4.3: External Ethmoidectomy and Frontal Sinusotomy/Trephine
- Page ID
- 15449
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
EXTERNAL ETHMOIDECTOMY & FRONTAL SINUSOTOMY/TREPHINE
Johan Fagan, Neil Sutherland, Eric Holbrook
External approaches to the frontal, ethmoid and maxillary sinuses are seldom used nowadays other than in centers in the developing world where endoscopic sinus surgery expertise and instrumentation are not available; CT scans are also often not available in such centers to permit endoscopic sinus surgery to be properly planned and safely executed.
Some indications for open approaches
- Drainage of an orbital abscess
- Ethmoid artery ligation for epistaxis
- External ethmoidectomy
- Sinus pathology when endoscopic surgery expertise and instrumentation not available
- Biopsy of tumors
- Transethmoidal sphenoidotomy
- External frontal sinusotomy/trephination
- Complicated acute frontal sinusitis
- Pott’s puffy tumor
- Lateral frontal sinus mucocele
- Repair of frontal sinus CSF leak
- Biopsy of tumors
- Removal of osteomata
- Frontal sinus obliteration
The classic external frontoethmoidectomy operation entailed removing the lamina papyracea, opening and stripping the mucosa from the ethmoid sinuses up to cribriform plate, nibbling away the lateral wall of the frontonasal duct and floor of the frontal sinus, and stripping the mucosa from the frontal sinus.
This classic external frontoethmoidectomy operation is however contrary to modern principles of endoscopic sinus surgery which include:
- Limiting surgery to diseased sinuses
- Sparing mucosa
- Avoiding surgery to the frontal recess and frontonasal duct
- Preserving the middle turbinate
- Limiting resection of lamina papyricea to avoid medial prolapse of orbital soft tissues
This chapter focuses on the relevant surgical anatomy and techniques of external ethmoid and frontal sinus surgery, and incorporates principles borrowed from our current understanding of sinus anatomy, pathophysiology, and endoscopic sinus surgical techniques.
Anatomy of ethmoid & frontal sinuses
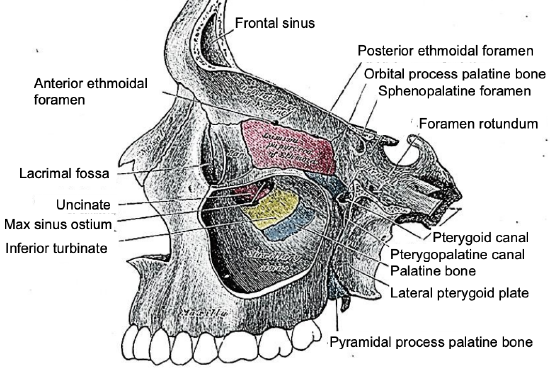
Figure 1: Lateral view of maxilla with windows cut in lateral and medial walls of left maxillary sinus
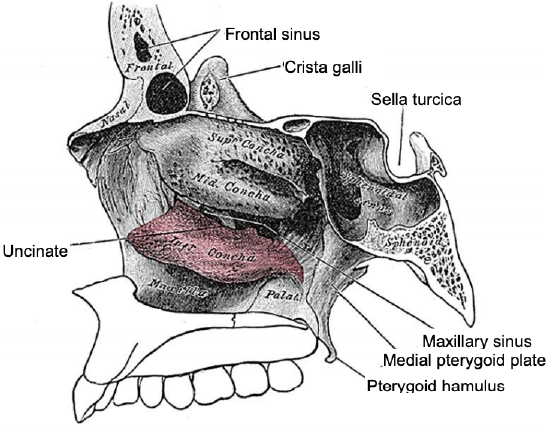
Figure 2: Bony anatomy of the lateral wall of the right nose
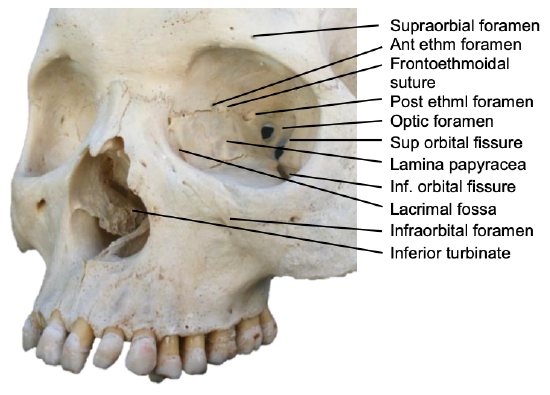
Figure 3: Bony anatomy in cadaver
Figures 1-3 illustrate the detailed bony anatomy relevant to external ethmoidectomy. Figure 2 illustrates the bony anatomy of the lateral wall of the nose.
Figure 3 demonstrates the anatomy of the medial wall of the orbit in a cadaveric skull; note in particular the thin lamina papyracea, the lacrimal fossa, the frontoethmoidal suture line and the anterior and posterior ethmoidal foramina and the infraorbital foramen.
