9.1: Bone Structure and Function
- Page ID
- 21154
Learning Objectives
- Identify the functions of the skeletal system.
- Identify the two types of bone tissue.
- Explain the process of bone remodeling.
Your bones are stronger than reinforced concrete. Bone tissue is a composite of fibrous collagen strands that resemble the steel rebar in concrete and a hardened mineralized matrix that contains large amounts of calcium, just like concrete. But this is where the similarities end. Bone outperforms reinforced concrete by several orders of magnitude in compression and tension strength tests. Why? The microarchitecture of bone is complex and built to withstand extreme forces. Moreover, bone is a living tissue that is continuously breaking down and forming new bone to adapt to mechanical stresses.
Why is the Skeletal System Important?
The human skeleton consists of 206 bones and other connective tissues called ligaments, tendons, and cartilage. Ligaments connect bones to other bones, tendons connect bones to muscles, and cartilage provides bones with more flexibility and acts as a cushion in the joints between bones. Bone has multiple functions related to structure, support, and metabolic processes as outlined in Table \(\PageIndex{1}\) below.
| Functions Related to Structure and Support | Functions Related to Metabolic Processes |
|---|---|
|
|
Bone Anatomy and Structure
The composition of bone allows for the bone to be hard and flexible at the same time. Bone contains about 65% minerals (e.g., calcium, phosphorus) that provide the hardness of bone. The other 35% of bone is made up of organic structures (e.g., collagen) that provide strength, durability, and flexibility. Bones consist of two different tissue types. There is spongy (or trabecular) bone and compact (or cortical) bone (Figure \(\PageIndex{1}\)).
- Trabecular bone is 50-90% porous and appears as a lattice-like structure under the microscope. Trabecular bone supports cortical bone and can be thought of as the "scaffolding" on the inside of bones. It is found at the ends of long bones, in the cores of vertebrae, inside flat bones, and in the pelvis. Trabecular bone tissue makes up about 20% of the adult skeleton.
- Cortical bone is found on the outer surface of all bones. The more dense cortical bone is about 10% porous and makes up approximately 80% of the adult skeleton. It surrounds all trabecular tissue and is the only bone tissue in the shafts of long bones.
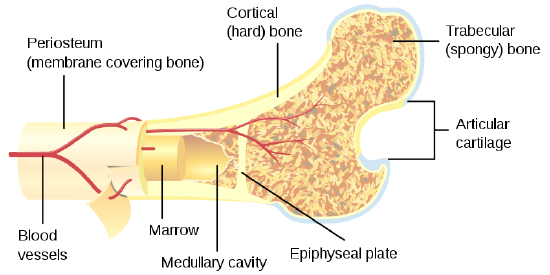
Bone tissue is arranged in an organized manner. A thin membrane, called the periosteum, surrounds the bone; it contains connective tissue with many blood vessels and nerves. Lying below the periosteum is the cortical bone. In some bones, the cortical bone surrounds the less-dense trabecular bone and the bone marrow lies within the trabecular bone, but not all bones contain trabecular tissue or marrow.
Bone Tissues and Cells
Bone tissue contains many different cell types that constantly resize and reshape bones throughout growth and adulthood. Bone tissue cells include osteoprogenitor cells, osteoblasts, osteoclasts, and osteocytes. The osteoprogenitor cells are cells that have not matured yet. Once they are stimulated, some will become osteoblasts, the bone builders, and others will become osteoclasts, the cells that break bone down. Osteocytes are the most abundant cells in bone tissue. Osteocytes are star-shaped cells that are connected throughout the bone and exchange nutrients from bones to the blood and lymph.
Bone Modeling and Remodeling
During infancy, childhood, and adolescence, bones are continuously growing and changing shape through two processes called growth and modeling. In fact, in the first year of life, almost 100% of the bone tissue in the skeleton is replaced. In the process of modeling, bone tissue is dismantled at one site and built up at a different site. In adulthood, our bones stop growing and modeling, but continue to go through a process of bone remodeling. In the process of remodeling, bone tissue is degraded and built up at the same location. Bone remodeling has multiple purposes including repairing damaged bone, recycling bone tissue, and maintaining blood calcium levels. About 10 percent of bone tissue is remodeled each year in adults.
The first step in bone remodeling is osteocyte activation. Osteocytes detect changes in mechanical forces, calcium homeostasis, or hormone levels. In the second step, osteoclasts are recruited to the site of the degradation. Osteoclasts are large cells with a highly irregular ruffled membrane (Figure \(\PageIndex{2}\))2. These cells fuse tightly to the bone and secrete hydrogen ions, which acidify the local environment and dissolve the minerals in the bone tissue matrix. This process is called bone resorption and resembles pit excavation. Our bodies excavate pits in our bone tissue because bones act as storehouses for calcium and other minerals. Bones supply these minerals to other body tissues as the demand arises. Bone tissue also remodels when it breaks so that it can repair itself.
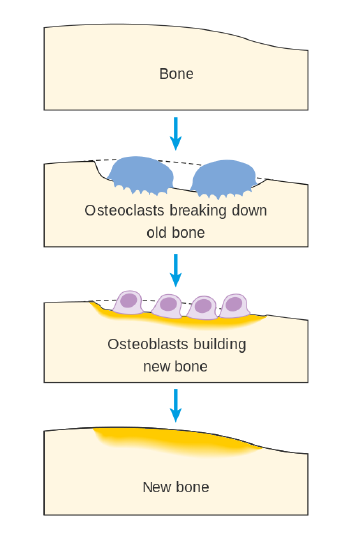
After a certain amount of bone is excavated, the osteoclasts begin to die and bone resorption stops. In the third step of bone remodeling, the site is prepared for building. In this stage, sugars and proteins accumulate along the bone’s surface, forming a cement line which acts to form a strong bond between the old bone and the new bone that will be made. These first three steps take approximately two to three weeks to complete. In the last step of bone remodeling, osteoblasts lay down new osteoid tissue that fills up the cavities that were excavated during the resorption process (Figure \(\PageIndex{2}\)). Osteoid is bone matrix tissue that is composed of proteins such as collagen and is not mineralized yet. To make collagen, vitamin C is required. A symptom of vitamin C deficiency (known as scurvy) is bone pain, which is caused by diminished bone remodeling. After the osteoid tissue is built up, the bone tissue begins to mineralize. The last step of bone remodeling continues for months, and for much longer afterwards, the mineralized bone is continuously packed in a more dense fashion.
Thus, we can say that bone is a living tissue that continually adapts itself to mechanical stress through the process of remodeling. For bone tissue to remodel, certain nutrients such as calcium, phosphorus, magnesium, fluoride, vitamin D, and vitamin K are required. Watch these short videos for more on osteoblasts, osteoclasts, and bone remodeling:
"Osteoblasts and Osteoclasts" by Amgen
"Bone Remodeling and Modeling" by Amgen
Key Takeaways
- The skeletal system aids in movement, provides support for and protects organs, synthesizes platelets and red and white blood cells, and serves as a storage depot for minerals, such as calcium.
- Bones consist of two different tissue types: compact (cortical) bone and trabecular (spongy) bone.
- Bone remodeling is a multifaceted process involving four steps: osteocyte activation, osteoclast-mediated bone resorption, surface preparation, and osteoblast-mediated bone building.
- The bone remodeling process requires certain nutrients such as calcium, phosphorus, magnesium, fluoride, vitamin D, and vitamin K.

