4.12: Rhinoplasty surgery of the osseocartilaginous vault
- Page ID
- 49748
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
RHINOPLASTY: SURGERY OF THE OSSEOCARTILAGINOUS VAULT
GJ Nolst Trenité
Looking at the sequence of operative steps, most rhinoplastic surgeons prefer to perform surgery of the osseocartilaginous vault after tip surgery. One of the main reasons for this is that, by applying an external nasal dressing immediately after osteotomy, edema and ecchymosis can be prevented or at least diminished. Another reason is that, in order to obtain an aesthetic balance, in certain cases it is easier to adapt the form of the osseocartilaginous vault to the form of the tip, rather than vice versa.
In this chapter, surgery of the osseocartilaginous vault is divided into five sections:
- Hump resection
- Osteotomies
- Management of special bony pyramid problems
- Radix nasi surgery
- Cartilaginous vault surgery
Hump resection
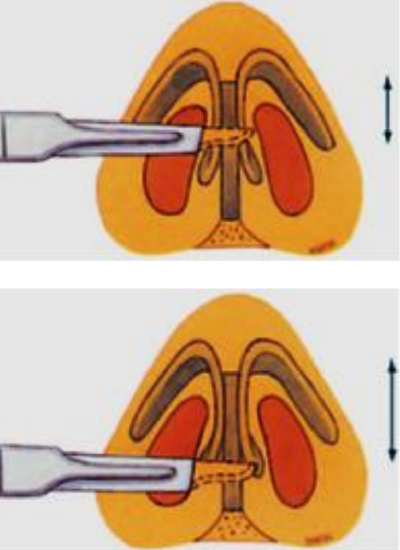
Figure 1a: partial transfixion incision; b: complete transfixion incision
The nasal hump consists of a cartilaginous and a bony part. In most cases, the bony part of the hump is much smaller than the cartilaginous part. With the endonasal approach, intercartilaginous incisions are connected by a transfixion incision to obtain ample access to the hump. It is important to dissect carefully between the upper and lower lateral cartilage in order to prevent postoperative irregularities of the lateral nasal wall. The intercartilaginous incision from lateral to medial, just caudal of the nasal valve, must be carried around the anterior septal angle. The two intercartilaginous incisions will then be connected by a partial transfixion incision, unless there is a specific indication for a complete transfixion incision. With a complete transfixion incision an important support of the tip in its connection between the medial crura and the anterior edge of the nasal septum will be disturbed (Figures 1a,b).
