Blood Vessels and Blood Vocabulary
Acquired immunodeficiency syndrome (AIDS): A disease caused by the human immunodeficiency virus (HIV). People with acquired immunodeficiency syndrome are at an increased risk for developing certain cancers and for infections that usually occur only in individuals with a weak immune system (National Cancer Institute, n.d.)
Anaphylaxis: An acute hypersensitivity reaction due to exposure to a previously encountered antigen.
Anemia: A condition in which the number of red blood cells or hemoglobin is deficient.
Aneurysm: Weakening of the wall of a blood vessel, causing it to thin and balloon out, and possibly eventually burst, resulting in internal bleeding.
Angiography: A procedure to x-ray blood vessels.
Angioplasty: A procedure in which an occlusion is mechanically widened with a balloon.
Angioscope: Instrument used for visual examination of blood vessels.
Angioscopy: Endoscopic examination of blood vessels.
Anti-B antibodies: Proteins that will mount an immune response against B antigens.
Antibodies: Proteins made by plasma cells (a type of white blood cell) in response to an antigen (a substance that causes the body to make a specific immune response). Each antibody can bind to only one specific antigen. The purpose of this binding is to help destroy the antigen.
Antigens: Substances that provokes an immune response. This happens because the immune system sees the antigen as foreign, or ‘non-self” (does not belong in that body).
Aortic stenosis: A condition in which the aortic valve becomes rigid and may calcify over time.
Artery: A blood vessel that transports blood away from the heart.
Arteriole: A very small artery that leads to a capillary.
Arteriogram: An x-ray of arteries.
Arteriosclerosis: The generalized loss of compliance; “hardening of the arteries”.
Atherectomy: Excision of fatty plaque.
Atherosclerosis: A hardening of the arteries that involves the accumulation of fatty plaque.
Brachial artery : The large artery in the upper arm near the biceps muscle.
Capillaries: The smallest type of blood vessel. A capillary connects an arteriole (small artery) to a venule (small vein) to form a network of blood vessels in almost all parts of the body.
Cardiac output: The measurement of blood flow from the heart through the ventricles and is usually measured in liters per minute. Any factor that causes cardiac output to increase, by elevating heart rate or stroke volume or both, will elevate blood pressure and promote blood flow.
Cardiac tamponade: A potentially fatal condition in which excess fluid builds within the pericardial space, preventing the heart from beating effectively.
Cardiogenic: Originating from the heart.
Carotid artery: Located in the neck, it is one of the three major branches of the aortic arch.
Centrifugation: Process of using a rotating machine to generate centrifugal force to separate substances of different densities, remove moisture, or simulate gravitational effects.
Chemoreceptors: Cells that sense changes in chemical levels.
Chemotaxis: Movement in response to chemicals; a phenomenon in which injured or infected cells and nearby leukocytes emit the equivalent of a chemical “911” call, attracting more leukocytes to the site.
Compliance: The ability of the blood vessels to dilate and constrict as needed.
Coronary artery bypass graft (CABG): Surgery in which a healthy blood vessel taken from another part of the body is used to make a new path for blood around a blocked artery leading to the heart. This restores the flow of oxygen and nutrients to the heart.
Coronary heart disease: A disease in which there is a narrowing or blockage of the coronary arteries.
Crohn’s disease: A condition in which the gastrointestinal tract is inflamed over a long period of time.
Diapedesis: The migration of blood cells through the intact walls of blood vessels into the surrounding tissue.
Diastolic pressure: The arterial pressure of blood during ventricular relaxation, or diastole.
Edema: Swelling due to excessive liquid in the tissues.
Embolus: An obstruction such as a blood clot or plaque that blocks the flow of blood in an artery or vein.
Endarterectomy: Excision of plaque from within the artery.
Endothelium: Epithelium that lines vessels in the lymphatic and cardiovascular systems.
Epiphyses: The wider section at the end of long bones.
Erythrocyte: A red blood cell.
Erythropoietin (EPO): A hormone produced by the kidneys that triggers the production of red blood cells.
Extramedullary hematopoiesis: Hematopoiesis outside the medullary cavity of adult bones.
Heart rate: The number of times the heart beats within a certain time period, usually a minute.
Hematocrit: A lab test which measures the percentage red blood cells in a sample of whole blood.
Hematologist: A doctor who has special training in diagnosing and treating blood disorders.
Hematology: The study of blood and blood-forming issues.
Hematoma: A pool of mostly clotted blood that forms in an organ, tissue, or body space.
