21.9D: Carbon Dioxide Transport
- Page ID
- 8000
- Describe the process of carbon dioxide transport
Carbon Dioxide Transport
Carbon dioxide is the product of cellular respiration, and is transported from the cells of tissues in the body to the alveoli of the lungs through the bloodstream. Carbon dioxide is carried in the blood through three different ways.
About 5% of carbon dioxide is transported in the plasma of the blood as dissolved CO2 molecules that aren’t bound to anything else. Carbon dioxide has a much higher solubility than oxygen, which explains why a relatively greater amount of carbon dioxide is dissolved in the plasma compared to oxygen. While oxygen binds to the iron content in the heme of hemoglobin, carbon dioxide can bind to the amino acid chains on hemoglobin. When carbon dioxide clings to hemoglobin it forms carbanimohemoglobin. About 10% of carbon dioxide in the human body is transported this way. Carbanimohemoglobin gives red blood cells a bluish color, which is one of the reasons why the veins that carry deoxygenated blood appear to be blue.
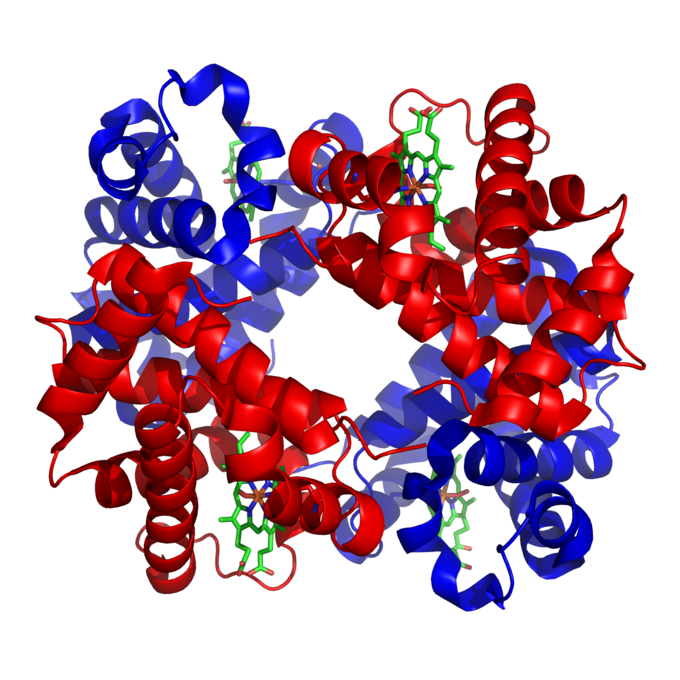
Structure of human hemoglobin: Hemoglobin is a tetramer of alpha (red) and beta (blue) subunits with iron containing heme groups (green).
A property of hemoglobin called the Haldane effect states that deoxygenated blood has an increased capacity to carry carbon dioxide, while oxygenated blood has a decreased capacity to carry carbon dioxide.
This property means that hemoglobin will primarily carry oxygen in systemic circulation until it unloads that oxygen and is able to carry a relatively higher amount of carbon dioxide. This is due to deoxygenated blood’s increased capacity to carry carbon dioxide, and from the carbon dioxide loaded from the tissues during tissue gas exchange.
Bicarbonate Ions
The majority (85%) of carbon dioxide travels in the blood stream as bicarbonate ions. The reaction that describes the formation of bicarbonate ions in the blood is:
\[\ce{CO2 + H2O → H2CO3 → H^{+} + HCO3^{-}}\]
This means that carbon dioxide reacts with water to form carbonic acid, which dissociates in solution to form hydrogen ions and bicarbonate ions. The main implication of this process is that the pH of blood becomes a way of determining the amount of carbon dioxide in blood. This is because if carbon dioxide increases in the body, it will manifest as increased concentrations of bicarbonate and increased concentrations of hydrogen ions that reduce blood pH and make the blood more acidic. Conversely, if carbon dioxide levels are reduced, there will be less bicarbonate and less hydrogen ions dissolved in the blood, so pH will increase and blood will become more basic. Bicarbonate ions act as a buffer for the pH of blood so that blood pH will be neutral as long as bicarbonate and hydrogen ions are balanced.