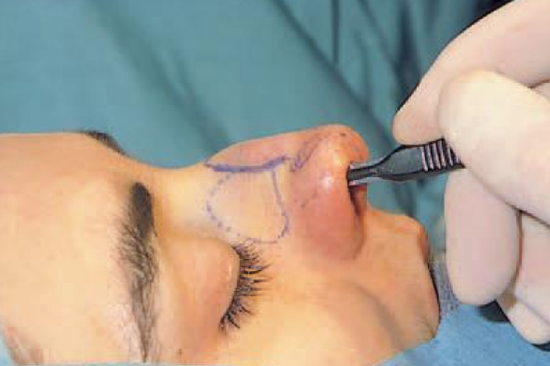
Figure 2: Sharp dissection in the surgical plane (close to the perichondrium) to free the cartilaginous dorsum from the overlying soft tissue
The next step is to free the cartilaginous part of the hump from the overlying soft tissues. With careful and sharp dissection (No. 15 blade) in the supraperichondrial surgical plane, damage to the musculus transversus nasi, together with unnecessary scarring and bleeding, will be prevented (Figure 2).
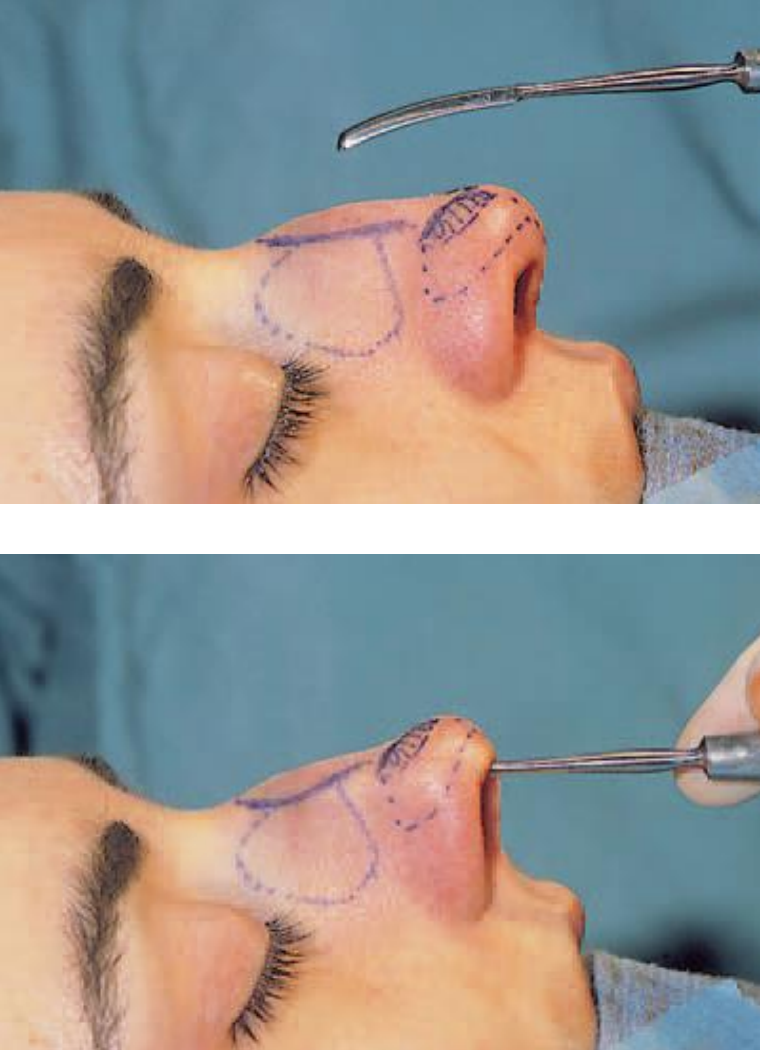
Figures 3a,b: Elevation of the periosteum of the nasal bone (only of the hump area) with a Joseph elevator
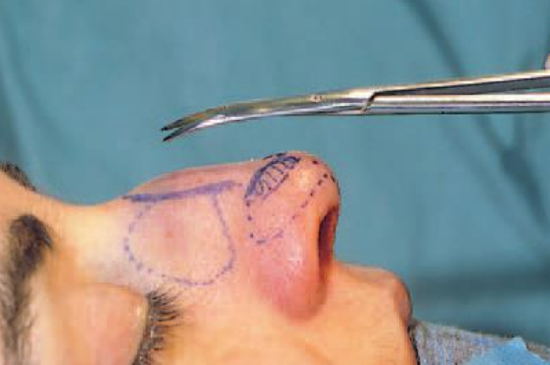
Figure 4: Dissection of the periosteum attached to the sutura intranasalis
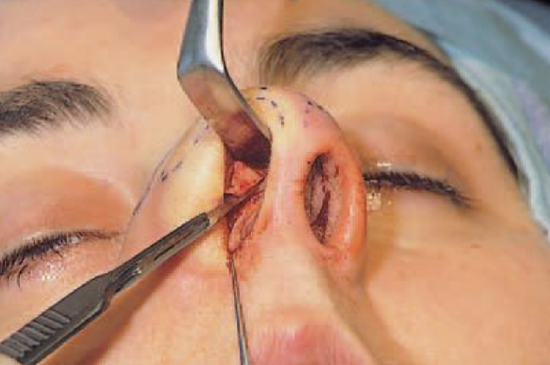
Figure 5: Incising the cartilaginous vault under direct vision at the ‘planned’ resection line
After freeing the cartilaginous vault from the overlying soft tissues, the periosteum is incised at the caudal end of the nasal bone and elevated with a Joseph elevator (Figures 3a,b). There is no need to elevate the periosteum very far laterally. The procedure should be limited to the area of the hump to be resected. Periosteum attached to the sutura intranasalis can simply be cut from the bony vault with a long pair of scissors (Figure 4). With an ‘Aufricht’ retractor in place, the cartilaginous vault can now be incised by a through-and-through incision (No. 15 blade) from cephalic to caudal at the ‘planned’ resection line (Figure 5).
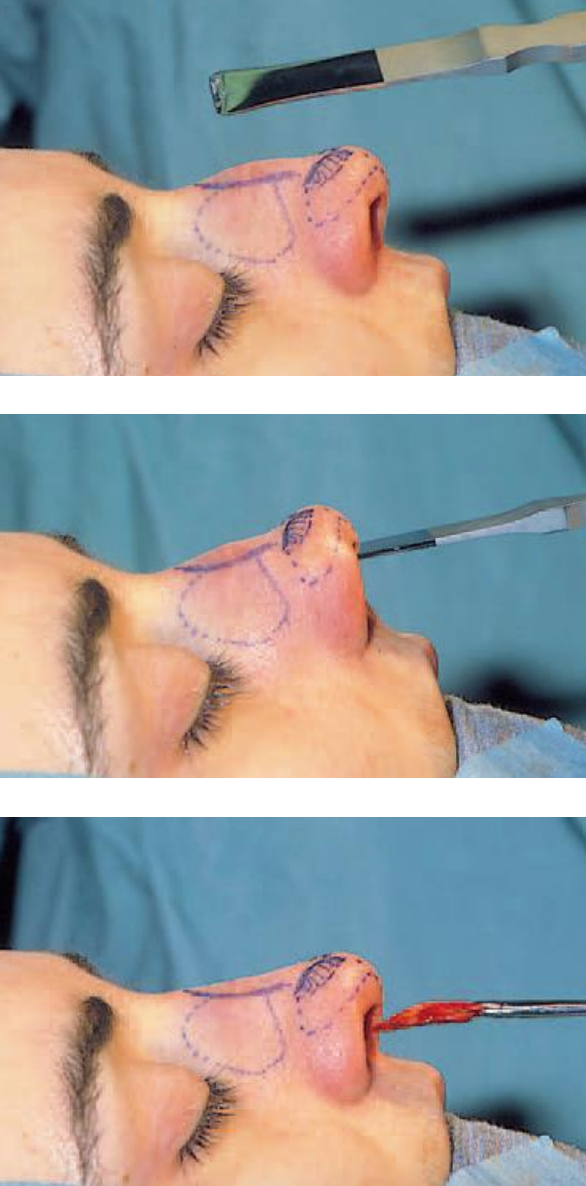
Figures 6a,b,c: Resection of the osseocartilaginous hump with a 14 mm hump osteotome
Using this cartilaginous cutting face as a guideline, the hump osteotome is introduced to loosen the bony part at the hump, followed by the removal of the osseocartilaginous hump ‘en bloc’ (Figures 6a,b,c).
