3.5: Pediatric Tracheostomy
- Page ID
- 15444
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
PEDIATRIC TRACHEOSTOMY
Hasnaa Ismail-Koch and Nico Jonas
The open tracheostomy technique in the pediatric patient differs from that undertaken in the adult. In the pediatric patient a formal stoma is created by suturing the tracheal wall to the skin with maturation sutures in addition to safety stay sutures placed in the tracheal wall.
Terminology
Tracheotomy refers to making an opening into the trachea whilst tracheostomy refers to creating a formal stoma and a communication between the trachea and the overlying skin.
Indications
- Upper airway obstruction due to congenital or acquired causes
- Patients requiring long-term ventilation
- Failure to wean from conventional orotracheal or nasotracheal ventilation (eliminates dead space)
- Pulmonary toilet
Preoperative evaluation
Careful evaluation of each patient must be undertaken as to whether any other intervention might avoid a tracheostomy.
Examination of nasopharynx, oropharynx and microlaryngoscopy and bronchoscopy
Patients with airway obstruction should undergo examination of the upper airways as well as microlaryngoscopy and bronchoscopy to exclude treatable causes of obstruction, thus eliminating the need for tracheostomy. It also permits accurate documentation of airway pathology for future comparison.
Anatomy of the neck
The cricoid and thyroid cartilages are difficult to palpate in the neonate and younger child because the neck is short, the laryngeal structures are more pliable and subcutaneous fat is more prominent. Hyperextending the neck may cause mediastinal structures to present in the neck. Check whether patients have undergone previous surgical procedures e.g. sternotomies resulting in scarring and altered anatomy.
Chest X-ray
Chest X-ray following assessment of the respiratory system is important to detect pulmonary disease that might be improved prior to surgery. It is also useful measure to establish the position of the trachea and to confirm that it is situated in the midline.
Blood tests and coagulopathy
Pediatric patients undergoing tracheostomy will in general have other comorbidities; therefore, blood tests are almost always required. Full blood count and electrolytes may be required for anesthetic purposes. Cross matching blood might be required in patients with anemia, especially in neonates where a small amount of blood loss can be clinically significant. Coagulopathies must be corrected prior to surgery.
Cardiorespiratory status
The cardiorespiratory status should be optimized preoperatively. A cardiology review must be obtained if there is any suspicion of underlying cardiac pathology. Relieving prolonged upper airway obstruction with a tracheostomy may result in respiratory distress due to loss of hypoxic drive because of sudden change in CO2 levels, or pulmonary edema.
Tracheostomy technique
Microlaryngoscopy and bronchoscopy should be undertaken prior to tracheostomy if the airway has not been previously assessed. If possible, this is done with the child breathing spontaneously. The surgeon or anesthetist can subsequently intubate the child and the surgeon may then proceed with the tracheostomy.
Minimum Kit
A pediatric tracheostomy kit should include: size 11 & 15 scalpels, bipolar diathermy, fine dissecting scissors, fine artery clips x3, toothed forceps, skin retractors, suction, needle holder and suture cutting scissors, a local anesthetic agent, size 4/0 non-absorbable suture (e.g. prolene), and size 4/0 absorbable suture (e.g. vicryl).
| Age | Tube size |
| 0-1 month | 3.0 |
| 1-6 months | 3.5 |
| 6-18 months | 4.0 |
| 18 months - 3 yrs | 4.5 |
| 3-6 yrs | 5.0 |
| 6-9 yrs | 5.5 |
| 9-12 yrs | 6.0 |
| 12-14 yrs | 6.5 |
Table 1: Age-appropriate tracheostomy tube sizes. Tube sizes vary with different companies having different outer diameters. The figures stated refer to Shiley tubes
The tracheostomy tube should be checked prior to the procedure; if a cuffed tracheostomy tube is required, the cuff should be checked for leaks. Select an appropriately sized tracheostomy tube and a one-size smaller tracheostomy tube (Table 1). Regarding tracheostomy tube length, a 1 year old child requires a longer ‘paed’ tube.
