1.20: Neck Dissection- Modified and Radical
- Page ID
- 17636
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
MODIFIED & RADICAL NECK DISSECTION
Johan Fagan
Neck dissection removes potential or proven metastases to cervical lymph nodes. It is a complex operation and requires a sound knowledge of the 3-dimensional anatomy of the neck.
Indications
Neck dissection may be elective (END) when done for clinically occult metastases, therapeutic (clinical metastases) or may be a salvage procedure (previously treated neck with surgery +/ radiation). END is indicated when the risk of having occult cervical nodal metastases exceeds 15-20%.
Nodal Levels
The neck is conventionally divided into 6 levels; Level VII is in the superior mediastinum (Figure 1).
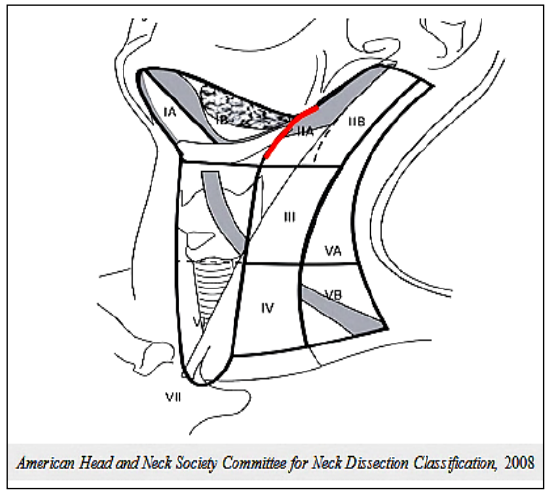
Figure 1: Classification of cervical nodal levels (Consensus statement on the classification and terminology of neck dissection. Arch Otolaryngol Head Neck Surg 2008; 134: 536–8)
Level I is bound by the body of the mandible above, the stylohyoid muscle posteriorly, and the anterior belly of the contralateral digastric muscle anteriorly. The revised classification (Figure 1) uses the posterior margin of the submandibular gland as the boundary between Levels I and II as it is clearly identified on ultrasound, CT, or MRI. Level I is subdivided into Level Ia, (submental triangle) which is bound by the anterior bellies of the digastric muscles and the hyoid bone, and Level Ib (submandibular triangle).
Level II extends between the skull base and hyoid bone. The posterior border of the sternocleidomastoid defines its posterior border. The stylohyoid muscle (alternately the posterior edge of the submandibular gland) defines its anterior border. The accessory nerve (XIn) traverses Level II obliquely and subdivides it into Level IIa (anterior to XIn) and Level IIb (behind XIn).
Level III is located between the hyoid bone and the inferior border of the cricoid cartilage. The sternohyoid muscle marks its anterior limit and the posterior border of the sternocleidomastoid its posterior border.
Level IV is located between the inferior border of the cricoid cartilage and the clavicle. The anterior boundary is the sternohyoid muscle, and the posterior border is the posterior border of sternocleidomastoid.
Level V is bound anteriorly by the posterior border of the sternocleidomastoid, and posteriorly by the trapezius muscle. It extends from the mastoid tip to the clavicle and is subdivided by a horizontal line drawn from the inferior border of the cricoid cartilage into Level Va superiorly, and Level Vb inferiorly.
Level VI is the anterior, or central, compartment of the neck. It is bound laterally by the carotid arteries, superiorly by the hyoid bone, and inferiorly by the suprasternal notch.
Neck Dissection Classification
Neck dissection operations are classified according to the cervical lymphatic regions that are resected (Figures 1, 2).
Selective neck dissection (SND) is done for N0 necks (no clinical evidence of neck nodes) or for very limited cervical metastases (Figure 2). Central neck dissection encompasses only Level VI (Figure 1).
Comprehensive or therapeutic neck dissection involves surgical clearance of Levels 1-V and may either be a radical (RND) or modified (MND) neck dissection. RND includes resection of sternocleidomastoid muscle (SCM) and accessory nerve (XIn) and internal jugular vein (IJV). MND preserves SCM and/or XIn and/or IJV. MND type I entails preservation of 1/3, usually XIn; MND type II entails preservation of 2/3, usually XIn and IJV; with MND type III all 3 structures are preserved. MND type II is most commonly done and is oncologically acceptable in the absence of adherence of cervical nodal metastases to XIn or IJV.
Extended neck dissection includes additional lymphatic groups (parotid, occipital, Level VI, mediastinal, retropharyngeal) or non-lymphatic structures (skin, muscle, nerve, blood vessels etc.) not usually included in a comprehensive neck dissection.
It has been proposed that neck dissections be more logically and precisely described and classified by naming the structures and the nodal levels that have been resected. (Ferlito A, Robbins KT, Shah JP, et al. Proposal for a rational classification of neck dissections. Head Neck. 2011;33(3):445- 50)
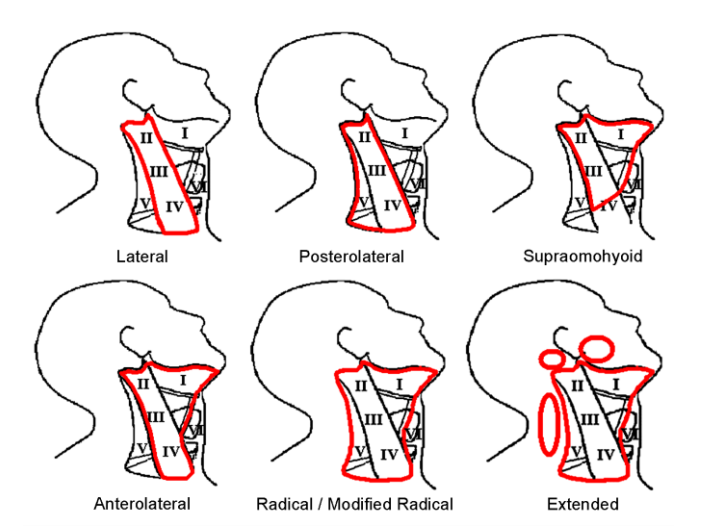
Figure 2: Common types of neck dissection
Modified neck dissection: Operative steps
The detailed step-by-step description of neck dissection that follows refers to a right sided MND type I or II.
RND involved the same surgical steps, other than that the IJV is double ligated superiorly and inferiorly with silk and with a silk transfixion suture passed through the vein, taking care not to include the vagus nerve (Xn) in the ligature.
Anesthesia, positioning and draping
The operation is done under general anesthesia without muscle relaxation as eliciting movement on mechanical or electrical stimulation of the marginal mandibular, hypoglossal (XIIn) and accessory nerves assist with locating and preserving these nerves. It is a clean operation unless the upper aerodigestive tract is entered, and antibiotics are therefore not required. With an experienced surgeon, blood transfusion is rarely required.
The patient is placed in a supine position with the neck extended and turned to the opposite side. Surgical draping must allow monitoring for movement of the lower lip with irritation of the marginal mandibular nerve, and must provide access to the clavicle inferiorly, the trapezius muscle posteriorly, the tip of the earlobe superiorly and the midline of the neck anteriorly. The drapes are sutured to the skin.
Incisions and flaps
Incisions should take into consideration access that may be required to resect the primary tumour, cosmetic factors, and the blood supply to the flaps. Flaps are elevated in a subplatysmal plane with a knife or with monopolar electrocautery. Making the flaps too thin may compromise the blood supply to the skin flaps.
Figure 3 demonstrates incisions commonly used for MND done in association with cancers of the oral cavity, oropharynx, nasal cavity sinuses and skin cancers of the midface. The transverse skin incision can be extended across to the opposite side with bilateral neck dissections or can be extended superiorly to split the lower lip in the midline to gain access to the oral cavity. Care should be taken not to place the trifurcation of the incision over the carotid artery, as skin loss at this point may expose the carotid artery with its attendant risks.
Figure 4 demonstrates the hockey stick incision. This can be extended into a preauricular skin crease and is particularly useful for combined parotidectomy and neck dissection. It has the advantage that the scar of the vertical limb along the anterior border of the trapezius can be hidden by long hair. Care must be taken in patients who have been previously irradiated as the posteroinferior corner has a tenuous blood supply and may slough, having to heal by secondary intention.
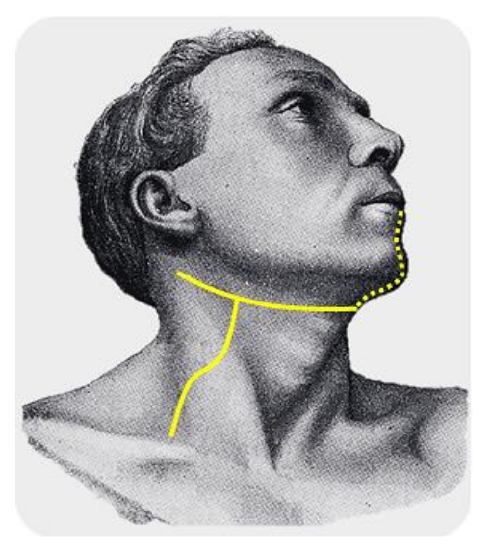
Figure 3: Incisions for neck dissection combined with oral cavity cancer resection
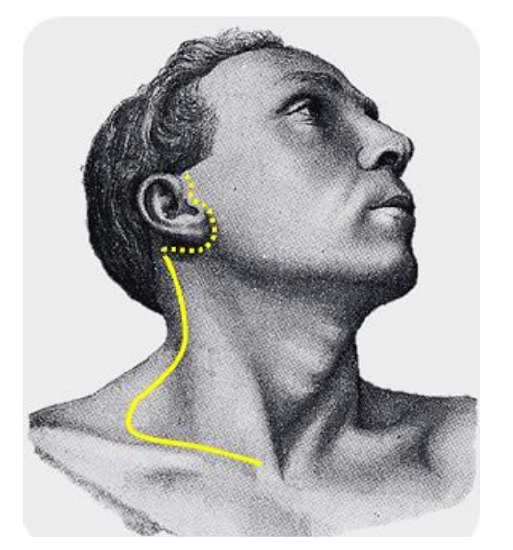
Figure 4: Hockey-stick incision for neck dissection combined with parotidectomy
With laryngectomy patients, MND can be done either via a wide apron flap, or by lateral extensions from the apron flap (Figures 5, 6).
