13.3: Hearing, Balance and Vision
- Page ID
- 46175
By the end of this section, you will be able to:
- Describe the gross and microscopic structures responsible for the special senses of hearing, balance, and vision
- List the supporting structures around the eye and describe the lacrimal apparatus
Audition (Hearing)
Hearing, or audition, is the transduction of sound waves into a neural signal that is made possible by the structures of the ear (Figure \(\PageIndex{1}\)). The large, fleshy structure on the lateral aspect of the head is known as the auricle. Some sources will also refer to this structure as the pinna, though that term is more appropriate for a structure that can be moved, such as the external ear of a cat. The C-shaped curves of the auricle direct sound waves toward the auditory canal, also called ear canal. The canal enters the skull through the external auditory meatus of the temporal bone. At the end of the auditory canal is the tympanic membrane, or ear drum, which vibrates after it is struck by sound waves. The auricle, ear canal, and tympanic membrane are often referred to as the external ear. The middle ear consists of a space spanned by three small bones called the ossicles. The three ossicles are the malleus, incus, and stapes, which are Latin names that roughly translate to hammer, anvil, and stirrup. The malleus is attached to the tympanic membrane and articulates with the incus. The incus, in turn, articulates with the stapes. The stapes is then attached to the inner ear, where the sound waves will be transduced into a neural signal. The middle ear is connected to the pharynx through the Eustachian (or auditory) tube, which helps equilibrate air pressure across the tympanic membrane. The tube is normally closed but will pop open when the muscles of the pharynx contract during swallowing or yawning. This helps to equalize the pressure on both sides of the ear drum with change in altitude, such as driving up the mountain or in a plane.
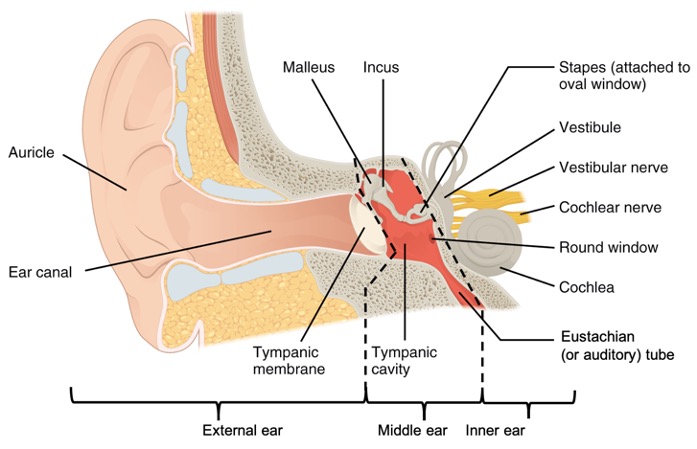
The inner ear is often described as a bony labyrinth, as it is composed of a series of canals embedded within the temporal bone. Within the bony labyrinth are membranes that separate tubes and spaces filled with liquid. This is called the membranous labyrinth. The space between the bony labyrinth and membranous labyrinth is filled with a fluid called perilymph which is similar to extracellular fluid. Inside the membranous labyrinth there is endolymph which has a high potassium and low sodium concentration compared to the perilymph and consequently is conducive to nerve impulses. The inner ear has three separate regions, the cochlea, the vestibule, and the semicircular canals. The cochlea is responsible for hearing while the vestibule and semicircular canals are important for balance. The neural signals from these regions are relayed to the brainstem through separate fiber bundles. called the cochlear nerve and the vestibular nerve. However, these two distinct bundles travel together from the inner ear to the brainstem as the vestibulocochlear nerve (CN VIII).
