14.2A: Preganglionic Neurons
- Page ID
- 7721
In the autonomic nervous system (ANS), nerve fibers that connect the central nervous system to ganglia are known as preganglionic fibers.
- Describe characteristics of preganglionic neurons of the autonomic nervous system
Key Points
- All preganglionic fibers of the ANS are cholinergic —meaning they have acetylcholine as their neurotransmitter, and are myelinated for faster transmission.
- Differences between sympathetic and parasympatheic preganglionic fibers include that sympathetic preganglionic fibers tend to be shorter than parasympathetic fibers and sympathetic fibers tend to form more synapses than parasympathetic fibers.
- The parasympathetic division (craniosacral outflow) consists of cell bodies from one of two locations: the brainstem (cranial nerves III, VII, IX, X) or the sacral spinal cord (S2, S3, S4).
- The sympathetic division (thoracolumbar outflow) consists of cell bodies in the lateral horn of the spinal cord (intermediolateral cell columns) from T1 to L2. These cell bodies are GVE (general visceral efferent ) neurons and are the preganglionic neurons.
Key Terms
- cholinergic: Pertaining to, activated by, producing, or having the same function as acetylcholine.
- postsynaptic neuron: The nerve cell that bears receptors for neurotransmitters released into the synaptic cleft by the presynaptic neuron.
- preganglionic fiber: In the autonomic nervous system, fibers from the CNS to the ganglion are known as preganglionic fibers.
- ganglion: A cluster of interconnecting nerve cells outside the brain.
- preganglionic neuron: The nerve fibers that supply a ganglion.
Preganglionic Neuron Properties
In the autonomic nervous system (ANS), fibers from the central nervous system to the ganglion are known as preganglionic fibers. All preganglionic fibers, whether they are in the sympathetic nervous system (SNS) or in the parasympathetic nervous system (PSNS), are cholinergic—that is, these fibers use acetylcholine as their neurotransmitter—and are myelinated.
The ANS is unique in that it requires a sequential two-neuron efferent pathway; the preganglionic neuron must first cross a synapse onto a postganglionic neuron before innervating the target organ. The preganglionic, or first neuron will begin at the outflow and will cross a synapse at the postganglionic, or second neuron’s cell body. The postganglionic neuron will then cross a synapse at the target organ.
Sympathetic preganglionic fibers tend to be shorter than parasympathetic preganglionic fibers because sympathetic ganglia are often closer to the spinal cord while parasympathetic preganglionic fibers tend to project to and synapse with the postganglionic fiber close to the target organ.
Outflow Sites
Properties of the SNS and PSNS preganglionic neurons also differ with respect to the spinal cord exit points. The sympathetic division has thoracolumbar outflow, meaning that the neurons begin at the thoracic and lumbar (T1–L2) portions of the spinal cord. The parasympathetic division has craniosacral outflow, meaning that the neurons begin at the cranial nerves (CN3, CN7, CN9, CN10) and sacral (S2–S4) spinal cord.
The sympathetic division (thoracolumbar outflow) consists of cell bodies in the lateral horn of the spinal cord (intermediolateral cell columns) from T1 to L2. These cell bodies are GVE (general visceral efferent) neurons and are the preganglionic neurons. There are several locations where preganglionic neurons create synapses with their postganglionic neurons:
- The paravertebral ganglia of the sympathetic chain (these run on either side of the vertebral bodies), cervical ganglia, thoracic ganglia, rostral lumbar ganglia, caudal lumbar ganglia, and pelvic ganglia.
- The prevertebral ganglia celiac ganglion, aorticorenal ganglion, superior mesenteric ganglion, inferior mesenteric ganglion.
- The chromaffin cells of the adrenal medulla. This is the one exception to the two-neuron pathway rule: they create a synapse directly onto the target cell bodies.
The parasympathetic division (craniosacral outflow) consists of cell bodies from one of two locations: the brainstem (cranial nerves III, VII, IX, X) or the sacral spinal cord (S2, S3, S4).
These are the preganglionic neurons that synapse with the postganglionic neurons in these locations:
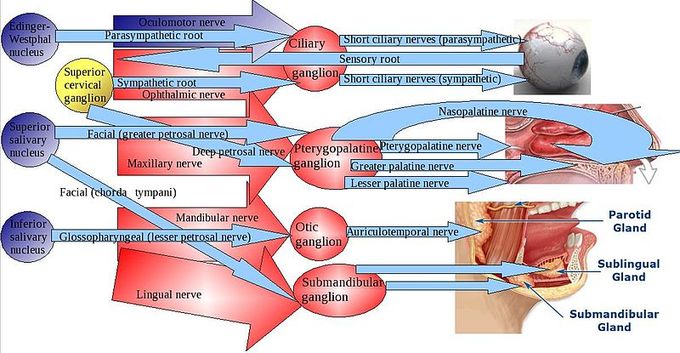
Parasympathetic ganglia of the head: The parasympathetic division has craniosacral outflow, meaning that the neurons begin at the cranial nerves (CN3, CN7, CN9, CN10) and the sacral (S2–S4) spinal cord. Pre- and post-ganglionic fibers and targets are depicted.
- Parasympathetic ganglia of the head (ciliary (CN III)).
- Submandibular (CN VII).
- Pterygopalatine (CN VII).
- Otic (CN IX)).
- In or near the wall of an organ innervated by the vagus (CN X) or sacral nerves (S2, S3, S4).
Divergence
Another major difference between the two ANS systems is divergence, or the number of postsynaptic fibers a single preganglionic fiber creates a synapse with. Whereas in the parasympathetic division there is a divergence factor of roughly 1:4, in the sympathetic division there can be a divergence of up to 1:20.
The site of synapse formation and this divergence for both the sympathetic and parasympathetic preganglionic neurons does, however, occur within ganglia situated within the peripheral nervous system.

