9.2: Micronutrients Essential for Bone Health - Calcium and Vitamin D
- Page ID
- 21155
Learning Objectives
- Describe the functions of calcium and vitamin D.
- Describe how blood calcium levels are regulated.
- Give examples of good food sources of calcium and vitamin D.
Calcium
The most abundant mineral in the body is calcium, and greater than 99% of it is stored in bone tissue. Although only 1% of the calcium in the human body is found in the blood and soft tissues, it is here that it performs the most critical functions. Blood calcium levels are rigorously controlled so that if blood levels drop the body will rapidly respond by stimulating bone resorption, thereby releasing stored calcium into the blood. Thus, bone tissue sacrifices its stored calcium to maintain blood calcium levels. This is why bone health is dependent on the intake of dietary calcium and also why blood levels of calcium do not always correspond to dietary intake.
Functions of Calcium
Calcium plays a role in a number of different functions in the body:
- Bone and tooth formation. The most well-known calcium function is to build and strengthen bones and teeth. Recall that when bone tissue first forms during the modeling or remodeling process, it is unhardened, protein-rich osteoid tissue. In the osteoblast-directed process of bone mineralization, calcium phosphates (salts) are deposited on the protein matrix. The calcium salts gradually crystallize into hydroxyapatite, which typically makes up about 65 percent of bone tissue. When your diet is calcium deficient, the mineral content of bone decreases causing it to become brittle and weak. Thus, increased calcium intake helps to increase the mineralized content of bone tissue which leads to greater bone strength.
- Nerve impulse transmission. Calcium facilitates electrical impulse transmission from one nerve cell to another. Calcium binds to vesicles that contain neurotransmitters, causing a release into the neural synapses (junction between nerve cells). This allows the flow of ions in and out of nerve cells. If calcium is lacking, nerve-cell function will fail.
- Muscle contraction. The flow of calcium ions along the muscle cell’s surface and the influx of calcium into the muscle cell are critical for muscle contraction. If calcium levels fall below a crucial range, the muscles can’t relax after contracting. The muscles become stiff and involuntary twitching may ensue in a condition known as tetany.
- Clotting factors. When a blood vessel is injured and bleeding starts, it must be stopped or death may result. Clotting factors and platelets are continuously circulating in the blood in case of such an emergency. When an injury occurs, the damaged tissue releases specific factors that activate the circulating clotting factors and platelets. Some of the clotting factors require calcium for activation. If clotting factors weren’t activated, blood clots would not form.
In addition to these primary functions calcium has several other minor functions that are also critical for maintaining normal physiology. For example, without calcium, the hormone insulin could not be released from cells in the pancreas and glycogen could not be broken down in muscle cells and used to provide energy for muscle contraction.
Maintaining Calcium Levels
Because calcium performs such vital functions in the body, blood calcium levels are closely regulated by the hormones parathyroid hormone (PTH), calcitriol, and calcitonin. Calcitriol is the active hormone produced from vitamin D. Parathyroid hormone and calcitriol act in a concert to increase calcium levels in the blood, while calcitonin does the opposite and decreases blood calcium levels. These hormones maintain calcium levels in the blood in a range between 9 and 11 milligrams per deciliter.
Parathyroid Hormone
Four parathyroid glands, each the size of a grain of rice, can be found in the neck on the sides of the thyroid gland. PTH increases blood calcium levels via three different mechanisms (Figure \(\PageIndex{1}\)). First, PTH stimulates the release of calcium stored in the bone. Second, PTH acts on kidney cells to increase calcium reabsorption and decrease its excretion in the urine. Third, PTH stimulates enzymes in the kidney that activate vitamin D to calcitriol which acts on intestinal cells to increase dietary calcium absorption. Thus, stored calcium is released, more calcium is absorbed from the diet, and less calcium is excreted, all of which increase calcium levels in the blood.