Key bony surgical landmarks include:
- The floor of the anterior cranial fossa (cribriform plate) corresponds with the frontoethmoidal suture line
- The anterior and posterior ethmoidal foramina are located along the frontoethmoidal suture line
- The proximity (5-11 mm) of the posterior ethmoidal foramen and artery to the optic nerve in the optic foramen
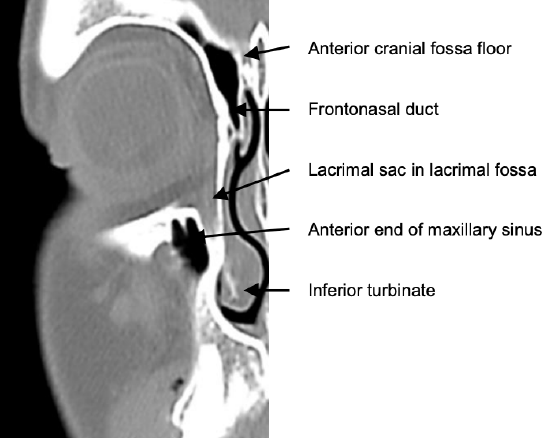
Figure 4: Coronal CT slice through lacrimal fossa and frontonasal duct
Figure 4 demonstrates the coronal anatomy at the level of the anterior limit of an external ethmoidectomy. Specifically note the lacrimal sac in the lacrimal fossa, which is preserved at surgery, and the relative heights of the floors of the antrum and the nasal cavity.
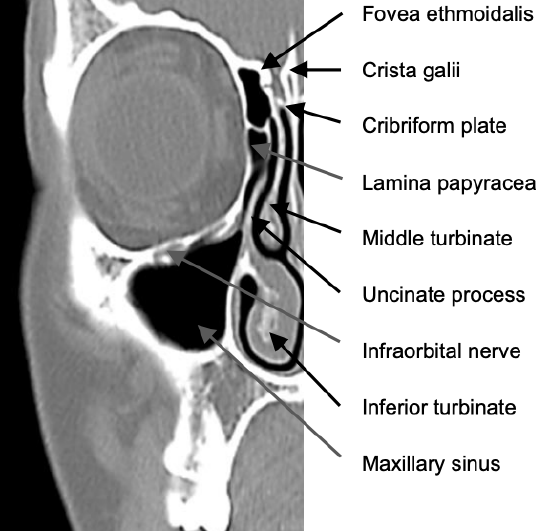
Figure 5: Coronal CT slice anterior to ethmoidal bulla
Figure 5 demonstrates the coronal anatomy anterior to the ethmoidal bulla. Specifically note the uncinate process, the vertical middle turbinate that attaches to the paperthin cribriform plate, and the thin lamina papyracea.
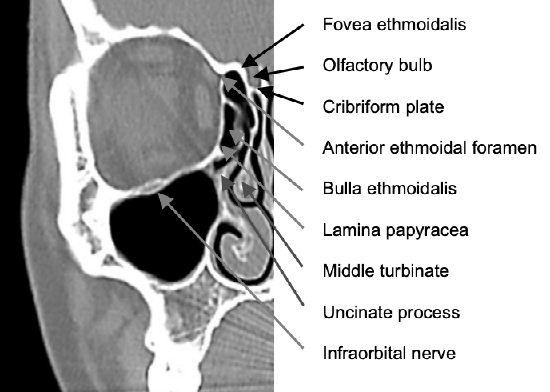
Figure 6: Note the position of the anterior ethmoidal artery where it passes through its foramen which is located in the frontoethmoidal suture line, and the anterior ethmoidal cells and it relationship to the middle turbinate and lamina papyracea
Figure 6 demonstrates the coronal anatomy through the ethmoidal bulla. It also illustrates the value of using the anterior ethmoidal artery and frontoethmoidal suture line to gauge the level of the floor of the anterior cranial fossa when opening the lamina papyracea from the orbital side e.g. for sepsis or tumor resection. Note the following relating to the anterior ethmoid sinus: the lamina papyracea constitutes its lateral wall; how small it is in the adult patient (24 mm high, 11 mm wide and 23 mm in length); and its relationships to the middle turbinate and uncinate process.
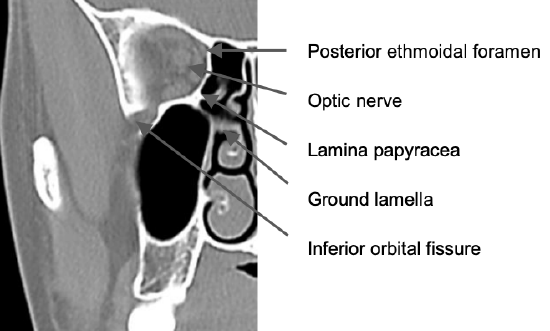
Figure 7: Coronal slice through posterior ethmoids demonstrating posterior ethmoidal foramen and optic nerve
Figure 7 is a coronal cut through the posterior ethmoids. Note the horizontally orientated ground lamella that divides the anterior from the posterior ethmoid sinuses, and how it attaches to the middle turbinate. It also illustrates the value of using the posterior ethmoidal artery and frontoethmoidal suture line to determine the level of the floor of the anterior cranial fossa when opening the lamina papyracea from the orbital side.
