2.2.5: Setting Boundaries
- Page ID
- 67560
It is important as a HHA/PCA that boundaries are set in order to best meet the needs of the patient. According to the National Council of State Boards of Nursing (2014), certain “red flag” behaviors can indicate boundaries are being blurred. These can include: discussing personal issues with a patient, keeping secrets with or for a patient, flirting with a patient, gossiping or “bad-mouthing” co-workers and others on the treatment team, spending more time than necessary with a patient, believing you are the only one who understands or can provide proper care for the patient, showing favoritism toward a patient, and meeting with a patient or their family outside of the designated treatment areas.
Behaviors such as over-helping, controlling, and possessiveness over the patient can indicate that boundaries have become blurred. When relationships are terminated, intense emotions may arise leading the health care worker to engage in behaviors such as continuing to visit the patient, which are unprofessional and unhealthy for the patient. These are important issues to consider in order to set and maintain appropriate professional boundaries with patients.
- Over–helping: Sometimes, we want to help others so much that we take away their independence. For HHAs/PCAs, it is important that they properly care for their patient and help them with what they cannot do for themselves. It is also equally important that they work to promote their independence so the patients do not become too reliant on the HHA/PCA and not do for themselves what they are capable. Promoting independence helps to boost a person’s self-esteem and helps to avoid feelings of helplessness and worthlessness. For instance a patient who is capable of cutting their food might say, “Can you cut this for me? I am too tired.” The response can be something like, “I understand that you are feeling tired today, but it is important that you do things for yourself that you are able. One of the goals we are working on together is to help you become independent and regain your strength. I will sit with you while you cut your food.” This reminds the patient of the established goals, provides encouragement for them, and demonstrates belief in their capabilities. It also demonstrates that the HHA/PCA will be there for them even when they must complete difficult or tiresome tasks.
- Controlling: At times it may seem easier to “take over” with a patient. Home Health Aides/Personal Care Aides may feel that doing something a certain way is best and that they know what is for the patient’s “own good”.Avoid being too controlling or authoritative (bossy) with patients. Instead of telling them what to do, help them to come to their own decisions by exploring their options. Give patients choices whenever possible. For instance, a HHA/PCA knows that their tasks for the day are to bathe their patient and walk them around their living room. While they may want to do a particular task before the other, give the patient a choice. “I am here to help you bathe and take a walk today. Which one would you like to do first?” Give patients options when meal planning rather than just deciding what food is best for them and that they should eat a certain food for their “own good.” For example, a HHA/PCA could ask, “Would you like a turkey sandwich, meatloaf, or pasta for lunch today?” or “What kind of vegetable would you like with your dinner?”
- Possessiveness: As Home Health Aides/Personal Care Aides develop strong working relationships with their patients and their families, they will come to know them very well. They may come to know them better than other members of the healthcare team. Sometimes, this can lead to feelings of possessiveness over the patient/family. They may feel that they know how to best treat their patient. This leads to a breakdown in the care of the patient among members of the healthcare team. It is important to be aware of these types of feelings.
Examples of feelings, thoughts, and behaviors that may indicate possessiveness over a patient include:
- Feeling angry toward other health-care team members when they make decisions that the HHA/PCA does not agree with
- Arriving to work early and leaving late to spend extra time with the patient
- Withholding information from other members of the health-care team
- Excessively disclosing personal information about yourself to the patient/family to form a close relationship
- Creating a “you and me against the world” attitude where the HHA/PCA views the patient as more than a patient and sides with their position regardless of the situation.
These types of feelings, thoughts, and behaviors are unhealthy for both the HHA/PCA and the patient. They only serve to create disconnection in the patient’s care and make the patient too reliant on the HHA/PCA. If a HHA/PCA finds that they are starting to become too possessive of their patient, they should speak with their supervisor about their feelings and how to work these out.