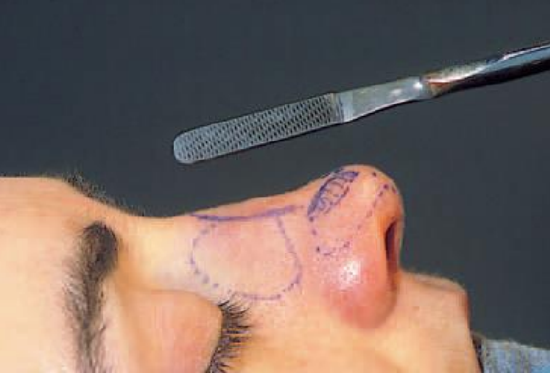
Figure 7: Smoothing of the bony surface after hump resection with a medium-fine (tungsten-carbide) rasp
A (medium-fine) tungsten-carbide or diamond rasp is now used to smoothen the bony surface (Figure 7) and, if necessary, some extra shaving of the cartilaginous dorsum is carried out to obtain the desired supratip-tip relation.
In case of a small hump, it is easier to start shaving off small pieces of the cartilaginous hump to the desired level and then to use a down-cutting rasp to lower the bony dorsum.
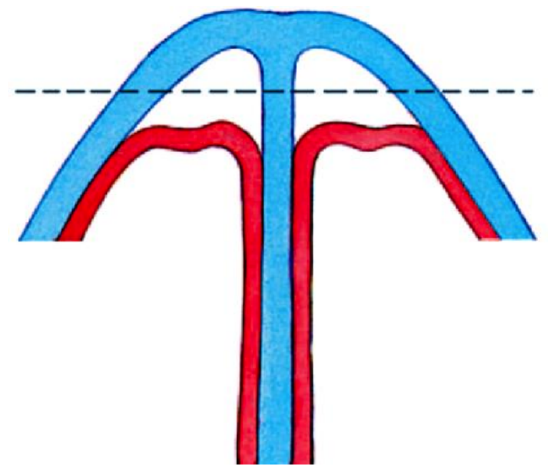
Figure 8: Stripping of the mucoperichondrium at first on the posterior side of the cartilaginous vault in case of a large hump
When a small bony hump is removed with a rasp, it is certainly less important to elevate the periosteum, the more so as this kind of bony hump resection guarantees a smooth contour of the bony pyramid. When removing the cartilaginous part of a very large hump, stripping off the mucoperichondrium at first on the posterior side of the cartilaginous vault (extramucosal technique), will prevent postoperative irregularities of the dorsum due to damage to the mucoperichondrium (Figure 8).
There are various additional important points to consider in hump resection:
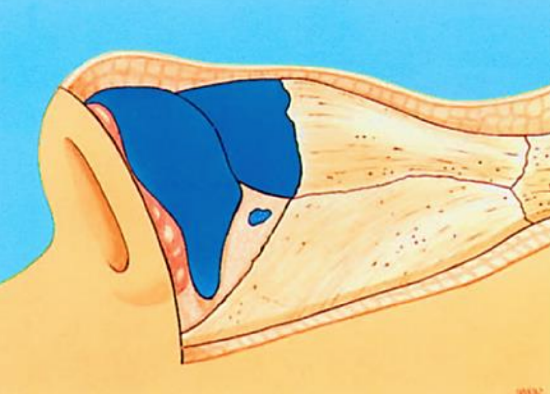
Figure 9: Illustration of the difference in thickness of the soft tissue lying over the osseocartilaginous vault
- Pay attention to the difference in thickness of the overlying soft tissue, which is at its thinnest at the rhinion (the caudal point of the ossa nasalia) (Figure 9)
- Check whether the nose dorsum shows any small irregularities after hump resection, which should be meticulously smoothed over
- Check whether enough cartilage has been resected from the anterior edge of the upper lateral
- Remove all loose bone particles, especially after rasping
- Correct over-resection by replacing the excised hump after trimming to the appropriate size (Skoog’s method), or use an autogenous septal cartilage graft
A frequently occurring postoperative complication is the ‘polly beak’, which can be divided into:
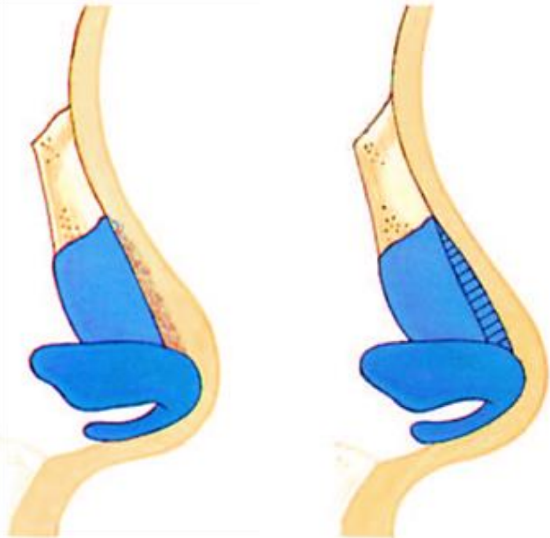
Figure 10a: Soft tissue ‘polly beak’; b: Cartilaginous ‘polly beak’
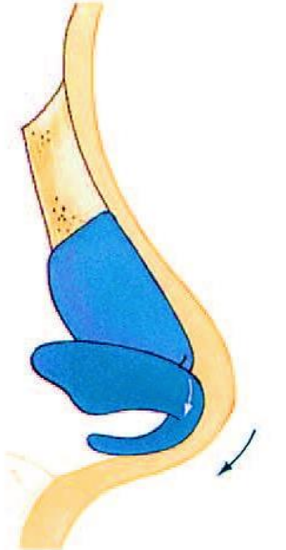
Figure 10c: Relative ‘polly beak’
- The soft-tissue ‘polly beak’ (Figure 10a). This arises when dissection in the surgical plane is not made carefully enough, resulting in scarring of the overlying soft tissues
- The cartilaginous ‘polly beak’ (Figure 10b). This is caused by too little resection of the cartilaginous part, or by a relatively excessive resection of the bony part of the hump
- The relative ‘polly beak’. This is the result of the tip drooping, due to tip surgery in which the tip support was insufficiently guaranteed (Figure 10c)
Osteotomies
Osteotomies are required to mobilize the bony pyramid for in-fracture, out-fracture or realignment. With traditional techniques and instruments, mobilization of the bony pyramids results in significant edema and ecchymosis.
