3.3: Digestion and Absorption
- Page ID
- 20951
Learning Objectives
- Identify the major organs of the digestive system.
- Describe the processes of digestion, absorption, and elimination by listing the role(s) of each organ of the digestive system.
Digestion begins even before you put food into your mouth. When you feel hungry, your body sends a message to your brain that it is time to eat. Sights and smells influence your body’s preparedness for food. Smelling food sends a message to your brain. Your brain then tells the mouth to get ready, and you start to salivate in preparation for a delicious meal.
Digestion and Absorption Overview
The food we eat undergoes three processes:
- Digestion: the process by which foods are broken down into molecules
- Absorption: the process of taking the products of digestion (molecules) across the gastrointestinal (GI) tract walls and into circulation
- Elimination: the process by which undigested food and waste products are removed from the body
These processes occur in the gastrointestinal tract.
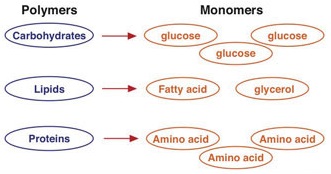
Once you have eaten, your digestive system breaks down the food into smaller components. The food we eat is made up of carbohydrates, lipids (fats), and protein (listed as 'polymers' in Figure \(\PageIndex{1}\)). The entire process of digestion converts the large polymers in food to smaller components (monomers) that can be absorbed. Carbohydrates are broken down to monosaccharides (e.g., glucose), lipids are broken down to fatty acids, and proteins are broken down to amino acids. Another word for the breakdown of complex molecules into smaller, simpler molecules is "catabolism" or a "catabolic reaction". To do this, catabolism functions on two levels, mechanical and chemical. Once the smaller particles have been broken down, they will be absorbed into the blood and delivered to cells throughout the body for energy or for building blocks needed for cells to function. The digestive system is one of the eleven organ systems of the human body and it is composed of several hollow tube-shaped organs including the mouth, esophagus, stomach, small intestine, and large intestine (or colon). It is lined with mucosal tissue that secretes digestive juices (which aid in the breakdown of food) and mucus (which facilitates the propulsion of food through the tract). Smooth muscle tissue surrounds the digestive tract and its contraction produces waves, known as peristalsis, that propel food down the tract. Nutrients as well as some non-nutrients are absorbed. Substances such as fiber get left behind and are appropriately excreted.
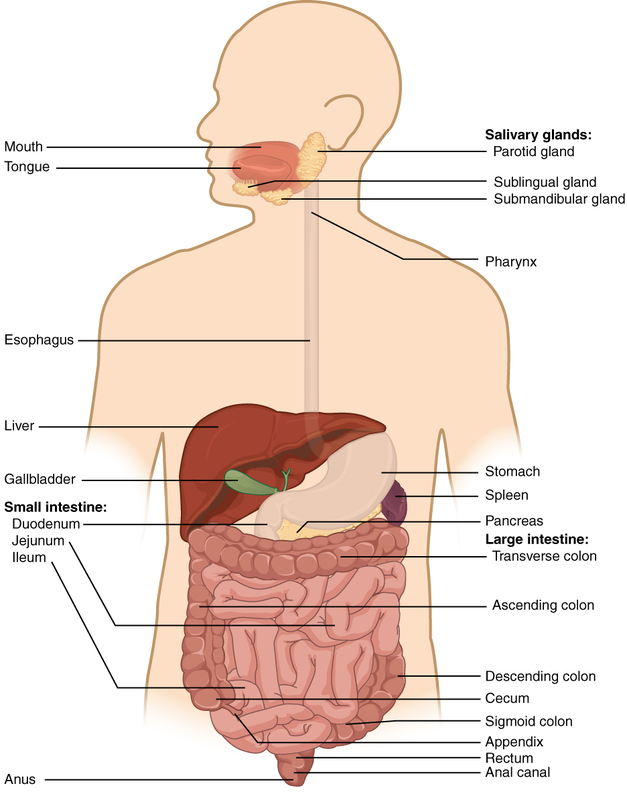
Mouth and Esophagus
There are multiple steps in the digestion process (Figure \(\PageIndex{2}\)). The first step is ingestion, which is the collection of food into the digestive tract. It may seem a simple process, but ingestion involves smelling food, thinking about food, and the involuntary release of saliva in the mouth to prepare for food entry. This first step/phase is called the cephalic phase and helps prepare the GI tract to digest food. The second step of digestion, mechanical and chemical breakdown of food, also begins in the mouth. The chemical breakdown of food in the mouth involves enzymes secreted by the salivary glands. These enzymes start to break apart the components in food. Enzymes are proteins that speed up chemical reactions; one of the enzymes in saliva, amylase, begins the process of carbohydrate digestion. Enzyme names typically end in "-ase" (e.g., amylase, lactase). Mechanical breakdown starts with mastication (chewing) in the mouth. Teeth crush and grind large food particles, while saliva moistens the food, begins the chemical breakdown of food and enables its movement downward.
