20.4: The Processes of the Respiratory System
- Page ID
- 22402
By the end of this section, you will be able to:
- Describe how the relationship between pressure and volume drives pulmonary ventilation
- Compare and contrast ventilation, the transport of gases, and the specific types of respiration
The processes of the respiratory system follow oxygen from its origin in the air you inhale to its use by cells of the body to convert glucose to cellular energy in the form of adenosine triphosphate (ATP). Since the conversion of glucose to ATP produces carbon dioxide as a waste, carbon dioxide originates at the cells of the body and takes the same journey in reverse to be eliminated form the body when you inhale. The processes of the respiratory system are pulmonary ventilation, external respiration, transport of gases, internal respiration, and cellular respiration.
Pulmonary Ventilation
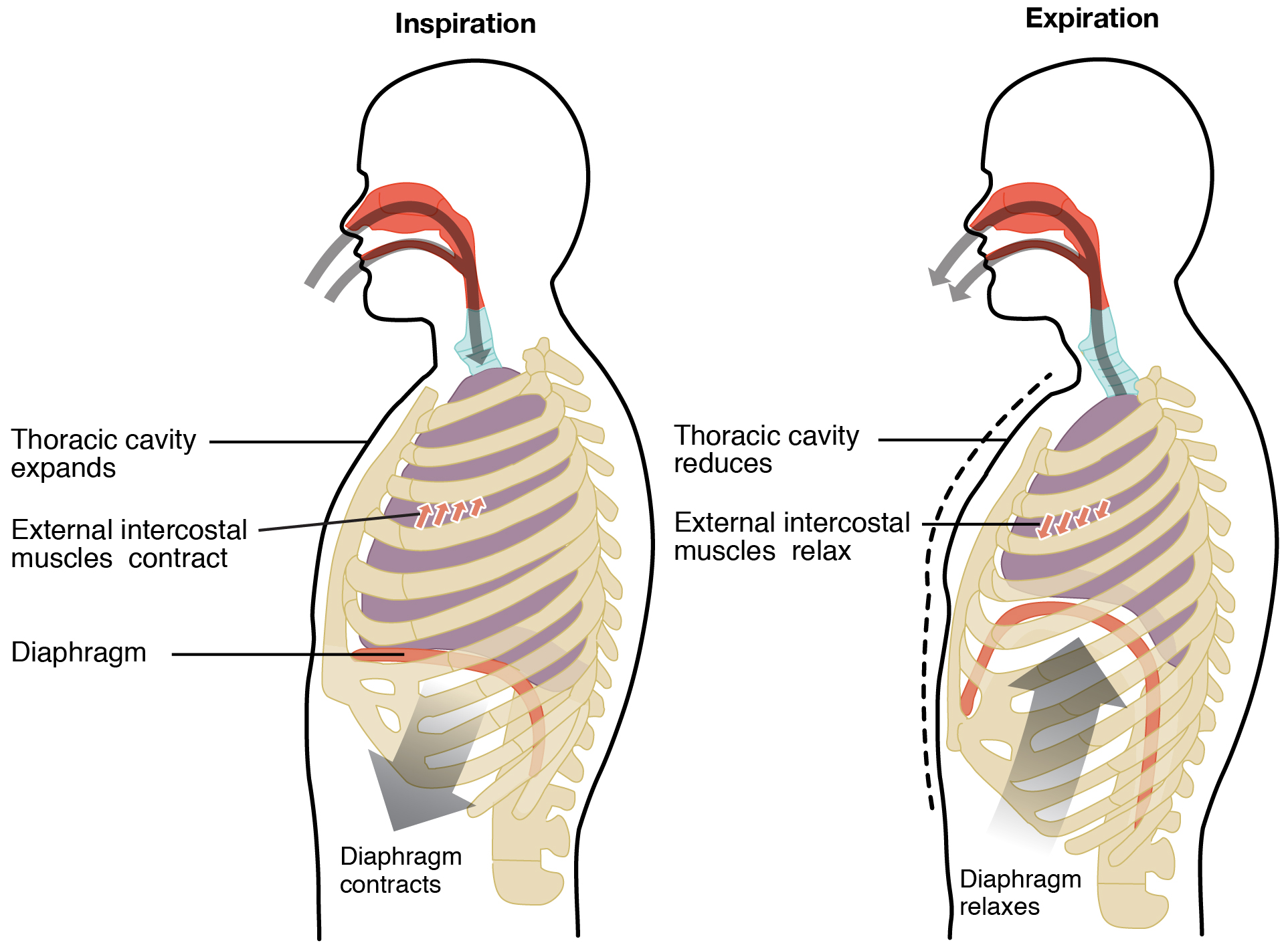
Pulmonary ventilation is the act of breathing, which can be described as the movement of air into and out of the lungs. When you take a deep breath, notice the expansion of your rib cage. Contraction of the diaphragm and external intercostal muscles increases the volume in the chest cavity, which in turn lowers the pressure and draws air into the lungs for inspiration. The process for expiration (or exhalation) is similar only in the reverse (Figure \(\PageIndex{1}\)). Boyle’s Law describes the relationship between volume and pressure in a gas at a constant temperature. Boyle discovered that the pressure of a gas is inversely proportional to its volume: If volume increases, pressure decreases. Likewise, if volume decreases, pressure increases.
