3.8: Tonsillotomy (Partial) and Complete Tonsillectomy Surgical Technique
- Page ID
- 18269
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
TONSILLOTOMY (PARTIAL) & COMPLETE TONSILLECTOMY - SURGICAL TECHNIQUE
Klaus Stelter and Goetz Lehnerdt
Acute tonsillitis is treated with steroids e.g. dexamethasone, NSAIDs e.g. ibuprofen and beta-lactam antibiotics e.g. penicillin or cefuroxime. Only 10 days of antibiotic therapy has proven to be effective to prevent rheumatic fever and glomerulonephritis.
Tonsillectomy is only done for recurrent acute bacterial tonsillitis, or for noninfectious reasons such as suspected neoplasia.
Partial tonsillectomy (tonsillotomy) is the 1st line treatment for snoring due to tonsillar hyperplasia. It is low-risk, and postoperative pain and risk of hemorrhage are much less than with tonsillectomy. It is immaterial whether the tonsillotomy is done with laser, radiofrequency, shaver, coblation, bipolar scissors or monopolar electrocautery, as long as the crypts remain open and some tonsil tissue remains.
Pain and hemorrhage are the main morbidity of tonsillectomy. Bleeding may occur anytime until the wound is completely healed, which is normally at 2-3 weeks. Patients have to be informed about what to do in case of hemorrhage. Life threatening hemorrhage often is preceded by smaller bleeds, which can spontaneously cease. That is why every hemorrhage, even the smallest, has to be treated as an inpatient. Massive hemorrhage is an extreme challenge for every paramedic or emergency doctor because of difficult airway management.
Function and anatomical structure of tonsils in childhood and adolescence
Tonsils allow one to acquire immunity and provide immune defense by antigen presentation. This is why they contain T-lymphocytes, germinal centers of B-lymphocytes1 and macrophages. They are the first and easiest-to-reach station of the mucosa associated lymphoid tissue system (MALT)2-4. As the main phase of the immune acquisition continues until the age of 6 years, the palatine tonsils are physiologically hyperplastic at this time5, 6. This is followed by involution, which is reflected by regression of tonsil size until age 12 years7.
The lymphoid tissue is separated by a capsule from the surrounding muscle (superior pharyngeal constrictor)8. The blood supply originates from four different vessels, the lingual artery, the ascending pharyngeal artery and the ascending and descending palatine arteries. These vessels radiate mainly to the upper and lower tonsillar poles, as well as to the center of the tonsil from laterally9. The tonsils have deep crypts that create a large surface area to provide a docking surface for potential antigens10.

Figure 1: Hyperplastic tonsils in a child
Tonsil diseases
Sore throat episodes (R07.0)
Synonyms include “acute sore throat”, and “throat infection”. "Sore throat" is an imprecise term and does not clinically distinguish between acute tonsillitis and pharyngitis. Neither the cause nor the exact location is determined11. In “sore throat” it remains unclear whether one is dealing with acute (bacterial) tonsillitis which, if recurrent, is an indication for tonsillectomy12.
Acute tonsillitis (J03.0 - J03.9)
Also known as “severe tonsillitis” 13, “true tonsillitis”, or “acute sore throat” 11, this refers to viral or bacterial tonsillitis with odynophagia, swelling and redness of the tonsils, possibly with a tonsillar exudate, cervical lymphadenopathy and fever >38.3°C (rectal)14, 15. Odynophagia for 24-48 hours, as part of prodromal symptoms of a common cold (viral infection of upper respiratory tract), is excluded from the term "acute tonsillitis" 11. Depending on the stage and appearance of the tonsillar deposits or exudate, one can distinguish catarrhal angina with redness and swelling of the tonsils (early stage), from follicular angina with stipple-like fibrin deposits, from lacunar angina with confluent deposits (late stage)16, 17. "Acute tonsillitis" can be diagnosed by a specialist purely on clinical grounds18. Smears, blood tests or viral evidence are unnecessary in most cases19-23. Penicillin or another beta-lactam antibiotic is the first line of treatment.
Chronic tonsillitis (J35.0 and J35.9)
Also called “chronic (hyperplastic) tonsillitis”, it is not well-defined and thus should not be used24. It is better to speak of (chronic) recurrent tonsillitis 25, 26, because true chronic tonsillitis with persistentsymptoms lasting >4 weeks with adequate treatment and recovery of the mucosa (as in rhinosinusitis) does not exist.
Recurrent acute tonsillitis (J35.0)
Also called “recurrent tonsillitis” or “recurrent throat infections” 27, this refers to recurrent bouts of acute tonsillitis. In contrast to a single attack of acute tonsillitis, it is usually caused by many different bacterial pathogens28, 29 and flare up again a few weeks after cessation of antibiotic therapy30. Depending on the frequency and severity of such episodes, this is an indication for tonsillectomy.
Peritonsillar abscess (J36)
This is also called “peritonsillitis”, or “quinsy” 31, 32, and is acute tonsillitis complicated by an abscess, typically unilateral33. The abscess may form in the intratonsillar, para/ peritonsillar or retrotonsillar spaces. The pathogens are typically staphylococci34, streptococci and fusobacterium necrophorum35. In contrast to acute tonsillitis, viruses play no role in abscesses36. A peritonsillar abscess is drained by aspiration or drainage or by unilateral tonsillectomy.
Tonsil hyperplasia (J35.1 and J35.3)
Tonsil hyperplasia37, also known as (idiopathic) tonsillar hypertrophy38, refers to abnormal enlargement of the palatine tonsil. It has to be distinguished from physiological pediatric palatine tonsil hyperplasia39, 40 which is not a sign or consequence of recurrent inflammation41, 42. Also, children with tonsil hyperplasia do not suffer from acute tonsillitis43, 44 or middle ear infections45. A pediatric tonsil is only "pathologically" hyperplastic if snoring (with or without obstructive sleep apnoea) or rarely dysphagia46 or even more rarely dysphonia47 occur.
Surgical procedures
Tonsillectomy
(Extracapsular) tonsillectomy means that the entire tonsil, including its capsule, is removed from the tonsil fossa; no lymphatic tissue remains between the anterior and posterior palatal arches48. Since the late 1960s, with the realization that the tonsil is a focus of infection49-52, this form of tonsil operation has been the gold standard and is still the most common surgery done in the world53.
Tonsillotomy (partial tonsillectomy)
Only the medial part of the tonsil is removed. It requires that the (well-perfused) lymphatic tissue is resected, and that the remaining crypts remain open to the oropharynx54, 55. Active lymphatic tissue, with secondary follicles and crypts, is left in the tonsil fossae56. Tonsillotomy can be done with most dissecting and coagulating methods. The most common are laser tonsillotomy and radiofrequency tonsillotomy and are described in detail in this chapter.
Intracapsular tonsillectomy
Intracapsular, subcapsular or subtotal tonsillectomy describes a method in which the lymphatic tissue of the tonsil, including all crypts and follicles, is removed 57, 58, but the capsule of the tonsil is preserved; thus the underlying muscles are not exposed59. At the end of the operation there is an empty tonsil fossa without typical subsequent scarring59. Indications for intracapsular tonsillectomy are fetor ex ore (halitosis) and recurrent detritus (debris) in the tonsillar crypts. It differs from tonsillotomy in which a lot more tonsillar tissue is left behind.
Thermal- or cryotherapy of palatine tonsil
The tonsil tissue is heated (or cooled) interstitially; subsequent scarring causes shrinkage of the lymphoid tissue. No tissue is removed and a large part of the lymphoid tissue allegedly remains functional. The indication is mild tonsillar hyperplasia. Synonyms and different techniques include interstitial (electro)coagulation, laser coagulation, thermal coagulation, and cryocoagulation of the palatine tonsil60, 61, photodynamic therapy, ultrasound therapy62, radiofrequency-induced thermotherapy63, temperature-controlled tonsil treatment64, 65, and tonsil thermotherapy.
