1.28: Percutaneous Dilational Tracheostomy
- Page ID
- 17651
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
PERCUTANEOUS DILATIONAL TRACHEOSTOMY TECHNIQUE
Thomas Deitmer, Johan Fagan
Percutaneous tracheostomy is a bedside procedure requiring a small surgical field and avoiding the need for an operating room. It was popularized in the 1990s as a minimally invasive technique requiring only a small skin incision. The widespread adoption of percutaneous techniques is in the opinion of the authors due to the possibility it gives ICU physicians to immediately perform a percutaneous tracheostomy for ventilation purposes once the need for tracheostomy has been identified, with its organizational and cost advantages.
Typically percutaneous tracheostomy is done by ICU physicians, although it should only be employed if a surgeon experienced with classic open tracheostomy and with coping with complications such as bleeding is immediately available to help.
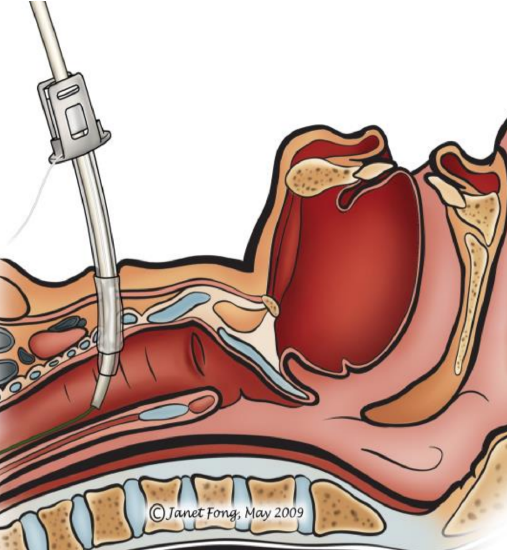
Figure 1: Tracheostomy tube being advanced over the trocar which has been passed over the guide wire (green)1. Note that the puncture site is too high…it should be below the 1st tracheal ring!
Percutaneous tracheostomy is similar to using a Seldinger technique to cannulate veins and arteries. The trachea is entered percutaneously with a thin needle through which a guide wire is advanced into the trachea. A bougie is passed over the guide wire and the tract between the skin and trachea is dilated until a tracheostomy tube can be advanced into the trachea (Figure 1). Unlike with conventional surgical tracheostomy, the trachea, thyroid gland and vascular structures cannot be visualized during placement of the tracheostomy or to achieve haemostasis should bleeding occur.
During the 1st weeks the tract between skin and trachea is unstable. The tract collapses with removing the tube during this time and makes reinserting a tube difficult and hazardous. Only after several weeks the tracheostomy tract is stabilized by granulation tissue making changing a tube possible.
Indications
Percutaneous dilational tracheostomy is indicated for selected ventilator-dependent patients in ICU, e.g. for prolonged transoral or transnasal endotracheal intubation.
Contraindications
Inability to palpate thyroid and cricoid cartilages: The tracheostomy should enter the trachea between the 1st and 3rd tracheal rings, and should avoid the cricoid and thyroid cartilages. It is therefore crucial that one is able to clearly palpate and identify the thyroid and cricoid cartilages. With a fat neck or a goiter one cannot always palpate the laryngeal and tracheal structures, and one ends up with a very long tracheostomy tract which may create complications.
Anatomical factors: Laryngeal and tracheal anatomy may vary widely depending on the patient and his/her age. A larynx situated in the thoracic inlet (laryngoptosis) makes all kinds of tracheostomy difficult and one gets critically close to big mediastinal vessels. In such cases open dissection under direct surgical vision is required.
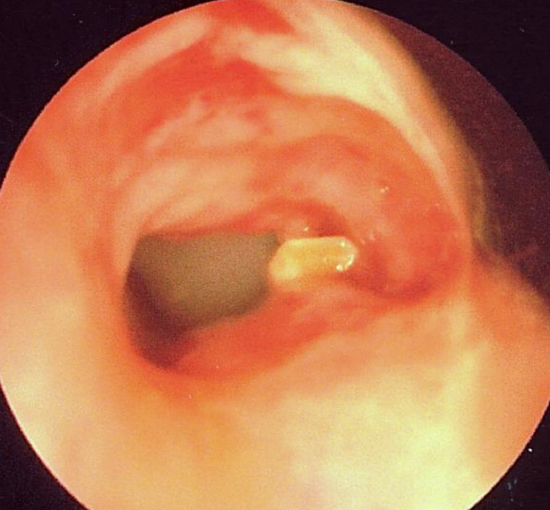
Figure 2: Fractured tracheal ring
Thyromegaly or suprasternal mass: Any mass between the skin and trachea such as an enlarged thyroid or a tumor is a contraindication to percutaneous tracheostomy. The thyroid gland and most tumors are vascular. Should bleeding occur following puncture and dilatation, one can compress the site. Subcutaneous bleeding may not be apparent with a tight skin collar. Bleeding can however enter the opened trachea as the hole in the trachea may be irregular especially in elderly patients with partial ossification of the tracheal rings that may even fracture (Figure 2).
Coagulation disorders: Percutaneous tracheostomy is contraindicated. The only means of hemostasis for bleeding from the tract is by compression with the dilating device or by exploring the neck.
Children: The authors do not advocate percutaneous tracheostomy in children <15 years of age as it is difficult to palpate the trachea because of its small diameter and because the cartilage rings are soft and compressible. Some force is also required to perforate the skin and trachea which diminishes the tracheal AP-diameter and increases the likelihood to perforate the paries membranaceus (very thin, vulnerable posterior tracheal wall).
