5.1: Pectoralis Major Flap
- Page ID
- 15454
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
THE PECTORALIS MAJOR FLAP
Johan Fagan
The pectoralis major flap comprises the pectoralis major muscle, with or without overlying skin, and may include the underlying ribs. It has an axial blood supply and is based superiorly on the pectoral branch of the thoracoacromial artery.
It is very useful in the head and neck, and can inter alia be used for the following: reconstruction of soft tissue defects of the oropharynx, oral cavity, hypopharynx, and skin of the neck; to augment pharyngeal repairs following salvage laryngectomy following previous chemoradiotherapy, and to cover carotid or jugular vein blowouts etc. Rib may be included to bridge mandibular defects.
Relevant Anatomy
Pectoralis major muscle (Figure 1)
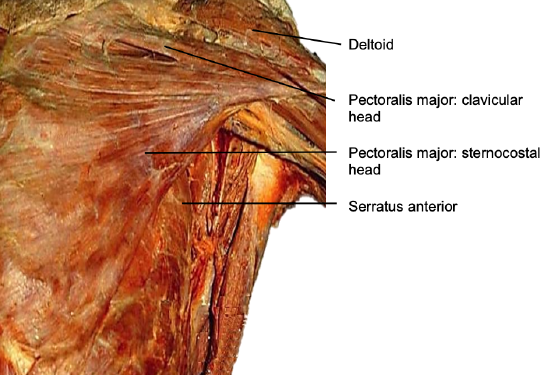
Figure 1: Superficial dissection
This muscle originates from the anterior aspect of the medial half of the clavicle; from the anterior surface of the sternum; from the cartilages of all the true ribs and from the aponeurosis of the abdominal external oblique muscle. The muscle fibers converge toward its insertion on the humerus. Muscle fibers arising from the clavicle pass transversely and are often separated from the rest of the muscle by a slight gap. The remainder of the muscle courses superolaterally.
Deep relations of pectoralis major muscle (Figure 2)
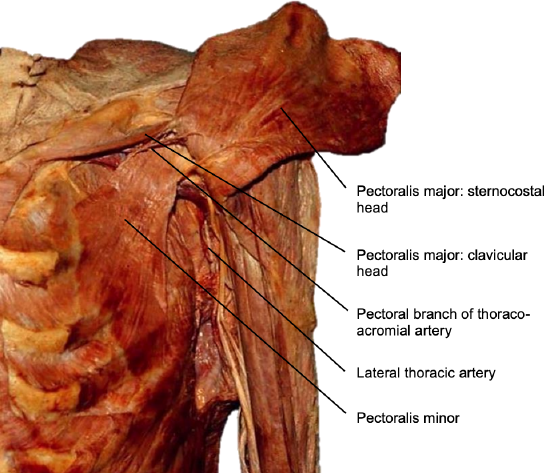
Figure 2: Deep relations of pectoralis major muscle
Deep to the pectoralis major muscle is its vascular pedicle, the pectoralis minor muscle, the costal cartilages, and inferiorly the costal attachments of the external oblique muscle.
Blood supply of pectoralis major flap (Figures 2, 3)
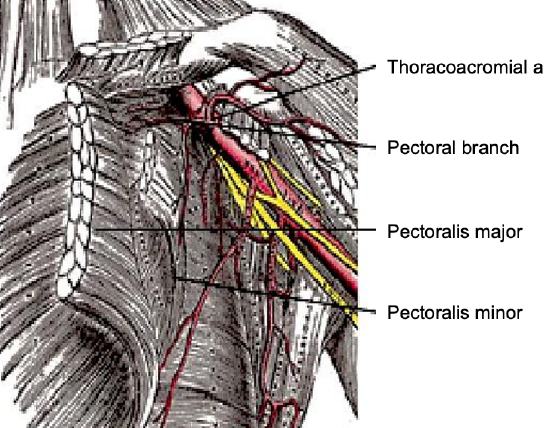
Figure 3: Blood supply of pectoralis major flap
The pectoralis major flap is an axial flap and is based primarily on the pectoral branch of the thoracoacromial artery and its accompanying veins. The thoracoacromial artery is a branch of the axillary artery, itself a continuation of the subclavian artery. The pectoral branch of the thoracoacromial artery courses within a well-defined fascial plane on the deep surface of the pectoralis major muscle (Figures 2, 9). There is a clear dissection plane between this fascial layer and the superficial aspect of the pectoralis minor muscle making it possible to strip the pectoralis major and its blood supply off the pectoralis minor with blunt finger dissection. Additional blood supply arises medially from the internal mammary artery, and laterally from the long thoracic artery, branches of which are generally sacrificed during elevation of the flap to secure adequate pedicle length. Care must be taken should the skin island be located distally in the region of the costal margin at, or beyond, the lower extent of the pectoralis major muscle, as the blood supply then becomes random as opposed to axial, making perfusion of the flap less reliable.
