10.16: Capillary Exchange
- Page ID
- 100152
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Capillary exchange is the process by which gases, nutrients, wastes, and fluids move between the bloodstream and tissues, using specialized mechanisms that keep every cell supplied.
- Identify and briefly explain the three mechanisms of capillary exchange: diffusion, transcytosis, and bulk flow.
- Explain how hydrostatic and osmotic pressures determine whether bulk flow leads to filtration or reabsorption.
- Describe the role of the lymphatic system in returning excess fluid to the bloodstream and how its failure leads to edema.
Capillaries are the smallest blood vessels in the body and the sites where all exchange between the bloodstream and tissues occurs. Most capillaries are less than 1 millimeter long and so narrow that red blood cells must pass through in single file and may even need to bend as they move along. Because capillaries weave densely among body cells, no cell is ever far from its supply line.
How Materials Move Across Capillary Walls
A main job of the cardiovascular system is to deliver gases, nutrients, and other substances to the body’s cells and carry away wastes. Capillary exchange is the term for the movement of substances between the blood and tissues. Three mechanisms support this exchange: diffusion, transcytosis, and bulk flow.
Diffusion is the most common mechanism of capillary exchange. Small, lipid-soluble molecules such as oxygen, carbon dioxide, and lipids diffuse directly through the endothelial cell membranes. Water-soluble small substances — like glucose, amino acids, and ions (sodium, potassium, calcium, chloride) — use specific channel proteins to cross by facilitated diffusion. (Module 2, pages 2.10–2.11). Some of these molecules can also move through the small spaces between endothelial cells called intercellular clefts. Fenestrated capillaries contain pores that allow medium-sized molecules to pass, and sinusoid capillaries have large gaps that permit even plasma proteins to move through.
Some large proteins and other macromolecules travel across the endothelial cells by transcytosis. In this process, they are packaged into vesicles on one side of the cell (endocytosis), transported across the interior, and released on the opposite side (exocytosis).
Finally, water and many dissolved substances move together across the capillary wall by bulk flow, a pressure-driven process. Bulk flow is especially important for regulating the distribution of fluids between the blood and interstitial spaces. Water follows its own concentration gradient by osmosis or is pushed and pulled across the wall by hydrostatic and osmotic pressures.
 1) Diffusion
1) Diffusion
Capillaries are designed for efficient exchange. Each capillary has a very thin wall made of a single layer of endothelial cells resting on a delicate basement membrane (see image on the right). Because this barrier is so thin, small molecules can move easily across it by simple or facilitated diffusion. Diffusion always moves substances from areas of higher concentration to lower concentration. As a result, materials that are more concentrated in the blood (such as oxygen and glucose) diffuse outward into the tissues, while substances produced by nearby cells (such as carbon dioxide and other wastes) diffuse into the blood.
Diffusion is the primary mechanism of capillary exchange and accounts for the movement of most small molecules between blood and tissues. The direction and rate of this movement depend on the concentration gradients between the blood and interstitial fluid.
2) Transcytosis
 Transcytosis, or vesicular transport, is the second mechanism that facilitates capillary exchange, along with diffusion and bulk flow.
Transcytosis, or vesicular transport, is the second mechanism that facilitates capillary exchange, along with diffusion and bulk flow.
Some large, water-insoluble molecules cannot use other transport methods, so they must move through the endothelial cells inside vesicles. Often, these molecules first attach to specific receptors on the endothelial cell surface, which triggers receptor-mediated endocytosis: the cell forms a small vesicle around the molecule and brings it inside. The vesicle then travels across the cell and releases the molecule on the opposite side. This allows important macromolecules to move from the blood into the tissues, or vice versa, even though they are too large to pass through pores or channels. Vesicles can merge with others, mix their contents, or be directed toward specific tissues as needed.
Although transcytosis is a normal and useful way for large molecules to cross a capillary wall, it can unfortunately also be used by harmful microbes. Some pathogens “hijack’’ this vesicle-transport system to move through epithelial barriers that would normally protect the body. Examples are:
- Cronobacter sakazakii is a bacterium that can contaminate powdered infant formula and cause severe infections in newborns, including sepsis and meningitis. It is dangerous because it can cross the intestinal wall and even the blood-brain barrier.
- Listeria monocytogenes is a bacterium found in foods like soft cheeses and deli meats. It can cause listeriosis, an illness that is especially serious for pregnant individuals, newborns, older adults, and immunocompromised people. Listeria is unusual because it can cross several body barriers, including the intestinal lining and the placenta.
Pharmaceutical researchers are exploring how to use transcytosis to carry medicines across the blood-brain barrier. Because this barrier blocks most drugs from entering the brain, using the body’s own transport system may help deliver treatments — especially large molecules like antibodies — to the brain more effectively.
3) Bulk Flow: Filtration and Reabsorption
Bulk flow is the pressure-driven movement of water and the small, lipid-insoluble solutes carried with it across the capillary wall. How much bulk flow occurs depends on the type of capillary and how porous it is. Continuous capillaries have very tight walls and allow only limited bulk flow. Fenestrated capillaries contain small pores that permit more flow. Discontinuous (sinusoid) capillaries have large gaps and allow the greatest amount of bulk flow.