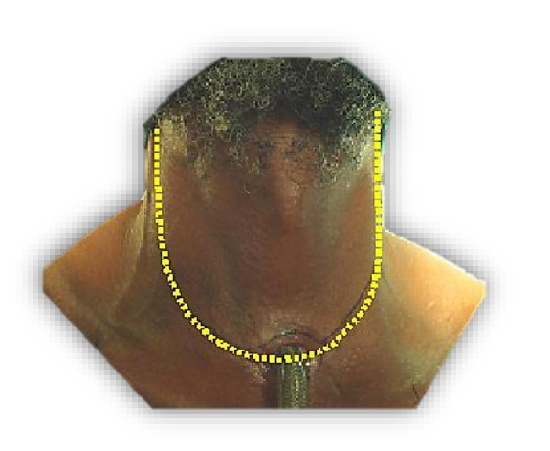
Figure 5: Wide apron flap
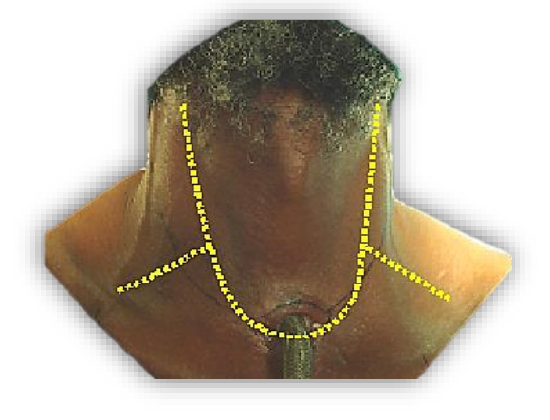
Figure 6: Apron flap with lateral extensions
Neck dissection: Operative steps
Figure 7 shows a completed right-sided MND type II. The superimposed numbers indicate the sequence of the main operative steps that will be referred to in the description of the surgery that follows.
Step 1 (Figure 7)
The neck is opened via a horizontal incision placed in a skin crease at about the level of the hyoid bone. The incision is made through skin, subcutaneous fat, and platysma muscle. Identify the external jugular vein and greater auricular nerve overlying the sternocleidomastoid muscle (SCM) (Figure 8).
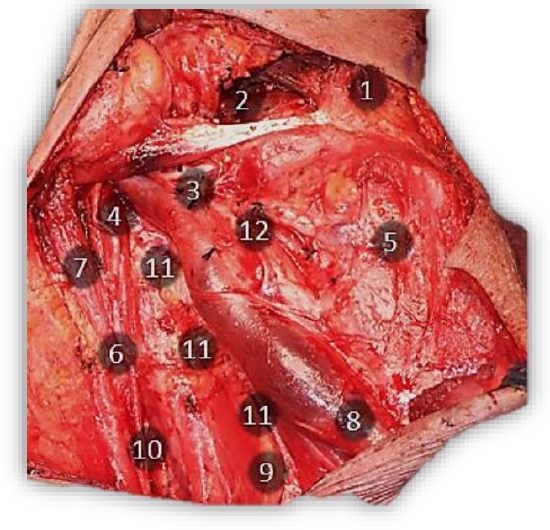
Figure 7: Completed right MND type II with sequence of operative steps
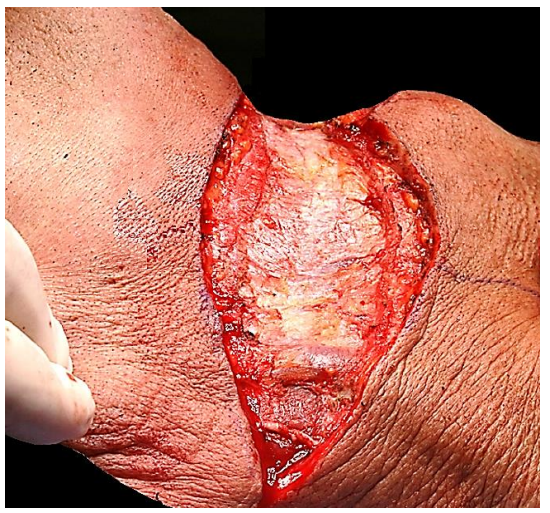
Figure 8: Note platysma muscle (transected), and the external jugular vein and greater auricular nerve overlying the SCM
Next the superior flap is elevated with cautery until the submandibular salivary gland is identified. The submandibular gland fascia is then incised inferiorly over the gland to avoid injury to the marginal mandibular nerve (Figure 9).
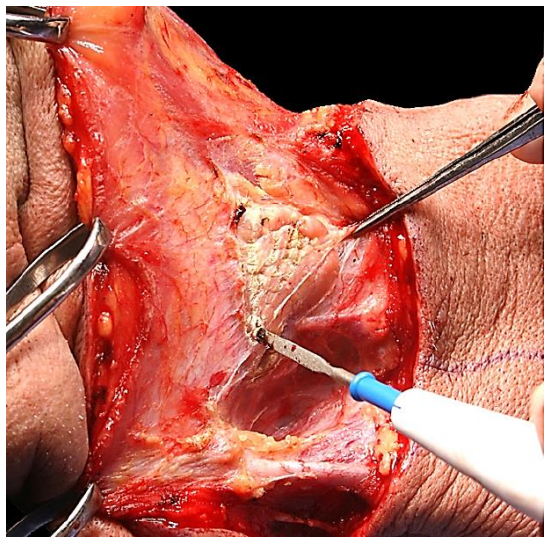
Figure 9: Incision of submandibular salivary gland capsule
The surgeon then resects the fat and lymph nodes from the submental triangle (Level Ia). A subplatysmal dissection of the overlying skin is extended to the opposite anterior belly of digastric muscle, taking care not to injure the anterior jugular veins. The submental triangle is resected inferiorly to the hyoid bone with electrocautery. The deep plane of dissection is the mylohyoid muscles (Figures 10 & 11).
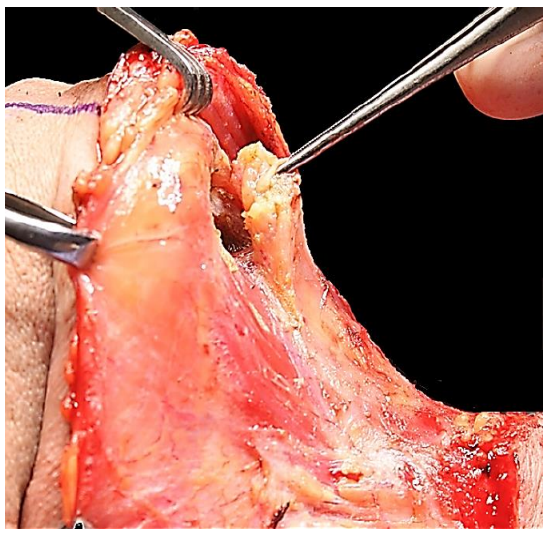
Figure 10: Resection of submental triangle
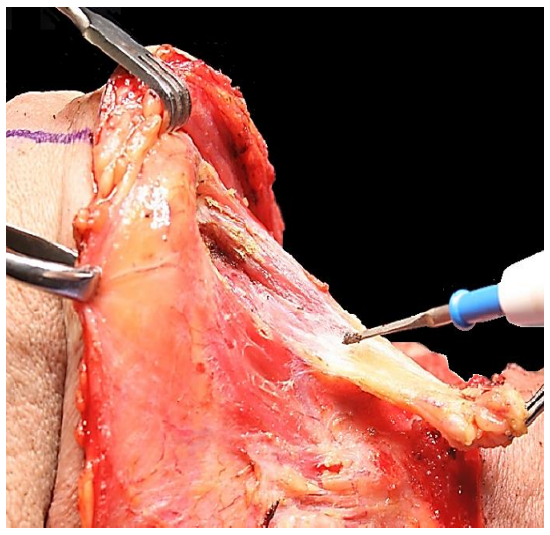
Figure 11: Resection of submental triangle onto mylohyoid muscles
Step 2 (Figure 7)
The surgeon next addresses Level Ib of the neck. Because the marginal mandibular nerve runs in an extracapsular plane, the submandibular gland capsule is dissected from the gland in a superior direction in a subcapsular plane (Figure 9). The marginal mandibular nerve does not need to be routinely identified. The assistant however watches for twitching of the lower lip, as this indicates proximity of the nerve. The facial artery and vein are identified by blunt dissection with a fine hemostat (Figure 12). The marginal mandibular nerve crosses the facial artery and vein (Figure 12).
Next attention is directed at the fat and lymph nodes tucked anteriorly and deeply between the anterior belly of digastric and mylohyoid muscle. These nodes are especially important to resect with malignancies of the anterior floor of mouth. To resect these nodes one retracts the anterior belly of digastric anteriorly and delivers the tissue using electrocautery dissection with the deep dissection plane being the mylohyoid muscle (Figures 12, 13).
