3.4: Pediatric Bronchoscopy for Foreign Bodies
- Page ID
- 15443
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
PEDIATRIC BRONCHOSCOPY FOR FOREIGN BODIES
Nico Jonas
This chapter only addresses the management of foreign bodies in the airway from the laryngeal inlet down to and including the bronchi.
Anatomical considerations
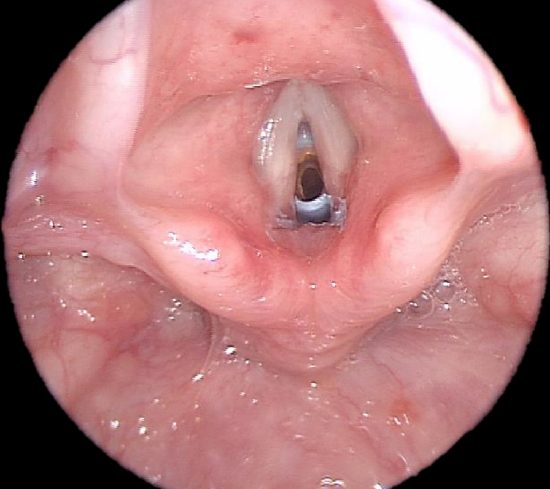
Figure 1: Subglottic non-organic foreign body
Due to the cone shape of the pediatric cricoid cartilage, the subglottis is the narrowest part of the trachea in the pediatric patient (Figure 1). If an aspirated foreign body is small enough to pass beyond the subglottic area then the most likely site of impaction is in the main bronchi. The right main bronchus is more vertically aligned and therefore the most common location of a distally lodged foreign body.
Classification
Foreign bodies are generally classified as organic vs. non-organic.
Decision to perform bronchoscopy
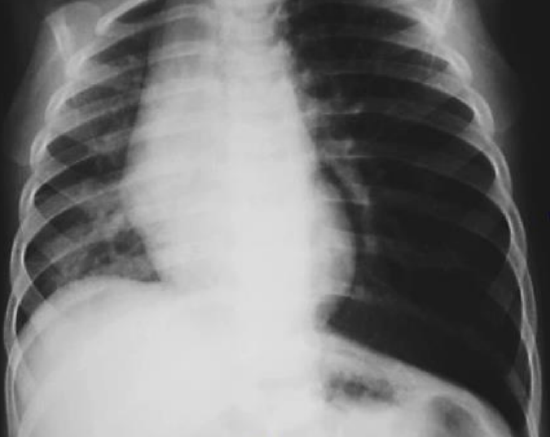
Figure 2: Collapse of right lung secondary to radiolucent foreign body in right main bronchus
The decision whether a bronchoscopy is required is based on the history, clinical examination and chest x-ray findings. If there is strong suspicion of a foreign body based on history, clinical findings and/or x-ray, then bronchoscopy should be performed. It is acceptable to have negative bronchoscopy findings, but unacceptable to miss a foreign body because bronchoscopy was omitted. X-ray findings can be conclusive in cases of radio-opaque foreign bodies, or subtle when dealing with radiolucent ones. In the latter case findings may include hyperinflation during air trapping, segmental consolidation or collapse (Figure 2).
Timing of procedure
Distressed patients or patients with suspected caustic foreign bodies (batteries) should have the foreign body removed as soon as possible. Asymptomatic patients or patients with longstanding symptoms should have bronchoscopy and removal of the foreign body done on the next available elective list to ensure an optimal operating room environment.
“Sharing the airway”
Foreign body retrieval from the airways can be extremely challenging both for surgeon and anesthetist. An understanding about sharing the airway with the anesthetist is paramount during the procedure, making good communication with anesthetic staff absolutely essential.
The surgeon should discuss how the patient will be induced and anesthetized and how the airway will be maintained during the procedure. It is also important to discuss how the airway will be maintained prior to inserting the ventilating bronchoscope. Options include ventilation by means of a nasopharyngeal airway, laryngeal mask, facemask, or by means of temporary endotracheal intubation. Prior to commencing the procedure, discuss with the anesthetist what you would do should the patient desaturate i.e. place a ventilating bronchoscope down to the level of the carina and ventilate the patient via the bronchoscope.
