16.4: Leukocytes and Platelets
- Page ID
- 22370
By the end of this section, you will be able to:
- Describe the general characteristics of leukocytes
- Classify leukocytes according to their lineage, their main structural features, and their primary functions
- Discuss the most common malignancies involving leukocytes
- Identify the lineage, basic structure, and function of platelets
Leukocytes
The leukocyte, commonly known as a white blood cell (or WBC), is a major component of the body’s defenses against disease. Leukocytes protect the body against invading microorganisms and body cells with mutated DNA, and they clean up debris. You may find it helpful to reference the image Formed Elements in a Blood Sample (Figure 16.3.1) and the Table 16.2.2 Summary of Formed Elements in Blood along with this content.
Characteristics of Leukocytes
Although leukocytes and erythrocytes both originate from hematopoietic stem cells in the red bone marrow, they are very different from each other in many significant ways. For instance, leukocytes are far less numerous than erythrocytes; typically there are only 5000 to 10,000 per µL. They are also larger than erythrocytes and are the only formed elements that are complete cells in circulation, possessing a nucleus and organelles. Although there is just one type of erythrocyte, there are many types of leukocytes. Most of these types have a much shorter lifespan than that of erythrocytes, some as short as a few hours, or even a few minutes in the case of acute infection.
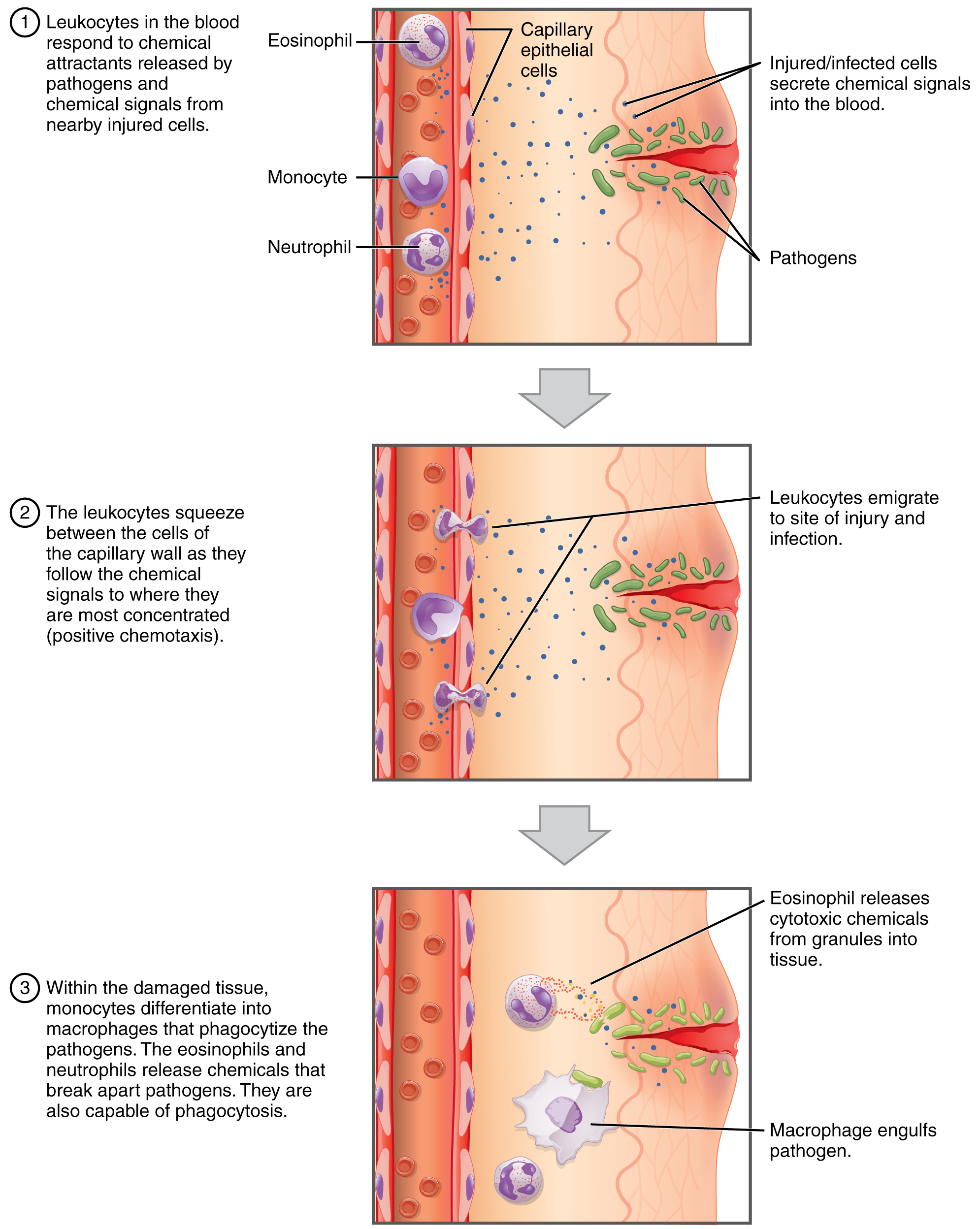
One of the most distinctive characteristics of leukocytes is their movement. Whereas erythrocytes spend their days circulating within the blood vessels, leukocytes routinely leave the bloodstream to perform their defensive functions in the body’s tissues. For leukocytes, the vascular network is often simply a highway they travel and soon exit to reach their true destination. When they arrive, they may differentiate further and be given distinct names, such as macrophage or microglia, depending on their function. As shown in Figure \(\PageIndex{1}\), they leave the capillaries—the smallest blood vessels—or other small vessels through a process known as emigration (from the Latin for “removal”) or diapedesis (dia- = “through”; -pedan = “to leap”) in which they squeeze through adjacent cells in a blood vessel wall.