The lungs themselves are passive during breathing, meaning they are not involved in creating the movement that helps inspiration and expiration. This is because of the adhesive nature of the pleural fluid, which allows the lungs to be pulled outward when the thoracic wall moves during inspiration. The recoil of the thoracic wall, partly due to lung elasticity, during expiration causes compression of the lungs. While typical expiration is a passive process caused by relaxation of muscles and elasticity of tissues, a forced or maximal expiration can involve contraction of the internal intercostals and other muscles that compress the rib cage.
The difference in pressures drives pulmonary ventilation because air flows down a pressure gradient, that is, air flows from an area of higher pressure to an area of lower pressure. By expanding the thoracic cavity and thus the lungs, the increased volume results in a decrease in the lung air pressure. At this time, atmospheric pressure is greater than pressure within the lungs and air flows in (inhalation). Air flows out of the lungs during expiration based on the same principle; when the lungs recoil, pressure within the lungs becomes greater than the atmospheric pressure.
DISORDERS OF THE...
Respiratory System: Chronic Obstructive Pulmonary Disorder (COPD)
Chronic Obstructive Pulmonary Disorder (COPD) is used to describe a number of closely related respiratory conditions including chronic bronchitis and emphysema. COPD is often associated with heavy smokers, although it can affect individuals that never smoked. In chronic bronchitis, the walls of the bronchioles are chronically inflamed, reducing the volume of the lumen and marked by an over-production of mucus that can obstruct the movement of air during ventilation. In emphysema, the alveolar walls lose their elasticity and are destroyed, often by a build-up of damage and debris being cleaned up by alveolar macrophages (Figure \(\PageIndex{2}\)). The damage leads to fibrosis in which normal tissue is replaced by scar tissue, further reducing the elasticity of the alveolar walls and perpetuating the progression fo the disease.
Patients with COPD can have shortness of breath and can have difficulty in particular with expiration, which affects the efficiency of ventilation. Coupled with alveolar damage, the result is reduced oxygen levels in the blood, which can affect the function of many systems of the body. Bronchodilators and anti-inflammatory medications are typically used to treat COPD. Eventually, in those with severe COPD, even treatment with supplemental oxygen will not be sufficient to prevent respiratory failure.
Respiratory Rate and Control of Ventilation
Breathing usually occurs without thought, although at times you can consciously control it, such as when you swim under water, sing a song, or blow bubbles. The respiratory rate is the total number of breaths, or respiratory cycles, that occur each minute. Respiratory rate can be an important indicator of disease, as the rate may increase or decrease during an illness or in a disease condition. The respiratory rate is controlled by the respiratory center located within the medulla oblongata in the brain, which responds primarily to input received from central and peripheral chemoreceptors that sense carbon dioxide and blood pH. While blood oxygen levels are not the primary drive of respiratory rate, the respiratory center will receive input if they get dangerously low.
The normal respiratory rate of a child decreases from birth to adolescence. A child under 1 year of age has a normal respiratory rate between 30 and 60 breaths per minute, but by the time a child is about 10 years old, the normal rate is closer to 18 to 30. By adolescence, the normal respiratory rate is similar to that of adults, 12 to 18 breaths per minute.
DISORDERS OF THE...
Respiratory System: Sleep Apnea
Sleep apnea is a chronic disorder that can occur in children or adults, and is characterized by the cessation of breathing during sleep. These episodes may last for several seconds or several minutes, and may differ in the frequency with which they are experienced. Sleep apnea leads to poor sleep, which is reflected in the symptoms of fatigue, evening napping, irritability, memory problems, and morning headaches. In addition, many individuals with sleep apnea experience a dry throat in the morning after waking from sleep, which may be due to excessive snoring.
There are two types of sleep apnea: obstructive sleep apnea and central sleep apnea. Obstructive sleep apnea is caused by an obstruction of the airway during sleep, which can occur at different points in the airway, depending on the underlying cause of the obstruction. For example, the tongue and throat muscles of some individuals with obstructive sleep apnea may relax excessively, causing the muscles to push into the airway. Another example is obesity, which is a known risk factor for sleep apnea, as excess adipose tissue in the neck region can push the soft tissues towards the lumen of the airway, causing the trachea to narrow.
In central sleep apnea, the respiratory centers of the brain do not respond properly to rising carbon dioxide levels and therefore do not stimulate the contraction of the diaphragm and intercostal muscles regularly. As a result, inspiration does not occur and breathing stops for a short period. In some cases, the cause of central sleep apnea is unknown. However, some medical conditions, such as stroke and congestive heart failure, may cause damage to the pons or medulla oblongata. In addition, some pharmacologic agents, such as morphine, can affect the respiratory centers, causing a decrease in the respiratory rate. The symptoms of central sleep apnea are similar to those of obstructive sleep apnea.