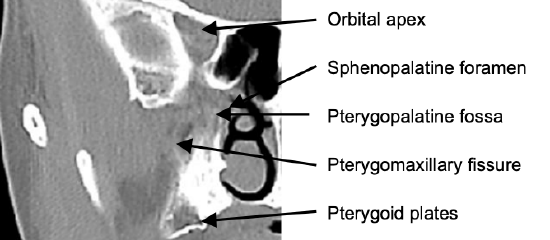
Figure 8: Coronal cut immediately behind maxillary sinus through the orbital apex, pterygoid plates and pterygopalatine fossa
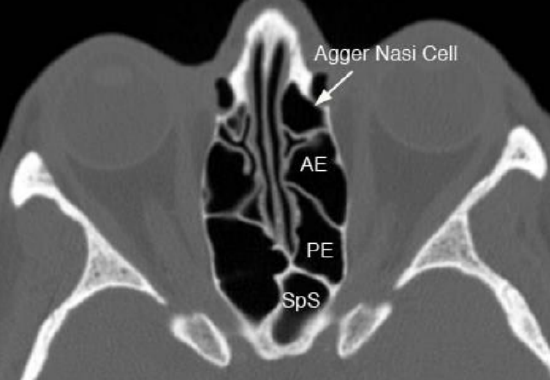
Figure 9: Axial view
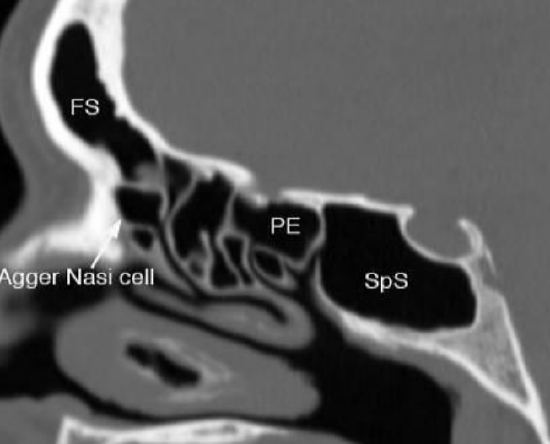
Figure 10: Sagittal view: Note relationship of frontal sinus to agger nasi and bulla
Figure 8 demonstrates the coronal anatomy immediately posterior to the maxillary sinus in which the internal maxillary artery and its branches as well as the sphenopalatine ganglion and its branches are encountered within the pterygopalatine fossa. The pterygopalatine fossa communicates laterally with the infratemporal fossa via the pterygomaxillary fissure; and medially with the nasal cavity via the sphenopalatine foramen. Figures 9 & 10 show axial and sagittal views of the sinus anatomy.
Vasculature
The paranasal sinuses are supplied by both the internal and external carotid artery systems.
Branches of the internal carotid artery of surgical significance include:
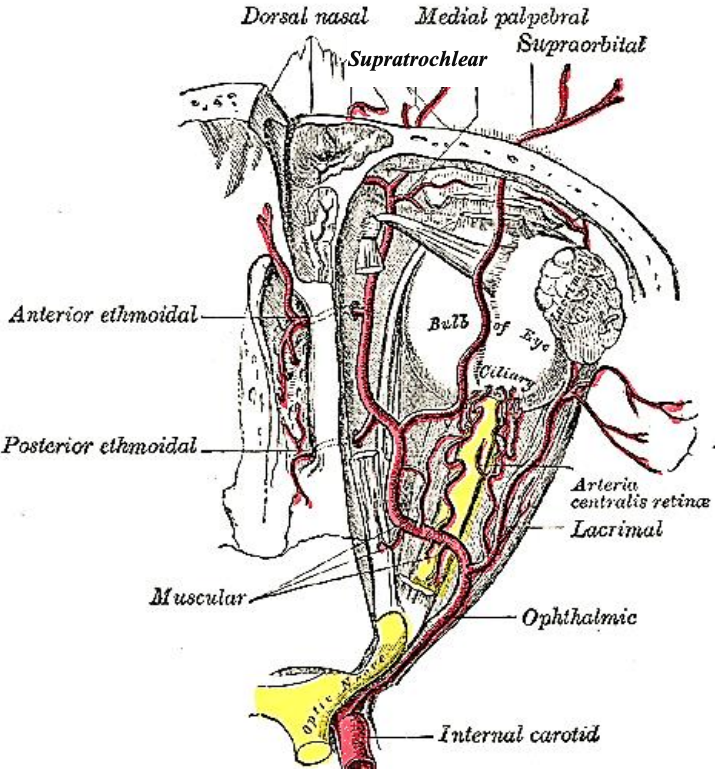
Figure 11: Ophthalmic artery gives rise to anterior and posterior ethmoidal arteries and the supratrochlear and supraorbital arteries
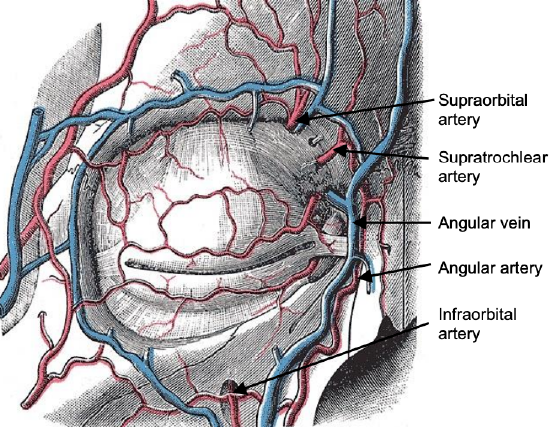
Figure 12: Vasculature around the orbit
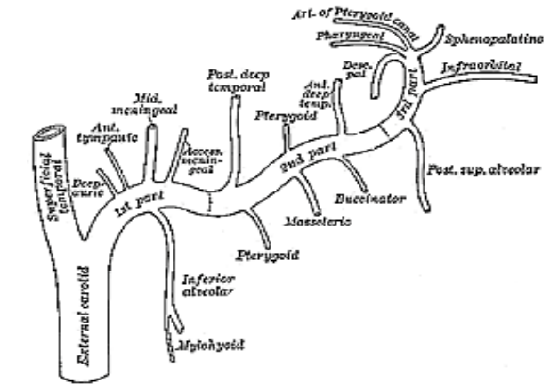
Figure 13: Branches of internal maxillary artery
- Ophthalmic artery (Figures 3, 11): It emerges with the optic nerve from the optic canal, 44 mm from the anterior lacrimal crest and approximately 6 mm (5-11 mm) from the posterior ethmoidal foramen
- Posterior ethmoidal artery (Figures 1, 3, 7, 11): It originates from the ophthalmic artery and enters the orbit through the posterior ethmoidal foramen which is located approximately 36 mm from the anterior lacrimal crest, and 12 mm (8-19 mm) from the anterior ethmoidal foramen. The vessel then courses through the posterior ethmoids near the anterior face of the sphenoid sinus close to the skull base to supply the posterior ethmoidal cells, the posterosuperior nasal septum, and parts of the superior and middle turbinates
- Anterior ethmoidal artery (Figures 1, 3, 6, 11): It originates from the ophthalmic artery and enters the orbit through the anterior ethmoidal foramen which is located 25 mm from the anterior lacrimal crest. It then courses across the fovea ethmoidalis before branching and supplying the cribriform plate and anterior and superior parts of the nasal septum. Although the vessel usually is flush with the skull base, it may be suspended in a mesentery; this places it at risk of injury during surgery
