4.2: Endoscopic Transsphenoidal Pituitary Tumor Resection
- Page ID
- 15448
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
ENDOSCOPIC TRANSSPHENOIDAL (ETSS) PITUITARY SURGERY TECHNIQUE
Moses Penduka, Patrick Semple, Darlene Lubbe
Endoscopic transsphenoidal pituitary surgery (ETSS) is generally indicated for patients with symptomatic pituitary micro and macroadenomas causing symptoms such as visual loss, headaches or hormone associated problems. It has become the standard approach, surpassing traditional microscopic approaches, although the literature does not conclusively prove which approach is superior with regards to complications and outcomes. The superiority of the endoscopic approach lies with better light penetration at the target area, improved visualization provided by angled telescopes, minimal collateral tissue damage with quicker recovery than with an open approach and preservation of intranasal anatomy and function. Access to the pituitary fossa in revision endoscopic transsphenoidal surgery is much quicker and less invasive than other approaches because the bony surgical corridor has already been made.
Endoscopic Anatomy
The transnasal transsphenoidal approach to the pituitary implies that the surgical corridor is created by working medial to the middle turbinates. A single nostril or bilateral approach can be used depending on whether one or two surgeons are working simultaneously and whether multiple instruments need to be manipulated at the target area. For small microadenomas, some surgeons use a single nostril approach. This usually means the mucoperichondrium of the septum from one side can be preserved. For a bilateral approach, a partial posterior septectomy is required.
ETSS is divided into 3 stages
- Nasal stage
- Sphenoid stage
- Sellar stage
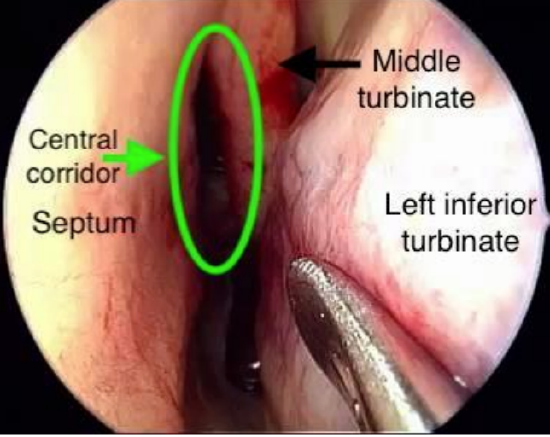
Figure 1: Initial view during nasal stage
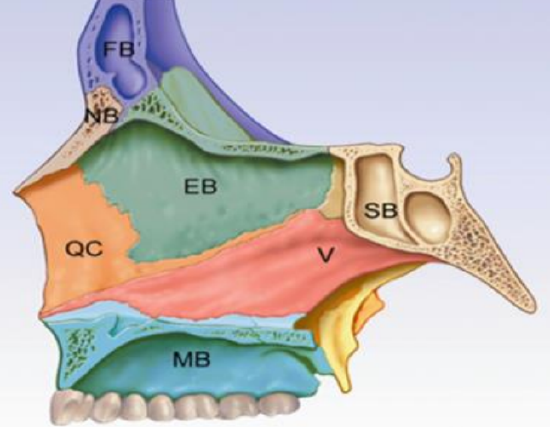
Figure 2: Nasal septum. QC: Quadrangular cartilage, EB: Ethmoid bone, V: Vomer, SB: Sphenoid bone, MB: Maxillary bone
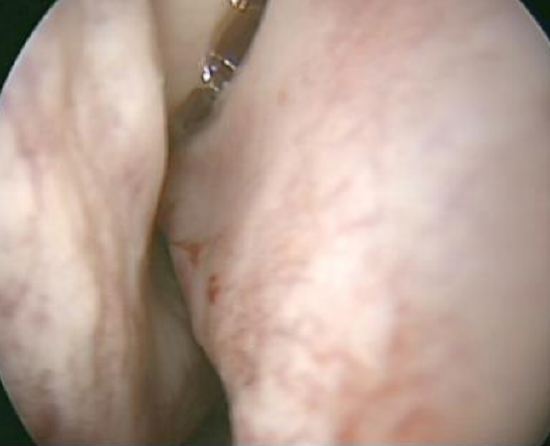
Figure 3: Right-sided septal spur
During the nasal stage, it is important to identify the anatomy of the related structures and to identify any anomalies that may hamper access to the pituitary fossa (Figures 1-3)
- Nasal septum: septal deviations, perforations, or a septal turbinate
- Inferior turbinates: hypertrophied turbinates
- Middle turbinates: concha bullosa, paradoxical turbinate
- Structures lateral to middle turbinate: uncinate process, ethmoid bullae - signs of infection draining from the maxillary sinus, nasal polyps
- At level of skull base: attachment of septum to cribriform plate. Olfactory mucosa at 1 cm superior aspect of septum to be preserved
The Open Access Atlas chapters on Endoscopic ethmoidectomy and Sphenopalatine artery ligation provide further detail of the anatomy of these structures.