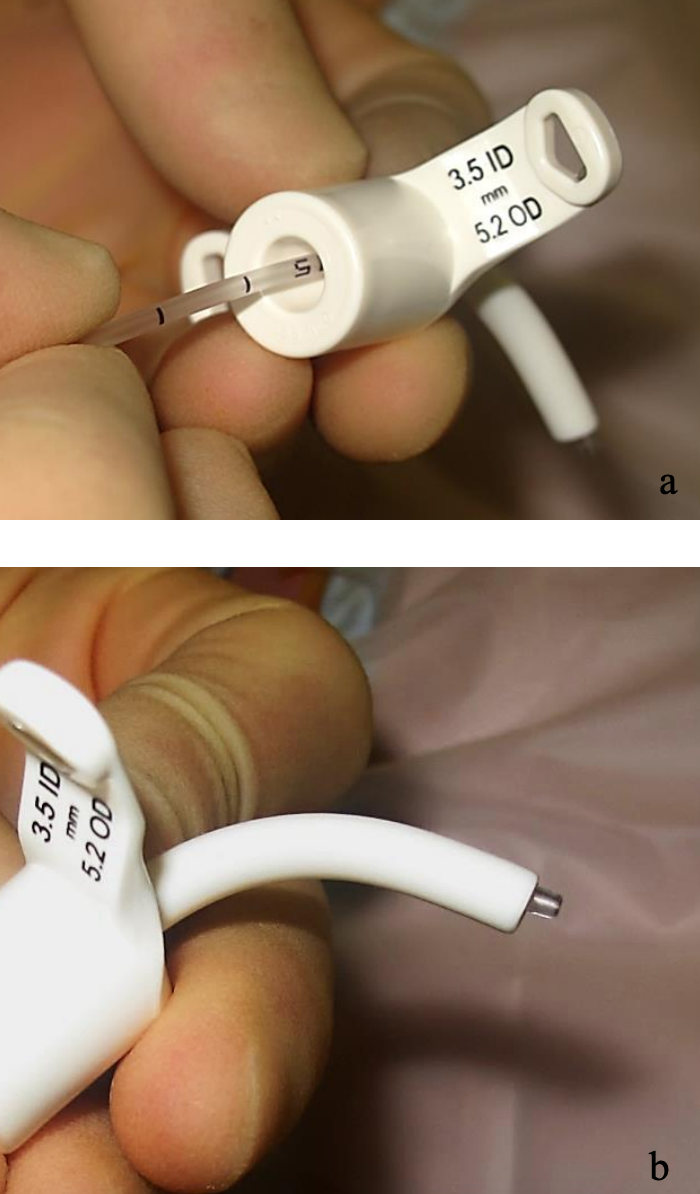
Figures 1 a, b: Measuring the correct suction tubing length which should not extend >5 mm past the tip of the tracheostomy tube
Select an appropriately sized tracheal suction catheter; usually double that of the tracheostomy tube size e.g. a size 8 catheter for size 4 tracheostomy tube. The length that the tube should be suctioned to should also be measured and recorded; this length is measured using an appropriately sized tracheal suction catheter and is generally accepted to be 0.5cm longer than to the tip of the tracheostomy tube (Figures 1a,b).
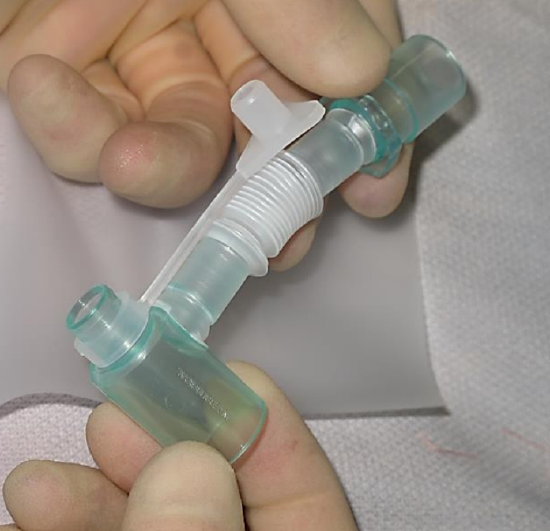
Figure 2: Connector between tracheostomy tube and anesthetic tubing
Check that the correct anesthetic connectors and tubing between the tracheostomy tube and anesthetic circuit are present (Figure 2).
Anesthesia
A child should ideally be intubated. Rarely when it is not possible to intubate the child, the most suitable way of maintaining the airway and oxygenation should be determined; it may vary from facemask ventilation to intubating the child using a ventilating bronchoscope.
