15.2: An Overview of the Endocrine System
- Page ID
- 22354
By the end of this section, you will be able to:
- Distinguish the types of intercellular communication and their importance
- Identify the major organs and tissues of the endocrine system and their location in the body
- Explain the role of hormones in controlling body functions via the bloodstream
- Discuss the role of feedback loops in hormone control
Communication is a process in which a sender transmits signals to one or more receivers to control and coordinate actions. In the human body, two major organ systems participate in relatively “long distance” communication: the nervous system and the endocrine system. Together, these two systems are primarily responsible for maintaining homeostasis in the body.
Neural and Endocrine Signaling
The nervous system uses two types of intercellular communication—electrical and chemical signaling—either by the direct action of an electrical potential, or in the latter case, through the action of chemical neurotransmitters such as serotonin or norepinephrine. In a synapse, neurotransmitters act locally and rapidly. When an electrical signal in the form of an action potential arrives at the synaptic terminal, neurotransmitters diffuse across the synaptic cleft (the gap between a sending neuron and a receiving cell). Once the neurotransmitters interact (bind) with receptors on the receiving (post-synaptic) cell, the receptor stimulation is transduced into a response such as continued electrical signaling or modification of cellular response. The target cell responds within milliseconds of receiving the chemical “message”; this response then ceases very quickly once the neural signaling ends. In this way, neural communication enables body functions that involve quick, brief actions, such as movement, sensation, and cognition.
In contrast, the endocrine system uses just one method of communication: chemical signaling. These signals are sent by the endocrine organs, which secrete chemicals—the hormone—into the extracellular fluid. Hormones are transported primarily via the bloodstream throughout the body, where they bind to receptors on target cells, inducing a characteristic response. As a result, endocrine signaling requires more time than neural signaling to prompt a response in target cells, though the precise amount of time varies with different hormones. For example, the hormones released when you are confronted with a dangerous or frightening situation, called the fight-or-flight response, occur by the release of adrenal hormones—epinephrine and norepinephrine—within seconds. In contrast, it may take up to 48 hours for target cells to respond to certain reproductive hormones.
In addition, endocrine signaling is typically less specific than neural signaling. The same hormone may play a role in a variety of different physiological processes depending on the target cells involved. For example, the hormone oxytocin promotes uterine contractions in women during labor. It is also important in breastfeeding, and may be involved in the sexual response and in feelings of emotional attachment in both males and females.
In general, the nervous system involves quick responses to rapid changes in the external environment, and the endocrine system is usually slower acting—taking care of the internal environment of the body, maintaining homeostasis, and controlling reproduction (Table \(\PageIndex{1}\)). So how does the fight-or-flight response that was mentioned earlier happen so quickly if hormones are usually slower acting? It is because the two systems are connected. It is the fast action of the nervous system in response to the danger in the environment that stimulates the adrenal glands to secrete their hormones. As a result, the nervous system can cause rapid endocrine responses to keep up with sudden changes in both the external and internal environments when necessary.
| Endocrine system | Nervous system | |
|---|---|---|
| Signaling mechanism(s) | Chemical | Chemical/electrical |
| Primary chemical signal | Hormones | Neurotransmitters |
| Distance traveled | Long or short | Always short |
| Response time | Fast or slow | Always fast |
Structures of the Endocrine System
The endocrine system consists of cells, tissues, and organs that secrete hormones as a primary or secondary function. The endocrine gland is the major player in this system. The primary function of these ductless glands is to secrete their hormones directly into the surrounding fluid. The interstitial fluid and the blood vessels then transport the hormones throughout the body. The endocrine system includes the pituitary, thyroid, parathyroid, adrenal, and pineal glands (summarized in Figure \(\PageIndex{1}\) and covered in more detail in subsequent sections of this chapter). Some glands have both endocrine and non-endocrine functions. For example, the pancreas contains cells that function in digestion as well as cells that secrete the hormones insulin and glucagon, which regulate blood glucose levels. The hypothalamus, thymus, heart, kidneys, stomach, small intestine, liver, skin, female ovaries, and male testes are other organs that contain cells with endocrine function. Moreover, adipose tissue has long been known to produce hormones, and recent research has revealed that even bone tissue has endocrine functions.