Nasal septum
Anatomical anomalies are common and that these may affect access and hinder the creation of an adequate surgical corridor for manipulation of multiple instruments using a binasal approach. It is important to perform anterior rhinoscopy at the initial ENT consultation to assess the need for a septoplasty. Performing a septoplasty may lengthen the time of the procedure and it is important to plan for this beforehand. Septal anomalies may include:
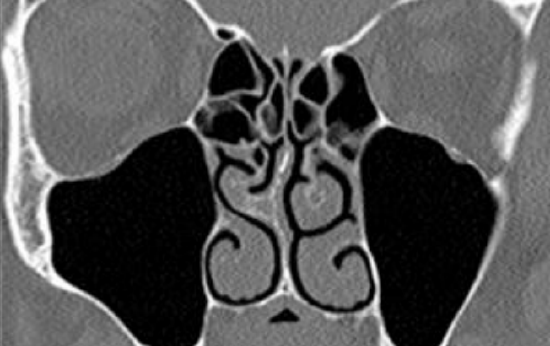
Figure 4: CT radiograph showing right sided septal spur
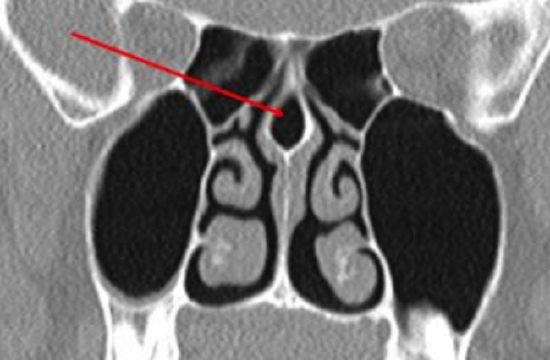
Figure 5: CT radiograph showing a septal turbinate
- Septal spurs can be removed with a simple Killian’s incision placed anterior to the spur (Figures 3, 4; Video clip)
- Septal deviations may require a formal septoplasty via a hemitransfixion incision before creating the surgical corridor. Harvesting a septal mucoperichondrial flap needs to be kept in mind since it is easier to elevate the flap with the perpendicular plate of the ethmoid and vomer still intact. Therefore, elevate the flap before a septoplasty is done
- Septal turbinates: It is important to recognize the presence of a pneumatized posterior septum since entering this ‘cavity’ can be misleading and an inexperienced surgeon may think the sphenoid sinus has been entered (Figure 5)
Lateral wall of nasal cavity
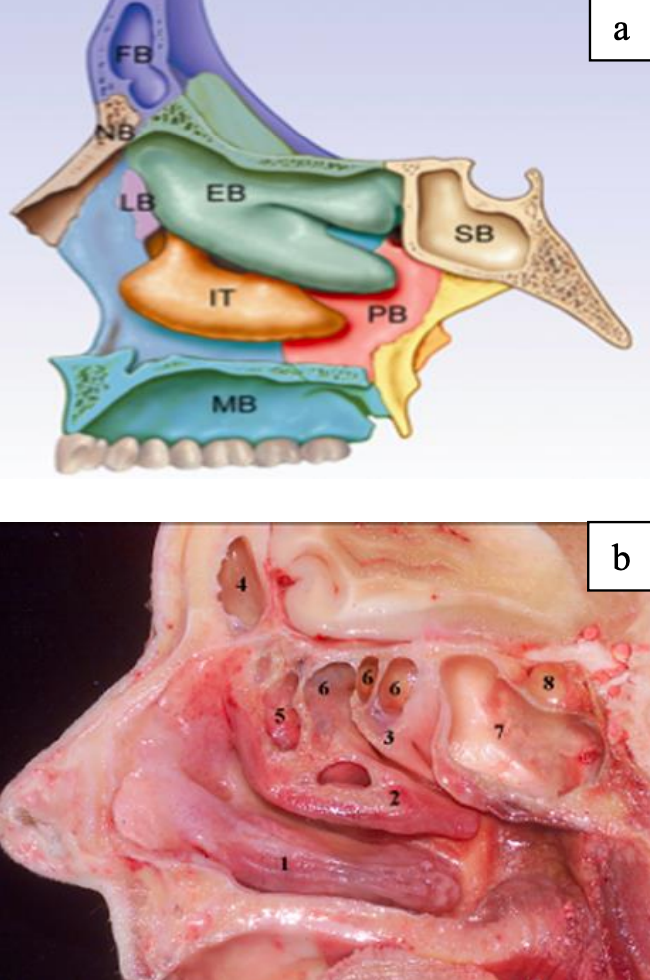
Figures 6a, b: Anatomy of the lateral wall. The top figure illustrates the various bones that form the lateral wall; IT (inferior turbinate), EB (ethmoid bone), SB (sphenoid bone), PB (palatine bone), LB (lacrimal bone). The lower figure illustrates the inferior, middle and superior turbinates (1, 2 & 3) and related air cells; frontal (4), agger nasi (5), ethmoid cells (6) and sphenoid sinus (7). The superior turbinate is an important landmark for the sphenoid sinus ostium
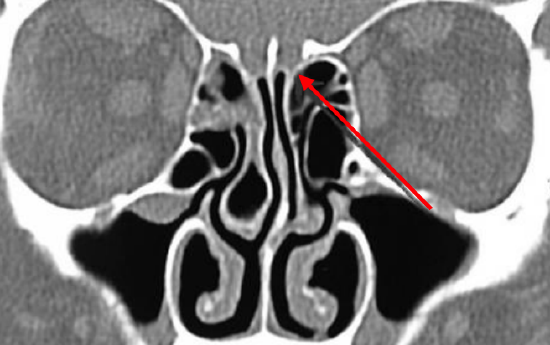
Figure 7: Attachment of middle turbinate to the skull base
Figures 6ab illustrate the anatomy of the lateral nasal wall of the nose. It is important to remember that the middle turbinate attaches to the skull base and that undue manipulation of the middle turbinate could lead to a fracture at the point where the middle turbinate attaches to the lateral lamella of the cribiform plate (Figure 7). This may cause a CSF leak.