Positioning and draping
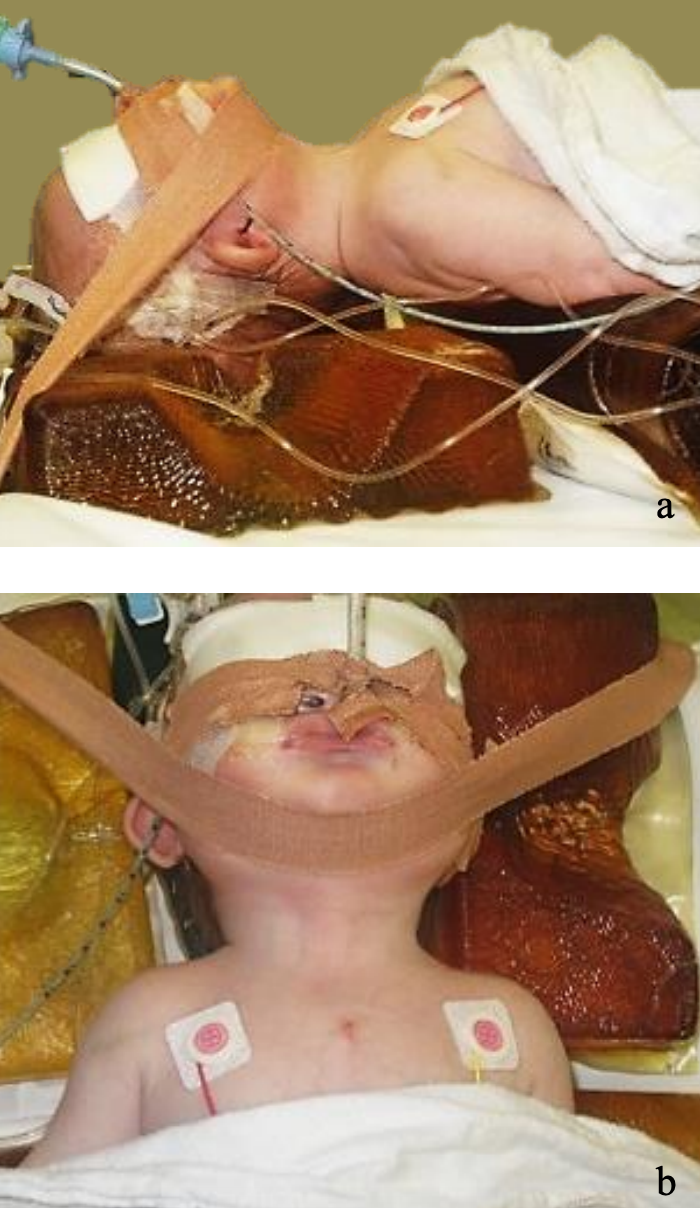
Figures 3a, b: Positioning with shoulder roll, head ring and chin tape
A shoulder roll is used to extend the neck and a head ring to stabilize the head. The head is taped in the midline position with an adherent surgical tape attached to the operating table, stuck down under the chin and then secured again to the operating table on the other side (Figures 3a,b). It may not be possible to fully extend the neck in certain cases for fear of causing atlantoaxial subluxation e.g. with Trisomy 21 (Down’s syndrome) or achondroplasia. Care is taken to avoid excessive cervical hyperextension as it may cause mediastinal structures to present in the neck and place them at risk of injury.
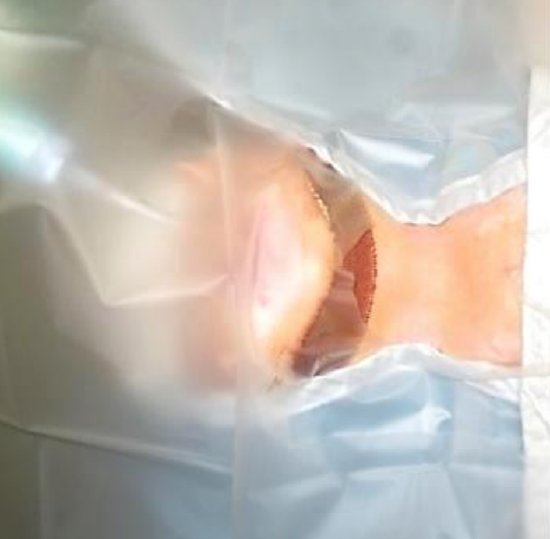
Figure 4: Clear sterile drape making it possible to monitor and manipulate the orotracheal tube during surgery
A clear sterile drape is ideally used over the head (Figure 4) as it makes it possible to observe the endotracheal tube throughout the procedure and makes it easier for the anesthetist to manipulate the endotracheal tube.
