2.4: Hammer and Gouge Mastoidectomy for Cholesteatoma
- Page ID
- 15436
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
HAMMER & GOUGE MASTOIDECTOMY FOR CHOLESTEATOMA
Johan Fagan & Robert Jackler
This surgical guide is intended for the many surgeons in the Developing World who do not have access to modern mastoid surgery equipment such functioning mastoid drills, or are regularly faced with power cuts and therefore may be compel led to proceed with a mastoidectomy using a hammer and gouge, and possibly only a headlight and operating loupes.
The text and illustrations are based on the description of mastoid surgery: A Treatise on the Surgical Technique of Otorhinolaryngology (1939) by Georges Portmann. The text has been modified to incorporate modern principles of otology. This operative guide should be read in conjunction with the chapter Hammer and Gouge Radical Mastoidectomy for Acute Mastoiditis, also on the IFOS educational website.
Mastoid surgery can only be safely performed when the surgeon has an intimate knowledge of temporal bone anatomy. It is imperative that surgeons practice temporal bone dissections as described in the IFOS educational website.
Informed Consent
This should include anesthetic and surgical risks and issues relating to aggravated hearing loss, facial nerve injury, vertigo, taste disturbance, injury to the brain and meninges, and wound complications.
Anesthesia
Surgery may be performed under local or general anesthesia.
General anesthesia: Avoid muscle paralysis to facilitate detection of facial nerve irritation or injury.
Local anesthesia: See chapters
Magnification and lighting
Magnification is ideally required once dissection reaches the middle ear, and for removal of the facial ridge. Should an operating microscope not be available, then operating loupes with 2.5x magnification should be used. Good lighting is essential, especially when working in the middle ear. In the absence of an operating microscope or strong operating lights, a headlight may suffice.
Instrumentation (Figures 1a, b)

Figure 1a: Instruments for bone work
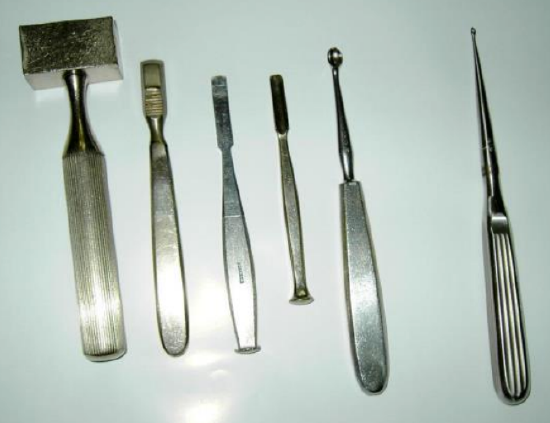
Figure 1b: Mallet, rasp, chisels, curette and gouge (From Professor Malick Diop)
Gouges and chisels should be kept extremely sharp, to ensure controlled bone resection. Blunt instrumentation requires undue force to be applied, and gouges/chisels may slip off bone and plunge and damage critical structures such as brain, lateral sinus, facial nerve, inner ear, and carotid artery. For the bone work the surgeon requires the following:
- Curved periosteal elevator
- Mallet
- Three gouges: Large, medium, small
- Flat chisel
- Curettes
- Rongeurs/bone nibblers (small, medium and large)
- Retractors (2), ideally self-retracting
- Canal elevator/McDonalds dissector
- Blunt probe
- Microinstruments: Curved needle, Plester knife, sickle knife, curette
- Suction tips
Position of Patient
The patient is laid supine with the head turned towards the normal ear.
Position of Surgeon and Assistants
The surgeon stands on the side of the affected ear. Two assistants are stationed on the other side, facing the surgeon. The 1st assistant is nearest to the head. The 2nd assistant is exactly opposite the surgeon.
Operative Field
The mastoid, auricle, and preauricular regions are extensively swabbed with tincture of iodine. The patient is covered to the neck with a sterile sheet. The operative field is isolated by four towels. Over them is placed a fenestrated sheet, the orifice of which encircles the auricle and mastoid.
Antibiotics
No antibiotics are required for mastoidectomy for uncomplicated cholesteatoma, other than when there is secondary infection (mastoiditis).
BIPP Paste
BIPP Paste can be prepared and used to impregnate ribbon gauze. This can be used to pack the mastoid cavity or ear canal, and because of its antiseptic properties, may be left in place for a few weeks. Bismuth subnitrate 20% w/w, iodoform 40% w/w, paraffin liquid 40% w/w (w/w = weight for weight).