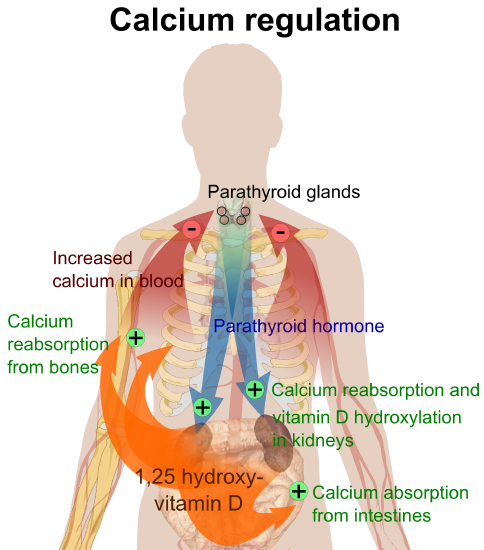
Calcitriol (1,25-dihydroxyvitamin D3)
Calcitriol functions as a second hand to PTH. It not only increases calcium release from bone tissue, but also it increases the absorption of calcium in the small intestine and increases calcium reabsorption by the kidneys. Neither hormone will work unless accompanied by the other. Vitamin D regulates PTH secretion and PTH regulates vitamin D activation to calcitriol. Adequate levels of vitamin D allow for a balance of the calcium between what is released by bone tissue and what is incorporated into bone tissue, so that bone health is not compromised. Calcitriol and PTH function together to maintain calcium homeostasis.
Calcitonin
Calcitonin is a hormone secreted by certain cells in the thyroid gland in response to high calcium levels in the blood. In comparison to PTH and calcitriol, calcitonin plays a small role in regulating calcium levels on a day-to-day basis. This is because as calcium levels rise in the blood, calcium feedback inhibits PTH release and effectively shuts off the actions of PTH and calcitriol. This route of feedback inhibition helps prevent calcium’s further accumulation in the blood. When needed, calcitonin lowers blood calcium levels by increasing calcium excretion in the urine, preventing further absorption of calcium in the gut and by directly inhibiting bone resorption.
Calcium Imbalances
As noted above, most excess calcium from food is excreted from the body. However, excessive intake from calcium supplements can lead to mineral imbalances (e.g., iron, zinc, magnesium). Hypercalcemia (high blood calcium levels) can be caused by cancer or overproduction of parathyroid hormone (PTH) as discussed in detail above.
Hypocalcemia (low blood calcium) can be caused by kidney disease, vitamin D deficiency, or limited PTH production. A long term effect of low calcium intake is known as osteoporosis (very low bone density); osteoporosis is discussed in more detail later in this chapter.
Calcium Recommendations
The Dietary Reference Intakes (DRIs) for calcium are listed in Table \(\PageIndex{1}\). The RDA increases to 1,300 milligrams per day during adolescence because this is the life stage with accelerated bone growth. Studies have shown that a higher intake of calcium during puberty increases the total amount of bone tissue that accumulates in the body. The bioavailability (degree to which our bodies can absorb and utilize any nutrient) of calcium is also considered in the recommendations. When calcium needs are high (infants, children, and pregnant and lactating women), our bodies can generally absorb more calcium. As we age, our ability to absorb nutrients generally decreases. This is why the RDAs for women older than 50 and men older than 70 are a bit higher. As we age, calcium absorption in the gut decreases, vitamin D3 activation is reduced, and maintaining adequate blood levels of calcium is important to prevent an acceleration of bone tissue loss.
| Age Group | RDA (mg/day) | UL (mg/day) |
|---|---|---|
| Infants (0–6 months) | 200* | 1,000 |
| Infants (7–12 months) | 260* | 1,500 |
| Children (1–3 years) | 700 | 2,500 |
| Children (4–8 years) | 1,000 | 2,500 |
| Children (9–13 years) | 1,300 | 3,000 |
| Adolescents (14–18 years) | 1,300 | 3,000 |
| Adults (19–50 years) | 1,000 | 2,500 |
| Adults (51–70 years) | 1,000 (males), 1,200 (females) | 2,000 |
| Adults (> 70 years) | 1,200 | 2,000 |
| * denotes Adequate Intake | ||
Sources of Calcium
Calcium can be obtained from dairy product as well as nondairy sources of calcium (Table \(\PageIndex{2}\)).
| Food | Calcium (mg) | % Daily Value |
|---|---|---|
| Yogurt, low fat, plain (8 ounces) | 415 | 32 |
| Almonds (1 cup) | 385 | 30 |
| Orange juice, calcium fortified (1 cup) | 349 | 27 |
| Sardines, canned in oil, with bones (3 ounces) | 325 | 25 |
| Cheddar cheese (1½ ounces) | 307 | 24 |
| Soymilk, calcium fortified (1 cup) | 299 | 23 |
| Milk, reduced fat 2% (1 cup) | 293 | 23 |
| Tofu, firm, made with calcium sulfate (½ cup) | 253 | 19 |
| Chickpeas/garbanzo beans (1 cup) | 210 | 16 |
| Kale, cooked from frozen (1 cup) | 179 | 14 |
Learn even more about this nutrient by reading the Calcium Fact Sheet from the National Institutes of Health, Office of Dietary Supplements.