Preoperative evaluation, swabs & diagnosis
Pathogens, biofilms, and normal findings
With the discovery of rheumatic fever, group A streptococci (GAS) were primarily blamed for all ills in the upper respiretory tract in the 70’s 66-73. However more recently, anaerobes, e.g. Fusobacterium necrophorum, Streptococcus Intermedius and Prevotella Melaninogenica and Histicola have also been incriminated28, 74, 75.
Children up to 8 years of age have a tendency towards diffuse intracellular pathogen enrichment with interstitial abscesses, while in adults or adolescents a more superficial bacterial accumulation at the edge of the crypts occurs. Particularly in the case of recurrent tonsillitis, several pathogens and microorganisms play a joint role. These can jointly form biofilms and bacterial clusters and thus evade antibiotics76. The oral cavity and especially the furrowed tonsil is a reservoir for multiple pathogens (viruses and bacteria), parasites77 and fungi78. However, all these microbes belong to resident flora with which we have lived symbiotically for eons28, 79. Streptococci still play the largest role in acute tonsillitis (30%) 80, followed by Hemophilus Influenza and Neisseria28. Mostly, however, mixed infections (viral and bacterial initially) are responsible81.
Diagnosis
"Acute tonsillitis" in children and adults is a clinical diagnosis82. In viral tonsillitis, in addition to pain and fever, primarily cough, hoarseness, and rhinorrhoea occur, while in bacterial tonsillitis, in addition to pain with lymph node swelling, there is mainly a tonsillar exudate and fever >38.3°C 83. A streptococcal antigen test can confirm the diagnosis and is 98% specific for streptococci, although not particularly sensitive. A problem with these tests is the high number of asymptomatic chronic carriers of staphylococci and streptococci (10% of healthy children), who are definitely not in need of therapy84-89. In the early stages, a distinction between viral and bacterial tonsillitis is often difficult to make, especially when one considers that in 97.5% of cases, at least one virus, even in bacterial tonsillitis, is found (adenovirus and parainfluenza virus respectively in 47.5% 90, 91) 81.
Conservative Treatment
Antibiotic therapy: In clinically apparent or proven bacterial tonsillitis associated with distress, antibiotics (beta-lactam) are justified. Beta-lactam antibiotic therapy also provides relatively reliable protection against the dreaded rheumatic fever and glomerulonephritis which often cause, especially in developing countries, arthritis, myocarditis and death. Studies have shown that antibiotic therapy can prevent sequelae such as peritonsillar abscesses, acute otitis and sinusitis. The penicillins, particularly in children and adolescents, have the greatest benefit at the lowest cost. There is no difference to cephalosporins. Macrolides and clindamycin have more side-effects with the same efficacy and should be reserved for patients with proven penicillin allergy92, 93.
Postoperative antibiotic therapy is not indicated as it neither reduces pain nor postoperative bleeding94, 95.
Steroids: In acute tonsillitis or after tonsillectomy, oral or intramuscular steroids (dexamethasone 10 mg), as well as betamethasone (8 mg) and prednisolone (60 mg), significantly improve symptoms with minimal side effects and no adverse effects relating to disease progression96-98.
Analgesics: Nonsteroidal anti-inflammatory drugs have been used successfully for pain relief for >40yrs 99. For acute tonsillitis, ibuprofen has the best efficacy with minimal side-effects compared to paracetamol and acetylsalicylic acid (ASA)100. Another advantage of ibuprofen is its longer duration of action (6-8 hrs) compared to paracetamol. Both substances have a large therapeutic range and at the correct dosage, the safety is comparable101, 102. Diclofenac and ketorolac are very effective, but in children have fewer docking sites and are metabolized more quickly, which is why the dose should be adjusted to a higher level than in adults)103. In postoperative management these substances play a role in opioid reduction, but as first-line therapy in pediatrics are not suitable for a sore throat104, 105. Metamizol is not recommended as first or second choice analgesic in children due to a small but real risk of agranulocytosis106.
Complications of tonsillitis
In general, acute tonsillitis runs its course without complications and heals within 3-4 days. Rare but serious complications after streptococcal tonsillitis are glomerulonephritis and rheumatic fever, which triggers cardiomyopathies and rheumatic-like joint pain107. Early and a long course (10 days) of antibiotics (penicillin or cephalosporin) reduces the frequency of both these complications by 70% 108. In parts of the developing world where rheumatic fever is more common, preventing this complication is the main argument in favor of penicillin therapy108.
Peritonsillar abscess is a second, more frequent complication. It is typically unilateral, although bilateral abscesses occur in up to 4% 109. It is preceded by acute tonsillitis in only 1/3 of cases110. Even correctly administered antibiotic treatment of acute tonsillitis cannot really prevent peritonsillar abscesses (in contrast to rheumatic fever) 111. Since peritonsillar abscesses can rapidly spread to the soft tissues of the neck and are potentially life-threatening, the primary therapy is urgent and surgical 112-114. It does not matter whether the abscess is needle aspirated, incised or treated by tonsillectomy115. But the surgeon has to keep in mind that a stab incision can fail to drain inferiorly located abscesses109, 116. Before the operation, high-dose steroid therapy, as well as penicillin should be administered, as is often done for mixed infections117.
Indications for tonsil surgery
Surgery is done for infections, to relieve airway obstruction, for halitosis and for diagnosis when a tumor is suspected. Surgery for recurrent tonsillitis depends on its frequency and severity, and the presence of additional diseases (antibiotic allergies, immunosuppression and PFAPA syndrome).
Paradise criteria for tonsillectomy 118
Paradise (1984) reported that tonsillectomy significantly lowers the frequency of severe recurrent sore throats in children aged 3-15 years. Most published guidelines incorporate the so-called Paradise criteria for tonsillectomy:
- 7 episodes of tonsillitis per year in one year or,
- 5 episodes of tonsillitis per year in 2 consecutive years or,
- 3 episodes of tonsillitis per year in 3 consecutive years
A diagnosis of "purulent tonsillitis" must however be documented and confirmed by an elevated temperature (>38.3°C), tonsillar exudate, enlarged lymph nodes at the angle of the jaw, and antibiotic treatment119, 120. The authors also reported that on average only a few (not all) throat infections can be prevented by tonsillectomy in the following 2 years; 47 of 187 patients withdrew from the planned three-year follow-up121. For less severe sore throat inflammation or less frequent throat inflammation, the risk of tonsillectomy does not outweigh the benefits122.
While tonsils contribute to immune competence until 12 years, a negative long-term effect on the immune system cannot be proven123. Nevertheless, in children under 8 years, the indications for complete removal must be strictly adhered to, as the risks of serious or fatal bleeding are higher124.
With tonsillotomy (unlike tonsillectomy), some active lymphatic tissue is retained; it continues to grow in about 15% of cases, but rarely causes problems such as renewed snoring or recurrent tonsillitis125. The fear that frequent tonsillitis or peritonsillar abscesses will occur after tonsillotomy is unfounded126-128. All crypts remain open during laser, ultrasound, shaver, high- and radiofrequency technique129, 130.
Surgical technique
Extracapsular tonsillectomy
Cold steel dissection is the most commonly performed surgical technique in children and adults, and is described in detail in the chapter on Pediatric Tonsillectomy. The technique is similar in adults.
The tonsils are dissected from the tonsil bed partly sharply and partly bluntly with a raspartorium and scissors. The feeding vessels, especially at the upper and lower tonsil pole, are pinched off and then selectively ligated. After removal of the tonsil, a dry swab is pressed for about 1 minute into the tonsil bed to stop bleeding from small vessels. Some surgeons perform additional suturing of the lower pole (so-called “pole suturing”, a controversial method 131).
This method of tonsillectomy has been known for decades and has been very commonly used, especially in the 70s and 80s with the discovery of that tonsils are a source of infection132. Optical magnification (microscope or loupes), makes it possible to specifically identify the smaller vessels and perform bipolar coagulation before dissection133.
Due to its good long-term results and low morbidity and mortality, cold steel dissection is still the most common method of tonsillectomy134.
Tonsillotomy (partial tonsillectomy)
The tonsil is not completely removed, but only the portion that bulges into the throat, which due to its size causes functional problems. By preserving some tonsil tissue a lymphatic and immunologically active rudiment is retained.