Surgical anatomy for Mastoidectomy
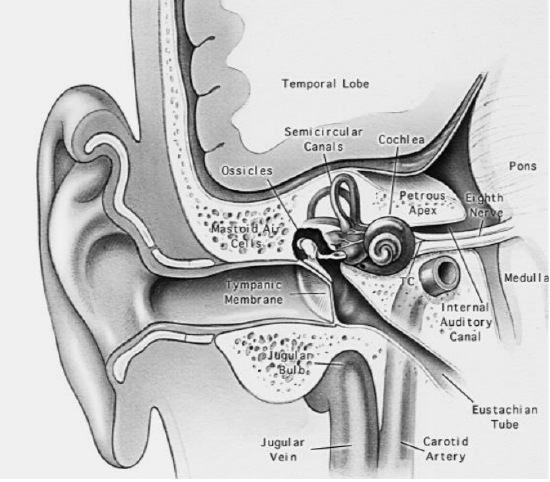
Figure 2: Coronal section through middle ear and temporal bone
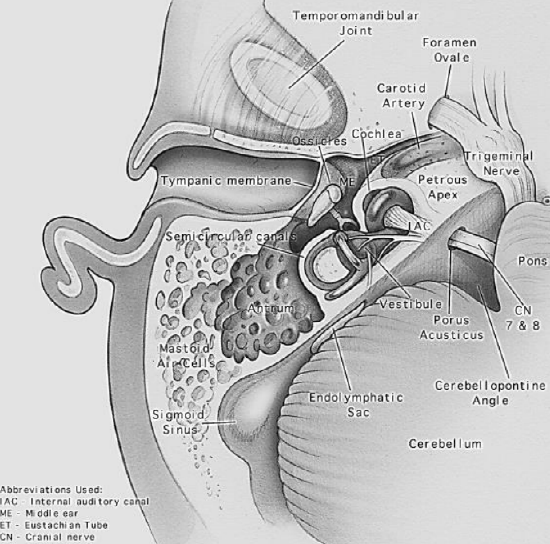
Figure 3: Axial view of temporal bone anatomy
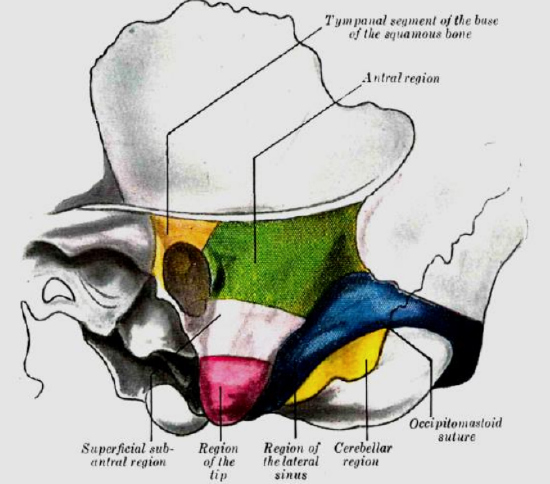
Brown: Tympanic segment of base of squamous bone; Green: Antral region; Rose: Subantral region; Red: Region of tip; Blue: Sinus region; Yellow: Cerebellar region or region of mastoid vein
Figure 4: Surface boundaries of mastoid regions
Surgical Steps: Radical Mastoidectomy
First Step: Incision of Superficial Tissues
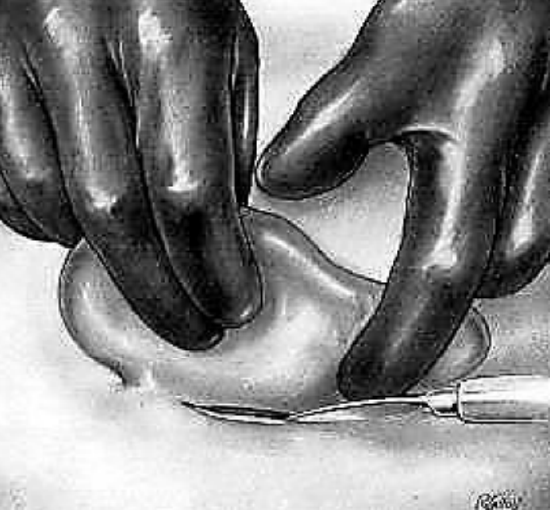
Figure 5: Incision of Superficial Tissues
The 1st assistant retracts the auricle towards himself, using both hands. The 3rd finger of the lower hand is pressed strongly under the mastoid tip in order to compress the posterior auricular artery. The other assistant is prepared to sponge/swab with mastoid sponges/swabs held in angular forceps. The surgeon incises the retroauricular crease down to bone from left to right, from the linea temporalis to the inferior part of the crease, or vice versa (Figure 5).
Second Step: Periosteal Elevation
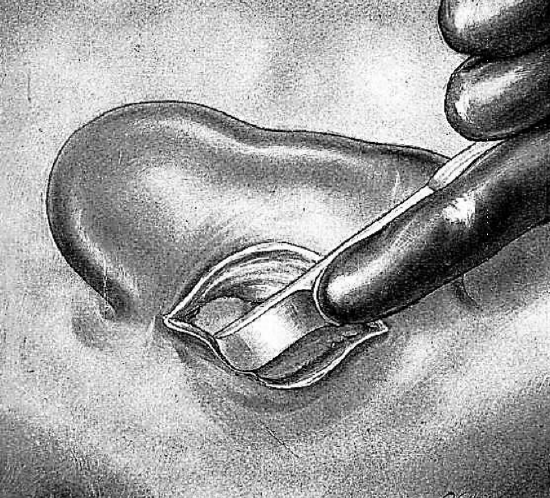
Figure 6: Periosteal elevation
After hemostasis and ligation of bleeding vessels, the periosteum of the antral region posteriorly is detached from the mastoid bone with the periosteal elevator; this is firmly retracted using a hooked retractor (Figure 6). Anteriorly a periosteal elevator separates the posterior wall of the canal from the spine of Henlé.
Third Step: Separation of Canal
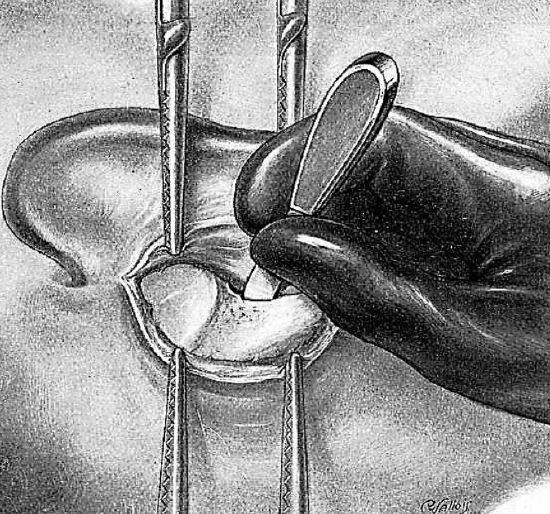
Figure 7: Separate canal skin from bone
A canal elevator is slipped against the posterior bony wall of the auditory canal and lowered forward in order to free the membranous canal (Figure 7). A pronged or self-retaining retractor grasps the membranous canal and auricle and retracts them forward. The elevator is then removed.