Once they have exited the capillaries, some leukocytes will take up residence in lymphatic tissue, bone marrow, the spleen, the thymus, or other organs. Others will move about through the tissue spaces very much like amoebae, continuously extending their plasma membranes, sometimes wandering freely, and sometimes moving toward the direction in which they are drawn by chemical signals. This attracting of leukocytes occurs because of positive chemotaxis (literally “movement in response to chemicals”), a phenomenon in which injured or infected cells and nearby leukocytes emit the equivalent of a chemical “911” call, attracting more leukocytes to the site. In clinical medicine, the differential counts of the types and percentages of leukocytes present are often key indicators in making a diagnosis and selecting a treatment.
Classification of Leukocytes
When scientists first began to observe stained blood slides, it quickly became evident that leukocytes could be divided into two groups, according to whether their cytoplasm contained highly visible granules:
- Granular leukocytes (granulocytes) contain abundant granules within the cytoplasm. They include neutrophils, eosinophils, and basophils (you can view their lineage from myeloid stem cells in Figure 16.5.1 Hemopoietic System of Bone Marrow).
- While granules are not totally lacking in agranular leukocytes (agranulocytes), they are far fewer and less obvious. Agranular leukocytes include monocytes, which also arise from myeloid stem cells and mature into macrophages that are phagocytic, and lymphocytes, which arise from the lymphoid stem cell line.
Granular Leukocytes
We will consider the granular leukocytes (granulocytes) in order from most common to least common. All of these are produced in the red bone marrow and have a short lifespan of hours to days. They typically have a lobed nucleus and are classified according to which type of stain best highlights their granules (Figure \(\PageIndex{2}\)).
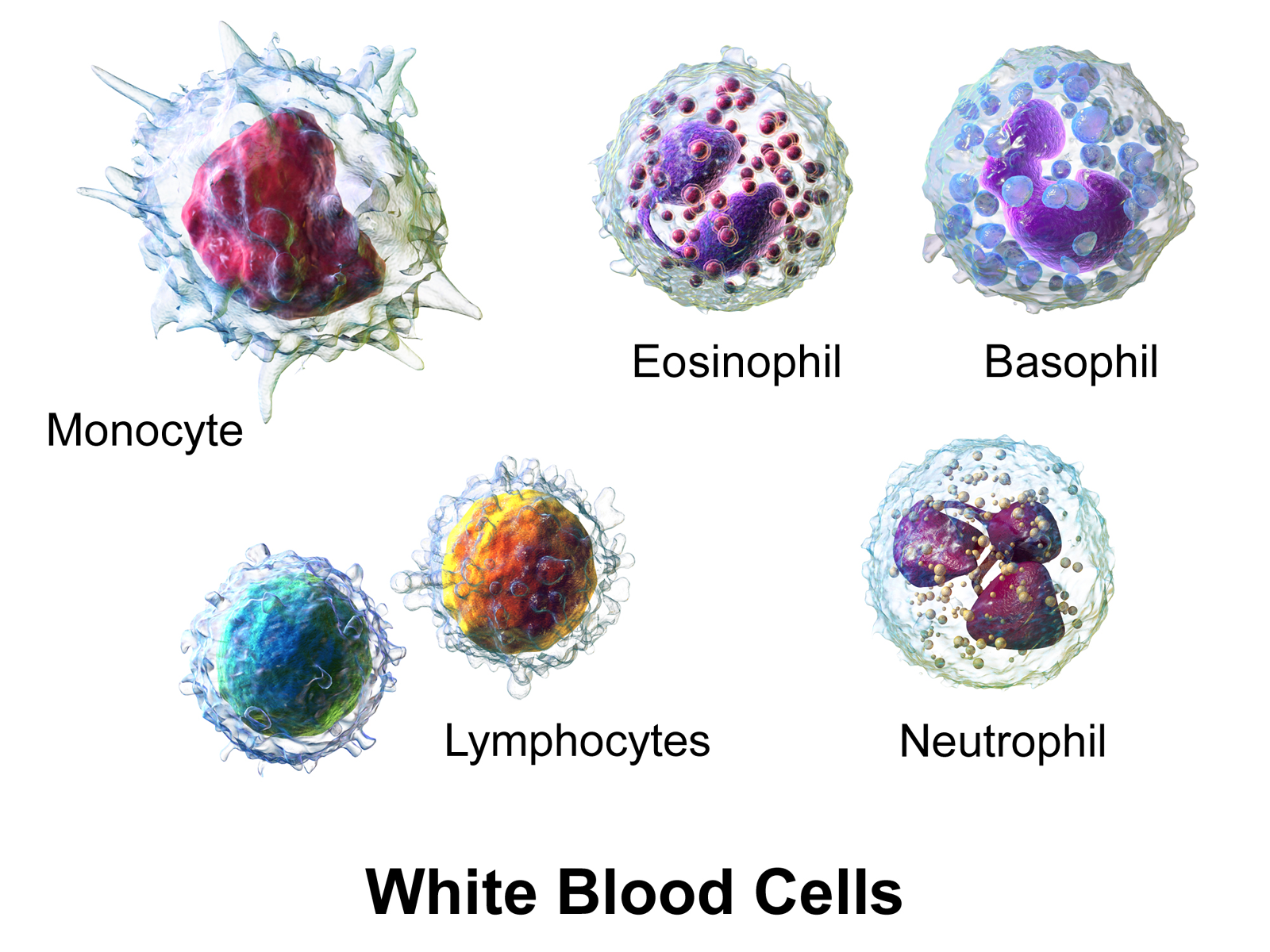 Figure \(\PageIndex{2}\): Leukocytes. A neutrophil has small granules that stain light lilac and a nucleus with two to five lobes. An eosinophil’s granules are slightly larger and stain reddish-orange, and its nucleus has two to three lobes. A basophil has large granules that stain dark blue to purple and a two-lobed nucleus. Lymphocytes are the smallest leukocytes, have no visible granules, and are almost entirely filled by a large nucleus. A monocyte is larger than other leukocytes, has no visible granules, and has an indented nucleus. (Image credit: “Blausen 0909 WhiteBloodCells" by Bruce Blaus is licensed under CC BY 3.0)