Patients requiring a tracheostomy after leaving ICU: A percutaneous tracheostomy tract will collapse for several weeks when the tube is removed to be changed. In ICU there is expert care to maintain a tracheostomy e.g. humidification and frequent suctioning to prevent crusting and obstruction. The tracheostomy may have to be changed immediately if obstruction occurs. This may not be possible in fresh percutaneous tracheostomies for the reasons given; hence emergency transoral intubation may be required and must be at hand. Therefore, if a patient is planned to have a tracheostomy for longer than his/her presence in ICU, an open, stable, surgical tracheostomy must be done which permits simple tube changes. This would include patients with poor lung function requiring prolonged weaning, or patients with dysphagia and aspiration that need prolonged rehabilitation and a protective tracheostomy.
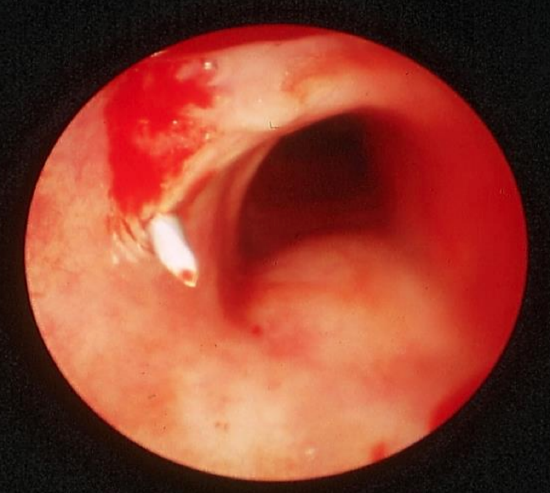
Figure 3: Puncture needle entering the sidewall of the trachea
Unavailability of flexible or rigid bronchoscope and/or ultrasound: Finding and entering the trachea with a pilot needle may be difficult. One can of course aspirate air and guess that you are within the trachea. This does not however ensure that the trachea has been entered in the midline as air will be aspirated even with a laterally placed puncture which is not at all suitable for a dilatation manoeuvre (Figure 3).
Therefore, the tracheal puncture must be controlled by endoscopic vision. This is best achieved with a flexible endoscope that is guided through the endotracheal tube while in situ. The endotracheal tube is withdrawn to clearly reveal the anatomy of the lower larynx and trachea. Alternatively, tracheoscopy can be performed with a rigid scope, in which case the endotracheal tube is pulled back and ventilation is secured through the rigid scope. Sonography may also be employed to ensure correct placement of the tracheal puncture.
Difficult airway: The patient must be easy to intubate in the event that alternative techniques of ventilation by oro- or nasotracheal intubation is required should the patient’s airway obstruct following removal of the endotracheal tube e.g. with incorrect placement of the percutaneous tracheostomy, accidental decannulation, bleeding etc.
Emergency procedures: Dilational tracheostomy should not be used in airway emergencies. Flexible or rigid tracheoscopy should be available (which is typically not the case in emergencies). Emergency access to the trachea should in such cases be achieved by cricothyroidotomy.
Surgical Technique: General principles
Several percutaneous dilational tracheostomy devices are commercially available. Each uses different tools and different surgical steps. It is advisable to stick to one system for reasons of quality assurance.
The trachea is first punctured with a small pilot cannula; next the tract is dilated into the trachea; finally the tracheostomy tube is inserted from externally into the trachea. It is strongly recommended that the tracheal puncture is done under endoscopic control. There is a technique that places the cannula from inside-to-outside as a translaryngeal pull-through technique.
- Three doctors are required: an ICU physician to take care of the patient’s ventilation and sedation; an “endoscopist” to perform flexible tracheoscopy to direct the tracheal puncture and the insertion of the tube, and a “surgeon” to perform the percutaneous tracheostomy.
- Position the patient supine with neck extended by a pillow or sandbag placed under the shoulders in order to deliver the trachea out of the thorax and to give the surgeon adequate access to the cervical trachea. Such extension may not be possible in patients with neck injuries, or rheumatoid and osteoarthritis of the cervical spine.
- Palpate and identify the thyroid cartilage, cricoid cartilage and trachea, and exclude a large thyroid gland. The tracheostomy is created below the 1st tracheal ring, so as to avoid subglottic stenosis as a result of scarring. Therefore palpating to determine the location of the cricoid cartilage is important. When you run your fingers up the midline of the neck starting inferiorly at the sternal notch, you 1st encounter the prominence of the thyroid isthmus, followed by the cricoid.
- Infiltrate skin and subcutaneous tissues in the midline overlying about the 3rd tracheal ring with local anesthesia with adrenaline.
- Sterilize and drape the anterior neck as for a classic tracheostomy.

Figure 4: Red arrow indicates point of entry of endoscope into swivel adaptor of anesthetic tubing
- The “endoscopist” introduces a flexible scope into the endotracheal tube through a swivel adapter without interrupting the ventilation (Figure 4).
- Advance the endoscope to the tip of the endotracheal tube.
- Carefully retract the endotracheal tube into the larynx under endoscopic vision, taking care not to deflate the cuff of the endotracheal tube.
- Do not to remove the endotracheal tube so that one can advance the endotracheal tube immediately if controlled ventilation is required in a critically ill patient.
- The “surgeon” again palpates and locates the thyroid and cricoid cartilages.
- While fixing the larynx with fingers of the non-dominant hand, insert the small needle, aiming at the 2nd/3rd tracheal rings.