The tonsil has a rich blood supply and has to be sufficiently cut and coagulated (not crushed) during surgery so that there is no postoperative bleeding, infection or pain. To this end, several dissection procedures have been developed (in principle, a tonsillectomy can also be performed with all these methods):
- CO² laser 135 136
- Monopolar high frequency current 137
- Ultrasound scalpel 138
- Bipolar radiofrequency coblation 139
- Bipolar scissors 140
- Argon gas-assisted monopolar needle 141
- Microdebrider 142
Advantages of tonsillotomy (regardless of what method is used to reduce the tonsils) are significantly less pain143 and a lower postoperative bleeding rate 144 compared with tonsillectomy.
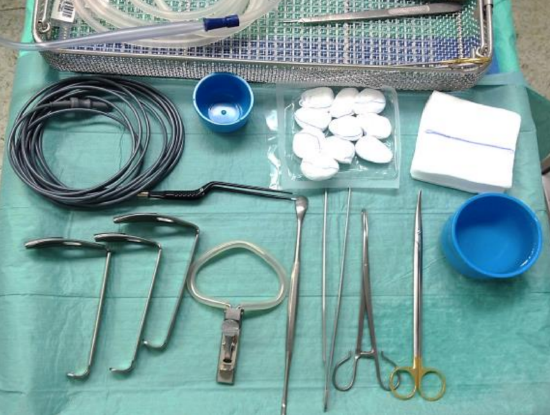
Figure 2: Instruments to perform radiofrequency dissected tonsillotomy / partial tonsillectomy
The quickest and easiest way to perform tonsillotomy is with monopolar high frequency dissection (Video 3). Instrumentation is shown in Figure 2.
- Following induction of general anesthesia the patient is positioned supine with neck slightly extended
- Select an appropriate length Boyle Davis blade and insert the gag to retract the tongue and expose the tonsils (Figure 1)
- Grasp a tonsil with a broad tonsil holding forceps and gently pull it toward the midline. Avoid pulling too hard to avoid doing a complete tonsillectomy
- Insert a Colorado needle into the tonsil at the edge of the anterior faucal pillar
- Spare the mucosa of the velopalatinal arch to avoid bleeding and pain in the incision line
- Amputate the protruding part of the tonsil by dissecting with continuous movements of the needle. Do not remain too long in the same place with the cutting needle as it may burn holes in the tonsil
- Pack the wound with a gauze swab for at least 1 minute
- Minor bleeding stops spontaneously. Larger bleeding vessels can be coagulated with bipolar forceps. A suture or ligature is not required
- Repeat the process on the contralateral side
Intracapsular (subtotal) tonsillectomy
The tonsil capsule covering the underlying muscle remains in the tonsil fossa 145. Slightly less postoperative pain and earlier food intake have been reported 146. The instrumentation and technique is similar to tonsillotomy. All the methods of tonsillotomy previously listed may also be used. The microdebrider has been reported to be a useful tool 147-152.
- The surgeon has to pull harder on the tonsil to subluxate the capsule, but the capsule itself has to remain in place and not be breached
- It may be very difficult to determine the exact proportion of residual tonsil that remains in the fossa
- After tonsillitis with subsequent scarring it is difficult even with loupes or a microscope to identify the exact plane of the tonsil capsule and only to remove only the active lymphatic tissue
- Because the vessels are bigger in the abyss of the crypts and near the capsule, bleeding has to be controlled with bipolar forceps more often than with (more superficial) tonsillotomy
Postoperative pain
Tonsillectomy is very painful, especially if the capsule is breached and the muscle is exposed. Severe pain and superinfection of the wound bed can cause delayed healing and prolong hospital stay. Especially adolescent and adult patients report pain, exhaustion and fatigue weeks after surgery. In tonsillectomy the wound remains open and heals in 2-3 weeks secondarily by granulation. Sealing the wound beds postoperatively e.g. with fibrin glue153 or sucralfate154 has no advantage in terms of postoperative bleeding or pain.
With tonsillotomy, however, pain was reported as only around 2-3 on the numerical analog scale.
Intracapsular tonsillectomy is allegedly less painful than tonsillectomy 155. However, it is unlikely that intracapsular tonsillectomy produces as little pain as tonsillotomy. Pain is perceived very differently by individuals. In children and adults, the differences, regardless of surgeon and method, can be enormous 156-158. Children of African descent have more postoperative pain than Europeans and respond better to opiates 159. This complicates both objective pain measurement (which does not exist), as well as a standard therapy. Pain therapy must therefore be individualized and adjusted, especially in children. Questionnaires (e.g. Ramsay Sedation Scale 160) for analgesic use, food intake, otalgia, and downtime use popular surrogate parameters.
Because pain is perceived and processed multimodally, the treatment must be multimodal. Firstly, a local long-lasting pain reliever (e.g. Bupivacaine or Ropivacaine 161) should be injected into the wound postoperatively or perioperatively to pre-vent activation of the early pain pathway 162-164 . Then already perioperatively it should be cooled locally by a cold compress165 and later a lot of ice should be eaten (local cooling and calorie intake) 166. Mouth-washes with gingicaine, benzocaine or tetracaine also provide pain relief, but also numb the taste buds and respiratory flow receptors, which is often perceived as very unpleasant.
The perioperative and postoperative administration of high-dose steroids (dexamethasone or prednisolone) is clearly recommended in all guidelines. This reduces postoperative nausea and analgesic consumption significantly 167-169.
A fixed analgesic regimen with ibuprofen or diclofenac makes sense in adults and adolescents, but for children and infants rescue medication is often enough 170, 171. An increased risk of bleeding due to nonsteroidal anti-inflammatory drugs, (except for aspirin) should not be feared 172, 173. One should therefore adhere to the WHO staging system174 (http://www.who.int/cancer/palliative/painladder/en/). After tonsillectomy, it may well be that in the first days WHO stage III drugs (strong opioid, e.g. piritramide iv) or even a pain pump must be administered to ensure pain under 4 on the visual analog scale and adequate food intake 175. Pain and nausea (with and without vomiting) after tonsillectomy are often trivialized by both nurses as well as physicians and therefore it is more likely that few analgesics will be administered postoperatively 176-178.
Post-tonsillectomy bleeding
Early and late postoperative bleeding
Postoperative bleeding can occur anytime until the wound is completely healed, despite careful intraoperative hemostasis and dissection; usually after 2-3 weeks.
Postoperative bleeding occurs either as so-called early bleeding within the first 24 hours, or in the form of late bleeding with a peak incidence between the 5th and 8th day after surgery. From the 3rd postoperative week bleeding occurs only very rarely. Therefore late postoperative bleeding presents a special problem because it often occurs only at home and therefore the time factor to get a professional play a major role.

Figure 3: Rigid tonsil or thoracic suction device manufactured by Cardinal Health, IL, USA (Medi-Vac ® Yankauer Suction Handle, REF KEX80)
The most common cause of late bleeding is the physiological detachment of the fibrin layer from the open wound bed and usually results in harmless bleeding. This bleeding almost always ends spontaneously, or due to local icing (sucking ice cubes, applying an ice cravat) or by tranexamic acid intravenously or locally (rinsing) 179. If bleeding does not spontaneously subside because a larger vessel is bleeding, vessel ligation or suturing under anesthesia is required. Massive hemorrhage is an extreme challenge for every paramedic or emergency doctor because of the difficult airway management. Intubation is only possible with suctioning the airway with suction tubes (Figure 3).
During induction and intubation, the ENT doctor should be present and prepared to perform emergency Cricothyroidotomy. Aspirated blood or incorrect intubation is the most common clinical complication of postoperative bleeding. Intraoperatively the surgeon must decide whether targeted bipolar coagulation and swab pressure are sufficient or whether suturing or ligation are necessary. If that fails, either the lingual artery, ascending pharyngeal artery, facial artery or even the external carotid artery must be ligated from externally or embolization the feeding vessels by interventional radiology should be done. Such massive bleeding is signaled in most cases by a minor "warning bleeding" 180, 181, so any bleeding must be taken seriously and the patient must be hospitalized.
