12.7: Iron
- Page ID
- 21692
There are 2 major dietary forms of iron: heme iron and non-heme iron. Heme iron is only found in foods of animal origin, within hemoglobin and myoglobin. The structure of heme iron is shown below.
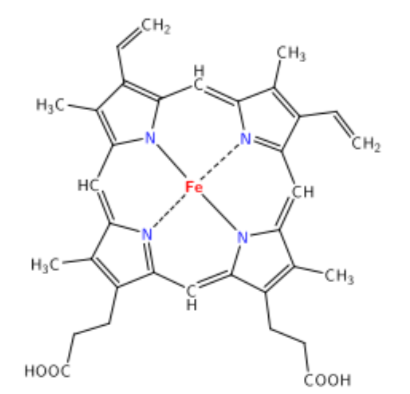
Approximately 40% of iron in meat, fish, and poultry is heme-iron, and the other 60% is non-heme iron2.
Non-heme iron is the mineral alone, in either its oxidized or reduced form. The 2 forms of iron are:
- Ferric (\(\ce{Fe^{3+}}\), oxidized)
- Ferrous (\(\ce{Fe^{2+}}\), reduced)
It is estimated that 25% of heme iron and 17% of non-heme iron are absorbed2. Approximately 85-90% of the iron we consume is non-heme iron2,3.
In addition to getting iron from food sources, if food is cooked in cast iron cookware, a small amount of iron can be transferred to the food.
Many breakfast cereals are fortified with reduced iron, which looks like iron filings, as the following video shows.
While the iron bioavailability of this reduced iron is low, some is absorbed4.
Supplements
Most iron supplements use ferrous (\(\ce{Fe^2+}\)) iron, because this form is better absorbed, as discussed in the next section. The figure below shows the percent of elemental iron in different supplements. This is the percentage of elemental iron that is in each compound.
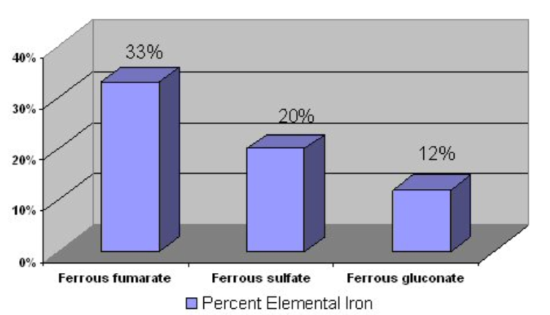
Iron chelates are marketed as being better absorbed than other forms of iron supplements, but this has not been proven5. It is recommended that supplements are not taken with meals, because they are better absorbed when not consumed with food2.
Iron Uptake & Absorption
There are 2 transporters for iron, one for heme iron and one for non-heme iron. The non-heme transporter is the divalent mineral transporter 1 (DMT1), which transports \(\ce{Fe^2+}\) into the enterocyte. Heme iron is taken up through heme carrier protein 1 (HCP-1), and then metabolized to \(\ce{Fe^2+}\). \(\ce{Fe^2+}\) may be used by enzymes and other proteins or stored in the enterocyte bound to ferritin, the iron storage protein. To reach circulation (and be absorbed), iron is transported through ferroportin5,6. This process is summarized in the figure below.
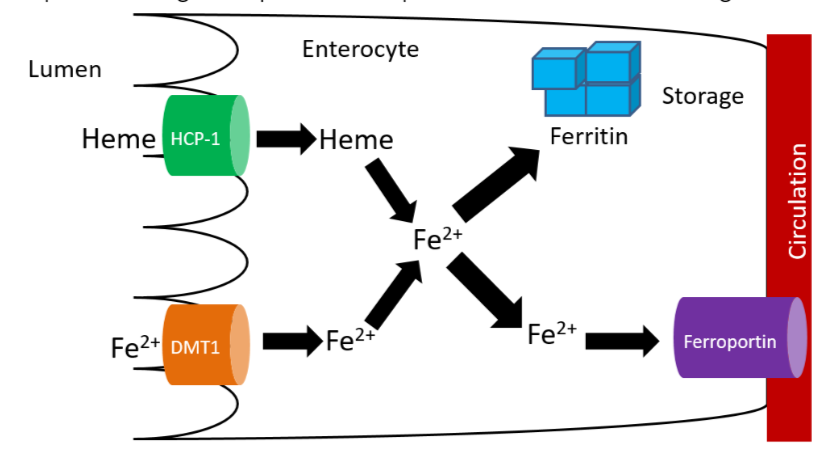
Since only the reduced form of non-heme iron (\(\ce{Fe^2+}\)) is taken up, \(\ce{Fe^3+}\) must be reduced. There is a reductase enzyme on the brush border, duodenal cytochrome b (Dcytb), that catalyzes the reduction of \(\ce{Fe^3+}\) to \(\ce{Fe^2+}\), as shown below. Vitamin C enhances non-heme iron absorption because it is required by Dcytb for this reaction. Thus, if dietary non-heme iron is consumed with vitamin C, more non-heme iron will be reduced to \(\ce{Fe^2+}\) and taken up into the enterocyte through DMT1. The exception is that vitamin C does not increase absorption of ferrous supplements because they are already in reduced form.
