30.3A: Development of the Skeleton
- Page ID
- 8418
Early in gestation, a fetus has a cartilaginous skeleton that becomes bone in the gradual process of endochondral ossification.
- Compare and contrast osteogenesis by intramembranous and endochondral ossification
Key Points
- At birth, a newborn baby has over 300 bones, while on average an adult human has 206 bones.
- Ossification or osteogenesis is the process of generating new bone material by precursor cells called osteoblasts.
- Two processes result in the formation of normal, healthy bone tissue: intramembranous ossification and endochondral ossification.
- Intramembranous ossification is the direct laying of bone into the primitive connective tissue (mesenchyme). The membrane that occupies the place of the future bone resembles connective tissue and ultimately forms the periosteum. It is composed of fibers and granular cells in a matrix.
- Endochondral ossification involves cartilage which is then mineralized.
- Bones are dynamic structures that respond to applied force over time. With chronic weight bearing and the forces from daily use and movement, bone mass can be maintained or increased.
Key Terms
- intramembranous ossification: Production of bone tissue during fetal development without a cartilage template. The membrane that occupies the place of the future bone resembles connective tissue and ultimately forms the periosteum, or outer bone layer.
- trabecula: A small, mineralized spicule that forms a network in spongy bone.
- mesenchyme: Undifferentiated cells of the early embryo that develop into the tissues of the lymphatic and circulatory systems, as well as connective tissues throughout the body such as bone and cartilage.
- endochondral ossification: The process by which bone tissue is created using a cartilage template during fetal development.
Early in gestation, a fetus has a cartilaginous skeleton from which the long bones and most other bones gradually form throughout development and for years after birth in a process called endochondral ossification. Ossification or osteogenesis is the process of laying new bone material by cells called osteoblasts. Two processes result in the formation of normal, healthy bone tissue. Intramembranous ossification is the direct laying of bone into the primitive connective tissue (mesenchyme). This is how the flat bones of the skull and the clavicles are formed. Endochondral ossification involves cartilage as a precursor. Ossification of the mandible occurs in the fibrous membrane covering the outer surfaces of Meckel’s cartilages.
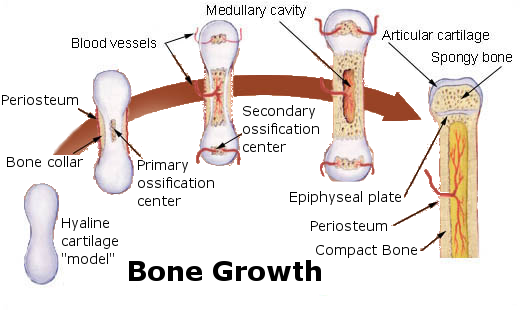
Endochondral Ossification: The development of the primary and secondary ossification centers
Intramembranous Ossification
In bones developed in membrane, no cartilaginous mold precedes the appearance of the bony tissue. The membrane that occupies the place of the future bone resembles connective tissue and ultimately forms the periosteum; it is composed of fibers and granular cells in a matrix. The peripheral portion is more fibrous, while in the interior the cells or osteoblasts predominate. The whole tissue is richly supplied with blood vessels. As the osteogenetic fibers grow out to the periphery, they continue to calcify and give rise to fresh bone spicules. Thus, a network of bone is formed, the meshes of which contain the blood vessels and a delicate connective tissue crowded with osteoblasts. Osteoblasts add layers of fresh bone to the trabeculae. These layers subsequently encroach upon the mesh, under the periosteum, and around the larger vascular channels that become the Haversian canals, thickening and developing the bones.
Endochondral Ossification
The perichondrium becomes the periosteum, which contains a layer of undifferentiated cells (osteoprogenitor cells) that later become osteoblasts. These osteoblasts secrete osteoid against the shaft of the cartilage model that serves as support for the new bone. Chondrocytes in the primary center of ossification begin to grow (hypertrophy). They stop secreting collagen and other proteoglycans and begin secreting alkaline phosphatase, an enzyme essential for mineral deposition. Then calcification of the matrix occurs and the hypertrophic chondrocytes begin to die, creating cavities within the bone. The hypertrophic chondrocytes (before apoptosis) secrete vascular endothelial cell growth factor, which induces the sprouting of blood vessels from the perichondrium. Blood vessels forming the periosteal bud invade the cavity left by the chondrocytes and branch in opposite directions along the length of the shaft. The blood vessels carry hemopoietic cells, osteoprogenitor cells, and other cells inside the cavity. The hemopoietic cells will later form the bone marrow. Osteoblasts, differentiated from the osteoprogenitor cells that entered the cavity via the periosteal bud, use the calcified matrix as a scaffold and begin to secrete osteoid, which forms the bone trabecula. Osteoclasts, formed from macrophages, break down spongy bone to form the medullary (bone marrow) cavity.

