4.7: Lipid Uptake, Absorption and Transport
- Page ID
- 21628
Once mixed micelles reach the brush border of the enterocyte, two different lipid uptake mechanisms are believed to occur, but lipid uptake is not completely understood. One mechanism is that individual components of micelles may diffuse across the enterocyte. Otherwise, it is believed that some components may be taken up through unresolved transporters. For example, cholesterol transporters have been identified, but their overall mechanism of absorption is not well understood. The individual compounds are taken up as shown below.
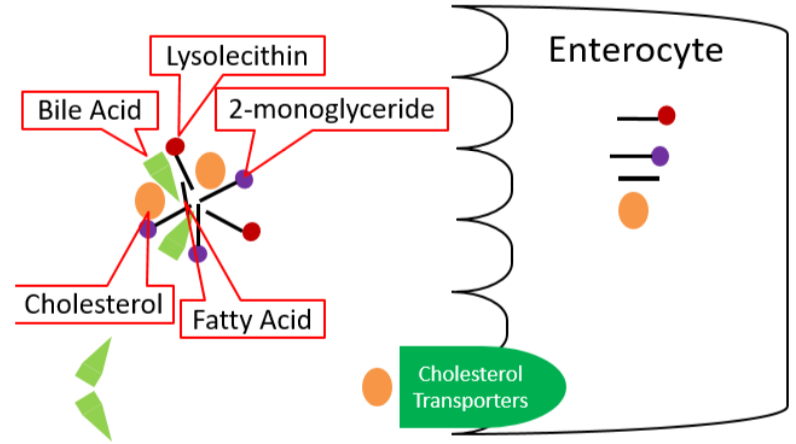
Once inside the enterocyte, there are different fates for fatty acids, depending on their length. Short- and medium-chain fatty acids move through the enterocyte and enter circulation through the capillaries; they are transported by the protein albumin. They will be carried to the liver by the portal vein, like monosaccharides and amino acids. Long-chain fatty acids, 2-monoglyceride, lysolecithin, and cholesterol will be re-esterified forming triglycerides, phosphatidylcholine, and cholesterol esters, respectively. These re-esterified lipids are then packaged into chylomicrons, which are lipoproteins, that are described in further detail in the next section. These chylomicrons are too large to fit through the pores in the capillaries, but they can fit through the larger fenestrations (openings) in the lacteal.
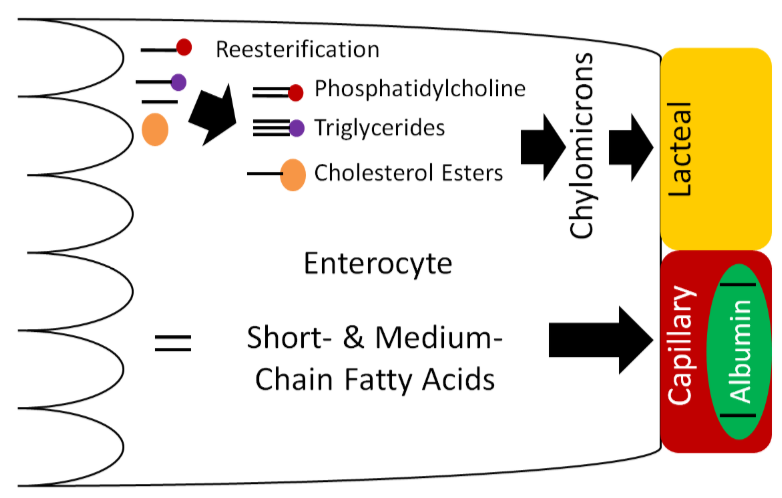
Lacteals (shown below) are small vessels that feed into the lymphatic system. Thus, the chylomicrons enter the lacteals and enter into lymphatic circulation.