This connection explains how ventilation rate and blood chemistry are related, as hyperventilation will cause alkalosis, and hypoventilation will cause acidosis, due to the changes in carbon dioxide levels that they cause. Bicarbonate is also carried in the fluids of tissues besides the blood vessels, especially in the duodenum and intestine, so problems in those organs can cause a respiratory system response.
Transport to the Alveoli
After carbon dioxide travels through the bloodstream to the capillaries covering the alveoli of the lungs through any of the 3 methods listed above, it must return to dissolved carbon dioxide form in order to diffuse across the capillary into the alveolus. Dissolved carbon dioxide is already able to diffuse into the alveolus, while hemoglobin-bound carbon dioxide is unloaded into the plasma.
For carbon dioxide stored in bicarbonate, it undergoes a reaction reversal. Bicarbonate ions dissolved in the plasma enter the red blood cells by diffusing across a chloride ion gradient (replacing chloride inside the cell), and combining with hydrogen to form carbonic acid.
Next, the action of carbonic anhydrase breaks carbonic acid down into carbon dioxide in water, which leaves the cell by diffusion. The dissolved carbon dioxide is then able to diffuse into the alveolus.
Key Points
- Carbon dioxide is transported through the bloodstream either dissolved in blood, bound the hemoglobin, or converted to bicarbonate ions.
- The Haldane effect is the decreased binding of carbon dioxide in hemoglobin due to increased oxygen levels and increased binding of carbon dioxide to hemoglobin from decreased oxygen levels.
- \(\ce{CO2 + H2O → H2CO3 → H^{+} + HCO3^{−}}\) is the bicarbonate formation reaction in the plasma.
- Increased carbon dioxide means increased blood acidity and conversely while decreased carbon dioxide means decreased blood acidity.
- The bicarbonate reaction is reversible, which allows bicarbonate to turn back into dissolved carbon dioxide to diffuse from the alveolus.
Key Terms
- red blood cell: A type of cell in the blood of vertebrates that contains hemoglobin and transports oxygen from the lungs to the tissues; an erythrocyte.
- Bicarbonate: A negatively charged ion that accumulates in plasma when carbon dioxide dissolves in water and reacts with it. It also acts as a buffer for blood pH.
- carbonic anhydrase: An enzyme that catalyzes the bicarbonate reaction in either direction.
LICENSES AND ATTRIBUTIONS
CC LICENSED CONTENT, SHARED PREVIOUSLY
- Curation and Revision. Authored by: Boundless.com. Provided by: Boundless.com. License: CC BY-SA: Attribution-ShareAlike
CC LICENSED CONTENT, SPECIFIC ATTRIBUTION
- passive diffusion. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/passive%20diffusion. License: CC BY-SA: Attribution-ShareAlike
- External respiration. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/External_respiration. License: CC BY-SA: Attribution-ShareAlike
- Boundless. Provided by: Boundless Learning. Located at: www.boundless.com//physiology...costal-muscles. License: CC BY-SA: Attribution-ShareAlike
- gas transport. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/gas%20transport. License: CC BY-SA: Attribution-ShareAlike
- Gas_exchange_in_the_aveolus_simple_en.svg 1.png. Provided by: Wikimedia Commons. Located at: commons.wikimedia.org/wiki/File:Gas_exchange_in_the_aveolus.svg. License: CC BY: Attribution
- Cellular respiration. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Cellular_respiration. License: CC BY-SA: Attribution-ShareAlike
- Gas exchange. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Gas_exchange. License: CC BY-SA: Attribution-ShareAlike
- External respiration. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/External_respiration. License: CC BY-SA: Attribution-ShareAlike