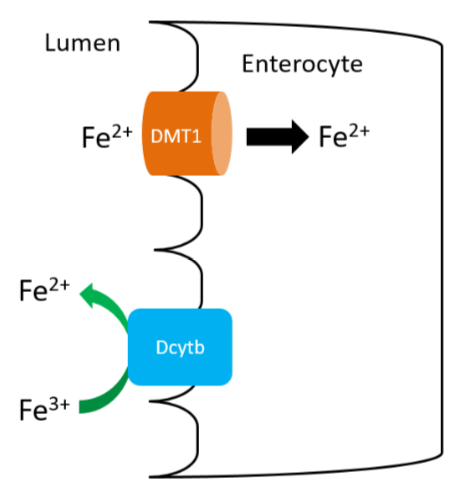
In addition to vitamin C, there is an unidentified factor in muscle that enhances non-heme iron absorption if consumed at the same meal7. This unidentified factor is referred to as meat protein factor (MPF). The table shows how MPF can increase non-heme iron absorption.
| Mean Fe Absorption
(% of Dose) |
Egg Albumin | Whole Muscle | Whole Muscle Protein | Heme-Free Muscle Protein |
|---|---|---|---|---|
| Chicken | 8.41 | 16.43 | 26.98 | 36.81 |
| Beef | 11.21 | 31.52 | 44.15 | 38.29 |
Albumin is a protein, so the egg albumin represents a non-meat protein standard for comparison. You can see that absorption is much higher with whole muscle. When only consuming muscle protein, there is a slight increase from muscle itself, and when they look at heme-free muscle iron, absorption is still higher than egg albumin7.
Inhibitors of non-heme iron absorption typically chelate, or bind, the iron to prevent absorption. Phytates (phytic acid), which also inhibit calcium absorption, chelate non-heme iron decreasing its absorption.

Other compounds that inhibit non-heme absorption are:
Polyphenols (coffee, tea)6

Oxalate (spinach, rhubarb, sweet potatoes, and dried beans)7

Calcium is also believed to inhibit iron uptake.
Iron Transport & Storage
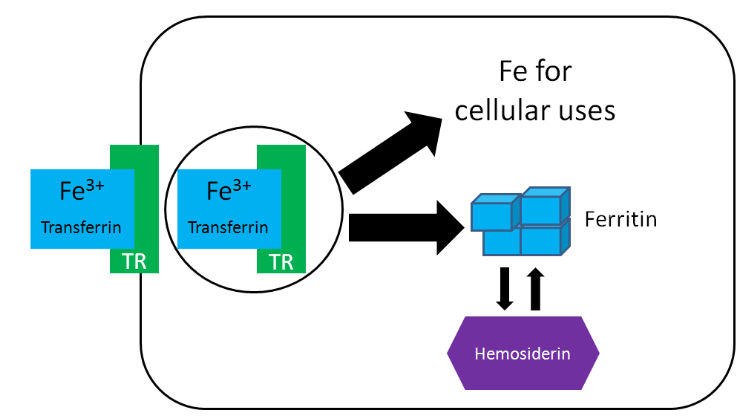
Transferrin is the major iron transport protein (transports iron through blood). \(\ce{Fe^3+}\) is the form of iron that binds to transferrin, so the \(\ce{Fe^2+}\) transported through ferroportin must be oxidized to \(\ce{Fe^3+}\). There are 2 copper-containing proteins that catalyze this oxidation of \(\ce{Fe^2+}\): hephaestin and ceruloplasmin. Hephaestin is found in the membrane of enterocytes, while ceruloplasmin is the major copper transport protein in blood. Hephaestin is the primary protein that performs this function in a coupled manner (occur together) with transport through ferroportin. This means that the \(\ce{Fe^2+}\) being transported through ferroportin is oxidized by hephaestin. Evidence suggests that ceruloplasmin is involved in oxidizing \(\ce{Fe^2+}\) when iron status is low11. Once oxidized, \(\ce{Fe^3+}\) binds to transferrin and is transported to a tissue cell that contains a transferrin receptor. Transferrin binds to the transferrin receptor and is endocytosed, as shown below5.