- Supraorbital artery (Figure 11, 12, 13): It originates from the ophthalmic artery and passes along the medial borders of the superior rectus and levator palpebrae superioris muscles, and then joins the supraorbital nerve between the roof of the orbit and levator palpebrae superioris; it exits the orbit via the supraorbital notch/foramen to supply levator palpebrae superioris, the frontal bone, frontal sinus, upper eyelid, and the skin of the forehead and scalp. It is absent in up to 20% of patients
- Supratrochlear artery (Figures 11, 12): It leaves the ophthalmic artery just behind the trochlea. It exits the orbit superomedially with the supratrochlear nerve, ascends on the forehead and supplies skin, muscle, and pericranium, anastomosing with the supraorbital artery and with the contralateral supratrochlear artery
Branches of the external carotid artery of surgical significance include:
- Internal maxillary artery: A branch of the external carotid artery (Figure 13), it passes through the pterygomaxillary fissure to enter the pterygopalatine fossa
- Sphenopalatine artery (Figure 13): This is the terminal end of the internal maxillary artery and enters the nasal cavity through sphenopalatine foramen at the back of the superior meatus where it gives origin to posterior lateral nasal branches. It supplies the posterior nasal cavity, as well as the maxillary, ethmoid, and sphenoid sinuses
- Posterior septal artery: This is a branch of the sphenopalatine artery and crosses the posterior nasal cavity just above the posterior choana to terminate on the nasal septum; one branch descends in a groove in the vomer to enter the incisive canal and to anastomose with the greater palatine artery
- Facial/external maxillary artery: A branch of the external carotid artery, it courses in the soft tissues of the face and past the medial canthus as the angular artery (Figure 12)
Veins of surgical significance: The only vein encountered during external frontoethmoidectomy is the angular vein which is situated medial to the medial canthus of the eye (Figure 12).
Nerves of surgical significance
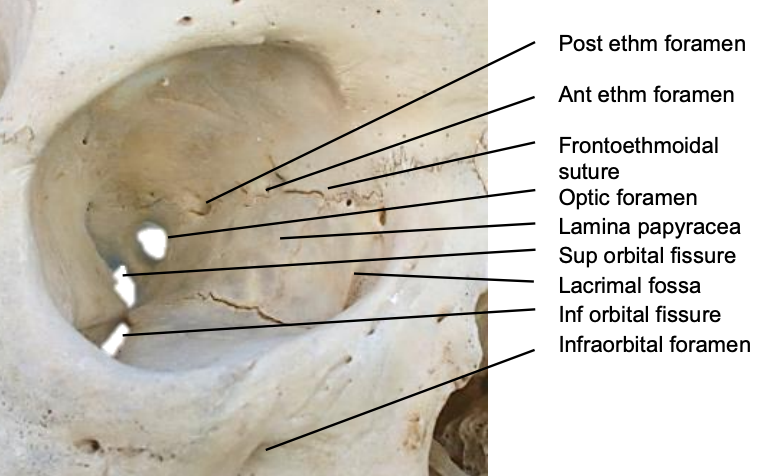
Figure 14: Right medial orbital wall
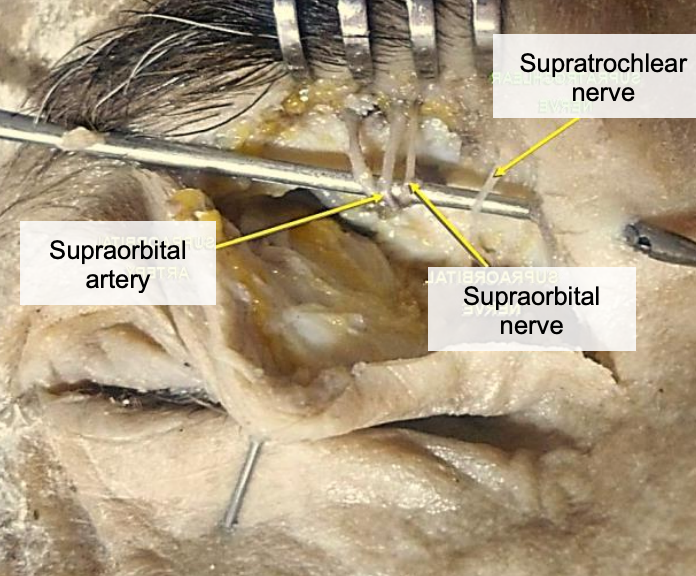
Figure 15: Supraorbital and supratrochlear nerves (Right eye)
- Optic nerve: The optic nerve enters the orbit via the optic foramen, 5-11 mm posterior to the posterior ethmoidal foramen (Figure 14)
- Supraorbital nerve (Figure 15): This is a terminal branch of the ophthalmic division (V1) of the trigeminal nerve. If it is injured where it passes through the supraorbital foramen or notch, the patient has sensory loss of the skin of the forehead extending to the vertex