Innervation
The pectoralis major is innervated by the lateral pectoral nerve which can be located just inferior to the clavicle with the pectoral branch of the thoracoacromial artery. The medial pectoral nerve passes through the pectoralis minor muscle and sends 2 to 3 branches to the pectoralis major. All these nerves are normally divided during elevation of the flap. The denervated muscle loses bulk with time which might be advantageous or disadvantageous, depending on the functional and cosmetic objectives of the flap.
Flap design
The flap may be employed either as a muscular or musculocutaneous flap, with or without the 4th or 5th ribs. The following discussion will focus on raising a musculocutaneous island flap.
Positioning, prepping and draping
The patient is placed in a supine position with the chest exposed and prepped up to the midline, and inferiorly to the costal margin. The upper arm is abducted slightly to expose the anterior axillary fold and lateral chest wall.
Surface markings of vascular pedicle
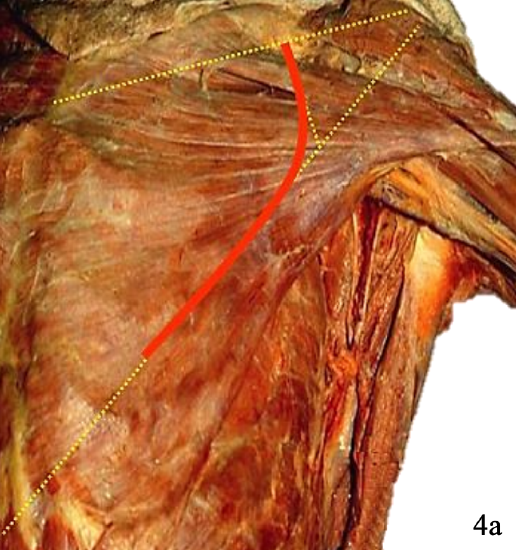
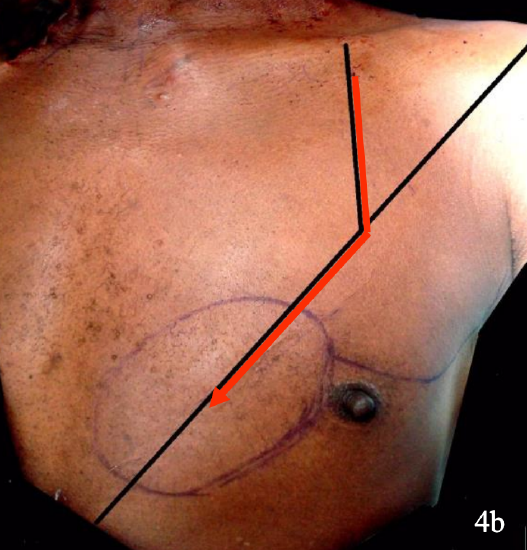
Figures 4a,b: Surface markings of pectoral branch of thoracoacromial artery
The surface markings of the vascular pedicle are determined by drawing a line from the shoulder to the xiphisternum and another line vertically from the midpoint of the clavicle to intersect the 1st line (Figures 4a, b).