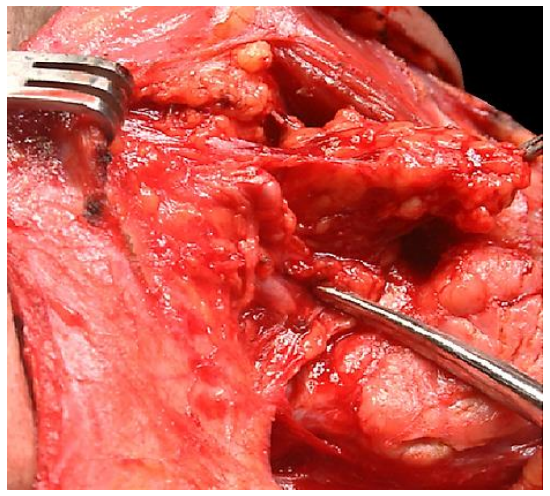
Figure 12: The submandibular gland has been dissected in a subcapsular plane; the marginal mandibular nerve is seen crossing the facial artery and vein (at tip of hemostat); fat and nodes are delivered from the anterior pocket deep to the digastric
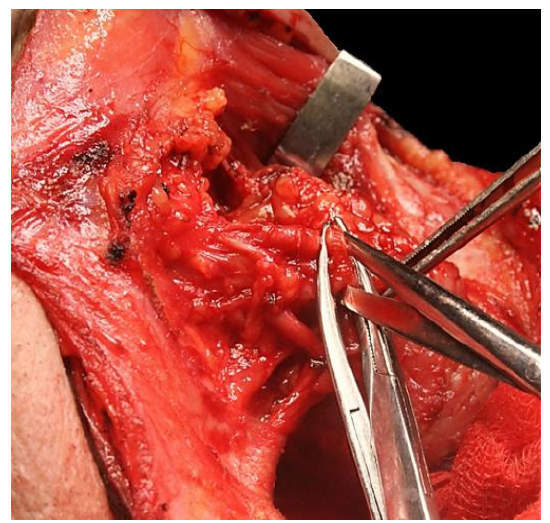
Figure 13: Dividing the facial vessels below the marginal mandibular nerve
Other than the nerve to mylohyoid and vessels that pierce the muscle that are cauterized or ligated, there are no significant structures until the dissection reaches the posterior free margin of the mylohyoid muscle. Next attention is directed at the region of the facial artery and vein. The surgeon palpates around the facial vessels for facial lymph nodes; if present, they are dissected free using fine hemostats, taking care not to traumatize the marginal mandibular nerve. The facial artery and vein are then divided and tied close to the submandibular gland so as not to injure the marginal mandibular nerve (Figure 13).
This frees up the gland superiorly, which can then be reflected away from the mandible (Figure 14).
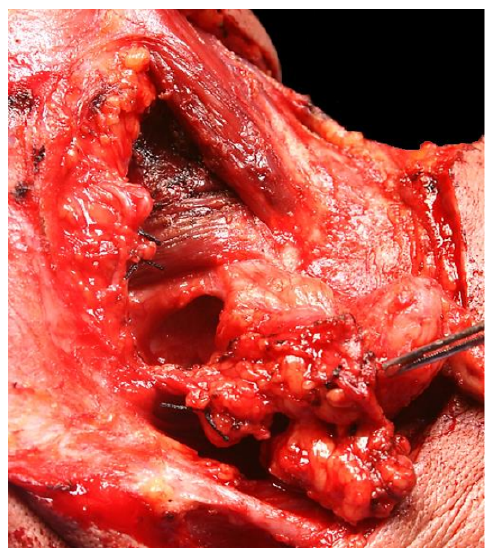
Figure 14: Marginal mandibular nerve visible over divided facial vessels; gland reflected inferiorly; mylohyoid muscle widely exposed
Next the surgeon addresses the lingual nerve, submandibular duct, and XIIn. The mylohyoid muscle is retracted anteriorly, and the clearly defined dissection plane between the deep aspect of the submandibular gland and the fascia covering the XIIn is opened. This is done with finger dissection taking care not to tear the thinwalled veins accompanying XIIn.
The XIIn is now visible in the floor of the submandibular triangle (Figure 15).
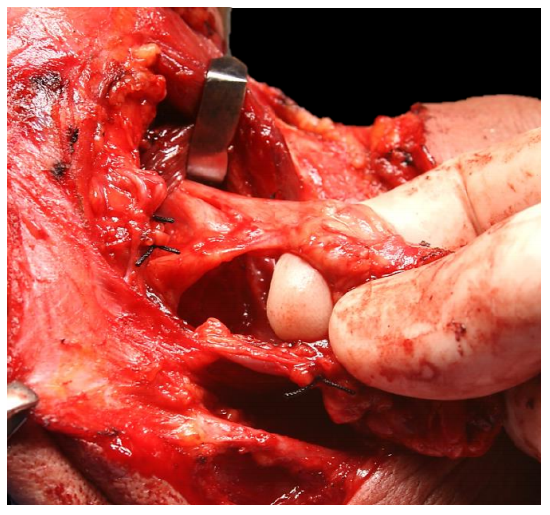
Figure 15: Finger dissection delivers the submandibular gland and duct and brings the lingual nerve into view. The proximal stump of the facial artery is visible at the tip of the thumb, and the XIIn behind the nail of the index finger
Inferior traction on the gland brings the lingual nerve and the submandibular duct into view (Figure 15). The submandibular duct is separated from the lingual nerve, divided and ligated (Figures 16, 17).
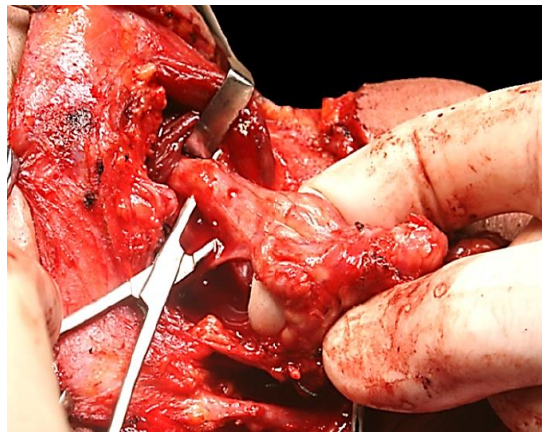
Figure 16: Submandibular duct
The submandibular ganglion, suspended from the lingual nerve, is clamped, divided and ligated, taking care not to cross-clamp the lingual nerve (Figure 17).
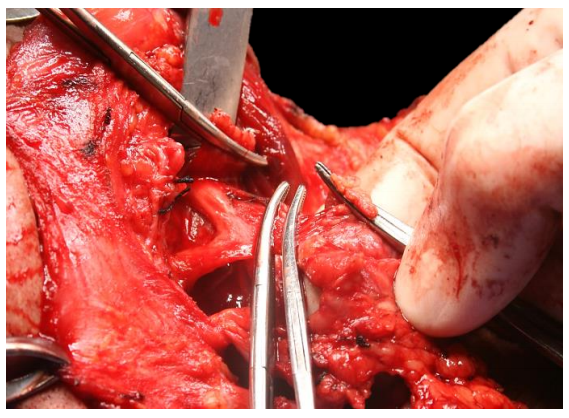
Figure 17: Separating the submandibular ganglion from the lingual nerve
The facial artery is divided and ligated just above the posterior belly of digastric (Figure 18).
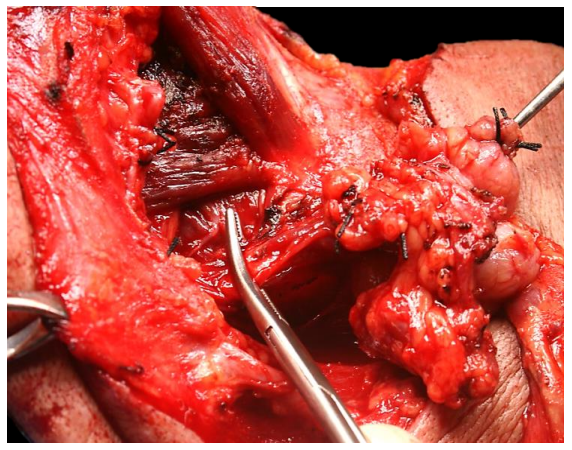
Figure 18: Clamping and dividing the facial artery just above the posterior belly of digastric
Note: A surgical variation of the above technique is to preserve the facial artery by dividing and ligating the 1-5 small branches that enter the submandibular gland. This is usually simple to do, it reduces the risk of injury to the marginal mandibular nerve and permits the use of a buccinator flap based on the facial artery (Figure 19).
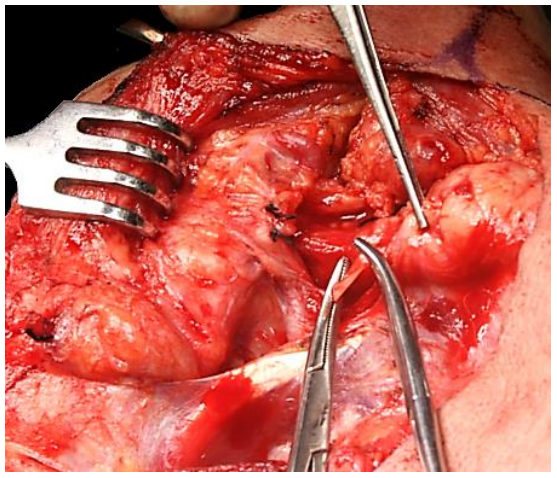
Figure 19: Facial artery has been kept intact; a branch is being divided
Step 3 (Figure 7)
This step entails identifying the XIIn in Level IIa and freeing and tracing the XIIn posteriorly where it leads the surgeon directly to the internal jugular vein (IJV). First divide the fascia along the lateral aspect of the digastric (Figure 20).
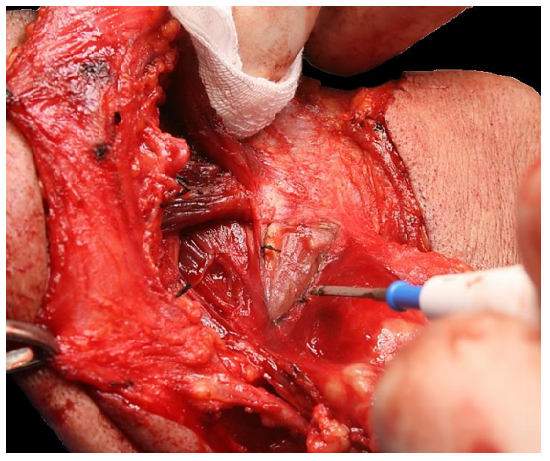
Figure 20: Divide the fascia overlying the posterior belly of the digastric muscle
Then divide the external jugular vein (Figure 21).
