9.5: Erythrocytes — Tiny Oxygen Taxis
- Page ID
- 140823
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Red blood cells are the most numerous formed elements in blood and play a vital role in gas transport and oxygen regulation.
- Describe the structure and function of erythrocytes.
- Discuss the various steps in the lifecycle of an erythrocyte
- Explain how hemoglobin transports oxygen and carbon dioxide.
- Outline how erythropoietin regulates red blood cell production
Red Blood Cells
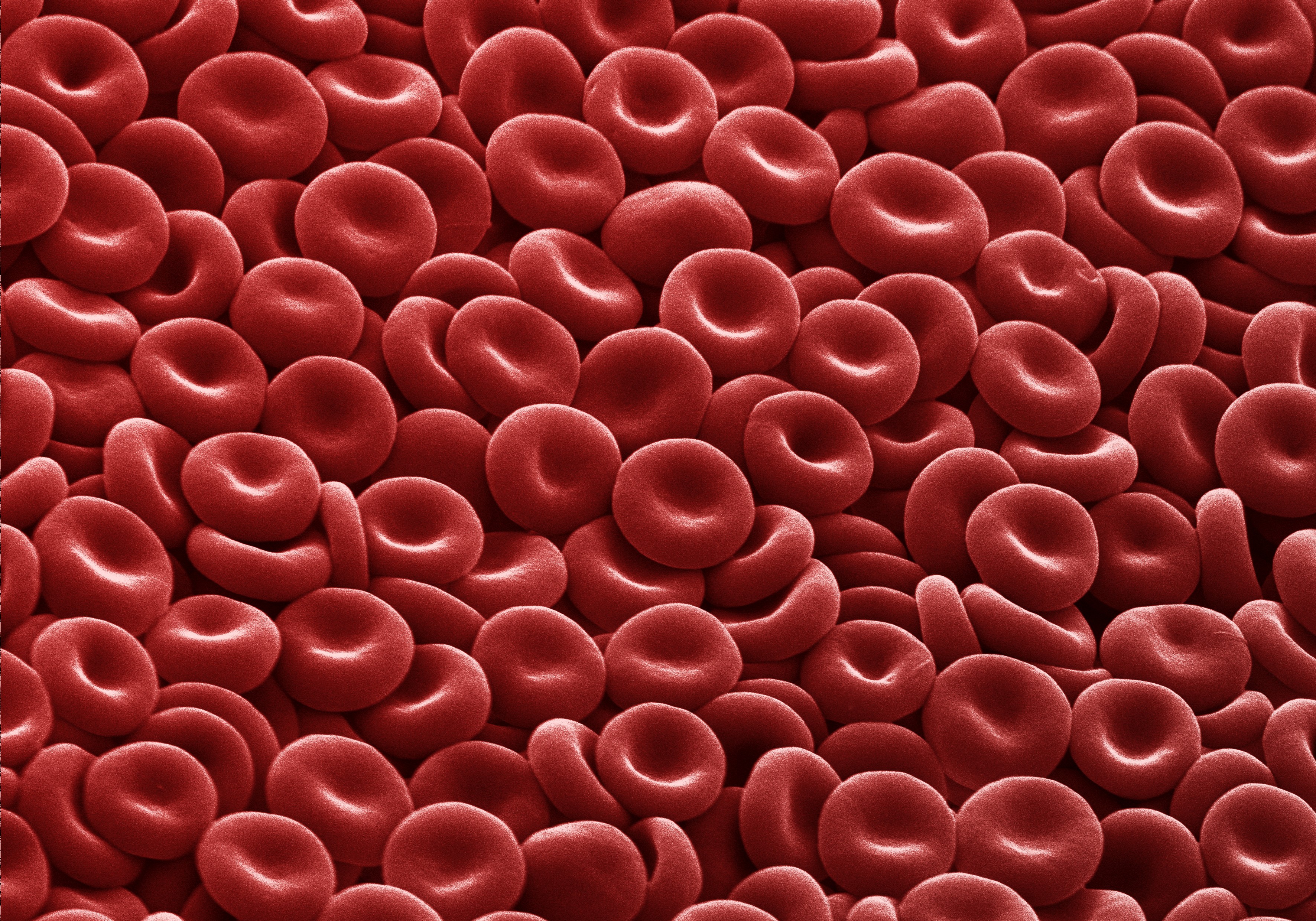
The erythrocyte, commonly known as a red blood cell (or RBC), is by far the most common formed element. A single drop of blood contains millions of erythrocytes and just thousands of leukocytes. Males typically have about 5.4 million red blood cells per microliter (µL) of blood, and females about 4.8 million per µL. In fact, erythrocytes are estimated to make up about 25 percent of the total cells in the body. Erythrocytes are also smaller than leukocytes and most other body cells — only about 7–8 micrometers (µm) wide, much smaller than most white blood cells.
The main job of red blood cells is to carry oxygen and carbon dioxide, since these molecules cannot be efficiently transported dissolved in plasma. RBCs pick up oxygen in the lungs and deliver it to tissues throughout the body, then carry part of the carbon dioxide waste back to the lungs to be exhaled.
Unlike white blood cells, which leave the bloodstream to fight infection, RBCs stay within the vessels — if they escape, something is wrong.
Red blood cells are made in the red bone marrow at an incredible rate — more than 2 million cells per second. Their production depends on nutrients such as glucose, amino acids, and lipids, as well as trace elements like iron, copper, zinc, folate, and vitamin B₁₂. Each red blood cell circulates for about 120 days before being broken down by macrophages in the bone marrow, liver, and spleen. The useful parts, including iron and amino acids, are recycled to make new cells.