Skin paddle design
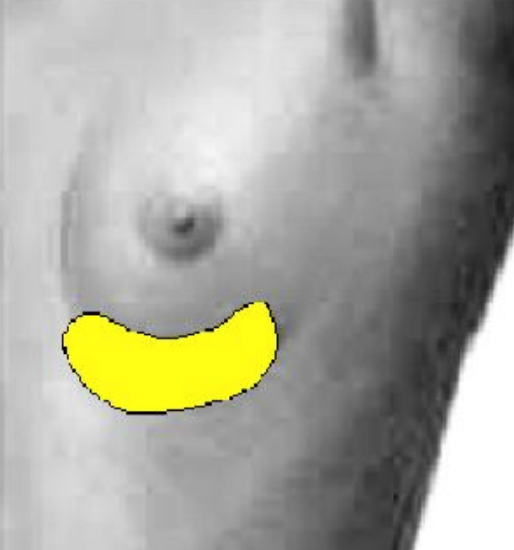
Figure 5: Inframammary skin paddle
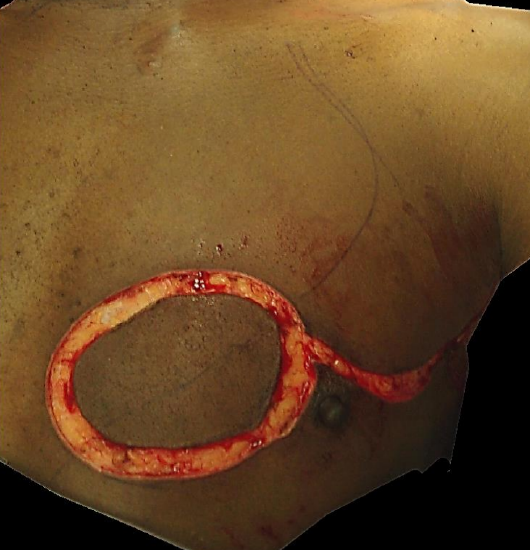
Figure 6: Dissection of skin paddle onto pectoralis major muscle, and incision along anterior axillary fold
The skin paddle is positioned over the pectoralis major muscle along the course of the pectoral branch of the thoracoacromial artery (Figures 4, 5, 6). In order to ensure that the pedicle is of adequate length, the distance between the top of the skin paddle and the inferior edge of the clavicle should equal or exceed the distance between the recipient site for the flap and the inferior edge of the clavicle. In women the paddle may be placed in the inframammary crease to include skin on either side of the crease, to avoid excessive bulk from breast tissue and for cosmetic reasons (Figure 5).
Should additional pedicle length be required, the flap may be extended up to 2.5 cm beyond the pectoralis major muscle inferiorly at the costal margin, with the knowledge that the flap then becomes a random pattern flap and the blood supply more tenuous.
Elevation of skin paddle
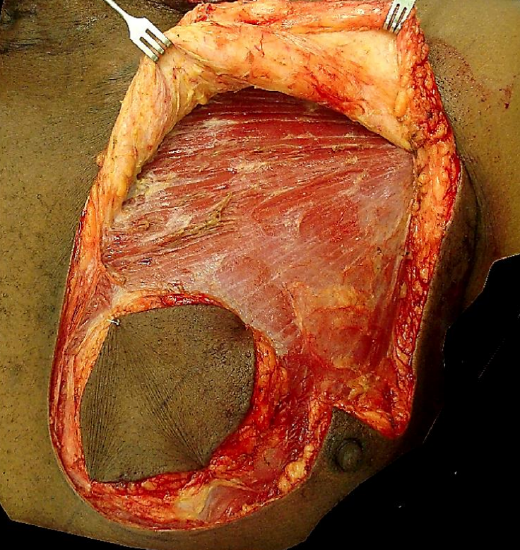
Figure 7: Exposure of pectoralis major muscle pedicle
The skin is incised around the skin paddle, and the dissection is extended onto the sursace of the pectoralis major muscle. As the vascular pedicle is located deep to the muscle, this may be quickly and safely performed using the bovie / monopolar diathermy. Care must be exercised not to undercut the skin paddle, but rather to bevel the dissection radially so as to include as many myocutaneous perforators as possible that supply the skin paddle (Figure 6). The skin paddle is tacked to the underlying pectoralis major muscle with a few sutures to minimize the risk of shearing injury to the myocutaneous perforators (Figure 7).
Exposure of pectoralis major muscle
An incision is extended laterally from the peripheral margin of the skin paddle along the anterior axillary fold, which corresponds with the lateral margin of the pectoralis major muscle (Figure 6). The skin and breast tissue above the skin paddle is then widely elevated from the pectoralis major muscle with diathermy up to the clavicle (Figure 7).
Elevation of pedicle
The pectoralis major muscle is incised with cautery medially and inferiorly to the skin paddle and is dissected from the ribs and intercostal muscles. The muscle is not divided superior to the skin paddle, as this might divide the vascular pedicle.
The pectoralis major muscle is then freed alongside the sternum with cautery. During this dissection perforators from the internal mammary artery are transected and cauterized.