Vitamin D
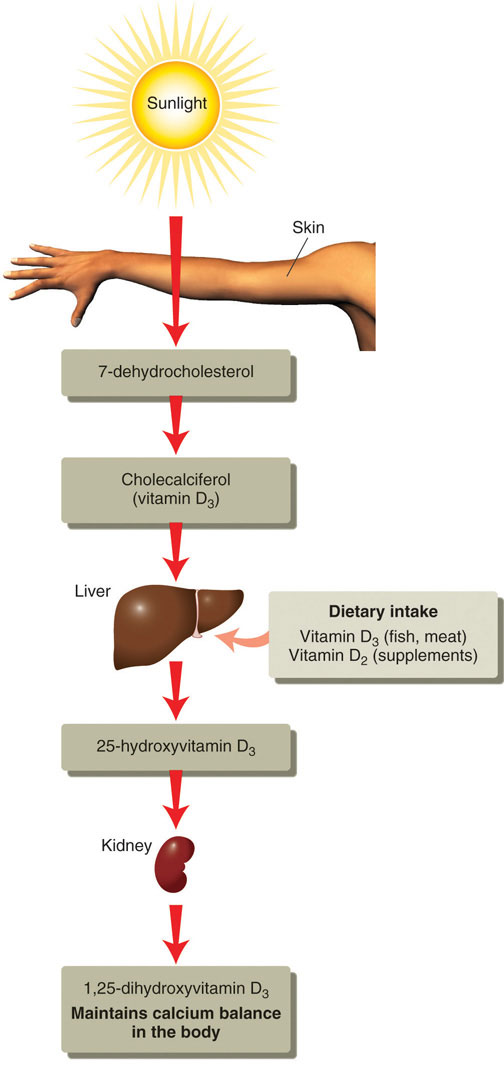
Vitamin D refers to a group of fat-soluble vitamins derived from cholesterol. Vitamins D2 and D3 are the only ones known to have biological actions in the human body. Although vitamin D3 is called a vitamin, the body can actually synthesize vitamin D3. When exposed to sunlight, a cholesterol precursor in the skin is transformed into vitamin D3 (Figure \(\PageIndex{2}\)). However, this is not the bioactive form of vitamin D. It first must be acted upon by enzymes in the liver and then transported to the kidney where vitamin D3 is finally transformed into the active hormone, calcitriol (1,25-dihydroxyvitamin D3).
The skin synthesizes vitamin D when exposed to sunlight. In fact, for most people, more than 90 percent of their vitamin D3 comes from the casual exposure to the UVB rays in sunlight. Anything that reduces your exposure to the sun’s UVB rays decreases the amount of vitamin D3 your skin synthesizes. That would include long winters, your home’s altitude, whether you are wearing sunscreen, and the color of your skin (including tanned skin). Twenty to thirty minutes of sun exposure 2-3 times per week is thought to provide adequate vitamin D synthesis.
A person’s vitamin D status is determined by measuring 25-hydroxyvitamin D3 levels in the blood because it reflects both the vitamin D obtained from production in the skin and that from dietary sources (see Figure \(\PageIndex{2}\)). Measuring the active hormone, calcitriol (1,25-dihydroxyvitamin D3), does not accurately reflect one’s vitamin D status because of its short half-life (six to twelve hours). The vast majority of nutrition experts consider a concentration of 25-hydroxyvitamin D3 in the blood less than 20 nanograms per milliliter as an indicator of vitamin D deficiency. The Institute of Medicine states that serum levels above 20 nanograms per milliliter are sufficient to maintain bone health in healthy individuals.4
Functions of Vitamin D
As previously discussed, activated vitamin D3 (calcitriol) regulates blood calcium levels in concert with parathyroid hormone (PTH). Vitamin D works with PTH to stimulate osteoclasts that break down bone when calcium is needed elsewhere in the body. Vitamin D is also required for calcium absorption; in the absence of an adequate intake of vitamin D, less than 15% of calcium is absorbed from foods or supplements.