Anatomical anomalies involving the turbinates are also common and include
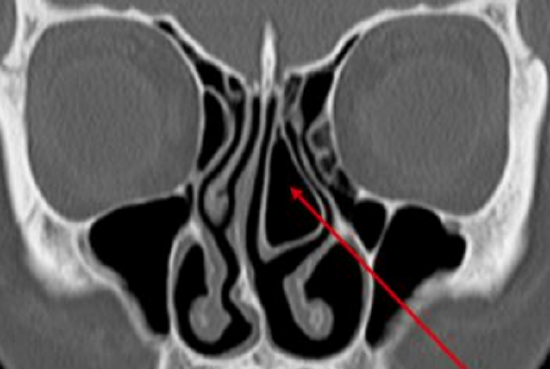
Figure 8: Concha bullosa of middle turbinate
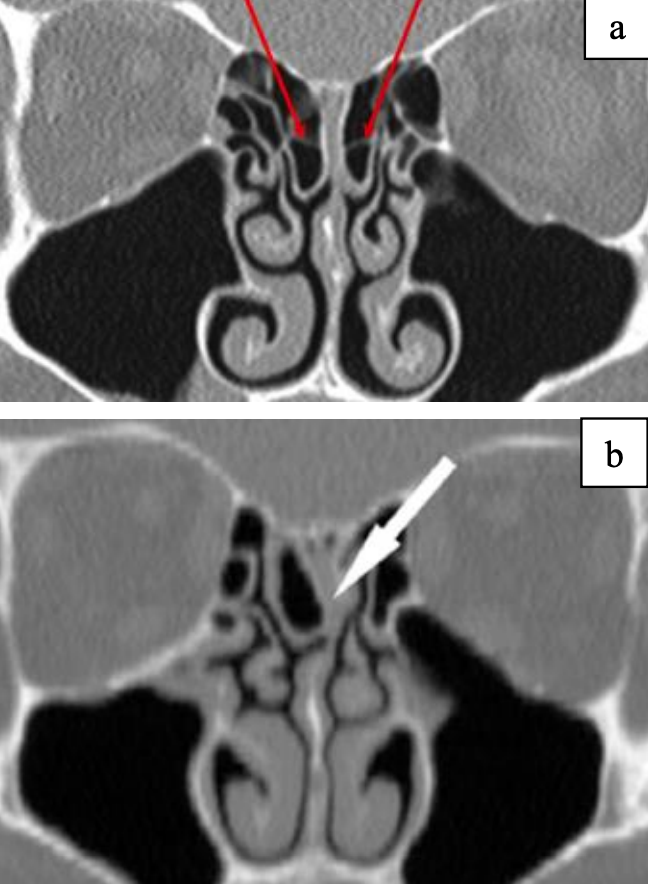
Figures 9ab: Superior turbinate conchae
- Inferior turbinate hypertrophy
- Turbinate conchae (concha bullosa) (Figures 7, 8, 9ab)
- Paradoxical/duplex middle turbinates
It is important that the olfactory epithelium be protected when working on these structures. Olfactory mucosa should be preserved in the following areas:
- Mucosa of superior-medial aspect of the middle turbinate
- Superior aspect of superior turbinate
- Superior aspect of the septal mucosa (superior ½ in relation to the height of the middle turbinate)
Sphenoid sinus
The sphenoid sinus must be approached after carefully reviewing the preoperative radiographs as anatomical variations are common. The ostium should be located prior to elevating the mucoperichondrial septal flap.
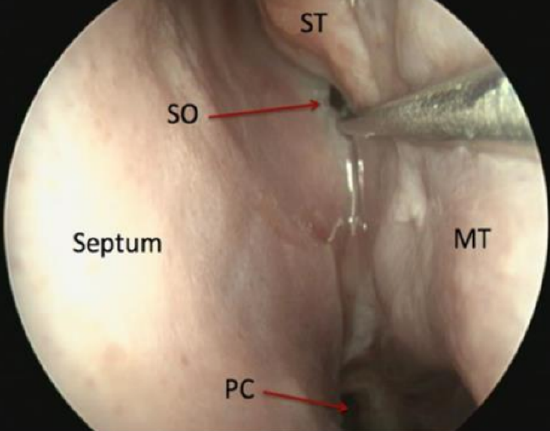
Figure 10: View of the sphenoid sinus ostium (SO) in sphenoethmoidal recess; this ostium is 2½ sucker tips above the posterior choana (PC)
The sphenoid ostium is located medial to the superior turbinate in about 85% of individuals at a level horizontal to the superior border of the natural ostium of the maxillary sinus (Figure 10).