- respiration. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/respiration. License: CC BY-SA: Attribution-ShareAlike
- metabolite. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/metabolite. License: CC BY-SA: Attribution-ShareAlike
- transport. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/transport. License: CC BY-SA: Attribution-ShareAlike
- Gas_exchange_in_the_aveolus_simple_en.svg 1.png. Provided by: Wikimedia Commons. Located at: commons.wikimedia.org/wiki/File:Gas_exchange_in_the_aveolus.svg. License: CC BY: Attribution
- CellRespiration. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/File:CellRespiration.svg. License: Public Domain: No Known Copyright
- Oxygen transport. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Oxygen_transport%23Oxygen_transport. License: CC BY-SA: Attribution-ShareAlike
- Boundless. Provided by: Boundless Learning. Located at: www.boundless.com//physiology/definition/dissociation-curve. License: CC BY-SA: Attribution-ShareAlike
- acidity. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/acidity. License: CC BY-SA: Attribution-ShareAlike
- Boundless. Provided by: Boundless Learning. Located at: www.boundless.com//physiology/definition/binding-capacity. License: CC BY-SA: Attribution-ShareAlike
- Hemoglobin. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Hemoglobin. License: CC BY-SA: Attribution-ShareAlike
- Oxygenu2013haemoglobin dissociation curve. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Oxygen%E2%80%93haemoglobin_dissociation_curve. License: CC BY-SA: Attribution-ShareAlike
- Gas_exchange_in_the_aveolus_simple_en.svg 1.png. Provided by: Wikimedia Commons. Located at: commons.wikimedia.org/wiki/File:Gas_exchange_in_the_aveolus.svg. License: CC BY: Attribution
- CellRespiration. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/File:CellRespiration.svg. License: Public Domain: No Known Copyright
- 1904%20Hemoglobin. Provided by: Wikimedia%20Commons. Located at: commons.wikimedia.org/wiki/File:1904_Hemoglobin.jpg. License: CC BY-SA: Attribution-ShareAlike
- Oxyhaemoglobin dissociation curve. Provided by: Wikimedia Commons. Located at: en.Wikipedia.org/wiki/File:Oxyhaemoglobin_dissociation_curve.png. License: Public Domain: No Known Copyright
- Carbaminohemoglobin. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Carbaminohemoglobin. License: CC BY-SA: Attribution-ShareAlike
- Hemoglobin. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Hemoglobin. License: CC BY-SA: Attribution-ShareAlike
- Carbon dioxide. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Carbon_dioxide%23Transport_in_the_blood. License: CC BY-SA: Attribution-ShareAlike
- Boundless. Provided by: Boundless Learning. Located at: www.boundless.com//physiology/definition/carbamino. License: CC BY-SA: Attribution-ShareAlike
- enzyme. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/enzyme. License: CC BY-SA: Attribution-ShareAlike
- red blood cell. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/red_blood_cell. License: CC BY-SA: Attribution-ShareAlike
- Gas_exchange_in_the_aveolus_simple_en.svg 1.png. Provided by: Wikimedia Commons. Located at: commons.wikimedia.org/wiki/File:Gas_exchange_in_the_aveolus.svg. License: CC BY: Attribution
- CellRespiration. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/File:CellRespiration.svg. License: Public Domain: No Known Copyright
- 1904%20Hemoglobin. Provided by: Wikimedia%20Commons. Located at: commons.wikimedia.org/wiki/File:1904_Hemoglobin.jpg. License: CC BY-SA: Attribution-ShareAlike
- Oxyhaemoglobin dissociation curve. Provided by: Wikimedia Commons. Located at: en.Wikipedia.org/wiki/File:Oxyhaemoglobin_dissociation_curve.png. License: Public Domain: No Known Copyright
- Hemoglobin. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Hemoglobin. License: Public Domain: No Known Copyright

