1.1: Immunosuppression for Solid Organ Transplantation
- Page ID
- 10633
The success of solid organ and bone marrow transplantation (BMT) has correlated with improvements in selective immunosuppression. Immunosuppression decreases both the incidence of acute and chronic organ graft and bone marrow rejection, and a potentially life threatening complication of BMT known as graft-vs-host disease (GVHD). Selective immunosuppression targets specific pathways of immune signaling and activation, and minimizes the incidence of deleterious side effects.
History
- 1954: First successful human kidney transplant
- 1960s: Introduction of effective immunosuppressive drugs. Steroids, ATG, azathioprine
- 1968: Successful bone marrow transplants for congenital immunodeficiency syndromes
- 1970s: Cyclosporine introduced
- 1980s: OKT3, tacrolimus, mycophenolate mofetil introduced
- In 1988 1 year renal cadaver graft survival was 76% and 1 year renal living donor graft survival was 89%
- ▫ By 1995, graft survival rates improved to 87% and 93% respectively
- 1980s: The addition of cyclosporine to GVHD prophylaxis regimens halved the incidence of severe disease and improved survival post -transplant
- 1990s: Leflunomide, TNF antagonists, and selective mAbs introduced; additional mAb therapies expected in future
Balancing Benefits and Risks of Immunosuppression
Benefits: Immunosuppression decreases risks of both acute and chronic organ graft and bone marrow rejection, and GVHD
Risks: Immunosuppression poses risk of several types of side effects to the patient:
- Acute effects: gastrointestinal upset
- Opportunistic infection because patient is immunocompromised: CMV, Candida,Pneumocystis carinii, etc.
- Malignancies (lymphomas, skin cancer, etc.)
- Toxicities specific to particular immunosuppressive agent: steroids, etc.
Types of Organ Graft Rejection
- Hyperacute: Occurs within minutes after transplant. Mediated by preformed anti- donor antibodies in recipient. Involves small vessel thrombosis and graft infarction.
- Acute: Occurs weeks after transplant. Delayed-type hypersensitivity / Cell mediated response of cytotoxic T lymphocytes reacting against the foreign MHC molecules of the graft. Histologically characterized by mononuclear infiltrate, hemorrhage, and edema in graft. Reversible with immunosuppressive therapy.
- Chronic: Occurs months to years post transplant. Results from antibody mediated vascular damage (fibrinoid necrosis) and is irreversible. Vascular damage results in vascular cell wall proliferation which may occlude vessel lumen resulting in graft ischemia and fibrosis. Can progress insidiously despite increased immunosuppressive therapy.
Graft Rejection and GVHD Following Bone Marrow Transplantation
- Graft rejection occurs uncommonly (<1%) after conventional myeloablative bone marrow/stem cell transplantation, with increased incidence (1-15%) after HLA- mismatched BMT/cord blood transplantation.
- The rate of graft rejection is higher after nonmyeloablative preparative therapy for BMT
- Acute GVHD, which is usually evident before day 100 post-transplant, occurs in 1/3 of HLA matched transplants and 2/3 of HLA-mismatched transplants.
- Chronic GVHD (>day 100) occurs in approximately 1⁄2 of transplants
- Acute GVHD affects predominantly skin, the GI tract, and liver. Tissue injury involves effector cells (initiated by T-cells), particularly of the TH1 subset, and cytokines (e.g. TNF-alpha, interferon-gamma, and interleukin-1).
- Chronic GVHD may affect almost any organ/tissue and often mimics a collagen vascular disease in its clinical presentation.
Molecular Basis of Immune Response and Immunosuppression
The immune response involves both humoral and cellular responses: Humoral: The humoral response involves recognition of foreign antigens which causes the differentiation of B-cells into memory cells and plasma cells. Plasma cells secrete antibodies into circulation. Cellular: Macrophages ingest and present antigen via the major histocompatibility (MHC) II molecule. The macrophage is a type of antigen presenting cell which binds to CD4 T lymphocytes cells via the MHC II – T cell receptor (TCR) interaction. CD3 is a necessary accessory molecule to the MHC II – TCR interaction. The interaction induces proliferation of the CD4 T-cell (see diagram page 4), and release of IL-2, which promotes activation of cytotoxic CD8 T-cells. CD8 T cells bind to MHC I molecules. When CD8 cells recognize an antigen presented on an MHC I molecule (which indicates the presenting cell is foreign, or, for example, a tumor cell or virally infected cell) the CD8 cell induces the death of the target.