A diagnosis of sleep apnea is usually done during a sleep study, where the patient is monitored in a sleep laboratory for several nights. The patient’s blood oxygen levels, heart rate, respiratory rate, and blood pressure are monitored, as are brain activity and the volume of air that is inhaled and exhaled. Treatment of sleep apnea commonly includes the use of a device called a continuous positive airway pressure (CPAP) machine during sleep. The CPAP machine has a mask that covers the nose, or the nose and mouth, and forces air into the airway at regular intervals. This pressurized air can help to gently force the airway to remain open, allowing more normal ventilation to occur. Other treatments include lifestyle changes to decrease weight, eliminate alcohol and other sleep apnea–promoting drugs, and changes in sleep position. In addition to these treatments, patients with central sleep apnea may need supplemental oxygen during sleep.
Respiration and Transport of Gases
External respiration is the process of gas exchange between the air in the alveoli of the lungs and the blood in capillaries wrapped around them. Oxygen moves by simple diffusion from an area of higher concentration in the air across two simple squamous epithelium linings: the first lining the alveolus and the second lining the blood capillary. The oxygen then moves into an erythrocyte and binds to a molecule of hemoglobin. In exchange, carbon dioxide moves from the blood into the alveolus by the same process in the reverse direction.
Once oxygen binds to hemoglobin in the bloodstream of the pulmonary circuit, it is transported back to the heart and then delivered to another capillary bed at a tissue of the body via the systemic circuit. Carbon dioxide is a metabolic waste product that travels through the bloodstream from the tissues so it may be eliminated from the body during expiration. Some carbon dioxide travels in erythrocytes, but most of it travels in the plasma and may be in the form of carbonic acid (a weak acid) or sodium bicarbonate (a weak base) to help balance the pH of the blood. Thereby, levels of carbon dioxide eliminated during expiration may be adjusted to help balance blood pH. In these ways, blood acts as the medium of transport of respiratory gases.
Internal respiration is the process of gas exchange between the blood in capillaries at the cells of the tissues of the body. The process is similar to that of external respiration, but in the reverse direction: oxygen moves by simple diffusion from the capillary into the cells while carbon dioxide moves by simple diffusion from the cells into the capillary. The mitochondria of the cells in the destination tissue will use the oxygen to complete cellular respiration, the chemical process by which glucose is converted to ATP cellular energy to power various activities of the cell. Carbon dioxide is produced as a metabolic waste product of cellular respiration and must be removed from the tissue and transported for elimination from the body.
Concept Review
Pulmonary ventilation is the process of breathing, which is driven by pressure differences between the lungs and the atmosphere. Pulmonary ventilation consists of the process of inspiration (or inhalation), where air enters the lungs, and expiration (or exhalation), where air leaves the lungs. During inspiration, the diaphragm and external intercostal muscles contract, causing the rib cage to expand and move outward, and expanding the thoracic cavity and lung volume. This creates a lower pressure within the lung than that of the atmosphere, causing air to be drawn into the lungs. During expiration, the diaphragm and intercostals relax, causing the thorax and lungs to recoil. The air pressure within the lungs increases to above the pressure of the atmosphere, causing air to be forced out of the lungs. However, during forced exhalation, the internal intercostals and abdominal muscles may be involved in forcing air out of the lungs.
Both respiratory rate and depth are controlled by the respiratory centers of the brain, which are stimulated by factors such as chemical and pH changes in the blood. A rise in carbon dioxide or a decline in oxygen levels in the blood stimulates an increase in respiratory rate and depth.
External respiration is the process of gas exchange that occurs between the alveoli and the bloodstream. Transport of gases describes the movement of oxygen and carbon dioxide through the bloodstream from where each gas originates to its destination in the body. Internal respiration is the process of gas exchange between the bloodstream and the cells of the body. Cellular respiration is the metabolic process of consuming oxygen to convert glucose into ATP energy.
Review Questions
Q. Which of the following processes does atmospheric pressure play a role in?
A. pulmonary ventilation
B. production of pulmonary surfactant
C. resistance
D. surface tension
- Answer
-
A
Q. A decrease in volume leads to a(n) ________ pressure.
A. decrease in
B. equalization of
C. increase in
D. zero
- Answer
-
C
Critical Thinking Questions
Q. What is respiratory rate and how is it controlled?
- Answer
-
Respiratory rate is defined as the number of breaths taken per minute. Respiratory rate is controlled by the respiratory center, located in the medulla oblongata. Conscious thought can alter the normal respiratory rate through control by skeletal muscle, although one cannot consciously stop the rate altogether. A typical resting respiratory rate is about 14 breaths per minute.
Glossary
- atmospheric pressure
- amount of force that is exerted by gases in the air surrounding any given surface
- Boyle’s law
- relationship between volume and pressure as described by the formula: P1V1 = P2V2
- expiration
- (also, exhalation) process that causes the air to leave the lungs
- inspiration
- (also, inhalation) process that causes air to enter the lungs
- pulmonary ventilation
- exchange of gases between the lungs and the atmosphere; breathing
- respiratory rate
- total number of breaths taken each minute
Contributors and Attributions
OpenStax Anatomy & Physiology (CC BY 4.0). Access for free at https://openstax.org/books/anatomy-and-physiology