Postoperative bleeding depending on method of surgery
In principle, intraoperative and postoperative bleeding can occur with all interventions involving the tonsils. However, for the tonsillotomy the postoperative bleeding rate is, by a factor of 5-10, lower than that for tonsillectomy 182. In cryptolysis and thermotherapy of the tonsils postoperative bleeding is a rarity 183, 184. Only extracapsular tonsillectomy remains problematic. "Cold dissection" with ligature or suturing has the lowest postoperative bleeding rates. Significantly more severe late bleeding has been reported after laser, coblation, monopolar or bipolar techniques 185-187.
References
- Westermann J. Organe des Abwehrsystems. Springer; 2010. 361-2
- Brandtzaeg P. The B-cell development in tonsillar lymphoid follicles. Acta Otolaryngol Suppl. 1996;523:55-9
- Nave H, Gebert A, Pabst R. Morphology and immunology of the human palatine tonsil. Anat Embryol (Berl). 2001 Nov;204(5):367-73
- Brandtzaeg P. Immune functions of nasopharyngeal lymphoid tissue. Adv Otorhinolaryngol. 2011;72:20-4
- Perry M, Whyte A. Immunology of the tonsils. Immunol Today. 1998 Sep;19(9):414-21
- Kaygusuz I, Godekmerdan A, Karlidag T, et al. Early stage impacts of tonsillectomy on immune functions of children. Int J Pediatr Otorhinolaryngol. 2003 Dec;67(12):1311-5
- Kaygusuz I, Alpay HC, Godekmerdan A, et al. Evaluation of long-term impacts of tonsillectomy on immune functions of children: a follow-up study. Int J Pediatr Otorhinolaryngol. 2009 Mar;73(3):445-9
- Perry ME, Slipka J. Formation of the tonsillar corpuscle. Funct Dev Morphol. 1993;3(3):165-8
- Westermann J. Organe des Abwehrsystems. Springer; 2010. 361-362.
- Drucker M, Drucker I, Neter E, Bernstein J, Ogra PL. Cell mediated immune responses to bacterial antigens on human mucosal surfaces. Adv Exp Med Biol. 1978;107:479-88
- Georgalas CC, Tolley NS, Narula A. Tonsillitis. Clin Evid (Online). 2009
- Paradise JL. Etiology and management of pharyngitis and pharyngotonsillitis in children: a current review. Ann Otol Rhinol Laryngol Suppl. 1992 Jan;155:51-7
- Lange G. [Angina and chronic tonsillitis--indications for tonsillectomy]. Z Allgemeinmed. 1973 Mar 20;49(8):366-70
- Österreichische Gesellschaften für HalsNasen-Ohren-Heilkunde KuH, Kinderund Jugendheilkunde. Gemeinsame Empfehlung zur Entfernung der Gaumenmandeln (Tonsillektomie). Monatsschr Kinderheilkd. 2008 Mar 7;3(156):268-71
- Stuck BA, Gotte K, Windfuhr JP, Genzwurker H, Schroten H, Tenenbaum T. Tonsillectomy in children. Dtsch Arztebl Int. 2008 Dec;105(49):852-60
- Berghaus A. [Chronic inflammation of the upper airways. Operation instead of antibiotic]. MMW Fortschr Med. 2005 Sep 29;147(39):27
- Berghaus A, Pirsig W. Mundhöhle und Pharynx. In: Berghaus A, Rettinger G, Böhme G., eds. Hals-Nasen-Ohren-Heilkunde. 1 ed. Stuttgart: Hippokrates Verlag; 1996. 386-453
- Stuck BA, Gotte K, Windfuhr JP, Genzwurker H, Schroten H, Tenenbaum T. Tonsillectomy in children. Dtsch Arztebl Int. 2008 Dec;105(49):852-60
- Stuck BA, Genzwurker HV. [Tonsillectomy in children: preoperative evaluation of risk factors]. Anaesthesist. 2008 May;57(5):499-504
- Stuck BA, Gotte K, Windfuhr JP, Genzwurker H, Schroten H, Tenenbaum T. Tonsillectomy in children. Dtsch Arztebl Int. 2008 Dec;105(49):852-60
- Kurien M, Stanis A, Job A, Brahmadathan, Thomas K. Throat swab in the chronic tonsillitis: how reliable and valid is it? Singapore Med J. 2000 Jul;41(7):324-6
- Fujikawa S, Hanawa Y, Ito H, Ohkuni M, Todome Y, Ohkuni H. Streptococcal antibody: as an indicator of tonsillectomy. Acta Otolaryngol Suppl. 1988;454:286-91
- Borschmann ME, Berkowitz RG. Oneoff streptococcal serologic testing in young children with recurrent tonsillitis. Ann Otol Rhinol Laryngol. 2006 May;115(5):357-60
- Stuck BA, Gotte K, Windfuhr JP, Genzwurker H, Schroten H, Tenenbaum T. Tonsillectomy in children. Dtsch Arztebl Int. 2008 Dec;105(49):852-60
- Stuck BA, Gotte K, Windfuhr JP, Genzwurker H, Schroten H, Tenenbaum T. Tonsillectomy in children. Dtsch Arztebl Int. 2008 Dec;105(49):852-60
- Burton MJ, Towler B, Glasziou P. Tonsillectomy versus non-surgical treatment for chronic / recurrent acute tonsillitis. Cochrane Database Syst Rev. 2000;(2):CD001802
- Georgalas CC, Tolley NS, Narula A. Recurrent throat infections (tonsillitis). Clin Evid (Online). 2007
- Jensen A, Fago-Olsen H, Sorensen CH, Kilian M. Molecular mapping to species level of the tonsillar crypt microbiota associated with health and recurrent tonsillitis. PLoS One. 2013;8(2):e56418
- Swidsinski A, Goktas O, Bessler C, et al. Spatial organisation of microbiota in quiescent adenoiditis and tonsillitis. J Clin Pathol. 2007 Mar;60(3):253-60
- Jensen JH, Larsen SB. Treatment of recurrent acute tonsillitis with clindamycin. An alternative to tonsillectomy? Clin Otolaryngol Allied Sci. 1991 Oct;16(5):498-500
- Raut VV. Management of peritonsillitis/peritonsillar. Rev Laryngol Otol Rhinol (Bord). 2000;121(2):107-10
- Fried MP, Forrest JL. Peritonsillitis. Evaluation of current therapy. Arch Otolaryngol. 1981 May;107(5):283-6
- Dalton RE, Abedi E, Sismanis A. Bilateral peritonsillar abscesses and quinsy tonsillectomy. J Natl Med Assoc. 1985 Oct;77(10):807-12
- Klug TE, Henriksen JJ, Rusan M, Fuursted K, Ovesen T. Bacteremia during quinsy and elective tonsillectomy: an evaluation of antibiotic prophylaxis recommendations for patients undergoing tonsillectomy. J Cardiovasc Pharmacol Ther. 2012 Sep;17(3):298-302
- Klug TE, Henriksen JJ, Fuursted K, Ovesen T. Significant pathogens in peritonsillar abscesses. Eur J Clin Microbiol Infect Dis. 2011 May;30(5):619-27
- Rusan M, Klug TE, Henriksen JJ, Ellermann-Eriksen S, Fuursted K, Ovesen T. The role of viruses in the pathogenesis of peritonsillar abscess. Eur J Clin Microbiol Infect Dis. 2012 Sep;31(9):2335-43