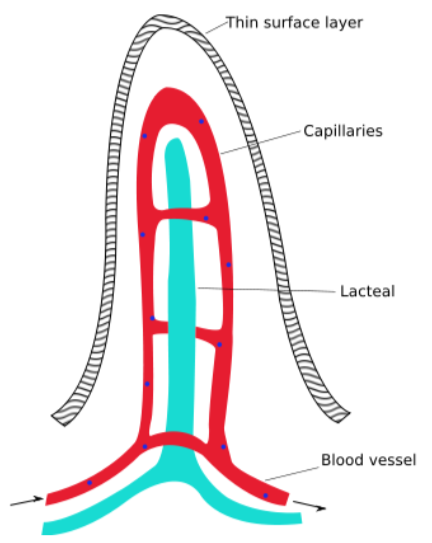
The lymphatic system is a system similar to the circulatory system in that it contains vessels that transport fluid. However, instead of blood, the lymphatic system contains a clear fluid known as lymph. There are a number of lymph nodes (small glands) within the lymphatic system that play a key role in the body's immune system. The figure below shows the lymphatic system.
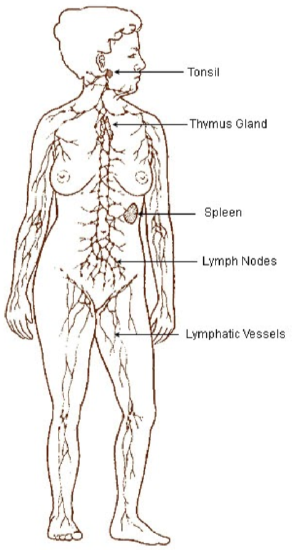
The following videos describe and illustrate how the lymphatic system and lymph functions.
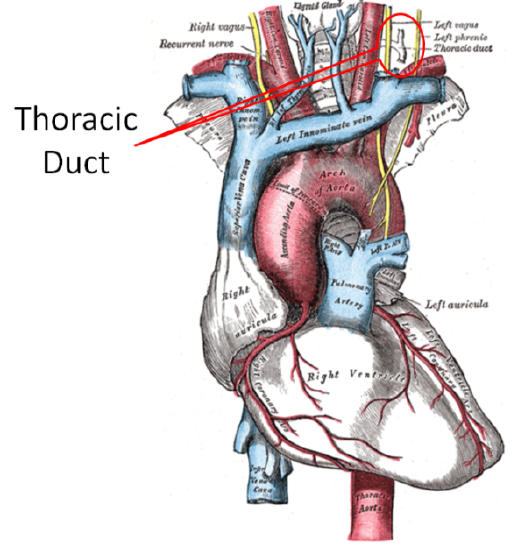
The lymphatic system enters general circulation through the thoracic duct that enters the left subclavian vein as shown below. General in this case means that it is not directed to the liver like other components that have been absorbed.
Lipoproteins
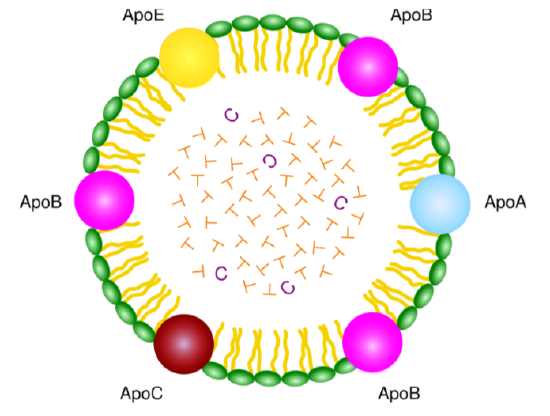
Lipoproteins, as the name suggests, are complexes of lipids and protein. The proteins within a lipoprotein are called apolipoproteins (aka apoproteins). There are a number of different apolipoproteins that are abbreviated apo-, then an identifying letter (i.e. Apo A) as shown in the chylomicron below.
The following video does a nice job of illustrating the different lipoprotein components.