Preoperative procedure
| Age | Bronchoscope Size |
| 1-6 months | 3.0 |
| 6-18 months | 3.5 |
| 18 months-3 yrs | 4.0 |
| 3-6 yrs | 4.5 |
| 6-9 yrs | 5.0 |
| 9-14 yrs | 6.0 |
Table 1: Age-appropriate bronchoscope sizes
Age-appropriate ventilating bronchoscopes should be ready; one size smaller should be on standby (Table 1).

Figure 3: Equipment required for airway foreign body removal: 1. Side-arm forceps 2. Optical forceps & accompanying endoscope 3. Rigid ventilating bronchoscope & accompanying endoscope 4. Flexible sucker & adrenaline 5. Proximal bronchoscope fittings
It is essential that the surgeon be familiar with all the bronchoscopy equipment, especially how to assemble and disassemble the ventilating bronchoscopes (Figure 3). Equipment should be set out and ready to use (white balancing done, lenses cleaned with anti-fog and tested) prior to putting the patient to sleep.
Instructional Video: How to assemble a Pediatric Bronchoscope
Anesthetic
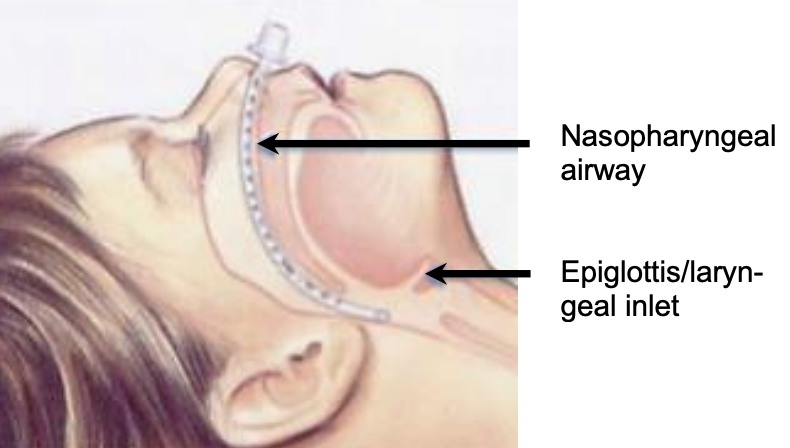
Figure 4: Position of nasopharyngeal tube for ventilation
The most commonly employed anesthetic technique is gas induction with the patient breathing spontaneously and maintaining his/her own airway. The anesthetist will thereby gain some information about how stable the airway is, how much support is required and what oxygen saturation the patient is maintaining. As soon as the patient is asleep, topical local anesthetic is sprayed onto the vocal cords. The airway can then be maintained using a facemask, nasopharyngeal airway (Figure 4), laryngeal mask or endotracheal tube ventilation until the ventilating bronchoscopes is inserted.
Positioning the patient
A shoulder roll is used to hyperextend the neck and a head ring is employed to stabilize the head. Care should be taken in patients with known or suspected atlantooccipital instability.
Equipment
An age-appropriate ventilating bronchoscope is used (Table 1). Note that a size 3.5 ventilating scope is the smallest bronchoscope that will allow the use of a flexible suction catheter as well as permit sufficient ventilation.
Procedure
A gum/tooth guard is inserted. The bronchoscope is then inserted. The anesthetist’s laryngoscope can be used to facilitate passage of the bronchoscope through the vocal cords. Withdrawing the endoscope within the bronchoscope allows visualization of the entire circumference of the tip of the bronchoscope and allows easy placement of the bronchoscope into the larynx. As soon as the bronchoscope is passed through the vocal cords the anesthetist can ventilate the patient through the bronchoscope.

Figure 5: Flexible suction catheter inserted via side-arm of bronchoscope. Inset shows endoscope and suction catheter side-by-side at distal end of bronchoscope
The trachea and bronchi should be thoroughly examined. If a foreign body is identified, then careful suctioning should be done around it using a flexible suction catheter that is passed through the side port of the bronchoscope (Figure 5).