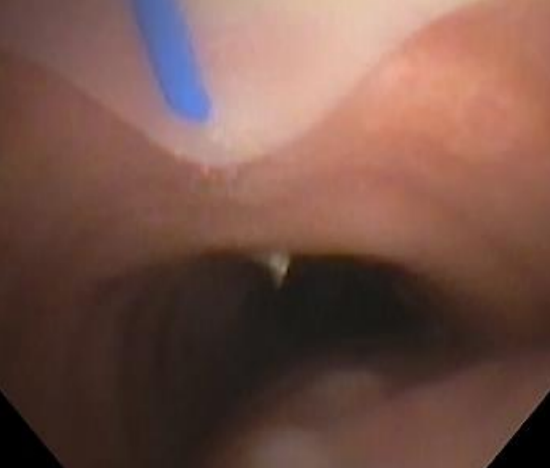
Figure 5: Entry of the needle into trachea in correct position2
- The “endoscopist” monitors entry of the needle into the trachea and ensures that it is the correct position (Figure 5).
- Midline of trachea
- Not too high (touching cricoid)
- Not too low (creates very long tracheostomy tract between skin and trachea)
- Once satisfied with placement of the needle in the trachea, insert a guidewire through the needle and advance it into the tracheal lumen.
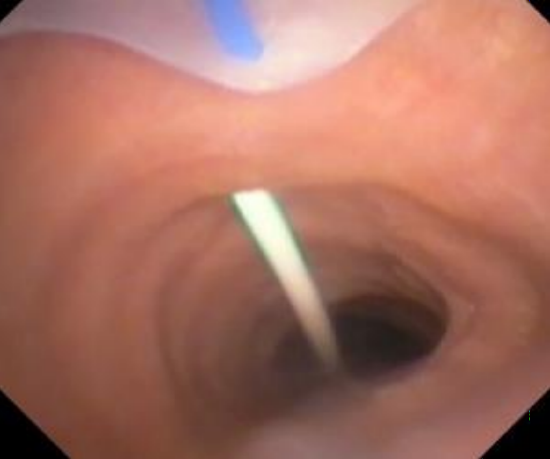
Figure 6: Guidewire in place following retraction of needle2
- Retract the needle leaving the guidewire in situ (Figure 6).
- Make a small skin incision at the point of insertion of the guide wire.
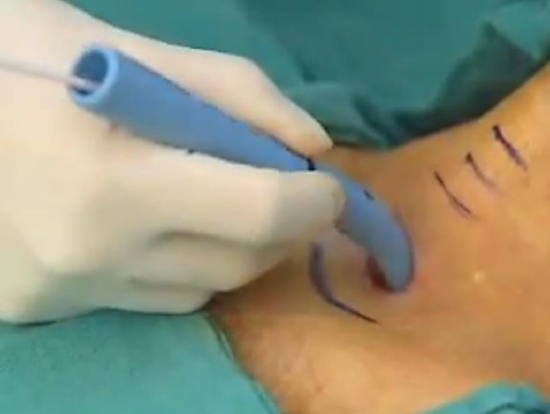
Figure 7: Dilating the tract
- Dilate the tract following the detailed instructions of the percutaneous tracheostomy kit being used (Figure 7).
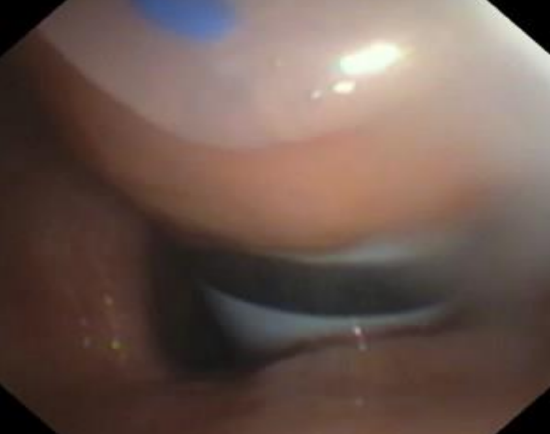
Figure 8: Endoscopic view of Blue Rhino dilator entering the trachea2
- The “endoscopist” monitors the procedure from inside the trachea to ensure correct placement of the opening into the trachea, and to avoid fracture of cartilage, bleeding, or injury to the posterior tracheal wall (Figure 8).
- With the tract fully dilated, railroad the tracheostomy tube into its final position.
- Remove the dilator.
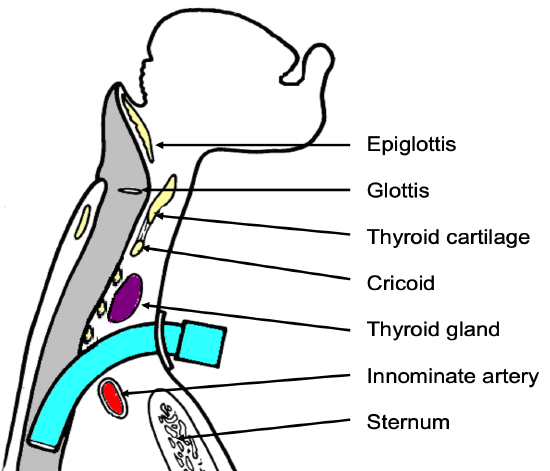
Figure 9: Position of tracheostomy tube
- Inflate the cuff, attach the anesthetic tubing, and hand-ventilate until correct placement of the tube within the trachea has been confirmed (Figure 9).
- Secure the tracheostomy tube to the neck with tapes. Thread the tapes through the holes in the flanges of the tracheostomy tube and pass it around the neck and tie them with the neck flexed.
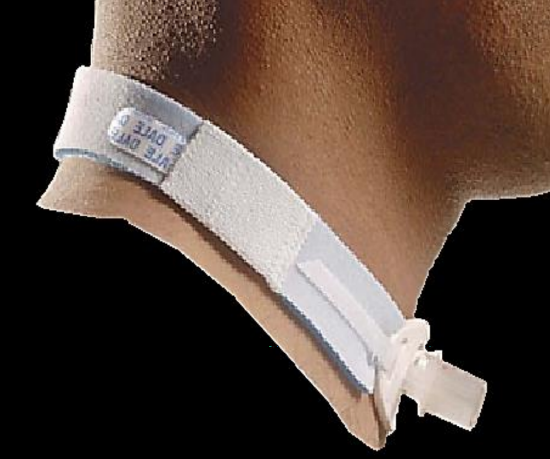
Figure 10: Tracheostomy tube secured with Velcro tape
- If the ties are tied with the neck extended, they are too loose when the patient flexes the neck. The ties should be tight enough to admit no more than a single finger under the tape (Figure 10).
