3.16: Primary Presurgical Treatment for Cleft Nose, Lip, Dentoalveolar Arches and Palate
- Page ID
- 47881
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
CLEFT LIP AND PALATE SURGICAL TECHNIQUES: PRIMARY PRESURGICAL TREATMENT FOR CLEFT NOSE, LIP, DENTOALVEOLAR ARCHES & PALATE
Kurt Bütow and Roger Zwahlen
Functional jaw-orthognathic (FJO) suction and drinking plates are important elements in the management of cleft lip and palate (CLAP) deformities. They allow patients to eat and drink while awaiting surgical repair, and actively rotate smaller dentoalveolar segments prior to surgical intervention.
This chapter focuses on indications, contraindications, timing and methodology of functional jaw-orthognathic suction and drinking plates for patients with CLAP deformities.
Description and variations
Various devices are employed for primary treatment of cleft patients according to the type of cleft deformity:
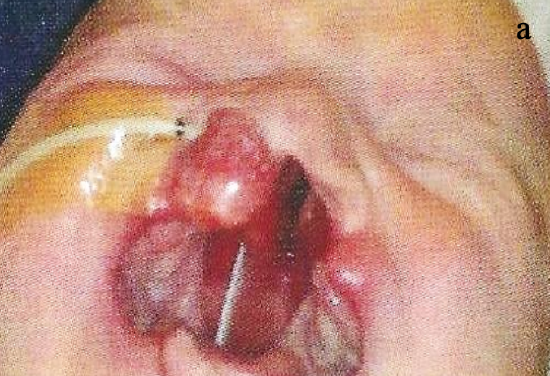
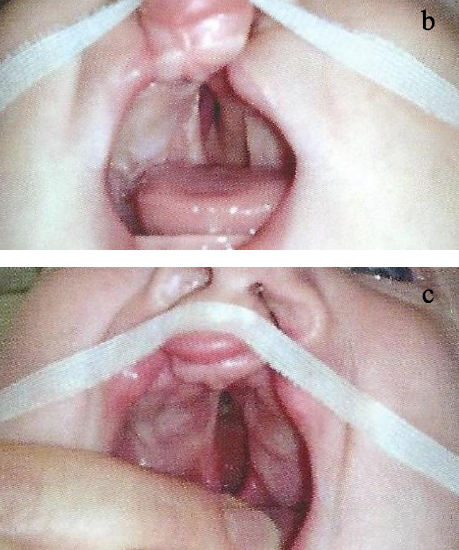
Figure 1: Lip bandage and FJO used to reposition the premaxilla with bilateral CLAP (a); at 2¾ months (b) at 5 months (c)

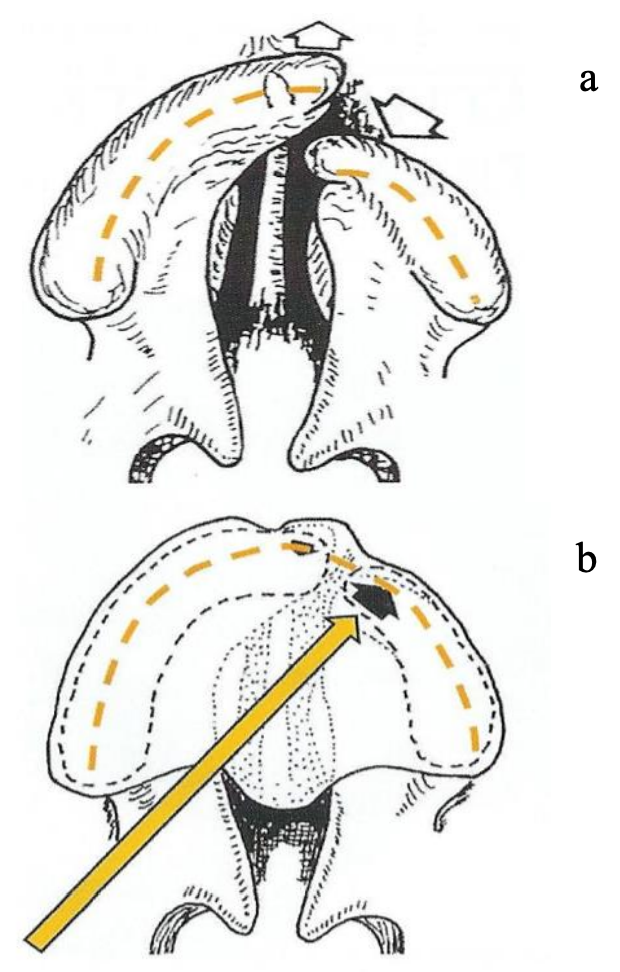
Figure 2a: Action of FJO