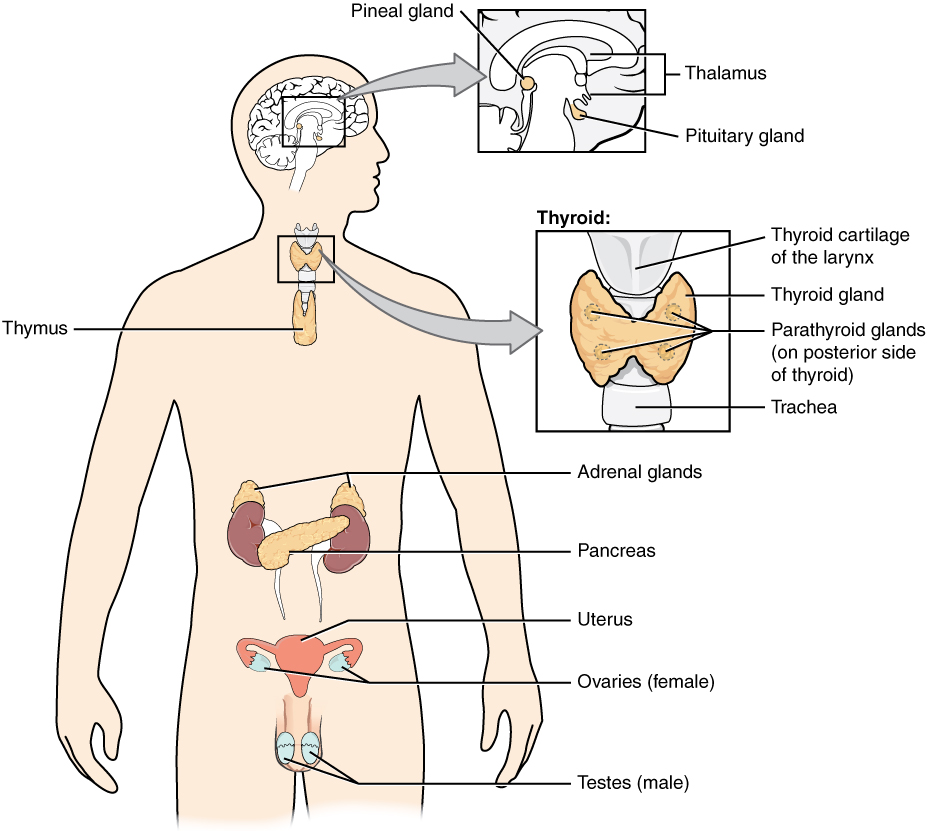
The ductless endocrine glands are not to be confused with the body’s exocrine system, whose glands release their secretions through ducts. Examples of exocrine glands include the sebaceous and sweat glands of the skin. As just noted, the pancreas also has an exocrine function: most of its cells secrete pancreatic juice through the pancreatic and accessory ducts to the lumen (inside) of the small intestine.
Other Types of Chemical Signaling
In endocrine signaling, hormones secreted into the extracellular fluid diffuse into the blood or lymph (fluid of the lymphatic system), and can then travel great distances throughout the body. In contrast, autocrine signaling takes place within the same cell. An autocrine (auto- = “self”) is a chemical that elicits a response in the same cell that secreted it. Interleukin-1, or IL-1, is a signaling molecule that plays an important role in the inflammatory response. The cells that secrete IL-1 have receptors on their cell surface that bind these molecules, resulting in autocrine signaling.