Vitamin D Imbalances
We can't get too much vitamin D from sun exposure or from food intake. However, vitamin D toxicity can occur from vitamin supplements. Getting too much vitamin D results in hypercalcemia (high blood calcium); symptoms of hypercalcemia include weakness, loss of appetite, constipation, mental confusion. Hypercalcemia can also lead to calcium deposits in soft tissues such as the kidneys, liver, and heart.
A deficiency of vitamin D leads to loss of bone mass. In children, a vitamin D deficiency causes a bone disease called rickets. Rickets is characterized by soft, weak, deformed bones that are exceptionally susceptible to fracture. In adults, vitamin D deficiency causes a similar disease called osteomalacia, which is characterized by low bone density. Vitamin D deficiency is common, especially in the elderly population, dark-skinned populations, and in people who live in the northern latitudes where sunlight exposure is decreased during the long winter season. Vitamin D deficiency can also happen in people who have diseases that reduce intestinal absorption of fat; the decreased fat absorption leads to decreased absorption of fat-soluble vitamins (e.g. vitamin D).
Vitamin D Recommendations
The DRIs for vitamin D for different age groups are listed in Table \(\PageIndex{3}\). For adults, the RDA is 15 micrograms of vitamin D. The National Osteoporosis Foundation recommends slightly higher levels and that adults under age fifty get 400-800 international units (10-20 micrograms) of vitamin D every day, and adults fifty and older get 800-1,000 international units (20-25 micrograms) of vitamin D every day.5 Toxicity from excess vitamin D is rare, but certain diseases such as hyperparathyroidism, lymphoma, and tuberculosis make people more sensitive to the increases in calcium caused by high intakes of vitamin D.
| Age Group | RDA (mcg/day) | UL (mcg/day) |
|---|---|---|
| Infant (0–6 months) | 10* | 25 |
| Infants (7–12 months) | 10* | 38 |
| Children (1–3 years) | 15 | 63 |
| Children (4–8 years) | 15 | 75 |
| Children (9–13 years) | 15 | 100 |
| Adolescents (14–18 years) | 15 | 100 |
| Adults (19–70 years) | 15 | 100 |
| Adults (> 70 years) | 20 | 100 |
| * denotes Adequate Intake | ||
Sources of Vitamin D
There are few food sources of vitamin D. Oily fish, such as salmon, is one of the best. Many foods, including dairy products, orange juice, and cereals are now fortified with vitamin D. Many people are deficient in vitamin D as a result of the few dietary sources for this vitamin.
| Food | Vitamin D (mcg) | % Daily Value |
|---|---|---|
| Cod liver oil (1 tablespoon) | 34 | 170 |
| Rainbow trout (3 ounces) | 16.2 | 81 |
| Salmon (3 ounces) | 14.2 | 71 |
| Mushrooms (1/2 cup) | 9.2 | 46 |
| 2% milk, vitamin D fortified (1 cup) | 2.9 | 15 |
Learn even more about this nutrient by reading the Vitamin D Fact Sheet from the National Institutes of Health, Office of Dietary Supplements.
Key Takeaways
- Calcium is the most abundant mineral in the body and has four primary functions: making bones strong and healthy, facilitating nerve-to-nerve communication, stimulating muscle contraction, and activating blood-clotting factors.
- Blood levels of calcium are controlled by three hormones: parathyroid hormone (PTH), calcitriol, and calcitonin.
- Vitamin D is essential for maintaining calcium levels in the body. Once activated to calcitriol, it acts in concert with PTH to keep blood levels of calcium constant, especially by enhancing its intestinal absorption.
References
- Summary Report of the Dietary Reference Intakes. nationalacademies.org. www.nationalacademies.org/our-work/summary-report-of-the-dietary-reference-intakes. Accessed June 30, 2020.
- Calcium - Health Professional Fact Sheet. ods.od.nih.gov. https://ods.od.nih.gov/factsheets/Calcium-HealthProfessional/. Accessed June 30, 2020.
- Calcium Content. ods.od.nih.gov. https://ods.od.nih.gov/pubs/usdandb/Calcium-Content.pdf. Accessed June 30, 2020.
- Vitamin D - Health Professional Fact Sheet. ods.od.nih.gov.https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/. Accessed July 1, 2020.
- Calcium and Vitamin D. nof.org. https://www.nof.org/patients/treatment/calciumvitamin-d/. Accessed July 1, 2020.

