1: Setting the Groundwork for Evidence-Based Massage
- Page ID
- 59108
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)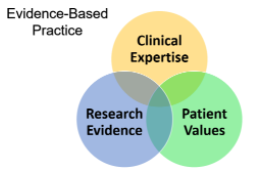
Evidence-based massage therapy is an approach based on three principles (best available evidence, clinical expertise and patient values).
Being a recognized treatment option for people in pain means the profession of massage therapy is moving into new formal settings. As this shift occurs, it is important that therapists adhere to evidence-based medicine and use critical thinking and research literacy skills. In the early 1990’s David Sackett and Gordon Guyatt introduced evidence-based medicine (EBM) as the conscientious use of current best evidence in making decisions about patient care. It is a process intended to reduce the risk of harm and improve decision-making by emphasizing the use of evidence from well-designed research. This includes the use of logical reasoning and the gathering of ideas and knowledge from many overlapping disciplines.
- Patient Values – The needs and requests of your patient will influence your decision making. Therapists need to be able to hear the patient’s values and create a working relationship with the patient. Shared-decision making will include developing a plan of care based on individualized goals and needs of the patient.
- Research Evidence – Research helps guide clinical decisions and to warn of known harm, the higher the quality of the evidence the more confident we can be as a therapist making an informed decision.
- Clinical Expertise – Clinical experience is used to create individualized treatment plans as patient presentation will vary on a case by case basis. Making sound decisions requires the clinician to assess the patient’s personal, social, and clinical context and integrate this information with the values and preferences of the informed patient. The therapist will use his/her clinical expertise and allow the evidence to guide this process, rather than dictate it.
Evidence-based medicine integrates research evidence with clinical expertise and patient values to achieve the best possible patient management, while minimizing the potential for harm. The widespread adoption of evidence-based practice has led to improved healthcare and a cohesive approach essential for improving patient outcomes.
References and Sources
Albarqouni, L., Hoffmann, T., Straus, S., Olsen, N. R., Young, T., Ilic, D., … Glasziou, P. (2018). Core Competencies in Evidence-Based Practice for Health Professionals: Consensus Statement Based on a Systematic Review and Delphi Survey. JAMA network open, 1(2), e180281. doi:10.1001/jamanetworkopen.2018.0281
Baskwill, A. (2016). A guiding framework to understand relationships within the profession of massage therapy. Journal of bodywork and movement therapies, 20(3), 542–548. doi:10.1016/j.jbmt.2015.12.003
Baskwill, A. J., & Dore, K. (2016). Exploring the awareness of research among registered massage therapists in Ontario. Journal of complementary & integrative medicine, 13(1), 41–49. doi:10.1515/jcim-2015-0006
Baskwill, A., Vanstone, M., Harnish, D., & Dore, K. (2019). “I am a healthcare practitioner”: A qualitative exploration of massage therapists’ professional identity. Journal of complementary & integrative medicine, 17(2), /j/jcim.2020.17.issue-2/jcim-2019-0067/jcim-2019-0067.xml. https://doi.org/10.1515/jcim-2019-0067
Baskwill, A., Vanstone, M., Harnish, D., & Dore, K. (2021). Identification of common features within massage therapists’ professional identity. Journal of complementary & integrative medicine, 10.1515/jcim-2020-0368. Advance online publication. https://doi.org/10.1515/jcim-2020-0368
Djulbegovic, B., & Guyatt, G. H. (2017). Progress in evidence-based medicine: a quarter century on. Lancet (London, England), 390(10092), 415–423. https://doi.org/10.1016/S0140-6736(16)31592-6
Gowan-Moody, D. M., Leis, A. M., Abonyi, S., Epstein, M., & Premkumar, K. (2013). Research utilization and evidence-based practice among Saskatchewan massage therapists. Journal of complementary & integrative medicine, 10, /j/jcim.2013.10.issue-1/jcim-2012-0044/jcim-2012-0044.xml. doi:10.1515/jcim-2012-0044
Greenhalgh, T., Howick, J., Maskrey, N., & Evidence Based Medicine Renaissance Group (2014). Evidence based medicine: a movement in crisis?. BMJ (Clinical research ed.), 348, g3725. doi:10.1136/bmj.g3725
Guyatt, G., Cairns, J., Churchill, D., Cook, D., Haynes, B., Hirsh, J., … & Sackett, D. (1992). Evidence-based medicine: a new approach to teaching the practice of medicine. JAMA, 268(17), 2420-2425.
Kennedy, A. B., Cambron, J. A., Sharpe, P. A., Travillian, R. S., & Saunders, R. P. (2016). Clarifying Definitions for the Massage Therapy Profession: the Results of the Best Practices Symposium. International journal of therapeutic massage & bodywork, 9(3), 15–26. doi:10.3822/ijtmb.v9i3.312
Kennedy, A. B., Cambron, J. A., Sharpe, P. A., Travillian, R. S., & Saunders, R. P. (2016). Process for massage therapy practice and essential assessment. Journal of bodywork and movement therapies, 20(3), 484–496. doi:10.1016/j.jbmt.2016.01.007
Larsen, C. M., Terkelsen, A. S., Carlsen, A. F., & Kristensen, H. K. (2019). Methods for teaching evidence-based practice: a scoping review. BMC medical education, 19(1), 259. doi:10.1186/s12909-019-1681-0
Ooi, S. L., Smith, L., & Pak, S. C. (2018). Evidence-informed massage therapy – an Australian practitioner perspective. Complementary therapies in clinical practice, 31, 325–331. doi:10.1016/j.ctcp.2018.04.004
Patelarou, A. E., Kyriakoulis, K. G., Stamou, A. A., Laliotis, A., Sifaki-Pistolla, D., Matalliotakis, M., … Patelarou, E. (2017). Approaches to teach evidence-based practice among health professionals: an overview of the existing evidence. Advances in medical education and practice, 8, 455–464. doi:10.2147/AMEP.S134475
Riley, S. P., Petrosino, C., & Cleland, J. A. (2020). Do you really have the only, right, or best evidence-based approach to treat your patients?. The Journal of manual & manipulative therapy, 28(5), 251–253. https://doi.org/10.1080/10669817.2020.1847413
Sackett, D. L., Rosenberg, W. M., Gray, J. A., Haynes, R. B., & Richardson, W. S. (1996). Evidence based medicine: what it is and what it isn’t. BMJ (Clinical research ed.), 312(7023), 71–72. doi:10.1136/bmj.312.7023.71
Smith, R., & Rennie, D. (2014). Evidence-based medicine–an oral history. JAMA, 311(4), 365–367. doi:10.1001/jama.2013.286182