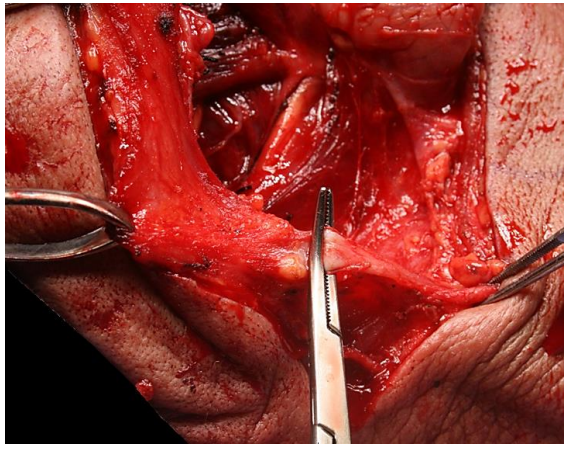
Figure 21: Divide the external jugular vein
Continue to expose the posterior belly of digastric along its entire length, taking care not to wander above the muscle as this would jeopardise the facial nerve (Figure 22). This step is the key to facilitating subsequent exposure of the IJV and XIn.
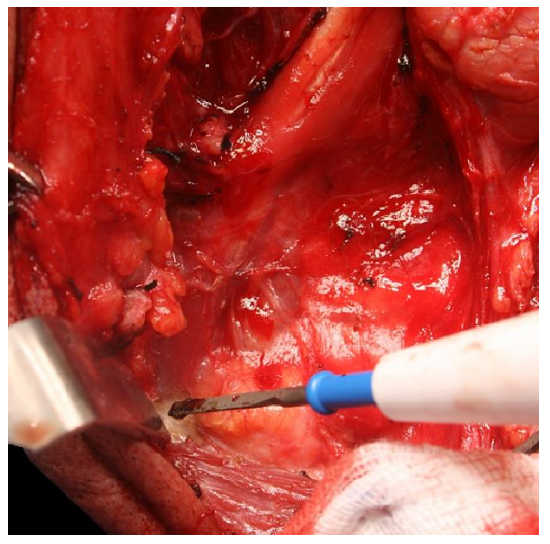
Figure 22: Dissect the entire length of the digastric
Next identify the XIIn below the greater cornu of the hyoid bone before it crosses the external carotid artery. It is generally more superficial than expected and is located just deep to the veins that cross the nerve. Carefully dissect in a posterior direction and divide the veins to expose the XIIn (Figure 23).
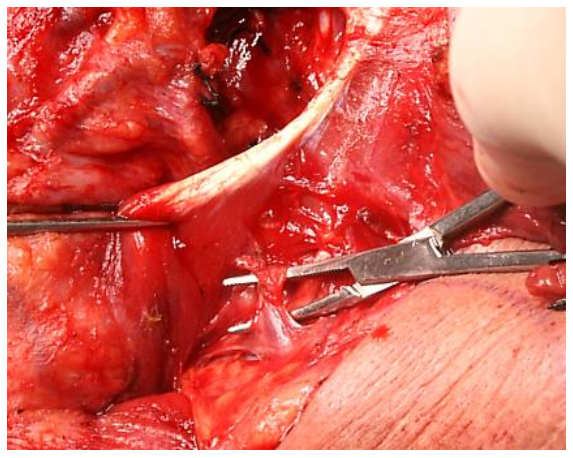
Figure 23: Dividing the veins that cross the XIIn
After the nerve has crossed the external carotid artery, identify the sternomastoid branch of the occipital artery that tethers the XIIn (Figure 24).
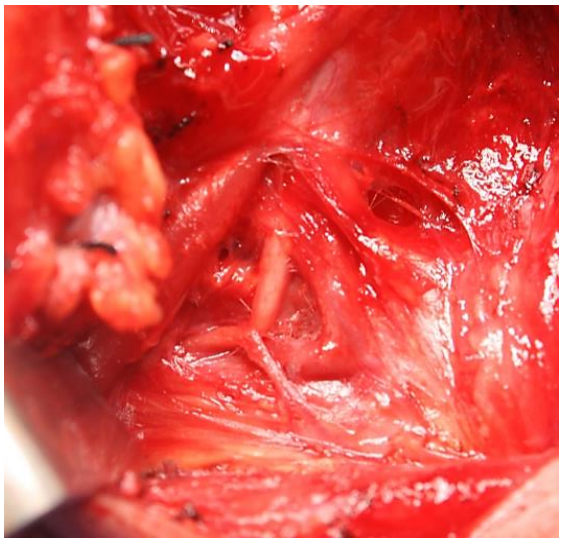
Figure 24: Sternomastoid branch of occipital artery tethering the XIIn
Dividing this artery releases the XIIn (Figure 25). The nerve then courses vertically and leads the surgeon directly to the anterior border of the IJV (Figure 25).
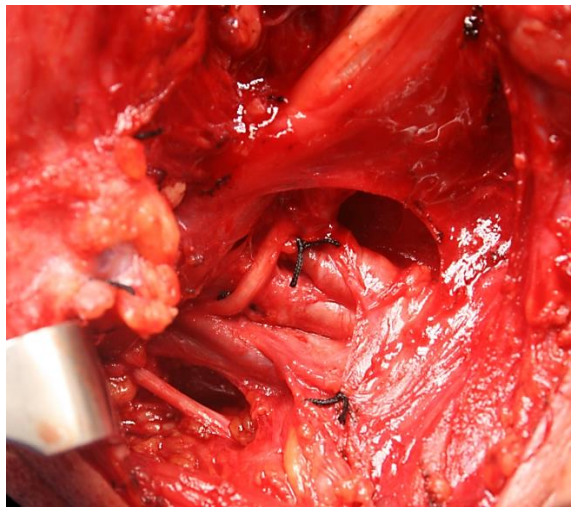
Figure 25: Dividing the sternomastoid branch of the occipital artery frees the XIIn that then leads directly to IJV. Note the XIn and the tunnel created behind IJV
Step 4 (Figure 7)
Using dissecting scissors or a hemostat to part the fatty tissue in Level II, the surgeon next identifies the XIn which may course lateral, medial or very rarely through the IJV (Figure 26).
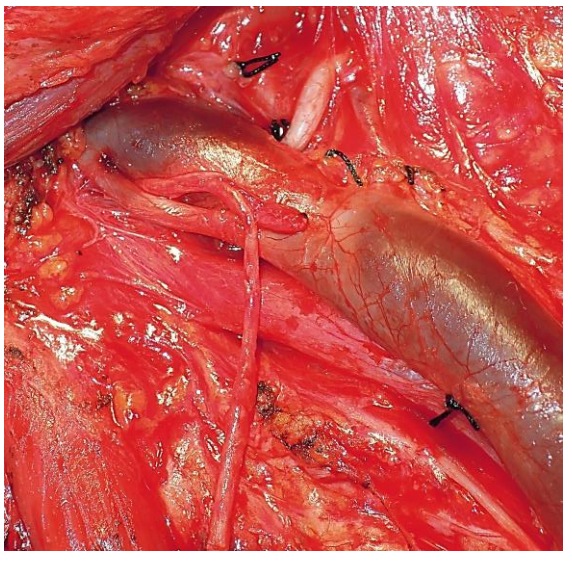
Figure 26: XIn passing through the IJV
Create a tunnel immediately posterior to the IJV (Figure 25). This maneuver speeds up the subsequent dissection of Level 2 (Steps 4 & 7). The transverse process of the C1 vertebra can be palpated immediately posterior to the XIn and IJV and serves as an additional landmark for these structures in difficult surgical cases. Note that the occipital artery crosses the IJV at the top of Level II, branches of which may need to be cauterized should they be severed while dissecting in Level II.
Step 5 (Figure 7)
Surgery now is directed at the anterior neck. The surgeon raises an anteriorly based subplatysmal flap and exposes the omohyoid muscle and the SCM muscle inferiorly down the clavicle, leaving the anterior jugular vein in the elevated flap (Figure 27). The anterior margin of the omohyoid corresponds with the anterior margin of the neck dissection.
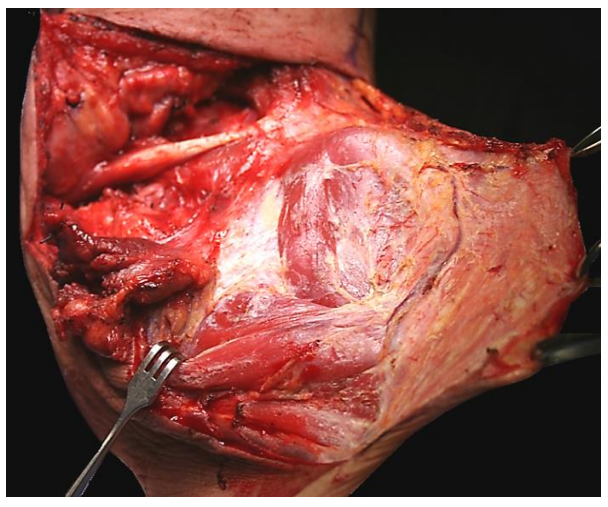
Figure 27: Anteriorly based flap elevated to expose the omohyoid and SCM
The omohyoid is divided with cautery and freed up posteriorly with the surrounding fatty tissue of Levels II and III (Figure 28). Finger dissection deep to the omohyoid after it disappears behind the SCM exposes the carotid sheath.