The technical refinements of the last decade have produced a considerable reduction in ecchymosis and edema, resulting in quicker and better healing. The most important factors are:
- Precise placement of local vasoconstrictive and anesthetic solution
- Use of micro-osteotomes
- Preservation of periosteal attachment
- Medial-oblique osteotomy to eliminate transverse osteotomy
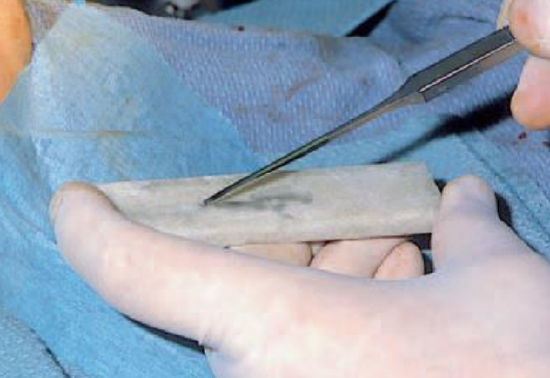
Figure 11: Sharpening of the microosteotome ‘durante operationem’
Well-placed local anesthesia at least 15 minutes prior to the surgery (on the bony pyramid) is very helpful in reducing bleeding. With the microosteotome if necessary sharpened during surgery (Figure 11), it is not necessary to elevate the periosteum. This gives less surgical trauma and leaves the periosteum intact to a large extent in which way it can act as an internal splint.
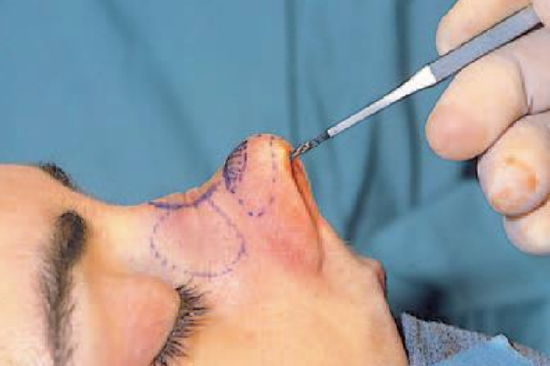
Figure 12: Medial-oblique osteotomy
When a medial-oblique osteotomy is combined with a slightly curved lateral osteotomy, there is no need for the traditional transverse osteotomy (Figure 12).
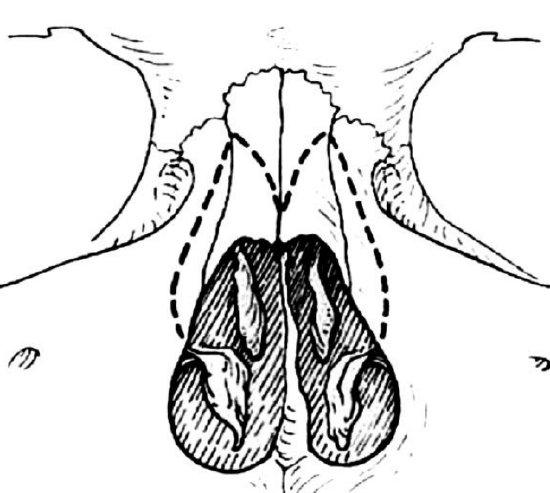
Figure 13: Osteotomy pathway (dotted line) of medial-oblique and lateral osteotomies
The crossover point of both osteotomies should not be (and aesthetically there is no need) more cephalic than the intercanthal line, thereby avoiding the thick bone of the radix nasi (Figure 13). It is important to leave the (external) periosteal and (internal) mucoperiosteal lining intact as far as possible.
Lateral osteotomies can be performed percutaneously as well as intranasally.