In the context of an MHC mismatched organ or bone marrow transplant, the MHC molecules of the cells of the organ (or bone marrow) graft are recognized by the host
TCR not as self-MHC molecules, but rather in the same manner as a self-MHC plus the foreign peptide it is presenting. The immunologic response to the foreign MHC molecules is a major cause of most graft rejection. Conversely the donor immune system may recognize disparate MHC antigens in the host and initiate an immunologic response in the form of GVHD.
MHC molecules are divided into class I and class II antigens; inheritance involves multiple alleles, and all loci are found on chromosome 6. Class I antigens include HLA A, HLA-B, and HLA-C alleles . Class II antigens include HLA-DR, HLA-DQ, and HLA-DP alleles. Minimization of the antigenic differences between donor and recipient, by matching their MHC alleles, has decreased rejection and GVHD and improved graft survival. Identical twins have identical MHC genes (6/6 loci), siblings have half similarity (3/6), and the match of unrelated persons must be determined by tissue typing.
As most bone marrow/stem cell transplants are from HLA matched (or only minor mismatched) related or unrelated donors, minor histocompatibility antigens play a large role in eliciting an immune response (GVHD). Polymorphisms of minor histompatibility antigens have been identified as risk factors for GVHD in the HLA-matched setting.
Types of Immunosuppressive Agents and Sites of Action
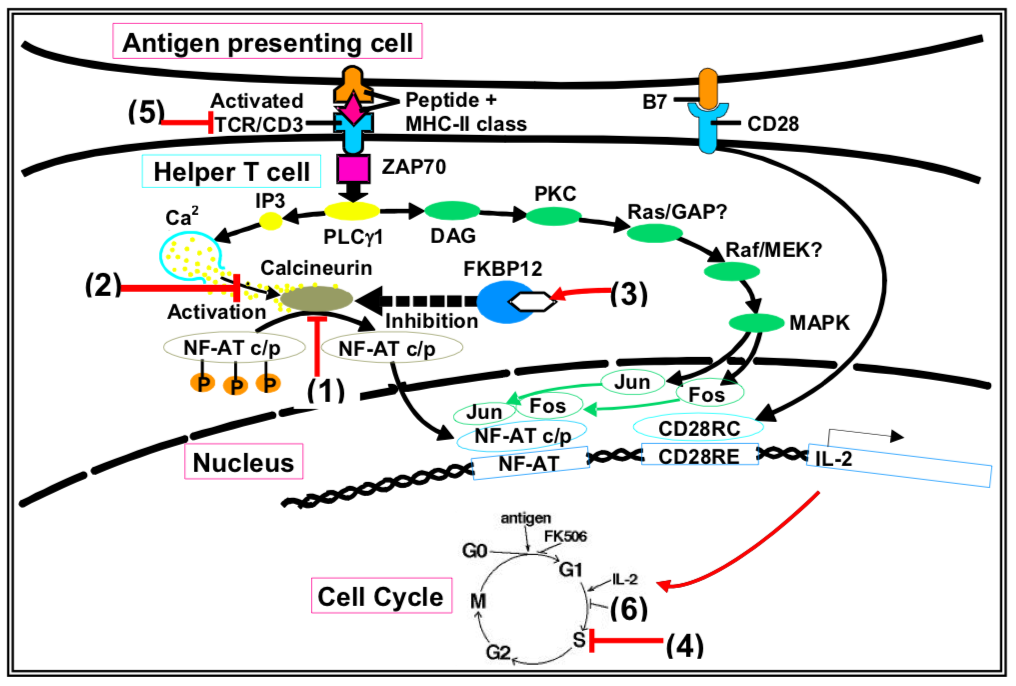
The schematic on page 4 shows the molecular pathways that are activated in a helper T cell after it contacts an antigen presenting cell which presents an antigen on its MHC II molecule. Superimposed on the pathways are sites of pharmacologic intervention which will inhibit signaling and thus can be used as immunosuppressive agents.