Once inside cells, the iron can be used for cellular purposes (cofactor for enzyme etc.) or it can be stored in the iron storage proteins ferritin or hemosiderin. Ferritin is the primary iron storage protein, but at higher concentrations, iron is also stored in hemosiderin5.
There are 3 major compartments of iron in the body12:
- Functional Iron
- Storage Iron
- Transport Iron
Functional iron consists of iron performing some function. There are 3 functional iron subcompartments.
- Hemoglobin
- Myoglobin
- Iron-containing enzymes
The functions of these subcompartments are discussed in the next section.
Iron Stores consist of:
- Ferritin
- Hemosiderin
The liver is the primary storage site in the body, with the spleen and bone marrow being the other major storage sites.
Circulating iron is found in transferrin12.
The following table shows how much iron is distributed among the different compartments.
| Men | Women | |
|---|---|---|
|
Functional iron |
||
|
Hemoglobin |
32 | 28 |
|
Myoglobin |
5 | 4 |
|
Fe-containing enzymes |
1-2 | 1-2 |
|
Storage iron |
||
|
Ferritin and hemosiderin |
~11 | ~6 |
|
Transport iron |
||
|
Transferrin |
0.04 | 0.04 |
Hopefully you notice that the majority of iron is in the functional iron compartment. The figure below further reinforces this point, showing that most iron is found in red blood cells (hemoglobin) and tissues (myoglobin).
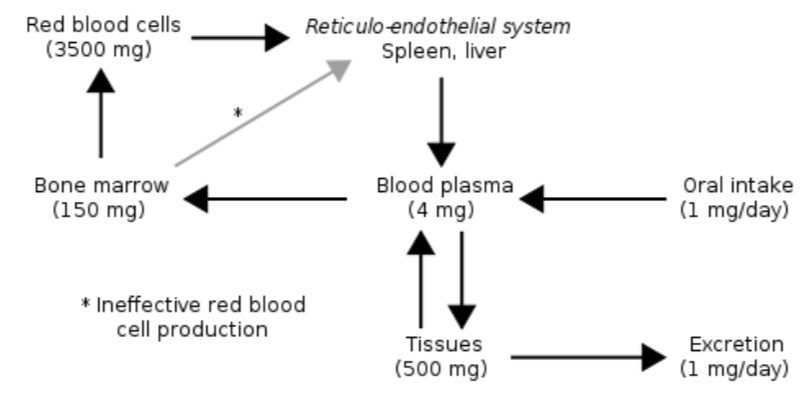
Also notice how small oral intake and excretion are compared to the amount found in the different compartments in the body. As a result, iron recycling is really important, because red blood cells only live for 120 days. Red blood cells are broken down in the liver, spleen, and bone marrow and the iron can be used for the same purposes as described earlier: cellular use, storage, or transported to another tissue on transferrin5. Most of this iron will be used for heme and ultimately red blood cell synthesis. The figure below summarizes the potential uses of iron recycled from red blood cells.
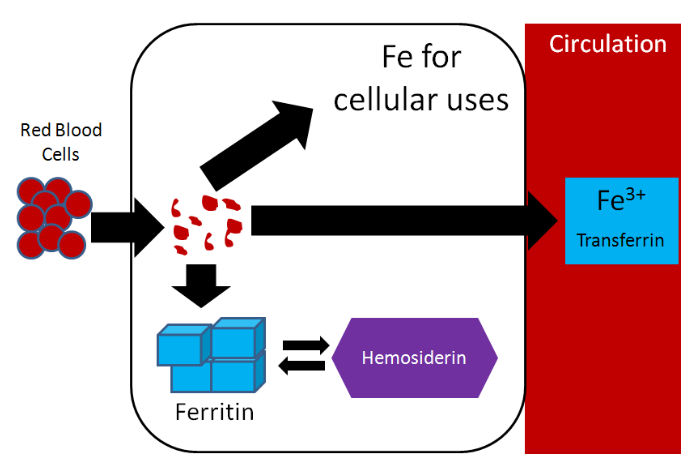
Iron is unique among minerals in that our body has limited ability to excrete it. Thus, absorption is really the only way to regulate iron status. Absorption is controlled by the hormone hepcidin. The liver has an iron sensor so when iron concentrations get high, this sensor signals for the release of hepcidin. Hepcidin travels to the enterocytes where it causes degradation of ferroportin. Thus, the iron is not able to be transported into circulation (since ferroportin is the transporter through which this typically occurs)14.