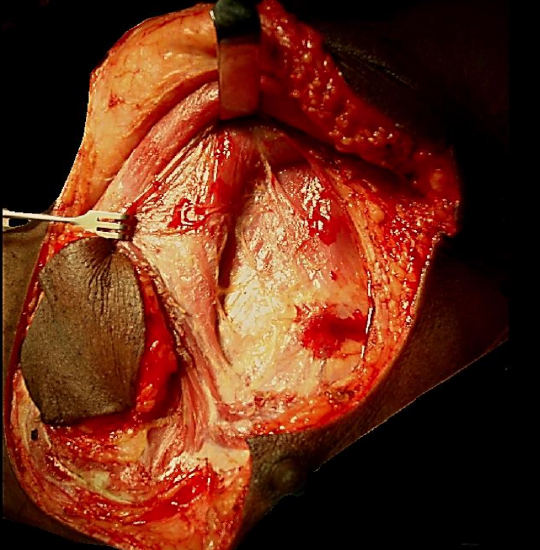
Figure 8: Elevating pectoralis major from pectoralis minor along lateral margin of muscle
The dissection plane between the pectoralis minor and major muscles and the vascular pedicle is found by dissecting along the lateral border of the pectoralis major muscle with electrocautery (Figure 8). Once this intermuscular plane has been identified, one can readily free the pectoralis major and its vascular pedicle from the pectoralis minor by stripping with a finger towards the clavicle (Figure 8).
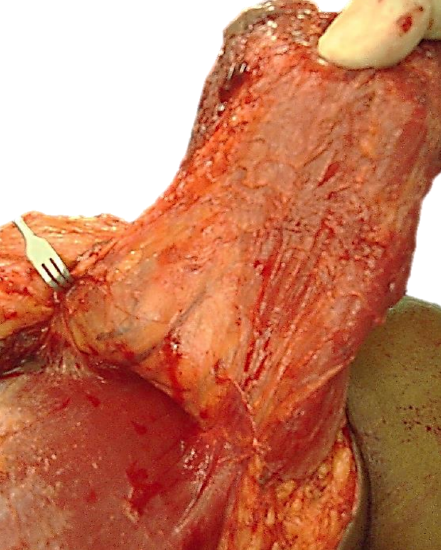
Figure 9: Vascular pedicle visible on deep aspect of pectoralis major muscle
This brings the vascular pedicle (pectoral branch of thoracoacromial artery) clearly into view within the fascia on the deep surface of the pectoralis major muscle (Figure 9). The pedicle is kept in view and protected from injury while the branches from the lateral thoracic artery, and the branches of the medial pectoral nerve that traverse the pectoralis minor and enter the deep surface of the flap, are divided. The pectoralis major muscle is divided lateral to the pedicle while keeping the pedicle in view, thereby freeing it from the humerus.
Skin tunnel over clavicle
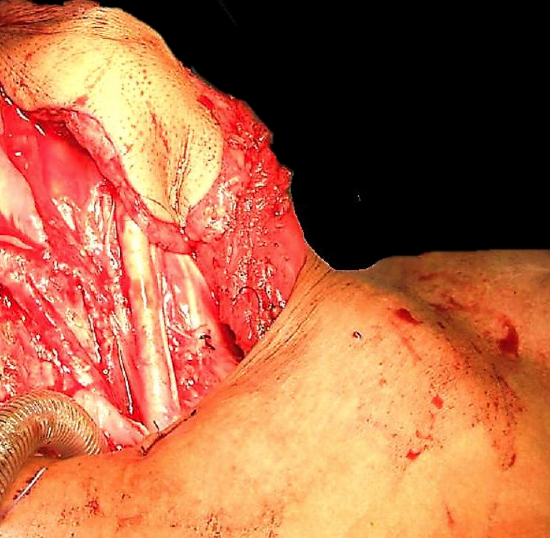
Figure 10: Flap is passed over the clavicle though a wide skin tunnel
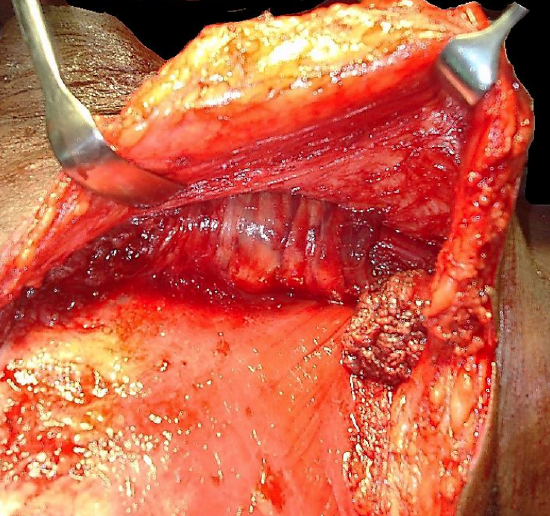
Figure 11: Check that pedicle is not twisted
The flap is generally passed into the neck superficial to the clavicle through a wide subcutaneous tunnel (Figure 10). The tunnel should be large enough to permit easy delivery of the flap into the neck without shearing the musculocutaneous perforators supplying the skin paddle, and to avoid strangulating the vascular pedicle. Dividing the subdermal connective tissue fibers of the skin above the skin tunnel with an upturned scalpel is a helpful adjunct to gain additional space.