Hemolysis: The breakdown of red blood cells.
Hemopoiesis: The process by which the body produces blood.
Hemopoietic growth factors: Chemical messengers which promote the proliferation and differentiation of formed elements and include erythropoietin, thrombopoietin, colony-stimulating factors, and interleukins.
Hemorrhage: Excessive bleeding.
Hemostasis: The process by which the body seals a ruptured blood vessel to prevent further blood loss.
Homeostasis: The state of steady internal conditions maintained by living things.
Hypertension: Abnormally high blood pressure.
Hypothermia: Abnormally low body temperature.
Hypothyroidism: The disease state caused by insufficient production of thyroid hormone by the thyroid gland.
Hypovolemic: An abnormally low volume of blood circulating through the body.
Hypoxemia: Below-normal level of oxygen saturation of blood (typically <95 percent).
Hypoxia: Lack of oxygen supply to the tissues.
Immunodeficiency: The decreased ability of the body to fight infections and other diseases.
Intravenous: Into or within the vein.
Ischemia: Lack of blood flow to body tissues.
Leukocyte: White blood cell(s).
Leukocytopenia: An abnormal decrease in the number of leukocytes.
Lupus: A chronic, inflammatory, connective tissue disease that can affect the joints and many organs.
Lymphadenitis: Inflammation of lymph nodes.
Lymphadenopathy: Disease or swelling of the lymph nodes.
Lymphoma: A form of cancer in which masses of malignant T and/or B lymphocytes collect in lymph nodes, the spleen, the liver, and other tissues. These leukocytes do not function properly, and the patient is vulnerable to infection.
Macrophage: A large cell derived from a monocyte; they participate in innate immune responses.
Medulla oblongata: A part of the brain stem responsible for control of heart rate and breathing.
Myeloma: Cancer that arises in plasma cells.
Myelopoiesis: Formation of bone marrow.
Pancytopenia: A condition in which there is a lower-than-normal number of red and white blood cells and platelets in the blood.
Perfusion: Penetration of blood.
Peripheral arterial disease: Obstruction of vessels in peripheral regions of the body.
pH: A measure of how acidic or alkaline a substance is, as determined by the number of free hydrogen ions in the substance.
Phagocytized: The process by which certain cells are able to “eat” other cells or substances by engulfing them.
Phlebitis: Inflammation of a vein.
Phlebotomist: A medical professional trained to draw blood, typically by performing a venipuncture of a surface vein of the arm.
Phlebotomy: A procedure in which a needle is used to take blood from a vein, usually for laboratory testing.
Placenta: The organ that supplies oxygen and nutrients to the fetus, excretes waste products, and produces and secretes estrogens and progesterone.
Plaque: A fatty material including cholesterol, connective tissue, white blood cells, and some smooth muscle cells.
Plasma cells: A type of B lymphocyte that produces antibodies which bind to specific foreign or abnormal antigens, in order to destroy them.
Plasmapheresis: A procedure in which a machine is used to separate the plasma from the blood cells.
Pneumothorax: An abnormal collection of air in the space between the thin layer of tissue that covers the lungs and the chest cavity that can cause all or part of the lung to collapse.
Polycythemia vera: A type of bone marrow disease that causes an excessive production of immature erythrocytes.
Pulmonary embolism: A blood clot within the lung.
Rheumatoid arthritis: An autoimmune disorder in which the body mounts an immune response against its own joint tissues, causing inflammation and damage to the joints.
Sepsis: Organismal-level inflammatory response to a massive infection.