Figure \(\PageIndex{2}\): Leukocytes. A neutrophil has small granules that stain light lilac and a nucleus with two to five lobes. An eosinophil’s granules are slightly larger and stain reddish-orange, and its nucleus has two to three lobes. A basophil has large granules that stain dark blue to purple and a two-lobed nucleus. Lymphocytes are the smallest leukocytes, have no visible granules, and are almost entirely filled by a large nucleus. A monocyte is larger than other leukocytes, has no visible granules, and has an indented nucleus. (Image credit: “Blausen 0909 WhiteBloodCells" by Bruce Blaus is licensed under CC BY 3.0)
The most common of all the leukocytes, neutrophils will normally comprise 50–70 percent of the total leukocyte count. They are 10–12 µm in diameter, significantly larger than erythrocytes. They are called neutrophils because their granules show up most clearly with stains that are chemically neutral (neither acidic nor basic). The granules are numerous but quite fine and normally appear light lilac. The nucleus has a distinct lobed appearance and may have two to five lobes, the number increasing with the age of the cell. Older neutrophils have increasing numbers of lobes and are often referred to as polymorphonuclear (a nucleus with many forms), or simply “polys.” Younger and immature neutrophils begin to develop lobes and are known as “bands.”
Neutrophils are rapid responders to the site of infection and are efficient phagocytes with a preference for bacteria. Their granules include vesicles filled with substances that help them neutralize infectious agents: lysozyme, an enzyme capable of lysing, or breaking down, bacterial cell walls; oxidants such as hydrogen peroxide; and defensins, proteins that bind to and puncture bacterial and fungal plasma membranes so that the cell contents leak out. Abnormally high counts of neutrophils indicate infection and/or inflammation, particularly triggered by bacteria, but are also found in burn patients and others experiencing unusual stress. A burn injury increases the proliferation of neutrophils in order to fight off infection that can result from the destruction of the barrier of the skin. Low counts may be caused by drug toxicity and other disorders, and may increase an individual’s susceptibility to infection.