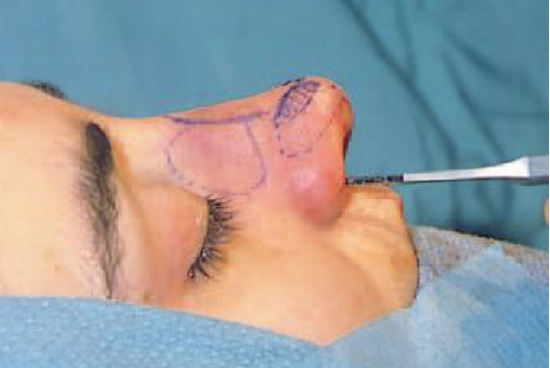
Figure 14: Low lateral osteotomy
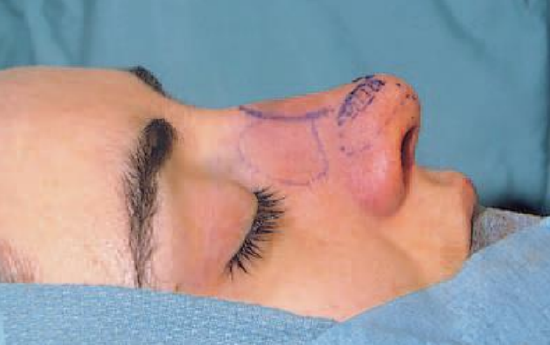
Figure 15: Dorsum of the nose after hump resection and micro-osteotomies
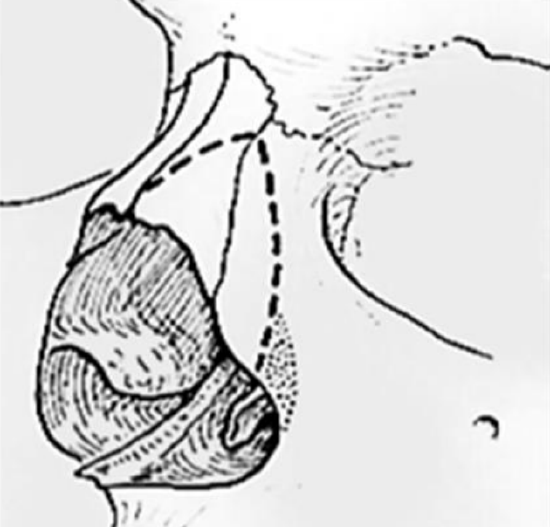
Figure 16: Bony ridge at base of lateral wall of piriform aperture (dotted area) to be preserved in performing a low lateral osteotome followed by in-fracture of nasal bone
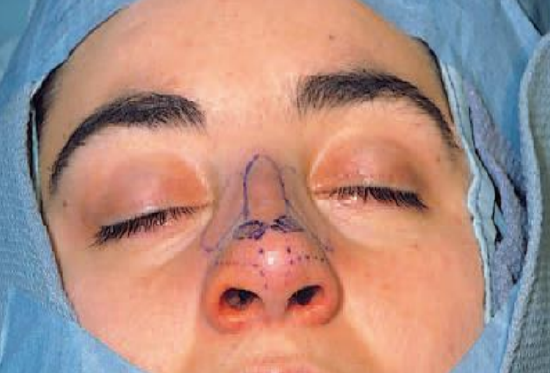
Figure 17: Readjusted bony vault after infracture of the nasal bones
The micro-osteotome is inserted through the soft tissue of the lateral wall of the piriform aperture, starting at the ascending process of the maxilla at the superior margin of the inferior turbinate. For a low lateral osteotomy, it should then proceed laterally, preserving a bony ridge at the base of the lateral wall of the piriform aperture (Figures 14-17). In this way, any possible narrowing of the airway by in-fracture of the os nasale can be prevented (Figure 17).
It should then proceed, slowly bending from lateral to medial, as far as the intercanthal line where the medial-oblique osteotomy is carried out. Readjustment of the osteotome after sliding off the bone, prevents unnecessary lesions of the periosteum. A 2 mm osteotome is often sufficient. When the bone is thicker than normal, a 3-mm osteotome is indicated.
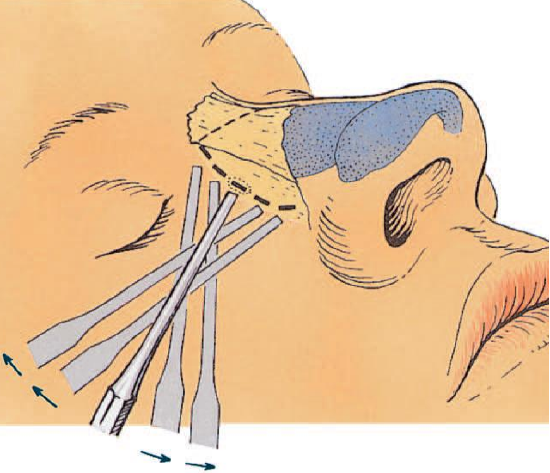
Figure 18a: Percutaneous lateral osteotomy making small point osteotomies along the planned osteotomy line
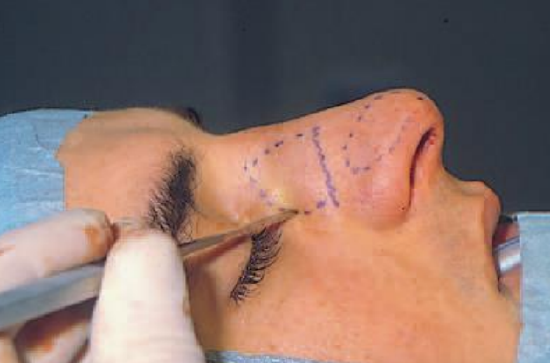
Figure 18b: Percutaneous lateral osteotomy through a skin incision halfway along the planned osteotomy line
In percutaneous lateral osteotomy, a skin incision of 23 mm is made halfway along the planned osteotomy line, after which small point-osteotomies are made cephaliccally and caudally along the osteotomy line (Figures 18a,b). Although the percutaneous technique is rather more traumatic than the intranasal one, it gives excellent control.
In order to prevent a hematoma, it is wise to put pressure paranasally on both sides at the level of the skin incision after the procedure for 3-5 minutes.
Additional intermediate osteotomies are indicated in an asymmetric bony pyramid.
If the traditional transverse osteotomy is indicated, this can either be done percutaneously via a small incision at the level of nasion or an incision in the eyebrow with a micro-osteotome, or intranasally via the lateral osteotomy line, with a special transversely curved osteotome.
