19.2A: Lymphatic Vessel Structure
- Page ID
- 7905
The lymphatic structure is based on that of blood vessels.
- Describe lymphatic circulation and the structure of lymphatic vessels
Key Points
- Lymph (or lymphatic ) vessels are thin-walled valved structures that carry lymph.
- Lymph vessels are lined by endothelial cells and have a thin layer of smooth muscles and adventitia that bind the lymph vessels to the surrounding tissue.
- Lymph movement occurs despite low pressure due to smooth muscle action, valves, and compression during contraction of adjacent skeletal muscle and arterial pulsation.
- When the pressure inside a lymphangion becomes high enough, lymph fluid will push through the semilunar valve into the next lymphangion, while the valve then closes.
- Lymph vessels are structurally very similar to blood vessels.
- Valves prevent backwards flow of lymph fluid, which allows the lymphatic system to function without a central pump.
Key Terms
- lymphagion: The space between two semilunar valves of the lymphatic vessels that forms a distinct functional unit for the forward flow of lymph.
- adventitia: The outermost layer of connective tissue encasing a visceral organ or vessel.
- ISF: Interstitial (or tissue) fluid, a solution that bathes and surrounds the cells of multicellular animals. It is the main component of extracellular fluid, which also includes plasma and transcellular fluid.
- endothelial cells: A thin layer of cells that lines the interior surface of blood and lymphatic vessels, forming an interface between circulating blood or lymph in the lumen and the rest of the vessel wall.
The general structure of lymphatic vessels is similar to that of blood vessels since these are the only two types of vessels in the body. While blood and lymph fluid are two separate substances, both are composed of the same water (plasma or fluid) found elsewhere in the body.
Layers of Lymph Vessels
The endothelium, a general term for the inner layer of a vessel, is composed of an inner lining of single, flattened epithelial cells (simple squamous epithelium). This layer mechanically transports fluid. It sits on a highly permeable basement membrane made out of extracellular matrix that separates the endothelium from the other layers. The endothelium is designed with junctions between cells that allow interstitial fluid to flow into the lumen when pressure becomes high enough (such as from blood capillary hydrostatic pressure), but does not normally allow lymph fluid to leak back out into the interstitial space.
The next layer is smooth muscles arranged in a circular fashion around the endothelium that alters the pressure inside the lumen (space) inside the vessel by contracting and relaxing. The activity of smooth muscles allows lymph vessels to slowly pump lymph fluid through the body without a central pump or heart. By contrast, the smooth muscles in blood vessels are involved in vasoconstriction and vasodilation instead of fluid pumping.
The outermost layer is the adventitia, consisting of fibrous tissue. It is made primarily out of collagen and serves to anchor the lymph vessels to structures within the body for stability. Larger lymph vessels have many more layers of adventitia than do smaller lymph vessels. The smallest vessels, such as the lymphatic capillaries, may have no outer adventitia. As they proceed forward and integrate into the larger lymph vessels, they develop adventitia and smooth muscle. Blood vessels also have adventitia, sometimes referred to as tunica.
Lymphatic Valves
One of the main structural features of lymph vessels is their valves, which are semilunar structures attached to opposite sides of the lymphatic endothelium. Valves are found in larger lymph vessels and collecting vessels and are absent in the lymphatic capillaries. The valves is to prevent backflow of fluid, so that lymph eventually flows forward instead of falling backwards. When the pressure of lymph fluid increase to a certain point due to filling with more lymph fluid or from smooth muscle contraction, the fluid will be pushed through the valve (opening it) into the next chamber of the vessel (called a lymphangion). As the pressure falls, the open valve then closes so that the lymph fluid cannot flow backwards.
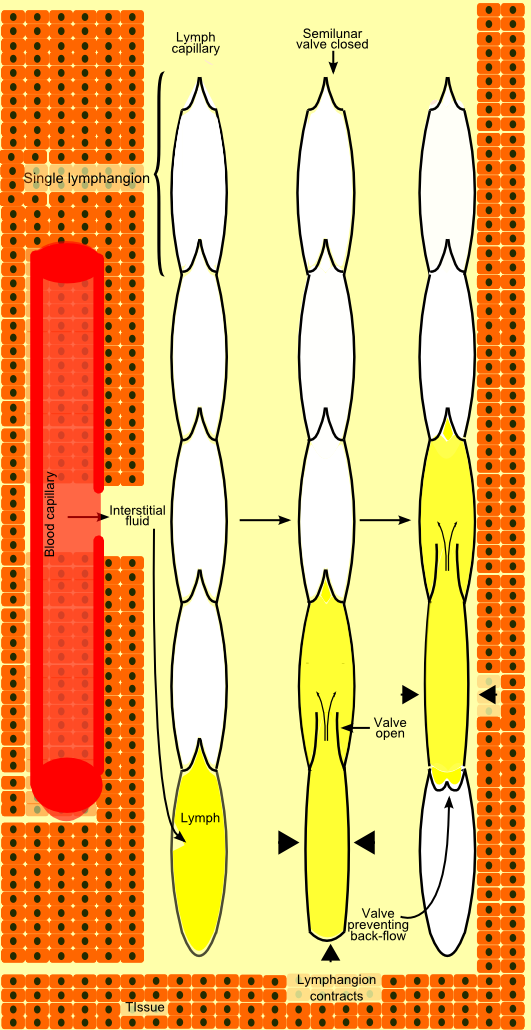
Lymph Vessel: Diagram representing propulsion of lymph through a lymph vessel.
A lymphangion is the term for the space between two semilunar valves in a lymphatic vessel, functional unit of the lymphatic system. Lymph fluid can only flow forward through lymphangions due to the closing of valves after fluid is pushed through by fluid accumulation, smooth muscle contraction, or skeletal muscle contraction.
Without valves, the lymphatic system would be unable to function without a central pump. Smooth muscle contractions only cause small changes in pressure and volume within the lumen of the lymph vessels, so the fluid would just move backwards when the pressure dropped. Blood vessels also have valves, but only in low pressure venous circulation. They function similarly to lymphatic valves, though are comparatively more dependent on skeletal muscle contractions.