- Affect NFAT pathway: Steroids (1)
- Affect Calcineurin: Cyclosporine (2); Tacrolimus (3)
- Affect Cell Cycle by inhibiting DNA synthesis (4): azathioprine, MMF, leflunomide, cyclophosphamide
- Anti-TCR/CD3 antibody agents (5): Polyclonal agents are ATG, ALG. OKT3 is a monoclonal agent.
- Inhibit IL-2 dependent signaling: Sirolimus (6)
(1) Steroids (corticosteroids):
Biochemical Mechanism: Affect NF-AT mediated pathway of signal transduction, which results in ultimate blockade of IL-1 and IL-6 production in macrophages at the earliest stage of immune response.
Physiological Effects: Inhibits leukocyte proliferation, reduce leukocyte migration into bloodstream (by decreasing production of endothelial adhesion molecules). Steroids are non-specific and broad spectrum anti-inflammatory agents used in a large number of medical conditions.
Side Effects: Cushing’s Syndrome [hypertension, hyperglycemia, insulin resistance, weight gain, moon facies, osteoporosis, impaired wound healing, ulcers], hyperlipidemia, adrenal suppression which may result in crisis if withdrawn abruptly
(2) Cyclosporine
Biochemical Mechanism: Cyclosporine complexes with immunophilin protein in T cell. The complex blocks the phosphatase calcineurin. Without calcineurin activity, NF-AT is not dephosphorylated, is not translocated to the nucleus, and cannot activate transcription.
Physiological Effects: Transcription of cytokines, including IL-2, is blunted. Consequently, T cell proliferation is inhibited, secretion of gamma interferon declines, and macrophage activation is limited.
Nephrotoxicity (preventable with mannitol diuresis; chronic cyclosporine nephrotoxicity may produce irreversible interstitial fibrosis), Neurotoxicity (tremor, headache, tinnitus),
Neoplasms (lymphoproliferative malignancy);
Hypertension, Hyperkalemia, Hepatotoxicity, Hirsutism, Hypertrophy of gingiva,
Hyperglycemia, Hyperlipidemia
(3) Tacrolimus (similar to cyclosporine)
Biochemical Mechanism: Binds to FK506 Binding Protein (FKBP). The Tacrolimus- FKBP complex inhibits calcineurin. The mechanism is therefore the same as that of cyclosporine.
Physiological Effects: 10-100 times more potent than cyclosporine, but similar mechanism: decreased production of IL-2
Side Effects: Similar to cyclosporine. Do not use with cyclosporine!
(4) Cell Cycle Inhibitors
Azathioprine: Azathioprine is metabolized in vivo to 6-mercaptopurine (6MP). 6MP is a purine anti-metabolite that prevents DNA and RNA synthesis which inhibits proliferation of lymphocytes. Side effects include pancytopenias, gastrointestinal symptoms, and hepatic dysfunction (hepatitis).
Mycophenolate mofetil (MMF): MMF is a prodrug of mycophenolic acid (MPA), which is an inhibitor of inosine monophosphate dehydrogenase (IMPDH). Inhibition of IMPDH limits production of guanosine nucleotides required for nucleic acid synthesis, and thus exerts a potent, selective cytostatic effect on B- and T- lymphocytes (decreased antibody production and generation of cytotoxic T-cells). Side effects include pancytopenias, infections and malignancies, and gastrointestinal symptoms.
Leflunomide: Leflunomide inhibits dihydroorotate dehydrogenase (an enzyme involved in de novo pyrimidine synthesis); as a result, nucleic acid synthesis and lymphocyte proliferation are inhibited. Side effects include pancytopenias, hepatotoxicity, risk of lymphoproliferative disorders, and rare cases of Stevens- Johnson syndrome and toxic epidermal necrolysis.
Cyclophosphamide: Cyclophosphamide is an extremely potent alkylating agent which destroys proliferating lymphoid cells. Cyclophosphamide causes pancytopenias, hemorrhagic cystitis, alopecia, and infertility.
