18.5B: Arterial Blood Pressure
- Page ID
- 7857
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)The measurement of blood pressure without further specification usually refers to systemic arterial pressure measured at the upper arm.
- Distinguish between arterial blood pressure and venous blood pressure
Key Points
- Systemic blood pressure refers to the pressure exerted on blood vessels in systemic circulation, and is often measured using arterial pressure, or pressure exerted upon arteries during heart contractions.
- Blood pressure (BP), sometimes referred to as arterial blood pressure, is the pressure exerted by circulating blood upon the walls of blood vessels, and is one of the principal vital signs.
- All levels of arterial pressure put mechanical stress on the arterial walls. Higher pressures increase heart workload and progression of unhealthy tissue growth ( atheroma ) that develops within the walls of arteries.
Key Terms
- atheroma: An abnormal fatty deposit that develops within the walls of arteries.
- arterial blood pressure: The pressure of the blood within an arterial vessel, typically the brachial artery in the upper arm. Calculated over a cardiac cycle and determined by the cardiac output (CO), systemic vascular resistance (SVR), and central venous pressure (CVP). It can be approximately determined from measurements of the systolic pressure and the diastolic pressure while there is a normal resting heart rate.
- systemic circulation: The part of blood circulation that carries oxygenated blood away from the heart to the body, and returns deoxygenated blood back to the heart.
The measurement of blood pressure without further specification usually refers to the systemic arterial pressure, defined as the pressure exerted by circulating blood upon the walls of blood vessels. Pressure is typically measured with a blood pressure cuff ( sphygmomanometer ) wrapped around a person’s upper arm, which measures the pressure in the brachial artery. A person’s blood pressure is usually expressed in terms of the systolic pressure over diastolic pressure and is measured in millimeters of mercury (mmHg), for example 140/90.
Blood pressure in the arteries is much higher than in the veins, in part due to receiving blood from the heart after contraction, but also due to their contractile capacity. The tunica media of arteries is thickened compared to veins, with smoother muscle fibers and elastic tissue. Together, these generate of elastic recoil and blood vessel contraction, allowing for the maintenance of a higher pressure.
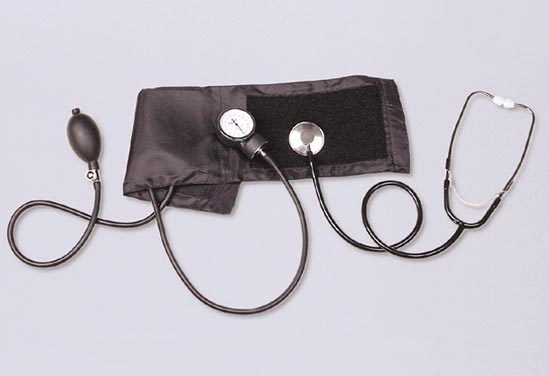
Typical Tools of Auscultatory Measurement: Shown here are a stethoscope and a sphygmomanometer, used for ascultatory measurement.
Blood Pressure and Cardiovascular Disease
While average values for arterial pressure could be computed for any given population, there is extensive variation from person to person and even from minute to minute for an individual. Additionally, the average arterial pressure of a given population has only a questionable correlation with its general health. However, in a study of 100 human subjects with no known history of hypertension, the average blood pressure of 112/64 mmHg, currently classified as a desirable or “normal” value. Normal values fluctuate through the 24-hour cycle, with the highest readings in the afternoons and lowest readings at night
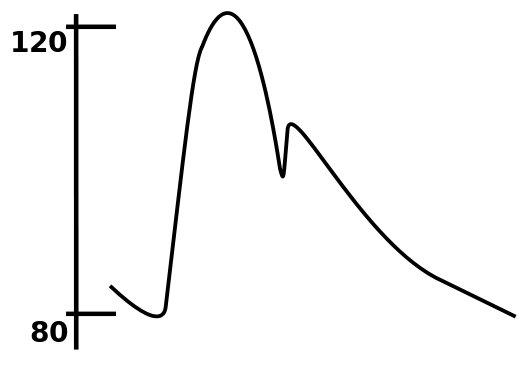
Changes in Arterial Pressure: Arterial pressures changes across the cardiac cycle.
The risk of cardiovascular disease increases progressively above 115/75 mmHg. In the past, hypertension was only diagnosed if secondary signs of high arterial pressure were present along with a prolonged high systolic pressure reading over several visits. Hypotension is typically diagnosed only if noticeable symptoms are present. Clinical trials demonstrate that people who maintain arterial pressures at the low end of these ranges have much better long-term cardiovascular health. The principal medical debate concerns the aggressiveness and relative value of methods used to lower pressures into this range for those with high blood pressure. Elevations more commonly seen in older people, though often considered normal, are associated with increased morbidity and mortality.
Arterial Hypertension
Arterial hypertension can be an indicator of other problems and may have long-term adverse effects. Sometimes it can be an acute problem, such as a hypertensive emergency. All levels of arterial pressure put mechanical stress on the arterial walls. Higher pressures increase heart workload and progression of unhealthy tissue growth (atheroma) that develops within the walls of arteries. The higher the pressure, the more stress that is present, the more the atheroma tends to progress, and the more heart muscle may thicken, enlarge, and weaken over time.
Persistent hypertension is one of the risk factors for strokes, heart attacks, heart failure, and arterial aneurysms, and is the leading cause of chronic renal failure. Even moderate elevation of arterial pressure leads to shortened life expectancy. At mean arterial pressures 50% or more above average, a person can expect to live no more than a few years unless appropriately treated.
In the past, most attention was paid to diastolic pressure, but now we know that both high systolic pressure and high pulse pressure (the numerical difference between systolic and diastolic pressures) are also risk factors for disease. In some cases, a decrease in excessive diastolic pressure can actually increase risk, probably due to the increased difference between systolic and diastolic pressures. If systolic blood pressure is elevated (>140) with a normal diastolic blood pressure (<90), it is called “isolated systolic hypertension” and may present a health concern.