After passing the flap into the neck, check that the pedicle is not twisted (Figure 11).
Gaining additional length
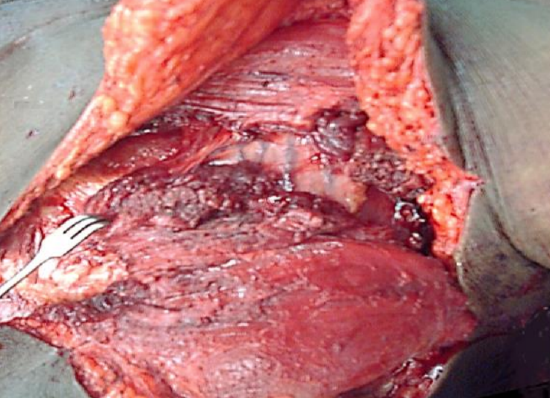
Figure 12: Vascular pedicle visible following division of muscular pedicle
If the pedicle is too short, two maneuvers may add additional length. The 1st is to transect the pectoralis major muscle just below the clavicle, taking great care to preserve the vascular pedicle (Figure 12). An infraclavicular segment of muscle may also be excised. This has the benefit that the pedicle is directly applied to the clavicle, without intervening muscle. It has the added bonus of avoiding an unsightly, bulky pedicle over the clavicle.
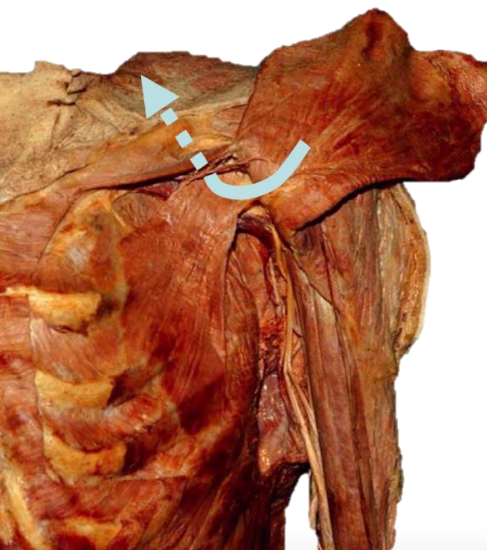
Figure 13: Gaining additional length by passing pedicle behind clavicle
A 2nd maneuver to gain additional length is to pass the flap behind the clavicle (Figure 13).
Should there be a concern about injury to the vascular structures deep to the clavicle, one can create a subperiosteal tunnel by incising the clavicular periosteum longitudinally along both the superior and inferior aspects of the clavicle. Since the periosteum is by its nature unyielding, this tunnel may be overly tight, but it can be relaxed by making incisions through the periosteum at its medial and distal ends, allowing easy passage of the flap. This maneuver adds some 3-4 cm to the reach of the flap which may be just enough in a tight situation.
Closure of donor site defect
The donor site is either closed primarily with a closed suction drain, or a split skin graft is applied. Primary closure may be facilitated by undermining the surrounding skin.