Eosinophils typically represent 2–4 percent of the total leukocyte count. They are also 10–12 µm in diameter. The granules of eosinophils stain best with an acidic stain known as eosin. The nucleus of the eosinophil will typically have two to three lobes and, if stained properly, the granules will have a distinct red to orange color.
The granules of eosinophils include vesicles filled with antihistamine molecules, which counteract the activities of histamines, inflammatory chemicals produced by basophils and mast cells. Some eosinophil granules contain molecules toxic to parasitic worms, which can enter the body through the integument, or when an individual consumes raw or undercooked fish or meat. Eosinophils are also capable of phagocytosis and are particularly effective at disposing of antigen-antibody complexes. Antibodies are immunoglobulin proteins produced by certain lymphocytes that carry out several functional aspects of the specific immune response. Antibodies are designed to match-up to a specific molecule, typically a protein called an antigen, on the surface of an invading pathogen such as a parasitic worm, bacterium, or viral particle. Antibodies can also match up with a ubiquitous molecule (such as one on the surface of a pollen granule) and cause an allergic reaction. In this case the antigen is called an allergen, but antibody-antigen complexes are formed during the body's response to the presence of the allergen as if it were the antigen of an invading pathogen. Because it is the function of the eosinophils to use phagocytosis to clear out the debris associated with antibody-antigen complexes, high counts of eosinophils are typical of patients experiencing allergies and some autoimmune diseases, but eosinophils can also be elevated in the case of parasitic worm infestations. Low counts may be due to drug toxicity and stress.
Basophils are the least common leukocytes, typically comprising less than one percent of the total leukocyte count. They are slightly smaller than neutrophils and eosinophils at 8–10 µm in diameter. The granules of basophils stain best with basic (alkaline) stains. Basophils contain large granules that pick up a dark blue stain and are so common they may make it difficult to see the two-lobed nucleus.
In general, basophils intensify the inflammatory response. They share this trait with mast cells of connective tissue proper. In the past, mast cells were considered to be basophils that left the circulation. However, this appears not to be the case, as the two cell types develop from different lineages.
The granules of basophils release histamines, which contribute to inflammation, and heparin, which opposes blood clotting. High counts of basophils are associated with allergies, parasitic infections, and hypothyroidism. Low counts are associated with pregnancy, stress, and hyperthyroidism.
Agranular Leukocytes
Agranular leukocytes (agranulocytes) contain smaller, less-visible granules in their cytoplasm than do granular leukocytes. The nucleus is simple in shape, sometimes with an indentation but without distinct lobes. There are two major types of agranulocytes: lymphocytes and monocytes (Figure \(\PageIndex{2}\)).
Lymphocytes are the only formed element of blood that arises from lymphoid stem cells. Although they form initially in the red bone marrow, much of their subsequent development and reproduction occurs in the lymphatic tissues. Lymphocytes are the second most common type of leukocyte, accounting for about 20–30 percent of all leukocytes, and are an essential part of the immune response. The size range of lymphocytes is quite extensive, with some authorities recognizing two size classes and others three. Typically, the large cells are 10–14 µm and have a smaller nucleus-to-cytoplasm ratio and more granules. The smaller cells are typically 6–9 µm with a larger volume of nucleus to cytoplasm, creating a “halo” effect. A few cells may fall outside these ranges, at 14–17 µm. This finding has led to the three size range classification.
The three major groups of lymphocytes include natural killer cells, B cells, and T cells. Natural killer (NK) cells are capable of recognizing cells that do not express “self” proteins on their plasma membrane or that contain foreign or abnormal markers. These “non-self” cells include abnormal body cells such as cancer cells, cells infected with a virus, and other cells with atypical surface proteins. Thus, they provide generalized, nonspecific immunity. The larger lymphocytes are typically NK cells.
B cells and T cells, also called B lymphocytes and T lymphocytes, play prominent roles in defending the body against specific pathogens (disease-causing microorganisms) and are involved in specific immunity. One form of B cells (plasma cells) produces the antibodies or immunoglobulins that bind to specific foreign or abnormal components of plasma membranes. This is also referred to as humoral (body fluid) immunity, since antibodies are proteins dissolved in body fluids. T cells provide cellular-level immunity by physically attacking foreign or diseased cells. A memory cell is a variety of both B and T cells that forms after exposure to a pathogen and mounts rapid responses upon subsequent exposures. Unlike other leukocytes, memory cells may live for many years. B cells undergo a maturation process in the bone marrow (B for bone marrow), whereas T cells undergo maturation in the thymus (T for thymus). This site of the maturation process gives rise to the name B and T cells. The functions of lymphocytes are complex and will be covered in detail in the chapter covering the lymphatic system and immunity. Smaller lymphocytes are either B or T cells; they cannot be differentiated in a normal blood smear.