Complications which can occur in osteotomies of the bony pyramid are the following:
- An osteotomy carried out insufficiently, after which the bony part springs back into its original position
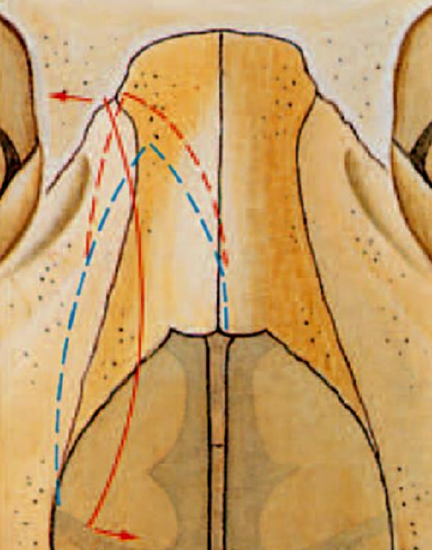
Figure 19: “Rocker phenomenon” due to too far cephalically performed osteotomies (red dotted lines)
- ‘Rocker phenomenon’ which can occur in osteotomies carried out too far cephalically. When the concave bony part, now curved medially, is repositioned on the caudal or cephalic side, the other part will project (Figure 19)
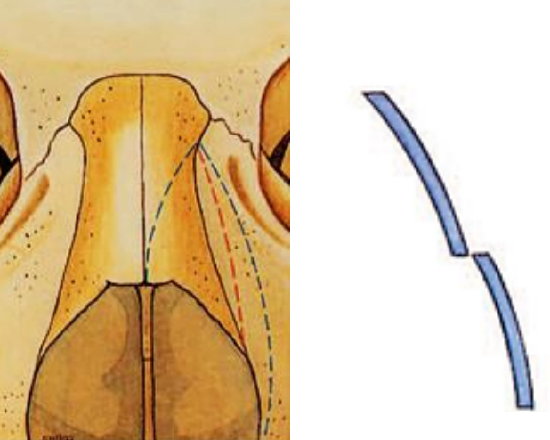
Figure 20: Staircase phenomenon due to a too medially-placed osteotomy (red dotted line)
- Lateral osteotomies carried out too far medially, in which a “staircase phenomenon” arises (Figure 20)
- Callosus (which often disappears spontaneously)
Management of special bony pyramid problems
Asymmetric bony pyramid due to lateral deviation
In a strong deviation of the nose, there may be a large difference between the size of the left and right os nasale, in which case exact repositioning in the midline after standard osteotomies is not possible.
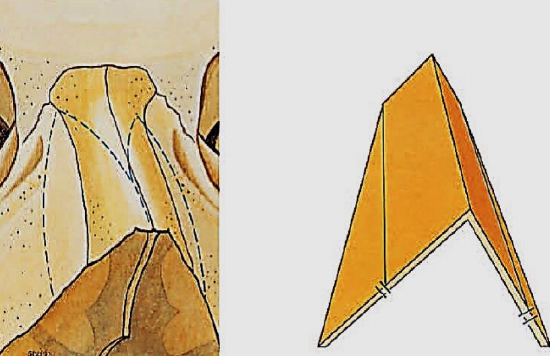
Figures 21: More medially placed lateral osteotomy (green dotted line) to correct moderate asymmetry of bony pyramid
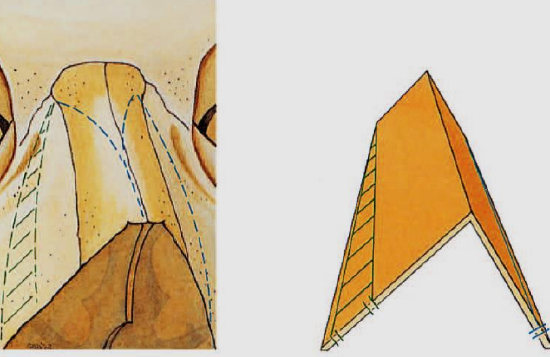
Figure 22: Resection of bony wedge (green striped area) in case of severe asymmetry of bony pyramid
If these asymmetries are not too large, a lateral osteotomy, placed more medially on the long side, is often sufficient (Figure 21). In a very seriously asymmetric bony pyramid, a wedge resection is indicated, whereby a bony wedge is removed on the lateral side of the longest side wall (Figure 22). When removing a bony wedge, the periosteum will have to be stripped off both sides of the wedge in order to be removed. To obtain adequate repositioning, the septum will also have to be mobilized and corrected, otherwise the chance of the deviation reappearing postoperatively is high.
Abnormally curved nasal bones
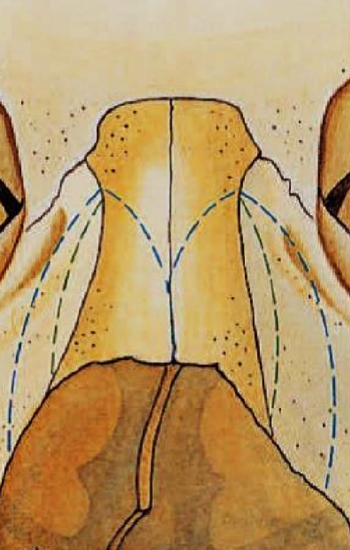
Figure 23: Supplementary intermediate osteotomies (green dotted lines) to remodel concave and convex bony side walls
In case of a concavity or convexity of a side wall, it is necessary to perform one or more intermediate osteotomies to remodel the bony pyramid (Figure 23).
Broad trapezoid bony pyramid
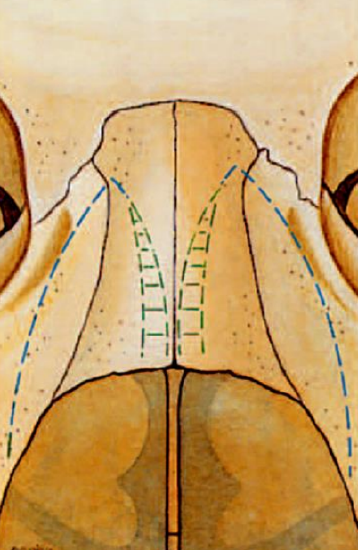
Figure 24: Resection of medial wedges (green striped areas) to correct a broad trapezoid bony pyramid
With this type of bony pyramid, in-fracture is not possible by medial-oblique and lateral osteotomies alone. Therefore a medial wedge resection is mandatory on both medial parts of the nasal bones (Figure 24).