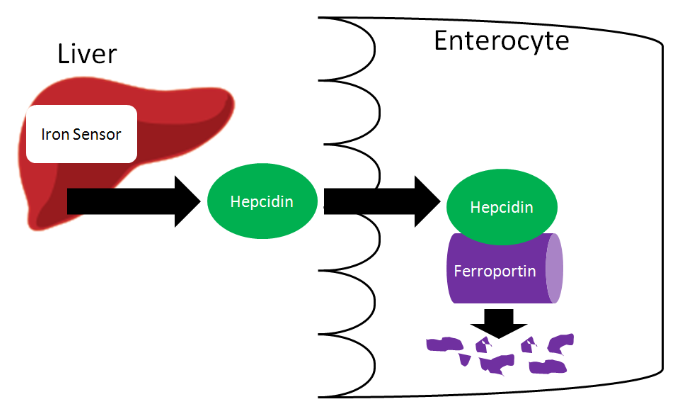
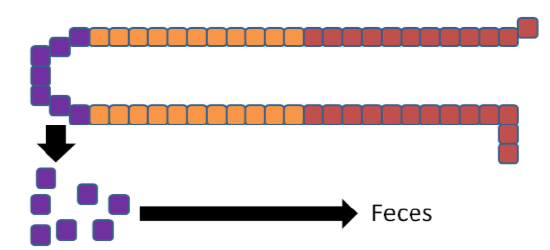
The iron is now trapped in the enterocytes, which are eventually sloughed off and mostly excreted in feces (some may be digested for uptake by new enterocytes on the villi). Thus, iron absorption is decreased through the action of hepcidin.
Iron Functions
As we talked about in the previous subsection, there are 3 primary functional iron subcompartments.
- Hemoglobin
- Myoglobin
- Iron-containing enzymes
Hemoglobin contains heme that is responsible for red blood cells’ red color. Hemoglobin allows red blood cells to carry oxygen to tissues as illustrated below.
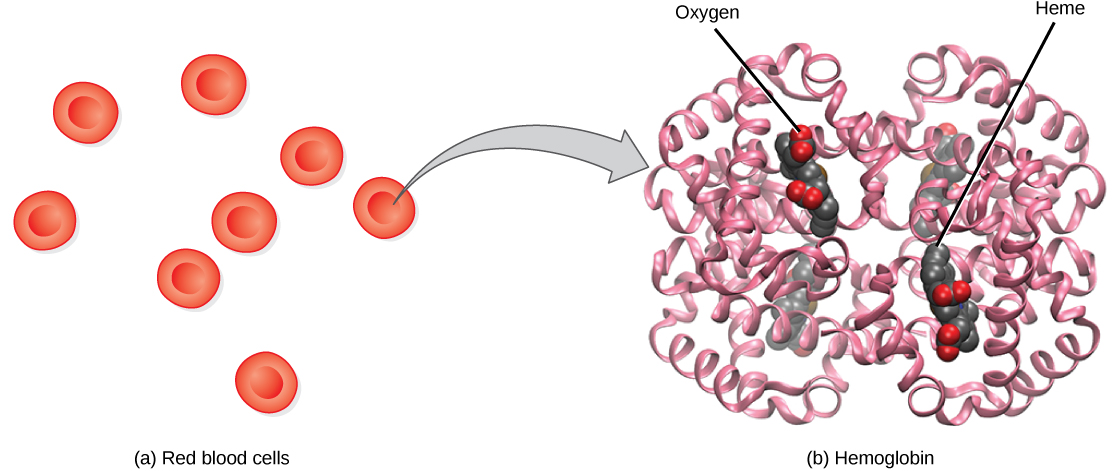
Myoglobin is similar to hemoglobin in that it can bind oxygen. However, instead of being found in blood, it is found in muscle. The color of meat products is a result of the state that myoglobin is in, as shown in the link below.