Sound is transduced into neural signals within the cochlear region of the inner ear, which contains the sensory neurons of the spiral ganglia. These ganglia are located within the spiral-shaped cochlea of the inner ear. The cochlea is attached to the stapes through the oval window. The oval window is located at the beginning of a fluid-filled tube within the cochlea called the scala vestibuli. The scala vestibuli extends from the oval window, travelling above the cochlear duct, which is the central cavity of the cochlea that contains the sound-transducing neurons. At the uppermost tip of the cochlea, the scala vestibuli curves over the top of the cochlear duct. The fluid-filled tube, now called the scala tympani, returns to the base of the cochlea, this time travelling under the cochlear duct. The scala tympani ends at the round window, which is covered by a membrane that contains the fluid within the scala.
A cross-sectional view of the cochlea shows that the scala vestibuli and scala tympani run along both sides of the cochlear duct (Figure \(\PageIndex{2}\) and Figure \(\PageIndex{3}\)). The cochlear duct contains several organs of Corti, which tranduce the wave motion of the two scala into neural signals. The organs of Corti lie on top of the basilar membrane, which is the side of the cochlear duct located between the organs of Corti and the scala tympani. Another membrane called the vestibular membrane separates the cochlear duct from the scala vestibuli.
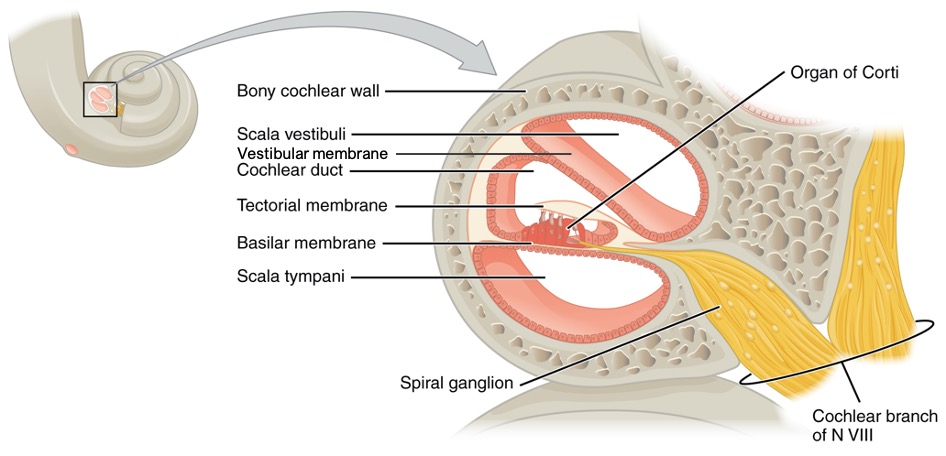
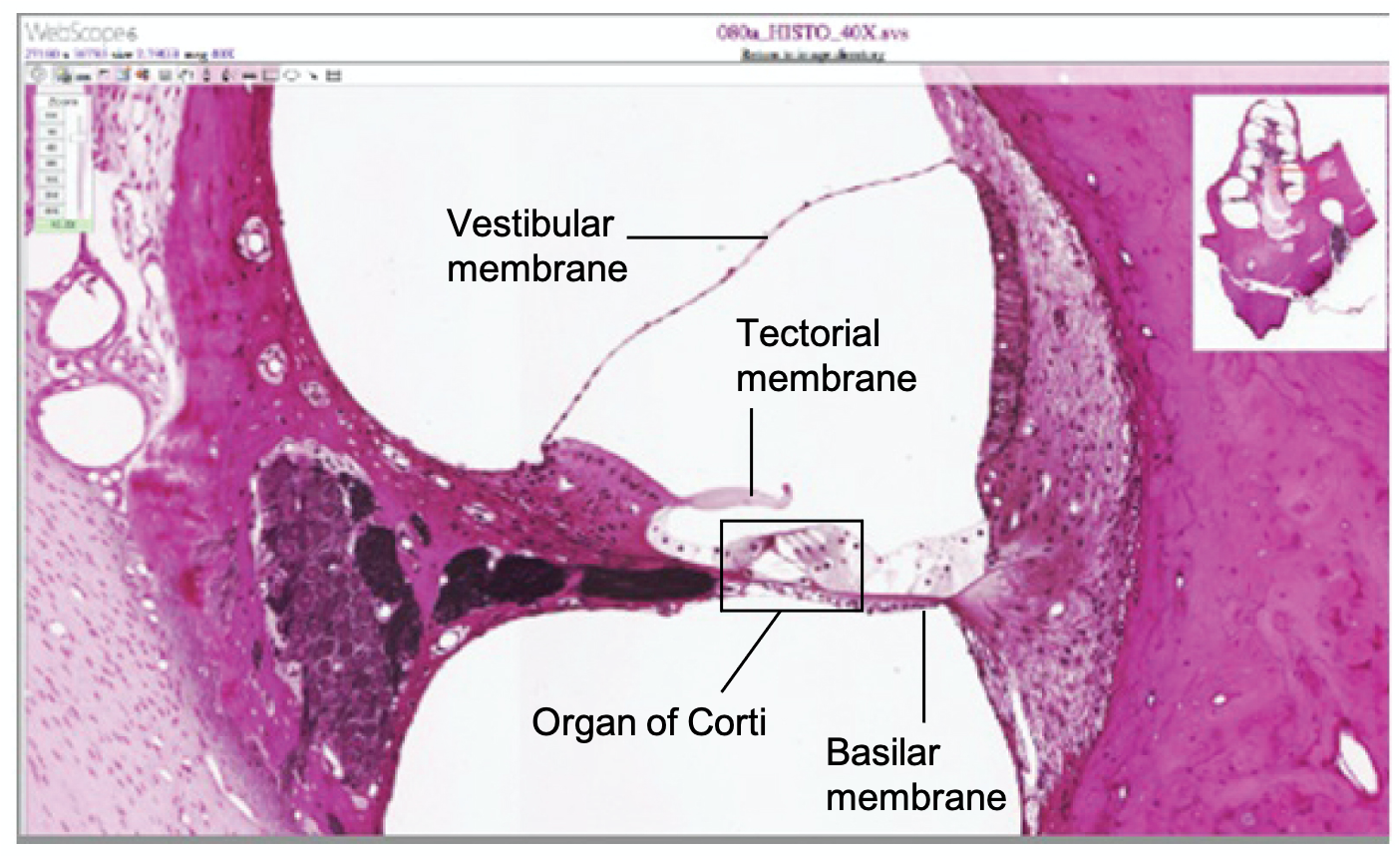
The organs of Corti contain hair cells, which are named for the hair-like stereocilia extending from the cell’s apical surfaces (Figure \(\PageIndex{4}\)). The stereocilia are an array of microvilli-like structures arranged from tallest to shortest. Protein fibers tether adjacent hairs together within each array, such that the array will bend in response to movements of the basilar membrane. The stereocilia extend up from the hair cells to the overlying tectorial membrane, which is attached medially to the organ of Corti.
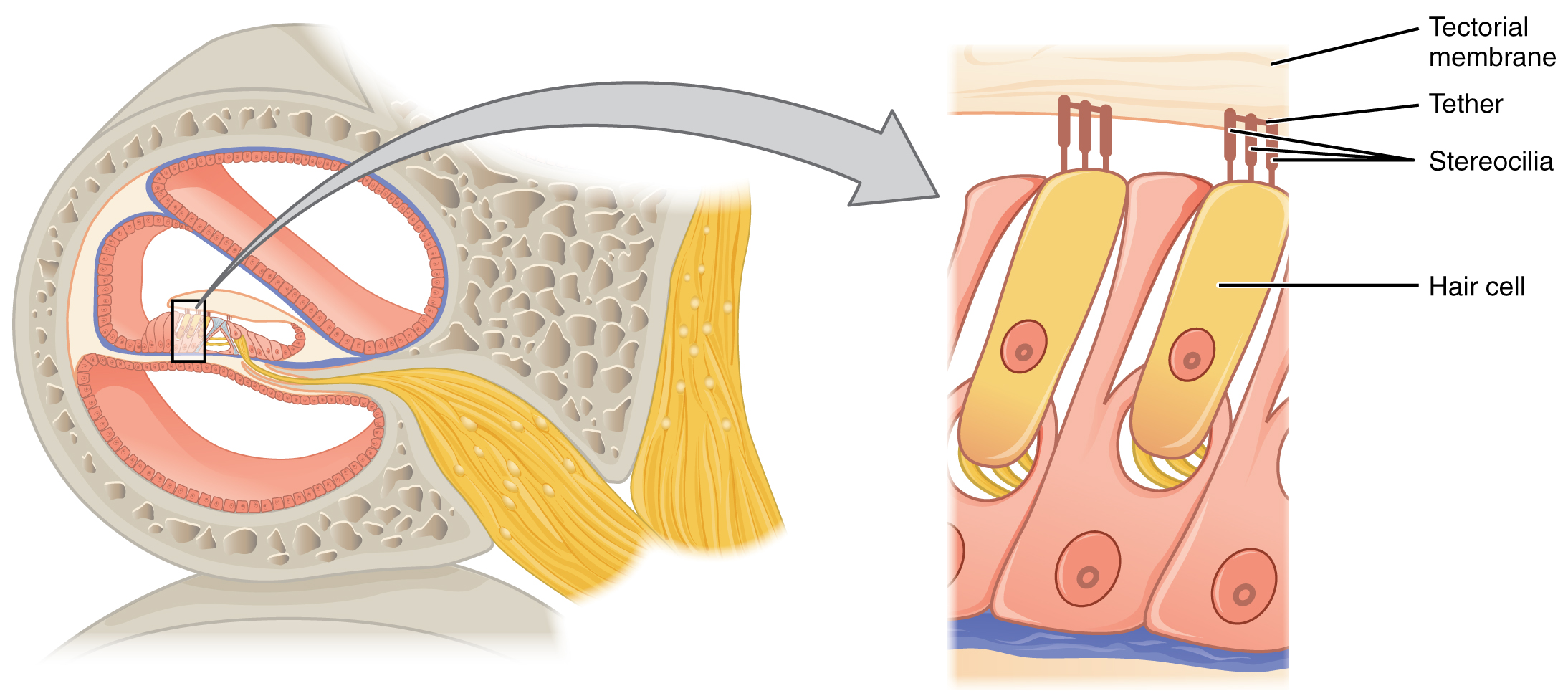
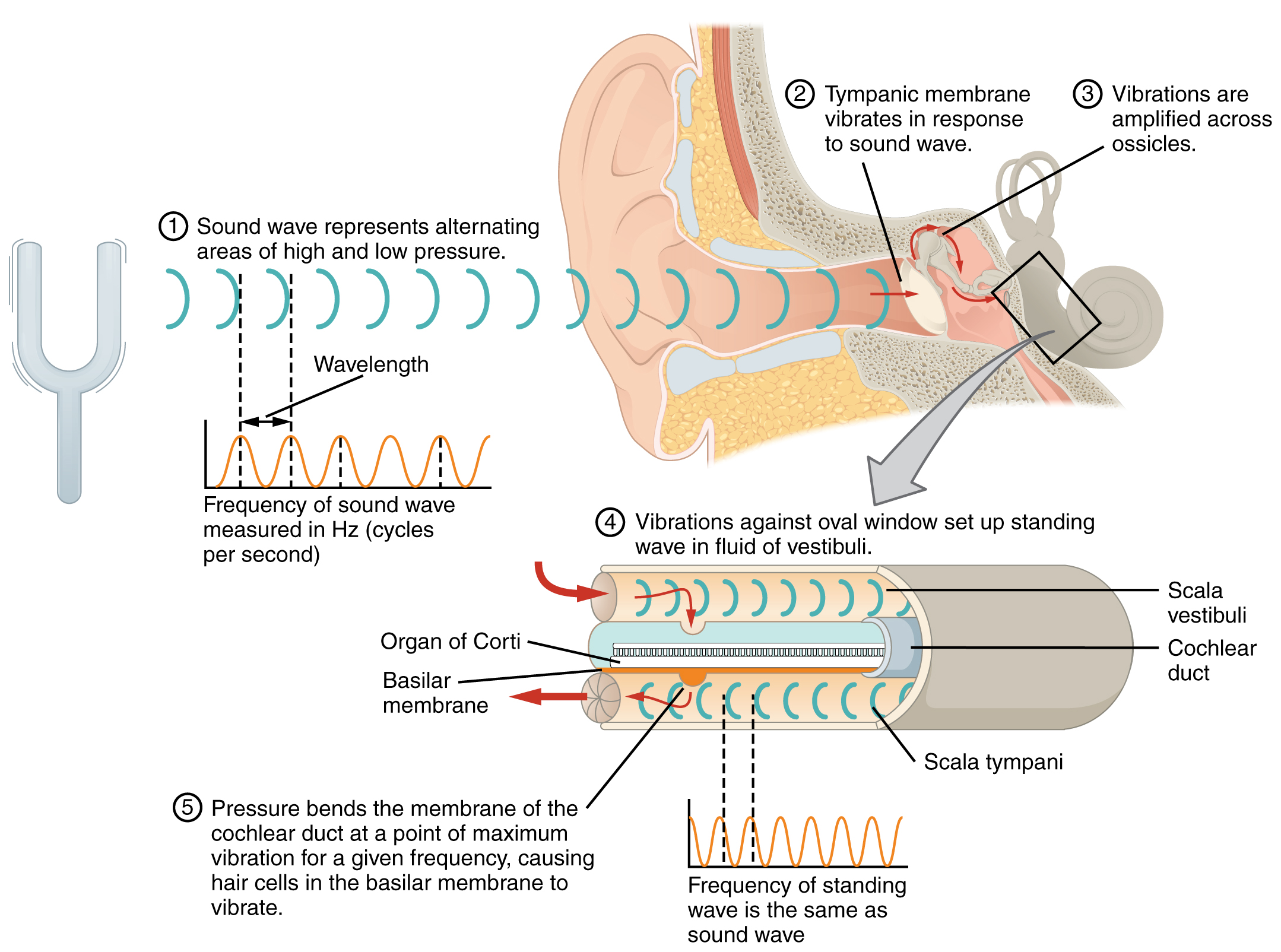
The transmission and transduction of sound require the participation of the majority of the structures of the ear. Each sound wave has a specific frequency, which depends on its pitch, and amplitude, which depends on its loudness. Sound waves are funneled into the ear canal by the auricle and reach the tympanic membrane (Figure \(\PageIndex{5}\)). The vibration of the tympanic membrane is amplified across the ossicles. As vibrations of the ossicles travel through the oval window, the fluid of the scala vestibuli and scala tympani moves in a wave-like motion. The frequency of the fluid waves match the frequencies of the sound waves. The membrane covering the round window will bulge out or pucker in with the movement of the fluid within the scala tympani. As the fluid waves move through the scala vestibuli and scala tympani, the basilar membrane moves at a specific spot of the cochlea, depending on the frequency of the waves. Higher frequency waves move the region of the basilar membrane that is close to the base of the cochlea. Lower frequency waves move the region of the basilar membrane that is near the tip of the cochlea. When the fluid waves from the scala move the basilar membrane, the tectorial membrane slides across the stereocilia. This bends the stereocilia either toward or away from the tallest member of each array of stereocilia. When the stereocilia bend toward the tallest member of their array, tension in the protein tethers opens ion channels