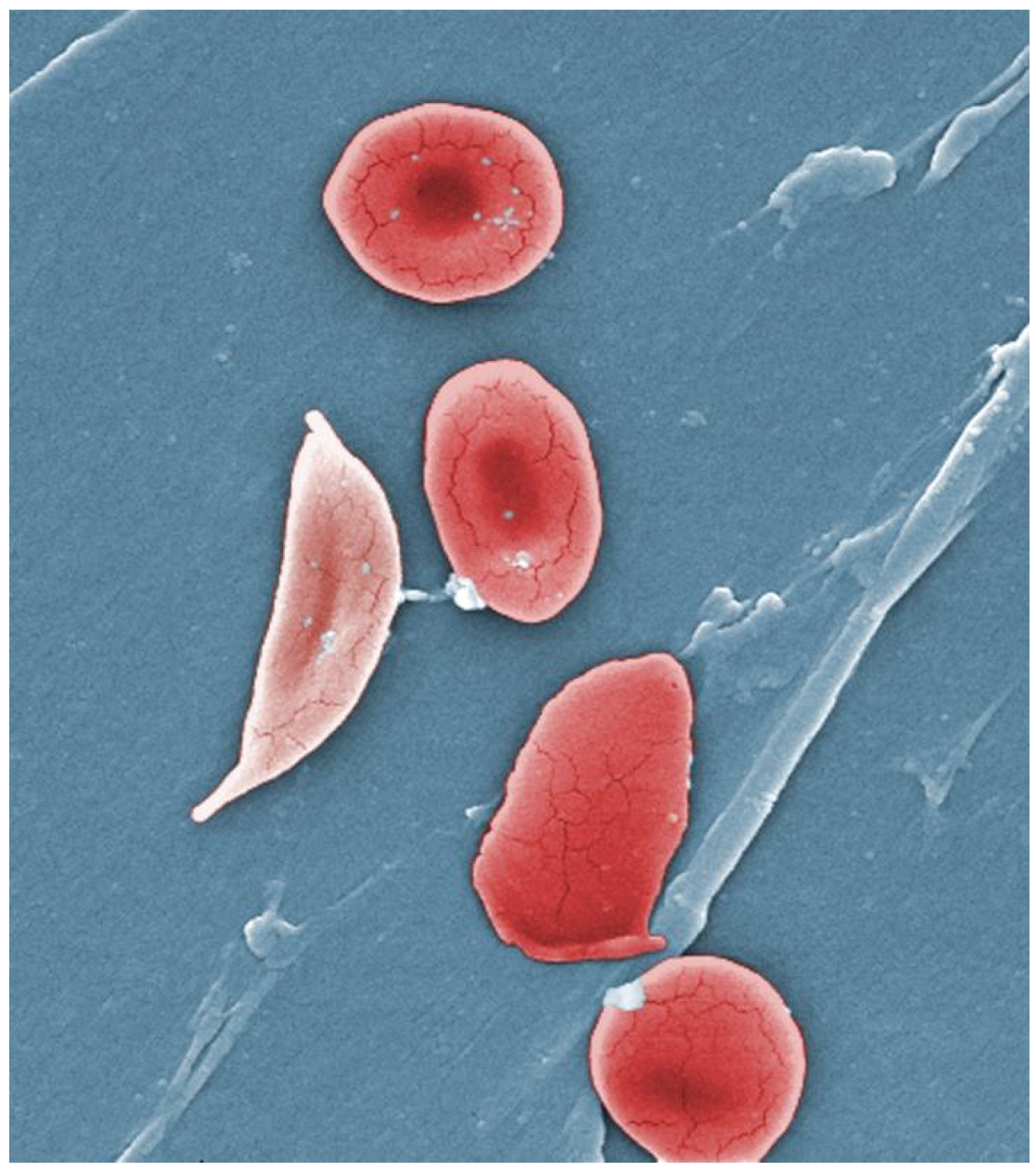
Sickle cell disease: An inherited disease in which the red blood cells have an abnormal crescent shape, block small blood vessels, and do not last as long as normal red blood cells; also called sickle cell anemia.
Splenectomy: Excision of the spleen.
Splenomegaly: Enlarged spleen.
Sphygmomanometer: A blood pressure cuff attached to a measuring device, or gauge.
Systolic pressure: The arterial pressure resulting from the ejection of blood during ventricular contraction, or systole.
Thalassemia: A genetic disorder characterized by abnormal synthesis of globin proteins and excessive destruction of erythrocytes.
Thrombocyte: Platelets.
Thrombocytopenia: A condition in which there is an insufficient number of platelets.
Thrombocytosis: A condition in which there are too many platelets.
Thrombophlebitis: Inflammation of a vein that occurs when a blood clot forms.
Thrombosis: The formation of unwanted blood clots.
Thrombus: Aggregation of fibrin, platelets, and erythrocytes in an intact artery or vein.
Thrombolysis: The process of breaking up a thrombus that is blocking blood flow.
Thymectomy: Excision of the thymus gland.
Thymoma: Tumor of the thymus gland.
Tissue rejection: The recipient’s immune system recognizes the transplanted tissue as non-self and mounts an immune response against it, ultimately destroying it.
Vasoconstriction: The physiological narrowing of blood vessels by contraction of the vascular smooth muscle.
Vasodilation: The physiological widening of blood vessels by relaxing the vascular smooth muscle.
Veins: Blood vessels that carry blood back to the heart.