There are a number of enzymes that use iron as a cofactor. You've already learned about two.
Iron is a cofactor for the antioxidant enzyme, catalase, which converts hydrogen peroxide to water, as shown below.
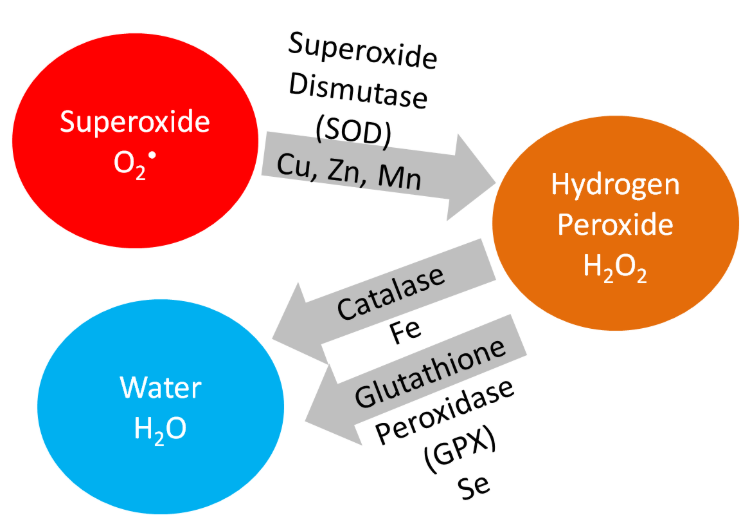
Iron is also a cofactor for prolyl and lysyl hydroxylases that are important in collagen cross-linking in tropocollagen. This was discussed previously in the vitamin C section. The function of these enzymes is shown below.
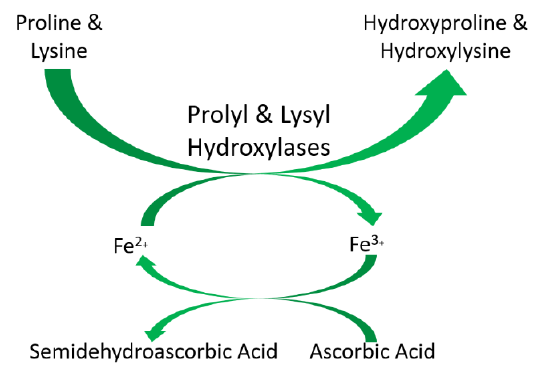
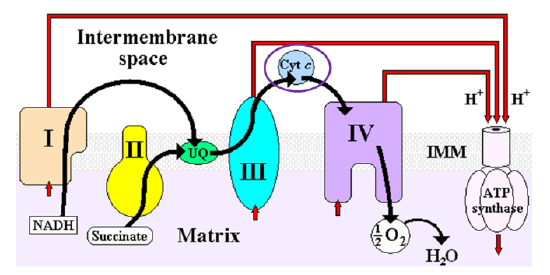
Heme iron is also found in cytochromes, like cytochrome c in the electron transport chain as shown below5.
Iron Deficiency & Toxicity
The levels of iron in the different compartments is illustrated by the figure below. The red above the table is meant to represent the amount of iron in the different compartments. In early negative iron balance stage, iron stores are slightly depleted. Once the stores are almost completely exhausted, this state is referred to as iron depletion. In iron deficiency, stores are completely exhausted and the circulating and functional iron levels are also depleted. In iron anemia, the circulating and functional iron levels are further depleted from iron-deficiency.