in the hair cell membrane. This will electrically change the hair cell membrane, triggering nerve impulses that travel down the afferent nerve fibers attached to the hair cells. When the stereocilia bend toward the shortest member of their array, the tension on the tethers slackens and the ion channels close. The relative movement of different arrays of stereocilia along the length of the basilar membrane allows the brain to perceive frequency, or pitch. The greater force of louder sounds causes an increase in the range of movement of the stereocilia of the hair cells, determining the loudness of a sound. The hair cells then transmit neural signals through the release of neurotransmitters to the cochlear nerve which travels within the vestibulocochlear nerve (CN VIII). The nerve carries the auditory information into the brain, through the thalamus, and into the primary auditory cortex of the temporal lobe.
Interactive Link
Cochlea

View a histological slide of the cochlea at the University of Michigan WebScope to explore the tissue sample in greater detail. The basilar membrane is the thin membrane that extends from the central core of the cochlea to the edge. What is anchored to this membrane so that they can be activated by movement of the fluids within the cochlea?
- Answer
-
The hair cells are located in the organ of Corti, which is located on the basilar membrane. The stereocilia of those cells would normally be attached to the tectorial membrane (though they are detached in the micrograph because of processing of the tissue).
Equilibrium (Balance)
Along with audition, the inner ear is responsible for encoding information about equilibrium, the sense of balance. A similar mechanoreceptor—a hair cell with stereocilia—senses head position, head movement, and whether our bodies are in motion. These cells are located in the vestibule and semicircular canals within the inner ear. Vestibule and semicircular canals compose the vestibular system. The vestibule is the central part of the bony labyrinth, and is located posterior to the cochlea and anterior to the semicircular canals. Within the vestibule, the membranous labyrinth forms two chambers, the utricle and saccule, which contain endolymph. The utricle and saccule are interconnected by a narrow endolymphatic duct and their endolymph is confluent with that of the semicircular ducts and cochlear duct. Head position is sensed by the utricle and saccule, whereas head movement is sensed by the semicircular canals.
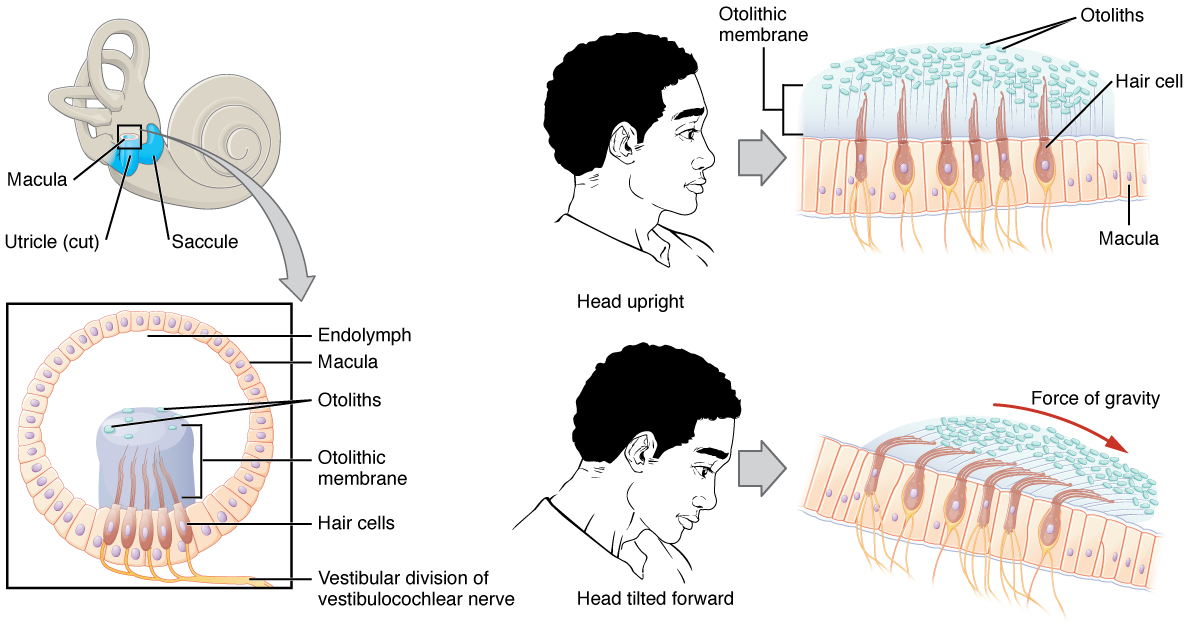
The utricle and saccule are both largely composed of macula tissue (plural = maculae). The macula is composed of hair cells surrounded by supporting cells. The stereocilia of the hair cells extend into a viscous gel called the otolithic membrane (Figure \(\PageIndex{6}\)). On top of the otolithic membrane is a layer of calcium carbonate crystals, called otoliths. The otoliths essentially make the otolithic membrane top-heavy. The otolithic membrane moves separately from the macula in response to head movements. Tilting the head causes the otolithic membrane to slide over the macula in the direction of gravity. The moving otolithic membrane, in turn, bends the sterocilia, causing the hair cells to elicit electrical changes. The exact position of the head is interpreted by the brain based on the pattern of hair-cell activation.
