14.2C: Postganglionic Neurons
- Page ID
- 7723
In the autonomic nervous system, fibers from the ganglion to the effector organ are called postganglionic fibers.
- Describe sympathetic and parasympathetic postganglionic neurons
Key Points
- Postganglionic fibers in the sympathetic division are adrenergic and use norepinephrine (also called noradrenalin) as a neurotransmitter. By contrast, postganglionic fibers in the parasympathetic division are cholinergic and use acetylcholine as a neurotransmitter.
- In the sympathetic nervous system, the postganglionic neurons of sweat glands release acetylcholine for the activation of muscarinic receptors.
- Chromaffin cells of the adrenal medulla are analogous to post-ganglionic neurons; the adrenal medulla develops in tandem with the sympathetic nervous system and acts as a modified sympathetic ganglion.
- In the sympathetic nervous system, presynaptic nerves ‘ axons terminate in either the paravertebral ganglia or prevertebral ganglia. In all cases, the axon enters the paravertebral ganglion at the level of its originating spinal nerve.
Key Terms
- postganglionic fiber: In the autonomic nervous system, these are the fibers that run from the ganglion to the effector organ.
- cholinergic: Pertaining to, activated by, producing, or having the same function as acetylcholine.
- adrenergic: Containing or releasing adrenaline.
- postganglionic neuron: A nerve cell that is located distal or posterior to a ganglion.
In the autonomic nervous system, fibers from the ganglion to the effector organ are called postganglionic fibers. The post-ganglionic neurons are directly responsible for changes in the activity of the target organ via biochemical modulation and neurotransmitter release.
The neurotransmitters used by postganglionic fibers differ. In the parasympathetic division, they are cholinergic and use acetylcholine as their neurotransmitter. In the sympathetic division, most are adrenergic, meaning they use norepinephrine as their neurotransmitter.
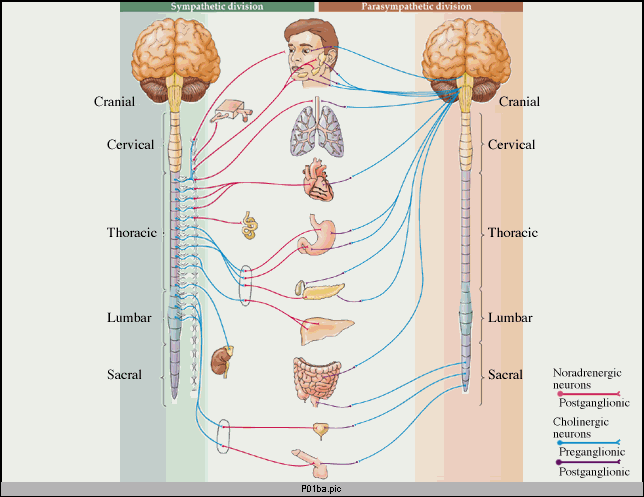
Postganglionic nerve fibers: In the autonomic nervous system, preganglionic fibers (shown in light blue) carry information from the CNS to the ganglion.
The Sympathetic Fibers
At the synapses within the ganglia, the preganglionic neurons release acetylcholine, a neurotransmitter that activates nicotinic acetylcholine receptors on postganglionic neurons. In response to this stimulus, postganglionic neurons—with two important exceptions—release norepinephrine, which activates adrenergic receptors on the peripheral target tissues. The activation of target tissue receptors causes the effects associated with the sympathetic system.
The two exceptions mentioned above are the postganglionic neurons of sweat glands and the chromaffin cells of the adrenal medulla. The postganglionic neurons of sweat glands release acetylcholine for the activation of muscarinic receptors. The chromaffin cells of the adrenal medulla are analogous to post-ganglionic neurons—the adrenal medulla develops in tandem with the sympathetic nervous system and acts as a modified sympathetic ganglion. Within this endocrine gland, the pre-ganglionic neurons create synapses with chromaffin cells and stimulate the chromaffin cells to release norepinephrine and epinephrine directly into the blood.
Presynaptic nerves’ axons terminate in either the paravertebral ganglia or prevertebral ganglia. In all cases, the axon enters the paravertebral ganglion at the level of its originating spinal nerve.
After this, it can then either create a synapse in this ganglion, ascend to a more superior ganglion, or descend to a more inferior paravertebral ganglion and make a synapse there, or it can descend to a prevertebral ganglion and create a synapse there with the postsynaptic cell. The postsynaptic cell then goes on to innervate the targeted end effector (i.e., gland, smooth muscle, etc.).
Because paravertebral and prevertebral ganglia are relatively close to the spinal cord, presynaptic neurons are generally much shorter than their postsynaptic counterparts, which must extend throughout the body to reach their destinations.
The Parasympathetic Fibers
The axons of presynaptic parasympathetic neurons are usually long. They extend from the CNS into a ganglion that is either very close to or embedded in their target organ. As a result, the postsynaptic parasympathetic nerve fibers are very short.
In the cranium, preganglionic fibers (cranial nerves III, VII, and IX) usually arise from specific nuclei in the central nervous system (CNS) and create a synapse at one of four parasympathetic ganglia: ciliary, pterygopalatine, otic, or submandibular.
From these four ganglia the postsynaptic fibers complete their journey to target tissues via cranial nerve V (the trigeminal ganglion with its ophthalmic, maxillary, and mandibular branches).
The vagus nerve does not participate in these cranial ganglia, as most of its fibers are destined for a broad array of ganglia on or near the thoracic viscera (esophagus, trachea, heart, lungs) and the abdominal viscera (stomach, pancreas, liver, kidneys). It travels all the way down to the midgut/hindgut junction, which occurs just before the splenic flexure of the transverse colon.
The pelvic splanchnic efferent preganglionic nerve cell bodies reside in the lateral gray horn of the spinal cord at the S2–S4 spinal levels. Their axons continue away from the CNS to synapse at an autonomic ganglion close to the organ of innervation. This differs from the sympathetic nervous system, where synapses between pre- and post-ganglionic efferent nerves in general occur at ganglia that are farther away from the target organ.
The parasympathetic nervous system uses acetylcholine (ACh) as its chief neurotransmitter, although peptides (such as cholecystokinin) may act on the PSNS as a neurotransmitter. The ACh acts on two types of receptors, the muscarinic and nicotinic cholinergic receptors.
Most transmissions occur in two stages: When stimulated, the preganglionic nerve releases ACh at the ganglion, which acts on the nicotinic receptors of the postganglionic neurons. The postganglionic nerve then releases ACh to stimulate the muscarinic receptors of the target organ.

