3.2: Body Mechanics
- Page ID
- 9996
Body mechanics involves the coordinated effort of muscles, bones, and the nervous system to maintain balance, posture, and alignment during moving, transferring, and positioning patients. Proper body mechanics allows individuals to carry out activities without excessive use of energy, and helps prevent injuries for patients and health care providers (Perry, Potter, & Ostendorf, 2014).
Musculoskeletal Injuries
A musculoskeletal injury (MSI) is an injury or disorder of the muscles, tendons, ligaments, joints or nerves, blood vessels, or related soft tissue including a sprain, strain, or inflammation related to a work injury. MSIs are the most common health hazard for health care providers (WorkSafeBC, 2013). Table 3.1 lists risk factors that contribute to an MSI.
|
Table 3.1 Factors That Contribute to an MSI |
|||
|
Factor |
Special Information |
||
| Ergonomic risk factors | Repetitive or sustained awkward postures, repetition, or forceful exertion | ||
| Individual risk factors | Poor work practice; poor overall health (smoking, drinking alcohol, and obesity); poor rest and recovery; poor fitness, hydration, and nutrition | ||
| Data source: Perry et al., 2014; Workers Compensation Board, 2001; WorkSafeBC, 2013 | |||
When health care providers are exposed to ergonomic risk factors, they become fatigued and risk musculoskeletal imbalance. Additional exposure related to individual risk factors puts health care providers at increased risk for an MSI (WorkSafeBC, 2013). Preventing an MSI is achieved by understanding the elements of body mechanics, applying the principles of body mechanics to all work-related activities, understanding how to assess a patient’s ability to position or transfer, and learning safe handling transfers and positioning techniques.
Elements of Body Mechanics
Body movement requires coordinated muscle activity and neurological integration. It involves the basic elements of body alignment (posture), balance, and coordinated movement. Body alignment and posture bring body parts into position to promote optimal balance and body function. When the body is well aligned, whether standing, sitting, or lying, the strain on the joints, muscles, tendons, and ligaments is minimized (WorkSafeBC, 2013).
Body alignment is achieved by placing one body part in line with another body part in a vertical or horizontal line. Correct alignment contributes to body balance and decreases strain on muscle-skeletal structures. Without this balance, the risk of falls and injuries increase. In the language of body mechanics, the centre of gravity is the centre of the weight of an object or person. A lower centre of gravity increases stability. This can be achieved by bending the knees and bringing the centre of gravity closer to the base of support, keeping the back straight. A wide base of support is the foundation for stability. A wide base of support is achieved by placing feet a comfortable, shoulder width distance apart. When a vertical line falls from the centre of gravity through the wide base of support, body balance is achieved. If the vertical line moves outside the base of support, the body will lose balance.
The diagram in Figure 3.1 demonstrates (A) a well-aligned person whose balance is maintained and whose line of gravity falls within the base of support. Diagram (B) demonstrates how balance is not maintained when the line of gravity falls outside the base of support, and diagram (C) shows how balance is regained when the line of gravity falls within the base of support.

Figure 3.1 Centre of gravity
Principles of Body Mechanics
Table 3.2 describes the principles of body mechanics that should be applied during all patient-handling activities.
|
Table 3.2 Principles of Body Mechanics |
|||
|
Action |
Principle |
||
| Assess the environment. | Assess the weight of the load before lifting and determine if assistance is required. | ||
| Plan the move. | Plan the move; gather all supplies and clear the area of obstacles. | ||
| Avoid stretching and twisting. | Avoid stretching, reaching, and twisting, which may place the line of gravity outside the base of support. | ||
| Ensure proper body stance. | Keep stance (feet) shoulder-width apart.
Tighten abdominal, gluteal, and leg muscles in anticipation of the move. Stand up straight to protect the back and provide balance. |
||
| Stand close to the object being moved. | Place the weight of the object being moved close to your centre of gravity for balance.
Equilibrium is maintained as long as the line of gravity passes through its base of support. 
Hold objects close to your centre of gravity |
||
| Face direction of the movement. | Facing the direction prevents abnormal twisting of the spine. | ||
| Avoid lifting. | Turning, rolling, pivoting, and leverage requires less work than lifting.
Do not lift if possible; use mechanical lifts as required. Encourage the patient to help as much as possible. |
||
| Work at waist level. | Keep all work at waist level to avoid stooping.
Raise the height of the bed or object if possible. Do not bend at the waist. |
||
| Reduce friction between surfaces. | Reduce friction between surfaces so that less force is required to move the patient. | ||
| Bend the knees. | Bending the knees maintains your centre of gravity and lets the strong muscles of your legs do the lifting. | ||
| Push the object rather than pull it, and maintain continuous movement. | It is easier to push an object than to pull it.
Less energy is required to keep an object moving than it is to stop and start it. |
||
| Use assistive devices. | Use assistive devices (gait belt, slider boards, mechanical lifts) as required to position patients and transfer them from one surface to another. | ||
| Work with others. | The person with the heaviest load should coordinate all the effort of the others involved in the handling technique. | ||
| Data source: Berman & Snyder, 2016; Perry et al., 2014; WorkSafeBC, 2013 | |||
Assistive Devices
An assistive device is an object or piece of equipment designed to help a patient with activities of daily living, such as a walker, cane, gait belt, or mechanical lift (WorkSafeBC, 2006). Table 3.3 lists some assistive devices found in the hospital and community setting.
|
Table 3.3 Assistive Devices |
|||
| Type | Definition | ||
| Gait belt or transfer belt | Used to ensure a good grip on unstable patients. The device provides more stability when transferring patients. It is a 2-inch-wide (5 mm) belt, with or without handles, that is placed around a patient’s waist and fastened with Velcro. The gait belt must always be applied on top of clothing or gown to protect the patient’s skin. A gait belt can be used with patients in both one-person or two-person pivot transfer, or in transfer with a slider board.

Gait belt |
||
| Slider board or transfer board |
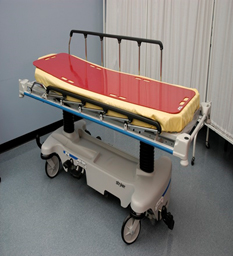
Slider board (red) on a stretcher 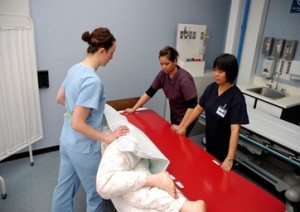
Placing a slider board (transfer board) under a patient A slider board is used to transfer immobile patients from one surface to another while the patient is lying supine. The board allows health care providers to safely move immobile, bariatric, or complex patients. |
||
| Mechanical lift | A mechanical lift is a hydraulic lift, usually attached to a ceiling, used to move patients who cannot bear weight, who are unpredictable or unreliable, or who have a medical condition that does not allow them to stand or assist with moving.

Mechanical lift |
||
| Data source: Perry et al., 2014; WorkSafeBC, 2006 | |||
Special considerations:
- Use assistive devices only if properly trained in their safe use.
- Always tell patients what you are about to do and how they should assist you in the procedure.
- Always perform a patient risk assessment or mobility assessment prior to using any assistive devices. The following link provides additional information regarding assistive devices from WorkSafeBC.
- Use proper body mechanics when using assistive devices.
Critical Thinking Exercises
- How do body alignment and body balance contribute to proper body mechanics?
- John is asked to lift a heavy box from a table onto a trolley. Name five principles of body mechanics John can implement to prevent an MSI.