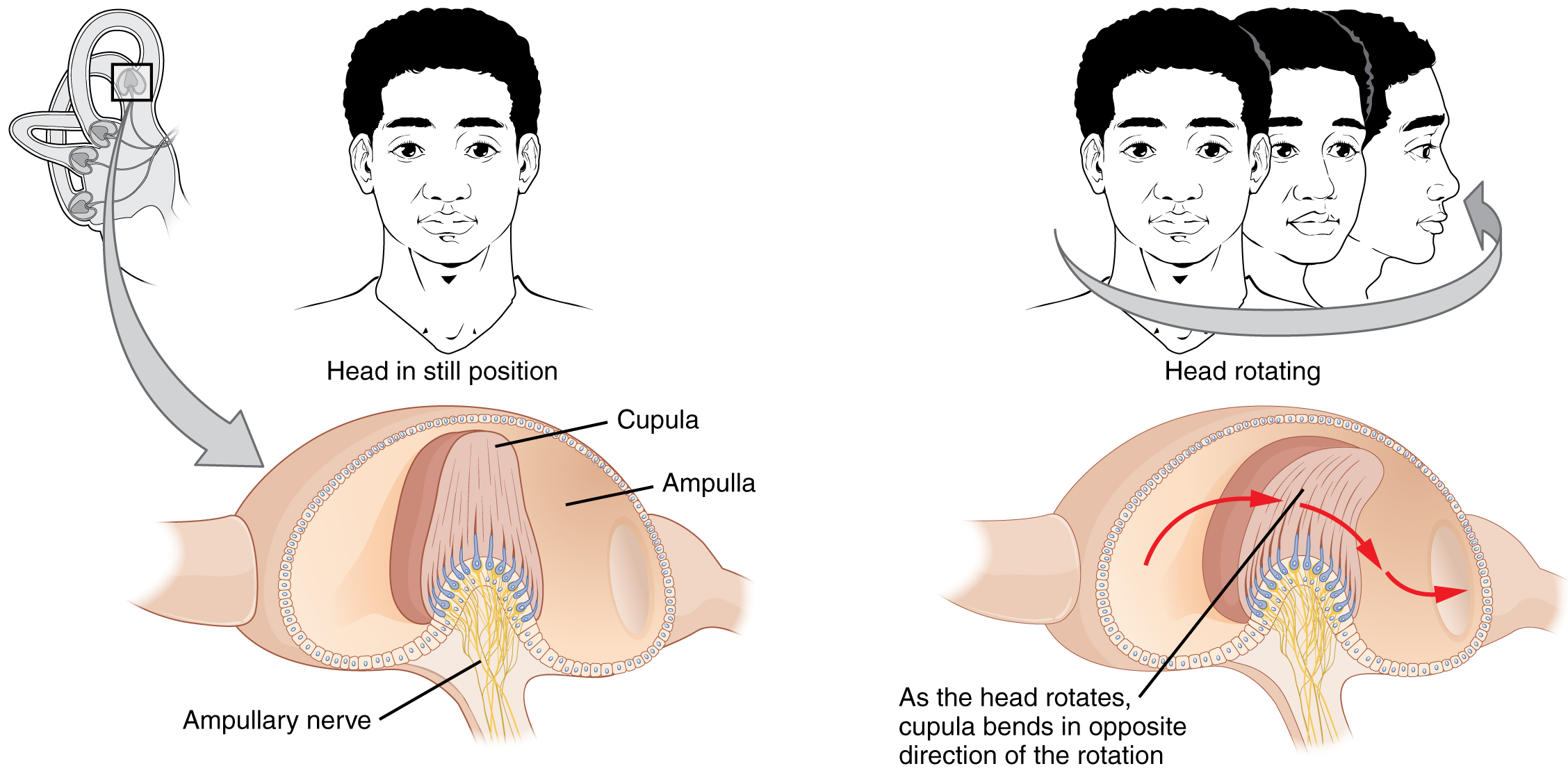
The semicircular canals are three ring-like extensions of the vestibule. One is oriented in the horizontal plane, whereas the other two are oriented in the vertical plane. The anterior and posterior vertical canals are oriented at approximately 45 degrees relative to the sagittal plane (Figure \(\PageIndex{7}\)). The base of each semicircular canal, where it meets with the vestibule, connects to an enlarged region known as the ampulla. The ampulla contains the hair cells that respond to rotational movement, such as turning the head while saying “no.” The stereocilia of these hair cells extend into the cupula, a gelatinous membrane that attaches to the top of the ampulla. As the head rotates in a plane parallel to the semicircular canal, the fluid lags, deflecting the cupula in the direction opposite to the head movement. The semicircular canals contain several ampullae, with some oriented horizontally and others oriented vertically. By comparing the relative movements of both the horizontal and vertical ampullae, the vestibular system can detect the direction of most head movements within three-dimensional (3-D) space.
The neural signals generated in the vestibule and semicircular canals are transmitted through the vestibular nerve which travels within the vestibulocochlear nerve (CN VIII). The nerve carries the equilibrium information into the brain, through the thalamus, and to cerebral nuclei, brainstem and cerebellum.
Vision
Vision is the special sense of sight that is based on the transduction of light stimuli received through the eyes. The eyes are located within either orbit in the skull. Supportive structures protect the eye, prevent objects from entering the eye, keep its surface lubricated and moist and provide superficial covering.
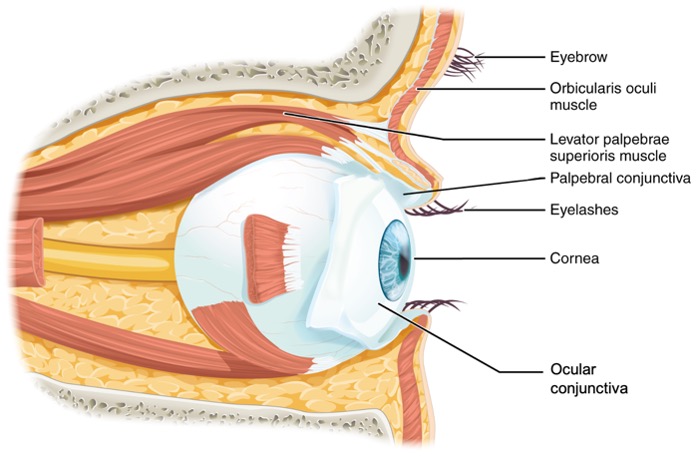
The bony orbits surround the eyeballs, protecting them and anchoring the soft tissues of the eye (Figure \(\PageIndex{8}\)). The eyelids, with lashes at their leading edges, help to protect the eye from abrasions by blocking particles that may land on the surface of the eye. Each eyelid contains a thin covering of skin, a fibrous core and tarsal muscles and glands. The tarsal muscles is composed of smooth muscle innervated by the sympathetic nervous system and helps maintaining the elevation of the superior eyelid. The tarsal glands are sebaceous glands that produce an oily substance which prevents the eyelids from attaching together and prevents the overflow of tears from the open eye. The inner lid is a thin membrane known as the palpebral conjunctiva. The palpebral conjunctiva connects the eyelids to the eyeball. At the connection with the eyeball, a thin layer called the ocular conjunctiva forms a continuous layer on the external and anterior surface of the eye. The most anterior part of the eye is called the cornea and the ocular conjunctiva is absent here. Underneath the ocular conjunctiva lies a white layer called the sclera. The conjunctiva contains blood vessels and nerves that support the avascular sclera and detect foreign particles entering the eye. Bacteria and viruses can infect the conjunctiva, which then becomes red and swollen, as in pink eye (another name for pink eye is conjunctivitis).
