9.3: Other Essential Micronutrients for Bone Health
- Page ID
- 21156
Learning Objectives
- Identify additional nutrients that are vital in maintaining bone health and state their primary role.
- Identify food sources for each nutrient.
Bone tissue is greater than 70% inorganic material and as such, minerals are important for maintaining skeletal health. In addition to calcium, other minerals critical for bone health include phosphorus, magnesium, fluoride and vitamin K. But that is not all—iron, copper, zinc, and vitamin C are also essential for the synthesis of collagen. Consuming too much or too little vitamin A affects bone health too, as it plays a role in osteoclast and osteoblast activities. The fact that there are many bone-friendly nutrients provides us with one more reason why it is better to eat a diet rich in many nutrients than take one particular supplement. In Table \(\PageIndex{1}\), notice the important nutrients for bone health and good food sources for each.
| Micronutrient | Functional Role in Bone Health | Food Sources |
|---|---|---|
| Calcium |
|
collards, mustard greens, kale, turnips, broccoli, beans, black molasses, fortified juices, milk |
| Phosphorus |
|
soy, legumes, whole grains, dairy, nuts, seeds |
| Magnesium |
|
whole grains, legumes, almonds, cashews, hazelnuts, beets, collards, kelp |
| Fluoride |
|
fluoridated water (tap water), foods prepared in fluoridated water, seafood (because the ocean contains natural sodium fluoride) |
| Vitamin D |
|
salmon, rainbow trout, sardines, mushrooms, cod liver oil, egg yolks, fortified milk |
| Vitamin K |
|
kale, spinach, turnip, dark leafy vegetables |
| Boron |
|
avocado, nuts, peanut butter, green and orange vegetables, grapes, raisins |
| Iron |
|
red meat, egg yolks, dark leafy vegetables, dried fruit, iron-fortified foods, beans, lentils, chick peas, liver, artichoke |
| Vitamin C |
|
citrus fruits, tomatoes and tomato juice, potatoes, Brussels sprouts, cauliflower, broccoli, strawberries, cabbage, spinach |
| Zinc |
|
oysters, wheat germ, pumpkin seeds, squash, watermelon seeds, beans, sesame seeds, tahini, beef, lamb |
Phosphorus
Phosphorus is classified as a macromineral (major mineral). Macrominerals are those that the body requires in amounts of at least 100 mg per day.
Functions of Phosphorus
Phosphorus is the second most abundant mineral in the human body; 85% of it is housed in the skeleton. In addition to serving as a primary mineral in the skeleton, phosphorus in the form of phosphate is a component of RNA, DNA, adenosine triphosphate (ATP; the cell's energy storing molecule), and phospholipids. Because phosphorus is present with calcium in mineralized bone, it is somewhat regulated in parallel to calcium. PTH and calcitriol stimulate bone resorption, increasing not only blood levels of calcium, but also blood phosphate levels. However, in contrast to the effect of PTH on calcium reabsorption by the kidney, PTH stimulates the renal excretion of phosphate so that it does not accumulate to toxic levels. You may also remember that phosphorus is the primary negatively charged electrolyte in intracellular fluid and helps maintain fluid balance. In addition, phosphorus helps activate and deactivate enzymes in various metabolic processes throughout the body.
Phosphorus Imbalances
Excessive vitamin D supplements can cause high phosphorus levels, muscle spasms, and convulsions. Deficiencies of phosphorus are rare in healthy adults.
Phosphorus Recommendations
The Dietary Reference Intakes (DRIs) for phosphorus are listed in Table \(\PageIndex{2}\).