Fourth Step: Exploration of Operative Region
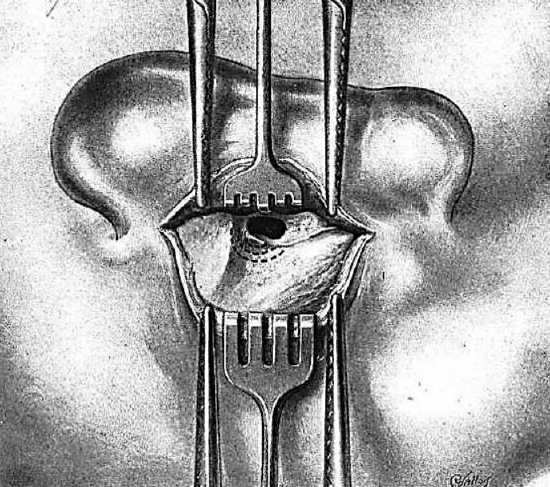
Figure 8: Transected ear canal and exposure of spine of Henlé and tympanic membrane
The skin of the posterior canal wall is transected parallel to the annulus of the tympanic membrane, thereby entering the ear canal, and exposing the tympanic membrane. The bony auditory canal is identified anteriorly and the tympanic cavity medially (Figure 8). Above, the finger identifies the crest of the linea temporalis. Above and behind the canal is the spine of Henlé; this is the guiding landmark to direct the following step.
Fifth Step: Search for Aditus and Antrum
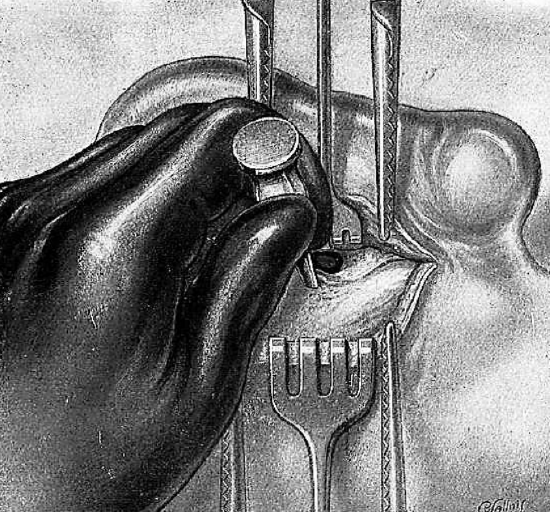
Figure 9: Gouge placed behind spine of Henlé
The search for the antrum begins by enlarging the auditory canal postero-superiorly. In Figure 8 the black dotted concentric lines indicate the course to be followed with the gouge during trephination; it is centered at the spine of Henlé. A large gouge is placed immediately behind the spine of Henlé, which is removed (Figure 9).
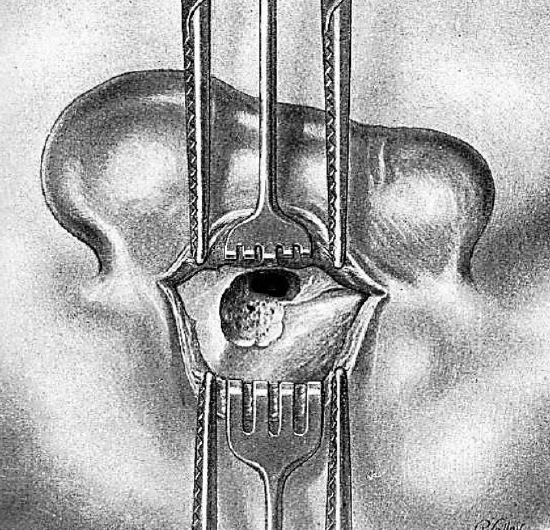
Figure 10: Excavation towards antrum
The instrument is held between the thumb and first two fingers of the left hand with the last two fingers resting on the bony surface, acting as a buffer to avoid plunging. The first tap of the gouge determines the direction of those following, which will be eccentric to it but always in the same direction. The canal is thus progressively enlarged by successive bites of the gouge, which should not extend above the linea temporalis (Figure 10). The excavation proceeds deeper until the gouge slips into a cavity: the antrum. The gouge is removed as soon as it penetrates to the cavity. The angular probe locates the aditus ad antrum, which confirms the presence of the antrum.
Sixth Step: Enlargement of Antrum

Figure 11: Entering the antrum
After ascertaining the presence of the antrum, the cavity is enlarged with the gouge along its superior, posterior, and inferior walls (Figure 11). The objective is to create a smooth, well rounded, regular cavity. The gouge is held between the thumb and first two fingers of the left hand with the last two fingers resting on the adjacent bony surface and acting as a buffer to avoid mishaps. The gouge is successively placed as follows: Superiorly it should not go beyond the linea temporalis, which approximately outlines the separation between the mastoid and middle cranial fossa dura, so as not to uncover the dura mater superiorly. Posteriorly it is handled very carefully and directed obliquely to avoid rupturing the lateral sinus, which may be prominent.
Seventh Step: Opening of Tympanomastoid Canal
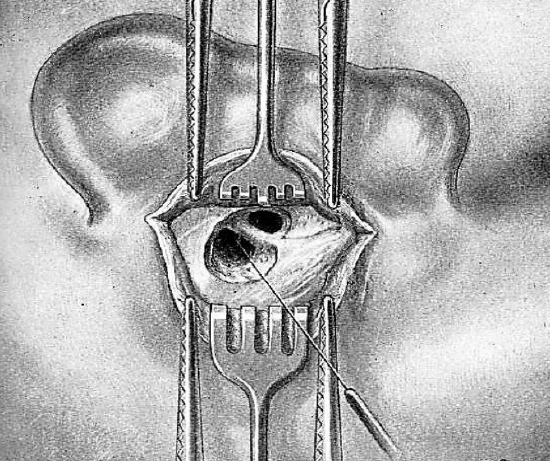
Figure 12: Probing the aditus to determine width of bony bridge
After extensively widening the antrum with a gouge, the surgeon reduces the thickness of the bony bridge, which forms the external wall of the aditus, and which separates the antrum from the tympanic cavity. Removal of this bridge is required to create a free communication via the tympanomastoid canal between the tympanic and mastoid cavities. The width of the bridge is determined by placing a curved probe in the aditus so that the tip is visible in the tympanic cavity (Figure 12).
