26.4E: Hormonal Regulation of the Male Reproductive System
- Page ID
- 8247
The male reproductive system is regulated by the production, stimulation, and feedback of specific hormones.
LEARNING OBJECTIVE
Differentiate among the hormones of the male reproductive system
Key Takeaways
Key Points
- GnRH is made in the hypothalamus and travels to the pituitary where it stimulates FSH and LH secretion.
- FSH is necessary for sperm maturation.
- LH binds to Leydig cells to stimulate testosterone secretion and androgen production.
- Testosterone stimulates sex drive.
- Inhibin acts as negative feedback to slow the release of FSH and GnRH.
Key Terms
- GnRH: Gonadotropin-releasing hormone is a trophic peptide hormone responsible for the release of follicle-stimulating hormone (FSH) and luteinizing hormone (LH) from the anterior pituitary.
- LH: Luteinizing hormone is produced by the anterior pituitary gland and in males causes the synthesis and secretion of testosterone and androgen.
- FSH: Follicle-stimulating hormone stimulates both the production of androgen-binding protein by Sertoli cells and the formation of the blood-testis barrier.
Hormonal control of spermatogenesis varies among species. In humans, the mechanisms are not completely understood. However, it is known that initiation of spermatogenesis occurs at puberty due to the interaction of the hypothalamus, pituitary gland, and Leydig cells. If the pituitary gland is removed, spermatogenesis can still be initiated by follicle-stimulating hormone (FSH) and testosterone.
The Role of Hormones in Male Reproduction
Studies from rodent models suggest that gonadotropin hormones (both LH and FSH) support the process of spermatogenesis by suppressing the proapoptotic signals and thus promoting spermatogenic cell survival. The Sertoli cells themselves mediate parts of spermatogenesis through hormone production. They are capable of producing the hormones estradiol and inhibin. The Leydig cells are also capable of producing estradiol in addition to their main product, testosterone.
Gonadotropin-Releasing Hormone
Gonadotropin-releasing hormone (GnRH) is mainly made in the preoptic area of the hypothalamus before traveling to the pituitary gland. There it stimulates the synthesis and secretion of the gonadotropins, FSH and luteinizing hormone (LH).
Follicle-Stimulating Hormone
Follicle-stimulating hormone (FSH) is released by the anterior pituitary gland. Its presence in males is necessary for the maturation of spermatozoa. Follicle-stimulating hormone stimulates both the production of androgen-binding protein by Sertoli cells and the formation of the blood-testis barrier. Increasing the levels of FSH increases the production of spermatozoa by preventing the apoptosis of type A spermatogonia.
Luteinizing Hormone
Luteinizing hormone (LH) is released by the anterior pituitary gland. In the testes, LH binds to receptors on Leydig cells, which stimulates the synthesis and secretion of testosterone.
Testosterone
Testosterone is made in the interstitial cells of the testes. It stimulates the sex drive and is associated with aggression. Androgen-binding protein is essential to concentrating testosterone in levels high enough to initiate and maintain spermatogenesis, which can be 20-50 times higher than the concentration found in blood. The sequestering of testosterone in the testes is initiated by FSH, and only testosterone is required to maintain spermatogenesis.
Inhibin
Inhibin is secreted by the Sertoli cells and acts to decrease the levels of FSH. The hormone is released into the circulation when the sperm count is too high.
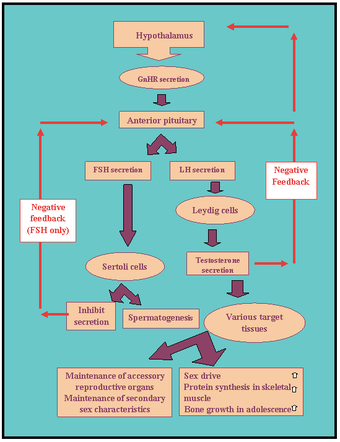
Hormonal Influence: This flowchart details the steps involved in hormonal control of male reproduction.
This diagram depicts the hormonal regulation of male reproduction, including the following steps: hypothalamus, GnHR secretion, anterior pituitary, FSH and LH secretion, negative feedback, Leydig cells, Sertoli cells, testosterone secretion, inhibit secretion, spermatogenesis, various target tissues, maintenance of accessory reproductive organs and secondary sex characteristics, sex drive, protein synthesis in skeletal muscle, and bone growth in adolescents.
LICENSES AND ATTRIBUTIONS
CC LICENSED CONTENT, SHARED PREVIOUSLY
- erection. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/erection. License: CC BY-SA: Attribution-ShareAlike
- refractory period. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/refractory_period. License: CC BY-SA: Attribution-ShareAlike
- genitalia. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/genitalia. License: CC BY-SA: Attribution-ShareAlike
- Sexual arousal. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Sexual_arousal. License: CC BY-SA: Attribution-ShareAlike
- Oogamy. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Oogamy. License: CC BY-SA: Attribution-ShareAlike
- spermatozoa. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/spermatozoa. License: CC BY-SA: Attribution-ShareAlike
- Anisogamy. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Anisogamy. License: CC BY-SA: Attribution-ShareAlike
- Sperm. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Sperm. License: CC BY: Attribution
- acrosome. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/acrosome. License: CC BY-SA: Attribution-ShareAlike
- sperm. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/sperm. License: CC BY-SA: Attribution-ShareAlike
- Spermatogenesis. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Spermatogenesis. License: CC BY-SA: Attribution-ShareAlike
- spermatid. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/spermatid. License: CC BY-SA: Attribution-ShareAlike
- spermatocyte. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/spermatocyte. License: CC BY-SA: Attribution-ShareAlike
- spermatogonium. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/spermatogonium. License: CC BY-SA: Attribution-ShareAlike
- Seminiferous_tubule_and_sperm. Authored by: Nephron. Provided by: Wikimedia. Located at: commons.wikimedia.org/wiki/F..._and_sperm.jpg. License: CC BY-SA: Attribution-ShareAlike
- seminal vesicle. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/seminal_vesicle. License: CC BY-SA: Attribution-ShareAlike
- seminal fluid. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/seminal_fluid. License: CC BY-SA: Attribution-ShareAlike
- Semen. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/Semen. License: CC BY-SA: Attribution-ShareAlike
- semen. Provided by: Wiktionary. Located at: en.wiktionary.org/wiki/semen. License: CC BY-SA: Attribution-ShareAlike
- Male Reproductive System. Provided by: brookingsapbiology. Located at: http://brookingsapbiology.wikispaces...ductive+System. Project: Wikispace. License: CC BY-SA: Attribution-ShareAlike
- GnRH. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/GnRH. License: CC BY-SA: Attribution-ShareAlike
- LH. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/LH. License: CC BY-SA: Attribution-ShareAlike
- FSH. Provided by: Wikipedia. Located at: en.Wikipedia.org/wiki/FSH. License: CC BY-SA: Attribution-ShareAlike
- Curation and Revision. Authored by: Boundless.com. Provided by: Boundless.com. License: CC BY-SA: Attribution-ShareAlike
PUBLIC DOMAIN CONTENT
- Sperm-egg. Authored by: Unknown. Located at: en.Wikipedia.org/wiki/File:Sperm-egg.jpg. License: Public Domain: No Known Copyright
- Sperm. Authored by: LadyofHats. Located at: commons.wikimedia.org/wiki/F...matozoa_en.svg. License: Public Domain: No Known Copyright
- Male reproductive hormone chart. Authored by: Stephaniegreenwood. Provided by: Wikimedia. Located at: commons.wikimedia.org/wiki/Fi...mone_chart.gif. License: Public Domain: No Known Copyright