There are a number of lipoproteins in the body. They differ by the apolipoproteins they contain, size (diameter), density, and composition. The table below shows the difference in density and diameter of different lipoproteins. Notice that as diameter decreases, density increases.
| Lipoprotein | Density (g/dL) | Diameter (nm) |
|---|---|---|
| Chylomicrons | 0.95 | 75-1200 |
| VLDL (very low-density lipoproteins) | 0.95-1.006 | 30-80 |
| IDL (intermediate-density lipoproteins) | 1.006-1.019 | 25-35 |
| LDL (low-density lipoproteins) | 1.019-1.063 | 18-25 |
| HDL (high-density lipoproteins) | 1.063-1.21 | 5-12 |
This inverse relationship is a result of the larger lipoproteins being composed of a higher percentage of triglyceride and a lower percentage of protein as shown below.
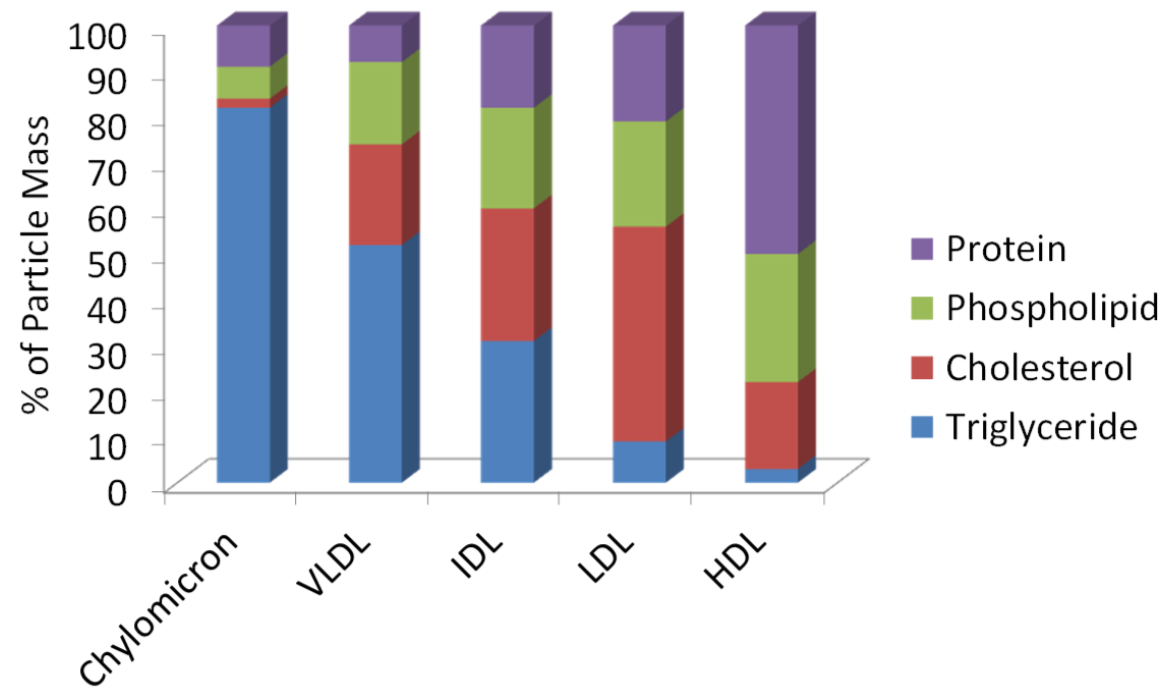
Protein is more dense than triglyceride (why muscle weighs more than fat), thus the higher protein/lower triglyceride composition, the higher the density of the lipoprotein. Many of the lipoproteins are named based on their densities (i.e. very low-density lipoproteins).
As described in the last subsection, the lipoproteins released from the small intestine are chylomicrons.
The endothelial cells that line blood vessels, especially in the muscle and adipose tissue, contain the enzyme lipoprotein lipase (LPL). LPL cleaves the fatty acids from lipoprotein triglycerides so that the fatty acids can be taken up into tissues. The figure below illustrates how endothelial cells are in contact with the blood that flows through the lumen of blood vessels.