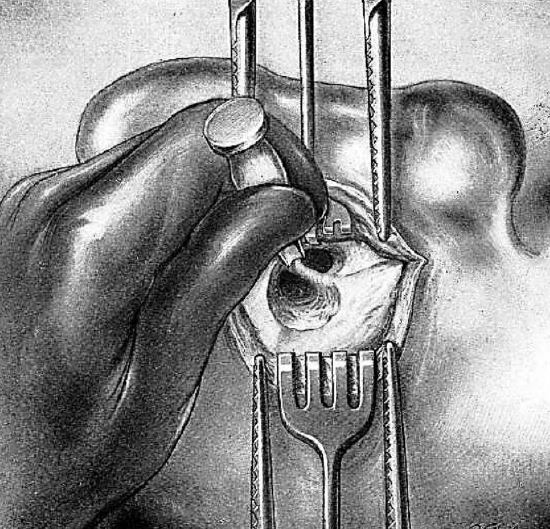
Figure 13: Removing bony bridge
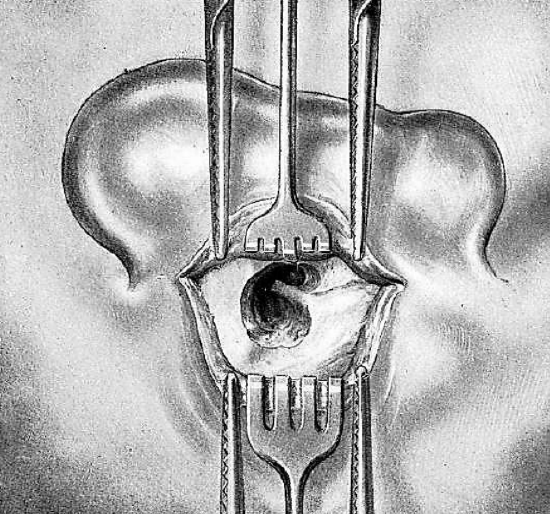
Figure 14: Removing bony bridge
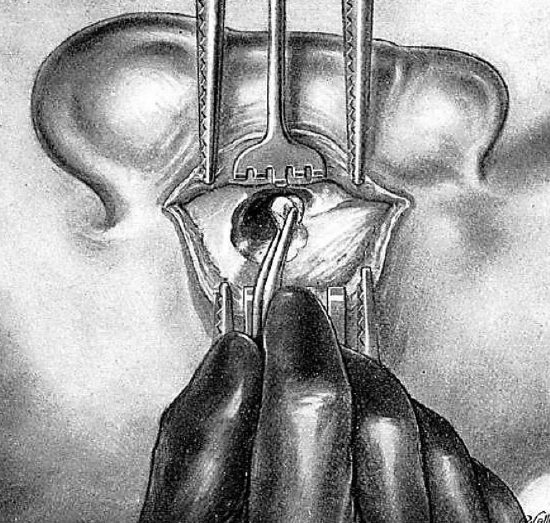
Figure 15: Removing bony bridge
When the bony bridge has been sufficiently reduced in size, its superior portion is removed with a gouge (Figures 13, 14 & 15).
The instrument is held perpendicularly between the thumb and first two fingers of the left hand, the other two fingers resting on the adjacent bone. The concavity of the gouge always faces inferiorly. At this point the operator should avoid injury to the facial nerve which is found much lower and also the lateral semicircular canal, which is internal to and below the line of section. Light taps of the gouge are applied horizontally at the superior end of the bony bridge where there is no danger of injuring the facial nerve, and should extend upwards and forwards over the wall of the attic. The tympanomastoid canal is reached by light taps of the hammer and is thus opened.
The wall of the middle ear is then completely smoothed with the gouge, which is always held in the same direction, in order to bring the roof of the antrum, the tympanic cavity, and the aditus to the same level. No bony ridges or irregularities are left.
Eighth Step: Removal of Facial Ridge
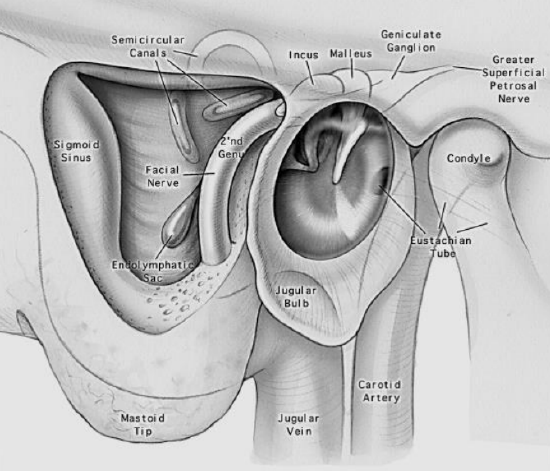
Figure 16: Anatomical relations of facial nerve
The middle ear and the antrum thus constitute a common bean-shaped cavity. They communicate widely superiorly but are separated inferiorly by the inferior margin of the aditus. A rounded elevation is present inferiorly in the antrum; this is the bony shell of the lateral semicircular canal. It serves as a useful marker for the location of the 2nd genu of the facial nerve, which is located anteroinferiorly to the lateral semicircular canal. The inferior aspect of the aditus is particularly thick and contains the 2nd genu of the facial nerve giving rise to the vertical limb of the Fallopian canal (Figure 16).