- Reichel O, Mayr D, Winterhoff J, de la CR, Hagedorn H, Berghaus A. Tonsillotomy or tonsillectomy?--a prospective study comparing histological and immunological findings in recurrent tonsillitis and tonsillar hyperplasia. Eur Arch Otorhinolaryngol. 2007 Mar;264(3):277-84
- Semberova J, Rychly B, Hanzelova J, Jakubikova J. The immune status in situ of recurrent tonsillitis and idiopathic tonsillar hypertrophy. Bratisl Lek Listy. 2013;114(3):140-4
- Perry M, Whyte A. Immunology of the tonsils. Immunol Today. 1998 Sep;19(9):414-21
- Goldberg S, Shatz A, Picard E, et al. Endoscopic findings in children with obstructive sleep apnea: effects of age and hypotonia. Pediatr Pulmonol. 2005 Sep;40(3):205-10
- Reichel O, Mayr D, Winterhoff J, de la CR, Hagedorn H, Berghaus A. Tonsillotomy or tonsillectomy?--a prospective study comparing histological and immunological findings in recurrent tonsillitis and tonsillar hyperplasia. Eur Arch Otorhinolaryngol. 2007 Mar;264(3):277-84
- Ericsson E, Lundeborg I, Hultcrantz E. Child behavior and quality of life before and after tonsillotomy versus tonsillectomy. Int J Pediatr Otorhinolaryngol. 2009 Sep;73(9):1254-62
- Stelter K, Ihrler S, Siedek V, Patscheider M, Braun T, Ledderose G. 1-year follow-up after radiofrequency tonsillotomy and laser tonsillotomy in children: a prospective, double-blind, clinical study. Eur Arch Otorhinolaryngol. 2012 Feb;269(2):679-84
- Sarny S, Ossimitz G, Habermann W, Stammberger H. [The Austrian tonsil study 2010--part 1: statistical overview]. Laryngorhinootologie. 2012 Jan;91(1):16-21
- Braun T, Dreher A, Dirr F, Reichel O, Patscheider M. [Pediatric OSAS and otitis media with effusion]. HNO. 2012 Mar;60(3):216-9
- Gronau S, Fischer Y. [Tonsillotomy]. Laryngorhinootologie. 2005 Sep;84(9):685-90
- Fischer Y, Gronau S. [Identification and evaluation of obstructive sleep apnea in children before adenotonsillectomy using evaluative surveys]. Laryngorhinootologie. 2005 Feb;84(2):121-35
- Alavoine J, Graber A. [Extracapsular tonsillectomy under general anesthesia]. Rev Laryngol Otol Rhinol (Bord). 1968 Sep;89(9):568-79
- Feinstein AR, Levitt M. Tonsils and rheumatic fever. N Engl J Med. 1970 Apr 2;282(14):814
- Rapkin RH. Tonsils and rheumatic fever. N Engl J Med. 1970 Apr 2;282(14):814
- Wannamaker LW. Tonsils, rheumatic fever and health delivery. N Engl J Med. 1970 Feb 5;282(6):336-7
- Feinstein AR, Levitt M. The role of tonsils in predisposing to streptococcal infections and recurrences of rheumatic fever. N Engl J Med. 1970 Feb 5;282(6):285-91
- van den Akker EH, Hoes AW, Burton MJ, Schilder AG. Large international differences in (adeno)tonsillectomy rates. Clin Otolaryngol Allied Sci. 2004 Apr;29(2):161-4
- Scherer H, Fuhrer A, Hopf J, et al. [Current status of laser surgery in the area of the soft palate and adjoining regions]. Laryngorhinootologie. 1994 Jan;73(1):14-20
- Koltai PJ, Solares CA, Mascha EJ, Xu M. Intracapsular partial tonsillectomy for tonsillar hypertrophy in children. Laryngoscope. 2002 Aug;112(8 Pt 2 Suppl 100):17-9
- Reichel O, Mayr D, Winterhoff J, de la CR, Hagedorn H, Berghaus A. Tonsillotomy or tonsillectomy?--a prospective study comparing histological and immunological findings in recurrent tonsillitis and tonsillar hyperplasia. Eur Arch Otorhinolaryngol. 2007 Mar;264(3):277-84
- CHAMPEAU D. [Intracapsular tonsillectomy.]. Ann Otolaryngol Chir Cervicofac. 1961 Dec;78:866-9
- FALCAO P. [Total intracapsular palatine tonsillectomy; systematization of technic.]. Rev Bras Otorrinolaringol. 1954 Jul;22(4-5):309-32
- Anand A, Vilela RJ, Guarisco JL. Intracapsular versus standard tonsillectomy: review of literature. J La State Med Soc. 2005 Sep;157(5):259-61
- Almqvist U. Cryosurgical treatment of tonsillar hypertrophy in children. J Laryngol Otol. 1986 Mar;100(3):311-4
- Principato JJ. Cryosurgical treatment of the lymphoid tissue of Waldeyer's ring. Otolaryngol Clin North Am. 1987 May;20(2):365-70
- Chatziavramidis A, Constantinidis J, Gennadiou D, Derwisis D, Sidiras T. [Volume reduction of tonsil hyperplasia in childhood with a surgical ultrasound device]. Laryngorhinootologie. 2007 Mar;86(3):177-83
- Pfaar O, Spielhaupter M, Schirkowski A, et al. Treatment of hypertrophic palatine tonsils using bipolar radiofrequency-induced thermotherapy (RFITT.). Acta Otolaryngol. 2007 Nov;127(11):1176-81
- Zhu X, Yang H, Chen X, Jin Y, Fan Y. [Temperature-controlled radiofrequency-assisted endoscopic tonsillectomy and adenoidectomy in children]. Lin Chung Er Bi Yan Hou Tou Jing Wai Ke Za Zhi. 2011 Jun;25(12):551-3
- Coticchia JM, Yun RD, Nelson L, Koempel J. Temperature-controlled radiofrequency treatment of tonsillar hypertrophy for reduction of upper airway obstruction in pediatric patients. Arch Otolaryngol Head Neck Surg. 2006 Apr;132(4):425-30
- Feinstein AR, Levitt M. Tonsils and rheumatic fever. N Engl J Med. 1970 Apr 2;282(14):814
- Rapkin RH. Tonsils and rheumatic fever. N Engl J Med. 1970 Apr 2;282(14):814
- Wannamaker LW. Tonsils, rheumatic fever and health delivery. N Engl J Med. 1970 Feb 5;282(6):336-7
- Feinstein AR, Levitt M. The role of tonsils in predisposing to streptococcal infections and recurrences of rheumatic fever. N Engl J Med. 1970 Feb 5;282(6):285-91
- el Barbary Ae, Mohieddin O, Fouad HA, Khalifa MC. The tonsils and rheumatic fever. Ann Otol Rhinol Laryngol. 1969 Jun;78(3):648-56
- Stryjecki J. [Tonsillectomy in the course of rheumatic fever in children]. Pediatr Pol. 1968 Dec;43(12):1531-4
- Matanoski GM, Price WH, Ferencz C. Epidemiology of streptococcal infections in rheumatic and nonrheumatic families. II. The interrelationship of streptococcal infections to age, family transmission and type of group A. Am J Epidemiol. 1968 Jan;87(1):190-206
- Alpert JJ, Peterson OL, Colton T. Tonsillectomy and adenoidectomy. Lancet. 1968 Jun 15;1(7555):1319
- Klug TE, Henriksen JJ, Fuursted K, Ovesen T. Similar recovery rates of Fusobacterium necrophorum from recurrently infected and non-infected tonsils. Dan Med Bull. 2011 Jul;58(7):A4295