Venules: Small blood vessels that carry blood to a vein.
Viscosity: A measure of a fluid’s thickness or resistance to flow.
Image Descriptions
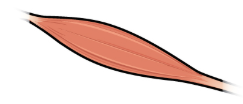
Figure 10.1 image description: The left panel shows the structure of a skeletal muscle vein pump when the muscle is relaxed, and the right panel shows the structure of a skeletal muscle vein pump when the muscle is contracted.[Return to Figure 10.1].
Figure 10.2 image description: The top left panel of this figure shows the ultrastructure of an artery (labels read from top: tunica externa, tunica media, tunica intima, smooth muscle, internal elastic membrane, vasa vasorum, external elastic membrane, nervi vasorum, endothelium, elastic fiber), and the top right panel shows the ultrastructure of a vein (labels read from top: tunica externa, tunica media, tunica intima, vasa vasorum, smooth muscle, endothelium). The bottom panel shows a micrograph with the cross-sections of an artery and a vein. [Return to Figure 10.2].
Figure 10.3 image description: The major arteries in the human body. Labels read (from the top, clockwise) right common carotid, left common carotid, axillary, pulmonary trunk, descending aorta, diaphragm, renal, superior mesenteric, gonadal, inferior mesenteric, common iliac, internal iliac, deep femoral, femoral, descending genicular, dorsalis pedis, plantar arch, fibular, anterior tibial, posterior tibial, popliteal, palmar arches, external iliac, ulnar, radial, brachial, celiac trunk, ascending aorta, aortic arch, brachiocephalic trunk, right subclavian, vertebral. [Return to Figure 10.3].
Figure 10.4 image description: The major veins in the human body. Labels read (from the top, clockwise) internal jugular, brachiocephalic, superior vena cava, intercostal, inferior vena cava, gonadal, lumbar, right and left common iliac, external iliac, internal iliac, deep femoral, femoral, posterior tibial, anterior tibial, dorsal venous arch, plantar venous arch, fibular, small saphenous, popliteal, great saphenous, digital, palmar venous arches, ulnar, median antebrachial, medial cubital, hepatic, basilic, brachial, cephalic, axillary, subclavian, external jugular. [Return to Figure 10.4].
Figure 10.5 image description: This diagram shows how oxygenated and deoxygenated blood flows through the major organs in the body. Pulmonary circulation involves the lungs, pulmonary artery and vein, vena cava, and aorta. Systemic circulation involves the upper body, hepatic vein, renal vein, aorta, liver, hepatic artery, hepatic portal vein, stomach, intestines, renal artery, kidneys, and lower body. [Return to Figure 10.5].
Figure 10.6 image description: The pulse points as shown on a woman’s body. Labels read (from top) temporal artery, facial artery, common carotid artery, brachial artery, radial artery, femoral artery, popliteal artery, posterior tibial artery, dorsalis pedis artery. [Return to Figure 10.6].
Figure 10.7 image description: This figure shows three test tubes with a red and yellow liquid in them. The left panel shows normal blood, the center panel shows anemic blood and the right panel shows polycythemia. Labels indicate plasma (water, proteins, nutrients, hormones et cetera), buffy coat (white blood cells, platelets), and hematocrit (red blood cells). [Return to Figure 10.7].
Figure 10.8 image description: This flowchart shows the pathways in which a multipotent hematopoietic stem cell differentiates into the different cell types found in blood. From the top (multipotent hematopoietic stem cells can divide and some cells remain stem cells, while the remaining cell goes down one of two paths depending on the chemical signals received: myeloid stem cell or lymphoid stem cell. A myeloid stem cell then can become either a megakaryoblast (which then turns into a megakaryocyte, then becomes platelets), or it can become a proerythroblast (which then becomes a reticulocyte, then becoming an erythrocyte), or it can become a myeloblast (which then becomes either a basophil, neutrophil, eosinophil), or it can become a monoblast (which then it becomes a monocyte). If the cell becomes a lymphoid stem cell, it then becomes a lymphoblast, which then becomes either a natural killer cell or a small lymphocyte ( either T or B lymphocyte). [Return to Figure 10.8].
Figure 10.9 image description: This image shows a microscopic view of erythrocytes (red blood cells). Erythrocytes have the appearance of a disc with a shallow center, which aids their function. [Return to Figure 10.9].
