5.5A: Steps of Tissue Repair
- Page ID
- 7449
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Wound healing is divided into four overlapping states: 1) homeostasis, 2) inflammatory, 3) proliferative, and 4) remodeling.
- Describe the overlapping phases of tissue repair
Key Points
- Wound healing is the process whereby the skin repairs itself after injury.
- Wound healing can be divided into four overlapping processes; maintenance of homoeostasis, an inflammatory response, a proliferative phase, and remodeling.
- Maintenance of homoeostasis is achieved by clotting in any damaged regions of the circulatory system.
- The inflammatory response clears the wound site of debris and prevents infection.
- During the proliferative phase new tissue and an extra cellular matrix to support tissue repair are laid down.
- During the remodelling stage, the rapidly laid down tissue is altered to more closely mimic surrounding, mature tissues.
- The wound healing process can be interrupted, leading to the formation of chronic wounds or the development of fibrosis.
Key Terms
- fibrin: A fibrous protein involved in blood clotting.
- fibronectin: An extra cellular matrix protein, often laid down as a component of the temporary granulation tissue seen in wound healing.
- Granulation: The temporary connective tissue laid down during wound healing to facilitate wound closure.
Wound Healing
Wound healing is the process by which the skin, or any injured organ, repairs itself after injury. The main aim of wound healing is to prevent or limit further damage, to clean and seal the wound against infection, to restore tissue strength, and, if possible, tissue function.
Wounds in the skin can either be classed as epidermal (shallow, in which the dermis remains intact) or deep (in which the dermis is damaged; this is sometimes referred to as a full thickness wound).
Phases of the Wound Healing Process
The wound healing process can be characterized by four overlapping phases:
- An initial response to maintain homoeostasis.
- An inflammatory response to prevent infection.
- A proliferative phase to reconstitute the wound site.
- A remodelling phase where tissue strength and function are restored.
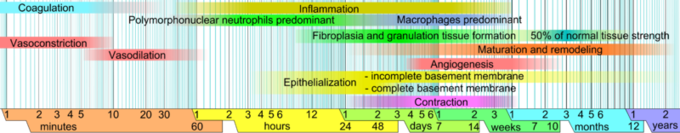
Critical developments that occur during a localized inflammatory response: The phases of wound healing during an inflammatory response to infection. Limits vary within faded intervals, mainly by wound size and healing conditions. The image does not include major impairments that cause chronic wounds.
Homoeostasis
Upon wounding, the first phase of the wound response is concerned with maintaining homoeostasis within the body. Most wounds, even superficial shallow wounds, result in damage to the circulatory system. To prevent blood loss and reduce the chance of infection spreading throughout the body, circulation platelets within the blood begin to form a fibrin clot, which seals the wound site.
Additionally, vasoconstriction initially occurs around the wound site as a means of isolating the wound site. However, this is soon followed by vasodilation so the required cells are able to be recruited to the wound site. Factors are released from damaged cells, and those around the wound site initiate the inflammatory response. This phase is very quick.
Inflammatory
Immune cells, such as neutrophils and macrophages, are attracted by factors released from the wound site and begin to accumulate, travelling through the circulatory system. These cells are responsible for the removal of debris and killing of bacteria that easily colonize the wound site, and prepare the wound for the proliferative/remodelling phase.
Proliferative
The proliferative phase can itself be divided into four phases; in the case of shallow wounds the first two steps may not occur:
- Re-vascularisation: New blood vessels are formed around the wound site in order to supply the cells and nutrients required to remodel the wound.
- Granulation: Fibroblasts attracted to the wound site quickly lay down a temporary extra cellular matrix, comprised of collagen and fibronectin, upon which the epidermis can be reconstituted.
- Re-epithelialization: The exact mechanism of re-epithelialization is poorly understood. It is thought that surviving epithelial cells around the wound edge become more motile and stretch to cover the wound site. Once a continuous epidermis is formed they lose this motility and begin to divide.
- Contraction: Re-epithelization is thought to occur simultaneously with contraction, where myo-fibroblasts recruited around the wound site pull against each other to contract the size of the wound.
Remodeling
Following closure of the wound, remodeling can occur. The epidermis proliferates and returns to its normal character; fibroblasts and immune cells which were recruited to the site are degraded; and the temporary extra cellular matrix that was laid down is remodelled into a stronger, more permanent structure.
Issues with Wound Healing
The above mechanism describes a best-case scenario that results in the restoration of a fully functional dermis and epidermis. However, as the main aim of the wound healing process in the initial stage is to prevent further damage or infection, the intial stages can lead to a less than optimum result, as evidenced by the formation of scars. The larger and more severe the wound the more likely this is to occur.
The response to wounding is also susceptible to disruptions that can lead to the formation of chronic, non-resolving wounds such as ulcers; or the development of fibrosis if the proliferative phase does not resolve.