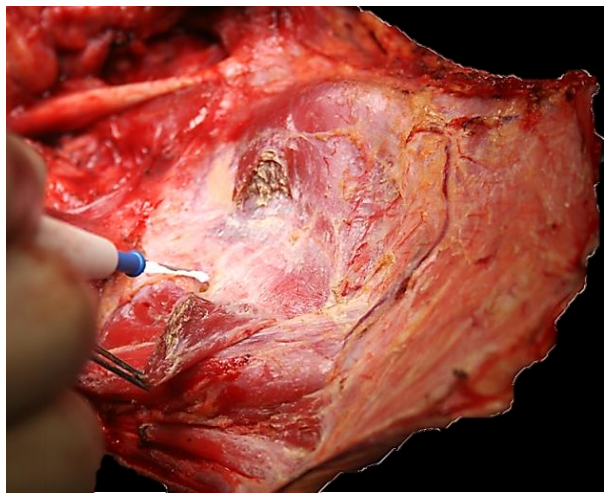
Figure 28: Dividing the omohyoid and clearing Levels II and III
Step 6 (Figure 7)
The surgeon elevates a posteriorly based flap using electrocautery or a knife, with good counter traction provided by an assistant. The platysma is often absent posteriorly and the flap may be very thin. Placing the index finger behind the flap permits the surgeon to gauge the thickness of the flap and avoid “buttonholing” the skin (Figure 29).
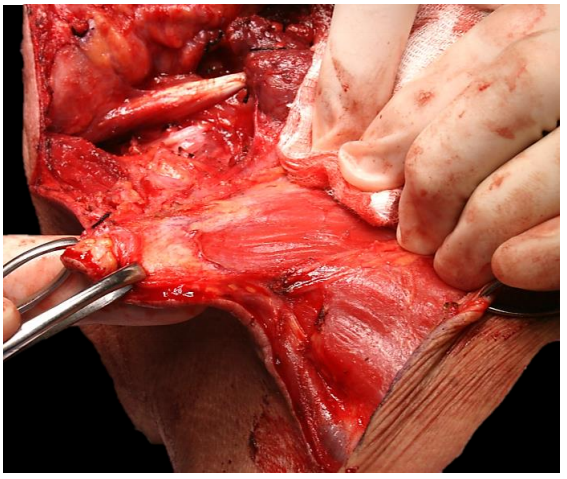
Figure 29: Technique of elevating the posterior skin flap
Take care not to elevate the external jugular vein or the greater auricular nerve with the flap, but to leave them lying on the SCM muscle. Movement of the shoulder is noted as one approaches the XIn or the trapezius muscle. The dissection continues until the anterior border of trapezius is reached (Figure 30). In a thin patient the XIn may be extremely close to skin. Note that the XIn, unlike branches of the cervical plexus, passes deep to the trapezius muscle.
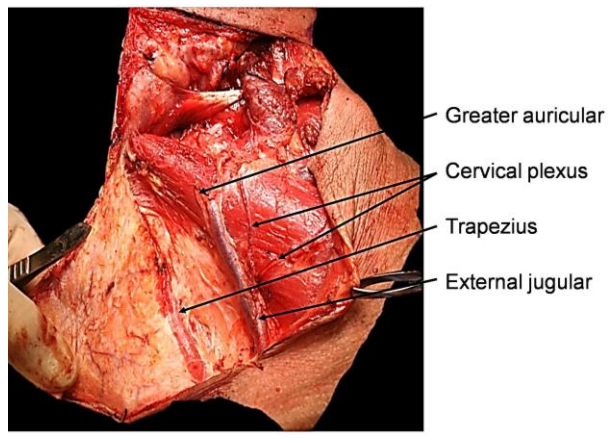
Figure 30: Posterior flap fully elevated to the trapezius muscle
Step 7 (Figure 7)
This step involves dissecting out the XIn and mobilizing Level IIb. The XIn is identified by dissecting with a hemostat at the posterior border of the SCM muscle, approximately 1-2 cm posterior to the point where the greater auricular nerve curves around the muscle (Figure 31). The nerve is often located by seeing movement of the shoulder due to mechanical stimulation of the nerve. The XIn passes through the SCM, unlike the cervical plexus that passes deep to the muscle. It is dissected up-ward through the SCM muscle by tunnel-ing though the muscle over the nerve with a hemostat, and the cutting the muscle with diathermy (Figure 32). The lesser occipital nerve (C2) crosses the XIn at the inferior margin of the SCM (Figure 33). Take care not to mistake it for the XIn when dissecting superiorly through the SCM muscle.
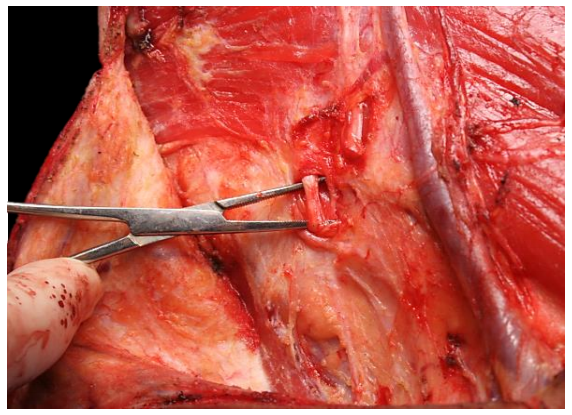
Figure 31: The XIn is located 1-2 cm behind the greater auricular nerve
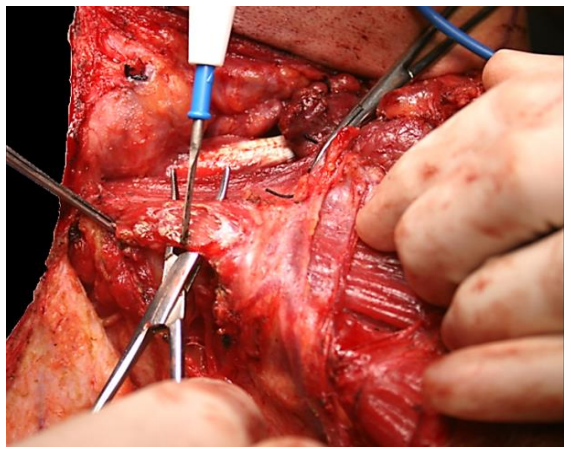
Figure 32: XIn is dissected upward through the SCM muscle
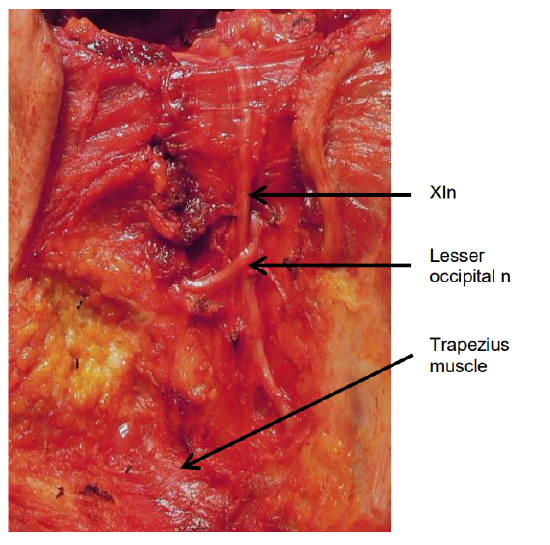
Figure 33: The lesser occipital nerve (C2) can be confused with the XIn
Once the XIn has been exposed up to and freed from the IJV, expose the nerve distally to where it disappears behind the trapezius muscle, and then free the nerve completely and section the branches to SCM (Figure 34, 35).
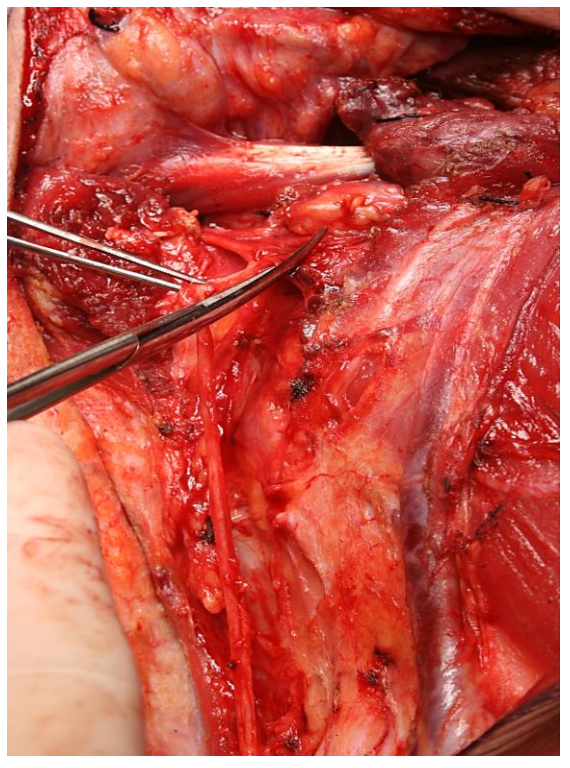
Figure 34: Free the XIn and divide its branches to SCM
Step 8: (Figure 7)
This step involves dissection of Level IIb and transposition of the XIn. The SCM is divided below the mastoid. This exposes fat at the top of Level IIb. The dissection is carried deeper until the deep muscles of the neck that run in a posteroinferior direction appear. The only structure that can be injured here is the occipital artery, and this is simply ligated or cauterized. The dissection is then directed posteroinferiorly, where the greater occipital nerve (C1) is divided (Figure 36).