(5) Anti-TCR/CD3 antibody agents:
anti-lymphocyte globulin (ALG) and anti-thymocyte globulin (ATG) both inactivate peripheral lymphocytes and impair cellular immunity. These antibodies are used for induction of immunosuppression, treating initial rejection, and treating steroid resistant rejection. Side effects include anaphylactic response (because these antibodies are foreign proteins), serum sickness, antigen-antibody induced glomerulonephritis, reactivation of latent viral infections, post transplant lymphoproliferative disease, and development of human anti(mouse) antibodies.
OKT3: OKT3 is a murine monoclonal antibody that blocks the binding of the TCR to antigen, thus downregulating the activity of the entire TCR/CD3 receptor complex. Compared to ALG and ATG, there are fewer serum proteins associated with OKT3 preparations than with those polyclonal antibody preparations (which may result in a more specific effect and fewer side effects). Side effects of OKT3 include fever, myalgias, arthralgias, CNS symptoms, GI irritation, and B-cell lymphoproliferative disorders.
(6) Sirolimus (rapamycin, a macrolide antbiotic)
Biochemical Mechanism: Inhibits IL-2 mediated signaling by inhibiting Target of Rapamycin (TOR), an enzyme active in IL-2 cascades in proliferating lymphocytes.
Physiological Effects: Cell cycle progression from G1 to S is blocked; T- cell and B- cell proliferation is limited, and B-cell antibody production is inhibited.
Side Effects: Hyperlipidemia, Hypertension, Hypokalemia, Pancytopenias, decreased GFR / increased Serum Creatinine, metallic taste in mouth
Newer agents:
Anti-TNF agents include etanercept and infliximab (see Dr. Weinblatt’s lecture).Etanercept is a form of soluble TNF receptor. Infliximab is a chimeric IgG1 monoclonal with a human Fc and murine Fab. By limiting TNF activity, the generation of pro- inflammatory cytokines IL-1 and IL-6 are diminished. In addition, anakinra is recombinant version of the human IL-1 receptor antagonist that inhibits IL-1 by blocking its receptor. Soluble IL-1 receptor antagonists are being developed.
Daclizumab is a humanized monoclonal murine IgG1 antibody that binds to a subunit of the IL-2 (CD25) receptor on the surface of activated lymphocytes. Daclizumab thereby functions as an IL-2 inhibitor. Side effects include hypersensitivity, cellulitis, and wound infection.
Basiliximab is a chimeric murine/human monoclonal IgG1 antibody that blocks the alpha chain of the IL-2 (CD25) receptor on the surface of activated T-cell lymphocytes. Basiliximab is indicated for the prophylaxis of acute organ rejection in renal transplantation. Side effects include hypersensitivity and gastrointestinal disorders.
ALG/ATG can deplete the lymphocyte population. Since daclizumab and basiliximab preferentially affect activated T cells, they are less apt to cause lymphocyte depletion.
Relationship Between Immunosuppressive and Cancer Chemotherapy.
Many cytotoxic drugs are used for both immunotherapy and cancer chemotherapy, but the therapeutic goals are tied to important differences in the cellular targets.
- Cancer cells undergo largely unregulated, asynchronous proliferation, while immune cells proliferate in a burst of activity when antigen (i.e. transplant) is presented. This means immunosuppressant therapy can be timed for maximal effect on the smallest population of immune cells.
- An antigen stimulates proliferation by specific clones of precursor cells, so a cytotoxic drug will have greatly enhanced effects on those clones (i.e. the drug will be relatively selective for rapidly dividing cells). In cancer chemotherapy, selectivity of cell cycle active drugs depends upon the innate growth characteristics of the tumor relative to normal tissue (see Dr. Kufe’s lecture) and is much harder to achieve.
- Immunosuppressants are usually given in low, continuous dose regimens in order to maintain suppression of cellular and inflammatory responses to a persistent antigenic stimulus. In cancer chemotherapy high-dose pulse administration is more common because it allows for recovery of immune function and re-growth of normal cell populations.