Abnormally high lymphocyte counts are characteristic of viral infections as well as some types of cancer. Abnormally low lymphocyte counts are characteristic of prolonged (chronic) illness or immunosuppression, including that caused by HIV infection and drug therapies that often involve steroids.
Monocytes originate from myeloid stem cells. They normally represent 2–8 percent of the total leukocyte count. They are typically easily recognized by their large size of 12–20 µm and indented or horseshoe-shaped nuclei. Macrophages are monocytes that have left the circulation and further differentiated; macrophages are larger than monocytes and feature many extensions of the plasma membrane spread evenly around their periphery to increase their surface area. Macrophages phagocytize debris, foreign pathogens, worn-out erythrocytes, and many other dead, worn out, or damaged cells. Macrophages also release antimicrobial defensins and chemotactic chemicals that attract other leukocytes to the site of an infection. Some macrophages reside permanently in specific locations of the body, whereas others wander primarily through the matrix of connective tissues patrolling for abnormal cells.
Abnormally high counts of monocytes are associated with viral or fungal infections, tuberculosis, some forms of leukemia, and other chronic diseases. Abnormally low counts are typically caused by suppression of the red bone marrow.
Lifecycle of Leukocytes
Most leukocytes have a relatively short lifespan, typically measured in hours or days. Production of all leukocytes begins in the bone marrow under the influence of CSFs and interleukins. Secondary production and maturation of lymphocytes occurs in specific regions of lymphatic tissue known as germinal centers. Lymphocytes are fully capable of mitosis and may produce clones of cells with identical properties. This capacity enables an individual to maintain immunity throughout life to many threats that have been encountered in the past.
DISORDERS OF THE....
Leukocytes
Leukopenia is a condition in which too few leukocytes are produced. If this condition is pronounced, the individual may be unable to ward off disease. Excessive leukocyte proliferation is known as leukocytosis. Although leukocyte counts are high, the cells themselves are often nonfunctional, leaving the individual at increased risk for disease.
Leukemia is a cancer involving an abundance of leukocytes. It may involve only one specific type of leukocyte from either the myeloid line (myelocytic leukemia) or the lymphoid line (lymphocytic leukemia). In chronic leukemia, mature leukocytes accumulate and fail to die. In acute leukemia, there is an overproduction of young, immature leukocytes. In both conditions the cells do not function properly.
Lymphoma is a form of cancer in which masses of malignant T and/or B lymphocytes collect in lymph nodes, the spleen, the liver, and other tissues. As in leukemia, the malignant leukocytes do not function properly, and the patient is vulnerable to infection. Some forms of lymphoma tend to progress slowly and respond well to treatment. Others tend to progress quickly and require aggressive treatment, without which they are rapidly fatal.
Platelets
Platelets are essential for the formation of blood clots to prevent blood loss in the event of damage to a blood vessel wall.
Characteristics and Functions of Platelets
You may occasionally see platelets referred to as thrombocytes, but because this name suggests they are a type of cell, it is misleading. A platelet is not a cell but rather a fragment of the cytoplasm of a cell called a megakaryocyte that is surrounded by a plasma membrane. Megakaryocytes are descended from myeloid stem cells (see Figure 16.5.1 Hematopoietic System of Bone Marrow) and are large, typically 50–100 µm in diameter, and contain an enlarged, lobed nucleus. Thrombopoietin, a glycoprotein secreted by the kidneys and liver, stimulates the proliferation of megakaryoblasts, which mature into megakaryocytes. These remain within red bone marrow tissue and ultimately form platelet-precursor extensions that extend through the walls of bone marrow capillaries to release into the circulation thousands of cytoplasmic fragments, each enclosed by a bit of plasma membrane. These enclosed fragments are platelets. Each megakarocyte releases 2000–3000 platelets during its lifespan. Following platelet release, megakaryocyte remnants, which are little more than a cell nucleus, are consumed by macrophages.