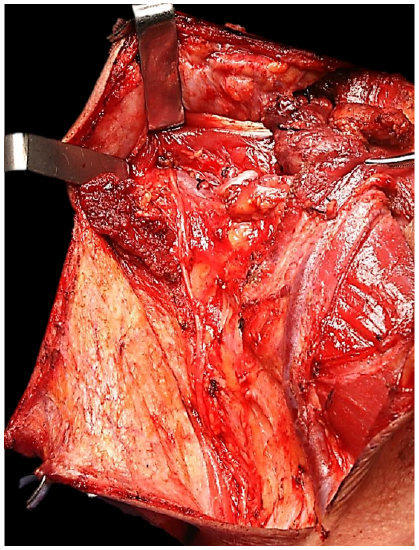
Figure 35: Operative field at end of Step7; note divided SCM along course of XIn
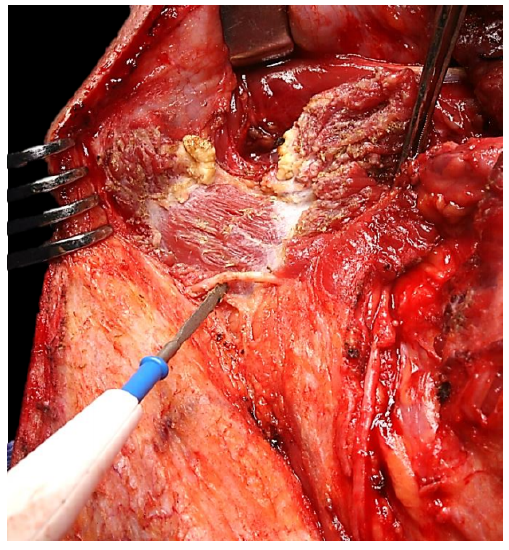
Figure 36: Division of SCM and identification and division of greater occipital nerve and deep muscles of the neck
The contents of Level IIb and IIa are then dissected off the deep muscles of the neck deep to the epimysium until the upper branches of the cervical plexus come into view (Figure 37). The XIn is now trans-located posteriorly (Figure 38). Figure 39 illustrates the status of the neck dissection at this point.
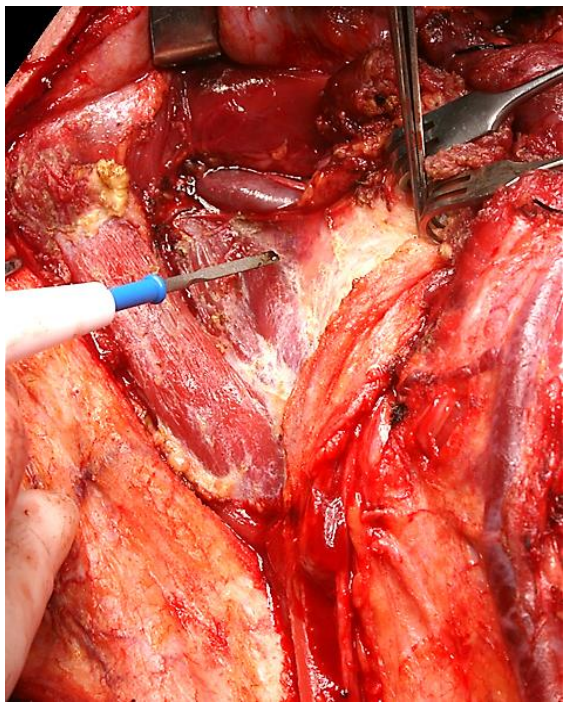
Figure 37: Dissecting Level II
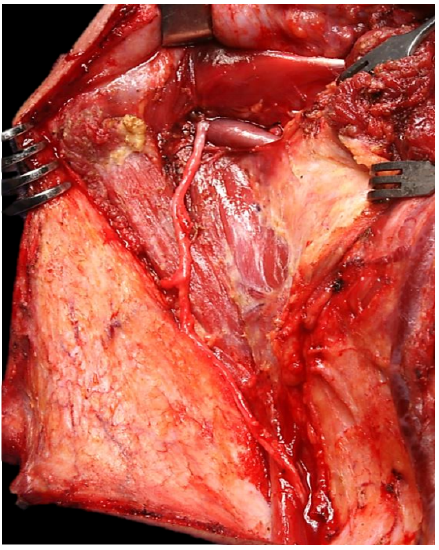
Figure 38: The XIn has been translocated posteriorly
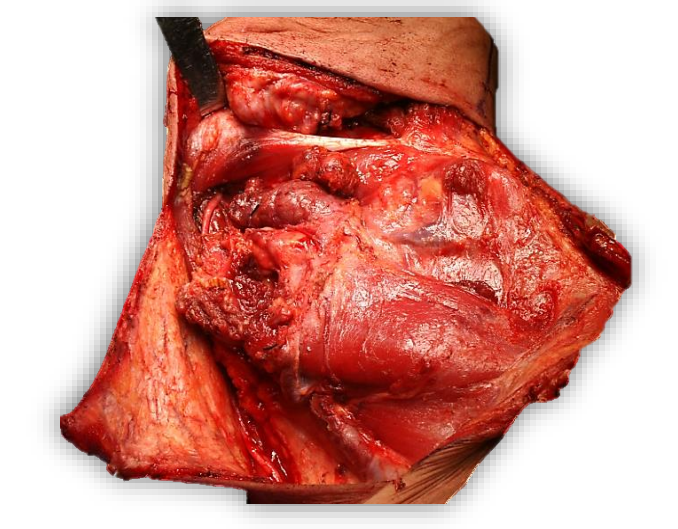
Figure 39: Status of neck dissection before proceeding to Step 9. Note the transected SCM superiorly
Step 9: (Figure 7)
The clavicular and sternal heads of the SCM are next divided with cautery just above the clavicle (Figure 40).
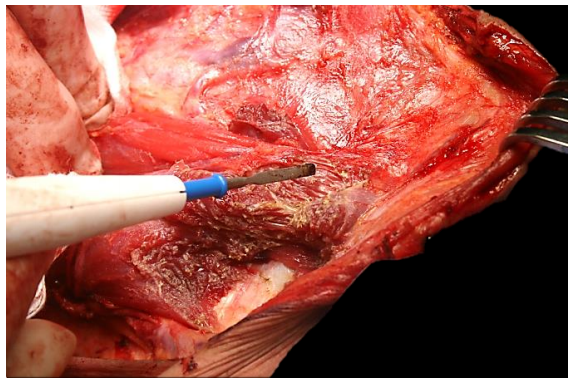
Figure 40: Transecting the sternal head of the SCM
The surgeon applies continuous traction to the muscle during the dissection to part the muscle fibres as they are transected and to visualise the IJV immediately deep to the muscle (Figure 41). A scalpel is used to cut through the carotid sheath onto the IJV (Figure 41).
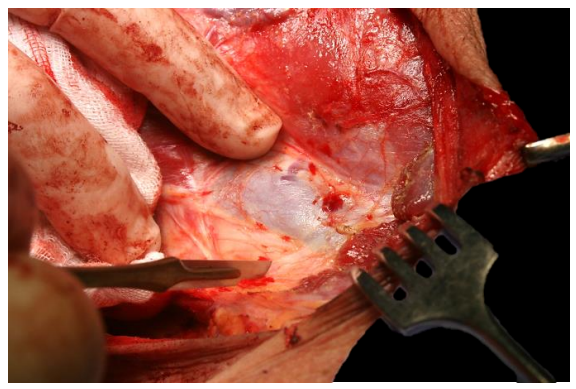
Figure 41: Exposing the IJV by incising the carotid sheath
Take care not to dissect immediately lateral to the IJV, as the right lymphatic duct (right neck) or thoracic duct (left neck) may be injured leading to a troublesome chyle leak (Figure 42).
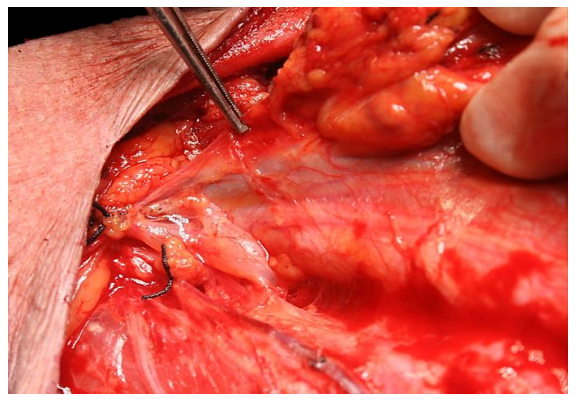
Figure 42: A distended thoracic duct immediately lateral to the carotid artery and IJV in the (L) neck
Next identify the external jugular vein and the omohyoid muscle (Figure 43).
The external jugular vein is divided and ligated, followed by division of the omohyoid with cautery (Figures 44, 45).
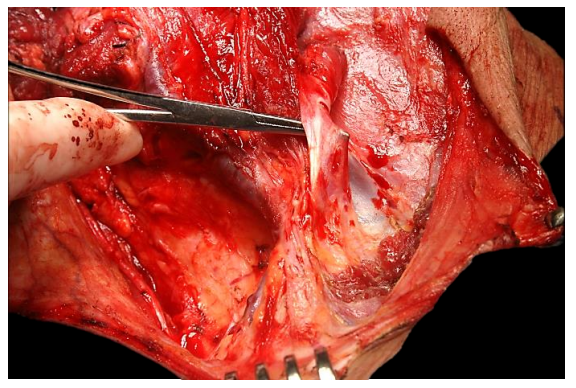
Figure 43: The hemostat is under the omohyoid; the external jugular vein is more posteriorly
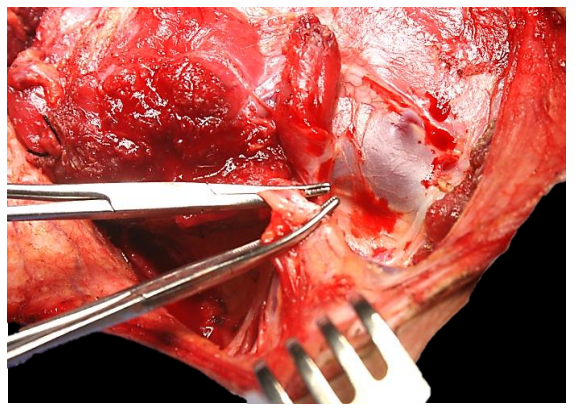
Figure 44: External jugular vein is divided
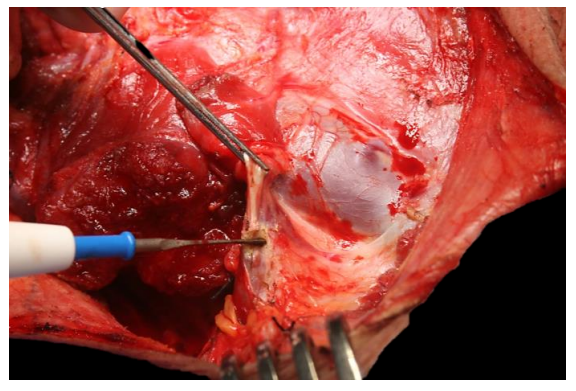
Figure 45: Division of the omohyoid with cautery
The surgeon then incises the fascia overlying the supraclavicular fat just above the clavicle, once again steering clear of the right lymphatic duct or thoracic duct (Figure 46).