Local intercellular communication is carried out by a paracrine, also called a paracrine factor, which is a chemical that induces a response in neighboring cells within the same tissue. Although paracrine hormones may enter the bloodstream, their concentration is generally too low to elicit a response from distant tissues. Histamine, released by immune cells of the bronchial tree, is a familiar example of a paracrine that is harmful to people with asthma. Histamine causes the walls of the bronchi to become inflamed and causes the smooth muscle cells of the bronchi to constrict, narrowing the airways. Neurotransmitters of the nervous system, acting locally within the synaptic cleft, are another example of paracrine signaling.
Hormones
Although a given hormone may travel throughout the body in the bloodstream, it will affect the activity only of its target cells; that is, cells with receptors for that particular hormone. Once the hormone binds to the receptor, a chain of events is initiated that leads to the target cell’s response. Hormones play a critical role in the regulation of physiological processes because of the target cell responses they regulate. These responses contribute to human reproduction, growth and development of body tissues, metabolism, fluid and electrolyte balance, sleep, and many other body functions. The major hormones of the human body and their effects are identified in Table \(\PageIndex{2}\).
| Endocrine gland | Associated hormones | Effect |
|---|---|---|
| Pituitary (anterior) | Growth hormone (GH) | Promotes growth of body tissues |
| Pituitary (anterior) | Prolactin (PRL) | Promotes milk production |
| Pituitary (anterior) | Thyroid-stimulating hormone (TSH) | Stimulates thyroid hormone release |
| Pituitary (anterior) | Adrenocorticotropic hormone (ACTH) | Stimulates glucocorticoid release by adrenal cortex |
| Pituitary (anterior) | Follicle-stimulating hormone (FSH) | Stimulates gamete (egg or sperm) production |
| Pituitary (anterior) | Luteinizing hormone (LH) | Stimulates androgen production by gonads |
| Pituitary (posterior) | Antidiuretic hormone (ADH; aka vasopressin) | Stimulates water reabsorption by kidneys |
| Pituitary (posterior) | Oxytocin | Stimulates uterine contractions during childbirth |
| Thyroid | Thyroxine (T4), triiodothyronine (T3) | Stimulate basal metabolic rate |
| Thyroid | Calcitonin | Reduces blood Ca2+ levels |
| Parathyroid | Parathyroid hormone (PTH) | Increases blood Ca2+ levels |
| Adrenal (cortex) | Aldosterone | Increases blood Na+ levels |
| Adrenal (cortex) | Cortisol, corticosterone, cortisone | Increase blood glucose levels, involved in stress response |
| Adrenal (medulla) | Epinephrine, norepinephrine | Stimulate fight-or-flight response |
| Pineal | Melatonin | Regulates sleep cycles |
| Pancreas | Insulin | Reduces blood glucose levels |
| Pancreas | Glucagon | Increases blood glucose levels |
| Testes | Testosterone | Stimulates development of male secondary sex characteristics and sperm production |
| Ovaries | Estrogens and progesterone | Stimulate development of female secondary sex characteristics and prepare the body for childbirth |
Types of Hormones
The hormones of the human body can be divided into two major groups on the basis of their chemical properties: hormones that are soluble in water, most of which are derived from amino acids (the building blocks of proteins), and steroid hormones, which are not soluble in water as they are derived from the lipid cholesterol. The chemical properties of the hormones in each group affect much of how they work including how they are distributed to target cells, the type of receptors they bind to, and other aspects of function such as how long effects can last.
Pathways of Hormone Action
The message a hormone sends is received by a hormone receptor, a protein located either inside the cell or within the cell membrane. The receptor will process the message by initiating other signaling events or cellular mechanisms that result in the target cell’s response. Hormone receptors recognize molecules with specific shapes and side groups, and respond only to those hormones that are recognized. The same type of receptor may be located on cells in different body tissues, and trigger somewhat different responses. Thus, the response triggered by a hormone depends not only on the hormone, but also on the target cell.
Once the target cell receives the hormone signal, it can respond in a variety of ways. The response may include the stimulation of protein synthesis, activation or deactivation of enzymes, alteration in the permeability of the cell membrane, altered rates of mitosis and cell growth, and stimulation of the secretion of products. Moreover, a single hormone may be capable of inducing different responses in a given cell.