| Age Group | RDA (mg/day) | UL (mg/day) |
|---|---|---|
| Infants (0–6 months) | 100* | ND |
| Infants (7–12 months) | 275* | ND |
| Children (1–3 years) | 460 | 3,000 |
| Children (4–8 years) | 500 | 3,000 |
| Children (9–13 years) | 1,250 | 4,000 |
| Adolescents (14–18 years) | 1,250 | 4,000 |
| Adults (19–70 years) | 700 | 4,000 |
| Adults (> 70 years) | 700 | 3,000 |
| * denotes Adequate Intake; ND=not determined | ||
| Food | Phosphorus (mg) | % Daily Value |
|---|---|---|
| Yogurt, plain, low fat (6 ounces) | 245 | 20 |
| 2% milk (1 cup) | 226 | 18 |
| Salmon (3 ounces) | 214 | 17 |
| Chicken breast (3 ounces) | 182 | 15 |
| Lentils (1/2 cup) | 178 | 14 |
| Hamburger, 90% lean (3 ounces) | 172 | 14 |
Learn even more about this nutrient by reading the Phosphorus Fact Sheet from the National Institutes of Health, Office of Dietary Supplements.
Magnesium
Magnesium is classified as a macromineral (major mineral).
Functions of Magnesium
Approximately 60% of magnesium in the human body is stored in the skeleton, making up about 1% of mineralized bone tissue. Magnesium is not an integral part of the hydroxyapatite crystal, but it does reside on the surface of the crystal and helps maximize bone structure. Observational studies link magnesium deficiency with an increased risk for osteoporosis. A magnesium-deficient diet is associated with decreased levels of parathyroid hormone and the activation of vitamin D, which may lead to an impairment of bone remodeling.
In addition to participating in bone maintenance, magnesium has several other functions in the body. Every reaction that involves ATP requires magnesium. More than three hundred enzymatic reactions require magnesium. Magnesium plays a role in the synthesis of DNA and RNA, carbohydrates, and lipids, and is essential for nerve conduction and muscle contraction. Another health benefit of magnesium is that it may decrease blood pressure.
Magnesium Imbalances
Generally, people don't get magnesium toxicity from food. However, magnesium supplements can cause diarrhea, nausea, cramps, and dehydration. Hypermagnesemia can also occur in individuals with impaired kidney function.
Magnesium is found in a variety of foods. Therefore, if you eat an adequate and varied diet you will most likely consume required amounts. Hypomagnesemia can result in low blood calcium and osteoporosis. Hypomagnesemia can be caused by kidney disease, chronic diarrhea, or chronic alcohol intake.
Magnesium Recommendations
The DRIs for magnesium are listed in Table \(\PageIndex{4}\). It's important to note that the upper limit (UL) for magnesium applies only to magnesium supplements and is not a UL for magnesium intake from food and water.
| Age Group | RDA (mg/day) | UL (mg/day) |
|---|---|---|
| Infants (0–6 months) | 30* | ND |
| Infants (7–12 months) | 75* | ND |
| Children (1–3 years) | 80 | 65 |
| Children (4–8 years) | 130 | 110 |
| Children (9–13 years) | 240 | 350 |
| Adolescents (14–18 years) | 410 (males), 360 (females) | 350 |
| Adults (19–30 years) | 400 (males), 310 (females) | 350 |
| Adults (> 30 years) | 420 (males), 320 (females) | 350 |
| * denotes Adequate Intake | ||
Sources of Magnesium
Magnesium is part of the green pigment, chlorophyll, which is vital for photosynthesis in plants; therefore green leafy vegetables are a good dietary source for magnesium (Table \(\PageIndex{5}\)). Magnesium is also found in high concentrations in fish, dairy products, meats, whole grains, and nuts. Additionally chocolate, coffee, and hard water contain a good amount of magnesium. Most people in America do not fulfill the RDA for magnesium in their diets.
| Food | Magnesium (mg) | % Daily Value |
|---|---|---|
| Almonds (1 ounce) | 80 | 19 |
| Spinach, boiled (1/2 cup) | 78 | 19 |
| Soy milk (1 cup) | 61 | 15 |
| Black beans, cooked (1/2 cup) | 60 | 14 |
Learn even more about this nutrient by reading the Magnesium Fact Sheet from the National Institutes of Health, Office of Dietary Supplements.
Fluoride
Fluoride is classified as a trace mineral. Trace minerals are nutrients that we need to consume in amounts less than 100 mg per day.