- Klug TE, Henriksen JJ, Fuursted K, Ovesen T. Significant pathogens in peritonsillar abscesses. Eur J Clin Microbiol Infect Dis. 2011 May;30(5):619-27
- Ramirez-Camacho R, Gonzalez-Tallon AI, Gomez D, et al. [Environmental scanning electron microscopy for biofilm detection in tonsils]. Acta Otorrinolaringol Esp. 2008 Jan;59(1):16-20
- Mucke W, Huber HC, Ritter U. [The microbe colonization of the palatine tonsils of healthy school age children]. Zentralbl Hyg Umweltmed. 1994 Aug;196(1):70-4
- Mitchelmore IJ, Reilly PG, Hay AJ, Tabaqchali S. Tonsil surface and core cultures in recurrent tonsillitis: prevalence of anaerobes and betalactamase producing organisms. Eur J Clin Microbiol Infect Dis. 1994 Jul;13(7):542-8
- Schwaab M, Gurr A, Hansen S, et al. Human beta-Defensins in different states of diseases of the tonsilla palatina. Eur Arch Otorhinolaryngol. 2010 May;267(5):821-30
- Brook I, Foote PA, Jr. Comparison of the microbiology of recurrent tonsillitis between children and adults. Laryngoscope. 1986 Dec;96(12):1385-8
- Proenca-Modena JL, Pereira Valera FC, Jacob MG, et al. High rates of detection of respiratory viruses in tonsillar tissues from children with chronic adenotonsillar disease. PLoS One. 2012;7(8):e42136
- Stuck BA, Gotte K, Windfuhr JP, Genzwurker H, Schroten H, Tenenbaum T. Tonsillectomy in children. Dtsch Arztebl Int. 2008 Dec;105(49):852-60
- Österreichische Gesellschaften für HalsNasen-Ohren-Heilkunde KuH, Kinderund Jugendheilkunde. Gemeinsame Empfehlung zur Entfernung der Gaumenmandeln (Tonsillektomie). Monatsschr Kinderheilkd. 2008 Mar 7;3(156):268-71
- Kaplan EL. The group A streptococcal upper respiratory tract carrier state: an enigma. J Pediatr. 1980 Sep;97(3):337- 45
- Kaplan EL, Top FH, Jr., Dudding BA, Wannamaker LW. Diagnosis of streptococcal pharyngitis: differentiation of active infection from the carrier state in the symptomatic child. J Infect Dis. 1971 May;123(5):490-501
- Tanz RR, Shulman ST. Chronic pharyngeal carriage of group A streptococci. Pediatr Infect Dis J. 2007 Feb;26(2):175-6
- Tanz RR, Shulman ST. Streptococcal pharyngitis: the carrier state, definition, and management. Pediatr Ann. 1998 May;27(5):281-5
- Wessels MR. Clinical practice. Streptococcal pharyngitis. N Engl J Med. 2011 Feb 17;364(7):648-55
- Roberts AL, Connolly KL, Kirse DJ, et al. Detection of group A Streptococcus in tonsils from pediatric patients reveals high rate of asymptomatic streptococcal carriage. BMC Pediatr. 2012;12:3
- Drago L, Esposito S, De VE, et al. Detection of respiratory viruses and atypical bacteria in children's tonsils and adenoids. J Clin Microbiol. 2008 Jan;46(1):369-70
- Piacentini GL, Peroni DG, Blasi F, et al. Atypical bacteria in adenoids and tonsils of children requiring adenotonsillectomy. Acta Otolaryngol. 2010 May;130(5):620-5
- Chiappini E, Regoli M, Bonsignori F, et al. Analysis of different recommendations from international guidelines for the management of acute pharyngitis in adults and children. Clin Ther. 2011 Jan;33(1):48-58
- Chiappini E, Principi N, Mansi N, et al. Management of acute pharyngitis in children: summary of the Italian National Institute of Health guidelines. Clin Ther. 2012 Jun;34(6):1442-58
- Al-Layla A, Mahafza TM. Antibiotics do not reduce post-tonsillectomy morbidity in children. Eur Arch Otorhinolaryngol. 2013 Jan;270(1):367-70
- Dhiwakar M, Clement WA, Supriya M, McKerrow W. Antibiotics to reduce post-tonsillectomy morbidity. Cochrane Database Syst Rev. 2012;12:CD005607
- Hayward G, Thompson MJ, Perera R, Glasziou PP, Del Mar CB, Heneghan CJ. Corticosteroids as standalone or addon treatment for sore throat. Cochrane Database Syst Rev. 2012;10:CD008268
- Hayward G, Thompson MJ, Perera R, Del Mar CB, Glasziou PP, Heneghan CJ. Corticosteroids for the common cold. Cochrane Database Syst Rev. 2012;8:CD008116
- Hayward G, Thompson M, Heneghan C, Perera R, Del MC, Glasziou P. Corticosteroids for pain relief in sore throat: systematic review and metaanalysis. BMJ. 2009;339:b2976
- Moore N. Forty years of ibuprofen use. Int J Clin Pract Suppl. 2003 Apr;(135):28-31
- van den Anker JN. Optimising the management of fever and pain in children. Int J Clin Pract Suppl. 2013 Jan;(178):26-32
- Hay AD, Redmond NM, Costelloe C, et al. Paracetamol and ibuprofen for the treatment of fever in children: the PITCH randomised controlled trial. Health Technol Assess. 2009 May;13(27):iii-x,1
- Hay AD, Costelloe C, Redmond NM, et al. Paracetamol plus ibuprofen for the treatment of fever in children (PITCH): randomised controlled trial. BMJ. 2008;337:a1302
- Forrest JB, Heitlinger EL, Revell S. Ketorolac for postoperative pain management in children. Drug Saf. 1997 May;16(5):309-29
- Romsing J, Ostergaard D, Drozdziewicz D, Schultz P, Ravn G. Diclofenac or acetaminophen for analgesia in paediatric tonsillectomy outpatients. Acta Anaesthesiol Scand. 2000 Mar;44(3):291-5
- Romsing J, Ostergaard D, WaltherLarsen S, Valentin N. Analgesic efficacy and safety of preoperative versus postoperative ketorolac in paediatric tonsillectomy. Acta Anaesthesiol Scand. 1998 Aug;42(7):770-5
- Barzaga AZ, Choonara I. Balancing the risks and benefits of the use of over-thecounter pain medications in children. Drug Saf. 2012 Dec 1;35(12):1119-25
- Feinstein AR, Levitt M. The role of tonsils in predisposing to streptococcal infections and recurrences of rheumatic fever. N Engl J Med. 1970 Feb 5;282(6):285-91
- Del Mar CB, Glasziou PP, Spinks AB. Antibiotics for sore throat. Cochrane Database Syst Rev. 2006;(4):CD000023
- Lehnerdt G, Senska K, Fischer M, Jahnke K. Bilateral peritonsillar abscesses. Eur Arch Otorhinolaryngol. 2005 Jul;262(7):573-5
- Segal N, El-Saied S, Puterman M. Peritonsillar abscess in children in the southern district of Israel. Int J Pediatr Otorhinolaryngol. 2009 Aug;73(8):1148-50
- Powell EL, Powell J, Samuel JR, Wilson JA. A review of the pathogenesis of adult peritonsillar abscess: time for a reevaluation. J Antimicrob Chemother. 2013 Apr 23.