It can also be easily located by counting about 2½ sucker tips above the posterior choana.
- Pass the endoscope to the posterior aspect of the nasal cavity
- Locate the posterior aspect of the middle turbinate
- Then gently lateralize the posterior aspect of the middle turbinate
- Slide the 0-degree endoscope into the area between the middle turbinate and the nasal septum
- Identify the superior turbinate
- Use a Freer suction elevator to gently palpate the sphenoid face just medial to where the mid-1/3 of the superior turbinate meets the lower 2/3 of the turbinate
- The Freer should easily slide into the natural ostium
- Turn the Freer sideways to open the membranous part of the sphenoid ostium
- Commence the mucoperichondrial septal flap at this level to avoid injury to the posterior septal artery which lies just below the ostium
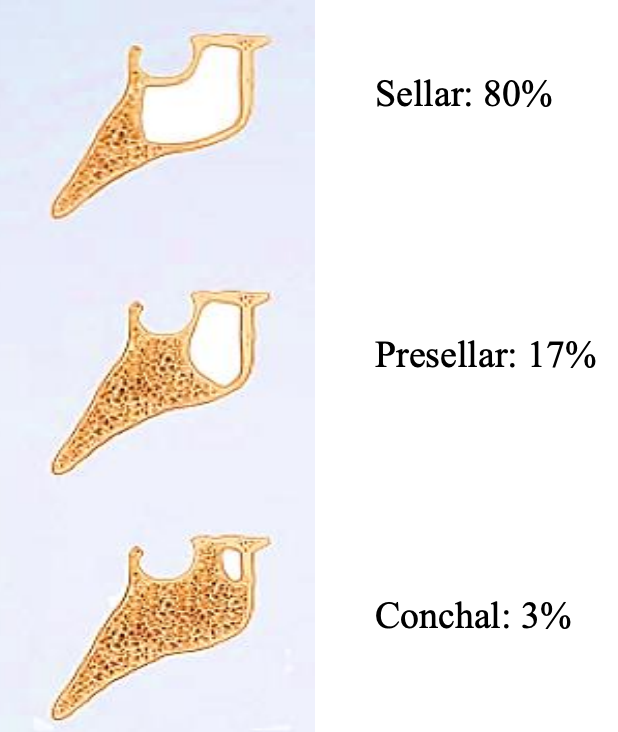
Figure 11: Variations in the sellar configurations
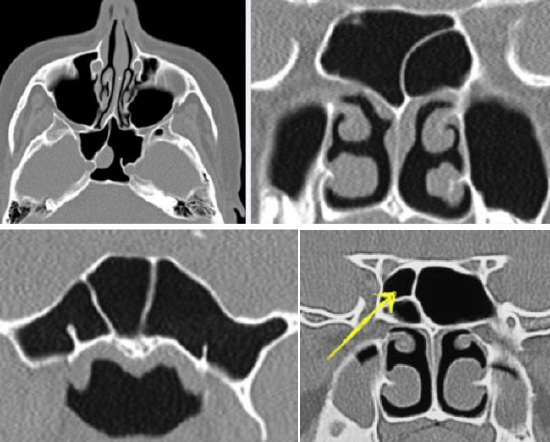
Figure 12: Variety of sphenoid intersinus septum configurations
In a study by Ossama et al variations of the sphenoid sinus include pneumatization, sellar configuration (Figure 11) and septation (Figure 12).
Pneumatisation affects access to the sella especially if the sellar bulge is ill-defined. Intersphenoid and accessory septa may attach laterally to the carotid prominence (Figure 12). As a rule, one should assume that any septa may attach to the carotid canal and assess this risk carefully on imaging before ETSS.
The posterior branch of the sphenopalatine artery (posterior septal artery) must be preserved as it is the basis of the Hadad Bassagastagy flap. It runs across the face of the sphenoid below the sphenoid ostium to supply the posterior septum. This blood vessel can be sacrificed on the opposite side, but care must always be taken with this vessel since it is the most common reason for significant postoperative bleeding requiring further surgery to arrest the bleeding.