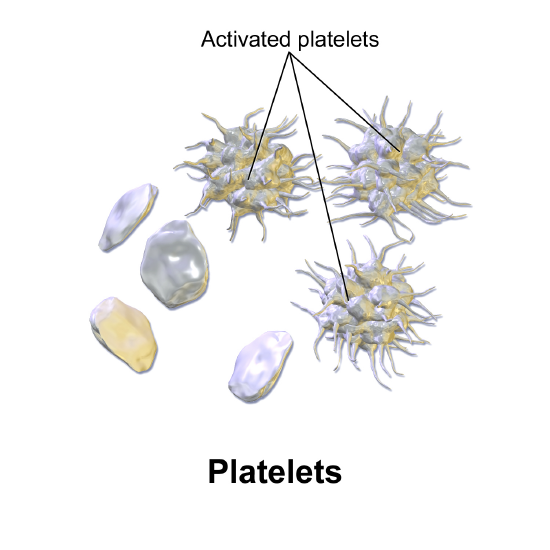 Figure \(\PageIndex{3}\): Platelets. A platelet is a fragment of a cell. When activated, its plasma membrane gains surface area with many hairlike extensions and becomes sticky. (Image credit: "Blausen 0740 Platelets" by Bruce Blaus is licensed under CC BY 3.0)
Figure \(\PageIndex{3}\): Platelets. A platelet is a fragment of a cell. When activated, its plasma membrane gains surface area with many hairlike extensions and becomes sticky. (Image credit: "Blausen 0740 Platelets" by Bruce Blaus is licensed under CC BY 3.0)
Platelets are relatively small, 2–4 µm in diameter, but numerous, with typically 150,000–160,000 per µL of blood (Figure \(\PageIndex{3}\)). After entering the circulation, approximately one-third migrate to the spleen for storage for later release in response to any rupture in a blood vessel. They then become activated to perform their primary function, which is to limit blood loss. Activated platelets develop hair-like extensions to increase their surface area and become sticky. Platelets remain only about 10 days, then are phagocytized by macrophages.
Platelets are critical to hemostasis, the stoppage of blood flow following damage to a vessel. The process of hemostasis involves three steps: vascular spasm, platelet plug formation, and coagulation (formation of a blood clot). During vascular spasm, smooth muscle in the wall of the damaged vessel responds to signal chemicals and pain receptors detecting the damage by constricting to restrict blood flow through the damaged area (the body's own way of applying pressure to the bleeding wound). The platelet plug is a temporary attempt to seal the damaged vessel wall. It forms when activated platelets clump and attach to the damaged area of the vessel wall. As the platelets form this initial plug, they also release signaling chemicals to initiate a cascade of events that allows the more durable and long-lasting blood clot to form. A blood clot is comprised of a mesh of elongated, fibrous fibrin proteins (activated from the plasma protein fibrinogen by clotting factors) that trap sticky platelets and red blood cells (Figure \(\PageIndex{4}\)). Platelets also secrete a variety of growth factors essential for growth and repair of tissue, particularly connective tissue. Infusions of concentrated platelets are now being used in some therapies to stimulate healing.
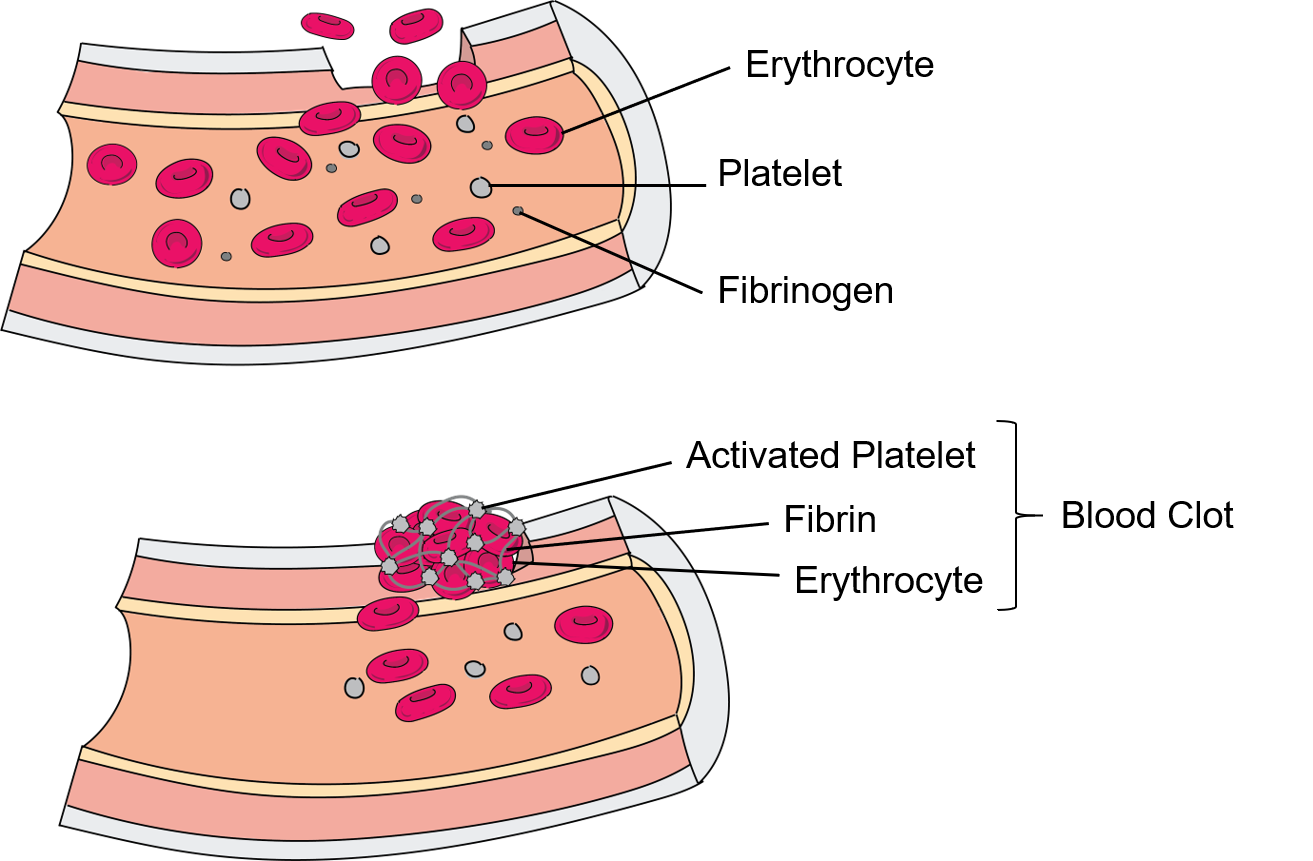 Figure \(\PageIndex{4}\): Blood Clot. A blood clot forms when a vessel wall is damaged. Inactive platelets and fibrinogen circulate in blood and both are activated if a vessel wall is damaged. Activated platelets grow in surface area and stick together, while fibrin becomes fibrous, creating a net-like mesh that sticks to the platelets and traps erythrocytes in the clot as well. ("Blood Clot" by Julie Jenks is a derivative from the original work of Daniel Donnelly and is licensed under CC BY 4.0)