- Segal N, El-Saied S, Puterman M. Peritonsillar abscess in children in the southern district of Israel. Int J Pediatr Otorhinolaryngol. 2009 Aug;73(8):1148-50
- Powell J, Wilson JA. An evidence-based review of peritonsillar abscess. Clin Otolaryngol. 2012 Apr;37(2):136-45
- Herzon FS, Martin AD. Medical and surgical treatment of peritonsillar, retropharyngeal, and parapharyngeal abscesses. Curr Infect Dis Rep. 2006 May;8(3):196-202
- Powell J, Wilson JA. An evidence-based review of peritonsillar abscess. Clin Otolaryngol. 2012 Apr;37(2):136-45
- Lehnerdt G, Senska K, Jahnke K, Fischer M. Post-tonsillectomy haemorrhage: a retrospective comparison of abscess- and elective tonsillectomy. Acta Otolaryngol. 2005 Dec;125(12):1312-7
- Powell J, Wilson JA. An evidence-based review of peritonsillar abscess. Clin Otolaryngol. 2012 Apr;37(2):136-45
- Paradise JL, Bluestone CD, Bachman RZ, et al. Efficacy of tonsillectomy for recurrent throat infection in severely affected children. Results of parallel randomized and nonrandomized clinical trials. N Engl J Med. 1984 Mar 15;310(11):674-83
- Paradise JL, Bluestone CD, Bachman RZ, et al. Efficacy of tonsillectomy for recurrent throat infection in severely affected children. Results of parallel randomized and nonrandomized clinical trials. N Engl J Med. 1984 Mar 15;310(11):674-83
- Paradise JL, Bluestone CD, Bachman RZ, et al. History of recurrent sore throat as an indication for tonsillectomy. Predictive limitations of histories that are undocumented. N Engl J Med. 1978 Feb 23;298(8):409-13
- Paradise JL, Bluestone CD, Bachman RZ, et al. Efficacy of tonsillectomy for recurrent throat infection in severely affected children. Results of parallel randomized and nonrandomized clinical trials. N Engl J Med. 1984 Mar 15;310(11):674-83
- Paradise JL, Bluestone CD, Colborn DK, Bernard BS, Rockette HE, KursLasky M. Tonsillectomy and adenotonsillectomy for recurrent throat infection in moderately affected children. Pediatrics. 2002 Jul;110(1 Pt 1):7-15
- Kaygusuz I, Alpay HC, Godekmerdan A, et al. Evaluation of long-term impacts of tonsillectomy on immune functions of children: a follow-up study. Int J Pediatr Otorhinolaryngol. 2009 Mar;73(3):445-9
- Windfuhr JP, Schloendorff G, Baburi D, Kremer B. Serious post-tonsillectomy hemorrhage with and without lethal outcome in children and adolescents. Int J Pediatr Otorhinolaryngol. 2008 Jul;72(7):1029-40
- Stelter K, Ihrler S, Siedek V, Patscheider M, Braun T, Ledderose G. 1-year follow-up after radiofrequency tonsillotomy and laser tonsillotomy in children: a prospective, double-blind, clinical study. Eur Arch Otorhinolaryngol. 2012 Feb;269(2):679-84
- Stelter K, de la CR, Patscheider M, Olzowy B. Double-blind, randomised, controlled study of post-operative pain in children undergoing radiofrequency tonsillotomy versus laser tonsillotomy. J Laryngol Otol. 2010 Aug;124(8):880-5
- Scherer H, Fuhrer A, Hopf J, et al. [Current status of laser surgery in the area of the soft palate and adjoining regions]. Laryngorhinootologie. 1994 Jan;73(1):14-20
- Ericsson E, Graf J, Hultcrantz E. Pediatric tonsillotomy with radiofrequency technique: long-term follow-up. Laryngoscope. 2006 Oct;116(10):1851-7
- Scherer H, Fuhrer A, Hopf J, et al. [Current status of laser surgery in the area of the soft palate and adjoining regions]. Laryngorhinootologie. 1994 Jan;73(1):14-20
- Stelter K, de la CR, Patscheider M, Olzowy B. Double-blind, randomised, controlled study of post-operative pain in children undergoing radiofrequency tonsillotomy versus laser tonsillotomy. J Laryngol Otol. 2010 Aug;124(8):880-5
- Watson MG, Dawes PJ, Samuel PR, et al. A study of haemostasis following tonsillectomy comparing ligatures with diathermy. J Laryngol Otol. 1993 Aug;107(8):711-5
- Kristensen S, Tveteras K. Posttonsillectomy haemorrhage. A retrospective study of 1150 operations. Clin Otolaryngol Allied Sci. 1984 Dec;9(6):347-50
- Andrea M. Microsurgical bipolar cautery tonsillectomy. Laryngoscope. 1993 Oct;103(10):1177-8
- Ewah B. An evaluation of pain, postoperative nausea and vomiting following the introduction of guidelines for tonsillectomy. Paediatr Anaesth. 2006 Oct;16(10):1100-1
- Scherer H, Fuhrer A, Hopf J, et al. [Current status of laser surgery in the area of the soft palate and adjoining regions]. Laryngorhinootologie. 1994 Jan;73(1):14-20
- Unkel C, Lehnerdt G, Schmitz KJ, Jahnke K. Laser-tonsillotomy for treatment of obstructive tonsillar hyperplasia in early childhood: a retrospective review. Int J Pediatr Otorhinolaryngol. 2005 Dec;69(12):1615-20
- Davies J, Coatesworth AP. Double-blind randomized controlled study of coblation tonsillotomy versus coblation tonsillectomy on post-operative pain. Clin Otolaryngol. 2005 Dec;30(6):572-3
- Haegner U, Handrock M, Schade H. ["Ultrasound tonsillectomy" in comparison with conventional tonsillectomy]. HNO. 2002 Sep;50(9):836-43
- Pfaar O, Spielhaupter M, Schirkowski A, et al. Treatment of hypertrophic palatine tonsils using bipolar radiofrequency-induced thermotherapy (RFITT). Acta Otolaryngol. 2007 Apr 23;1-6
- Isaacson G. Pediatric intracapsular tonsillectomy with bipolar electrosurgical scissors. Ear Nose Throat J. 2004 Oct;83(10):702, 704-702, 706
- Huber K, Sadick H, Maurer JT, Hormann K, Hammerschmitt N. [Tonsillotomy with the argon-supported monopolar needle--first clinical results]. Laryngorhinootologie. 2005 Sep;84(9):671-5
- Lister MT, Cunningham MJ, Benjamin B, et al. Microdebrider tonsillotomy vs electrosurgical tonsillectomy: a randomized, double-blind, paired control study of postoperative pain. Arch Otolaryngol Head Neck Surg. 2006 Jun;132(6):599-604
- Stelter K, de la CR, Patscheider M, Olzowy B. Double-blind, randomised, controlled study of post-operative pain in children undergoing radiofrequency tonsillotomy versus laser tonsillotomy. J Laryngol Otol. 2010 Aug;124(8):880-5
- Scherer H. [Tonsillotomy versus tonsillectomy]. Laryngorhinootologie. 2003 Nov;82(11):754-5
- Windfuhr JP, Werner JA. Tonsillotomy: it's time to clarify the facts. Eur Arch Otorhinolaryngol. 2013 Aug 22
- Sobol SE, Wetmore RF, Marsh RR, Stow J, Jacobs IN. Postoperative recovery after microdebrider intracapsular or monopolar electrocautery tonsillectomy: a prospective, randomized, single-blinded study. Arch Otolaryngol Head Neck Surg. 2006 Mar;132(3):270-4
- Cantarella G, Viglione S, Forti S, Minetti A, Pignataro L. Comparing postoperative quality of life in children after microdebrider intracapsular tonsillotomy and tonsillectomy. Auris Nasus Larynx. 2012 Aug;39(4):407-10
- Nguyen CV, Parikh SR, Bent JP. Comparison of intraoperative bleeding between microdebrider intracapsular tonsillectomy and electrocautery tonsillectomy. Ann Otol Rhinol Laryngol. 2009 Oct;118(10):698-702
- Reilly BK, Levin J, Sheldon S, Harsanyi K, Gerber ME. Efficacy of microdebrider intracapsular adenotonsillectomy as validated by polysomnography. Laryngoscope. 2009 Jul;119(7):1391-3
- Vaughan AH, Derkay CS. Microdebrider intracapsular tonsillectomy. ORL J Otorhinolaryngol Relat Spec. 2007;69(6):358-63
- Sobol SE, Wetmore RF, Marsh RR, Stow J, Jacobs IN. Postoperative recovery after microdebrider intracapsular or monopolar electrocautery tonsillectomy: a prospective, randomized, single-blinded study. Arch Otolaryngol Head Neck Surg. 2006 Mar;132(3):270-4
- Sorin A, Bent JP, April MM, Ward RF. Complications of microdebrider-assisted powered intracapsular tonsillectomy and adenoidectomy. Laryngoscope. 2004 Feb;114(2):297-300