- Terminating the relationship: Different from your relationship with your own family or friends, there may be an end date to the relationship between a HHA/PCA and their patient and family. Some patients/families may want to continue to have a relationship with the HHA/PCA. They may ask them to call and visit. Ending a relationship with someone is often very difficult. It can awaken strong feelings in the patient and in the HHA/PCA. Patients may feel uncared for, angry, or depressed that they will no longer be working with the HHA/PCA. It is important for a HHA/PCA to remember to keep professional boundaries while also explaining to the patient how much they have enjoyed and have come to value the relationship you have with them. For example, a patient might say, “Will you come visit me even after you stop working here?” The HHA/PCA can say something like, “I have enjoyed working with you so much. I am not able to continue to come visit you once we have stopped working together. It is against my company‘s policy. Let‘s talk about how you feel about ending our relationship.”
Ending a relationship with their patient may also stir up strong feelings for them. It is important for a HHA/PCA to discuss their feelings and how to handle them with their supervisor and not their patient. They must remember that they are there to care for the patient, not the other way around. The company may have specific policies about termination of relationships. This is an important issue to discuss with a supervisor.
It can be difficult to decide if a behavior is crossing the lines of professional boundaries. A helpful way to decide whether one should proceed with a behavior or not is to follow the following decision tree.
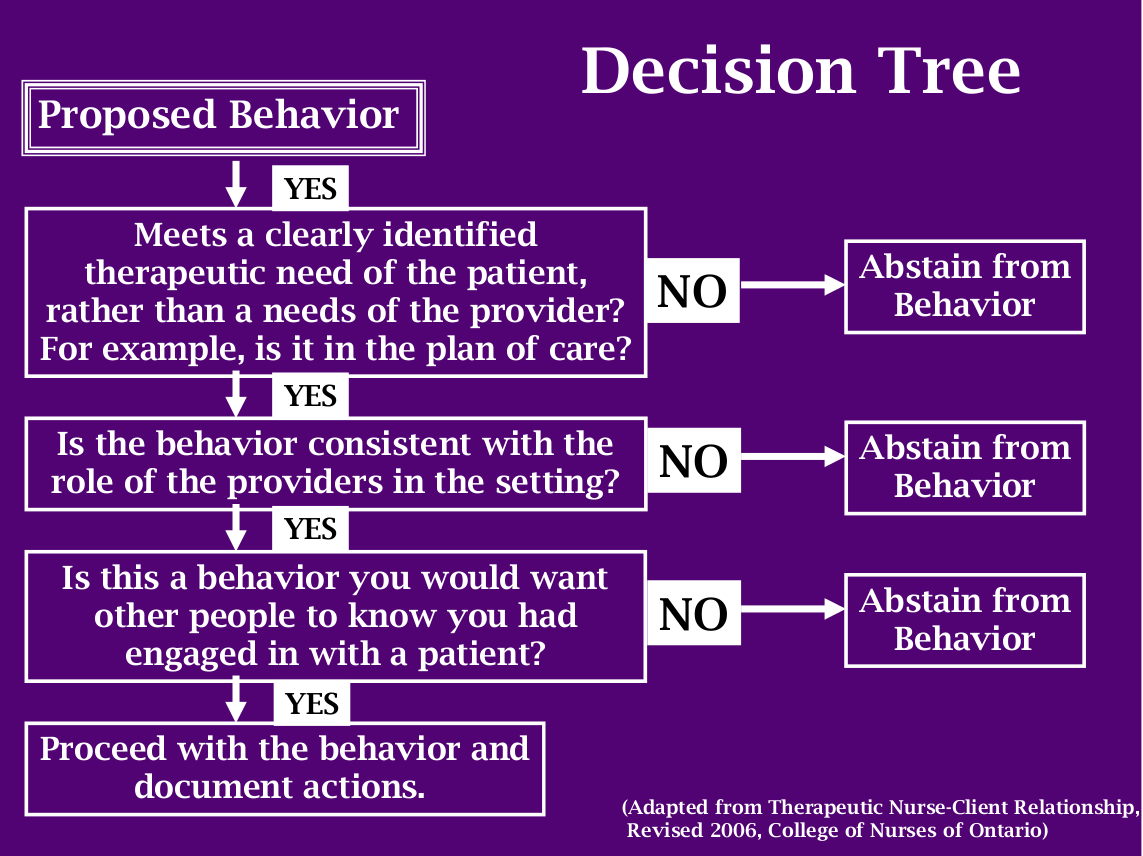
REMEMBER: If a Home Health Aide/Personal Care Aide comes to the realization that the behavior is not part of the care plan, and is not in the best interests of the patient/family, they should not engage in the behavior. If they realize that the behavior is outside of their scope of practice and not within their defined role as a Home Health Aide/Personal Care Aide, they should refrain from the behavior. If they realize that the behavior is not something they would want others to know that they did, they should refrain from the behavior.