Figure \(\PageIndex{1}\): Three Structural Types of Capillaries.
This figure compares the three main capillary types found in the human body. Continuous capillaries (left) have a solid endothelial lining with small intercellular clefts and an intact basement membrane, allowing only small molecules like gases and nutrients to pass through. Fenestrated capillaries (middle) contain pores called fenestrations that increase permeability, making them ideal for organs that require rapid exchange such as the kidneys, intestines, and endocrine glands. Sinusoidal capillaries (right) have large intercellular gaps and an incomplete basement membrane, creating wide openings that let whole cells and large proteins move through, as seen in the liver, spleen, and bone marrow.
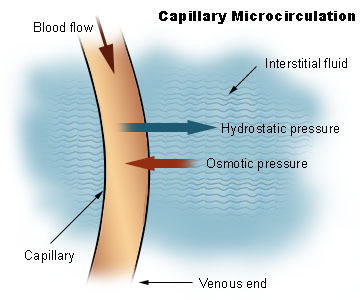
Bulk flow depends on two opposing pressures:
- Hydrostatic pressure. This is essentially the blood pressure, the “pushing” force created by the fluid inside the capillary. This pressure tends to push water and small solutes out into the surrounding tissues.
- Osmotic (also called oncotic) pressure. This pressure is the “pulling” force created mostly by plasma proteins that cannot leave the the capillaries and attract water back toward the bloodstream.
Bulk flow can therefore move fluid out of the bloodstream into the tissues or from the tissues back into the bloodstream, depending on which pressure is stronger.
When fluid moves out of the capillary and into the surrounding tissue, the process is called filtration. This happens when the fluid pressure inside the capillary is higher than the pressure in the surrounding tissue.
When fluid moves from the tissue back into the capillary, the process is called reabsorption. This happens when the “pulling” force of proteins in the blood is stronger than the pressure in the tissues.

The image above reflects the classical teaching of filtration and reabsorption. Newer research shows that capillaries do not reabsorb as much fluid at their venous end as older diagrams suggested. Instead, many capillaries tend to push fluid outward along most of their length, and the extra fluid is carried back to the bloodstream by the lymphatic system. Reabsorption does still happen, but mainly in special situations, such as after blood loss, or in certain organs like parts of the intestine and kidney.
In summary, bulk flow depends on two types of pressure:
-
Hydrostatic pressure, which pushes fluid outward.
-
Osmotic pressure, which pulls fluid inward.
The balance between these pressures determines whether filtration or reabsorption occurs.
Watch this great video about Capillaries and Capillary Exchange by ThePenguinProf
Lymphatic System
Capillary beds do not work alone! To help manage the fluid that leaves the capillaries, the body relies on a second circulation system, the lymphatic system.
Lymph vessels are thin, low-pressure tubes that run alongside blood capillaries and act as a drainage system for the body. In most capillary beds, more fluid is pushed out of the blood than is pulled back in, so a small amount of excess fluid collects in the surrounding tissues. Instead of letting this extra fluid build up and cause swelling, lymph vessels pick it up and return it to the bloodstream through a network of vessels and nodes. In other words, lymph vessels help keep capillary beds in balance by preventing fluid from accumulating in the tissues and by maintaining normal blood volume.

Figure \(\PageIndex{4}\): Overview of Blood and Lymph Circulation. Lymphatic capillaries are found wherever blood capillaries are located except in the central nervous system and bone marrow. Some fluid that left the blood capillaries enters nearby lymphatic capillaries (green), becoming lymph. Lymph flows through lymphatic vessels and lymph nodes, where it is filtered, before rejoining the bloodstream at the subclavian veins.

Figure \(\PageIndex{5}\): Relationship of blood and lymph. Lymphatic capillaries sit near blood capillaries and pick up the excess fluid that filters out of the bloodstream. These tiny vessels merge into larger lymphatic vessels, which resemble small veins and contain one-way valves to keep lymph moving forward. As nearby skeletal muscles contract, they squeeze the vessels and help push lymph along its one-way path toward the chest. Eventually, all lymph drains into either the subclavian or jugular veins.
When the lymphatic system is damaged or blocked by surgery, injury, infection, or genetic conditions, lymph fluid cannot drain efficiently. As fluid builds up in the tissue spaces, swelling develops, a condition known as lymphedema.

Vein problems can create a similar issue. Conditions such as chronic venous insufficiency, varicose veins, or deep vein thrombosis increase pressure inside the veins and push extra fluid out into the surrounding tissues. When this excess fluid exceeds the lymphatic system’s ability to remove it, edema forms.
video to explore the lymphatic system.