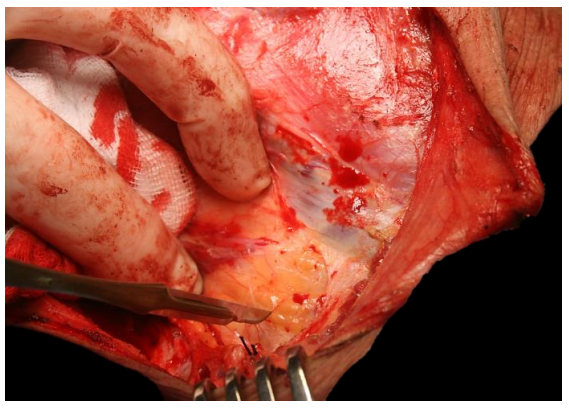
Figure 46: Exposing the supraclavicular fat
Once the fat has been exposed, a finger can be used to expose the fascia covering the brachial plexus (Figure 47). The finger is then swept medially to expose the phrenic nerve, laterally towards the axilla and superiorly along the carotid sheath. Take care not to tear the transverse cervical vessels with the medial sweep.
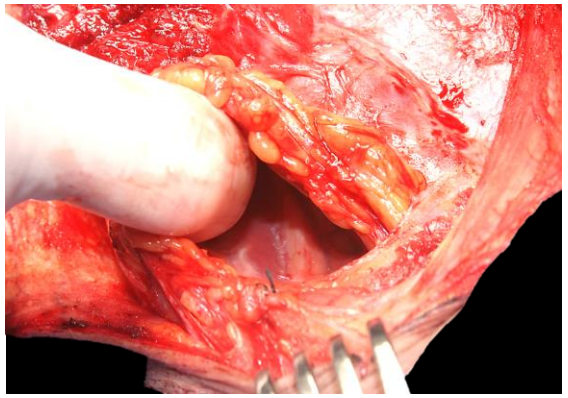
Figure 47: Exposing the brachial plexus
Step 10: Supraclavicular vascular pedicle (Figure 7)
This step involves freeing the inferolateral part of Level V. First identify and divide the supraclavicular nerves, which are branches of the cervical plexus (Figure 48).
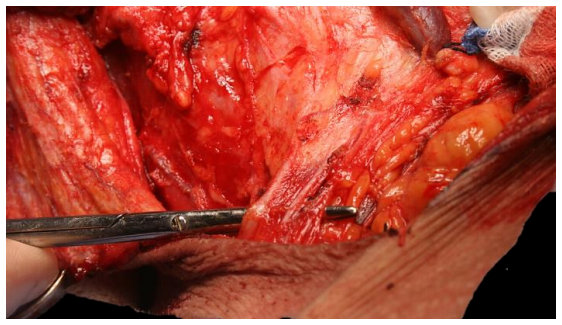
Figure 48: The supraclavicular nerves
Next incise the fatty vascular pedicle containing the transverse cervical artery and vein (Figure 49).
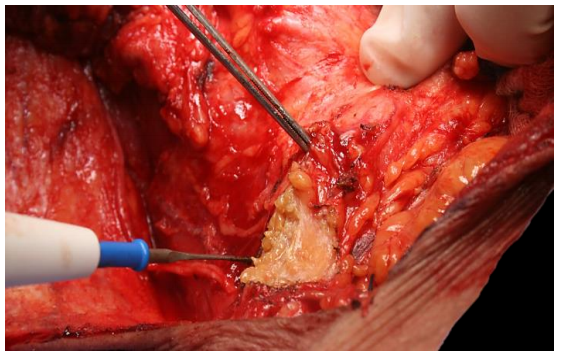
Figure 49 Note the proximity of the XIn (below the diathermy) when dividing the vascular pedicle.
Figures 50 and 51 demonstrate the isolation and division of the transverse cervical artery and its proximity to the XIn
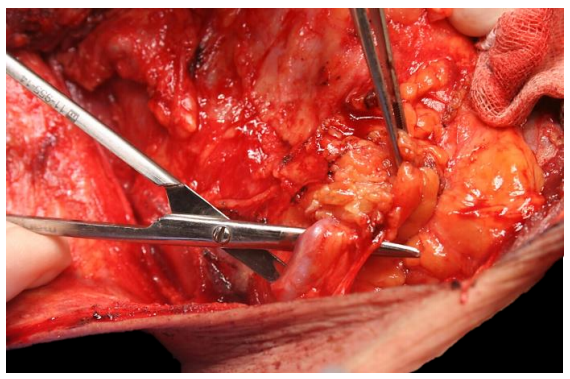
Figure 50: Transverse cervical vessels
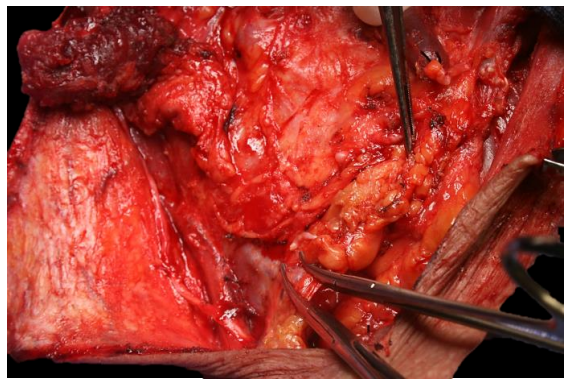
Figure 51: Division of transverse cervical vessels
Step 11: (Figure 7)
This part of the neck dissection involves anterograde dissection of Levels II – V and is done with a scalpel. The assistant maintains firm anterior traction on the neck dissection specimen, and the surgeon establishes a subepimysial dissection plane on the deep muscles of the neck, except over the brachial plexus where the overlying fascia is retained to protect the nerves (Figure 52).
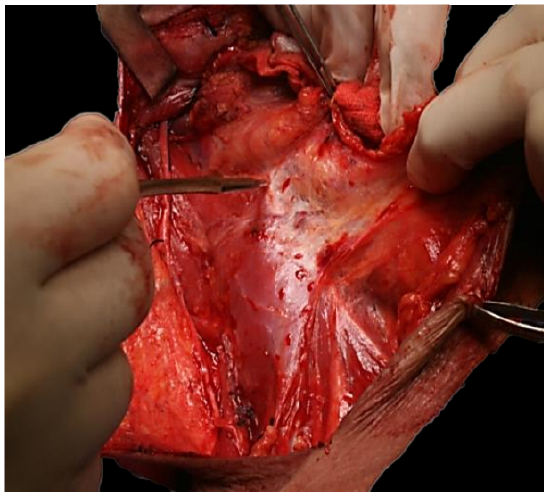
Figure 52: Anterograde dissection of Levels II – V
The dissection proceeds over a broad front until the entire cervical plexus has been exposed.The phrenic nerve is identified as it descends obliquely across the scalenius anterior muscle, deep to the prevertebral layer of deep cervical fascia (Figure 53).
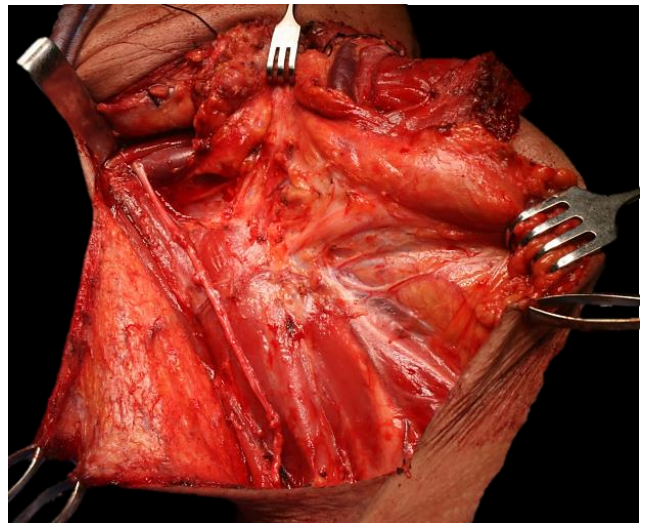
Figure 53: Dissection up to the cervical plexus; note the phrenic nerve running parallel to the IJV.
The cervical plexus nerves are each divided, taking care not to injure the phrenic nerve (Figure 54).