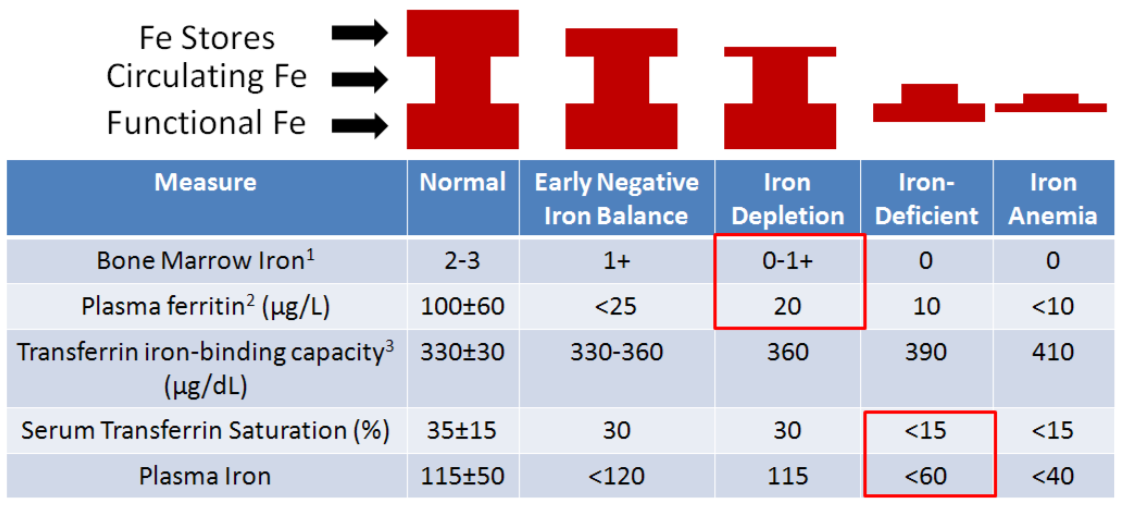
1 Great measure, but invasive
2 Small amount are released from liver, bone, and spleen – proportional to body stores
3 Also referred to as total iron-binding capacity
Figure \(\PageIndex{18}\): Measures of iron status5,12,17
The most common measures of iron status are hemoglobin concentrations and hematocrit (described below) levels. A decreased amount of either measure indicates iron deficiency, but these two measures are among the last to indicate that iron status is depressed. This is because, as you can see in the figure above, the functional iron compartment (which contains hemoglobin and is highly correlated to hematocrit values) is not altered until you reach iron deficiency. This is accomplished by using stores to maintain the circulating and functional iron compartments. It is important that you understand the limitations of these indicators so that you can interpret the meaning of their values5.
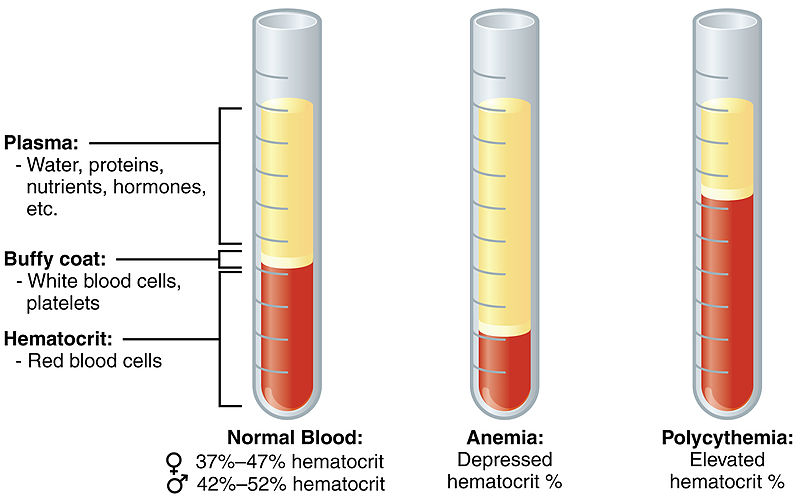
The hematocrit, as illustrated in the figure below, is a measure of the proportion of red blood cells (erythrocytes) as compared to all other components of blood. The components are separated by a centrifuge. The red blood cells remain at the bottom of the tube. They can be quantified by measuring the packed cell volume (PCV) relative to the total whole blood volume.
One of the best measures of iron status is bone marrow iron, but this is an invasive measure, and is therefore not commonly used. Plasma ferritin, the iron storage protein, is also found in lower amounts in the blood (plasma) and is a good indicator of iron stores. Thus, it is a sensitive measure to determine if someone is in negative iron status or iron depleted. It is not as useful of a measure beyond this stage because the iron stores have been exhausted for the most part. Transferrin iron binding capacity (aka total iron binding capacity), as it sounds, is a measure of how much iron transferrin can bind. An increase in transferrin iron binding capacity indicates deficiency (>400 indicates deficiency). But the best measure for deficiency or anemia is either percent serum transferrin saturation or plasma iron. A lower % saturation means that less of the transferrin is carrying the maximum amount of iron that they can handle. Plasma iron is easily understood as the amount of iron within the plasma19.