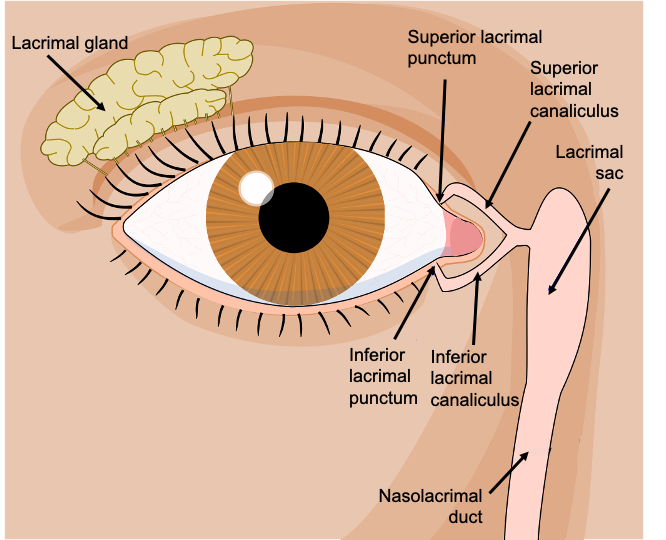
The lacrimal apparatus associated with each eye is responsible for the production and drainage of lacrimal fluid (tears). The lacrimal fluid helps protect the eye by reducing friction of the eyelids, continuously cleaning the anterior surface of the eye, and preventing bacterial infection through the action of lysozyme. Tears are produced by the lacrimal gland, located within the superolateral depression of each orbit (Figure \(\PageIndex{9}\)). Tears produced by this gland are dispersed on the external surface of the eye by the movement of the eyelids and then flow towards the medial surface of the eye. The superior and inferior lacrimal puncta (plural of "punctum") are small openings to drain the lacrimal fluid into channels called the superior and inferior lacrimal canaliculi. From there, the lacrimal fluid enters the lacrimal sac and drains into the nasolacrimal duct that delivers it into the nasal cavity where it mixes with the mucus.
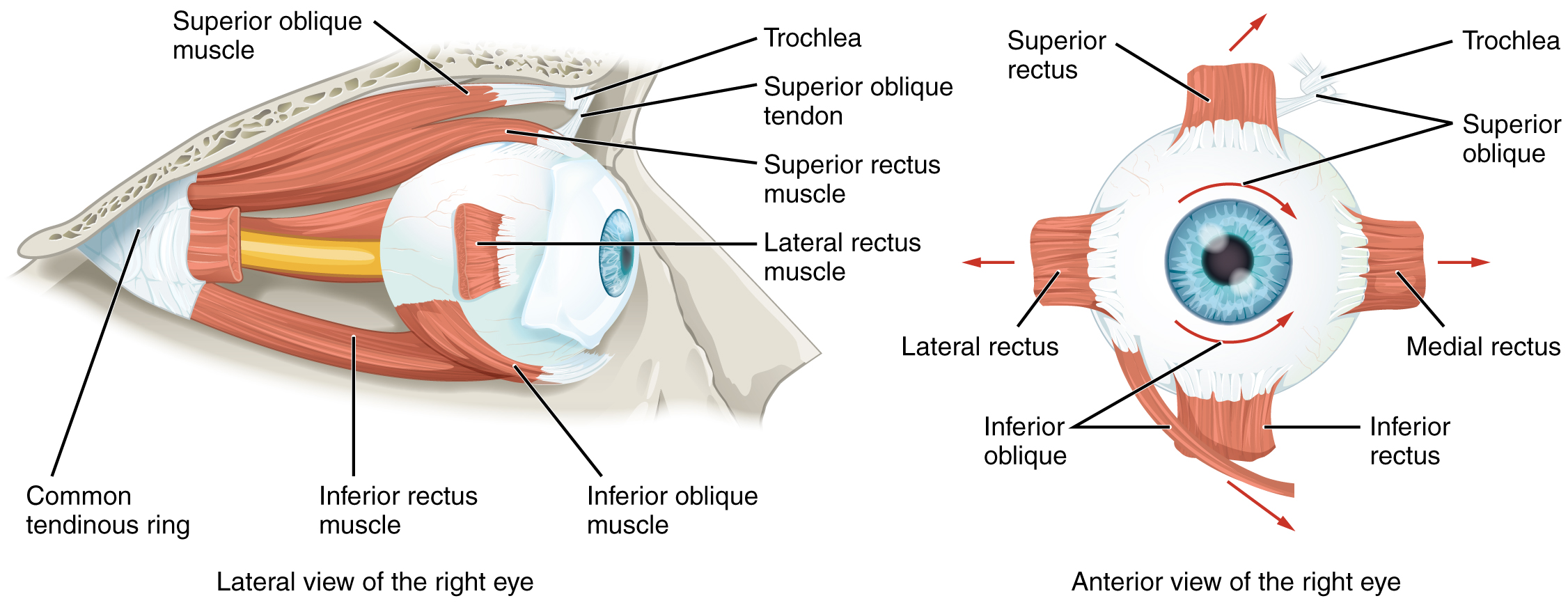
Movement of the eye within the orbit is accomplished by the contraction of six extraocular muscles that originate from the bones of the orbit and insert into the surface of the eyeball (Figure \(\PageIndex{10}\)). Four of the muscles are arranged at opposite sides of a cross around the eye and are named for those locations. They are the superior rectus, medial rectus, inferior rectus, and lateral rectus and originate at the common tendinous ring. When each of these muscles contract, the eye to moves toward the contracting muscle. For example, when the superior rectus contracts, the eye rotates to look up. The superior oblique originates at the posterior orbit, near the origin of the four rectus muscles. However, the tendon of the superior oblique muscles threads through a pulley-like piece of cartilage known as the trochlea. The tendon inserts obliquely into the superior surface of the eye. The angle of the tendon through the trochlea means that contraction of the superior oblique abducts, depresses, and internally rotates (intorsion) the eye. The inferior oblique muscle originates from the floor of the orbit and inserts into the inferolateral surface of the eye. When it contracts, it abducts, elevates, and externally rotates (extorsion) the eye. Rotation of the eye by the two oblique muscles is necessary because the eye is not perfectly aligned on the sagittal plane. When the eye looks up or down, the eye must also rotate slightly to compensate for the superior rectus pulling at approximately a 20-degree angle, rather than straight up. The same is true for the inferior rectus, which is compensated by contraction of the inferior oblique. A seventh muscle in the orbit is the levator palpebrae superioris, which is responsible for elevating and retracting the upper eyelid, a movement that usually occurs in concert with elevation of the eye by the superior rectus (see Figure \(\PageIndex{10}\)).
The extraocular muscles are innervated by three cranial nerves. The lateral rectus, which causes abduction of the eye, is innervated by the abducens nerve (CN VI). The superior oblique is innervated by the trochlear nerve (CN IV). All of the other muscles are innervated by the oculomotor nerve (CN III), as is the levator palpebrae superioris. The motor nuclei of these cranial nerves connect to the brainstem, which coordinates eye movements.
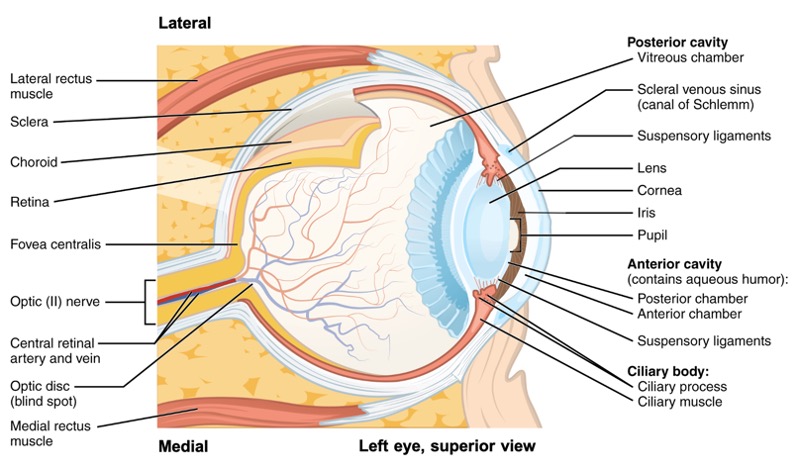
The eye itself is a hollow sphere composed of three layers of tissue. The outermost layer is the fibrous tunic, which includes the white sclera posteriorly and clear cornea anteriorly. The sclera accounts for five sixths of the surface of the eye, most of which is not visible, though humans are unique compared with many other species in having so much of the “white of the eye” visible (Figure \(\PageIndex{11}\)). The transparent cornea covers the anterior tip of the eye and allows light to enter the eye. The middle layer of the eye is the vascular tunic, which is mostly composed of the choroid, ciliary body, and iris. The choroid is a layer of highly vascularized connective tissue that provides a blood supply to the eyeball. The choroid is posterior to the ciliary body, a muscular structure that is attached to the lens by suspensory ligaments. These two structures pull the lens, allowing it to focus light on the back of the eye. Overlaying the ciliary body, and visible in the anterior eye, is the iris—the colored part of the eye. The innermost layer of the eye is the neural tunic, or retina, which contains the nervous tissue responsible for photoreception. The retina consists of two layers: a pigmented layer and a neural layer. The pigmented layer is a layer of pigmented cells that absorb light after it passes through the retina and provides vital metabolic support for the photoreceptors of the retina. The neural layer consists of photoreceptors and blood vessels that supply the neural layer.