Preoperative consent
A team approach to the workup of a patient is of utmost importance and should include the neurosurgeon and rhinologist. The patient must be informed of both the medical and surgical complications that may follow pituitary surgery that include:
- Diabetes insipidus
- Endocrine abnormalities and remission outcomes
- Visual outcomes
- Postoperative CSF leaks and their management, including meningitis
- Rhinologic complications such as adhesions, perforations, sinusitis, mucocoele formation
- Carotid artery injury
- Postoperative sellar hematoma
- Mortality
Anesthesia, positioning and draping
- The authors administer intravenous Cefazolin 1 gm at commencement at induction of anesthesia
- The surgical setup is similar to most endoscopic sinonasal procedures (see chapter on Endoscopic ethmoidectomy)
- General anesthesia with total intravenous anesthesia (TIVA) is preferred to achieve a normotensive state with low pulse rate
- A throat pack is not routinely used in our unit due to subsequent throat discomfort and the risk of patients swallowing the pack during the end of anesthesia. Others insert a throat pack to minimize risk of aspiration and swallowing of blood which may cause gastritis with postoperative nausea and vomiting
- The patient is placed supine with the head slightly flexed, elevated and turned towards the operating surgeon who usually stands on the right of the patient (right-handed surgeon)
- Cover the eyes with transparent adhesive plastic sheeting
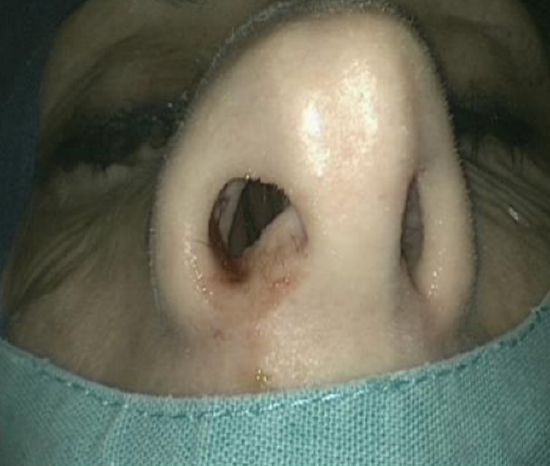
Figure 13: Pituitary preparation with the eyes and nose visible after draping
- Drapes are placed so that both eyes and the nasal cavity are visible (Figure 13)
Surgical steps
Numerous surgical steps must be followed to ensure an uneventful surgical exposure and pituitary resection:
- Field preparation: preoperative packing and infiltration
- Optimizing access: septoplasty, turbinate surgery
- Identifying sphenoid ostium
- Raising mucoperiosteal flap
- Posterior septectomy and sphenoidectomy
- Reducing sphenoid septations and exposing the sella
- Sellar stage of endoscopic pituitary surgery
- Closure of surgical corridor
- Postoperative care
1. Field preparation
Topical decongestion is achieved as described in the chapter on Endoscopic Ethmoidectomy.
- Neuropatties soaked with a mixture of 2 ampoules of 1:1000 adrenaline diluted with 1 mL oxymetazoline, achieve optimum decongestion
- Place the patties between the septum and the inferior and middle turbinates
- If possible, place a pattie between the septum and the middle turbinate. This makes elevation of the sphenoid ostium easier
- Allow at least 10 minutes of decongestion by packing the nasal cavity before the scrub nurse preps and drapes the patient
- Further decongestion is achieved at the start of the surgical procedure by submucosal injection with Xylotox into the inferior turbinate, middle turbinate and septum. This gives the added advantage of hydro-dissection for the Hadad flap that will be elevated off the septum. Be careful not to inject too rapidly as this may cause a rapid rise in blood pressure which may be detrimental especially in the elderly hypertensive patient. Very little (0.1 mL) Xylotox is injected into the inferior turbinate, and very slowly, as this structure is extremely vascular
2. Optimizing access
- Inspect the nose with the endoscope using the traditional 2-pass strategy. This is important in order to appreciate the anatomy and characteristics of any abnormalities that might be present
- Out-fracture the inferior turbinates using a Freer’s dissector to improve access. Placed in the inferior meatus, the Freer’s dissector is used to first infracture the inferior turbinate then placed medially to out-fracture
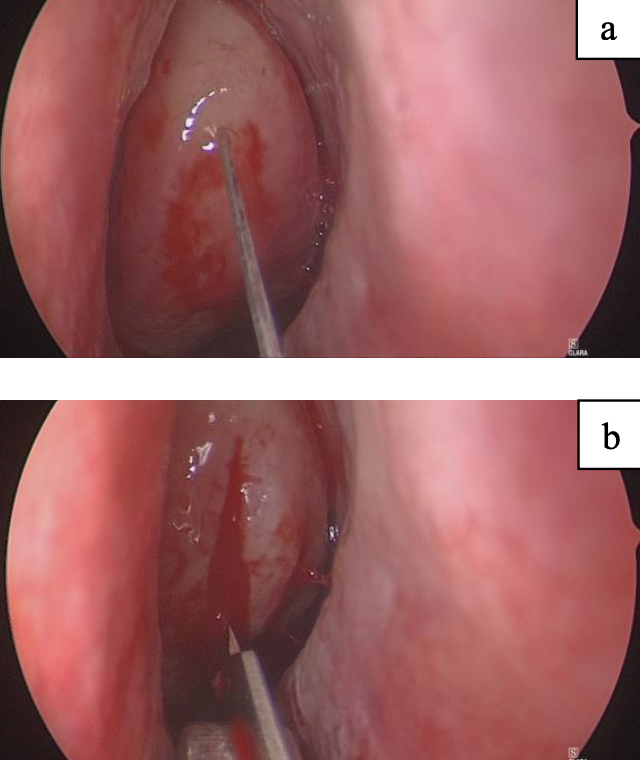
Figures 14 ab: Incising a concha bullosa
- If a concha bullosa has been identified it is reduced on its medial aspect to widen the transnasal corridor (vs lateral reduction required during FESS surgery). First confirm its presence by entering the concha using the needle of a dental syringe. A “give” is easily felt and is confirmed by unrestricted flow when injecting into this space. Enter the concha with a 12-scalpel blade and divide it along its length anteriorly and inferiorly (Figure 14). A through-biting instrument is then used to remove the medial aspect of the concha
- Septoplasty may not be required if a concha bullosa has been reduced. It will however be required if a septal spur compromises access. The technique for septoplasty is described in the chapter on septoplasty. It is important to remember that the Hadad flap will be raised and caution should be taken not to compromise the blood supply to the flap when doing the septoplasty. It is important to stay above the level of the sphenoid ostium when making the superior cut of the mucoperichondrial septal flap. A posterior septectomy is required for the binasal approach after the mucoperichondrial flap has been elevated on one side. The perpendicular plate of the ethmoid and the vomer and the opposite septal mucosa can be removed to create the posterior septectomy and corridor to the sphenoid sinus.