Iron deficiency is the most common deficiency worldwide, estimated to affect 1.6 billion people. In the US, it is less common, but an estimated 10% of toddlers and women of childbearing age are deficient. Iron deficiency often results in a microcytic (small cell), hypochromic (low color) anemia, that is a result of decreased hemoglobin production (there are other types of microcytic anemias). With decreased hemoglobin, the red blood cells cannot carry as much oxygen. Decreased oxygen leads to slower metabolism. Thus, a person with this anemia feels fatigued, weak, apathetic, and can experience headaches19. Other side effects include decreased immune function and delayed cognitive development in children20.
Those who are particularly at risk are5,20:
- Women of childbearing age - because of losses due to menstruation
- Pregnant women - because of increased blood volume
- Vegetarians/Vegans - because they do not consume heme iron sources
- Infants - because they have low iron stores that can quickly be depleted
To give you a better understanding of these risks, it is helpful to look at how much higher the RDAs are for women of reproductive age and pregnant women compared to men21.
Women of reproductive age 18 mg/day
Pregnancy 27 mg/day
Men 8 mg/day
To put this in perspective, 3 oz of beef contains ~3 mg of iron. Thus, it can be a challenge for some women to meet the requirement. The RDA committee estimates the iron requirements to be 80% and 70% higher for vegans and endurance athletes, respectively. The increased requirement for endurance athletes is based on loss due to "foot strike hemolysis", or the increased rupture of red blood cells due to the striking of the foot on hard surfaces17.
Iron toxicity is rare in adults, but can occur in children who consume too many supplements containing iron. Symptoms of this acute toxicity include nausea, vomiting, and diarrhea21.
50 out of 10,000 newborns in the United States are born with the genetic condition, hemochromatosis. In this condition, there is a mutation in a protein in the enterocyte that prevents the normal decrease of intestinal iron absorption. Without this protein these individuals cannot decrease iron absorption. Since the body cannot excrete iron, it accumulates in tissues, and ultimately can result in organ failure5.
References
- en.Wikipedia.org/wiki/File:Heme.svg
- Whitney E, Rolfes SR. (2011) Understanding nutrition. Belmont, CA: Wadsworth Cengage Learning.
- foodfix.ca/health.php#en65
- Garcia-Casal M, Layrisse M, Pena-Rosas J, Ramirez J, Leets I, et al. (2003) Iron absorption from elemental iron-fortified corn flakes in humans. role of vitamins A and C1-3. Nutr Res 23(4): 451-463.
- Gropper SS, Smith JL, Groff JL. (2008) Advanced nutrition and human metabolism. Belmont, CA: Wadsworth Publishing.
- Shils ME, Shike M, Ross AC, Caballero B, Cousins RJ, editors. (2006) Modern nutrition in health and disease. Baltimore, MD: Lippincott Williams & Wilkins.
- Hurrell R, Reddy M, Juillerat M, Cook J. (2006) Meat protein fractions enhance nonheme iron absorption in humans. J Nutr 136(11): 2808-2812.
- en.Wikipedia.org/wiki/File:Phytic_acid.png
- en.Wikipedia.org/wiki/File:Gallic_acid.svg
- en.Wikipedia.org/wiki/File:Calcium_oxalate.png
- Yehuda S, Mostofsky DI (2010) Iron Deficiency and Overload: From Basic Biology to Clinical Medicine. New York, NY. Humana Press.
- Stipanuk MH. (2006) Biochemical, physiological, & molecular aspects of human nutrition. St. Louis, MO: Saunders Elsevier.
- en.Wikipedia.org/wiki/File:Iron_metabolism.svg
- Nemeth E, Ganz T. (2006) Regulation of iron metabolism by hepcidin. Annu Rev Nutr 26: 323-342.
- https://commons.wikimedia.org/wiki/F...e_39_04_01.jpg
- http://wikidoc.org/index.php/File:ETC.PNG
- McGuire M, Beerman KA. (2011) Nutritional sciences: From fundamentals to food. Belmont, CA: Wadsworth Cengage Learning.
- https://commons.wikimedia.org/wiki/F...n_of_Blood.jpg
- Whitney E, Rolfes SR. (2011) Understanding nutrition. Belmont, CA: Wadsworth Cengage Learning.
- Byrd-Bredbenner C, Moe G, Beshgetoor D, Berning J. (2009) Wardlaw's perspectives in nutrition. New York, NY: McGraw-Hill.
- Anonymous. (2001) Dietary reference intakes for vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium, and zinc. Washington, D.C.: National Academies Press.