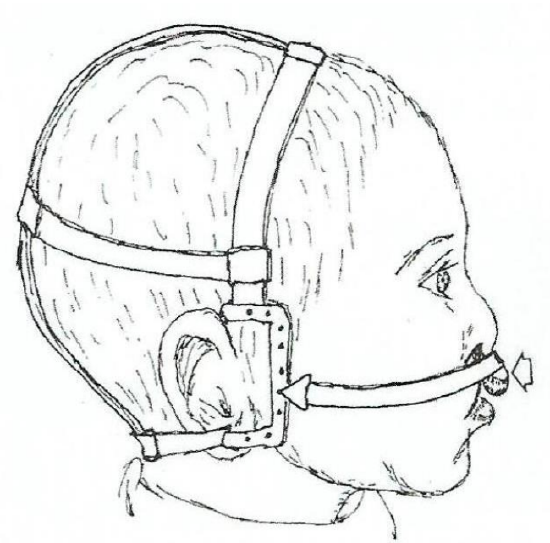
Figure 2b: Headgear for bilateral CLAP premaxilla repositioning
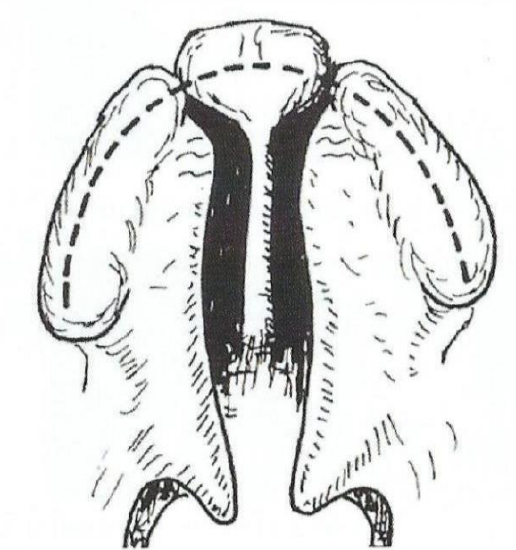
Figure 2c: Final reduction of CLAP prior to surgical intervention
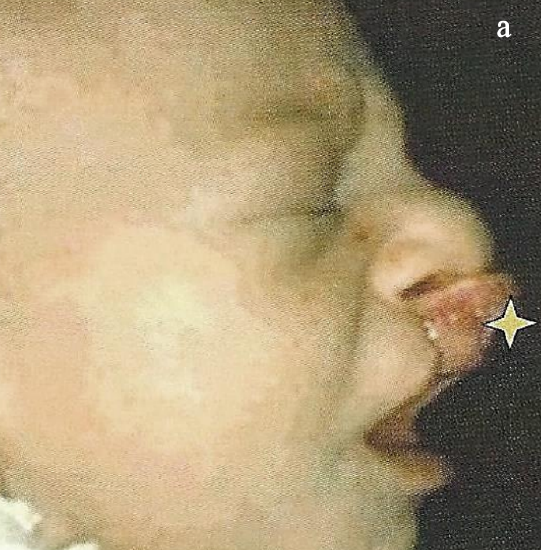
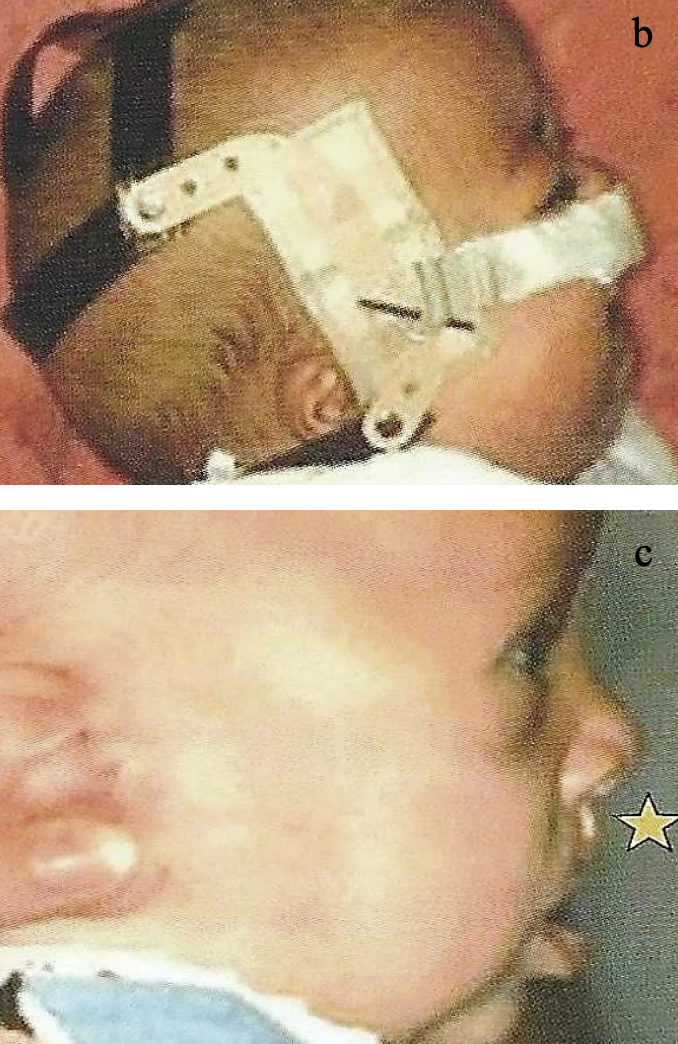
Figure 3: Protruded premaxilla-prolabium (a); headgear for bilateral CLAP premaxilla repositioning (b); result of conservative premaxilla repositioning achieved prior to surgery (c)
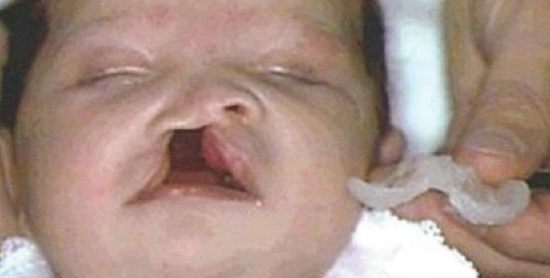
Figure 4: Example of orthopedic device (drinking plate)
Figures 5a,b: Functional jaw-orthognathic suction and drinking (FJO) plate