The eye is also divided into two cavities: the anterior cavity and the posterior cavity. The anterior cavity is the space between the cornea and lens, including the iris and ciliary body. It can be further divided into anterior and posterior chambers by the iris. These chambers are filled with a watery fluid called the aqueous humor. The posterior cavity is the space behind the lens that extends to the posterior side of the interior eyeball, where the retina is located. The posterior cavity is filled with a more viscous fluid called the vitreous humor. Aqueous humor is continually produced at the ciliary processes of the ciliary body. The aqueous humor passes through the pupil into the anterior chamber and drains into the scleral venous sinus at the edge of the cornea.
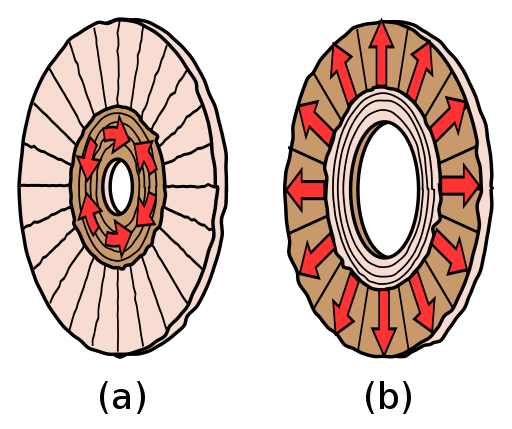
The iris is composed of pigmented layers that give the eye its color and two layers of smooth muscle that opens or closes the pupil, which is the hole at the center of the eye that allows light to enter. The layers of smooth muscle are organized circularly into the sphincter pupillae and radially into the dilator pupillae (Figure \(\PageIndex{12}\)). The sphincter pupillae constricts the pupil, while the dilator pupillae dilates the pupil. The iris constricts the pupil in response to bright light and dilates the pupil in response to dim light.
The retina is composed of several layers and contains specialized cells for the initial processing of visual stimuli. The photoreceptors change their membrane electrical properties when stimulated by light energy. Light falling on the retina causes chemical changes to pigment molecules in the photoreceptors. There are two types of photoreceptors called rods and cones. Cones in human eyes are specialized in perceiving three different primary colors: red, green, and blue. Rods are sensitive to vision in low light conditions, for example in a darkened room. The change in electrical properties of these photoreceptors alters the amount of neurotransmitter that the photoreceptor cells release onto bipolar cells (see Figure \(\PageIndex{13}\)). It is the bipolar cell in the retina that connects a photoreceptor to a retinal ganglion cell (RGC). There, amacrine cells and horizontal cells additionally contribute to retinal processing before an action potential is produced by the RGC. The axons of RGCs, which lie at the innermost layer of the retina, collect at the optic disc and leave the eye as the optic nerve. Because these axons pass through the retina, there are no photoreceptors at the very back of the eye, where the optic nerve begins. This creates a “blind spot” in the retina, and a corresponding blind spot in our visual field. The visual information of the optic nerve will be transmitted through the thalamus and sent to the primary visual cortex of the occipital lobe.
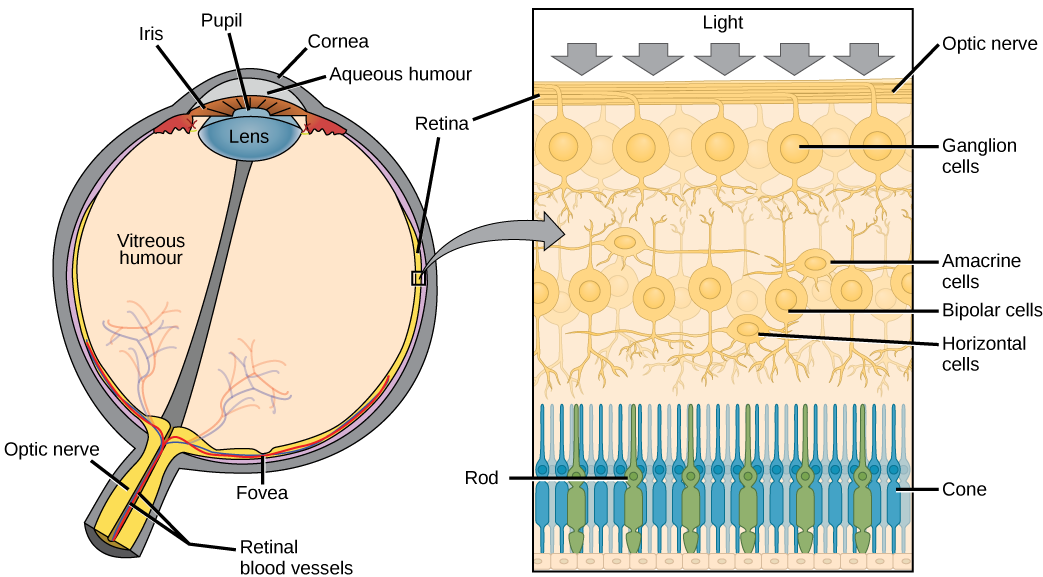
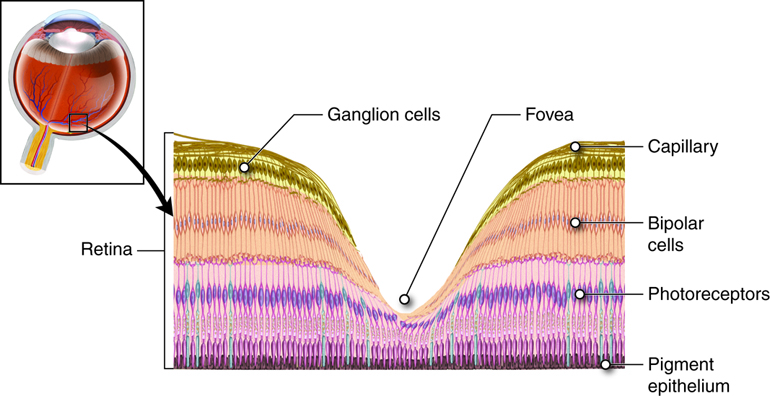
Note that the photoreceptors in the retina (rods and cones) are located behind the axons, RGCs, bipolar cells, and retinal blood vessels. A significant amount of light is absorbed by these structures before the light reaches the photoreceptor cells. However, at the exact center of the retina is a small region known as the macula lutea at which center there is a depression called the fovea (Figure \(\PageIndex{14}\)). In these regions, the retina lacks the supporting cells and blood vessels, and only contains cones. Therefore, visual acuity, or the sharpness of vision, is greatest at the fovea. As one moves in either direction from this central point of the retina, visual acuity drops significantly. In addition, each photoreceptor cell of the fovea is connected to a single RGC. Therefore, this RGC does not have to integrate inputs from multiple photoreceptors, which reduces the accuracy of visual transduction. Toward the edges of the retina, several photoreceptors converge on RGCs (through the bipolar cells) up to a ratio of 50 to 1. The difference in visual acuity between the fovea and peripheral retina is easily evidenced by looking directly at a word in the middle of this paragraph. The visual stimulus in the middle of the field of view falls on the fovea and is in the sharpest focus. Without moving your eyes off that word, notice that words at the beginning or end of the paragraph are not in focus. The images in your peripheral vision are focused by the peripheral retina, and have vague, blurry edges and words that are not as clearly identified. As a result, a large part of the neural function of the eyes is concerned with moving the eyes and head so that important visual stimuli are centered on the fovea.
