4.5: Staple Removal
- Page ID
- 10008
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Staples are made of stainless steel wire and provide strength for wound closure. The wound location sometimes restricts their use because the staples must be far enough away from organs and structures. The aesthetic outcome may not be as desirable as a suture line, but staples are strong, quick to insert, and simple to remove.
Removal of staples requires sterile technique and a staple extractor. An order to remove the staples, and any specific directions for removal, must be obtained prior to the procedure. The health care professional performing the removal must also inspect the wound prior to the procedure to ensure the wound is adequately healed to have the staples removed. Usually every second staple is removed initially; then the remainder are removed at a later time (Perry et al., 2014). In general, staples are removed within 7 to 14 days.
Checklist 36 outlines the steps for removing staples from a wound.
Checklist 36: Staple RemovalDisclaimer: Always review and follow your hospital policy regarding this specific skill. |
|||
Safety considerations:
|
|||
Steps |
Additional Information |
||
| 1. Confirm physician orders, and explain procedure to patient. | Explanation helps prevent anxiety and increases compliance with the procedure. Inform patient the procedure is not painful but the patent may feel some pulling or pinching of the skin during staple removal. | ||
| 2. Gather appropriate supplies. | Gather sterile staple extractors, sterile dressing tray, non-sterile gloves, normal saline, Steri-Strips, and sterile outer dressing. | ||
| 3. Position patient appropriately and create privacy for procedure. | Ensure proper body mechanics for yourself and create a comfortable position for the patient. | ||
| 4. Perform hand hygiene. | This reduces the risk of infection.

Perform hand hygiene |
||
| 5. Prepare the sterile field and add necessary supplies (staple extractor). | This step allows easy access to required supplies for the procedure.

Add sterile items to sterile field |
||
| 6. Remove dressing and inspect the wound. | Visually assess the wound for uniform closure of the edges, absence of drainage, redness, and inflammation.
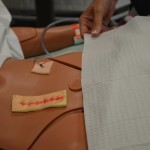
Remove dressing and inspect the wound After assessing the wound, determine if the wound is sufficiently healed to have the staples removed. If concerns are present, question the order and seek advice from the appropriate health care provider. |
||
| 7. Apply non-sterile gloves. | This reduces the risk of contamination.

Apply non-sterile gloves |
||
| 8. Clean incision site according to agency policy. | This reduces the risk of infection from microorganisms on the wound site or surrounding skin.
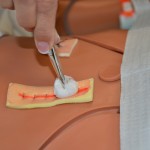
Clean incision site Cleaning also loosens and removes any dried blood or crusted exudate from the staples and wound bed. |
||
| To Remove Staples (start with every second staple). | |||
| 9. Place lower tip of staple extractor beneath the staple. Do not pull up while depressing handle on staple remover or change the angle of your wrist or hand. Close the handle, then gently move the staple side to side to remove. | The closed handle depresses the middle of the staple causing the two ends to bend outward and out of the top layer of skin.
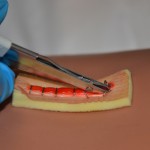
Close the handle, then gently move the staple from side to side to remove |
||
| 10. When both ends of the staple are visible, move the staple extractor away from the skin and place the staple on a sterile piece of gauze by releasing the handles on the staple extractor. | This avoids pulling the staple out prematurely and avoids putting pressure on the wound. It also prevents scratching the skin with the sharp staple.
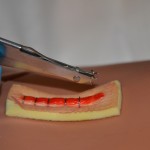
Keep the handle closed and move the staple extractor away from the skin |
||
| 11. Continue to remove every second staple to the end of the incision line. | Alternating removal of staples provides strength to incision line while removing staples and prevents accidental separation of incision line.
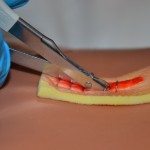
Continue to remove every second staple to the end of the incision line |
||
| 12. Using the principles of sterile technique, place Steri-Strips on location of every removed staple along incision line. | Cut Steri-Strips to allow them to extend 1.5 to 2 cm on each side of incision.
Remove sterile backing to apply Steri-Strips. 
Cut Steri-Strips Steri-Strips support wound tension across wound and eliminate scarring. This allows wound to heal by primary intention. 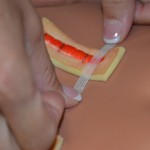
Cut Steri-Strips to allow them to extend 1.5 to 2 cm on each side of incision |
||
| 13. Remove remaining staples, followed by applying Steri-Strips along the incision line. | Steri-Strips support wound tension across wound and eliminate scarring. | ||
| 14. Apply dry, sterile dressing on incision site or leave exposed to air if wound is not irritated by clothing, or according to physician orders. | This reduces risk of infection.

Apply dry, sterile dressing if required |
||
| 15. Position patient, lower bed to safe height, and ensure patient is comfortable and free from pain. | This provides patient with a safe, comfortable place, and attends to pain needs as required. | ||
| 16. Complete patient teaching regarding Steri-Strips and bathing, wound inspection for separation of wound edges, and ways to enhance wound healing. | Instruct patient to take showers rather than bathe.
Instruct patient not to pull off Steri-Strips and to allow them to fall off naturally and gradually (usually takes one to three weeks). Instruct on the importance of not straining during defecation, and of adequate rest, fluids, nutrition, and ambulation for optional wound healing. |
||
| 17. Discard supplies according to agency policies for sharp disposal and biohazard waste. | Staple extractor may be disposed of or sent for sterilization. | ||
| 18. Perform hand hygiene and document procedure and findings according to agency policy. Report any unusual findings or concerns to the appropriate health care professional. | Hand hygiene reduces the risk of infection.

Hand hygiene with ABHR |
||
| Data source: BCIT, 2010c; Perry et al., 2014 | |||
Special Considerations:
- Confirm physician order to remove all staples or every second staple. All wounds held together with staples require an assessment to ensure the wound is sufficiently healed to remove the staples.
Staple removal may lead to complications for the patient. When removing staples, consider the length of time the staples have been in situ. Wound dehiscence, a mechanical failure of wound healing, remains a problem and can be affected by multiple factors (Spiliotis et al., 2009). Obese patients (greater than 30 kg/m2) have a higher risk of dehiscence than patients with a normal BMI. Additional risk factors for dehiscence include age over 75 years, COPD, diagnosis of cancer, use of steroids, malnutrition, anemia, sepsis, obesity, diabetes, tobacco use, and previous administration of chemotherapy or radiotherapy (Spiliotis et al., 2009). Table 4.5 lists other complications of removing staples.
| Table 4.5 Complications of Staple Removal | |||
|
Complication |
Solution |
||
| Unable to remove staple from tissue | Contact physician for further instructions. | ||
| Dehiscence: Incision edges separate during staple removal | Stop removing staples.
Apply Steri-Strips across open area. Notify physician. |
||
| Patient experiences pain when staples are removed | Allow small breaks during removal of staples.
Provide opportunity for the patient to deep breathe and relax during the procedure. |
||
| Data source: BCIT, 2010c; Perry et al., 2014 | |||
Critical Thinking Exercises
- You are about to remove your patient’s abdominal incision staples according to the physician’s orders. As you start to remove the staples, you notice that the skin edges of the incision line are separating. What would be your next steps?
- Your patient informs you that he is feeling significant pain as you begin to remove his staples. What would you do next?