- Remove the endotracheal tube only once ventilation has been fully established and there are no immediate complications.
- If any doubt exists about correct placement of the tracheostomy tube, endoscopy of trachea should be done through the tracheostomy tube to confirm correct placement.
Commercial percutaneous tracheostomy kits
Commercially available kits vary principally in terms of the dilation instrumentation. Every device is delivered with detailed guidelines which should be referred to before use!
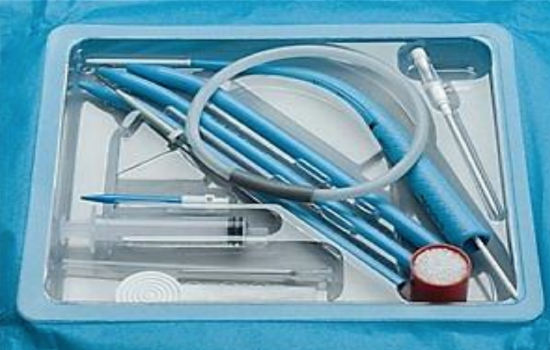
Figure 11: Ciaglia Blue Rhino kit contains needle, guide wire, and serial dilators
The Ciaglia Blue Rhino & Dolphin systems use serial dilators to dilate the tract over a guide wire, and the tracheostomy tube is advanced over the final dilator (Figures 1, 11).
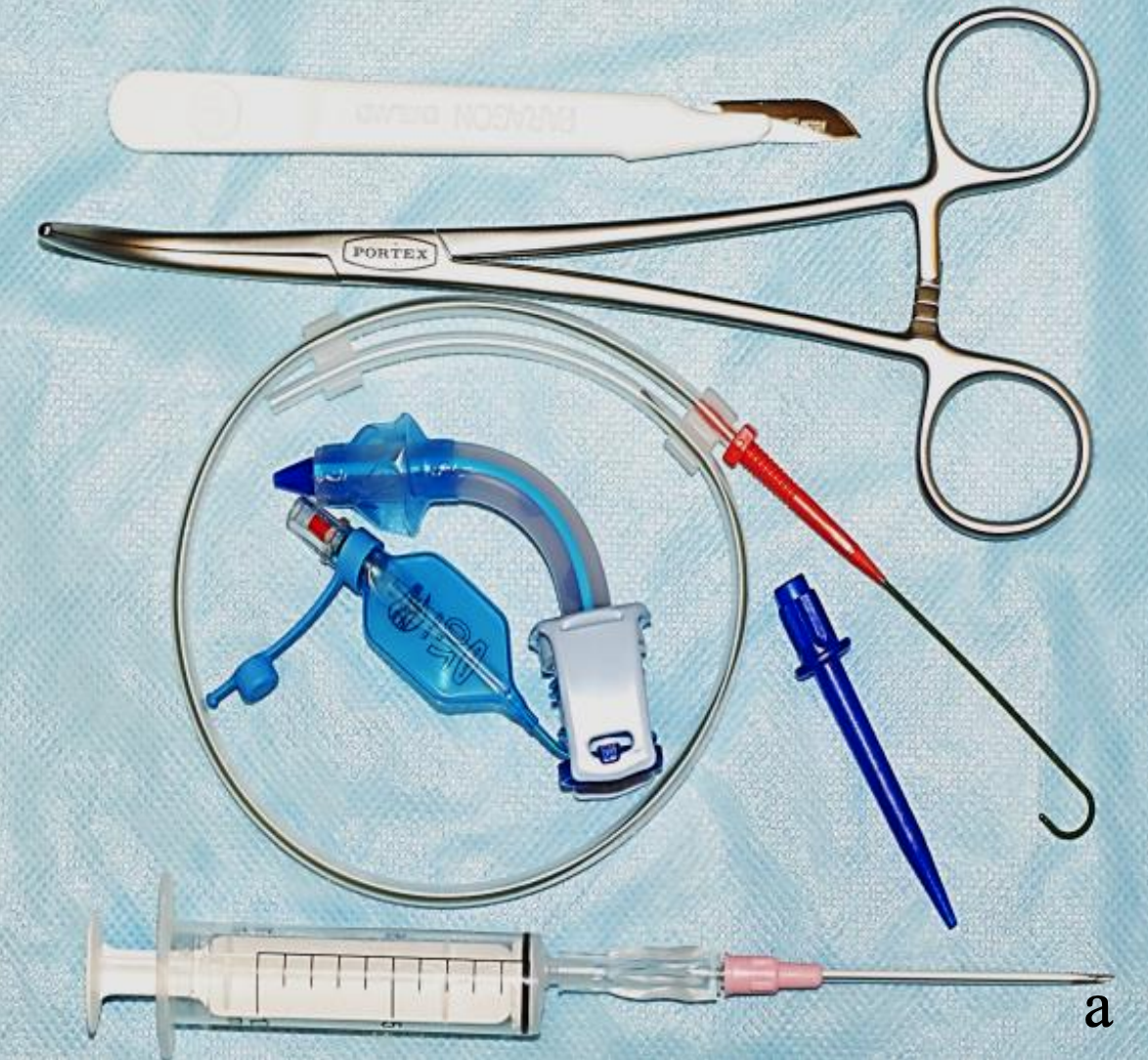
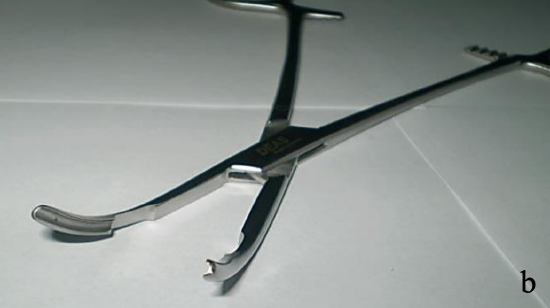
Figures 12a,b: Griggs kit with grooved forceps to accommodate the guidewire
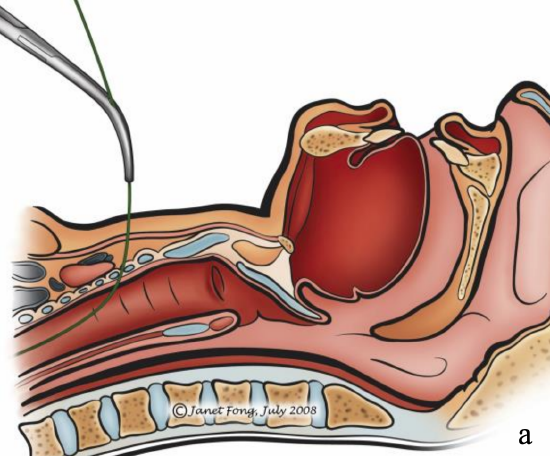
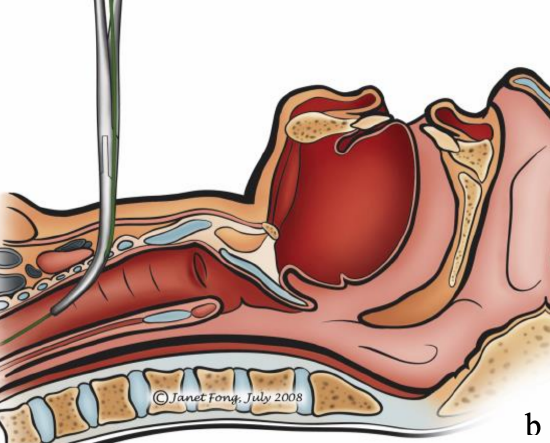
Figures 13a,b: Forceps being advanced over the guidewire1
With the Griggs and Rapitrach systems the tract is dilated with forceps, which is grooved so that it can be advanced over a guidewire (Figures 12, 13).
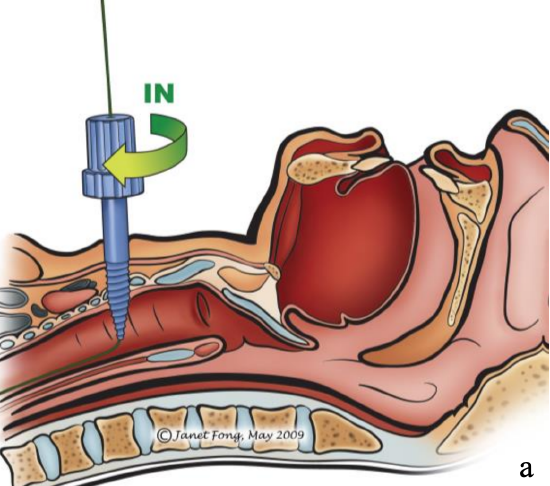
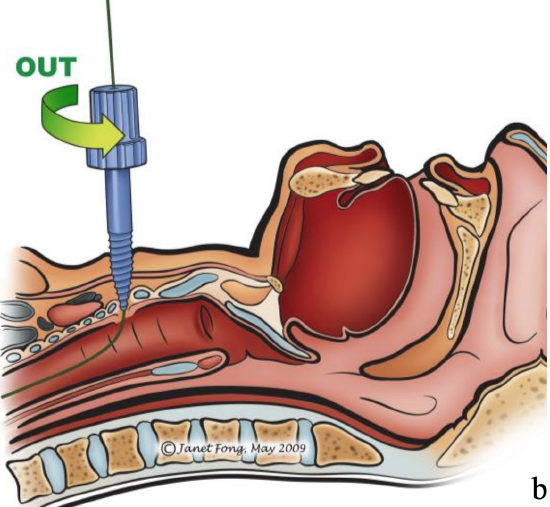
Figures 14a,b: The Percutwist system dilates the tract with a semi-sharp screw over a guide wire1 Note that the puncture site is too high…it should be below the 1st tracheal ring!
The Percutwist system dilates the tract with a conically shaped, semi-sharp screw over a guide wire (Figures 14a, b).
The screw exerts a radial force to open the trachea. Using the screw avoids impressing the anterior tracheal wall and flattening the tracheal lumen in its AP-diameter and, hence injuring the posterior tracheal wall.
Unlike the systems described above, the Fantoni system employs a translaryngeal tracheostomy technique. The tracheostomy tube is inserted by passing it transorally and then inside-out out from the trachea to the cervical skin. The endotracheal tube must first be replaced with a smaller tube. The trachea is then punctured percutaneously with a small needle under endoscopic vision. A metal guide wire is passed through the needle into the trachea and out through the mouth. The end of the guide wire is attached to a special tracheostomy tube with a dilating metal tip where it connects to the guide wire. This device is then drawn through the oral cavity and the larynx into the trachea adjacent to the endotracheal tube, and out through to the neck, by pulling on the guide wire. As the tracheostomy tube ends up with its tip facing upwards towards the larynx, it must be rotated 180° for its tip to be directed towards the carina. This turning procedure is done with a special device and must be carried out very carefully not to injure the larynx or trachea.