Skin Incision
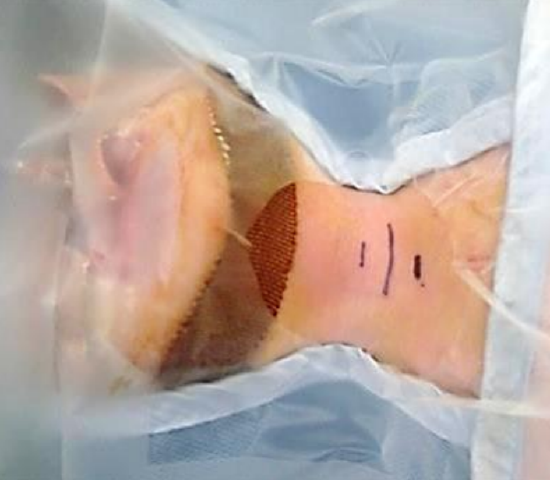
Figure 5: Surface landmarks: The incision (long line) is placed halfway between cricoid cartilage and suprasternal notch
The site of the incision is marked midway between the cricoid cartilage and suprasternal notch (Figure 5). Local anesthetic with adrenaline is infiltrated into the area of the planned incision. The maximum length of incision extends between the anterior borders of the sternocleidomastoid, although this is rarely required. A vertical skin incision is reserved for urgent tracheostomies where preoperative intubation cannot be achieved and a surgical airway is urgently required.
Removal of subcutaneous fat
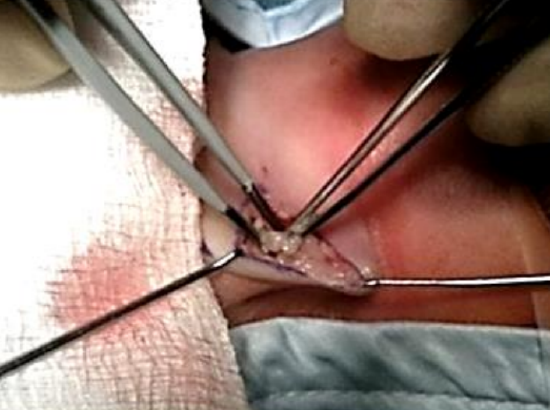
Figure 6: Removing subcutaneous fat using bipolar dissection technique
The incision is continued through skin into the subcutaneous layer of fat (more prominent in younger children). The subcutaneous fat is removed from both the superior and inferior skin flaps using bipolar diathermy (Figure 6); this facilitates positioning of the maturation sutures. Emphasis is placed on meticulous hemostasis as well as dissecting strictly in the midline.
Exposure and parting of strap muscles
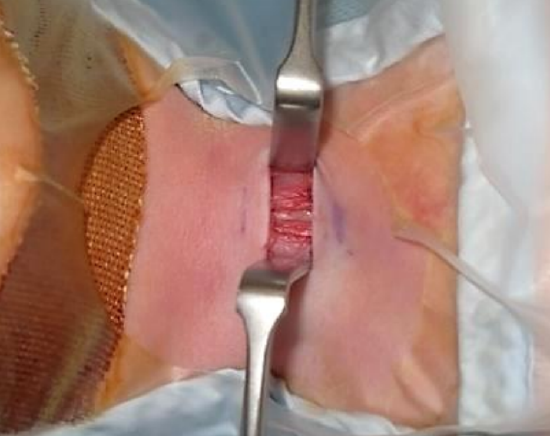
Figure 7: Skin and subcutaneous tissue retracted to expose strap muscles
The platysma muscle is generally absent in the midline. Care is taken not to transect the anterior jugular veins which are just superficial to the strap muscles within the investing cervical fascia; they can be preserved and retracted laterally. The midline cervical fascia between the strap muscles is identified (Figure 7). The strap muscles can then be parted in the midline using bipolar diathermy or blunt dissection and retracted laterally to expose the thyroid isthmus.