3. Identifying the sphenoid ostium
The sphenoid sinus ostium can be easily identified using the transethmoidal or transnasal corridors. However, in this instance, a middle meatal antrostomy and ethmoidectomy are hardly indicated. The only indication for doing a middle meatal antrostomy and ethmoidectomy would be for patients with concomitant sinus disease to avoid postoperative infection from these infected sinuses.
- Using the transnasal midline corridor between middle turbinate and nasal septum (Figure 1), the ostium is identified medial to the lower 1/3 of the superior turbinate
- The distance between the sphenoid sinus ostium and the posterior choana is gauged by counting 2½ sucker tips from the choana superiorly, staying medial to the superior turbinate (between superior turbinate and septum) (Figure 10)
- Once the ostium is located it is initially widened superiorly and medially
- Inferiorly, the posterior septal artery will be encountered
- On the side that the mucoperichondrial flap has been elevated, the artery must be preserved
- On the opposite side it can be sacrificed to drill the rostrum down to the floor of the sphenoid sinus
- The sphenoidotomy is widened using mushroom punch forceps, a Kerrison punch or endonasal drill
4. Raising mucoperiosteal flap
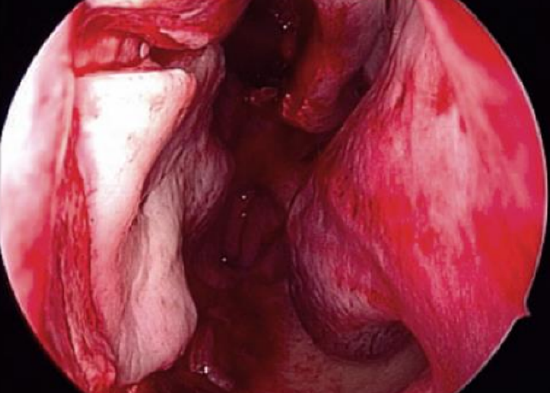
Figure 15: Harvesting the Hadad flap from the left nasal septum
The Hadad flap is important to repair CSF leaks, a known complication of skull base surgery (Figure 15). It is a robust, vascularized flap based on the posterior septal artery. Remember the anatomical relationships of the posterior septal artery to the sphenoid sinus ostium and the olfactory epithelium to preserve the blood supply to the flap.
- The authors prefer to create the flap on the left side to avoid neurosurgical instruments damaging the flap. The endoscope is usually held on the same side as the flap by the ENT surgeon while the neurosurgeon works on the opposite side, thereby avoiding damage to the flap
- The boundaries of the flap are
- Medial aspect of sphenoid sinus ostium
- Anteriorly, to just in front of the anterior end of the middle turbinate at a level of the midpoint of its height
- If additional length is required for a large CSF leak, the flap can be extended via a hemitransfixion incision onto the floor of the nose, lateral to the inferior turbinate
- Outline the flap using suction diathermy to ensure minimal bleeding
- Cut the mucoperiosteum down to the bone/cartilage along the boundaries described above, using a 15-blade or a Cottle dissector
- Elevate the flap in a submucoperiosteal plane as during a septoplasty
- Dissect from anterior-to-posterior up to the rostrum
- Once the anterior cut has been made and mucosa lifted, a turbinectomy scissors can be used to make the superior cut
- The inferior cut is only made if the flap is to be used for repair of a CSF leak
- If only a superior cut was made, then the flap is rolled inferiorly and out of the way of the surgical corridor
- If no CSF leak occurs, the flap is replaced to close the posterior septectomy defect
- Suture the middle turbinates on either side of the flap (Videoclip)
5. Posterior septectomy and sphenoidectomy
- A posterior septectomy is required to fully expose the anterior face of the sphenoid sinus (Videoclip)
- Once the flap has been raised, parts of the sphenoid face and bony septum are exposed
- The bony posterior septum is quite thin
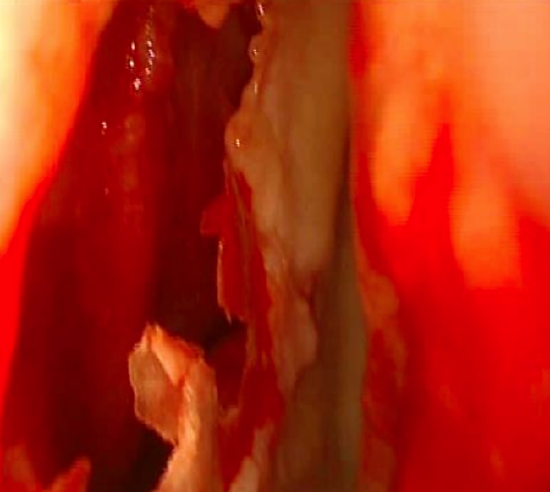
Figure 16: Posterior septectomy. Note the contralateral septal mucoperiosteum which may be sacrificed using back-biting forceps or a microdebrider
- Therefore, a posterior septectomy is performed by simply fracturing the perpendicular plate of the ethmoid with a Freer’s elevator and with back-biting forceps. Remove bone using Blakesley forceps (Figure 16)
- Elevate mucosa off the contralateral sphenoid sinus ostium using a Freer’s elevator
- Cauterize the mucosa of the sphenoid ostia using monopolar suction cautery
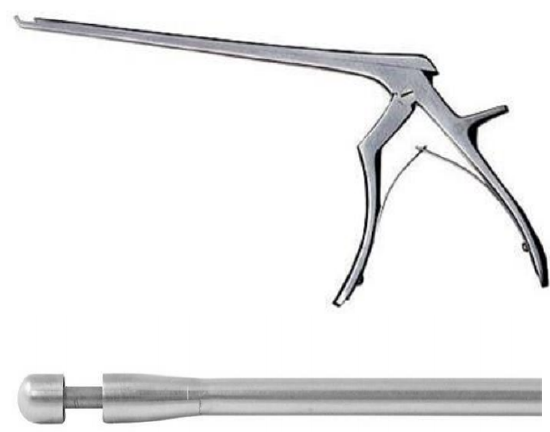
Figure 17: Kerrison punch (above) and tip of mushroom punch