Functions of Fluoride
Approximately 99% of the body's fluoride is stored in teeth and bones. So, it may not be surprising that it assists in tooth and bone development and maintenance. Fluoride is known mostly as the mineral that combats tooth decay. Fluoride combats tooth decay (cavities) via three mechanisms:
- Blocking acid formation by bacteria
- Preventing demineralization of teeth
- Enhancing remineralization of destroyed enamel
Fluoride Imbalances
Fluorosis (excess fluoride) creates porous tooth enamel; teeth become stained and pitted as shown in Figure \(\PageIndex{1}\). The highest risk for fluorosis is during the first 8 years of life when the permanent teeth are developing. Toothpastes that contain fluoride help reduce tooth decay. However, if fluoride toothpaste is swallowed by young children it can lead to fluorosis. This is why young children should be supervised while brushing their teeth and taught to spit out toothpaste instead of swallowing it.
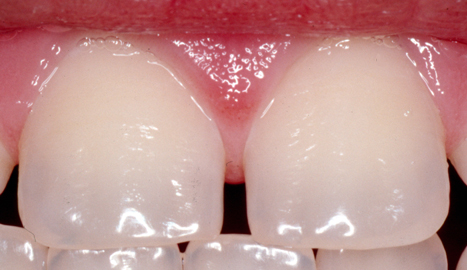
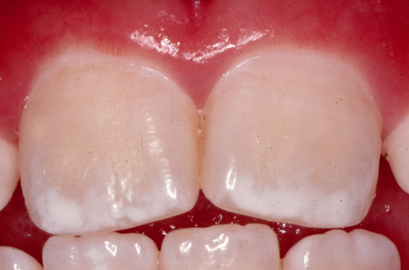
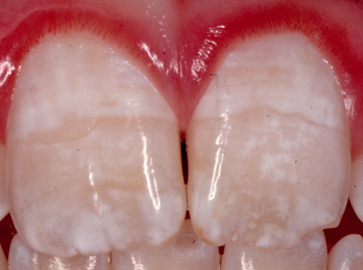
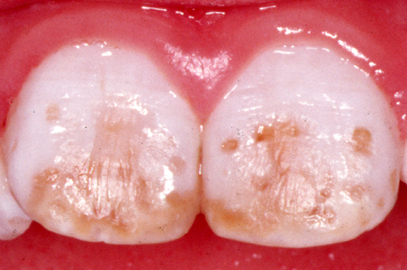
The largest risk associated with not consuming enough fluoride is development of tooth decay (cavities). The Centers for Disease Control and Prevention (CDC) has reported that fluoridation of water reduces tooth decay by about 25% in children and adults.4
Fluoride Recommendations
The Institute of Medicine has given Adequate Intakes (AIs) for fluoride, but has not yet developed RDAs (Table \(\PageIndex{6}\)). The AIs are based on the doses of fluoride shown to reduce the incidence of tooth decay, but not cause dental fluorosis.
| Age Group | AI (mg/day) | UL (mg/day) |
|---|---|---|
| Infants (0–6 months) | 0.01 | 0.7 |
| Infants (7–12 months) | 0.50 | 0.9 |
| Children (1–3 years) | 0.70 | 1.3 |
| Children (4–8 years) | 1.00 | 2.2 |
| Children (9–13 years) | 2.00 | 10.0 |
| Adolescents (14–18 years) | 3.00 | 10.0 |
| Adults (> 19 years) | 4.00 (males), 3.00 (females) | 10.0 |
Sources of Fluoride
More than 70% of a person’s fluoride intake comes from drinking fluoridated (tap) water when they live in a community that fluoridates the drinking water. Solid foods do not contain a large amount of fluoride. Fluoride content in foods depends on whether it was grown in soils and water that contained fluoride or cooked with fluoridated water. Canned meats and fish that contain bones do contain some fluoride. In addition, most toothpastes contain fluoride.
Vitamin K
Vitamin K refers to a group of fat-soluble vitamins that are similar in chemical structure.