Concept Review
Hearing and balance belong to the special senses and its specialized organ is the ear. The ear is divided in three regions: external, middle and inner ear. In the external ear, the auricle is the fleshy structure that convey sounds into the auditory canal. At the end of the canal is the tympanic membrane that vibrates and transforms sound waves into mechanical waves. The middle ear consists of a space spanned by three small bones called ossicles (malleus, incus, and stapes) that conduct the mechanical waves. The middle ear is connected to the pharynx through the Eustachian (or auditory) tube, which helps equilibrate air pressure across the tympanic membrane. The inner ear is made of a bony labyrinth lined with a membranous labyrinth that separate tubes and spaces. The space between the two labyrinths is filled with a fluid called perilymph. Inside the membranous labyrinth the space is filled with endolymph. The inner ear is responsible for transforming mechanical waves into electrical signals, which are then sent to the brain through the vestibulocochlear nerve (CN VIII).
The cochlea is a spiral-shaped tube, divided into three compartments: the scala vestibuli, scala tympani and cochlear duct. All compartments are filled with endolymph. The scala vestibuli starts at the oval window, curves over the top of the cochlear duct and becomes the scala tympani, that returns to the base of the cochlea, travelling under the cochlear duct and ends at the round window. As vibrations of the ossicles travel through the oval window, the fluid of the scala vestibuli and scala tympani moves in a wave-like motion. The cochlear duct contains several organs of Corti, which tranduce the wave motion of the two scala into neural signals. The organs of Corti lie on top of the basilar membrane, which is the side of the cochlear duct located between the organs of Corti and the scala tympani. The organs of Corti contain hair cells, which are named for the hair-like stereocilia extending from the cell’s apical surfaces. The stereocilia extend up from the hair cells to the overlying tectorial membrane, which is attached medially to the organ of Corti. When the pressure waves from the scala move the basilar membrane, the tectorial membrane slides across the stereocilia. This bends the stereocilia either toward or away from the tallest member of each array, which causes an electrical signal to be generated.
The vestibule and the semicircular canals are responsible for the sense of equilibrium. The vestibule is composed of the utricle and saccule. Hair cells are located in maculae of the utricle and saccule. The stereocilia of the hair cells extend into a viscous gel called the otolithic membrane, on top of which is a layer of calcium carbonate crystals, called otoliths. The vestibule senses the linear acceleration of the head and gravity. When the head moves, the otoliths move and the otolithic membrane bends the stereocilia of the hair cells. Hair cells are also located in ampullae at the base of the three semicircular canals. One is oriented in the horizontal plane, whereas the other two are oriented in the vertical plane. The stereocilia of these hair cells extend into the cupula, a membrane that attaches to the top of the ampulla. The semicircular canals sense the head rotation. As the head rotates in a plane parallel to the semicircular canal, the fluid lags, deflecting the cupula in the direction opposite to the head movement, and bending the stereocilia of the hair cells.
Vision belongs to the special senses and its specialized organ is the eye. The bony orbits, eyelids, tarsal glands and lacrimal apparatus protect the eyes. The inner eyelid is a thin membrane known as the palpebral conjunctiva. The conjunctiva connects the eyelids to the eyeball. At the connection with the eyeball, a thin layer called the ocular conjunctiva forms a continuous layer on the external and anterior surface of the eye (except for the corneal region), superior to the white part of the eye, the sclera. The conjunctiva contains blood vessels and nerves that support the avascular sclera and detect foreign particles entering the eye.
The lacrimal apparatus is responsible for the production and drainage of lacrimal fluid (tears). Tears reduce friction of the eyelids, continuously clean the anterior surface of the eye, and prevent bacterial infection through the action of lysozyme. Tears are produced by the lacrimal gland, located within the superolateral depression of each orbit. The superior and inferior lacrimal puncta are small openings to drain the lacrimal fluid into channels called the superior and inferior lacrimal canaliculi. From there, the lacrimal fluid enters the lacrimal sac and drains into the nasolacrimal duct that delivers it into the nasal cavity where it mixes with the mucus.
There are six extraocular muscles innervated by the abducens nerve (CN VI), trochlear nerve (CN IV) and oculomotor nerve (CN III). The superior rectus elevates the eye, the medial rectus adducts the eye, the inferior rectus depresses the eye, the lateral rectus abducts the eye. The superior oblique abducts, depresses, and internally rotates (intorsion) the eye. The inferior oblique abducts, elevates, and externally rotates (extorsion) the eye.
The eye walls are made by three layers of tissue called tunics. The fibrous tunic includes the white sclera and the clear cornea. The vascular tunic composed of the choroid, ciliary body attached to the lens by suspensory ligaments and iris (colored part of the eye). The iris is composed of pigmented layers and two layers of smooth muscle called the sphincter pupillae and dilator pupillae, that open and close the pupil. The neural tunic (or retina) includes a pigmented layer and a neural layer that contains the photoreceptors. The eye is divided in two cavities: the anterior cavity between the cornea and lens, filled with aqueous humor, and the posterior cavity behind the lens, filled with vitreous humor. The retina is composed of several layers of cells, connected to each other, that support vision transduction. The photoreceptors are rods for light vision and cones for color vision. Retinal ganglion cells (RGCs) have axons that collect at the optic disc and leave the eye as the optic nerve (CN II). At the exact center of the retina is a small area known as the macula lutea with a depression in the middle called the fovea. At the fovea, the retina lacks the supporting cells and blood vessels, and only contains cones. Therefore, visual acuity, or the sharpness of vision, is greatest at the fovea.
