4.6: Looking Closely at Diabetes
- Page ID
- 21116
Learning Objectives
- Compare and contrast Type 1 diabetes, Type 2 diabetes, and gestational diabetes.
- Describe the long-term health consequences of diabetes.
Diabetes is one of the top three diseases in America. It affects millions of people and causes tens of thousands of deaths each year. It has been estimated that by 2050, 1 in 3 American adults will have diabetes, which is closely related to the obesity epidemic in the U.S. Poorly treated or untreated diabetes has many serious side effects including kidney failure, blindness, limb loss and greatly accelerated risk of cardiovascular disease.
Diabetes is a metabolic disorder that results when the pancreas does not produce enough insulin to meet its needs or the body does not effectively utilize the insulin that it does produce. Remember from previous readings that insulin is one of the hormones that regulate blood glucose levels. The most common complication is hyperglycemia (elevated blood sugar), which gradually leads to damage in many of the body’s systems, most notably the eyes, kidneys, nerves, and heart and blood vessels. Uncontrolled diabetes can cause nerve damage, kidney damage, blindness, amputations, stroke, cardiovascular disease, and diabetic ketoacidosis (which can result in coma and/or death). Like other diseases, genetics, nutrition, environment, and lifestyle are all involved in determining a person’s risk for developing diabetes. There are three different types of diabetes: Type 1 diabetes, Type 2 diabetes, and gestational diabetes.
Type 1 Diabetes
Type 1 diabetes is an autoimmune condition in which the pancreas does not produce insulin. Type 1 diabetes accounts for 5-10% of diabetes cases. Its onset typically occurs before the age of thirty. The insulin-producing beta cells of the pancreas are destroyed so the body cannot produce enough insulin which causes hyperglycemia (high blood sugar). The only way to prevent the deadly symptoms of this disease is to inject insulin under the skin. Before this treatment was discovered, people with Type 1 diabetes died rapidly after disease onset. Death was the result of extremely high blood-glucose levels affecting brain function and leading to coma and death.
A person with Type 1 diabetes usually has a rapid onset of symptoms that include hunger, excessive thirst, excessive urination, and rapid weight loss (see Figure \(\PageIndex{1}\)). Because the main function of glucose is to provide energy for the body, when insulin is no longer present there is no message sent to cells to take up glucose from the blood. Instead, cells use fat and proteins to make energy, resulting in weight loss. If Type 1 diabetes goes untreated individuals with the disease will develop a life-threatening condition called ketoacidosis. This condition occurs when the body uses fats and not glucose to make energy, resulting in a build-up of ketone bodies in the blood. Ketoacidosis is a severe form of ketosis with symptoms of vomiting, dehydration, rapid breathing, and confusion. In extreme situations ketoacidosis can lead to coma and/or death.
People who have Type 1 diabetes must adhere to a strict diet to prevent the development of serious complications. Type 1 diabetics are advised to consume a diet low in the types of carbohydrates that rapidly spike glucose levels (high glycemic index foods), to count the carbohydrates they eat, to consume healthy-carbohydrate foods, to eat small meals frequently, and to inject appropriate amounts of insulin based on the amount of carbohydrates eaten. These guidelines are aimed at preventing large fluctuations in blood glucose.

Type 2 Diabetes
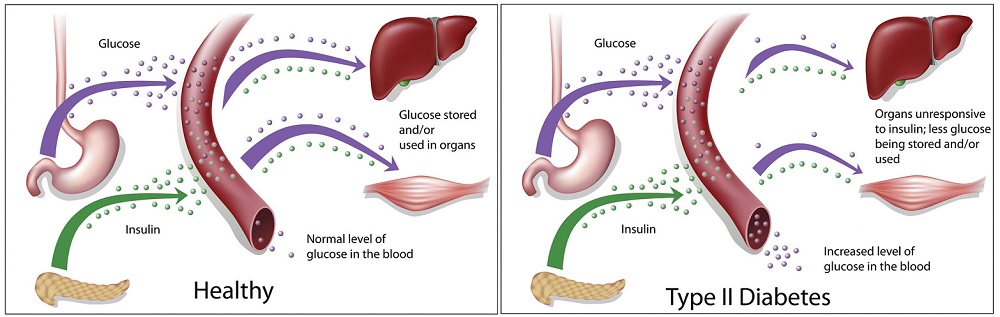
The other 90-95% of diabetes cases are Type 2 diabetes. Type 2 diabetes results when the pancreas produces enough insulin initially, but the body's cells no longer respond appropriately and are unable to use the hormone properly (insulin resistance). During insulin resistance, the body's cells no longer receive the full physiological message of insulin to take up glucose from the blood (Figure \(\PageIndex{2}\)). Hyperglycemia results because cells cannot take in the glucose from the blood. Thus, similar to patients with Type 1 diabetes, those with Type 2 diabetes also have high blood-glucose levels.