Dividing thyroid isthmus
The thyroid isthmus is retracted superiorly or divided using bipolar diathermy. The trachea is then cleaned using a small damp gauze swab or a peanut swab. Again, meticulous hemostasis is ensured. The positions of the cricoid cartilage and tracheal rings 2-5 are determined. It is important to avoid injury to the first tracheal ring so that subglottic stenosis does not occur. Care must be taken to avoid the innominate artery which crosses the trachea lower down (usually below the 5th tracheal ring), as injury or pressure of the tracheostomy tube on the artery can rupture the vessel wall and cause fatal hemorrhage.
Stay Sutures
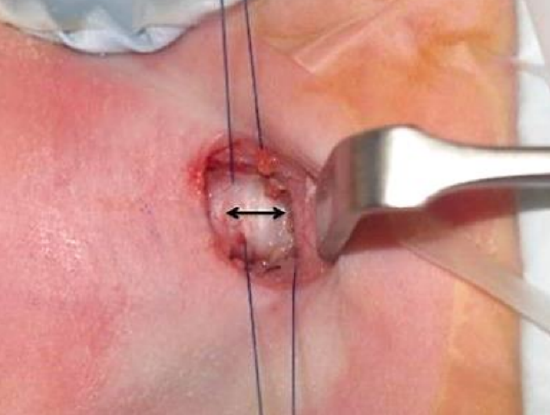
Figure 8: Placement of bilateral stay sutures in the tracheal wall on either side of the planned tracheal incision (double arrow)
Non-absorbable stay sutures are passed through the tracheal wall on either side of the midline prior to making any tracheal incisions (Figure 8).
The needles at the ends of the sutures are then removed and the ends of each suture are secured in an artery clip on each side of the neck. Upward and lateral pull on the stay sutures brings the trachea to the surface to allow easy insertion of the tube in the event of accidental decannulation or loss of the airway following incision of the trachea.
Tracheal incision
A vertical slit is made across two tracheal rings between the stay sutures in the midline of the tracheal wall between the 2nd - 5th tracheal rings.
Maturation sutures
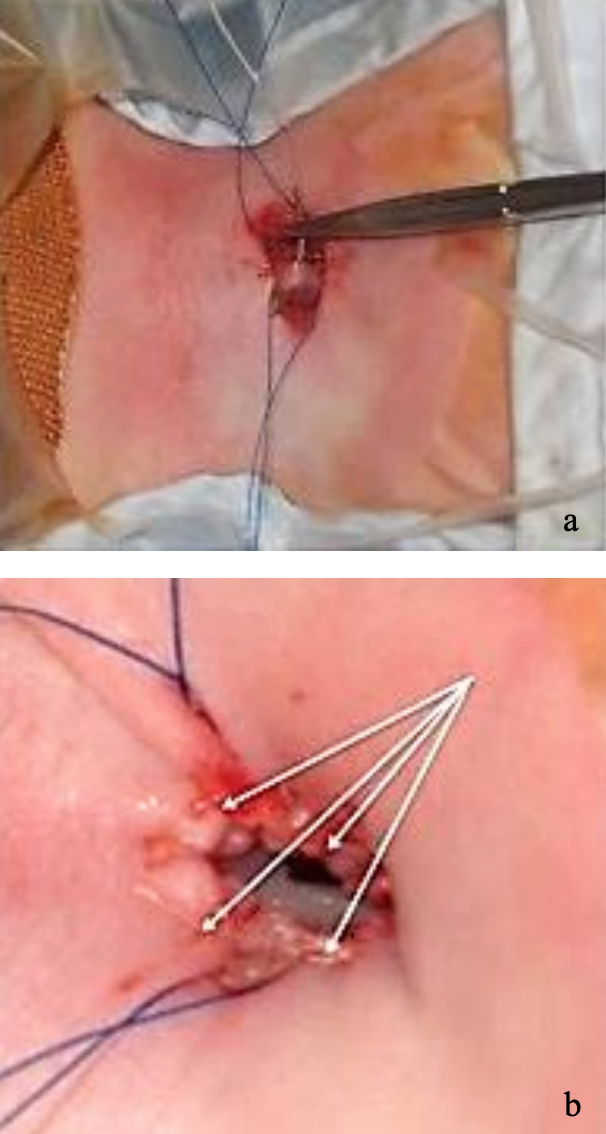
Figures 9 a, b: Placement of first maturation suture (a) and final formal stoma with four maturation sutures in place (b)
Maturation sutures are absorbable sutures that secure the trachea to the skin, creating a formal, safe stoma and making reinsertion of a tracheostomy tube easier in the event of accidental decannulation (Figure 9). They are placed prior to insertion of the tracheostomy tube with the endotracheal tube still in place. The inferior maturation sutures are the most important and are placed between the inferior end of the vertical tracheal slit and the inferior skin edge; they obliterate the space between the trachea and the skin and prevent formation of a false tract when inserting the tracheostomy tube.
