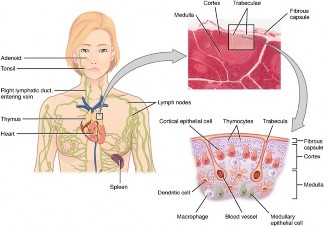
Figure 18.4 Location, Structure, and Histology of the Thymus The thymus lies above the heart. The trabeculae and lobules, including the darkly staining cortex and the lighter staining medulla of each lobule, are clearly visible in the light micrograph of the thymus of a newborn. LM × 100. (Micrograph provided by the Regents of the University of Michigan Medical School © 2012)
Lymph Nodes
Lymph nodes function to remove debris and pathogens from the lymph, and are thus sometimes referred to as the “filters of the lymph” (Figure 18.5). Any bacteria that infect the interstitial fluid are taken up by the lymphatic capillaries and transported to a regional lymph node. Dendritic cells and macrophages within this organ internalize and kill many of the pathogens that pass through, thereby removing them from the body. The lymph node is also the site of adaptive immune responses mediated by T cells, B cells, and accessory cells of the adaptive immune system. Like the thymus, the bean- shaped lymph nodes are surrounded by a tough capsule of connective tissue and are separated into compartments by trabeculae, the extensions of the capsule. In addition to the structure provided by the capsule and trabeculae, the structural support of the lymph node is provided by a series of reticular fibers laid down by fibroblasts.
The major routes into the lymph node are via afferent lymphatic vessels (see Figure 18.5). Cells and lymph fluid that leave the lymph node may do so by another set of vessels known as the efferent lymphatic vessels. Lymph enters the lymph node via the subcapsular sinus, which is occupied by dendritic cells, macrophages, and reticular fibers. Within the cortex of the lymph node are lymphoid follicles, which consist of germinal centers of rapidly dividing B cells surrounded by a layer of T cells and other accessory cells. As the lymph continues to flow through the node, it enters the medulla, which consists of medullary cords of B cells and plasma cells, and the medullary sinuses where the lymph collects before leaving the node via the efferent lymphatic vessels.
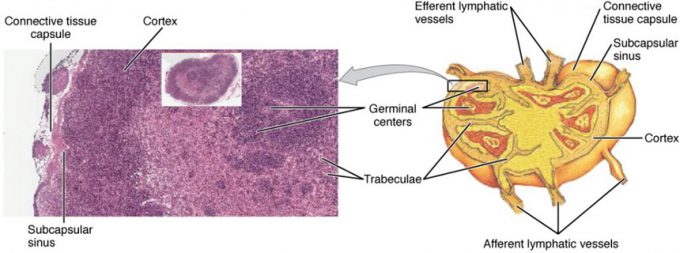
Figure 18.5 Structure and Histology of a Lymph Node Lymph nodes are masses of lymphatic tissue located along the larger lymph vessels. The micrograph of the lymph nodes shows a germinal center, which consists of rapidly dividing B cells surrounded by a layer of T cells and other accessory cells. LM × 128. (Micrograph provided by the Regents of the University of Michigan Medical School © 2012)
Spleen
In addition to the lymph nodes, the spleen is a major secondary lymphoid organ (Figure 18.6). It is about 12 cm (5 in) long and is attached to the lateral border of the stomach via the gastrosplenic ligament. The spleen is a fragile organ without a strong capsule, and is dark red due to its extensive vascularization.
The spleen is sometimes called the “filter of the blood” because of its extensive vascularization and the presence of macrophages and dendritic cells that remove microbes and other materials from the blood, including dying red blood cells. The spleen also functions as the location of immune responses to blood- borne pathogens.
The spleen is also divided by trabeculae of connective tissue, and within each splenic nodule is an area of red pulp, consisting of mostly red blood cells, and white pulp, which resembles the lymphoid follicles of the lymph nodes. Upon entering the spleen, the splenic artery splits into several arterioles (surrounded by white pulp) and eventually into sinusoids. Blood from the capillaries subsequently collects in the venous sinuses and leaves via the splenic vein. The red pulp consists of reticular fibers with fixed macrophages attached, free macrophages, and all of the other cells typical of the blood, including some lymphocytes.
The white pulp surrounds a central arteriole and consists of germinal centers of dividing B cells surrounded by T cells and accessory cells, including macrophages and dendritic cells. Thus, the red pulp primarily functions as a filtration system of the blood, using cells of the relatively nonspecific immune response, and white pulp is where adaptive T and B cell responses are mounted.