For Type 2 diabetics, the onset of symptoms is more gradual and less noticeable than for Type 1 diabetics. The symptoms are increased thirst and urination, unexplained weight loss, and hunger. The first stage of Type 2 diabetes is characterized by high glucose and insulin levels. This is because the insulin-secreting cells in the pancreas attempt to compensate for insulin resistance by making more insulin. In the second stage of Type 2 diabetes, the insulin-secreting cells in the pancreas become exhausted and die. At this point, Type 2 diabetics also have to be treated with insulin injections. As with Type 1 diabetes, chronically high-glucose levels cause big detriments to health over time, so another goal for patients with Type 2 diabetes is to properly manage their blood-glucose levels. Since major contributing factors to the development of Type 2 diabetes include excessive body weight and physical inactivity, the front-line approach for treating Type 2 diabetes includes eating a healthy diet and increasing physical activity.
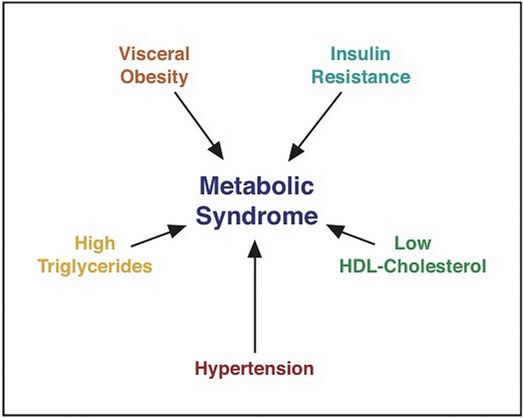
Genetics, environment, nutrition, and lifestyle all play a role in determining a person’s risk for Type 2 diabetes. Having more than one risk factor for Type 2 diabetes substantially increases a person’s chances for developing the disease. Metabolic syndrome refers to a medical condition in which people have three or more risk factors for Type 2 diabetes and cardiovascular disease (Figure \(\PageIndex{3}\)). According to the International Diabetes Federation (IDF) people are diagnosed with this syndrome if they have central (abdominal) obesity and any two of the following health parameters: triglycerides greater than 149 mg/dL; high density lipoproteins (HDL) lower than 40 mg/dL for males (lower than 50 mg/dL for females); systolic blood pressure above 129 mmHg, or diastolic blood pressure above 84 mmHg; fasting blood glucose levels greater than 99 mg/dL.1 The IDF estimates that 20-25% of adults worldwide have metabolic syndrome and people with metabolic syndrome are 5 times more likely to develop Type 2 diabetes.1
Prediabetes
As the term infers, prediabetes is a metabolic condition in which people have moderately high glucose levels, but do not meet the criteria for a diabetes diagnosis. One out of every three adults in the United States have prediabetes.2 Over time, people with prediabetes may develop Type 2 diabetes. Although researchers don't fully understand what causes prediabetes, excess weight and lack of physical activity are considered to be major factors.
Gestational Diabetes
During pregnancy some women develop gestational diabetes. Gestational diabetes is characterized by high blood-glucose levels and insulin resistance. The exact cause is not known but does involve the effects of pregnancy hormones on how cells respond to insulin. Gestational diabetes can cause pregnancy complications and it is common practice for healthcare practitioners to screen pregnant women for this metabolic disorder. The disorder normally ceases when the pregnancy is over, but women who had gestational diabetes are more likely to develop Type 2 diabetes later in life.3 Gestational diabetes not only affects the health of a pregnant woman but also is associated with an increased risk of obesity and Type 2 diabetes in her child.