The slippery mass of partially broken-down food is called bolus, which moves down the digestive tract as you swallow. Swallowing may seem voluntary at first because it requires conscious effort to push the food with the tongue back toward the throat, but after this, swallowing proceeds involuntarily, meaning it cannot be stopped once it begins.
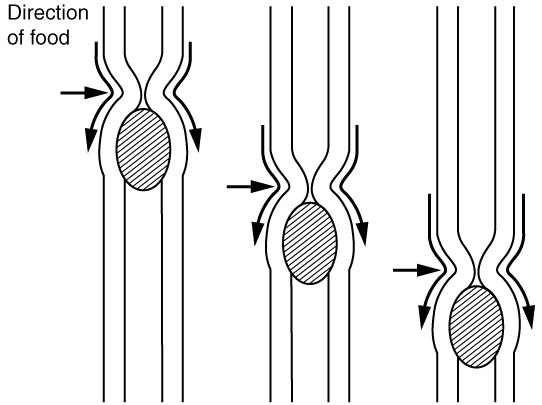
As you swallow, the bolus is pushed from the mouth through the pharynx and into a muscular tube called the esophagus. As it travels through the pharynx, a small flap called the epiglottis closes, to prevent choking by keeping food from going into the trachea. Peristalsis (the rhythmic contraction and relaxation of circular and longitudinal muscles that move food in one direction through the GI tract) in the esophagus propels the food down to the stomach. This movement of food via peristalsis is shown in Figure \(\PageIndex{3}\). At the junction between the esophagus and stomach there is a sphincter muscle that remains closed until the food bolus approaches. The pressure of the food bolus stimulates the lower esophageal sphincter to relax and open and food then moves from the esophagus into the stomach. Solid food takes four to eight seconds to travel down the esophagus, and liquids take about one second.
Stomach
The stomach has three basic tasks - to store food, mechanically and chemically break down food, and empty partially broken-down food into the small intestine.
When food enters the stomach, a highly muscular organ, powerful peristaltic contractions help mash, pulverize, and churn food into a semiliquid mass of partially digested food and gastric juices called chyme which is then periodically released into the small intestine through the pyloric sphincter. A digestive fluid in the stomach, called gastric juice, contains several important compounds:
- Hydrochloric acid (HCl) - keeps the stomach interior acidic which:
- protects the body from harmful bacteria
- denatures protein to allow protein to be digested further
- activates pepsin
- Pepsin - an enzyme that begins to digest protein
- Gastric lipase - an enzyme that starts to digest fat
Mucus protects the stomach lining from the acidic gastric juice.
The length of time that food spends in the stomach varies by the macronutrient composition of the meal. A high-fat or high-protein meal takes longer to break down than one high in carbohydrates. It usually takes a few hours after a meal to empty the stomach contents completely.
Small Intestine
Most digestion and absorption occurs in the small intestine.
The small intestine is divided into three structural parts: the duodenum (the first part), the jejunum (the middle), and the ileum (the last part). Once the chyme enters the duodenum, three accessory (or helper) organs - the pancreas, gallbladder, and liver - are stimulated to release juices that aid in digestion. The pancreas secretes pancreatic juice through a duct into the duodenum. Pancreatic juice consists mostly of water, but also contains bicarbonate ions (that neutralize the acidity of chyme) and enzymes that further breakdown proteins, carbohydrates, and lipids (proteases digest proteins, pancreatic amylase digests carbohydrates, pancreatic lipase digests lipids/fats). The gallbladder secretes bile through a different duct that also leads to the duodenum. Bile is made in the liver and stored in the gallbladder. Bile helps digest lipids/fats; bile’s components act like detergents by surrounding fats similar to the way dish soap removes grease from a frying pan. This allows for the movement of fats in the watery environment of the small intestine. Two different types of muscular contractions, called peristalsis and segmentation, move and mix the food in various stages of digestion through the small intestine. Similar to what occurs in the esophagus and stomach, peristalsis is circular waves of smooth muscle contraction that propel food forward. Segmentation sloshes food back and forth in both directions promoting further mixing of the chyme. Almost all the components of food are completely broken down to their simplest unit within the first 25 centimeters of the small intestine. Instead of proteins, carbohydrates, and lipids, the chyme now consists of amino acids, monosaccharides, and emulsified fatty acids.