Radix nasi surgery
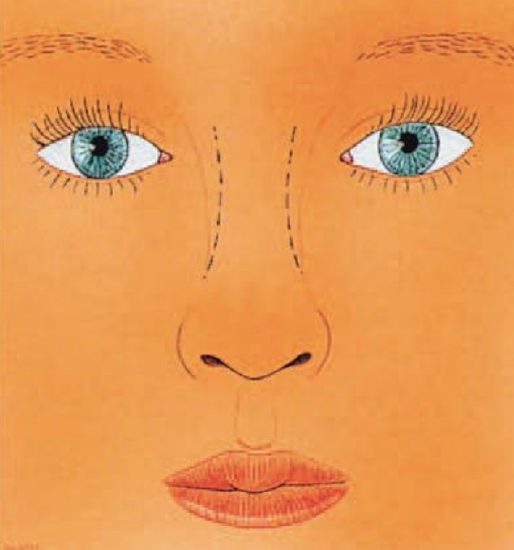
Figure 25: Proposed correction (dotted lines) of too wide a radix nasi
The role of the radix nasi is often underestimated in the aesthetic balance of the facial complex. In frontal view, the width of the radix nasi should be in good alignment with the natural curve from eyebrow to lateral nasal bone. Too wide radix nasi is very uncommon and can be corrected by infracture, after osteotomies have been placed more cephalically (above the intercanthal line) (Figure 25). In particular after rhinoplasty, when osteotomies have been placed too cephalically and after too much in-fracture of the bony pyramid, the radix nasi often becomes too narrow. This can be corrected with out-fracture after re-osteotomies. In profile, the radix nasi also plays a role in the aesthetic balance of the face and is characterized by the nasofrontal and nasofacial angles. A change in the horizontal or vertical position of the deepest depression of the root of the nose (nasion) has a direct effect on the apparent projection and length of the nose. A change in the position of the radix nasi, which is a relatively small surgical procedure, will have a great impact on the appearance of the nose. A dorsal onlay graft gives the nose a longer appearance and the (unchanged) nasal tip a shorter one. Deepening of the naso-facial groove using a chisel or glabella rasp has the opposite effect.
Cartilaginous vault surgery
Resection of the caudal border of the upper laterals
This is indicated as an additional procedure after a considerable shortening of the nose, due to which the caudal parts of the upper laterals protrude into the vestibulum.

Figure 26: The resected cartilaginous part of caudal border of the upper laterals and caudal septum in a nose shortening procedure should be approximately of equal length
Care should be taken not to over-shorten the upper lateral cartilages, as this may lead to unnatural narrowing of the middle third of the nose. Besides an unaesthetic appearance, over-resection of the upper lateral cartilages may result in functional problems due to inspiratory collapse of the weakened lateral nasal wall. When shortening the nose, it is a good rule not to resect more from the caudal end of the upper lateral than from the septum (Figure 26).
Other indications for caudal resection of the upper laterals are internal valve problems caused by pathological returning of the caudal end of the upper lateral, which interfere with normal internal valve functioning.
Narrowing the cartilaginous vault
In some cases, the cartilaginous vault is trapezoid in shape, due to the flat anterior part of the upper laterals. Resection of a small paraseptal strip of cartilage on both sides will narrow the cartilaginous vault. The technique used for adequate exposure of the cartilaginous dorsum in combination with extramucosal dissection is the same as the one used for resection of a large hump.
Widening the cartilaginous vault