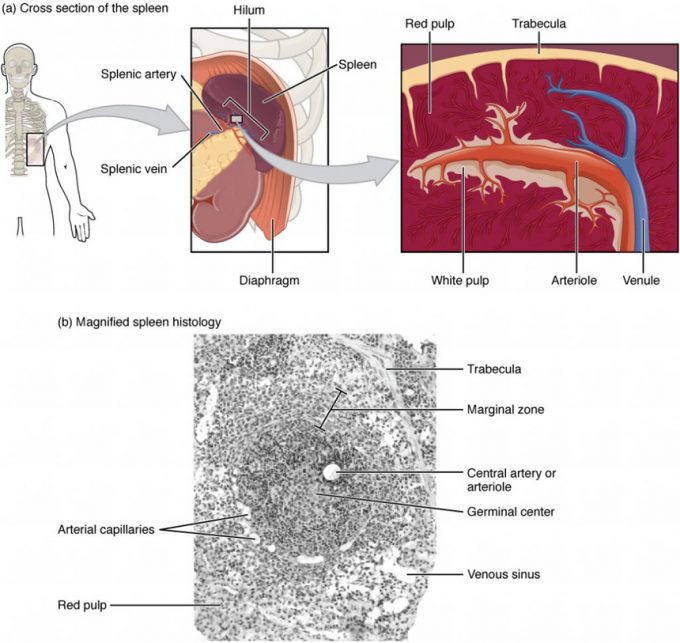
Figure 18.6 Spleen (a) The spleen is attached to the stomach. (b) A micrograph of spleen tissue shows the germinal center. The marginal zone is the region between the red pulp and white pulp, which sequesters particulate antigens from the circulation and presents these antigens to lymphocytes in the white pulp. EM × 660. (Micrograph provided by the Regents of the University of Michigan Medical School © 2012)
Lymphoid Nodules
Tonsils are lymphoid nodules located along the inner surface of the pharynx and are important in developing immunity to oral pathogens (Figure 18.7). The tonsil located at the back of the throat, the pharyngeal tonsil, is sometimes referred to as the adenoid when swollen. Such swelling is an indication of an active immune response to infection. Histologically, tonsils do not contain a complete capsule, and the epithelial layer invaginates deeply into the interior of the tonsil to form tonsillar crypts. These structures, which accumulate all sorts of materials taken into the body through eating and breathing, actually “encourage” pathogens to penetrate deep into the tonsillar tissues where they are acted upon by numerous lymphoid follicles and eliminated. This seems to be the major function of tonsils—to help children’s bodies recognize, destroy, and develop immunity to common environmental pathogens so that they will be protected in their later lives. Tonsils are often removed in those children who have recurring throat infections, especially those involving the palatine tonsils on either side of the throat, whose swelling may interfere with their breathing and/or swallowing.
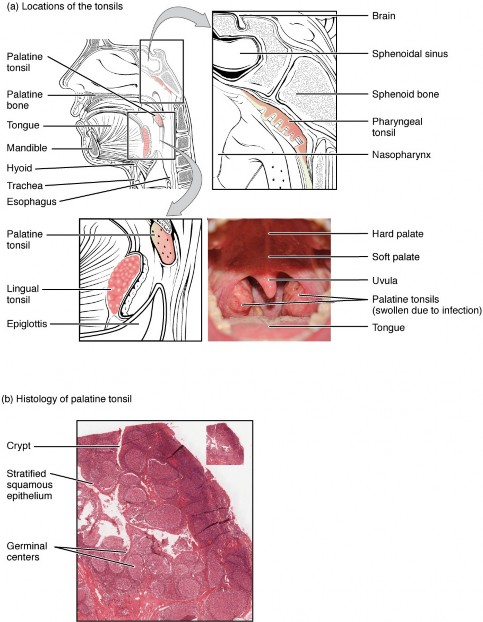
Figure 18.7 Locations and Histology of the Tonsils (a) The pharyngeal tonsil is located on the roof of the posterior superior wall of the nasopharynx. The palatine tonsils lay on each side of the pharynx. (b) A micrograph shows the palatine tonsil tissue. LM × 40. (Micrograph provided by the Regents of the University of Michigan Medical School © 2012)
B
LAB 18 EXERCISES 18-1

1
A
Match the following: Cisterna Chyli, R. lymphatic duct, Thoracic duct, Axillary lymph nodes, Abdominal lymph nodes, Cervical lymph nodes, Inguinal lymph nodes,
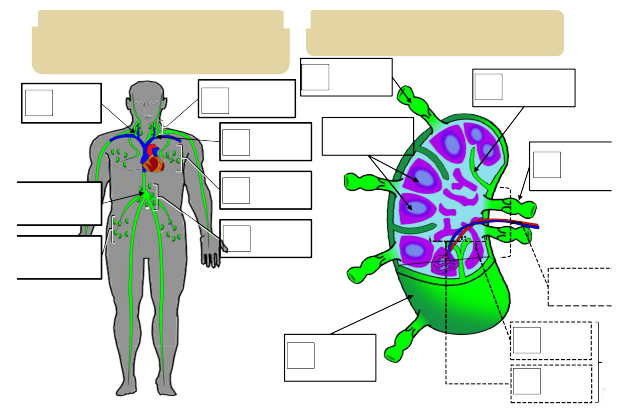
Match the following: Capsule, Afferent vessel, Efferent vessel, Hilus, Cortex, Medulla, Nodules, Trabeculae.