Regulation of Hormone Secretion
To prevent abnormal hormone levels and a potential disease state, hormone levels must be tightly controlled. The body maintains this control by balancing hormone production and degradation. Feedback loops govern the initiation and maintenance of most hormone secretion in response to various stimuli.
Role of Feedback Loops
The contribution of feedback loops to homeostasis will only be briefly reviewed here. Positive feedback loops are characterized by the release of additional hormone in response to an original hormone release. The release of oxytocin during childbirth is a positive feedback loop. The initial release of oxytocin begins to signal the uterine muscles to contract, which pushes the fetus toward the cervix, causing it to stretch. This, in turn, signals the pituitary gland to release more oxytocin, causing labor contractions to intensify. The release of oxytocin decreases after the birth of the child.
The more common method of hormone regulation is the negative feedback loop. Negative feedback is characterized by the inhibition of further secretion of a hormone in response to adequate levels of that hormone. This allows blood levels of the hormone to be regulated within a narrow range. An example of a negative feedback loop is the release of glucocorticoid hormones from the adrenal glands, as directed by the hypothalamus and pituitary gland. Glucocorticoids such as cortisol help the body respond to stress. If glucocorticoid concentrations in the blood fall below optimal, as measured by sensors in the bloodstream, the hypothalamus releases corticotropin-releasing hormone (CRH). The release of CRH signals the pituitary gland to initiate a cascade of hormone releases that ultimately signal the adrenal gland (aka suprarenal gland) to release glucocorticoids into the bloodstream. As glucocorticoid concentrations in the blood rise, the hypothalamus and pituitary gland reduce their signaling to the adrenal glands to prevent additional glucocorticoid secretion (Figure \(\PageIndex{2}\)).
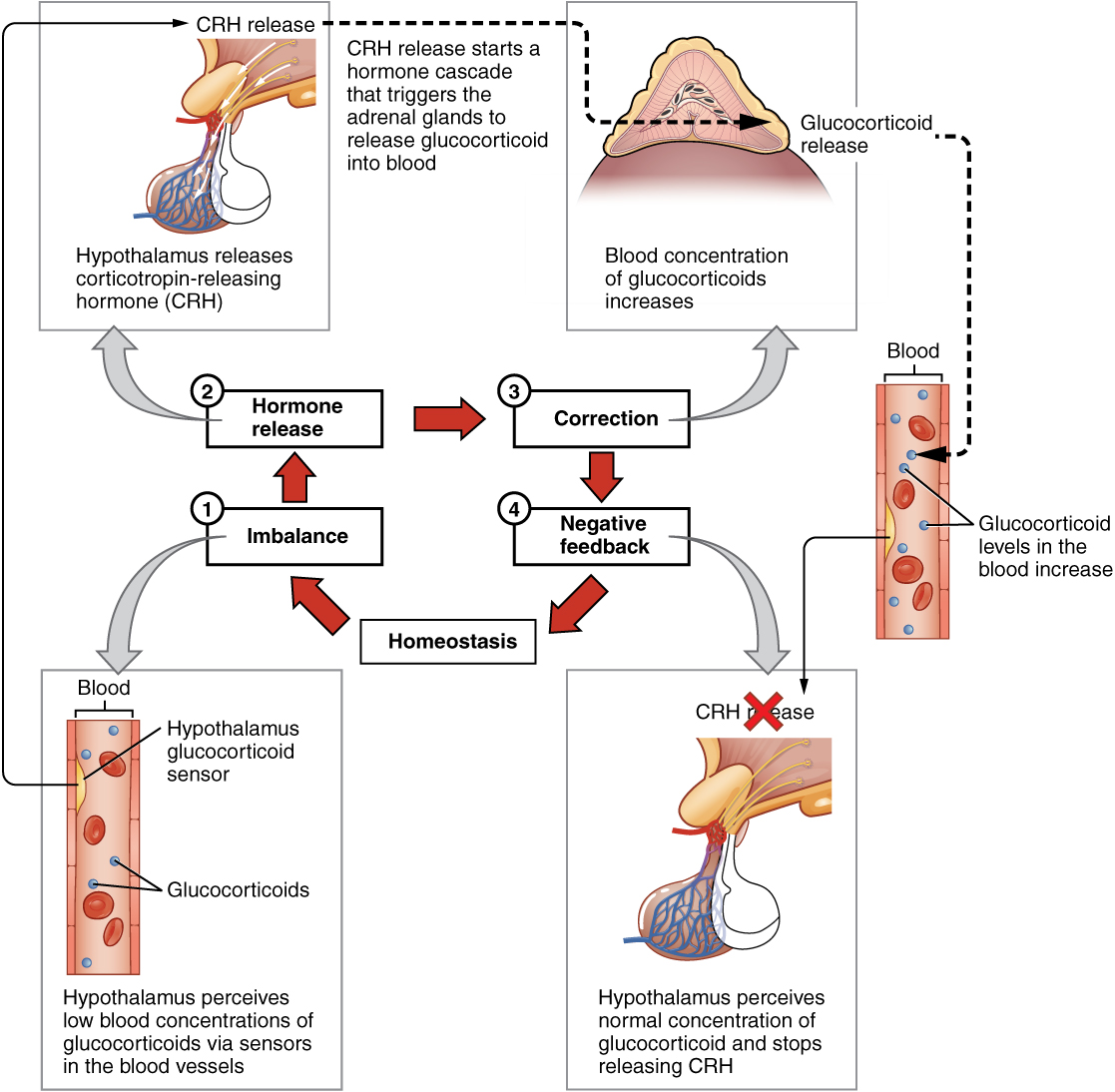
Role of Endocrine Gland Stimuli
Reflexes triggered by both chemical and neural stimuli control endocrine activity. These reflexes may be simple, involving only one hormone response, or they may be more complex and involve many hormones, as is the case with the hypothalamic control of various anterior pituitary–controlled hormones.