As red blood cells (erythrocytes) develop and mature in the red bone marrow, they gradually extrude (push out) most of their internal structures (organelles) and aslo the nucleus. In their final stage before full maturity, they are called reticulocytes. These young cells still contain a few bits of cellular machinery that finish making hemoglobin, the protein that carries oxygen. Within a day or two in the bloodstream, reticulocytes lose their remaining organelles and become mature erythrocytes — essentially flexible sacs packed with about 300 million hemoglobin molecules. Because they have no mitochondria, they rely on anaerobic respiration, so they do not use any of the oxygen they carry, leaving all of it available for delivery to tissues. Normally, reticulocytes make up about 1–2% of the circulating red blood cells, and their numbers give doctors a rough idea of how quickly new red blood cells are being made. Too few may mean underproduction, while too many may signal overproduction.
Mature erythrocytes have a distinctive biconcave disc shape — thicker around the edges and thinner in the center. This shape increases their surface area for gas exchange and, since they got rid of their nucleus and most of their organelles, there is more room inside for hemoglobin, the oxygen carrier protein. As they travel through the narrow capillaries, oxygen diffuses out of the red blood cells into body tissues, while carbon dioxide moves in to be carried away. The smallest capillaries are so narrow that erythrocytes must bend or fold to pass through, but flexible structural proteins like spectrin allow them to stretch and spring back into shape. In wider vessels, they often stack together like a roll of coins, a formation called a rouleaux (from the French word for “roll”).
Hemoglobin
Hemoglobin is a large, iron-containing protein that gives red blood cells their color and oxygen-carrying ability. Each hemoglobin molecule is made up of four folded chains of a protein called globin—two alpha chains and two beta chains. Each globin chain is bound to a red pigment molecule called heme, which contains an iron ion (Fe²⁺) at its center (see Figure below). Each iron ion can bind to one oxygen molecule, so one hemoglobin molecule can carry up to four oxygen molecules. Because a single erythrocyte contains about 300 million hemoglobin molecules, each red blood cell can transport roughly 1.2 billion oxygen molecules through the bloodstream.

Hemoglobin and Oxygen Transport
In the lungs, hemoglobin binds oxygen molecules to the iron ions within its heme groups, forming oxyhemoglobin. This bright red, oxygen-rich form of hemoglobin circulates through the bloodstream to deliver oxygen to body tissues. As it releases oxygen to the tissues, hemoglobin becomes darker red deoxyhemoglobin, sometimes called reduced hemoglobin. Oxygen release depends on the oxygen demand of the surrounding tissues, so hemoglobin almost never unloads all of its oxygen.

Carbon Dioxide Transport
When blood reaches the capillaries, carbon dioxide from the tissues enters the bloodstream. About 76% of this carbon dioxide dissolves in the plasma — some remaining as dissolved CO₂ and the rest is converted into bicarbonate ions (HCO₃⁻). Another 23–24% binds to the amino acids of hemoglobin to form carbaminohemoglobin. Hemoglobin then transports this carbon dioxide back to the lungs, where it is released in exchange for fresh oxygen.
 Measuring Oxygen Saturation
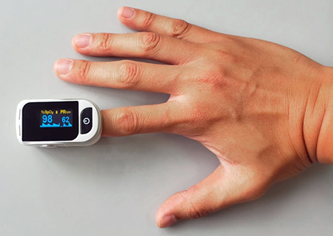
Measuring Oxygen Saturation
In healthcare, a key measure of tissue oxygenation is percent saturation, which reflects the percentage of hemoglobin binding sites occupied by oxygen. It is commonly measured using a pulse oximeter (see image on the right), a device clipped onto a thin part of the body — usually the fingertip. The oximeter sends red and infrared light through the tissue and measures how much light is absorbed. Because oxygenated and deoxygenated hemoglobin absorb light differently, the device can calculate the percentage of oxygen saturation.
Normal readings range from 95 to 100%. Lower values indicate hypoxemia, meaning low blood oxygen. The broader term hypoxia refers to generally low oxygen levels within tissues.
Erythropoietin and the Feedback Loop
The total blood volume circulating in your body is about 5 liters (a little over 10 pints). At any given moment, your kidneys receive about 20% of your resting cardiac output, meaning about one-fifth of all the blood that the heart pumps with each beat goes to the kidneys to be filtered. Over the course of a whole day, that adds up to a huge total volume: the kidneys filter about 180 liters (around 380 pints) of blood per day!
Therefore, the kidneys are well-positioned to monitor oxygen levels. When oxygen saturation falls (hypoxemia) the kidneys sense it and in response, interstitial fibroblasts in the kidney release the hormone erythropoietin (EPO), which stimulates red blood cell production in the bone marrow.
As oxygen levels rise again, EPO secretion declines — a classic negative-feedback loop that maintains oxygen homeostasis.