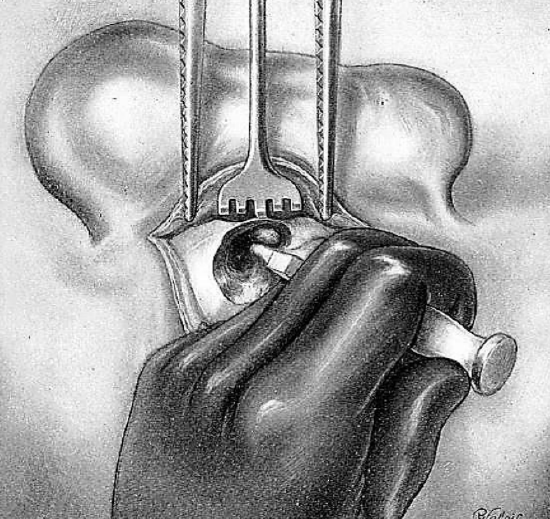
Figure 17: Removal of facial ridge
Removal and lowering of the facial ridge is a very delicate but necessary procedure for a good operative result. A small gauze pledget is placed in the tympanic cavity to catch the bony debris which otherwise would remain in the cavity. Removal of the facial ridge is accomplished with light taps of the mallet on the chisel. They are directed obliquely upwards from the base (inferiorly) to the summit (superiorly), the top of which overhangs the aditus (Figure 17).
Since the inferior portion is very thick, there is not much danger of injury to the facial nerve. However, the summit is adjacent to the 2nd genu. The operator proceeds very cautiously, chipping off smaller and smaller pieces of bone as the aditus is approached.
The anesthetist is advised not to paralyze the patient, and is asked to focus his attention on the patient’s face to observe muscular contractions in the area of distribution of the facial nerve, and to immediately advise the surgeon of any contractions which are indicative of trauma in the vicinity of the nerve. The surgeon stops at the slightest warning from the anesthetist. Generally the procedure is straightforward. Sometimes, however, the bone may bleed. This indicates proximity to the stylomastoid artery, which is external/superficial to the facial nerve. This is an important sign of proximity to the nerve.
All irregularities are removed, leaving a bony cavity with rounded contours and a smooth surface. The summit is continuous with the floor of the aditus. A rounded elevation appears on the internal slope of the facial ridge towards the antrum; this is the bony shell of the lateral semicircular canal.
Ninth step: Curettage of Tympanic Cavity
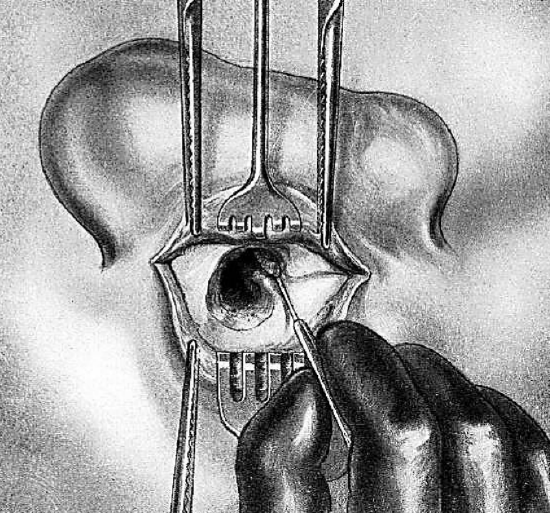
Figure 18: Curettage of middle ear, and removal of incus and malleus
The small pledget in the tympanic cavity is removed. The tympanic cavity is often filled with cholesteatomatous shreds and inflammatory granulations. All that remains to be done is curettage of this cavity. During this operative step, the anesthetist continues to watch the patient’s face and to warn the surgeon of any injury to the facial nerve. A small, middle ear curette is used. First to be removed are the malleus and incus, whose necrotic fragments are identified. The stapes is left undisturbed (Figure 18).
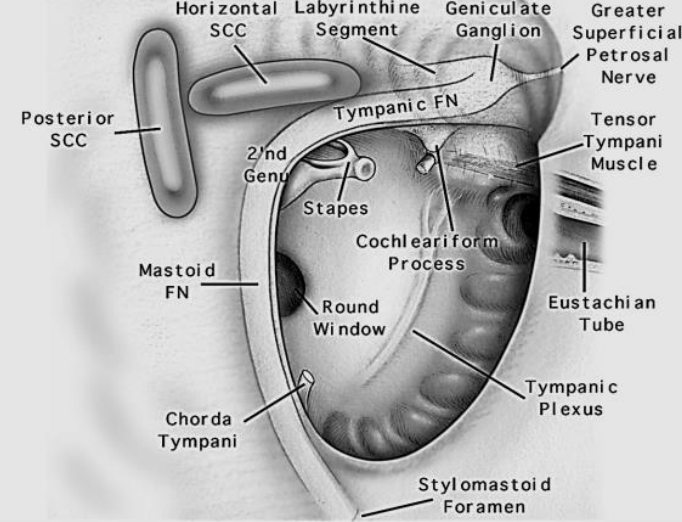
Figure 19: Anatomy following radical mastoidectomy and removal of malleus and incus
The walls are curetted systematically. The danger of dehiscence of the bone or of accidentally breaking through the bone with the curette should be constantly kept in mind. Curettage should therefore be very carefully performed. The superior wall (tegmen tympani) is very thin and is adjacent to the temporal meninges. The floor is slightly resistant and immediately above the jugular bulb. The medial wall contains the oval window with the stapes superstructure and round window, and the facial nerve which is often dehiscent and exposed by osteitis (Figure 19).
