14.4C: Agonists, Antagonists, and Drugs
- Page ID
- 7737
Drugs effecting cholinergic neurotransmission may block, hinder, or mimic the action of acetylcholine and alter post-synaptic transmission.
- Distinguish between the effects of an agonist versus an antagonist in the autonomic nervous system
Key Points
- Acetylcholine receptor agonists and antagonists have either direct effects on the receptors or act indirectly by affecting the enzyme acetylcholinesterase.
- Agents targeting ACh receptors may target either the nicotinic or muscarinic receptors for ACh.
- Atropine, an antagonist for muscarinic ACh receptors, lowers the parasympathetic activity of muscles and glands in the parasympathetic nervous system.
- Neostigmine is an indirect ACh receptor agonist that inhibits acetylcholinesterase, preventing the breakdown of acetylcholine. It is used in the treatment of myasthenia gravis and to reverse the effects of neuromuscular blockers used for anesthesia.
- Phenylephrine, marketed as a substitute for Sudafed for decongestant purposes, is an α1- adrenergic receptor agonist.
- Beta-blockers, as their name suggests, block the action of epinephrine and norepinephrine on β-adrenergic receptors and are used for the management of cardiac arrhythmias, cardio-protection after a heart attack, and hypertension.
Key Terms
- acetylcholinesterase: An enzyme that catalyzes the breakdown of the neurotransmitter acetylcholine.
- beta-blockers: Also called beta-adrenergic blocking agents, beta-adrenergic antagonists, beta-adrenoreceptor antagonists, or beta antagonists, these are a class of drugs used for various indications. As beta-adrenergic receptor antagonists, they diminish the effects of epinephrine (adrenaline) and other stress hormones.
- atropine: An alkaloid extracted from the plant deadly nightshade (Atropa belladonna) and other sources. It is used as a drug in medicine for its paralytic effects (e.g., in surgery to relax muscles, in dentistry to dry the mouth, in ophthalmology to dilate the pupils), though overdoses are fatal.
Blocking, hindering, or mimicking the action of acetylcholine has many uses in medicine. Drugs that act on the acetylcholine system are either agonists to the receptors that stimulate the system, or antagonists that inhibit it.
Acetylcholine receptor agonists and antagonists can have a direct effect on the receptors or exert their effects indirectly. For example, by affecting the enzyme acetylcholinesterase the receptor ligand is degraded. Agonists increase the level of receptor activation, antagonists reduce it.
Acetylcholine in the ANS
The vagus (parasympathetic) nerves that innervate the heart release acetylcholine (ACh) as their primary neurotransmitter. ACh binds to muscarinic receptors (M2) that are found principally on cells comprising the sinoatrial (SA) and atrioventricular (AV) nodes.
Muscarinic receptors are coupled to the Gi-protein; therefore, vagal activation decreases cAMP. Gi-protein activation also leads to the activation of KACh channels that increase potassium efflux and hyperpolarizes the cells.
Increases in vagal activity to the SA node decreases the firing rate of the pacemaker cells by decreasing the slope of the pacemaker potential and decreasing heart rate. By hyperpolarizing the cells, vagal activation increases the cell’s threshold for firing, which contributes to the reduction the firing rate.
Similar electrophysiological effects also occur at the atrioventricular AV node. However, in this tissue, these changes are manifested as a reduction in impulse conduction velocity through the AV node. In the resting state, there is a large degree of vagal tone on the heart, which is responsible for low, resting heart rates.
There is also some vagal innervation of the atrial muscle, and to a much lesser extent, the ventricular muscle. Vagus activation, therefore, results in modest reductions in atrial contractility (inotropy) and even smaller decreases in ventricular contractility.
Muscarinic Antagonists
Atropine: The 2D chemical structure of atropine is illustrated here.
Muscarinic receptor antagonists bind to muscarinic receptors, thereby preventing ACh from binding to and activating the receptor. By blocking the actions of ACh, muscarinic receptor antagonists very effectively block the effects of vagal nerve activity on the heart. By doing so, they increase heart rate and conduction velocity.