Between placing successive sutures, the tracheal slit may be occluded in order to prevent anesthetic gases escaping and to aid ventilation, by carefully pulling the stay sutures together and closing the tracheal incision.
Insertion of tracheostomy tube
Once the maturation sutures have been fashioned, the anesthetist is alerted and the anesthetic tubing, the circuit connection, the tracheostomy tube, an artery clip (in case dilatation of the stoma is required) and suction are made available. The surgeon should be ready with the tracheostomy tube while the assistant carefully pulls upwards and laterally on the stay sutures to bring the trachea to the surface.
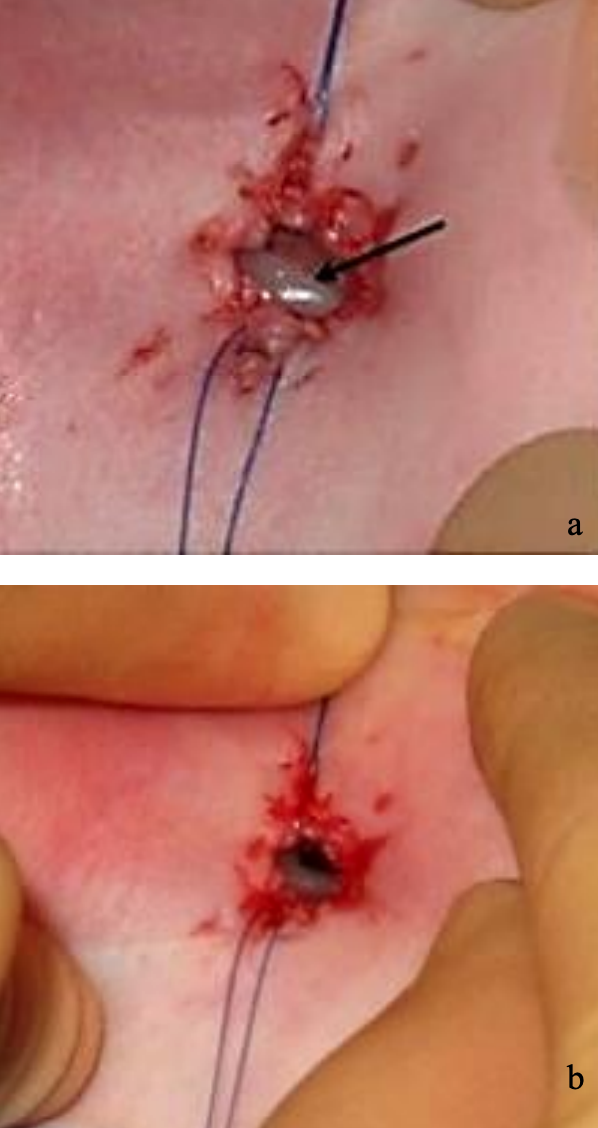
Figures 10 a, b: Endotracheal tube visible in stoma (a); the anesthetist is asked to withdraw the tube until only the tip is visible prior to insertion of the tracheostomy tube
The anesthetist is asked to slowly withdraw the endotracheal tube until only the distal tip of the endotracheal tube is visible; the tracheostomy tube is then inserted under direct vision (Figure 10). The obturator of the tracheostomy tube is then removed and the tube is connected to the anesthetic circuit. The tip of the endotracheal tube should remain in position extending beyond the glottis to just above the tracheostoma until the tracheostomy tube has been secured.
In the event of dislodgement or inability to ventilate via the tracheostomy tube the endotracheal tube can again be advanced past the stoma for the patient to be ventilated. The anesthetist confirms correct placement of the tube by listening to the chest and by confirming the presence of CO2 on the capnograph. The neck wound can then be partially sutured closed laterally if required. The tube is then secured around the neck using cotton tapes; the tension on the tapes should ensure that the tube is secure and cannot be pulled out when the head is flexed. A useful check to ensure correct tension on the tapes is that it should be possible to insert only one finger beneath the tapes.