It is necessary to see clearly, sponge or suction often, use small pledgets of adrenaline, and utilize magnification e.g. magnifying loupes, an endoscope or a microscope. The operation is terminated with curettage of the anterior wall. This wall contains the orifice of the Eustachian tube, the medial edge of which is adjacent to the carotid canal. The cutting edge of the curette should therefore be turned outwards as the lateral wall offers no dangers.
Tenth Step: Cleaning and Exploring Operative Cavity
The entire cavity is sponged/suctioned and irrigated with saline. Bony debris is meticulously removed; the slightest unevenness is smoothed with the gouge or curette. The blunt probe is used to determine that neither the dura mater nor the lateral sinus has been exposed in the tympanic cavity or antrum/mastoid. Carefully examine, with magnification, the lateral semicircular canal to rule out a labyrinthine fistula. This appears as a greyish dot where the probe reveals a loss of bony substance.
Eleventh Step: Meatoplasty
The next procedure is to adapt the auditory canal and auricle to the new cavity. A piece of gauze is placed in the tympanic cavity and antrum. The assistant retracts the pinna forward and introduces a gouge into the membranous canal with its concavity directed against the concha. The pinna and gouge are then angled forward towards the cheek. The surgeon incises the posterior wall of the membranous canal over the gouge from front to back. The gouge protects the underlying tissues as it guides the scalpel. The gouge is removed and the pinna, held by the assistant with both hands, is returned to its normal position.
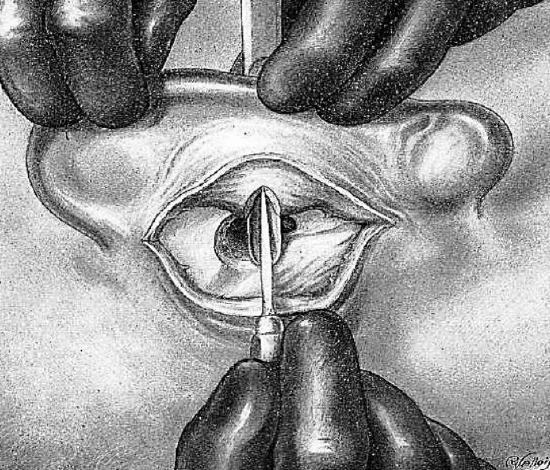
Figure 20: Initial meatoplasty incision
The scalpel is introduced into the canal from below, passing up through the operative gap. The blade is turned toward the auricle and follows the transverse incision backwards to the centre of the concha (Figure 20).
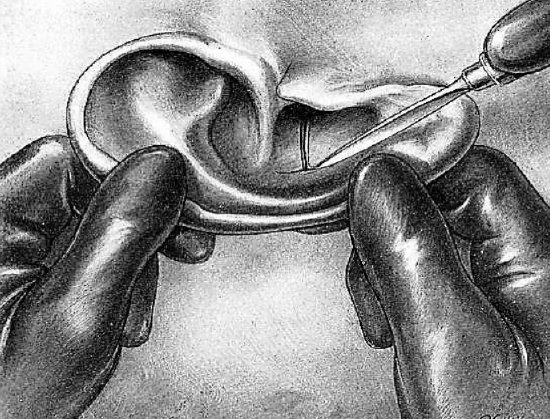
Figure 21: “T” incision in concha
The scalpel is removed and a “T” incision is made in the concha at right angles to the original incision (Figure 21). In this manner two triangular flaps are obtained, one superiorly and one inferiorly.
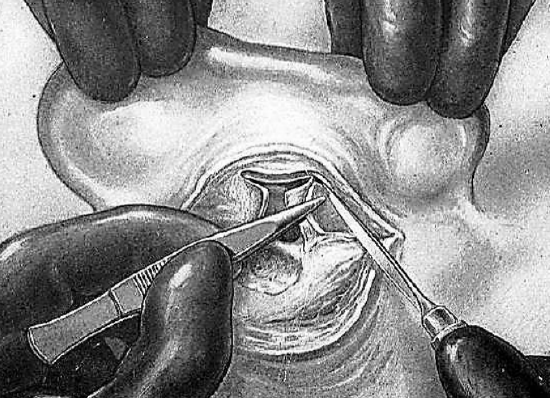
Figure 22: Thinning of flaps
The flaps are very thick and consist of the skin of the concha and canal as well as the lining cartilage and adipose tissue. Only the skin should be preserved in order to obtain a pliable flap that will conform to the cavity. The pinna is again drawn forward and the tips of the flaps are successively grasped with tissue forceps. Using the scalpel, the cartilage is then separated and excised from its adherent tissues. This excision causes minor hemorrhage and necessitates cautery or a few ligatures. The two flaps are then ready to be stitched into place. The surgeon now turns his attention to the posterior edge of the concha and here, too, excises the cartilage. The skin is grasped with tissue forceps and the scalpel separates the cartilage, of which 2 or 3 mm is resected (Figure 22).