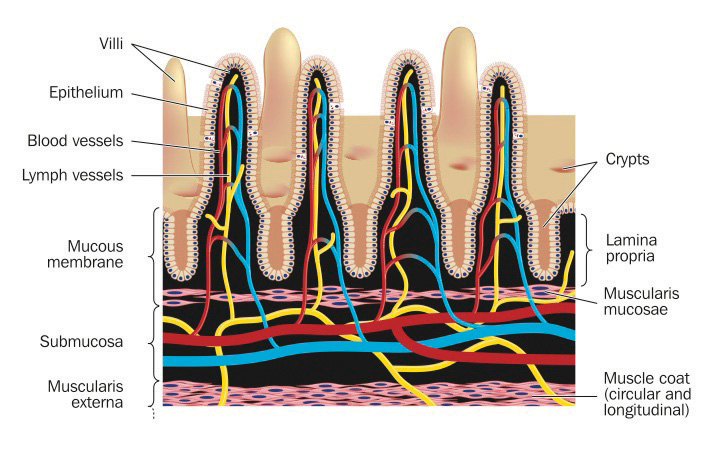
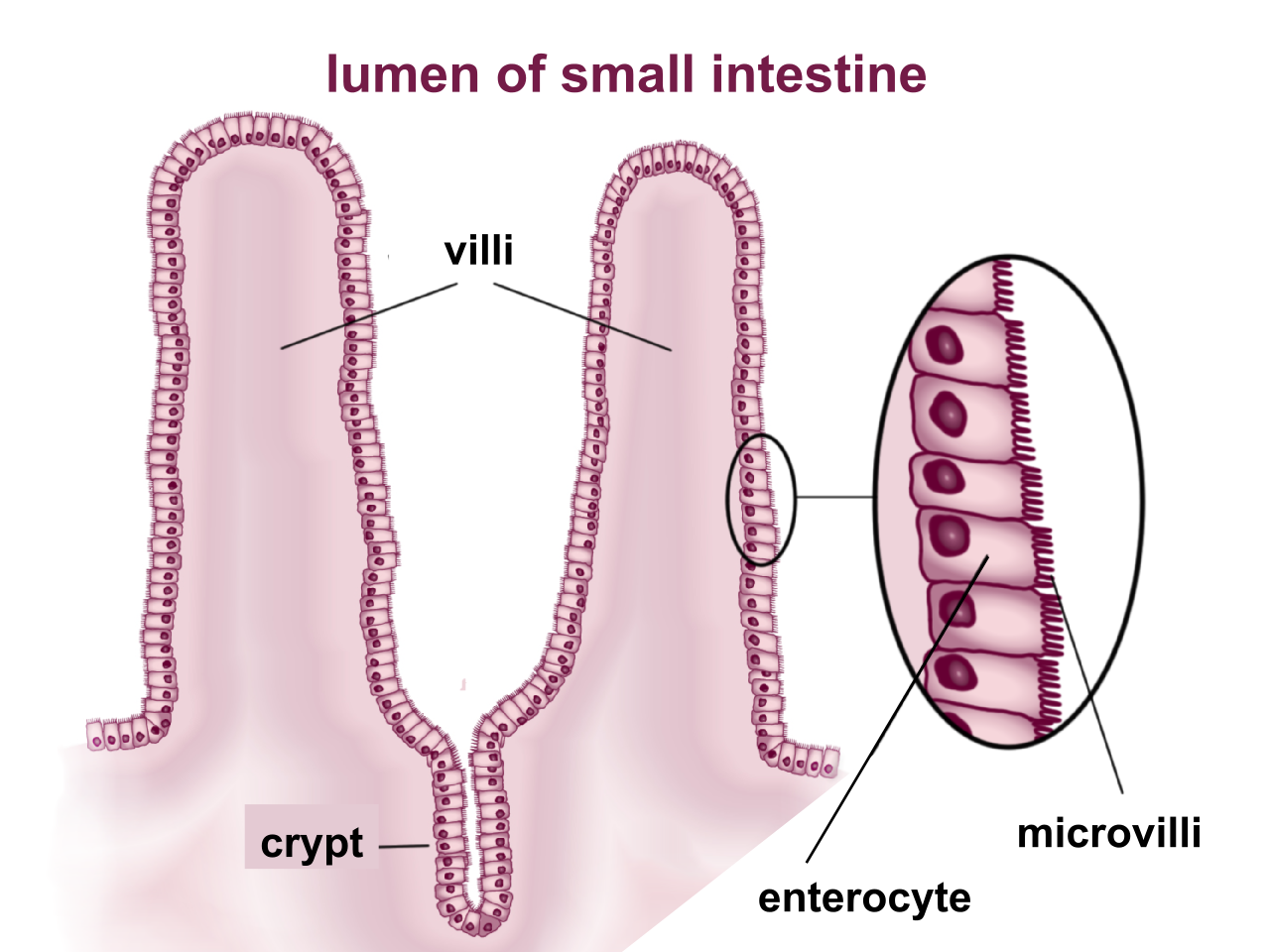
The third step of digestion (nutrient absorption) takes place in the remaining length of the small intestine, or ileum (> 5 meters). The small intestine is perfectly structured for maximizing nutrient absorption. Its surface area is greater than 200 square meters, which is about the size of a tennis court. The surface area of the small intestine increases by multiple levels of folding (see Figure \(\PageIndex{4}\)). The internal tissue of the small intestine is covered in villi, which are tiny finger-like projections that are covered with even smaller hair-like projections, called microvilli or the "brush border" (see Figure \(\PageIndex{5}\)). The digested nutrients pass through the absorptive cells of the intestine via diffusion or special transport proteins. Nutrients that are water-soluble like amino acids and monosaccharides (sugars) are transported from the intestinal cells into capillaries (blood), but the fat-soluble nutrients like fatty acids, fat-soluble vitamins, and other lipids are transported first through lymphatic vessels (lymph), which soon meet up with blood vessels.
Large Intestine
The process of digestion is fairly efficient. Any food that is still incompletely broken down (usually less than ten percent of food consumed) and the food’s indigestible fiber content moves from the small intestine to the large intestine (colon) through a connecting valve. The main task of the large intestine is to reabsorb water. Remember, water is present not only in solid foods, but also in the gastric juice released by the stomach as well as the secretions from the pancreas. For the body to conserve water, it is important that the water be reabsorbed. In the large intestine, no further chemical or mechanical breakdown of food takes place, unless it is accomplished by the bacteria that inhabit this portion of the digestive tract.