- Supratrochlear nerve (Figure 15): This is also a terminal branch of the ophthalmic division (V1) of the trigeminal nerve. It exits the orbit between the pulley of the superior oblique muscle and the supraorbital foramen/notch and ascends onto the forehead to provide sensory innervation to the skin of the lower part of the forehead close to the midline, conjunctiva and upper eyelid
Orbital structures of surgical significance
Figure 14 shows the detailed bony anatomy of the orbit. During dissection medially along the orbital wall, the following structures are encountered: medial palpebral ligament, orbital septum, lacrimal sac, periosteum, and anterior and posterior ethmoidal arteries
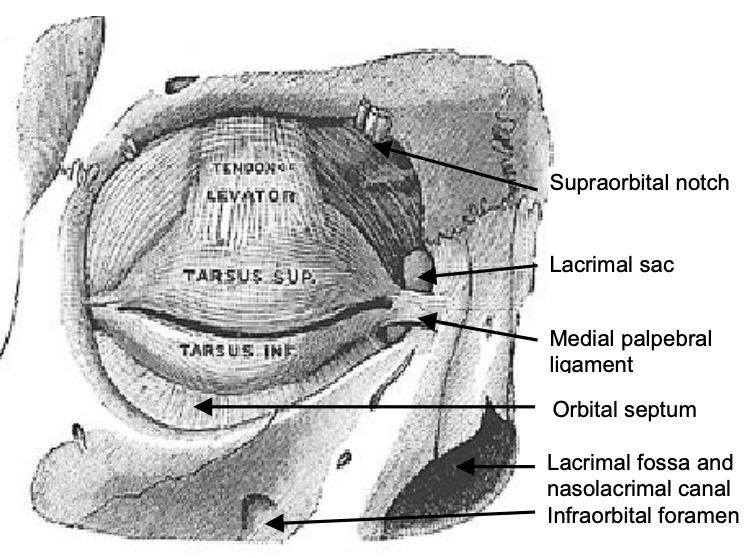
Figure 16: Right orbit: medial palpebral ligament, orbital septum, lacrimal sac and lacrimal fossa
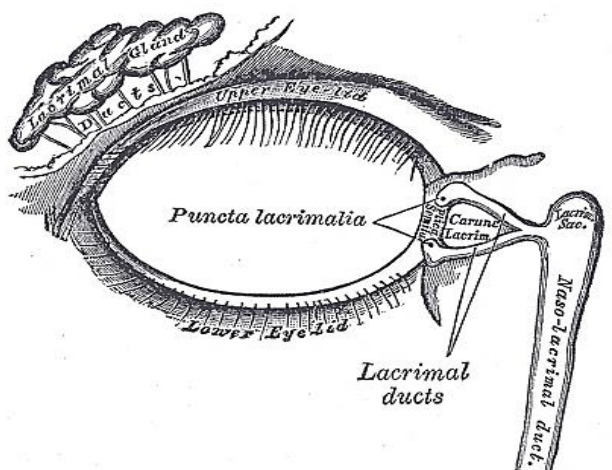
Figure 17: Right lacrimal system
- Orbital septum (Figure 16): This connective tissue structure attaches peripherally to the periosteum of the orbital margin and acts as a diaphragm that retains the orbital contents. Late-rally, it is attached to the orbital margin 1.5 mm anterior to the attachment of the lateral palpebral ligament to the lateral orbital tubercle. The septum continues along the superior orbital rim. Superomedially it crosses the supraorbital groove, passes inferomedially anterior to the trochlea, and follows the posterior lacrimal crest behind the lacrimal sac.
It then crosses the lacrimal sac to reach the anterior lacrimal crest, passes inferiorly along the anterior lacrimal crest and then laterally along the inferior orbital rim
- Medial palpebral ligament (medial canthal tendon) (Figure 16): This is a fibrous band that fixes the tarsi to the medial orbital wall. It is intimately related to the lacrimal drainage system. It lies anterior to the canaliculi, but a deep head inserts into the posterior lacrimal crest and onto the fascia of the lacrimal sac
- Lacrimal sac (Figures 14, 16, 17): It is located in the lacrimal fossa, which is bound medially by the lacrimal bone and the frontal process of the maxilla. It is related anteriorly, laterally, and posteriorly to the medial palpebral ligament
External ethmoidectomy
As was mentioned in the introductory paragraphs, the classic external frontoethmoidectomy operation entailed removing lamina papyracea, opening and stripping the mucosa from the ethmoid sinuses up to the cribriform plate, nibbling away the lateral wall of the frontonasal duct and floor of the frontal sinus, stripping the mucosa from the frontal sinus, and attempting to preserve the middle turbinate.