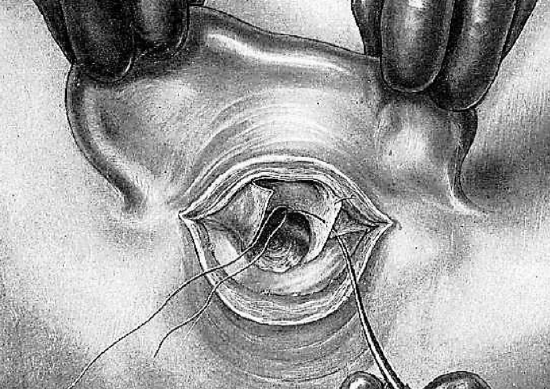
Figure 23: Suturing inferior flap
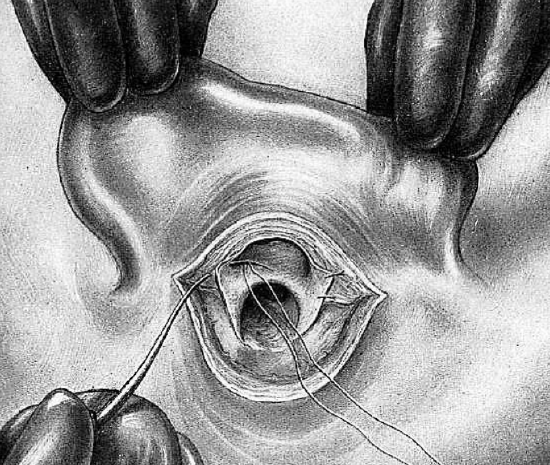
Figure 24: Suturing superior flap
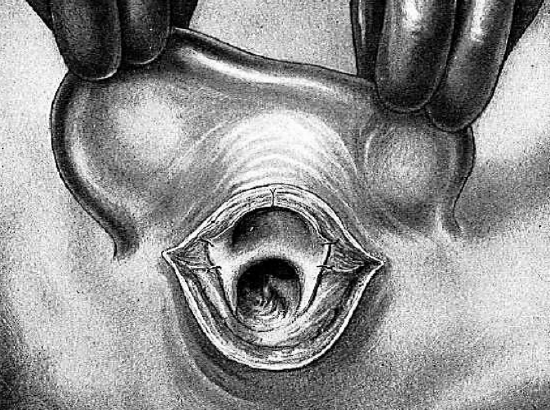
Figure 25: Suturing posterior lip
The concha, thus prepared for the meatoplasty, consists of two flaps and the posterior edge of the vertical incision. These two thin cutaneous flaps are the primary source of epithelialization of the bony cavity. They are everted and successively stitched to the adjacent tissues of the pinna so that they are well placed in relation to the contours of the antrum. The inferior flap, held with the tissue forceps, is transfixed. It is lightly turned back and the needle grasps the cellular tissue of the pinna beneath the flap. The flap is stitched with catgut/vicryl so that its everted free edge lies on the inferior part of the antrum (Figure 23). The same maneuver is executed with the superior flap which corresponds to the edge of the superior antral wall (Figure 24). The posterior lip of the conduit is then everted by two or three stitches (Figure 25). The meatoplasty is completed. The pinna remains mobile since at no point is it fastened to the mastoid.
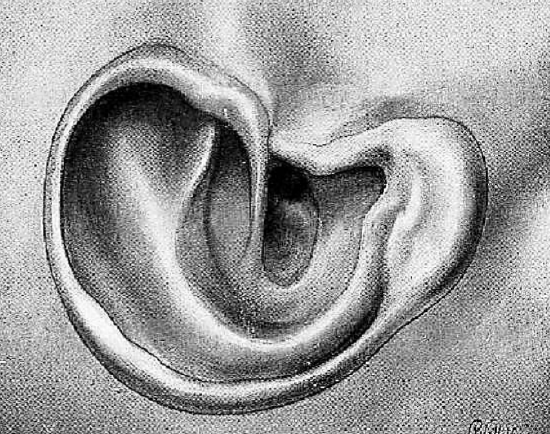
Figure 26: Final meatoplasty
After removing the temporary packing in the operative cavity, the pinna is returned to its original position. The surgeon should carefully inspect the meatoplasty to ascertain that there is no retraction of the skin of the pinna and that the orifice in the concha gives adequate access to the antrum and tympanic cavity for subsequent inspection and cleansing (Figure 26).
Twelfth Step: Packing of Cavity
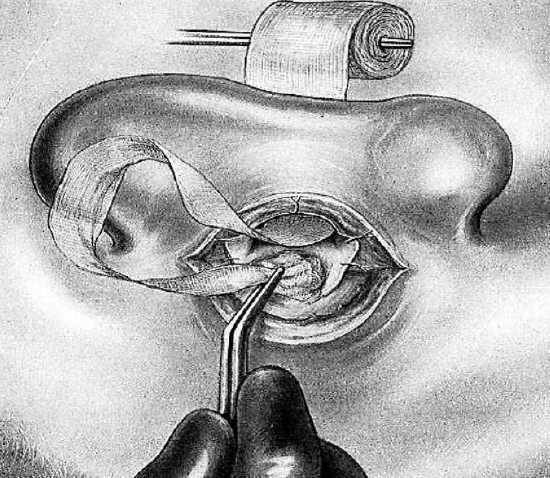
Figure 27: Ribbon gauze has been pulled through the meatoplasty to pack the mastoid cavity
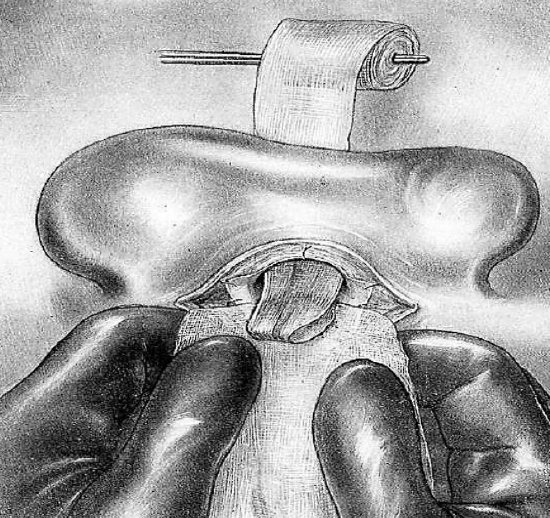
Figure 28: Interposed gauze prevents pressure on dressings of bony cavities during packing of meatus
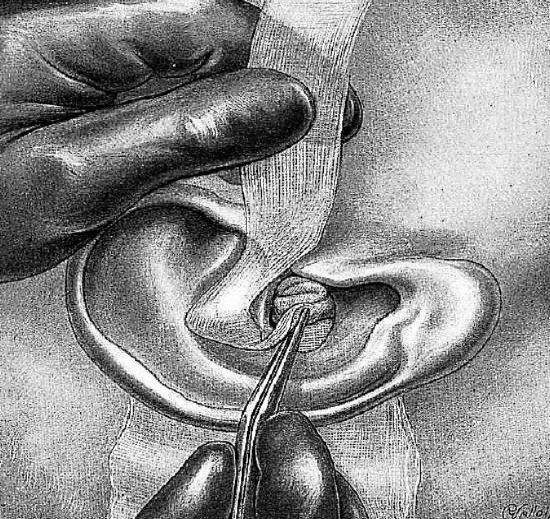
Figure 29: Packing the meatus
The operative cavity is packed with BIPP impregnated ribbon gauze mounted on a hemostat. The assistant retracts the pinna slightly forward. The end of the gauze passes through the orifice of the concha and exits into the retroauricular wound. The surgeon then pulls several centimeters of ribbon gauze towards himself; with it he packs the bony cavity (Figure 27).