Figure \(\PageIndex{4}\): Blood Clot. A blood clot forms when a vessel wall is damaged. Inactive platelets and fibrinogen circulate in blood and both are activated if a vessel wall is damaged. Activated platelets grow in surface area and stick together, while fibrin becomes fibrous, creating a net-like mesh that sticks to the platelets and traps erythrocytes in the clot as well. ("Blood Clot" by Julie Jenks is a derivative from the original work of Daniel Donnelly and is licensed under CC BY 4.0)
DISORDERS OF THE....
Platelets
Thrombocytosis is a condition in which there are too many platelets. This may trigger formation of unwanted blood clots (thrombosis), a potentially fatal disorder.
If there is an insufficient number of platelets, called thrombocytopenia, blood may not clot properly and excessive bleeding may result. Hemophilia is a group of genetic disorders also marked by excessive bleeding, but caused by inadequate production of one or more clotting factors, resulting in failure of the blood to properly clot.
Concept Review
Leukocytes function in body defenses. They squeeze out of the walls of blood vessels through emigration or diapedesis, then may move through tissue fluid or become attached to various organs where they fight against pathogenic organisms, diseased cells, or other threats to health. Granular leukocytes, which include neutrophils, eosinophils, and basophils, originate from myeloid stem cells, as do monocytes, one type of agranular leukocyte. The other agranular leukocytes, NK cells, B cells, and T cells, which are all types of lymphocytes, arise from the lymphoid stem cell line. The most abundant leukocytes are the neutrophils, which are first responders to infections, especially with bacteria. About 20–30 percent of all leukocytes are lymphocytes, which are critical to the body’s defense against specific threats. Leukemia and lymphoma are malignancies involving leukocytes. Platelets are fragments of cells known as megakaryocytes that dwell within the bone marrow. While many platelets are stored in the spleen, others enter the circulation and are essential for hemostasis; they also produce several growth factors important for repair and healing.
Review Questions
Q. The process by which leukocytes squeeze through adjacent cells in a blood vessel wall is called ________.
A. leukocytosis
B. positive chemotaxis
C. emigration
D. cytoplasmic extending
- Answer
-
Answer: C
Q. Which of the following describes a neutrophil?
A. abundant, agranular, especially effective against cancer cells
B. abundant, granular, especially effective against bacteria
C. rare, agranular, releases antimicrobial defensins
D. rare, granular, contains multiple granules packed with histamine
- Answer
-
Answer: B
Q. T and B lymphocytes ________.
A. are polymorphonuclear
B. are involved with specific immune function
C. proliferate excessively in leukopenia
D. are most active against parasitic worms
- Answer
-
Answer: B
Q. A patient has been experiencing severe, persistent allergy symptoms that are reduced when she takes an antihistamine. Before the treatment, this patient was likely to have had increased activity of which leukocyte?