- Remove the bone between the ostia with a Kerrison punch, mushroom punch (Figure 17), endonasal drill or hammer and chisel
- Lower the sphenoid face to the floor of the sphenoid sinus to allow instrumentation of the pituitary fossa
- Fully expose the sella
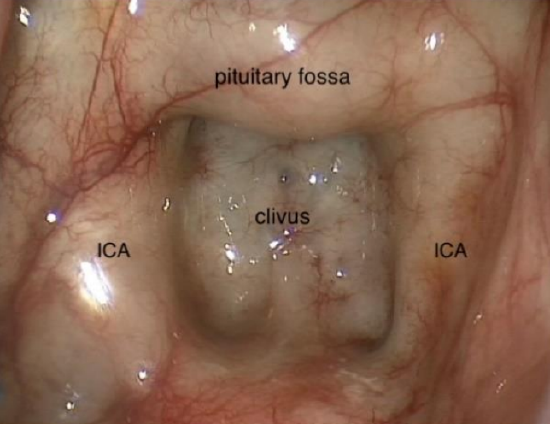
Figure 18: Sella, clivus, and internal carotid arteries (ICA)
- Identify the internal carotid arteries within the sphenoid sinuses (Figure 18)
6. Reducing sphenoid septations and exposing sella
- All sphenoid septations attached to the pituitary fossa are drilled down to expose the entire pituitary fossa
- Be extremely careful when reducing the sphenoidal septations as they may be attached to the internal carotid arteries (Figure 12). Therefore, sphenoidal septations must be reduced using through-biting instruments or a diamond drill
- Drill down the anterior wall of the pituitary fossa until only a thin eggshell of bone is left over the pituitary tumor or gland
7. Sellar stage of endoscopic pituitary surgery
The neurosurgeon performs the 2nd part of the surgery i.e. resection of the pituitary tumor. The ENT surgeon therefore moves to the opposite side of the table or to the head to manipulate the zero-degree 30 cm endoscope for the neurosurgeon.
- It is our practice for the otolaryngologist to hold the endoscope while the neurosurgeon uses two instruments in both hands to resect the pituitary tumor
- Both nostrils are used for access (binasal approach)
- With experience, the two surgeons become accustomed to working as a team and the movement of the endoscope and instruments become well-coordinated
- With the floor of the sella exposed, the neurosurgeon identifies the planum, optic prominences, opticocarotid recesses, carotid prominences and can identify the entry point to start the pituitary dissection (Figure 18)
- Use neuronavigation to confirm bony structures and the trajectory of the proposed opening in the floor of the sella
- The floor is usually very thin with macroadenomas
- Open the floor of the sella initially using a dissector and then a Kerrison upcutting forceps (Figure 17)
- If the floor is thicker it can safely be thinned using a drill prior to opening it
- The size of the opening is dependent on the size of the sella and the distance between the two carotid arteries, but should be large enough for insertion of instruments and to present an adequate view of the adenoma for its removal
- Neuronavigation provides added safety by using it to define the size of the opening, particularly relating to the internal carotid arteries, optic nerves and anterior fossa floor
- If neuronavigation is not available, then fluoroscopy can be used although it is limited to a lateral view
- Once an adequate opening in the floor of the sella has been made then the dura is incised
- Prior to incising dura, our practice is to use a Doppler at the proposed incision site to ensure that the carotid artery is not underlying and where it may be injured
- Open the dura with a cruciate incision or as an inferiorly based dural flap
- The tumor/adenoma now becomes visible, prolapsing through the opening
- Obtain a biopsy with a rongeur
- Most pituitary adenomas are soft; using an endoscopic approach is dependent on this characteristic
- If the pituitary adenoma is hard and firm and cannot be removed by a combination of curettage and suction, then this approach should be abandoned as there is an extremely high risk of injury to surrounding structures when the tumor is forcibly delivered
- Ideally, use 2 suction cannulae to methodically remove the tumor from the sella until the posterior capsule is seen
- Then proceed to remove tumor laterally up to the wall of the cavernous sinus
- A curette is used in conjunction with the 2 suction cannulae to remove tumor that is difficult to suck away
- The aim is to completely empty the sella of tumor and to allow suprasellar tumor to descend into the sellar field and to be removed
- Most of the surgery is done with a 0- degree endoscope, but a 30-degree endoscope can used to view and remove suprasellar and lateral tumor