Review Questions
Q. Axons from which neuron in the retina make up the optic nerve?
A. amacrine cells
B. photoreceptors
C. bipolar cells
D. retinal ganglion cells
- Answer
-
D
Q. What type of receptor cell is involved in the sensations of sound and balance?
A. photoreceptor
B. chemoreceptor
C. mechanoreceptor
D. nociceptor
- Answer
-
C
Glossary
- abducens nerve
- sixth cranial nerve; responsible for contraction of one of the extraocular muscles
- amacrine cell
- type of cell in the retina that connects to the bipolar cells near the outer synaptic layer and provides the basis for early image processing within the retina
- ampulla
- in the ear, the structure at the base of a semicircular canal that contains the hair cells and cupula for transduction of rotational movement of the head
- anterior cavity
- space of the eye between the cornea and the lens
- anterior chamber
- space within the anterior cavity of the eye that is anterior to the iris
- aqueous humor
- watery fluid that fills the anterior chamber containing the cornea, iris, ciliary body, and lens of the eye
- audition
- sense of hearing
- auditory canal
- passageway of the external ear that leads to the tympanic membrane; also known as ear canal
- auditory tube
- tube that connects the nasopharynx to the middle ear; also known as Eustachian tube
- auricle
- fleshy external structure of the ear
- basilar membrane
- in the ear, the floor of the cochlear duct on which the organ of Corti sits
- bipolar cell
- cell type in the retina that connects the photoreceptors to the RGCs
- bony labyrinth
- complex cavities in the inner ear made by bones
- brainstem
- region of the adult brain that includes the midbrain, pons, and medulla oblongata and develops from the mesencephalon, metencephalon, and myelencephalon of the embryonic brain
- cerebellum
- region of the adult brain connected primarily to the pons that developed from the metencephalon (along with the pons) and is largely responsible for comparing information from the cerebrum with sensory feedback from the periphery through the spinal cord
- cerebral nuclei
- deep gray matter of the cerebrum
- choroid
- highly vascular tissue in the wall of the eye that supplies the outer retina with blood
- ciliary body
- smooth muscle structure on the interior surface of the iris that controls the shape of the lens through the zonule fibers
- ciliary process
- vascular fold of the inner ciliary body that produce aqueous humor
- cochlea
- auditory portion of the inner ear containing structures to transduce sound stimuli
- cochlear duct
- space within the auditory portion of the inner ear that contains the organ of Corti and is adjacent to the scala tympani and scala vestibuli on either side
- cochlear nerve
- branch of the vestibulocochlear nerve projecting from the cochlea
- common tendinous ring
- ring of fibrous tissue surrounding the optic nerve at its entrance at the apex of the orbit
- cone photoreceptor
- one of the two types of retinal receptor cell that is specialized for color vision through the use of three photopigments distributed through three separate populations of cells
- cornea
- fibrous covering of the anterior region of the eye that is transparent so that light can pass through it
- cupula
- specialized structure within the base of a semicircular canal that bends the stereocilia of hair cells when the head rotates by way of the relative movement of the enclosed fluid
- dilator pupillae
- outer smooth muscle of the iris whose contraction increases the size of the pupil
- ear canal
- passageway of the external ear that leads to the tympanic membrane; also known as auditory canal
- endolymph
- fluid in the membranous labyrinth of the ear
- endolymphatic duct
- canal filled with endolymph connecting the utricle and saccule
- equilibrium
- sense of balance that includes sensations of position and movement of the head
- Eustachian tube
- tube that connects the nasopharynx to the middle ear; also known as auditory tube
- external ear
- structures on the lateral surface of the head, including the auricle and the ear canal back to the tympanic membrane
- extraocular muscle
- one of six muscles originating out of the bones of the orbit and inserting into the surface of the eye which are responsible for moving the eye
- fibrous tunic
- outer layer of the eye primarily composed of connective tissue known as the sclera and cornea
- fovea
- exact center of the retina at which visual stimuli are focused for maximal acuity, where the retina is thinnest, at which there is nothing but photoreceptors
- hair cells
- mechanoreceptor cells found in the inner ear that transduce stimuli for the senses of hearing and balance
- horizontal cell
- lateral interconnecting neurons of the retina
- incus
- (also, anvil) ossicle of the middle ear that connects the malleus to the stapes
- inferior oblique
- extraocular muscle responsible for lateral rotation of the eye
- inferior rectus
- extraocular muscle responsible for looking down
- inner ear
- structure within the temporal bone that contains the sensory apparati of hearing and balance
- iris
- colored portion of the anterior eye that surrounds the pupil
- lacrimal canaliculus
- duct in the medial corner of the orbit that drains tears into the nasal cavity
- lacrimal gland
- gland lateral to the orbit that produces tears to wash across the surface of the eye
- lacrimal punctum
- opening of the lacrimal canaliculus
- lacrimal sac
- superior end of the nasolacrimal duct
- lateral rectus
- extraocular muscle responsible for abduction of the eye
- lens
- component of the eye that focuses light on the retina
- levator palpebrae superioris
- muscle that causes elevation of the upper eyelid, controlled by fibers in the oculomotor nerve
- macula
- enlargement at the base of a semicircular canal at which transduction of equilibrium stimuli takes place within the ampulla
- macula lutea
- area surrounding the fovea near the center of the retina in the eye, which is the region of sharpest vision
- malleus
- (also, hammer) ossicle that is directly attached to the tympanic membrane
- medial rectus
- extraocular muscle responsible for adduction of the eye
- membranous labyrinth
- membranes of the the inner ear that line the bony labyrinth
- middle ear
- space within the temporal bone between the ear canal and bony labyrinth where the ossicles amplify sound waves from the tympanic membrane to the oval window
- nasolacrimal duct
- tube that connects the lacrimal sac to the nasal cavity
- neural layer
- one of the two layers of the neural tunic of the eye
- neural tunic
- layer of the eye that contains nervous tissue, namely the retina
- ocular conjunctiva
- part of the conjunctiva which covers the outer surface of the eye
- oculomotor nerve
- third cranial nerve; responsible for contraction of four of the extraocular muscles, the muscle in the upper eyelid, and pupillary constriction
- optic disc
- spot on the retina at which RGC axons leave the eye and blood vessels of the inner retina pass
- optic nerve
- second cranial nerve, which is responsible visual sensation
- organ of Corti
- structure in the cochlea in which hair cells transduce movements from sound waves into electrochemical signals
- ossicles
- three small bones in the middle ear
- otolith
- layer of calcium carbonate crystals located on top of the otolithic membrane
- otolithic membrane
- gelatinous substance in the utricle and saccule of the inner ear that contains calcium carbonate crystals and into which the stereocilia of hair cells are embedded
- oval window
- membrane at the base of the cochlea where the stapes attaches, marking the beginning of the scala vestibuli
- palpebral conjunctiva
- membrane attached to the inner surface of the eyelids that covers the anterior surface of the cornea
- perilymph
- fluid between the membranous labyrinth of the ear and the bony labyrinth
- pigmented layer
- one of the two layers of the neural tunic of the eye
- posterior cavity
- space of the eye posterior to the lens
- posterior chamber
- space within the anterior cavity of the eye that is posterior to the iris
- primary auditory cortex
- region of the cerebral cortex within the temporal lobe responsible for the perception of sounds
- primary visual cortex
- region of the cerebral cortex within the occipital lobe responsible for the perception of vision
- pupil
- open hole at the center of the iris that light passes through into the eye
- retina
- nervous tissue of the eye at which phototransduction takes place
- retinal ganglion cell (RGC)
- neuron of the retina that projects along the second cranial nerve
- rod photoreceptor
- one of the two types of retinal receptor cell that is specialized for low-light vision
- round window
- membrane that marks the end of the scala tympani
- saccule
- structure of the inner ear responsible for transducing linear acceleration in the vertical plane
- scala tympani
- portion of the cochlea that extends from the apex to the round window
- scala vestibuli
- portion of the cochlea that extends from the oval window to the apex
- sclera
- white of the eye
- scleral venous sinus
- circular channel in the eye that collects aqueous humor from the anterior chamber
- semicircular canals
- structures within the inner ear responsible for transducing rotational movement information
- sphincter pupillae
- inner smooth muscle of the iris whose contraction decreases the size of the pupil
- spiral ganglion
- location of neuronal cell bodies that transmit auditory information along the eighth cranial nerve
- stapes
- (also, stirrup) ossicle of the middle ear that is attached to the inner ear
- stereocilia
- array of apical membrane extensions in a hair cell that transduce movements when they are bent
- superior oblique
- extraocular muscle responsible for medial rotation of the eye
- superior rectus
- extraocular muscle responsible for looking up
- supporting cells
- cells that support the hair cells in the macula
- suspensory ligaments
- fibers that connect the ciliary body of the eye with the lens, holding it in place
- tarsal gland
- gland within the eyelid that produces an oily substance
- tarsal muscle
- smooth muscle that helps to raise the upper eyelid
- tectorial membrane
- component of the organ of Corti that lays over the hair cells, into which the stereocilia are embedded
- thalamus
- major region of the diencephalon that is responsible for relaying information between the cerebrum and the hindbrain, spinal cord, and periphery
- trochlea
- cartilaginous structure that acts like a pulley for the superior oblique muscle
- trochlear nerve
- fourth cranial nerve; responsible for contraction of one of the extraocular muscles
- tympanic membrane
- ear drum
- utricle
- structure of the inner ear responsible for transducing linear acceleration in the horizontal plane
- vascular tunic
- middle layer of the eye primarily composed of connective tissue with a rich blood supply
- vestibular membrane
- membrane separating the cochlear duct and scala vestibuli
- vestibular nerve
- branch of the vestibulocochlear nerve projecting from the vestibule
- vestibular system
- system composed of the vestibule and semicircular canals to sense equilibrium
- vestibule
- in the ear, the portion of the inner ear responsible for the sense of equilibrium
- vestibulocochlear nerve
- eighth cranial nerve; responsible for the sensations of hearing and balance
- vision
- special sense of sight based on transduction of light stimuli
- visual acuity
- property of vision related to the sharpness of focus, which varies in relation to retinal position
- vitreous humor
- viscous fluid that fills the posterior chamber of the eye
Contributors and Attributions
OpenStax Anatomy & Physiology (CC BY 4.0). Access for free at https://openstax.org/books/anatomy-and-physiology