Humoral stimuli are changes in blood levels of nutrients, ions, or other non-hormonal chemicals that cause the release or inhibition of a hormone to maintain homeostasis. For example, osmoreceptors in the hypothalamus detect changes in blood osmolarity (the concentration of solutes in the blood plasma). If blood osmolarity is too high, meaning that the blood is not dilute enough, osmoreceptors signal the hypothalamus to release ADH. The hormone causes the kidneys to reabsorb more water and reduce the volume of urine produced. This reabsorption causes a reduction of the osmolarity of the blood, diluting the blood to the appropriate level. The regulation of blood glucose is another example. High blood glucose levels cause the release of insulin from the pancreas, which increases glucose uptake by cells and liver storage of glucose as glycogen.
An endocrine gland may also secrete a hormone in response to the presence of another hormone produced by a different endocrine gland. Such hormonal stimuli often involve the hypothalamus, which produces releasing and inhibiting hormones that control the secretion of a variety of pituitary hormones.
In addition to these chemical signals, hormones can also be released in response to neural stimuli. A common example of neural stimuli is the activation of the fight-or-flight response by the sympathetic nervous system. When an individual perceives danger, sympathetic neurons signal the adrenal glands to secrete norepinephrine and epinephrine. The two hormones dilate blood vessels, increase the heart and respiratory rate, and suppress the digestive and immune systems. These responses boost the body’s transport of oxygen to the brain and muscles, thereby improving the body’s ability to fight or flee.
EVERYDAY CONNECTIONS
Bisphenol A and Endocrine Disruption
You may have heard news reports about the effects of a chemical called bisphenol A (BPA) in various types of food packaging. BPA is used in the manufacturing of hard plastics and epoxy resins. Common food-related items that may contain BPA include the lining of aluminum cans, plastic food-storage containers, drinking cups, as well as baby bottles and “sippy” cups. Other uses of BPA include medical equipment, dental fillings, and the lining of water pipes.