When there is consolidation, air trapping or collapse on preoperative X-ray due to a foreign body preventing free movement of air, then topical adrenaline can be very beneficial. Applying adrenaline onto the foreign body via the flexible suction causes vasoconstriction and decongestion of the surrounding mucosa. This may improve ventilation of the affected lung; it also reduces bleeding from inflamed mucosa and granulation tissue that surrounds the foreign body. Improved ventilation is evidenced by air bubbles forming around the foreign body due to air escaping from the affected airways and lung distal to the entrapped foreign body.
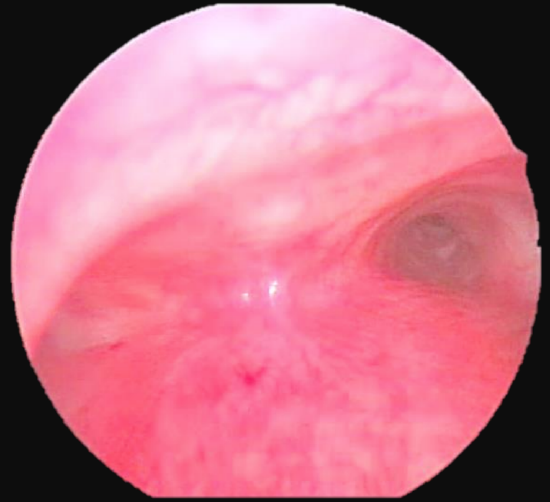
Figure 6: Placement of bronchoscope in distal trachea just above carina to facilitate optimum ventilation of both lungs
In order to ensure maximum oxygenation and delivery of anesthetic gases to the patient, always place the bronchoscope just above the carina and disconnect the suction if you are not actively doing anything (Figure 6).

Figure 7: Optical foreign body removal forceps: “crocodile forceps” (above) and “peanut forceps” (below)
Once you have a good view of the foreign body a decision is made about the most suitable forceps to use (Figure 7).
The optical foreign body removal forceps are introduced into the bronchoscope and advanced towards the foreign body. After grabbing hold of the foreign body, it should either be pulled inside the bronchoscope and removed through the bronchoscope, or in cases of large foreign bodies, pulled up to the end of the bronchoscope and retracted and removed with the bronchoscope. In the latter case the anesthetist should revert back to ventilating the patient via nasopharyngeal tube or facemask while the surgeon prepares to reintroduce the bronchoscope. The airway is re-examined to ensure that there are no residual foreign bodies, and bronchial lavage is done if required.

Figure 8: Flexible “sidearm forceps” can be inserted via the side port and is small enough to sit alongside the endoscope inside the bronchoscope
If a foreign body is situated distally in the main bronchus and out of the reach of the optical forceps, a side-arm forceps can be used as it can be advanced to reach a foreign body further down the airway than the optical forceps will reach (Figure 8).
Postoperative management
The patient should be observed in hospital for 24 hours and receive chest physiotherapy and antibiotics if indicated. Patients should be rescoped if there was evidence of circumferential granulations due to concerns about airway stenosis developing in future.
Important tips
- Use 90% of your time to prepare (with topical adrenaline and suctioning) and 10% of your time to remove the foreign body
- Apply adrenaline to decongest and optimize the visual field
- Use at least a size 3.5 bronchoscope to enable good ventilation and use of a flexible suction catheter
- If not actively doing something, disconnect the suction and place the bronchoscope in the distal trachea just above the carina to enable optimum ventilation
- Examine the postnasal space at the end of the procedure to exclude a foreign body in that location
Instructional Video: How to assemble a Pediatric Bronchoscope
Author and Pediatrics Editor
Nico Jonas MBChB, FCORL, MMed
Pediatric Otolaryngologist
Addenbrooke’s Hospital
Cambridge, United Kingdom
nico.jonas@gmail.com
Editor
Johan Fagan MBChB, FCS(ORL ), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