After a few hours in the stomach, plus three to six hours in the small intestine, and about sixteen hours in the large intestine, the digestion process enters step four, which is the elimination of indigestible food as feces. Feces contain indigestible food and gut bacteria (almost 50 percent of content). It is stored in the rectum until it is expelled through the anus via defecation.
Summary
The digestive system uses mechanical and chemical activities to break food down into absorbable substances during its journey through the digestive system. Table \(\PageIndex{1}\) provides a summary of the major functions of the digestive tract that you learned about above.
| Organ | Major Functions |
|---|---|
| Mouth |
|
| Esophagus |
|
| Stomach |
|
| Small intestine |
|
| Accessory organs |
|
| Large intestine |
|
Key Takeaways
- The role of the digestive system is to breakdown the complex macromolecules (carbohydrates, fats, and proteins) from food into simple absorbable components (glucose, fatty acids, and amino acids) to be processed into energy or used as building blocks by different cells throughout the body.
- The major organs of the digestive system include the mouth, esophagus, stomach, small intestine, and large intestine (or colon).
- There are four steps in the digestion process: ingestion, the mechanical and chemical breakdown of food, nutrient absorption, and elimination of indigestible food.
- The mechanical breakdown of food occurs via muscular contractions called peristalsis and segmentation. Enzymes secreted by the salivary glands, stomach, pancreas, and small intestine accomplish the chemical breakdown of food. Additionally, bile emulsifies fats.