Long-Term Health Consequences of Diabetes
The long-term health consequences of diabetes are severe and result from chronically high glucose concentrations in the blood accompanied by other metabolic abnormalities such as high blood lipid levels. People with diabetes are about twice as likely to die from cardiovascular disease compared to people without diabetes.4 Diabetes is the number one cause of new cases of blindness, lower-limb amputations, and kidney failure. Many people with diabetes develop peripheral neuropathy, characterized by muscle weakness, loss of feeling and pain in the lower extremities.
Diabetes Treatment
Keeping blood glucose levels in the target range (80–130 mg/dL before a meal) requires careful monitoring of blood-glucose levels with a blood glucose meter, strict adherence to a healthy diet, and increased physical activity. Type 1 diabetics begin insulin injections as soon as they are diagnosed (Figure \(\PageIndex{4}\)).
Type 2 diabetics may require oral medications and insulin injections to maintain blood glucose levels in the target range. The symptoms of high blood glucose, also called hyperglycemia, are difficult to recognize, diminish in the course of diabetes, and are mostly not apparent until levels become very high. The symptoms are increased thirst and frequent urination.
Having too low blood glucose levels, known as hypoglycemia, is also detrimental to health. Hypoglycemia is more common in Type 1 diabetics and is most often caused by injecting too much insulin or injecting it at the wrong time. The symptoms of hypoglycemia are more acute including shakiness, sweating, nausea, hunger, clamminess, fatigue, confusion, irritability, stupor, seizures, and coma. Hypoglycemia can be rapidly and simply treated by eating foods containing about 15 grams of simple carbohydrates (e.g., 1/2 cup of fruit juice). If symptoms are severe a person is either treated by emergency care providers with an intravenous solution of glucose or given an injection of glucagon, which breaks down glycogen in the liver into glucose.
Some people who are not diabetic may experience reactive hypoglycemia. This is a condition in which people are sensitive to the intake of sugars, refined starches, and high glycemic index foods. Individuals with reactive hypoglycemia have some symptoms of hypoglycemia. Symptoms are caused by a higher than normal increase in blood insulin levels. This rapidly decreases blood glucose levels to a level below what is required for proper brain function.
The major determinants of Type 2 diabetes that can be changed are overnutrition and a sedentary lifestyle. Therefore, reversing or improving these factors by lifestyle interventions can markedly improve the overall health of Type 2 diabetics and lower blood glucose levels. In fact, it has been shown that losing 5-7% of body weight and increasing physical activity to at least 150 minutes per week reduced the risk of developing Type 2 diabetes by 58% in adults at high risk.5
Key Takeaways
- Diabetes is a disease of insulin deficiency and glucose excess. Like other diseases, genetics, nutrition, environment, and lifestyle are all involved in determining a person’s risk for developing diabetes.
- Type 1 diabetes is treated with insulin injections. However, insulin injections do not cure the disease, and diabetics can suffer many disease complications. Diabetes complications can be relieved by strictly managing blood glucose levels, adhering to a healthy diet, and increasing physical activity.
- The front-line approach for treating Type 2 diabetes includes eating a healthy diet and increasing physical activity.
- The long-term health consequences of diabetes are severe and result from chronically high glucose concentrations in the blood and other metabolic abnormalities such as high blood lipid levels.
References
- IDF Consensus Worldwide Definition of the Metabolic Syndrome.idf.org. www.idf.org/e-library/consensus-statements/60-idfconsensus-worldwide-definitionof-the-metabolic-syndrome.html. Updated May 4, 2017. Accessed June 13, 2020.
- Insulin Resistance and Prediabetes. niddk.nih.gov. https://www.niddk.nih.gov/health-information/diabetes/overview/what-is-diabetes/prediabetes-insulin-resistance. Accessed June 13, 2020.
- Definition and Facts of Gestational Diabetes. niddk.nih.gov. https://www.niddk.nih.gov/health-information/diabetes/overview/what-is-diabetes/gestational/definition-facts. Accessed June 13, 2020.
- Emerging Risk Factors Collaboration, Sarwar N, Gao P, et al. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies [published correction appears in Lancet. 2010 Sep 18;376(9745):958. Hillage, H L [corrected to Hillege, H L]]. Lancet. 2010;375(9733):2215‐2222. doi:10.1016/S0140-6736(10)60484-9.
- Research Behind the National DPP. cdc.gov. https://www.cdc.gov/diabetes/prevention/research-behind-ndpp.htm. Accessed June 13, 2020.