Some Clinical examples
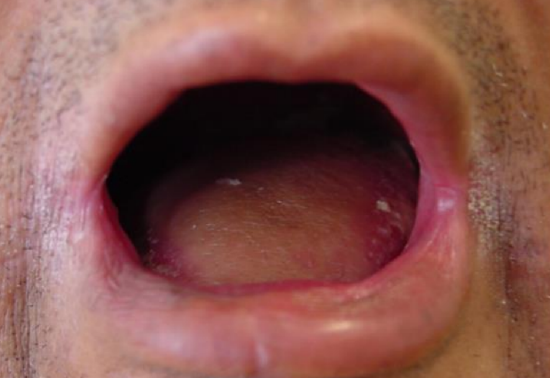
Figure 14: Reconstruction following total glossectomy
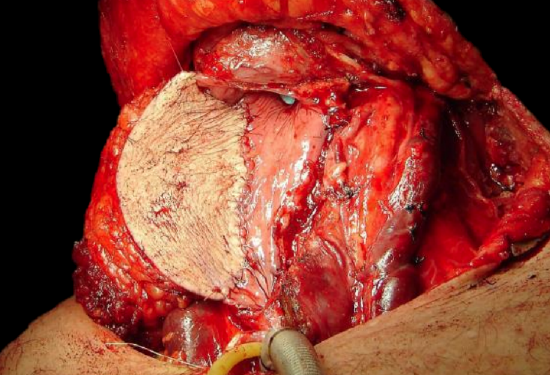
Figure 15: Augmentation of pharynx with pectoralis major myocutaneous flap following total laryngectomy with partial pharyngectomy
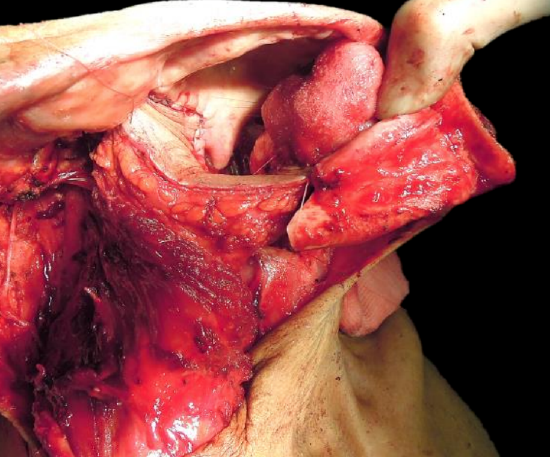
Figure 16: Reconstruction following segmental mandibulectomy and resection of tonsil, soft palate, and base of tongue
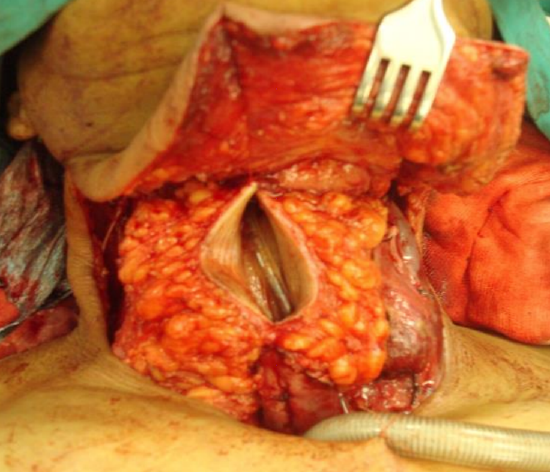
Figure 17: Laryngopharyngoesophagectomy defect reconstructed with tubed pectoralis major flap interposed between oropharynx and gastric pull-up that was too short to reach oropharynx
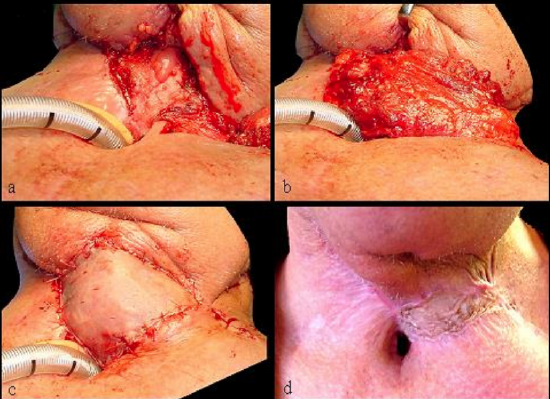
Figure 18: Reconstruction of (a) pharyngocutaneous fistula with (b) pectoralis major muscle flap and (c) split skin graft and (d) final result
Author & Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za
Other flaps described in The Open Access Atlas of Otolaryngology Head & Neck Operative Surgery
- Buccinator myomucosal flap
- Buccal fat pad flap
- Nasolabial flap
- Temporalis muscle flap
- Deltopectoral flap
- Paramedian forehead flap
- Upper and lower trapezius flaps
- Cervicofacial flaps
- Submental artery island flap
- Supraclavicular flap
- Latissimus dorsi flap
- Local flaps for facial reconstruction
- Radial free forearm flap
- Free fibula flap
- Rectus abdominis flap
- Anterolateral free thigh flap
- Thoracodorsal artery scapular tip (TDAST) flap
- Principles and technique of microvascular anastomosis for free tissue transfer flaps in head and neck reconstructive surgery