Research suggests that BPA is an endocrine disruptor, meaning that it negatively interferes with the endocrine system, particularly during the prenatal and postnatal development period. In particular, BPA mimics the hormonal effects of estrogens and has the opposite effect—that of androgens. The U.S. Food and Drug Administration (FDA) notes in their statement about BPA safety that although traditional toxicology studies have supported the safety of low levels of exposure to BPA, recent studies using novel approaches to test for subtle effects have led to some concern about the potential effects of BPA on the brain, behavior, and prostate gland in fetuses, infants, and young children. The FDA is currently facilitating decreased use of BPA in food-related materials. Many US companies have voluntarily removed BPA from baby bottles, “sippy” cups, and the linings of infant formula cans, and most plastic reusable water bottles sold today boast that they are “BPA free.” In contrast, both Canada and the European Union have completely banned the use of BPA in baby products.
The potential harmful effects of BPA have been studied in both animal models and humans and include a large variety of health effects, such as developmental delay and disease. For example, prenatal exposure to BPA during the first trimester of human pregnancy may be associated with wheezing and aggressive behavior during childhood. Adults exposed to high levels of BPA may experience altered thyroid signaling and male sexual dysfunction. BPA exposure during the prenatal or postnatal period of development in animal models has been observed to cause neurological delays, changes in brain structure and function, sexual dysfunction, asthma, and increased risk for multiple cancers. In vitro studies have also shown that BPA exposure causes molecular changes that initiate the development of cancers of the breast, prostate, and brain. Although these studies have implicated BPA in numerous ill health effects, some experts caution that some of these studies may be flawed and that more research needs to be done. In the meantime, the FDA recommends that consumers take precautions to limit their exposure to BPA. In addition to purchasing foods in packaging free of BPA, consumers should avoid carrying or storing foods or liquids in bottles with the recycling code 3 or 7. Foods and liquids should not be microwave-heated in any form of plastic: use paper, glass, or ceramics instead.
CAREER CONNECTIONS
Endocrinologist
Endocrinology is a specialty in the field of medicine that focuses on the treatment of endocrine system disorders. Endocrinologists—medical doctors who specialize in this field—are experts in treating diseases associated with hormonal systems, ranging from thyroid disease to diabetes mellitus. Endocrine surgeons treat endocrine disease through the removal, or resection, of the affected endocrine gland.
Patients who are referred to endocrinologists may have signs and symptoms or blood test results that suggest excessive or impaired functioning of an endocrine gland or endocrine cells. The endocrinologist may order additional blood tests to determine whether the patient’s hormonal levels are abnormal, or they may stimulate or suppress the function of the suspect endocrine gland and then have blood taken for analysis. Treatment varies according to the diagnosis. Some endocrine disorders, such as type 2 diabetes, may respond to lifestyle changes such as modest weight loss, adoption of a healthy diet, and regular physical activity. Other disorders may require medication, such as hormone replacement, and routine monitoring by the endocrinologist. These include disorders of the pituitary gland that can affect growth and disorders of the thyroid gland that can result in a variety of metabolic problems.
Some patients experience health problems as a result of the normal decline in hormones that can accompany aging. These patients can consult with an endocrinologist to weigh the risks and benefits of hormone replacement therapy intended to boost their natural levels of reproductive hormones.
In addition to treating patients, endocrinologists may be involved in research to improve the understanding of endocrine system disorders and develop new treatments for these diseases.
Concept Review
The endocrine system consists of cells, tissues, and organs that secrete hormones critical to homeostasis. The body coordinates its functions through two major types of communication: neural and endocrine. Neural communication includes both electrical and chemical signaling between neurons and target cells. Endocrine communication involves chemical signaling via the release of hormones into the extracellular fluid. From there, hormones diffuse into the bloodstream and may travel to distant body regions, where they elicit a response in target cells. Endocrine glands are ductless glands that secrete hormones. Many organs of the body with other primary functions—such as the heart, stomach, and kidneys—also have hormone-secreting cells.