Complications and its management
Some complications have already been mentioned under “Indications” and “Contraindications”.
Collapse of tracheostomy tract: The tracheostomy tract collapses every time a tracheostomy tube must be changed, especially in the initial weeks following percutaneous tracheostomy before the tract has matured. This may be particularly dangerous when accidental decannulation occurs in a tracheostomy-dependent patient outside an ICU setting. The solution is to create a formal surgical tracheostomy with a safe, stable tracheostomy tract in patients requiring a long-term tracheostomy.
Bleeding into neck or airway: This can be life-threatening when clots aggregate in the trachea and bronchi, even with the cuff inflated. When clots cannot be removed by suction, they have to be removed like foreign bodies by rigid endoscopy. Therefore if bleeding is encountered during the percutaneous procedure, it has to be converted to a formal surgical tracheostomy so that haemostasis can be achieved. Secondary bleeding also demands surgical revision.
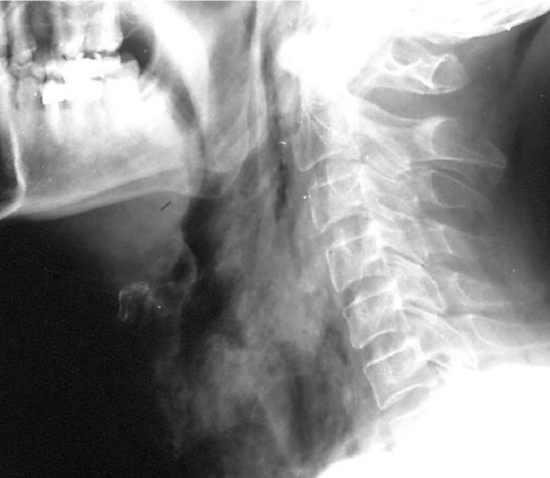
Figure 15: Surgical emphysema
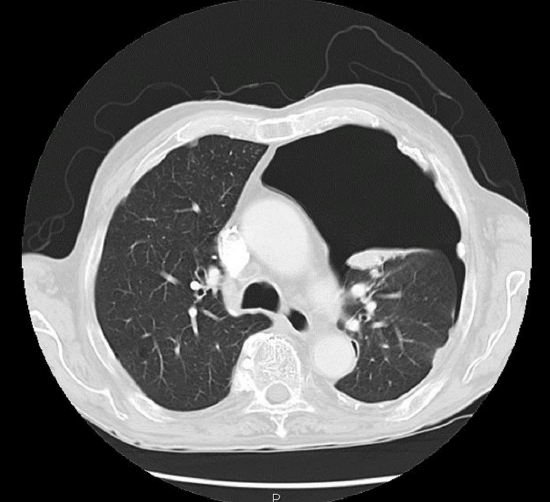
Figure 16: Pneumothorax
Surgical emphysema or pneumothorax (Figures 15, 16): Minor surgical emphysema of the neck can occur following surgical or percutaneous tracheostomy, is often self-limited and sometimes is not even clinically apparent, but apparent only on X-ray or CT-scan. As microbial contamination with air is possible, antibiotics are administered. If emphysema persists or extends into the mediastinum, or if there is a pneumothorax, the situation must be evaluated endoscopically to rule out tracheal perforation or other pathology requiring intervention. A pneumothorax may require an intercostal drain.
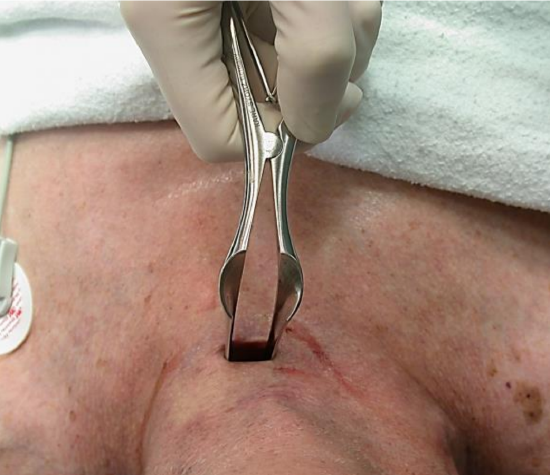
Figure 17: Nasal speculum used to reinsert a percutaneous tracheostomy tube
Accidental decannulation or displacement of tracheostomy tube: When a tracheostomy tube inadvertently slips out of the trachea it may not be possible to reinsert it if it occurs in the initial days after percutaneous tracheostomy because of an immature tracheostomy tract. One can try to probe and redilate the tract using percutaneous tracheostomy instruments or a nasal speculum (Figure 17), and reinsert the tracheostomy tube. In a ventilated patient one needs to immediately intubate the patient with an oro- or nasotracheal tube to continue ventilation. If one is unable to reinsert the tracheostomy, then a formal surgical tracheostomy should be performed.