Self–check for boundaries: The following is a list of helpful questions the HHA/PCA can ask themselves when determining whether a behavior is crossing a boundary. This list is adapted from Jane W. Barton’s Professional Boundaries: Discerning the Line in the Sand, which can be found at http://www.capnm.ca/Prof_Boundaries_Packet_2010.pdf
- Is this behavior or action in my patient’s best interests?
- Whose needs are being served by engaging in this behavior? Mine or the patient’s?
- Are my actions meant to best meet the needs of my patient or am I meeting my own needs?
- What emotions of my own are being stirred up by this patient/family and are these emotions affecting my ability to effectively make decisions and care for my patient?
- Am I treating this patient differently than other patients with whom I work?
- Will this behavior have an impact on the care I give my patient?
- How would others (healthcare team members, patient’s family) view this behavior?
- Am I taking advantage of the patient?
- Am I comfortable documenting this decision or behavior in the patient’s file?
- Does this decision or behavior go against my agency’s policies?
Which of the following would be considered a boundary violation? Answer Yes or No.
Preparing a pureed diet by following instructions listed in the care plan. ______
Staying one hour longer past the shift to visit with the patient, making you late for the next home health care patient. ______
Taking a ten dollar tip from the patient’s family. ______
Agreeing to continue to visit the patient even after their case has been closed by the agency and they are no longer receiving home health care services. ______
Providing a bed bath for a patient who requires one daily. ______
Visiting a patient when you are not scheduled to work. ______
Turning and positioning a bed bound patient every two hours. ______
Informing a supervisor about a suspicion about abuse. ______
Cooking lunch for yourself using the patient’s food. ______
Not informing a supervisor about a patient’s statement of wanting to die because the HHA/PCA told their patient they would keep it a secret. ______
- Answer
-
1. No
2. Yes
3. Yes
4. Yes
5. No
6. Yes
7. No
8. No
9. Yes
10. Yes
Feedback:
1. Following directions as stated in the care plan is providing competent care. This would not be a boundary violation.
2. Staying past the time your agency/supervisor has established is considered to be a boundary violation. This can indicate possessiveness of the patient and can lead to a breakdown in the care of the patient among members of the healthcare team.
3. Taking money or gifts from a patient or their family is considered to be a boundary violation and is unprofessional behavior. Many agencies have policies prohibiting this type of behavior.
4. Continuing to visit a patient once the relationship has ended is considered to be a boundary violation. While ending a relationship can stir up various emotions, it is wise for the HHA/PCA to discuss these emotions with their supervisor rather than with the patient. Many companies have specific policies about termination of relationships.
5. Providing a bed bath as required by the care plan is an assigned task and is considered to be providing competent care, which is not a boundary violation.
6. Visiting a patient outside of working hours is considered to be a boundary violation and is unprofessional behavior. This can indicate possessiveness of the patient and can lead to a breakdown in the care of the patient among members of the healthcare team. Many agencies may have policies in place to prohibit this type of behavior.
7. Turning and positioning a patient in bed is performing competent care and is not a boundary violation.
8. Informing a supervisor about suspicions of abuse is an important aspect of a HHA/PCA’s responsibilities and is not considered a boundary violation.
9. Using a patient’s food for your personal use is a boundary violation and should never be done. Many agencies may have policies in place to prohibit this type of behavior.
10. Keeping a secret from the rest of the health care team is a boundary violation. It is important to always inform your supervisor about important statements patients make about their health care, especially statements indicating suicidal thoughts or abuse.