Hormones are released upon stimulation that is of either chemical or neural origin. Regulation of hormone release is primarily achieved through negative feedback. Various stimuli may cause the release of hormones, but there are three major types. Humoral stimuli are changes in ion or nutrient levels in the blood. Hormonal stimuli are changes in hormone levels that initiate or inhibit the secretion of another hormone. Finally, a neural stimulus occurs when a nerve impulse prompts the secretion or inhibition of a hormone.
Review Questions
Q. Endocrine glands ________.
A. secrete hormones that travel through a duct to the target organs
B. release neurotransmitters into the synaptic cleft
C. secrete chemical messengers that travel in the bloodstream
D. include sebaceous glands and sweat glands
- Answer
-
Answer: C
Q. Chemical signaling that affects neighboring cells is called ________.
A. autocrine
B. paracrine
C. endocrine
D. neuron
- Answer
-
Answer: B
Q. A student is in a car accident, and although not hurt, immediately experiences pupil dilation, increased heart rate, and rapid breathing. What type of endocrine system stimulus did the student receive?
A. humoral
B. hormonal
C. neural
D. positive feedback
- Answer
-
Answer: C
Critical Thinking Questions
Q. Describe several main differences in the communication methods used by the endocrine system and the nervous system.
- Answer
-
A. The endocrine system uses chemical signals called hormones to convey information from one part of the body to a distant part of the body. Hormones are released from the endocrine cell into the extracellular environment, but then travel in the bloodstream to target tissues. This communication and response can take seconds to days. In contrast, neurons transmit electrical signals along their axons. At the axon terminal, the electrical signal prompts the release of a chemical signal called a neurotransmitter that carries the message across the synaptic cleft to elicit a response in the neighboring cell. This method of communication is nearly instantaneous, of very brief duration, and is highly specific.
Q. Compare and contrast endocrine and exocrine glands.
- Answer
-
A. Endocrine glands are ductless. They release their secretion into the surrounding fluid, from which it enters the bloodstream or lymph to travel to distant cells. Moreover, the secretions of endocrine glands are hormones. Exocrine glands release their secretions through a duct that delivers the secretion to the target location. Moreover, the secretions of exocrine glands are not hormones, but compounds that have an immediate physiologic function. For example, pancreatic juice contains enzymes that help digest food.
Q. True or false: Neurotransmitters are a special class of paracrines. Explain your answer.
- Answer
-
A. True. Neurotransmitters can be classified as paracrines because, upon their release from a neuron’s axon terminals, they travel across a microscopically small cleft to exert their effect on a nearby neuron or muscle cell.
Glossary
- autocrine
- chemical signal that elicits a response in the same cell that secreted it
- endocrine gland
- tissue or organ that secretes hormones into the blood and lymph without ducts such that they may be transported to organs distant from the site of secretion
- endocrine system
- cells, tissues, and organs that secrete hormones as a primary or secondary function and play an integral role in normal bodily processes
- exocrine system
- cells, tissues, and organs that secrete substances directly to target tissues via glandular ducts
- hormonal stimuli
- the presence of a hormone causes the release or inhibition of another hormone in an endocrine gland
- hormone receptor
- protein within a cell or on the cell membrane that binds a hormone, initiating the target cell response
- hormone
- secretion of an endocrine organ that travels via the bloodstream or lymphatics to induce a response in target cells or tissues in another part of the body
- humoral stimuli
- changes in blood levels of non-hormone chemicals such as ions or nutrients that cause release or inhibition of a hormone to maintain homeostasis of the chemical
- negative feedback loop
- type of regulation in which increasing levels of a substance signal that the substance no longer needs to be released, resulting in lowered levels of the substance
- neural stimuli
- a nerve impulse causes the release or inhibition of a hormone in an endocrine gland
- paracrine
- chemical signal that elicits a response in neighboring cells; also called paracrine factor
Contributors and Attributions
OpenStax Anatomy & Physiology (CC BY 4.0). Access for free at https://openstax.org/books/anatomy-and-physiology