1
4
4
2
5
5
2
6
3
7
6
8
3
7
Superficial and deep regions
LAB 18 EXERCISES 18-2
TONSILS
Label 4 tonsils
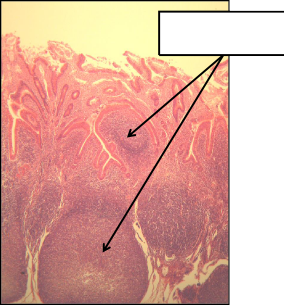
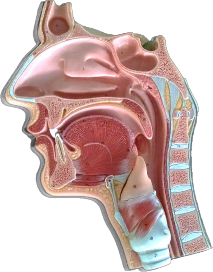
Label 3 Tonsils
Identify the lymphatic structure found in the

![]()
ileum & colon
1

LAB 18 EXERCISES 18-3
ABDOMINAL REGION
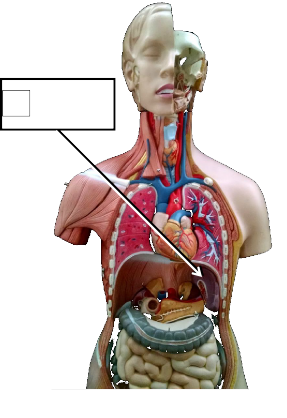
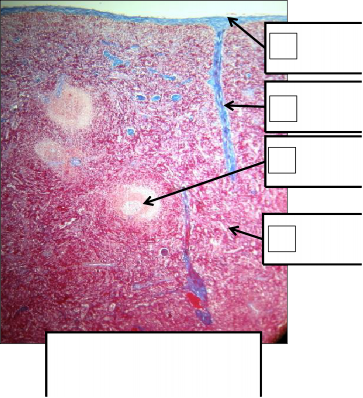
3
1
4
5
6
Organ:
2
LAB 14 EXERCISE 18-4
Peyer’s patches (Mucosal associated lymphatic tissue, MALT)
Tonsil
- Obtain a slide of each of the gland listed below from the slide box at your table.
- Follow the checklist above to set up your slide for viewing.
- View the slide on the objective which provides the best view. Find the representative object.
- In the circle below the name, draw a representative sample of the tissue, taking care to correctly and clearly draw their true shape in the slide. Draw your structures proportionately to their size in your microscope’s field of view.
- Fill in the blanks next to your drawing and identify the structures listed on the last page under, “Histology”
Repeat this for each of the tissue types seen below.
Lymph Node
Spleen

Peyer’s Patches
Tonsil
MODELS: Torsos and Mid-Sagittal Head
Appendix (vermiform)
Lymph node clusters:
- Cervical
- Inguinal
- Thoracic
- Axillary
Thoracic duct
Right lymphatic duct
Cisterna Chyli
Spleen
Tonsils:
- Pharyngeal tonsils
- Palatine tonsils
- Lingual tonsil
- Tubal tonsils
Histology:
Lymph node
- Medulla
- Cortex
- Hilus
- Afferent & efferent vessels
Spleen
- White pulp
- Red pulp

