29.10C: Syncope
- Page ID
- 8366
Syncope, the medical term for fainting, is a transient loss of consciousness.
- Identify the main factor associated with syncope
Key Points
- This loss of consciousness can arise due to changes in postural tone.
- The two broad categories of syncope are cardiogenic and reflex; of the two, cardiogenic syncope is more likely to result in morbidity or mortality.
- Vasovagal syncope is situational syncope which may arise in situations where the patient feels scared, threatened, embarrassed, or uneasy.
Key Terms
- cardiogenic syncope: The form of syncope that is more likely to produce serious morbidity or mortality and require prompt treatment.
- reflex syncope: Involuntary fainting.
- vasovagal syncope: Situational syncope which may arise in situations where the patient feels scared, threatened, embarrassed, or uneasy.
Syncope, the medical term for fainting, is defined as a transient loss of consciousness and postural tone characterized by rapid onset, short duration, and spontaneous recovery due to global cerebral hypoperfusion that most often results from hypotension.
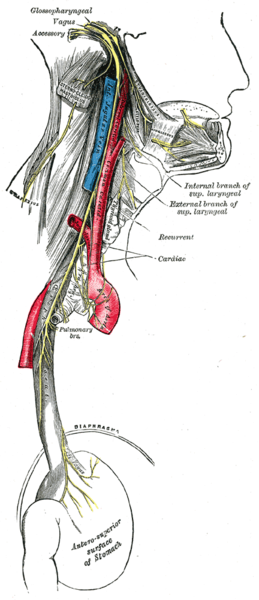
Vagus Nerve: The vagus nerve, labeled at the top left and colored in yellow, may lower heart rate, reducing blood flow to the brain and causing vasovagal syncope.
Many forms of syncope are preceded by a prodromal state that often includes dizziness and loss of vision (“blackout”) (temporary), loss of hearing (temporary), loss of pain and feeling (temporary), nausea and abdominal discomfort, weakness, sweating, a feeling of heat, palpitations, and other phenomena, which–if they do not progress to loss of consciousness and postural tone–are often denoted “presyncope.” Abdominal discomfort prior to loss of consciousness may be indicative of seizure which should be considered different than syncope.
Types of Syncope
There are two broad categories of syncope, cardiogenic or reflex, which underlie most forms of syncope. Cardiogenic forms are more likely to produce serious morbidity or mortality and require prompt or even immediate treatment. Although cardiogenic syncope is much more common in older patients, an effort to rule out arrhythmic, obstructive, ischemic, or cardiomyopathic causes of syncope and circulatory inadequacy is mandatory in each patient.
Variants of reflex syncope often have characteristic histories, including precipitants and time course which are made evident by skilled history taking. Thus, the clinical history is the foremost tool used in the differential diagnosis of syncope. Physical examination, and electrocardiogram are part of the initial evaluation of syncope and other more specific tools such as loop recorders may be necessary in clinically uncertain cases.
Vasovagal Syncope
Vasovagal (situational) syncope, one of the most common types, may occur in scary, embarrassing or uneasy situations, or during blood drawing, coughing, urination, or defecation. In vasovagal syncope, the vagus nerve decreases blood flow to the brain. Other types include postural syncope (caused by a change in body posture), cardiac syncope (due to heart-related conditions), and neurological syncope (due to neurological conditions). There are many other causes of syncope, including low blood sugar levels and lung disease such as emphysema and a pulmonary embolus. The cause of the fainting can be determined by a doctor using a complete history, physical, and various diagnostic tests.
The vasovagal type can be considered in two forms:
- Isolated episodes of loss of consciousness, unheralded by any warning symptoms for more than a few moments. These tend to occur in the adolescent age group, and may be associated with fasting, exercise, abdominal straining, or circumstances promoting vasodilation (e.g., heat, alcohol). The subject is invariably upright. The tilt-table test, if performed, is generally negative.
- Recurrent syncope with complex associated symptoms called neurally mediated syncope. It is associated with any of the following: preceding or succeeding sleepiness, preceding visual disturbance (“spots before the eyes”), sweating, and light-headedness. The subject is usually but not always upright. The tilt-table test, if performed, is generally positive.