Packing is done in the following manner (Figures 27-29): The end of the ribbon gauze is held in a forceps and is folded upon itself. It is inserted first in the tympanic cavity, which is filled without being tightly packed. The ribbon is next placed in the aditus and then the antrum. After packing the cavities, the surgeon packs the concha with the remainder of the ribbon. A gauze sponge/swab is placed in the retroauricular groove, isolating the pinna from the antrum and tympanic cavity. The concha is filled with the ribbon gauze which is tightly packed here since its object is to serve as support for the meatoplasty flaps. The interposed gauze sponge/swab prevents the latter packing from creating pressure on the dressings of the bony cavities.
Thirteenth Step: Retroauricular Suture and Dressing
The skin is carefully approximated and closed with three or four sutures.

Figure 30: Sutured wound
A small ball of absorbent cotton is placed at the entrance of the concha against the ribbon gauze so the latter will not adhere to the gauze dressing. A gauze sponge/swab is placed in the retroauricular groove; two or three other gauze sponges/swabs are placed on the pinna. The entire area is covered with sterile absorbent cotton which is held in place by a bandage wrapped around the head.
Postoperative Care
The surgeon assesses the facial nerve function. Patients are generally discharged the day following surgery. The mastoid dressings are removed 1-2 weeks following surgery. The mastoid cavity generally requires regular toilette lifelong at variable intervals.
Special Problems
Difficulty Finding Antrum
Locating the antrum is one of the main difficulties during the course of radical mastoidectomy. The bone is frequently sclerotic and the antrum small. The technique described always leads to the aditus, which the operator should be particularly anxious to locate. Should he/ she fail to find the antrum, a blunt probe, carefully directed and inserted into the tympanic cavity is used to locate the course of the tympanomastoid canal, and the location of the aditus ad antrum.
Exposure of Lateral Sinus or Temporal Meninges
The lateral sinus is sometimes inadvertently uncovered with the first taps of the gouge. The temporal meninges are covered by the thin bony tegmen tympani and may be exposed by osteitis of the roof of the tympanic cavity or by curettage. It is prudent to use a blunt probe quite often to explore the superior wall of the tympanic cavity, the aditus, or the antrum before curetting or when trauma with an instrument is feared. Extreme caution is always required. However exposure of the above structures does not generally present any serious danger. No special measures are required. In the postoperative course a close watch is kept for the possible appearance of intracranial complications.
Automastoidectomy
A cholesteatoma which has been present for a period of years may erode the bone to such an extent that it result in an autoradical mastoidectomy. The aditus may be deeply excavated and the antrum vast. Oftentimes the medial cortex is also destroyed. The task of the surgeon in such cases is much simpler and the bony surface is white and smooth. The only necessary procedure required is to complete the opening of the aditus and remove the facial ridge.
Labyrinthine Fistula
An unsuspected labyrinthine fistula, generally of the lateral semicircular canal, may be discovered during the course of the operation by careful inspection with magnification, probing, or the presence of a nystagmus noticed by the anesthetist; or by vertigo in the awake patient. The fistula should not be disturbed but simply covered with a patch of temporalis fascia.
Facial Nerve
The facial nerve may be affected preoperatively to various degrees. Some spontaneous contractions of the muscles of the face may have been noticed. Paresis or paralysis may be present. Whenever the facial nerve has been affected all maneuvers in the tympanic cavity and aditus should be done very cautiously. Facial nerve paralysis also raises the possibility of tuberculous mastoiditis. Tuberculous mastoiditis requires a lesser operation than for acute mastoiditis, the object being only to remove bony sequestra, and to obtain tissue for histological and bacteriologic diagnosis.
Complete paralysis as an unfortunate result of the operative procedure, is uncommon. Await resolution of local anesthetic, as it might be responsible for the paralysis. The mastoid packing should be loosened as it may be pressing on a dehiscent nerve. If there is a suspicion of the nerve having been transected or compressed by a spicule of bone, the ear should be urgently explored and the nerve decompressed, repaired, or grafted with a segment of greater auricular nerve.
Intracranial Complications
Meningitis and, less frequently, thrombophlebitis of the lateral/sigmoid sinus are serious complications during the first few postoperative days in patients with mastoiditis.
Labyrinthine Complications
During the immediate postoperative period of a radical mastoidectomy, the patient may experience dizziness and have nystagmus. These may be perilabyrinthine phenomena produced by mild irritation in the neighborhood of an unrevealed fistula, or may be due to a labyrinthine fistula, or dislocation of the stapes.
Author & Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za
Author
Robert Jackler MD
Sewall Professor and Chair
Department of Otolaryngology-Head & Neck Surgery
Associate Dean, Postgraduate Medical Education
Stanford University School of Medicine
Stanford, CA 94305-5101, USA