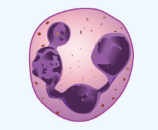
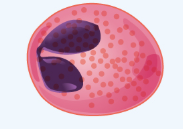
Figure 10.10 image description: This image shows a micrographic view of different leukocytes. From left to right: basophil, eosinophil, neutrophil, monocyte, lymphocyte. [Return to Figure 10.10].
Figure 10.11 image description: This figure shows how leukocytes respond to chemical signals from injured cells. The top panel shows chemical signals sent out by the injured cells (text labels read: 1) Leukocytes in the blood respond to chemical attractants released by pathogens and chemical signals from nearby injured cells). The middle panel shows leukocytes migrating to the injured cells (text labels read: 2)the leukocytes squeeze between the capillary wall as they follow the chemical signals to where they are most concentrated (positive chemotaxis)). The bottom panel shows macrophages phagocytosing the pathogens (text label reads: 3) Within the damaged tissue, monocytes differentiate into macrophages that phagocytize the pathogens. The eosinophils and neutrophils release chemicals that break apart pathogens. They are also capable of phagocytosis.). [Return to Figure 10.11].
Figure 10.12 image description: This figure details the steps in the clotting of blood. Each step is shown along with a detailed text box describing the steps on the left. On the right, a signaling pathway shows the different chemical signals involved in the clotting process. The steps described: 1. Injury: a blood vessel is severed. Blood and blood components (e.g. erythrocytes, white blood cells, et cetera) are leaking out of the breaks. 2. Vascular spasm: the smooth muscle in the vessel wall contracts near the injury point reducing blood loss. 3. Platelet plug formation: platelets are activated by chemicals released from the injury site and by contact with underlying collagen. The platelets become spiked and stick to each other and the wound site. Initial platelets are activated by chemicals released from the injured cells and by contact with broken collagen. Bound platelets release chemicals that activate and attract other platelets. platelets move toward the source of chemical signals and bind. Platelet plug grows in size. 4. Coagulation. In coagulation, fibrinogen is converted to fibrin (see part b), which forms a mesh that traps more platelets and erythrocytes, producing a clot. Part B Fibryn synthesis cascade: Intrinsic pathway (damaged vessel wall), Extrinsic pathway (trauma to extravascular cells), final common pathway (cross-linked fibrin clot). [Return to Figure 10.12].
Figure 10.13 image description: This chart shows the ABO blood group types. From left to right, the columns are blood types A, B, AB, and O. In descending order, the rows are: red blood cell type; antibodies in plasma; antigens in red blood cell; and blood types compatible in an emergency. Blood type A has anti-B antibodies and A antigens and is compatible with blood types A and O. Blood type B has anti-A antibodies and B antigens and is compatible with blood types B and O. Blood type AB has no antibodies, has A and B antigens, and is compatible with all blood types (AB+ is the universal recipient). Blood type O has anti-A and anti-B antibodies, has no antigens, and is compatible with blood type O (O is the universal donor). [Return to Figure 10.13].
Figure 10.15 image description: This figure shows three different red blood cells with different blood types. [Return to Figure 10.15].
Figure 10.14 image description: This figure shows an umbilical artery and vein passing through the placenta on the top left. The top right panel shows the first exposure to Rh+ antibodies in the mother. The bottom right panel shows the response when the second exposure in the form of another fetus takes place. Textboxes detail the steps in each process: First exposure birth of first Rh+ infant: 1. During birth, Rh+ fetal erythrocytes leak into maternal blood after breakage of the embryonic chorion, which normally isolates the fetal and maternal blood. 2) Maternal B cells are activated by the Rh antigen and produce large amounts of anti-Rh antibodies. Second exposure: Rh+ fetus: 3) Rh antibody titer in mother’s blood is elevated after first exposure. 4) Rh antibodies are small enough to cross the embryonic chorion and attach to the fetal erythrocytes. [Return to Figure 10.14].
Figure 10.16 image description: The left panel (a) shows the cross-section of a normal and a narrowed artery. A normal artery has no plaque along the artery walls which means there is normal blood flow. In a narrow artery, plague forms on the arterial walls causing abnormal blood flow. The right panel (b) shows a micrograph of an artery with plaque in it. [Return to Figure 10.16].
Figure 10.17 image description: This photograph shows varicose veins in the lower leg. Varicose veins are distended, twisted veins that may present in patients with edema. [Return to Figure 10.17].
Figure 10.18 image description: This photograph shows the red blood cells of a person suffering from sickle cell anemia. Instead of being discoid shaped like healthy blood cells, sickle red blood cells are shaped like a sickle. [Return to Figure 10.18].