Functions of Vitamin K
Vitamin K acts as a coenzyme and plays an essential role in blood coagulation. Without vitamin K, blood would not clot. Vitamin K is also required for maintaining bone health; it modifies the protein osteocalcin, which is involved in the bone remodeling process.
Vitamin K Imbalances
Based on current research, there are no known side effects when healthy individuals consume large amounts of vitamin K. Since vitamin K plays a role in blood coagulation, individuals taking blood thinners (e.g., coumadin, warfarin) should avoid large increases or decreases in their vitamin K intake.
Vitamin K deficiency is rare in healthy individuals but can lead to reduced blood clotting and excessive bleeding. People suffering with diseases that cause malabsorption of fat, such as celiac, Crohn's, and cystic fibrosis can suffer from a deficiency of vitamin K.
Vitamin K Recommendations
The Institute of Medicine has established Adequate Intakes (AIs) for vitamin K, but has not yet developed RDAs (Table \(\PageIndex{7}\)). A Tolerable Upper Intake Level (UL) for vitamin K has not been set.
| Age Group | AI (mcg/day) |
|---|---|
| Infants (0–6 months) | 2.0 |
| Infants (7–12 months) | 2.5 |
| Children (1–3 years) | 30 |
| Children (4–8 years) | 55 |
| Children (9–13 years) | 60 |
| Adolescents (14–18 years) | 75 |
| Adults (> 19 years) | 120 (males), 90 (females) |
Sources of Vitamin K
Vitamin K is present in many foods. It is found in highest concentrations in green vegetables such as broccoli, cabbage, kale, parsley, spinach, and lettuce (Table \(\PageIndex{8}\)).5 Additionally, vitamin K can be synthesized via bacteria in the large intestine. The exact amount of vitamin K synthesized by bacteria that is actually absorbed in the lower intestine is not known, but likely contributes less than 10% of the recommended intake. Newborns have low vitamin K stores and it takes time for the sterile newborn gut to acquire the good bacteria it needs to produce vitamin K. So, it has become a routine practice to inject newborns with a single intramuscular dose of vitamin K. This practice has basically eliminated vitamin K-dependent bleeding disorders in babies.
| Food | Vitamin K (mcg) | % Daily Value |
|---|---|---|
| Natto (3 ounces) | 850 | 708 |
| Collards, boiled (1/2 cup) | 530 | 442 |
| Spinach, raw (1 cup) | 145 | 121 |
| Broccoli, boiled (1/2 cup) | 110 | 92 |
| Soybean oil (1 tablespoon) | 25 | 21 |
| Pumpkin, canned (1/2 cup) | 20 | 17 |
Learn even more about this nutrient by reading the Vitamin K Fact Sheet from the National Institutes of Health, Office of Dietary Supplements.
Key Takeaways
- Phosphorous, a primary mineral component of bone, is regulated in parallel with calcium, and in high amounts is detrimental to bone health.
- Magnesium helps keep bones strong. A deficiency in magnesium can compromise bone health.
- Fluoride combats tooth decay and benefits teeth and bones when present in the diet at the recommended intake.
- Vitamin K is a coenzyme that participates in the modification of proteins that act in bone tissues and promotes normal blood clotting.
References
- Summary Report of the Dietary Reference Intakes. nationalacademies.org. www.nationalacademies.org/our-work/summary-report-of-the-dietary-reference-intakes. Accessed July 1, 2020.
- Phosphorus - Health Professional Fact Sheet. ods.od.nih.gov.https://ods.od.nih.gov/factsheets/Phosphorus-HealthProfessional/. Accessed July 1, 2020.
- Magnesium - Health Professional Fact Sheet. ods.od.nih.gov.https://ods.od.nih.gov/factsheets/Magnesium-HealthProfessional/. Accessed July 1, 2020.
- Community Water Fluoridation. cdc.gov. https://www.cdc.gov/fluoridation/index.html. Accessed July 1, 2020.
- Vitamin K - Health Professional Fact Sheet. ods.od.nih.gov.https://ods.od.nih.gov/factsheets/VitaminK-HealthProfessional/. Accessed July 1, 2020.