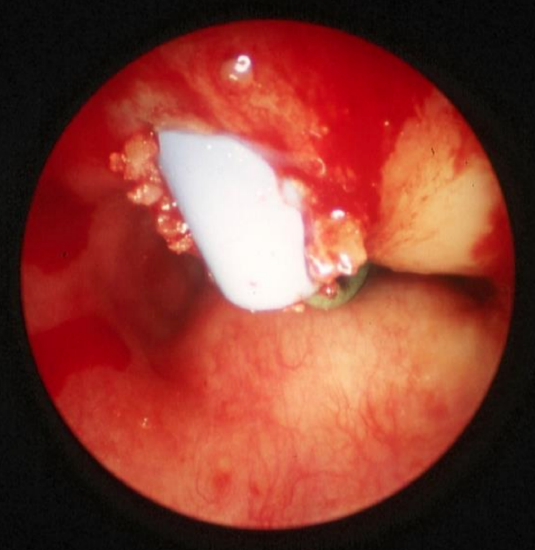
Figure 18: Guidewire impinging on the thin posterior wall of the trachea
Laceration of posterior tracheal wall: Figure 18 illustrates how easy it is to lacerate the posterior tracheal wall. A laceration may be superficial, or can be deep into the mediastinum with fat visible on endoscopy. A laceration may be aggravated by pressure exerted by the cuff. It must be suspected when more and more air in the cuff is required to achieve a seal. The solution is that the cuff of the tracheostomy tube must not be situated over the defect in the posterior tracheal wall. This may require that the tube be advanced so that the cuff is positioned further down the trachea. The cuff position needs to be checked endoscopically and one should ensure that both lungs are ventilated. Alternatively one should reassess whether the patient can be decannulated in order that the lesion can heal without intervention other than broad spectrum antibiotics to prevent mediastinitis. If the above solutions are not feasible, a special endotracheal tube is inserted that straddles the tracheal bifurcation without exerting pressure on the lesion and allows ventilation of both lungs. Such tubes can be passed transorally but may be difficult to pass without further injuring a lacerated trachea. Alternatively one can perform a wide surgical tracheostomy and pass such a tube via the neck. In selected cases when such a special tube could not be placed without a leak, the author inserted 2 small endotracheal tubes via a tracheostomy, one for each lung. Positioning the tubes is difficult and must be controlled endoscopically. Special care must be taken for the tube not to obstruct the upper lobe of the right lung. As most such patients are critically ill, the prognosis of a major laceration of the posterior tracheal wall in a ventilated patient is generally poor.
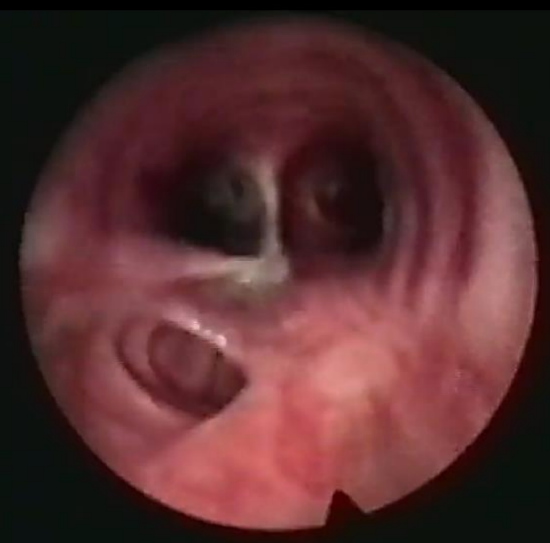
Figure 19: False tract extending posterior to the trachea just above the carina
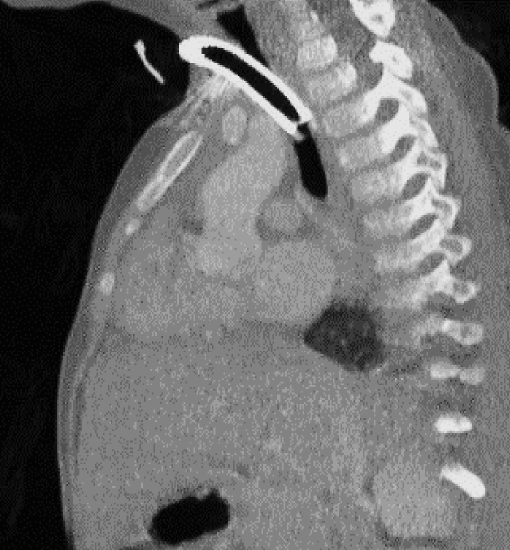
Figure 20: Note proximity of tracheostomy tube to innominate artery
False tract (Via falsa) (Figure 19): This occurs when a tracheostomy tube is inserted into a false tract ventral or lateral to the trachea. It may manifest as an inability to ventilate the patient or to pass a suction catheter through the tracheostomy into the lungs, high ventilation pressures, massive surgical emphysema, hypoxia and death. Endoscopy through the tube will verify that the tip of the tube is not in the tracheal lumen. The problem may be compounded by bleeding from lacerations of structures in the upper mediastinum e.g. veins, arteries or thyroid. The solution is that one should always check the position of the tracheostomy tube by one or more of the following means: use an endoscope during the percutaneous tracheostomy procedure to confirm correct placement of the puncture and tube; pass a suction tube into the lungs; ventilate the patient by hand and listen for breath sounds in both lungs; and order a chest X-ray to check the position if the tracheostomy tube and to exclude surgical emphysema, a pneumomediastinum and a pneumothorax. If the position of the tube remains in doubt, perform an open surgical approach, identify the trachea, and create a stable tracheostomy. If a false tract is found, attention must be directed especially to the space between the skin and the anterior tracheal wall as this access to the upper ventral mediastinum must be covered to protect the innominate artery or aberrant carotid to avert fatal bleeding (Figure 20).