A. basophils
B. neutrophils
C. monocytes
D. natural killer cells
- Answer
-
Answer: A
Q. Thrombocytes are more accurately called ________.
A. clotting factors
B. megakaryoblasts
C. megakaryocytes
D. platelets
- Answer
-
Answer: D
Critical Thinking Questions
Q. One of the more common adverse effects of cancer chemotherapy is the destruction of leukocytes. Before his next scheduled chemotherapy treatment, a patient undergoes a blood test called an absolute neutrophil count (ANC), which reveals that his neutrophil count is 1900 cells per microliter. Would his healthcare team be likely to proceed with his chemotherapy treatment? Why?
- Answer
-
A. A neutrophil count below 1800 cells per microliter is considered abnormal. Thus, this patient’s ANC is at the low end of the normal range and there would be no reason to delay chemotherapy. In clinical practice, most patients are given chemotherapy if their ANC is above 1000.
Q. A patient was admitted to the burn unit the previous evening suffering from a severe burn involving his left upper extremity and shoulder. A blood test reveals that he is experiencing leukocytosis. Why is this an expected finding?
- Answer
-
A. Any severe stress can increase the leukocyte count, resulting in leukocytosis. A burn is especially likely to increase the proliferation of leukocytes in order to ward off infection, a significant risk when the barrier function of the skin is destroyed.
Glossary
- agranular leukocytes
- leukocytes with few granules in their cytoplasm; specifically, monocytes, lymphocytes, and NK cells
- B lymphocytes
- (also, B cells) lymphocytes that defend the body against specific pathogens and thereby provide specific immunity
- basophils
- granulocytes that stain with a basic (alkaline) stain and store histamine and heparin
- blood clot
- mesh of fibrin proteins and sticky platelets and red blood cells that forms a more durable and long-lasting seal for a damaged blood vessel wall during hemostasis
- coagulation
- process of forming a blood clot during hemostasis
- defensins
- antimicrobial proteins released from neutrophils and macrophages that create openings in the plasma membranes to kill cells
- diapedesis
- (also, emigration) process by which leukocytes squeeze through adjacent cells in a blood vessel wall to enter tissues
- emigration
- (also, diapedesis) process by which leukocytes squeeze through adjacent cells in a blood vessel wall to enter tissues
- eosinophils
- granulocytes that stain with eosin; they release antihistamines and are especially active against parasitic worms
- fibrin
- activated form of the plasma protein fibrinogen; elongated, fibrous protein that forms a mesh framework within a blood clot
- granular leukocytes
- leukocytes with abundant granules in their cytoplasm; specifically, neutrophils, eosinophils, and basophils
- hemophilia
- a group of genetic disorders that can result in excessive bleeding related to inadequate production of one or more clotting factors
- hemostasis
- stoppage of blood flow following damage to a vessel
- leukemia
- cancer involving leukocytes
- leukocyte
- (also, white blood cell) colorless, nucleated blood cell, the chief function of which is to protect the body from disease
- leukocytosis
- excessive leukocyte proliferation
- leukopenia
- below-normal production of leukocytes
- lymphocytes
- agranular leukocytes of the lymphoid stem cell line, many of which function in specific immunity
- lymphoma
- form of cancer in which masses of malignant T and/or B lymphocytes collect in lymph nodes, the spleen, the liver, and other tissues
- lysozyme
- digestive enzyme with bactericidal properties
- megakaryocyte
- bone marrow cell that produces platelets
- memory cell
- type of B or T lymphocyte that forms after exposure to a pathogen
- monocytes
- agranular leukocytes of the myeloid stem cell line that circulate in the bloodstream; tissue monocytes are macrophages
- natural killer (NK) cells
- cytotoxic lymphocytes capable of recognizing cells that do not express “self” proteins on their plasma membrane or that contain foreign or abnormal markers; provide generalized, nonspecific immunity
- neutrophils
- granulocytes that stain with a neutral dye and are the most numerous of the leukocytes; especially active against bacteria
- platelet plug
- temporary seal for a damaged blood vessel wall during hemostasis; comprised of sticky platelets attached to the damaged vessel wall
- polymorphonuclear
- having a lobed nucleus, as seen in some leukocytes
- positive chemotaxis
- process in which a cell is attracted to move in the direction of chemical stimuli
- T lymphocytes
- (also, T cells) lymphocytes that provide cellular-level immunity by physically attacking foreign or diseased cells
- thrombocytes
- platelets, one of the formed elements of blood that consists of cell fragments broken off from megakaryocytes
- thrombocytopenia
- condition in which there are too few platelets, resulting in abnormal bleeding (hemophilia)
- thrombocytosis
- condition in which there are too many platelets, resulting in abnormal clotting (thrombosis)
Contributors and Attributions
OpenStax Anatomy & Physiology (CC BY 4.0). Access for free at https://openstax.org/books/anatomy-and-physiology


