16.5: Urinary Retention
- Page ID
- 52509
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
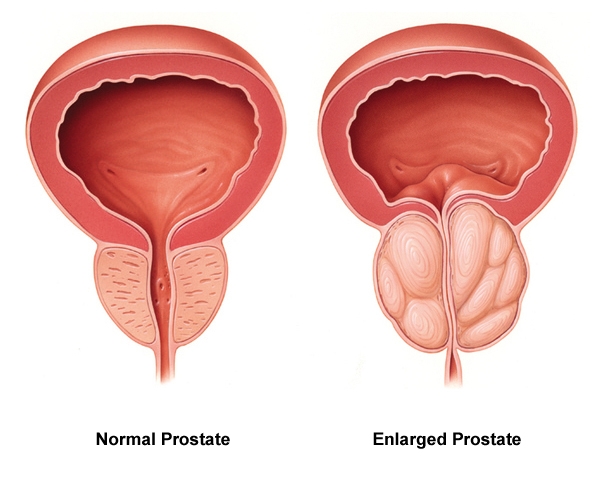
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Urinary retention is a condition when the patient cannot empty all of the urine from their bladder. Urinary retention can be acute (i.e., the sudden inability to urinate after receiving anesthesia during surgery) or chronic (i.e., a gradual inability to completely empty the bladder due to enlargement of the prostate gland in males). Urinary retention is caused by a blockage that partially or fully prevents the flow of urine or the bladder not being able to create a strong enough force to expel all the urine. In addition to causing discomfort, urinary retention increases the patient’s risk for developing a urinary tract infection (UTI). See Figure 16.5[1] for an image of an enlarged prostate gland blocking the flow of urine from the bladder into the urethra.
Symptoms of urinary retention can range from none to severe abdominal pain.[2] Health care providers use a patient’s medical history, physical exam finding, and diagnostic tests to find the cause of urinary retention. Nurses typically receive orders to measure post-void residual amounts when urinary retention is suspected. Post-void residual measurements are taken after a patient has voided by using a bladder scanner or inserting a straight urinary catheter to determine how much urine is left in the bladder. See the following box regarding how to perform a bladder scan at the bedside. Read about other diagnostic tests related to urinary retention, such as urodynamic testing and cystoscopy, under the “Applying the Nursing Process” section of this chapter.[3]
A bladder scanner is a portable, noninvasive medical device that uses sound waves to calculate the amount of urine in a patient’s bladder. Nurses use bladder scanners at the bedside to determine post-void residual urine amounts in patients to avoid the need to perform an invasive urinary catheterization. Typically the use of a bladder scan does not require a physician order, but be sure to check agency policy.
After the patient voids and is lying in a supine position, turn on the device and indicate if the patient is male or female. (If the female has had a hysterectomy, then “male” is selected.) Apply warmed gel to the transducer head, and then place it approximately one inch above the symphysis pubis with the probe directed towards the bladder. Press the “scan” button, making sure to hold the scanner steady until you hear a beep. The bladder scanner will display the volume measured using a display with crosshairs. If the crosshairs are not centered on the urine displayed, adjust the probe and rescan until it is properly centered. If the post-void residual is greater than 300 mL, the provider should be notified and typically an order will be received for a straight urinary catheterization. Whenever possible, indwelling urinary catheterization (also referred to as a “Foley”) placement is avoided to reduce the patient’s risk of developing a catheter-associated urinary tract infection (CAUTI).[4]
View this following YouTube video to see a bladder scanner in use[5]: How to Use BladderScan Prime Plus™ by Diane Newman
Interventions
Treatment for urinary retention depends on the cause. It may include urinary catheterization to drain the bladder, bladder training therapy, medications, or surgery.[6] Read more about bladder training therapy under the “Urinary Incontinence” section. Alpha blockers, such as tamsulosin (Flomax), are used to treat urinary retention caused by an enlarged prostate. A surgery called transurethral resection of the prostate (TURP) may be performed to treat urinary retention caused by an enlarged prostate that is not responsive to medication.
Read more about urinary catheterization and preventing catheter-associated urinary tract infection (CAUTI) in “Facilitation of Elimination” in Open RN Nursing Skills.
Read more about alpha-blocker medication (i.e., tamsulosin) in the “Autonomic Nervous System” chapter in Open RN Nursing Pharmacology.
- “Normal-vs-enlarged-prostate.jpg” by Akcmdu9 is licensed under CC BY-SA 3.0↵
- National Institute of Diabetes and Digestive and Kidney Diseases. (n.d.). Urinary retention. U.S. Department of Health and Human Services. https://www.niddk.nih.gov/health-information/urologic-diseases/urinary-retention↵
- National Institute of Diabetes and Digestive and Kidney Diseases. (n.d.). Urinary retention. U.S. Department of Health and Human Services. https://www.niddk.nih.gov/health-information/urologic-diseases/urinary-retention↵
- Agency for Healthcare Research and Quality. (2020, October). Toolkit for reducing catheter-associated urinary tract infections in hospital units: Implementation guide - Appendix C. Sample bladder scan policy. https://www.ahrq.gov/hai/cauti-tools/impl-guide/implementation-guide-appendix-c.html↵
- BladderScanDevice. (2017, Novemeber 13). How to use BladderScan Prime PlusTM by Diane Newman. [Video]. YouTube. All rights reserved. https://youtu.be/Q-sQu0T2oUY. ↵
- National Institute of Diabetes and Digestive and Kidney Diseases. (n.d.). Urinary retention. U.S. Department of Health and Human Services. https://www.niddk.nih.gov/health-information/urologic-diseases/urinary-retention↵