Atropine is a naturally occurring tropane alkaloid extracted from deadly nightshade (Atropa belladonna), Jimson weed (Datura stramonium), mandrake (Mandragora officinarum), and other plants of the family Solanaceae. Atropine’s pharmacological effects are due to its ability to bind to muscarinic acetylcholine receptors. It is an anti-muscarinic agent.
Working as a nonselective muscarinic acetylcholinergic antagonist, atropine increases firing of the sinoatrial node (SA) and conduction through the atrioventricular node (AV) of the heart, opposes the actions of the vagus nerve, blocks acetylcholine receptor sites, and decreases bronchial secretions. In overdoses, atropine is poisonous.
Nicotinic Agonists
A nicotinic agonist is a drug that mimics, in one way or another, the action of acetylcholine (ACh) at nicotinic acetylcholine receptors (nAChRs). Nicotinic acetylcholine receptors are receptors found in the central nervous system, the peripheral nervous systems, and skeletal muscles.
They are ligand-gated ion channels with binding sites for acetylcholine as well as other agonists. When agonists bind to a receptor it stabilizes the open state of the ion channel allowing an influx of cations.
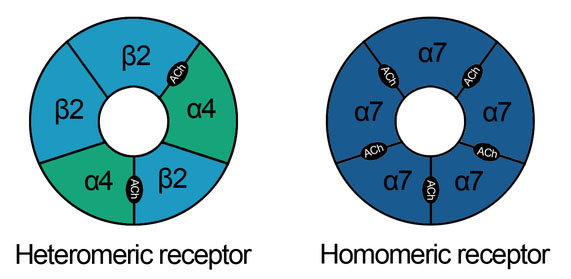
Nicotinic acetylcholine receptors: NAchR are cholinergic receptors that form ligand-gated ion channels in the plasma membranes of certain neurons and on the postsynaptic side of the neuromuscular junction.
The development of nicotinic acetylcholine receptor agonists began in the early nineties after the discovery of nicotine’s positive effects on animal memory. Nicotinic antagonists are mainly used for peripheral muscle paralysis in surgery, the classical agent of this type being tubocurarine, but some centrally acting compounds such as bupropion, mecamylamine, and 18-methoxycoronaridine block nicotinic acetylcholine receptors in the brain and have been proposed for treating drug addiction.
The nicotinic acetylcholine receptor agonists are gaining increasing attention as drug candidates for multiple central nervous system disorders such as Alzheimer’s disease, schizophrenia, attention-deficit hyperactivity disorder (ADHD), and nicotine addiction. In 2009 there were at least five drugs on the market that affect the nicotinic acetylcholine receptors.
Most indirect-acting ACh receptor agonists work by inhibiting the enzyme acetylcholinesterase. The resulting accumulation of acetylcholine causes a continuous stimulation of the muscles, glands, and central nervous system.
They are examples of enzyme inhibitors, and increase the action of acetylcholine by delaying degradation; some have been used as nerve agents (sarin and VX nerve gas) or pesticides (organophosphates and the carbamates). In clinical use, they are administered to reverse the action of muscle relaxants, to treat myasthenia gravis, and to treat symptoms of Alzheimer’s disease (rivastigmine increases cholinergic activity in the brain).
Beta Receptor Antagonists
Beta blockers (sometimes written as β-blockers) or beta-adrenergic blocking agents, beta-adrenergic antagonists, beta-adrenoreceptor antagonists, or beta antagonists, are a class of drugs used for various indications. They are particularly used for the management of cardiac arrhythmias, cardiac protection after myocardial infarction (heart attack), and hypertension.
As beta-adrenergic receptor antagonists, they diminish the effects of epinephrine (adrenaline) and other stress hormones. Beta blockers block the action of endogenous catecholamines —epinephrine (adrenaline) and norepinephrine (noradrenaline) in particular—on β-adrenergic receptors, part of the sympathetic nervous system that mediates the fight-or-flight response.