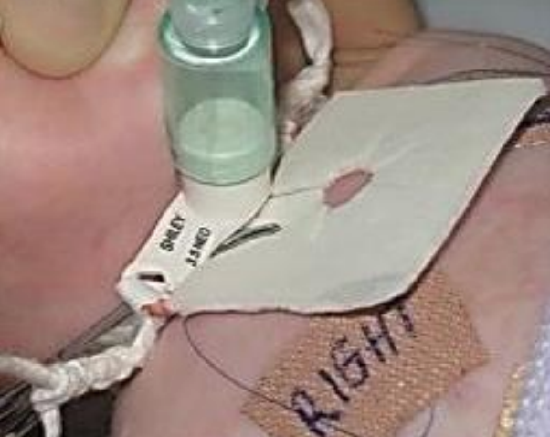
Figure 11: Placement of dressing under flanges of tracheostomy tube
The tracheostomy tube should never be secured by suturing it to the skin, as the skin in a pediatric patient is very lax and can result in accidental decannulation while still sutured to the skin. A nonadherent dressing is placed under the flanges of the tracheostomy tube using an artery clip (Figure 11).
The position of the tube is then assessed by passing a flexible fibreoptic scope through the tracheostomy tube. Ideally the tip of the tube should be positioned well above the carina so that the tip does not slip down one bronchus on hyperflexing the neck.
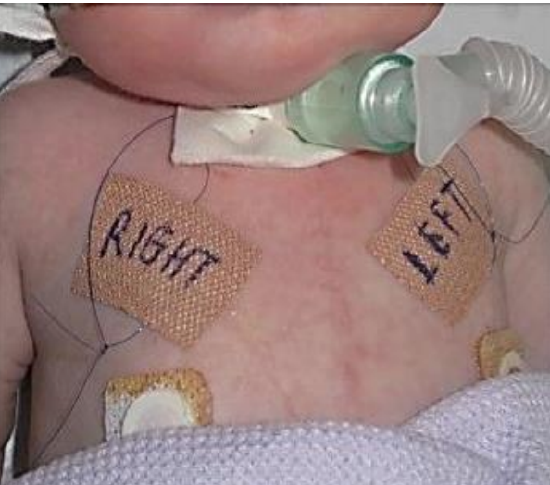
Figure 12: Stay sutures are taped to the chest at end of the procedure
The stay sutures are then stuck to the chest wall and labeled “RIGHT” and “LEFT”, and ‘DO NOT REMOVE’ (Figure 12).
Early postoperative complications
- Hemorrhage
- Pneumothorax, pneumomediastinum
- Damage to lateral structures such as the recurrent laryngeal nerves, carotid sheath or esophagus
- Loss of respiratory drive
- Pulmonary edema tracheostomy tube problems such as displacement and blockage
- Subcutaneous emphysema (avoid by not suturing skin too tightly)
- Swallowing difficulties
- Local infection
Postoperative care
- Chest X-ray to
- Exclude pneumothorax
- Exclude surgical emphysema
- Check tube length and confirm tip position relative to carina
- If a cuffed tube is required, the pressure in the cuff should be checked and monitored
- Antibiotics may be required for a week postoperatively
- Nursing staff should be informed how to use the stay sutures
- Nursing staff are informed about the correct length of the suction tube to avoid distal tracheal trauma and granulations distal to the tip of the tracheostomy tube
- The child should have a tracheostomy box for his/her sole use at the bedside that contains an introducer/obturator, spare tracheostomy tube of same type and size, tracheostomy tube one size smaller, appropriately sized suction catheters, spare tapes, spare non-adherent dressings, curved round-ended scissors and lubricant jelly. A Swedish nose used for humidification, and speaking valves may also be included
- A small artery clip or appropriately sized tracheal dilator should be available at the bedside
Resuscitation steps
In the event of finding an unresponsive tracheotomized child the following steps should be followed
- Attempt to arouse the child while calling for help
- Attempt to suction the airway
- If there is difficulty suctioning or the tracheostomy tube is blocked, change the tracheostomy tube immediately and attempt suctioning again
- If this fails, the smaller size tracheostomy tube is inserted
- If this fails a tracheal suction tube is passed down the lumen of the smaller tube and an attempt is made to guide the tracheostomy tube over the suction tube (Seldinger technique)
- If still unsuccessful, a flexible endoscope with a tube first threaded over it may be used by experienced staff to insert the tracheostomy tube under direct vision
- Concurrently with the above steps, any other possible means of ventilating the child are employed i.e. bag & mask, endotracheal tube intubation etc.; the possibility of doing this depends on the underlying pathology
- Only experienced personnel should use tracheostomy dilators or an artery clip to dilate the tracheal stoma if it has started to close down
- Check whether the child is breathing after reinserting the tracheostomy tube; a self-inflating bag ventilation device may be required to provide rescue breaths
First tube change
The first tube change should take place one week following tracheostomy. Essential equipment includes suctioning, supplementary oxygen, appropriate tracheostomy tube with tapes already attached, nonadherent dressing, 0.9% sterile saline solution, small sterile pot, water-based lubricant and gauze swabs.