However, the classic external frontoethmoidectomy operation is contrary to the modern principles of endoscopic sinus surgery which include:
- Limiting surgery to extent of disease
- Sparing mucosa
- Avoiding unnecessary surgery to the frontal recess and frontonasal duct
- Preserving middle turbinate
- Limiting resection of lamina papyricea to avoid medial prolapse of orbit soft tissues
Principles that should be applied to modern day external (fronto)ethmoidectomy include:
- Obtain CT imaging (if possible) to assess the extent of disease, and as a roadmap for surgery, especially to evaluate the anatomy of the skull base
- Make as small a defect as is possible in the lamina papyracea to avoid medial prolapse of orbital soft tissues
- Do a minimum surgical drainage procedure of the ethmoids and limit it to the extent of disease
- Spare mucosa
- Preserve the middle turbinate to avoid adhesions to the nasal septum affecting olfaction, and to keep it as a surgical landmark
- Handle the middle turbinate extremely gently to avoid fracturing the cribriform plate and causing a CSF leak
- If concern exists about frontal sinus drainage
- Avoid surgery to the frontonasal duct if possible; rather do a frontal sinusotomy and irrigate the frontal sinus
- If one elects to open the frontonasal duct, avoid stripping mucosa circumferentially to avoid ductal stenosis; remove only a lateral strip of mucosa and handle the remaining mucosa atraumatically
Surgical steps
- Preoperative consent includes discussing the facial incision, injury to the optic, supraorbital and supratrochlear nerves, diplopia, epiphora, enophthalmos, telecanthus, and CSF leak
- The operation is done under general anesthesia, with orotracheal intubation
- Perioperative broad spectrum antibiotics are administered for 24 hours
- The nasal cavity is decongested with a topical vasoconstrictor
- The eyelids may be sutured together with 6/0 silk taking care not to invert the eyelashes to avoid corneal abrasions, or a protective contact lens is inserted
- Local anesthetic with vasoconstrictor is injected in the planned skin incision
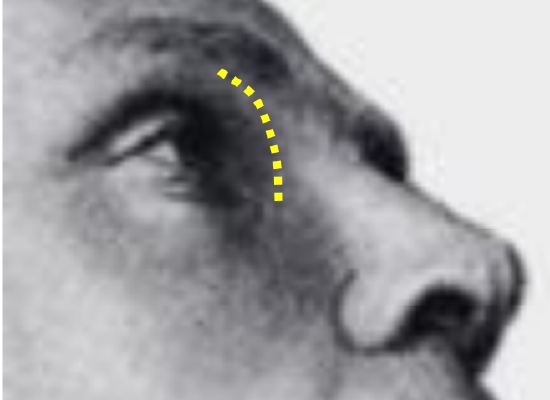
Figure 18: Lynch incision
- A 2.5-3 cm long curvilinear incision is made midway between the medial canthus and nasal dorsum taking care not to transect the supratrochlear and supraorbital nerves (Figure 18). A Z-plasty may be included to reduce the risk of bowstringing of the scar
- The remainder of the soft tissue dissection is done with electrocautery onto the nasal bone and frontal process of maxilla; the angular vessels are cauterized or ligated adjacent to the medial canthus of the eye (Figure 12)
- The incision is made through periosteum which is then elevated off lamina papyracea and floor of the frontal sinus
- Retract the orbital contents laterally taking care not to breach the periorbitum as fat then spills into the wound
- Sequentially identify the attachment of the medial palpebral ligament, anterior lacrimal crest, the lacrimal sac in the lacrimal fossa, and the posterior lacrimal crest. Displace the lacrimal sac laterally from the fossa but take care to limit dissection inferiorly to avoid avulsion of the medial ligament
- Identify the frontoethmoidal suture line; this is a crucial surgical landmark as it corresponds with the level of the cribriform plate and the anterior and posterior ethmoidal foramina
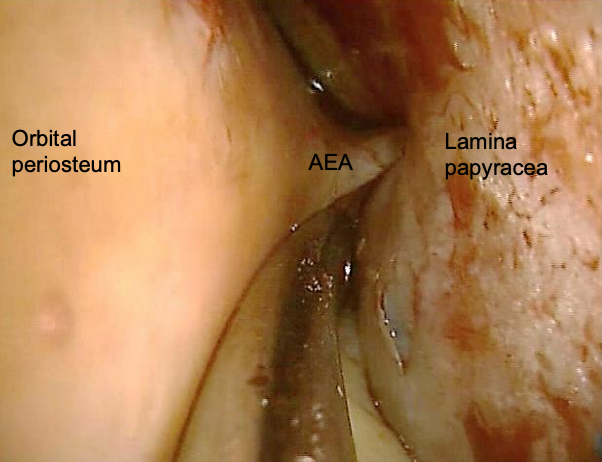
Figure 19: Anterior ethmoidal artery (AEA) exiting foramen at level of frontoethmoidal suture line (right eye)