- Segal N, Puterman M, Rotem E, et al. A prospective randomized double-blind trial of fibrin glue for reducing pain and bleeding after tonsillectomy. Int J Pediatr Otorhinolaryngol. 2008 Apr;72(4):469-73
- Sampaio AL, Pinheiro TG, Furtado PL, Araujo MF, Olivieira CA. Evaluation of early postoperative morbidity in pediatric tonsillectomy with the use of sucralfate. Int J Pediatr Otorhinolaryngol. 2007 Apr;71(4):645-51
- Cantarella G, Viglione S, Forti S, Minetti A, Pignataro L. Comparing postoperative quality of life in children after microdebrider intracapsular tonsillotomy and tonsillectomy. Auris Nasus Larynx. 2012 Aug;39(4):407-10
- Lavy JA. Post-tonsillectomy pain: the difference between younger and older patients. Int J Pediatr Otorhinolaryngol. 1997 Oct 18;42(1):11-5
- Stelter K, Hempel JM, Berghaus A, Andratschke M, Luebbers CW, Hagedorn H. Application methods of local anaesthetic infiltrations for postoperative pain relief in tonsillectomy: a prospective, randomised, double-blind, clinical trial. Eur Arch Otorhinolaryngol. 2009 Jan 22
- Stelter K, Hiller J, Hempel JM, et al. Comparison of two different local anaesthetic infiltrations for postoperative pain relief in tonsillectomy: a prospective, randomised, double blind, clinical trial. Eur Arch Otorhinolaryngol. 2010 Jul;267(7):1129-34
- Sadhasivam S, Chidambaran V, Ngamprasertwong P, et al. Race and unequal burden of perioperative pain and opioid related adverse effects in children. Pediatrics. 2012 May;129(5):832-8
- Tekelioglu UY, Apuhan T, Akkaya A, et al. Comparison of topical tramadol and ketamine in pain treatment after tonsillectomy. Paediatr Anaesth. 2013 Jun;23(6):496-501
- Ozkiris M, Kapusuz Z, Saydam L. Comparison of ropivacaine, bupivacaine and lidocaine in the management of post-tonsillectomy pain. Int J Pediatr Otorhinolaryngol. 2012 Dec;76(12):1831-4
- Stelter K, Hiller J, Hempel JM, et al. Comparison of two different local anaesthetic infiltrations for postoperative pain relief in tonsillectomy: a prospective, randomised, double blind, clinical trial. Eur Arch Otorhinolaryngol. 2010 Jul;267(7):1129-34
- Stelter K, Hempel JM, Berghaus A, Andratschke M, Luebbers CW, Hagedorn H. Application methods of local anaesthetic infiltrations for postoperative pain relief in tonsillectomy: a prospective, randomised, double-blind, clinical trial. Eur Arch Otorhinolaryngol. 2009 Jan 22
- Arikan OK, Ozcan S, Kazkayasi M, Akpinar S, Koc C. Preincisional infiltration of tonsils with ropivacaine in post-tonsillectomy pain relief: doubleblind, randomized, placebo-controlled intraindividual study. J Otolaryngol. 2006 Jun;35(3):167-72
- Rotenberg BW, Wickens B, Parnes J. Intraoperative ice pack application for uvulopalatoplasty pain reduction: a randomized controlled trial. Laryngoscope. 2013 Feb;123(2):533-6
- Sylvester DC, Rafferty A, Bew S, Knight LC. The use of ice-lollies for pain relief post-paediatric tonsillectomy. A single-blinded, randomised, controlled trial. Clin Otolaryngol. 2011 Dec;36(6):566-70
- Steward DL, Grisel J, Meinzen-Derr J. Steroids for improving recovery following tonsillectomy in children. Cochrane Database Syst Rev. 2011;(8):CD003997
- Windfuhr JP, Chen YS, Propst EJ, Guldner C. The effect of dexamethasone on post-tonsillectomy nausea, vomiting and bleeding. Braz J Otorhinolaryngol. 2011 Jun;77(3):373-9
- Randel A. AAO-HNS Guidelines for Tonsillectomy in Children and Adolescents. Am Fam Physician. 2011 Sep 1;84(5):566-73
- Baugh RF, Archer SM, Mitchell RB, et al. Clinical practice guideline: tonsillectomy in children. Otolaryngol Head Neck Surg. 2011 Jan;144(1 Suppl):S1- 30
- Sutters KA, Miaskowski C, HoldridgeZeuner D, et al. A randomized clinical trial of the effectiveness of a scheduled oral analgesic dosing regimen for the management of postoperative pain in children following tonsillectomy. Pain. 2004 Jul;110(1-2):49-55
- Lewis SR, Nicholson A, Cardwell ME, Siviter G, Smith AF. Nonsteroidal antiinflammatory drugs and perioperative bleeding in paediatric tonsillectomy. Cochrane Database Syst Rev. 2013 Jul 18;7:CD003591
- Riggin L, Ramakrishna J, Sommer DD, Koren G. A 2013 updated systematic review & meta-analysis of 36 randomized controlled trials; no apparent effects of non steroidal antiinflammatory agents on the risk of bleeding after tonsillectomy. Clin Otolaryngol. 2013 Apr;38(2):115-29
- Zernikow B, Smale H, Michel E, Hasan C, Jorch N, Andler W. Paediatric cancer pain management using the WHO analgesic ladder--results of a prospective analysis from 2265 treatment days during a quality improvement study. Eur J Pain. 2006 Oct;10(7):587-95
- Hadden SM, Burke CN, Skotcher S, Voepel-Lewis T. Early postoperative outcomes in children after adenotonsillectomy. J Perianesth Nurs. 2011 Apr;26(2):89-95
- Stelter K, Hempel JM, Berghaus A, Andratschke M, Luebbers CW, Hagedorn H. Application methods of local anaesthetic infiltrations for postoperative pain relief in tonsillectomy: a prospective, randomised, double-blind, clinical trial. Eur Arch Otorhinolaryngol. 2009 Jan 22
- Kamarauskas A, Dahl MR, Hlidarsdottir T, Mainz J, Ovesen T. Need for better analgesic treatment after tonsillectomy in ear, nose and throat practices. Dan Med J. 2013 May;60(5):A4639
- Stanko D, Bergesio R, Davies K, Hegarty M, von Ungern-Sternberg BS. Postoperative pain, nausea and vomiting following adeno-tonsillectomy - a longterm follow-up. Paediatr Anaesth. 2013 May 13
- Chan CC, Chan YY, Tanweer F. Systematic review and meta-analysis of the use of tranexamic acid in tonsillectomy. Eur Arch Otorhinolaryngol. 2013 Feb;270(2):735-48
- Sarny S, Habermann W, Ossimitz G, Stammberger H. Significant posttonsillectomy pain is associated with increased risk of hemorrhage. Ann Otol Rhinol Laryngol. 2012 Dec;121(12):776-81
- Windfuhr JP, Schloendorff G, Baburi D, Kremer B. Serious post-tonsillectomy hemorrhage with and without lethal outcome in children and adolescents. Int J Pediatr Otorhinolaryngol. 2008 Jul;72(7):1029-40
- Hessen Soderman AC, Ericsson E, Hemlin C, et al. Reduced risk of primary postoperative hemorrhage after tonsil surgery in Sweden: results from the National Tonsil Surgery Register in Sweden covering more than 10 years and 54,696 operations. Laryngoscope. 2011 Nov;121(11):2322-6
- Krespi YP, Kizhner V. Laser tonsil cryptolysis: In-office 500 cases review. Am J Otolaryngol. 2013 Apr 10
- Pfaar O, Spielhaupter M, Schirkowski A, et al. Treatment of hypertrophic palatine tonsils using bipolar radiofrequency-induced thermotherapy (RFITT.). Acta Otolaryngol. 2007 Nov;127(11):1176-81
- Sarny S, Ossimitz G, Habermann W, Stammberger H. Hemorrhage following tonsil surgery: a multicenter prospective study. Laryngoscope. 2011 Dec;121(12):2553-60
- Sarny S, Ossimitz G, Habermann W, Stammberger H. [Austrian tonsil study part 3: surgical technique and postoperative haemorrhage after tonsillectomy]. Laryngorhinootologie. 2013 Feb;92(2):92-6
- Windfuhr JP, Wienke A, Chen YS. Electrosurgery as a risk factor for secondary post-tonsillectomy hemorrhage. Eur Arch Otorhinolaryngol. 2009 Jan;266(1):111-6
Authors
PD Dr. med. Klaus Stelter
Dep. of Otorhinolaryngology, Head and Neck Surgery
RoMed Clinic Bad Aibling
Harthauser Str. 16
83043 Bad Aibling
info@alpenpraxisklinik.de
Prof. Dr. med. Götz Lehnerdt
Dep. of Otorhinolaryngology, Head and Neck Surgery
St. Anna Clinic Wuppertal
Vogelsangstr. 106
42109 Wuppertal
Hno.kh-anna@cellitinnen.de
Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