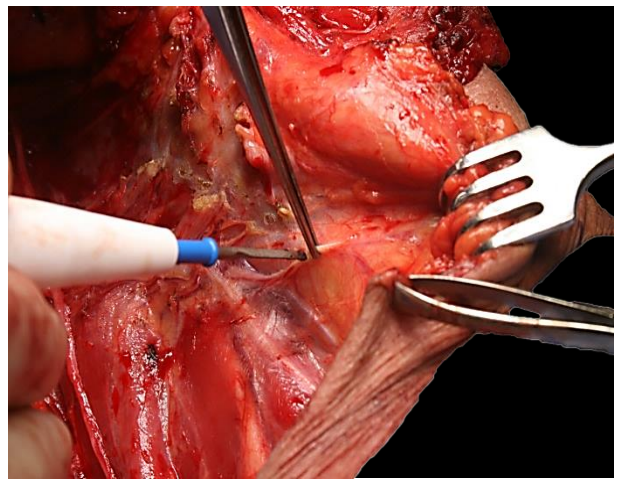
Figure 54: Division of nerves of cervical plexus, staying well clear of the phrenic nerve
This brings the carotid sheath containing common and internal carotid arteries, the vagus nerve and the IJV into view (Figure 55).
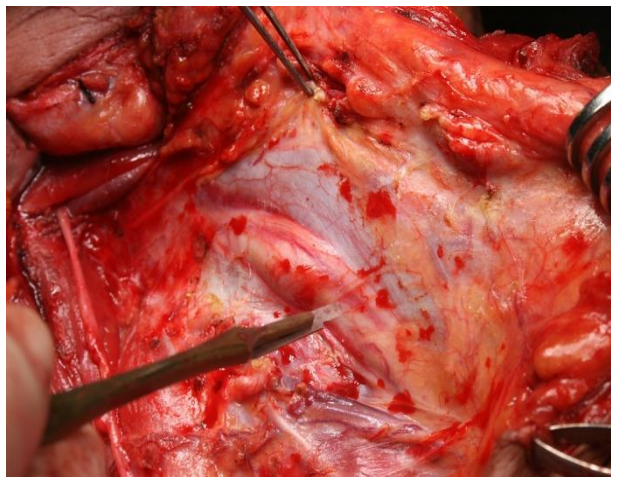
Figure 55: The common carotid artery, the vagus nerve and IJV
The carotid sheath is incised along the full course of the vagus nerve, and the neck dissection specimen is stripped off the IJV while remaining inside the carotid sheath. The ansa cervicalis, which courses either deep or superficial to the IJV may be preserved (Figure 56). Inferiorly the pedicle adjacent to the IJV containing fat, thoracic or right lymphatic duct, and transverse cervical artery and vein is divided, taking care not to include the vagus or phrenic nerves in the pedicle (Figure 57).
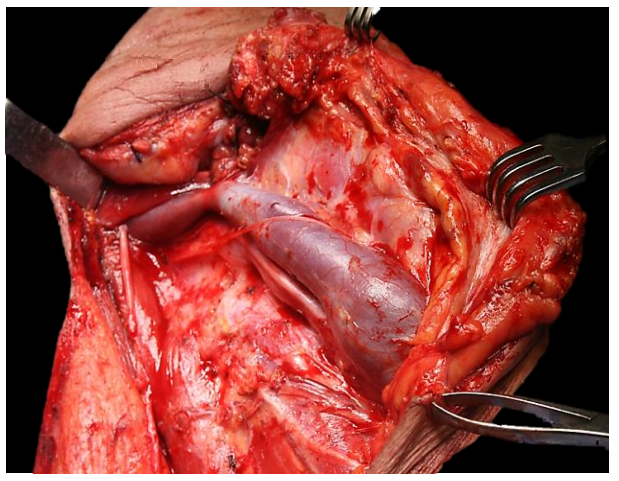
Figure 56: The neck dissection specimen has been stripped off the carotid, vagus and IJV in a plane deep to the carotid sheath; the ansa cervicalis has been preserved
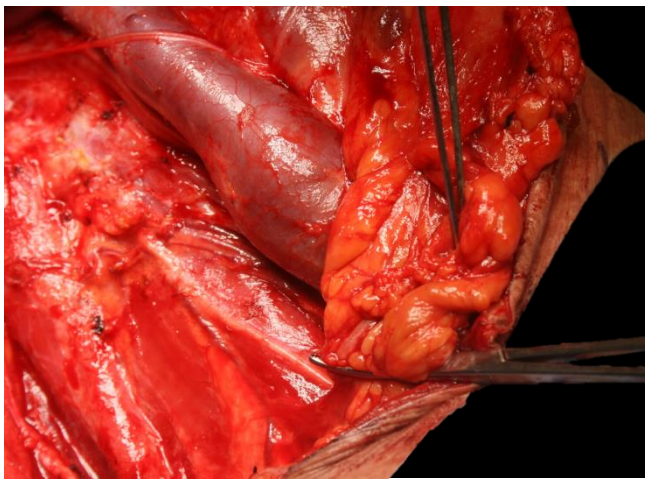
Figure 57: Inferiorly the pedicle adjacent to the IJV is divided; note the proximity of the phrenic nerve
Step 12: (Figure 7)
The final step is to strip the neck dissection specimen off the infrahyoid strap muscles, to identify and preserve the superior thyroid vascular pedicle, and to deliver the neck dissection specimen (Figure 58)
Closure
The neck is irrigated with water, the anesthetist is asked to do a valsalva maneuver to elicit unsecured bleeding vessels and chyle leakage, and a 5 mm suction drain is inserted. The neck is closed in layers with continuous vicryl to platysma and sutures/staples to skin
Postoperative care
The drain is maintained on continuous suction e.g. low-pressure wall suction, until the drainage volume is <50 mL /24 hrs.
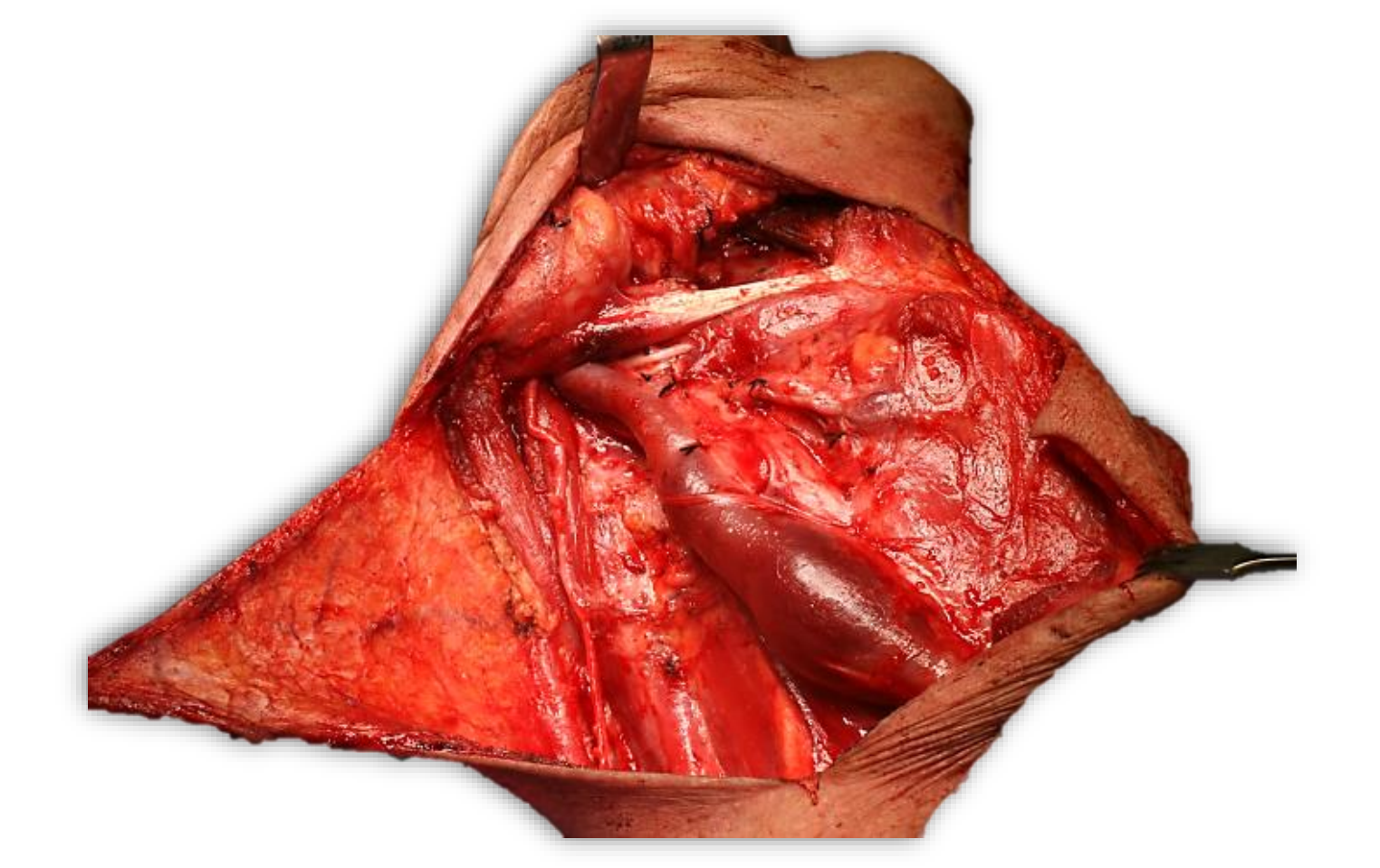
Figure 58: Completed MND type 2; note the superior thyroid pedicle and ansa cervicalis
Useful References
- Robbins KT, Shaha AR, Medina JE, et al. Consensus statement on the classification and terminology of neck dissection. Arch Otolaryngol Head Neck Surg 2008;134: 536–8
- Ferlito A, Robbins KT, Shah JP, et al Proposal for a rational classification of neck dissections. Head Neck. 2011 Mar;33(3):445-50
- Harris T, Doolarkhan Z, Fagan JJ. Timing of removal of neck drains following head and neck surgery. Ear Nose Throat J. 2011 Apr;90(4):186-9
Author & Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za

The Open Access Atlas of Otolaryngology, Head & Neck Operative Surgery by Johan Fagan (Editor) johannes.fagan@uct.ac.za is licensed under a Creative Commons Attribution - Non-Commercial 3.0 Unported License