- Identify the anterior ethmoidal artery as it bridges the divide between the anterior ethmoidal foramen and the periorbita (Figure 19)
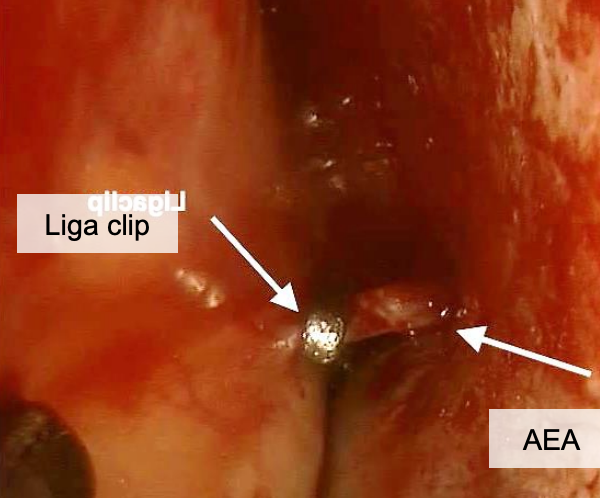
Figure 20: Liga clips being applied to anterior ethmoidal artery (AEA)
- Ligate/clip/bipolar the anterior ethmoidal artery, and divide it to reduce bleeding during ethmoidectomy (Figure 20); Blood flow courses from the direction of the orbit to the nasal cavity, so division of the artery should be medial to the clip if only one clip is placed
- This provides access to the posterior ethmoidal artery; it is generally not necessary to divide this vessel, and stopping short of the posterior ethmoidal artery safeguards the optic nerve
- Proceed to external ethmoidectomy
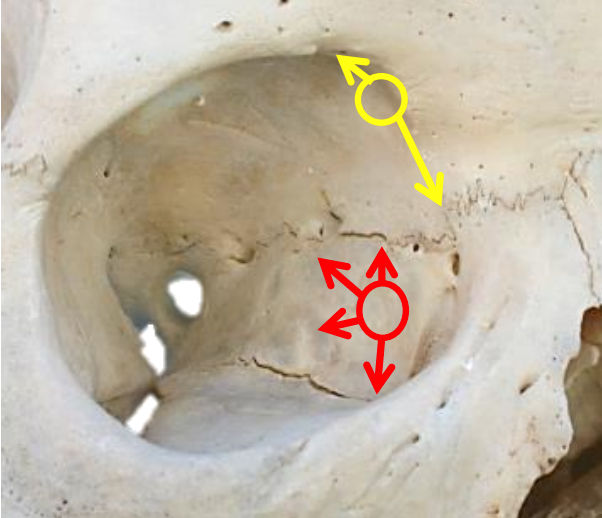
Figure 21: Ethmoidotomy (red) and frontal trephine (yellow) with subsequent directions of dissection
- Use a hammer and gouge to perforate the thin lamina papyracea immediately behind the posterior lacrimal crest, keeping well below the frontoethmoidal suture; this ethmoidotomy provides direct access to the anterior ethmoids (Figure 21)
- An alternative approach is to do a frontoethmoidectomy, initially entering the frontal sinus and using a Kerrison rongeur to carefully remove only the lateral wall of the frontonasal duct, sparing the remaining mucosa of the duct to avoid ductal stenosis (Figure 21). The bulla ethmoidalis is immediately posterior, and the agger nasi cells immediately anterior, to the termination of the frontonasal duct (Figures 9, 10)
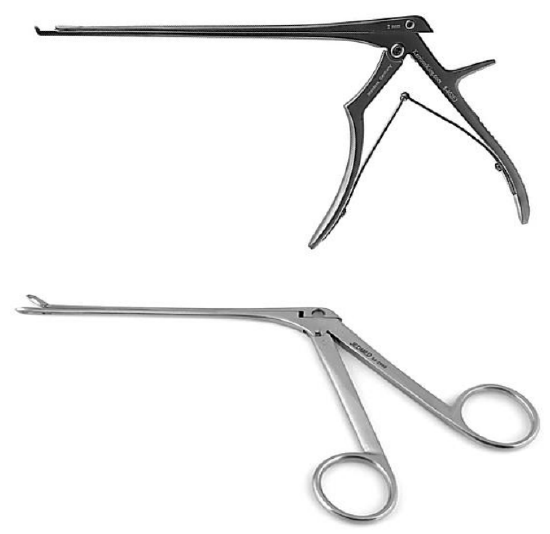
Figure 22: Kerrison’s rongeur (top) and Blakesley forceps
- Use a Kerrison’s rongeur or Blakesley forceps to enlarge the ethmoidotomy, keeping the defect as small as possible to prevent herniation of orbital soft tissue to a minimum (Figure 22)
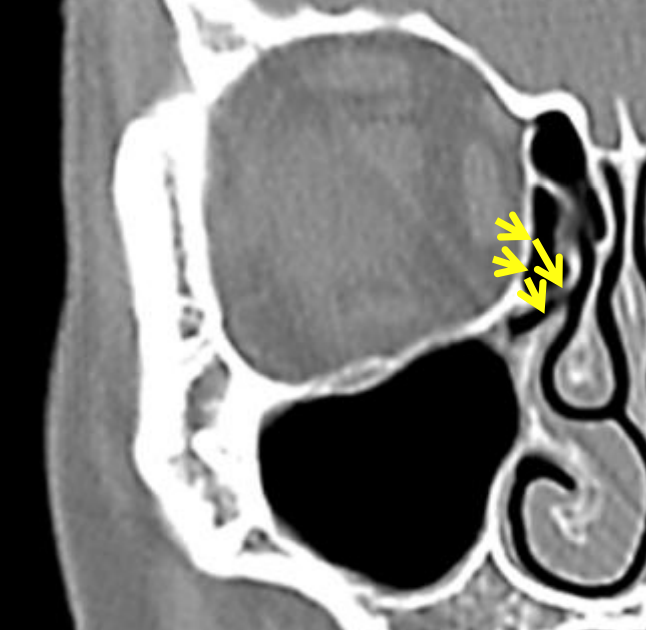
Figure 23: Direction of dissection of anterior ethmoidectomy
- Before proceeding with the ethmoidectomy, recall how small the anterior (24 mm high, 11 mm wide, 23 mm long) and posterior (21 mm high, 12 mm wide and 21 mm in length) ethmoids are (Figure 23)
- Remove the floor of the ethmoidal bulla by directing the Blakesley forceps anteroinferiorly (Figure 23)
- Keep middle turbinate intact taking care not to move it and fracture the cribriform plate
- To open the posterior ethmoids, direct the Blakesley forceps posteriorly (Figures 9, 10)
- An external ethmoidectomy may safely be completed up to the cribriform plate if necessary
- To do a sphenoidotomy, continue even further posteromedially keeping below the level of the frontoethmoidal suture (Figures 9, 10)
- Avoid disturbing the frontonasal duct
Key points: External frontoethmoidectomy
- Apply principles learned from endoscopic sinus surgery to open approaches
- Be aware of the positions of the supratrochlear and supraorbital nerves when making a Lynch incision
- Detailed knowledge of 3-dimensional anatomy of the paranasal sinuses, anterior skull base and orbit is essential
- Carefully follow the surgical steps in a well controlled surgical field in order to sequentially identify anatomical structures
- Know the anatomic landmarks of the cribriform plate
- The point at which the vertical lamella of the middle turbinate attaches to the lateral aspect of the cribriform plate and lateral lamella of the olfactory fossa may fracture with manipulation of the middle turbinate causing a CSF leak
- The lateral attachment of the posterior part of the middle turbinate to the lamina papyracea is called the ground lamella; it has a downward sloping orientation as one moves posteriorly