The child is kept starved for several hours to decrease the risk of aspiration. Wrap a younger child in a small sheet or blanket. A shoulder bolster is placed to extend the neck. The assistant swaddles the baby allowing exposure above the shoulders. The tracheostomy is suctioned if required prior to tube change.
The new tracheostomy tube is lubricated at the outside bend of the tube with a tiny amount of water-based lubricant. The stay sutures are left in position but freed from the chest wall in case they need to be used to apply traction to. Once everything is ready the old tube is removed and replaced with the new tube.
The assistant holds the new tube in position while ventilation is observed. While the assistant holds the tube in place the tapes are secured. The stay sutures are then removed.
Follow-up and aftercare
A child with a tracheostomy requires regular microlaryngoscopy and bronchoscopy to exclude granuloma formation or suprastomal collapse and to follow the progress of the underlying pathology that led to the tracheostomy. The frequency of microlaryngoscopy and bronchoscopy depends on the underlying etiology. Corrective surgery can be planned, working towards the ultimate goal of decannulation. As the child grows the tracheostomy tube may need to be upsized or the length adjusted.
Late complications
- Tracheal granulomas
- Accidental decannulation and blockage
- Suprastomal collapse
- Tracheomalacia
- Speech and language development delay
- Persistent tracheocutaneous fistula following successful decannulation
Decannulation
Prior to considering decannulation the initial reason for the tracheostomy should have been resolved or been effectively managed. Microlaryngoscopy and bronchoscopy should be undertaken a maximum of 6 weeks prior to planned decannulation to check the status of the trachea and in particular to look for suprastomal collapse or granulomas that may need treating prior to decannulation.
The child should be well at the time of decannulation; ideally it should be undertaken during seasons when infections are less frequent. The child should be admitted to the hospital for observation during any decannulation regime in case emergency reinsertion of the tube is required.
Decannulation protocol
The following steps should ensure safe decannulation
- Decannulation occurs over several days
- Pulse oximetry is undertaken during this time
- The tracheostomy tube is gradually downsized to size 3; if the child weighs <10 kg then they can be downsized to a size 2.5 tracheostomy tube
- Each tube remains in situ for 24 hrs
- The tube is then blocked, initially during the day for 12 hrs
- If successful, then this can be extended to 24 hrs
- Once the tracheostomy has been successfully plugged for 24 hrs then the tube is removed and the stoma closed with an adhesive dressing
- The child is observed on the ward for an additional 48 hrs
- If there is any airway compromise the procedure is abandoned and the tracheostomy tube is reinserted.
- Chest physiotherapy may be required to help clear secretions
- Parents/carers need to undergo resuscitation training
- The parents/guardians are advised that, should there be any concern regarding the airway, the child should be brought back to hospital
- The child is reviewed in an outpatient clinic 6 weeks following decannulation
Important tips
- Do tracheostomies under general anesthesia with an endotracheal or nasotracheal tube in situ
- Position the patient as described
- Excise sufficient subcutaneous fat
- Dissect in the midline at all times
- Ensure meticulous hemostasis
- Use both stay sutures and maturation sutures
Author
Hasnaa Ismail-Koch BM, DLO, DM, FRCS (ORL-HNS)
Consultant Otolaryngologist (Locum)
Southampton General Hospital
Hampshire, United Kingdom
hasnaa@doctors.org.uk
Author and Pediatric Section Editor
Nico Jonas MBChB, FCORL, MMed
Pediatric Otolaryngologist
Addenbrooke’s Hospital
Cambridge, United Kingdom
nico.jonas@gmail.com
Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