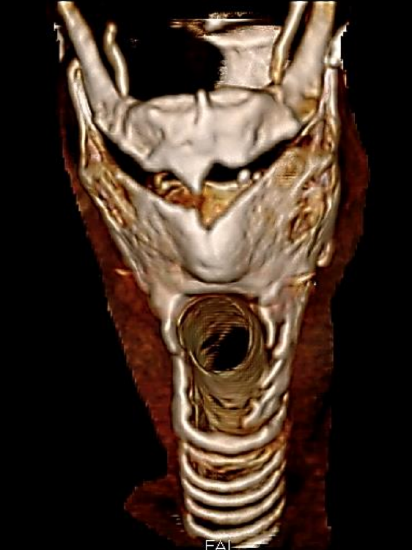
Figure 21: Sectio alta through cricoid
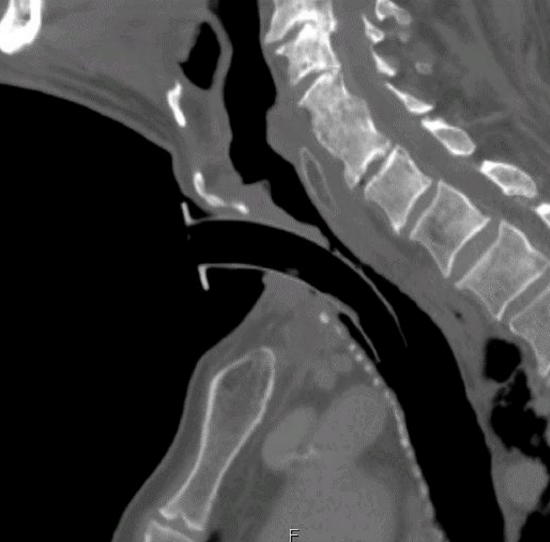
Figure 22: Sectio alta through cricothyroid membrane
High tracheostomy (Sectio alta): When a percutaneous tracheostomy is performed too high, it may violate the cricoid (Figure 21) or pass through the cricothyroid membrane (Figure 22), or in rare cases even enter the airway through the thyroid cartilage. This problem may be encountered in patients with massive laryngoptosis in whom the larynx sits in the suprasternal notch. Correct identification of the thyroid cartilage, cricothyroid membrane and cricoid can be difficult for inexperienced doctors and in patients with thick, short necks, or following prior surgery, or if the neck cannot be extended. For an inexperienced endoscopist, identification of the cricoid is difficult as well. A too-high tracheostomy may initially function well as the airway is secured. Significant problems arise after decannulation, as the airway manifests massive and irregular scarring with stenosis and/or functional problems relating to the vocal cords. Microbial inflammation of the cartilage may make it even worse. The solution is that should sectio alta be suspected, a clear diagnosis should be made by endoscopy and CT-scan or at least a lateral cervical X-ray. The situation must be addressed by creating a tracheostomy at the correct site. The “wrong” access must be closed and the airway reconstructed following the rules of reconstructive laryngeal surgery. In some cases internal stenting as is done after trauma may be necessary.
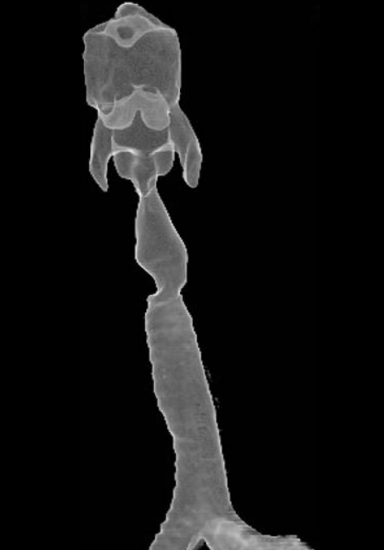
Figure 23: Tracheal stenosis on 3-D CT scan
Tracheal stenosis (Figure 23): This is a late complication of percutaneous tracheostomy. Once ventilation is no longer required the patient is decannulated and the tracheostomy site heals without complications. When the tracheal walls are partly destroyed by the procedure or by inflammation and chondritis, an unstable trachea results at the tracheostomy site (tracheomalacia) manifesting as stridor. This may not be clinically apparent immediately after decannulation, but may only manifest days, weeks or months later. Therefore if a patient develops inspiratory stridor and respiratory distress even weeks or months after closure of a tracheostomy (percutaneous or surgical), then an endoscopic evaluation with a flexible or rigid endoscope is required. Flexible endoscopy with spontaneous breathing is recommended, as one can better diagnose tracheomalacia in the extrathoracic trachea with spontaneous breathing. A major stenosis requires rigid endoscopy and bougienage or balloon dilatation of the stenotic segment. Further treatment of such a stenosis must follow the art of treatment of tracheal stenosis which may include retracheostomy, a Montgomery tube, tracheal resection and end-to-end anastomosis, and rib cartilage grafting etc.
Concluding remarks
Percutaneous tracheostomy is often promoted as being “fast, safe, and easy” to perform. It is being performed more-and-more successfully and safely, especially when doctors adhere to the correct indications and contraindications. However in clinical practice one is seeing tendencies to expand indications which may sometimes be to the detriment of a typically critically ill patient, who may then experience additional problems as a consequence of injudicious use of a percutaneous as opposed to a formal surgical tracheostomy.
As the use of percutaneous tracheostomy increases, fewer physicians and surgeons have the expertise to perform a good surgical tracheostomy. In the era of percutaneous tracheostomy, surgical tracheostomies are typically reserved for difficult cases such as very thick necks, bleeding disorders or significant laryngoptosis. This makes it hard to teach young surgeons how to perform a good surgical tracheostomy, as a surgical tracheostomy is not an easy procedure for beginners to perform alone at 4 pm! In difficult cases it can be hard to identify the trachea and make a tracheal opening that is wide enough to allow for safe cannulation, but narrow enough not to cause tracheomalacia and later stenosis, at the former tracheostomy site.
Each procedure remains as good as the indication used to perform it!
Related chapters
Closure of pediatric tracheocutaneous fistula – surgical technique
Reproduced with permission
Figures 1, 13, 14: http://www.aic.cuhk.edu.hk/web8/Trac...20diagrams.htm (Janet Fong)
Figures 5, 6, 8: http://resusreview.com/2015/perc-tra...step-tutorial/ (Charles Bruen)
Author
Prof. Dr. med. Thomas Deitmer
Director
ENT Department
Klinikum Dortmund
Germany
thomas.deitmer@klinikumdo.de
Editor, Co-author
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