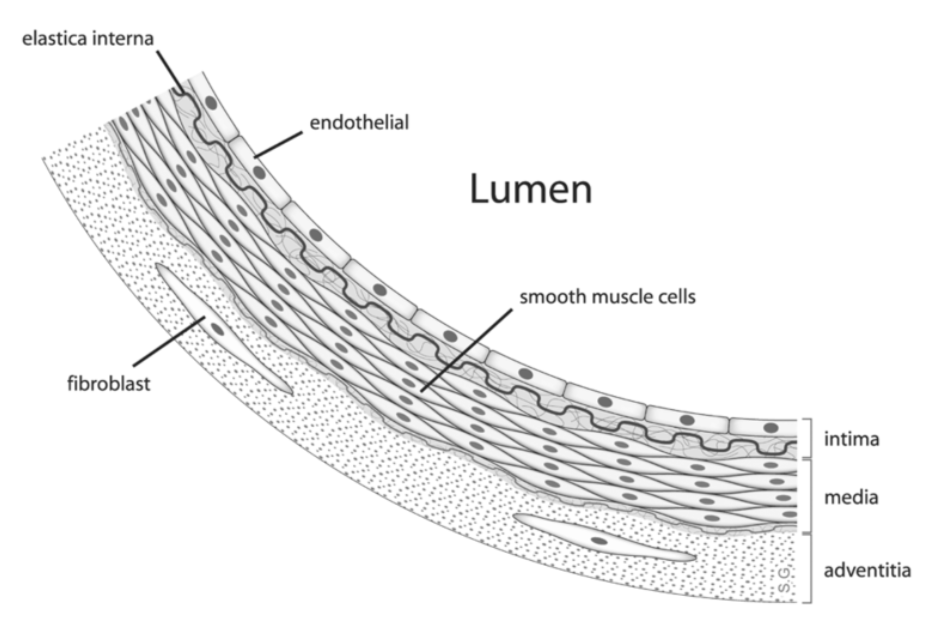
LPL cleaves fatty acids from the triglycerides in the chylomicron, decreasing the amount of triglyceride in the lipoprotein. This lipoprotein with less triglycerides becomes what is known as a chylomicron remnant, as shown below.
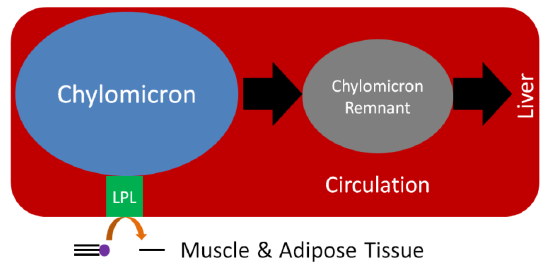
Now in the form of a chylomicron remnant, the digested lipid components originally packaged into the chylomicron are directed to the liver where the chylomicron remnant is endocytosed. This process of clearing chylomicrons from the blood takes 2-10 hours after a meal5. This is why people must fast 12 hours before having their blood lipids (triglycerides, HDL, LDL etc.) measured. This fast allows all the chylomicrons and chylomicron remnants to be cleared before blood is taken. However, whether patients should be asked to fast has been questioned.
After the chylomicron remnant is endocytosed, it is broken down to its individual components (triglycerides, cholesterol, protein etc.). In the liver, VLDL are produced, similar to how chylomicrons are produced in the small intestine. The individual components are packaged into VLDL and secreted into circulation as shown below.
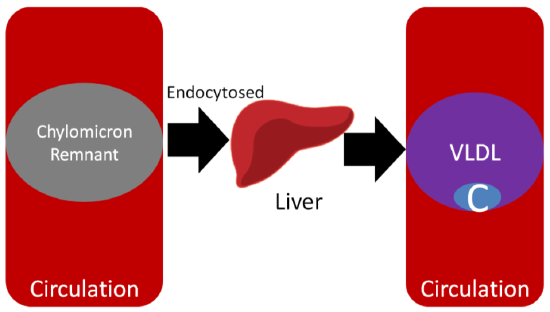
Like it does to chylomicrons, LPL cleaves fatty acids from triglycerides in VLDL, forming the smaller IDL (aka VLDL remnant). Further action of LPL on IDL results in the formation of LDL. The C in Figures 4.711 and 4.712 represents cholesterol, which is not increasing; rather, since triglyceride is being removed, it constitutes a greater percentage of particle mass of lipoproteins. As a result, LDL is composed mostly of cholesterol, as depicted in the figure below.