LICENSES AND ATTRIBUTIONS
CC LICENSED CONTENT, SHARED PREVIOUSLY
- Curation and Revision. Authored by: Boundless.com. Provided by: Boundless.com. License: CC BY-SA: Attribution-ShareAlike
CC LICENSED CONTENT, SPECIFIC ATTRIBUTION
- Acetylcholine receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Acetylcholine_receptor. License: CC BY-SA: Attribution-ShareAlike
- Acetylcholine. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Acetylcholine. License: CC BY-SA: Attribution-ShareAlike
- Cholinergic. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Cholinergic. License: CC BY-SA: Attribution-ShareAlike
- choline acetyltransferase. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/choline...tyltransferase. License: CC BY-SA: Attribution-ShareAlike
- nicotinic receptors. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/nicotinic%20receptors. License: CC BY-SA: Attribution-ShareAlike
- autonomic ganglia. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/autonomic%20ganglia. License: CC BY-SA: Attribution-ShareAlike
- Acetylcholine. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Acetylcholine. License: Public Domain: No Known Copyright
- Muscarinic acetylcholine receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Muscari...oline_receptor. License: Public Domain: No Known Copyright
- Drug Discovery and Development: Nicotinic Acetylcholine Receptor Agonists. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Drug_Di...eptor_Agonists. License: CC BY-SA: Attribution-ShareAlike
- Adrenergic receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Adrenergic_receptor. License: CC BY-SA: Attribution-ShareAlike
- G protein-coupled receptors. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/G%20pro...ed%20receptors. License: CC BY-SA: Attribution-ShareAlike
- adrenoreceptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/adrenoreceptor. License: CC BY-SA: Attribution-ShareAlike
- adrenergic receptor. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/adrenergic_receptor. License: CC BY-SA: Attribution-ShareAlike
- Acetylcholine. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Acetylcholine. License: Public Domain: No Known Copyright
- Muscarinic acetylcholine receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Muscari...oline_receptor. License: Public Domain: No Known Copyright
- Drug Discovery and Development: Nicotinic Acetylcholine Receptor Agonists. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Drug_Di...eptor_Agonists. License: CC BY-SA: Attribution-ShareAlike
- Adrenergic receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Adrenergic_receptor. License: Public Domain: No Known Copyright
- Adrenergic receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Adrenergic_receptor. License: Public Domain: No Known Copyright
- Adrenergic receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Adrenergic_receptor. License: CC BY-SA: Attribution-ShareAlike
- Drug Discovery and Development: Nicotinic Acetylcholine Receptor Agonists. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Drug_Di...eptor_Agonists. License: CC BY-SA: Attribution-ShareAlike
- Nicotinic antagonist. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Nicotinic_antagonist. License: CC BY-SA: Attribution-ShareAlike
- Phenylephrine. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Phenylephrine. License: CC BY-SA: Attribution-ShareAlike
- Acetylcholine. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Acetylcholine. License: CC BY-SA: Attribution-ShareAlike
- Beta blockers. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Beta_blockers. License: CC BY-SA: Attribution-ShareAlike
- Atropine. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Atropine. License: CC BY-SA: Attribution-ShareAlike
- acetylcholinesterase. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/acetylcholinesterase. License: CC BY-SA: Attribution-ShareAlike
- atropine. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/atropine. License: CC BY-SA: Attribution-ShareAlike
- beta-blockers. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/beta-blockers. License: CC BY-SA: Attribution-ShareAlike
- Acetylcholine. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Acetylcholine. License: Public Domain: No Known Copyright
- Muscarinic acetylcholine receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Muscari...oline_receptor. License: Public Domain: No Known Copyright
- Drug Discovery and Development: Nicotinic Acetylcholine Receptor Agonists. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Drug_Di...eptor_Agonists. License: CC BY-SA: Attribution-ShareAlike
- Adrenergic receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Adrenergic_receptor. License: Public Domain: No Known Copyright
- Adrenergic receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Adrenergic_receptor. License: Public Domain: No Known Copyright
- Adrenergic receptor. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Adrenergic_receptor. License: CC BY-SA: Attribution-ShareAlike
- Drug Discovery and Development: Nicotinic Acetylcholine Receptor Agonists. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Drug_Di...eptor_Agonists. License: CC BY-SA: Attribution-ShareAlike
- Atropine. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Atropine. License: Public Domain: No Known Copyright