- Neuronavigation can also be used at this stage to confirm the position of the instruments with regard to the image of the tumor as well as the position of other bony and neurological structures. However, it is important to realize that the navigation is not in real time and as the tumor is removed the position on the image is no longer accurate, except for the bony landmarks
- When working laterally in the region of the cavernous sinuses, a Doppler may again be useful to locate the internal carotid arteries and to protect them from injury
- Once the majority of the tumor has been removed, the capsule/arachnoid will often descend into the operative field/sella. This is inspected and any residual pockets of tumor identified and gently removed
- It is important to realize if the tumor is soft, it may rapidly be removed, and the capsule may come into view very early in the procedure – so the operator must be aware of this to prevent an arachnoid tear and an unnecessary cerebrospinal fluid (CSF) leak
- Obtain hemostasis by gentle irrigation
- If the tumor has been completely removed, then bleeding is generally minimal
- More time may be required to ensure hemostasis when there is residual tumor
- Inspect the surgical field for a CSF leak
- The anesthetist can provide positive end-expiratory pressure (PEEP) to assist the descent of suprasellar adenoma and to ensure there is no CSF leak
- If a CSF leak is identified, then a repair needs to be done
- We generally do not reconstruct the defect in the floor of the sella, but usually fill the sphenoid sinus with fat or Surgiflo
8. Closure of surgical corridor
- The ENT surgeon now resumes control of the surgery to repair and reconstruct nasal structures as required
- If no CSF leak has occurred during the surgery, the Hadad flap is laid back over the septal defect. A suture is placed anteriorly to anchor the flap where the anterior incision was made and to secure it to the nasal septum, similar to septoplasty surgery. A suture can also be placed through the middle turbinate and septum to secure the flap
- Nasal plugging is not used, but a simple dressing is applied to the external nose
9. Postoperative care
- Postoperative antibiotics are not routinely given
- Patients are transferred to the neurosurgical intensive care unit for observation, specifically to monitor for a CSF leak, level of consciousness (GCS), signs of visual compromise and inappropriate antidiuretic hormone secretion (SIADH)
- Patients usually stay in ICU for 3-5 days post-surgery to monitor for SIADH. SIADH is the most important reason for postoperative monitoring in ICU. Electrolytes and fluid must be replaced if SIADH occurs
- Topical Oxymetazoline and a saline nasal spray are commenced on Day 1 following surgery for a period of 5 days
- If a postoperative CSF leak is noticed
- Immediate repair is required using fat harvested from the abdomen
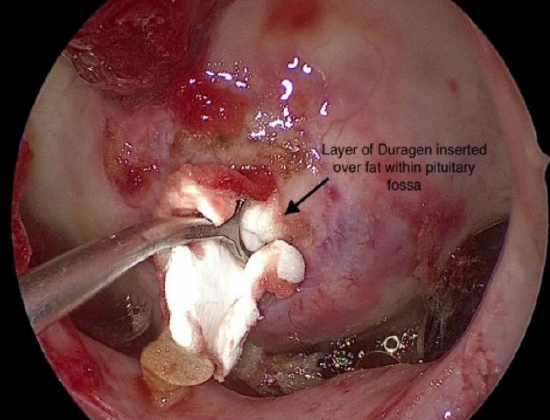
- Figure 19: Repair of a CSF leak
- This can be followed by a layer of fascia lata or Duragen (Figure 19)
- A Hadad flap is used if needed
- Lumbar drains are not routinely used
- Patients are followed up at a combined pituitary clinic where the neurosurgeon, endocrinologist and oncologist make decisions regarding need for hormone replacement, radiotherapy and long term follow-up
- Patients see an endocrinologist regularly to discuss hormone replacement therapy
- A follow-up MRI is done at 3 months
- It is usually not necessary for ENT follow-up if the surgical corridor has been closed. However, if turbinectomies or a posterior septectomy has been performed, regular debridement will be necessary. This can be avoided by careful creation and closure of the surgical corridor (Video taking down adhesions)
Authors
Moses Penduka MBChB, FCORL
University of Cape Town Karl Storz Rhinology Fellow
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
mfpenduka@yahoo.co.uk
Patrick Semple MMed, FCS (Neurosurg), PhD
Professor
Division of Neurosurgery
University of Cape Town
Cape Town, South Africa
patrick.semple@uct.ac.za
Darlene Lubbe MBChB, FCORL
Associate Professor
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
doclubbe@gmail.com
Editor
Johan Fagan MBChB, FCS (ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