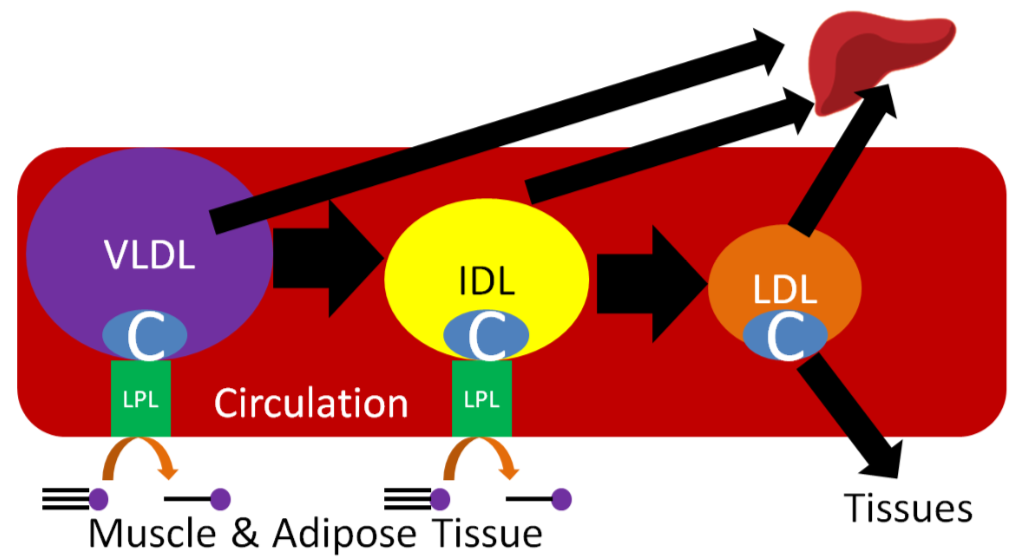
LDL contains a specific apolipoprotein (Apo B100) that binds to LDL receptors on the surface of target tissues. The LDL are then endocytosed into the target tissue and broken down to cholesterol and amino acids.
HDL are made up of mostly protein and are produced by the liver and small intestine. HDL participates in reverse cholesterol transport, which is the transport of cholesterol back to the liver. HDL picks up cholesterol from tissues/blood vessels and returns it to the liver itself or transfers it to other lipoproteins returning to the liver.
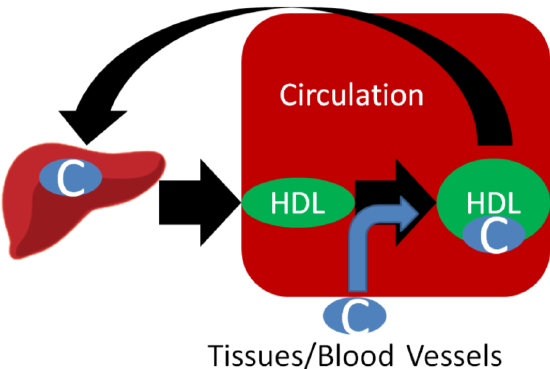
You are probably familiar with HDL and LDL being referred to as "good cholesterol" and "bad cholesterol," respectively. This is an oversimplification to help the public interpret their blood lipid values, because cholesterol is cholesterol; it's not good or bad. LDL and HDL are lipoproteins, and as a result you can't consume good or bad cholesterol, you consume cholesterol. A more appropriate descriptor for these lipoproteins would be HDL "good cholesterol transporter" and LDL "bad cholesterol transporter."
