20.1D: Inflammation
- Page ID
- 7941
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Inflammation is part of the biological response of vascular tissues to harmful stimuli.
- Describe the biological mechanisms of inflammation and its role in innate immunity
Key Points
- Acute inflammation occurs due to infection, injury, or irritation, and is an essential part of the healing process to remove pathogens and start the wound-healing process.
- During inflammation, vasodilation occurs, the endothelium becomes more permeable as exudate leaks into the tissues, and neutrophils migrate to the site of inflammation.
- Acute inflammation is initiated by cells already present in all tissues, such as mast cells that recognize pathogen-associated molecular patterns (PAMPs) with toll-like receptors, but other cells like natural killer (NK) cells can trigger inflammation as well.
- Acute inflammation is characterized by pain, redness, immobility (loss of function), swelling, and heat.
- Neutrophils migrate to inflamed tissues by rolling onto the endothelium with selectins, adhering to it with integrins, and sliding through its gaps with PECAM-1. Then they follow chemokines to the tissues to find pathogens to destroy.
- Repeated bouts of acute inflammation lead to chronic inflammation, a process of constant healing and inflammation-induced damage as the initial problem is never truly healed.
- Allergic reactions are the result of an inappropriate immune response that triggers inflammation.
Key Terms
- extravasion:
- exudate: Protein-rich edema caused by proteins flowing into the tissues during inflammation due to increased vascular permeability and oncotic pressure.
- inflammatory mediator: Any chemical released from cells that stimulates the vasodilation and increased permeability that occur during acute inflammation.
Inflammation is part of the complex biological response of vascular tissues to harmful stimuli, such as pathogens, injury or trauma, and irritants. Inflammation is a protective attempt by the organism to remove injurious stimuli and initiate the healing process. Inflammation is not a synonym for infection, even in cases where inflammation is caused by infection. Rather, it refers to the response of the body to try and fight the infection. While inflammation is an important mechanism of innate immunity, it can harm the body in cases of allergy, autoimmunity, and infections in tissues with poor regenerative capacity such as the heart.
Functions and Components of Inflammatory Response
The main function of inflammation is to trigger an immune response in an area of the body that needs it to fight off pathogens that may cause an infection or to help heal an injury. The main symptoms of acute inflammation are swelling, redness, pain, loss of function, and heat. Three components to the basic acute inflammatory response occur every time: vasodilation, increased vascular permeability, and migration of leukocytes to the affected tissues.
Vasodilation
An inflammatory response can be caused by any of numerous inflammatory mediators released from innate immune system cells. The most common short term mediators are histamine and seratonin from mast cells, but bradykinin, complement proteins, some interleukins, prostaglandins, and TNF-alpha may also trigger inflammation from other types of cells. Circulating mast cells contain toll-like receptors, which can detect pathogen-associated molecular patterns (PAMPS) on the surface of pathogens and release an inflammatory mediator such as histamine in response. Alternatively, mast cells may release inflammatory mediators due to signals from damaged cells (which will release clotting factors) during trauma or injury.
After an inflammatory mediator is released in the bloodstream, a period of transient vasoconstriction, lasting only a few seconds, occurs. Then blood vessels expand to undergo vasodilation from the stimulus of the vasoactive inflammatory mediator, which increases blood flow to the area. This causes slowing and stasis of red blood cells, which can be involved in the clotting response needed to stop bleeding in the case of injury. Vasodilation is the reason for the redness, heat, and pain associated with inflammation.
Increased Vascular Permeability
The next step of acute inflammation is an increase in vascular permeability due to inflammatory mediator activity, which causes the blood vessels to become more permeable. Normally only water and small compounds can exit the bloodstream into the tissues, but during inflammation, large proteins in the bloodstream, such as serum albumins, can leak out and into the tissues. Water follows these proteins due to the force of oncotic pressure that the proteins exert. This is called exudate, a form of edema. As exudate accumulates within the tissues, they become swollen. The exudate may carry antimicrobial proteins and antibodies into the tissues, and stimulates lymphatic drainage.
Leukocyte Migration to the Tissues
The next step of the acute inflammatory response is chemotaxis migration of neutrophils to the affected area. Neutrophils are recruited to the site of inflammation by various cytokines. Other inflammatory mediators, such as TNF-alpha and IL-1, increase the expression of adhesion molecules on vascular endothelial cells. The neutrophils loosely attach to the endothelial cells through use of selectins, a process called rolling. Then integrins firmly attach to the adhesion molecules on the endothelial cells, which is called adhesion.Together, rolling and adhesion are referred to as margination, the accumulation of leukocytes on the endothelium.
The next step is for neutrophils to squeeze through the gaps in the endothelium into the tissues through binding with PECAM-1 expressed on the endothelium, a process called extravasion. Then the neutrophils follow a chemotactic gradient to the site of infection of injury in the tissues, where they will degranulate and phagocytize pathogens. Later, macrophages enter the tissues through a similar process to clean up dead neutrophils and cellular debris.
Outcomes of Acute Inflammation
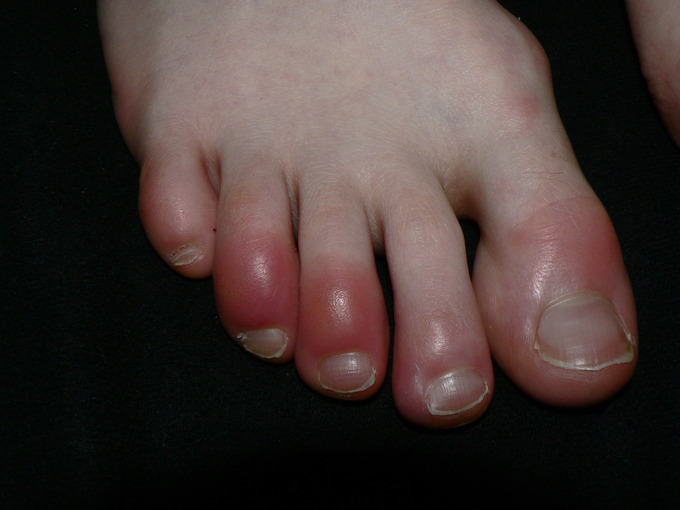
Inflammation: Toes inflamed by chilblains
When acute inflammation ends (typically by release of anti-inflammatory mediators such as IL-10 or an end to the release of inflammatory mediators) resolution will occur if the problem is alleviated. Resolution involves physiological responses that are part of the healing process, such as wound healing. If the problem is not resolved, acute inflammation could occur again. Repeated bouts of acute inflammation, known as chronic inflammation, leads to a progressive shift in the type of cells present at the site of inflammation and is characterized by simultaneous destruction and healing of the tissue from the inflammatory process. In particular, fibrosis (scarring) and tissue necrosis are common outcomes of chronic inflammation.