- The height of the fovea ethmoidalis and its attachment to the lateral lamella of the olfactory fossa is variable
- The anatomy of the anterior ethmoidal artery is variable; it may be suspended in a mesentery below the skull base
- The anatomical relations of the frontonasal duct are: agger nasi cells (anteriorly); bulla ethmoidalis (posteriorly); nasal septum (medially); and lamina papyracea (laterally) (Figures 9, 10)
- Prevent cicatrical scarring of the frontonasal duct by avoiding circumferential mucosal trauma
- Be aware of the location of the sphenopalatine artery where it emerges on the lateral nasal wall just behind the crista ethmoidalis; bleeding can be controlled with liga clips or bipolar cautery
External frontal sinusotomy/trephine
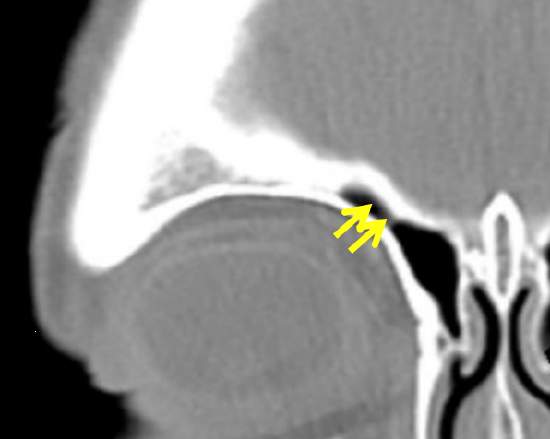
Figure 24: Frontal sinusotomy

Figure 25: Position of external frontal sinusotomy/trephine
- Examine the sinus x-rays and/or CT scan to determine the extent of pneumatization of the frontal sinuses (Figure 24)
- Make a Lynch incision if the surgery is combined with an external ethmoidectomy, or a 1 cm incision just below/ within the medial eyebrow
- Avoid injury to the supraorbital and supratrochlear nerves
- The thinnest bone is in the medial floor of the sinus: open the frontal sinus medially in the orbital roof with a burr, chisel or currette (Figure 25)
Closure
- Hemostasis is achieved with topical hemostatic agents; it is only rarely necessary to pack the nose
- Avoid cautery near the cribriform plate as perforate the paper-thin bone and cause a CSF leak
- Suture any tears in the periorbita to avoid herniation of orbital fat
- The skin is carefully repaired to optimize the cosmetic results
- Patients are instructed about regular nasal douching with saltwater, and are recalled for nasal toilette
Frontal sinus mini-trephination
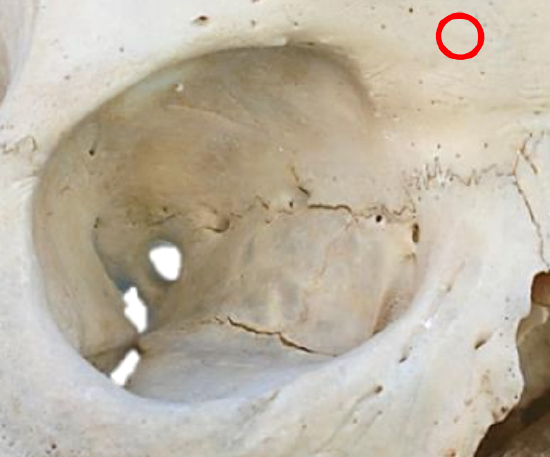
Figure 26: Position of frontal sinus mini-trephination
This technique is used to delineate the position of the frontonasal duct during endoscopic sinus surgery, or to irrigate an infected frontal sinus. Unlike formal frontal sinus trephine, the sinusotomy is placed above the orbital rim (Figure 26). It is therefore critical that it first be radiologically confirmed that the frontal sinus extends high enough above the orbital rim to permit this approach to avoid intracranial penetration by the drill
- Mark the position of the mini-trephine 1 cm from midline at the level of the medial end of the eyebrows
- Infiltrate skin and subcutaneous tissue with local anesthetic & adrenaline
- Make a stab incision in a skin crease (vertical or transverse) with a scalpel onto bone
- Spread the soft tissues with sharp ended scissors down to bone
- While distracting the skin edges, insert the drill guide firmly against the bone
- Pass the drill through the guide and drill the hole through the anterior table into the sinus
- While keeping the guide firmly in place, immediately remove the drill and irrigate the guide to avoid burning the skin and soft tissues
- Feed the wire stilette through the guide into the sinus
- Pass the cannula over the stilette through the mini-trephine into the sinus
Author & Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za
Authors
Neil Sutherland MBChB, FCORL
Otolaryngologist
Cape Town, South Africa
nsquared@ctonline.co.za
Eric H Holbrook MD
Co-Director of Sinus Center
Massachusetts Eye and Ear Infirmary
Boston, MA, USA
Eric_Holbrook@meei.harvard.edu