What's so bad about LDL? LDL enters the endothelium where it is oxidized. This LDL and/or oxidized LDL is engulfed by white blood cells (macrophages), leading to the formation of what are known as foam cells. The foam cells eventually accumulate so much LDL that they die and accumulate, forming a fatty streak. From there the fatty streak, which is the beginning stages of a lesion, can continue to grow until it blocks the artery. This can result in a myocardial infarction (heart attack) or a stroke. HDL is good in that it scavenges cholesterol from other lipoproteins or cells and returns it to the liver. The figure below shows the formation of the fatty streak and how this can progress to a point where it greatly alters blood flow.
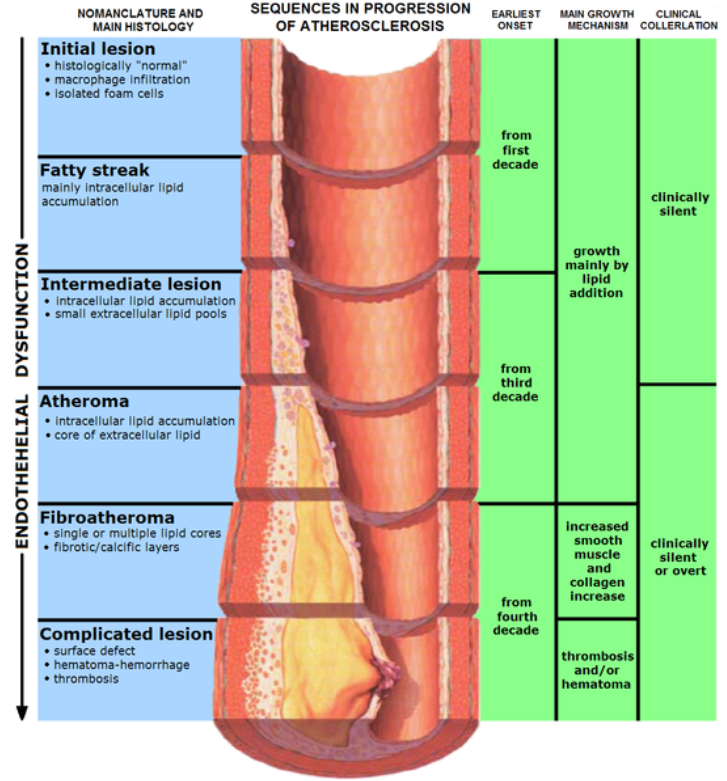
The video below does an excellent job of illustrating this process. However there are two caveats to point out. First, it incorrectly refers to cholesterol (LDL-C etc.), and second, it is clearly made by a drug company, so keep these factors in mind. The link below is the American Heart Association’s simple animation of how atherosclerosis develops.
Despite what you learned above about HDL, a recent study questions its importance in preventing cardiovascular disease. It found that people who have genetic variations that lead to higher HDL levels were not at decreased risk of developing cardiovascular disease. You can read more about this interesting finding in the link below.
References
- en.Wikipedia.org/wiki/File:In...simplified.svg
- en.Wikipedia.org/wiki/File:Il...tic_system.jpg
- en.Wikipedia.org/wiki/File:Gray505.png
- en.Wikipedia.org/wiki/File:Chylomicron.svg
- Byrd-Bredbenner C, Moe G, Beshgetoor D, Berning J. (2009) Wardlaw's perspectives in nutrition. New York, NY: McGraw-Hill.
- Gropper SS, Smith JL, Groff JL. (2008) Advanced nutrition and human metabolism. Belmont, CA: Wadsworth Publishing.
- en.Wikipedia.org/wiki/File:Anatomy_artery.png
- Erdman JW Jr., MacDonald IA, Zeisel SH, editors. (2012) Present knowledge in nutrition - 10th ed. Ames, IA: Wiley-Blackwell.
- en.Wikipedia.org/wiki/File:En...ion_Athero.PNG