Spreader grafts to widen the cartilaginous vault are indicated for aesthetic reasons when there is a very narrow mid-nose or because of functional problems caused by too sharp an angle (smaller than 10 degrees) of the internal valve. Small strips of autogenic septal cartilage are the first choice as graft material. Using the intranasal approach, they should be placed in an extramucosal pocket between the septum and the lateral cartilages. However, the external approach gives far better control.
Clinical examples of osseocartilaginous vault surgery
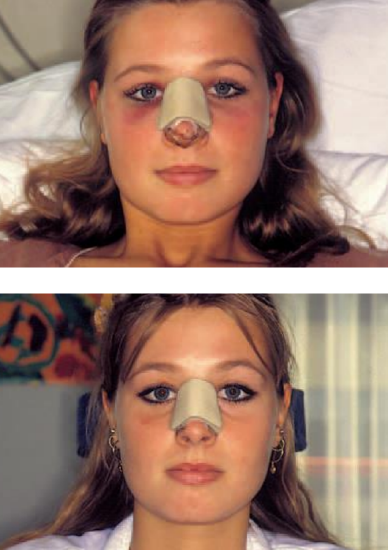
Figure 27: A patient who underwent a hump resection followed by medial oblique, (endonasal) lateral micro-osteotomies and in-fracture with moderate edema and ecchymosis two days postoperatively (top); and already resolving ecchymosis six days postoperatively (bottom) just before removal of the Denver splint
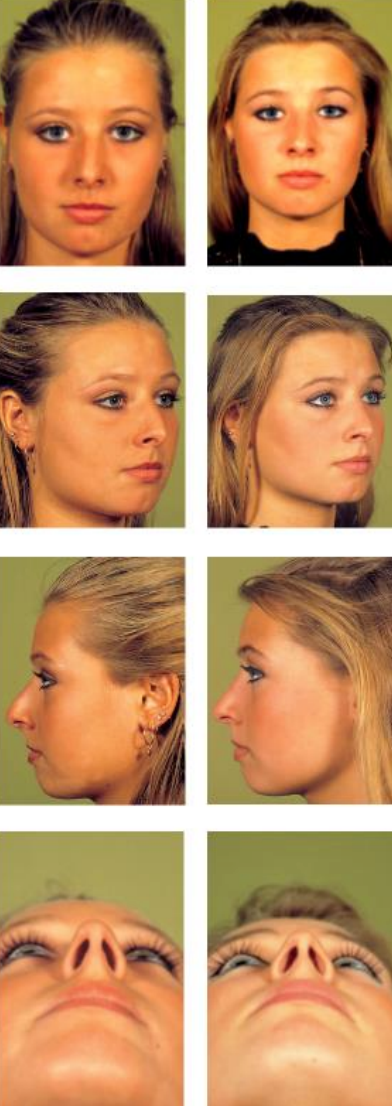
Figure 28: Pre- (L) and longterm (R) postoperative views after hump resection followed by predialoblique (endonasal) lateral view-osteotomies and in-fracture of the nasal bones
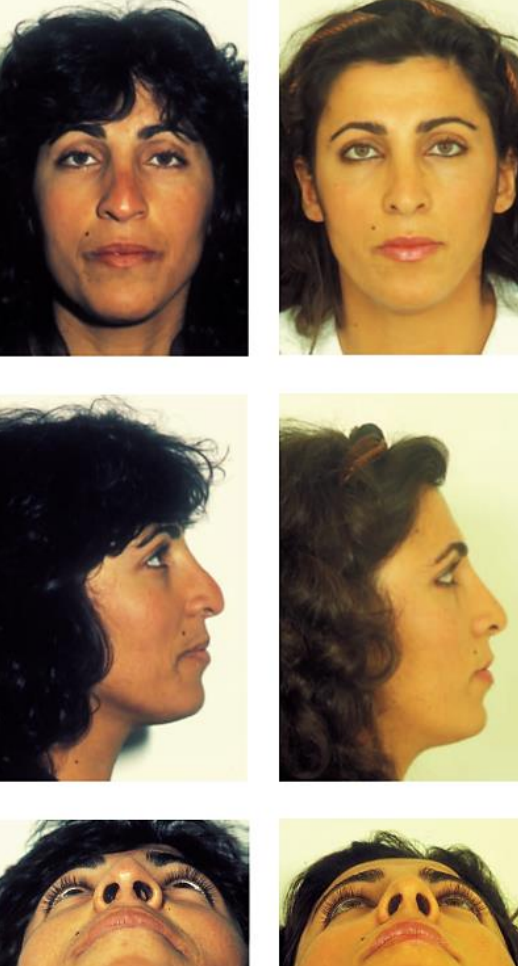
Figure 29: Pre- and postoperative views of a patient who underwent revision rhinoplasty to correct a cartilaginous polly beak
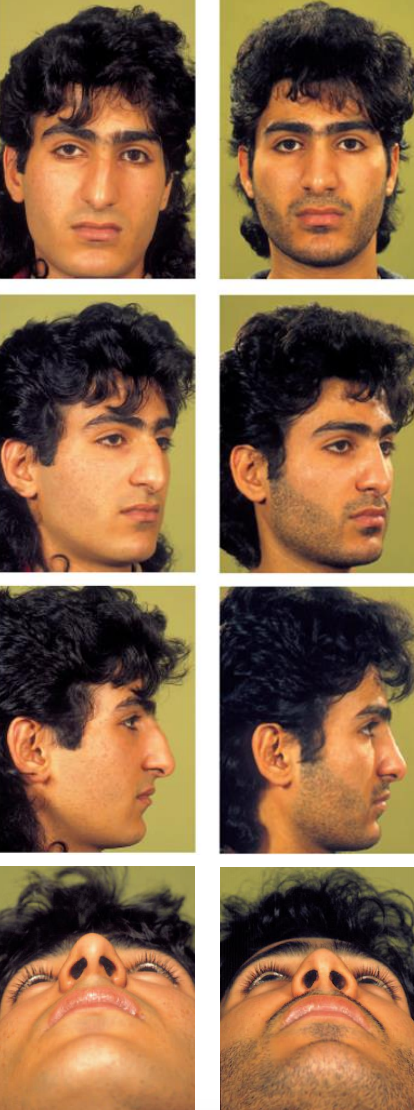
Figure 30: Pre- and postoperative views of a patient with a tension nose due to overdevelopment of the cartilaginous septum who underwent a rhinoplasty by the endonasal approach to reduce the osseocartilaginous vault and to correct a slight downward rotation of the tip with resection of a caudal strip of septal cartilage

Figure 31: Pre- and postoperative views of a ten-year-old girl who underwent endonasal septorhinoplasty due to posttraumatic septal deviation with nasal airway impairment and a gradually increasing deviation of the nasal dorsum. Realignment of the dorsum was performed with medial oblique and (endonasal) lateral osteotomies. When performing rhinoplasties in children, the surgeon should be aware that operating on a growing nose can interfere with midfacial growth. He/she has to weigh up the possible advantages (psychological and growth directional) against possible disadvantages (growth inhibition). From the experimental work of the Verwoerd group, we know that, in contrast to surgery of the cartilaginous vault, mobilization of the nasal bones does not lead to specific morphological anomalies in further growth
In Figures 27-31, pre- and postoperative views of patients are shown who underwent osseocartilaginous vault surgery.
The material in this chapter originates from the textbook “Rhinoplasty: A practical guide to functional and aesthetic surgery of the nose” G.J. Nolst Trenité (ed) https://www.rhinoplasty.nl/store/
Author
Gilbert Nolst Trenité MD, PhD
Professor of Otorhinolaryngology
Former President of European Academy of Plastic Surgery
Amsterdam, Netherlands
nolsttrenite@gmail.com
Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