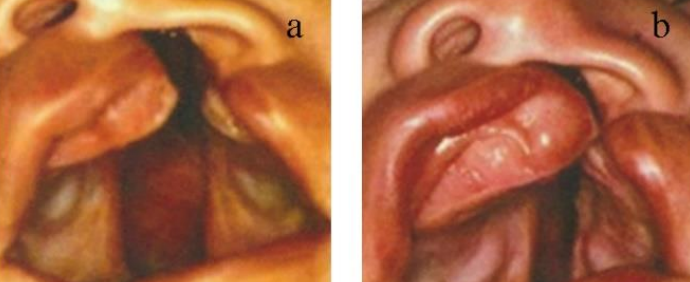
Figures 6a,b: Functional jaw-orthognathic movement after 5 months of treatment with a FJO
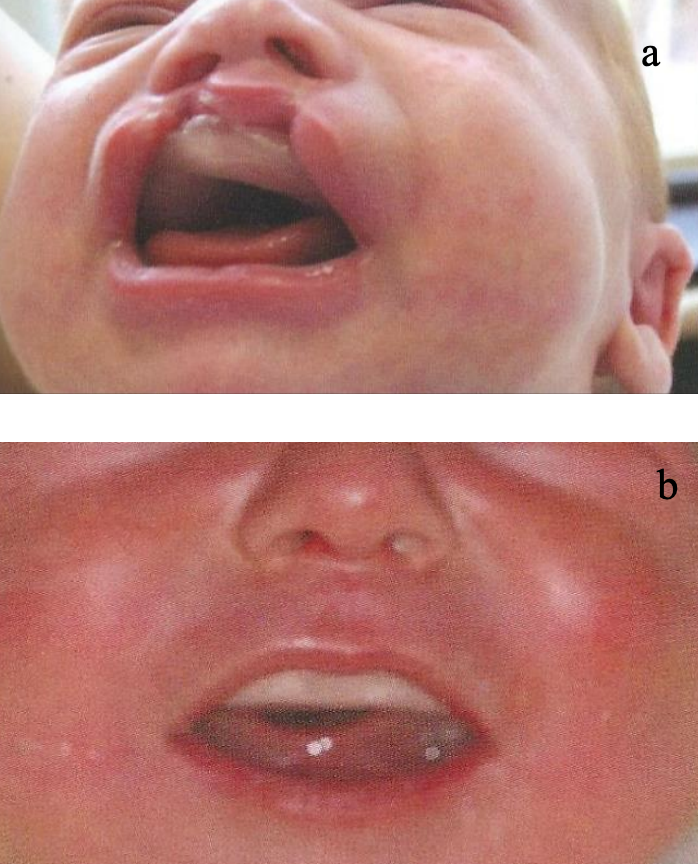
Figures 7ab: Example of an orthopedic devices (drinking plates) in situ
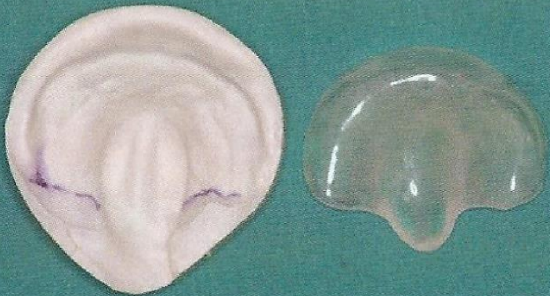
Figure 8: Suction and drinking plate (obturator with dorsal extension)
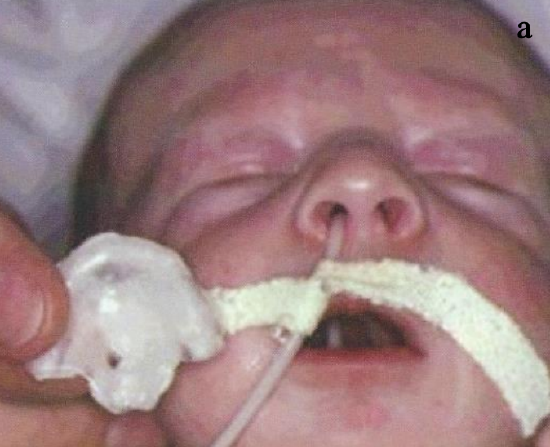
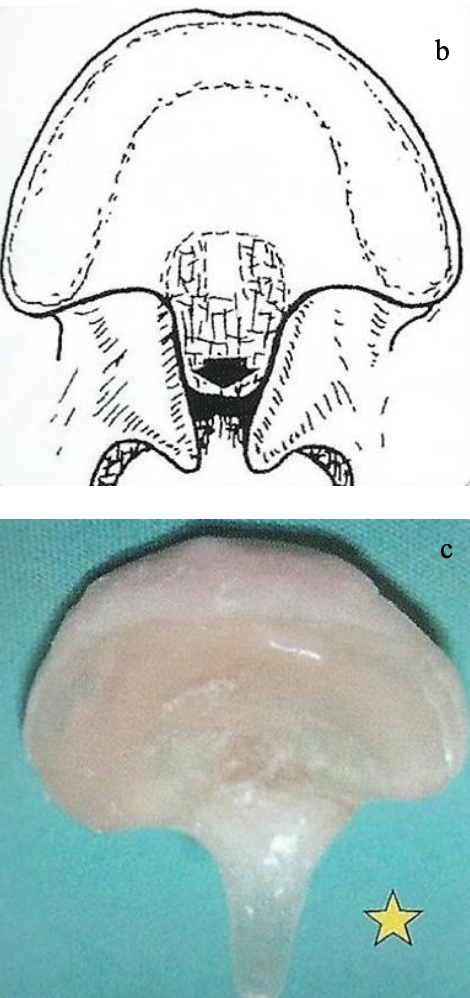
Figures 9a-c: Suction and drinking plate with posterior extension for hPsP cleft
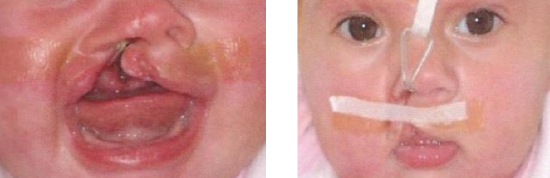
Figure 10: Nasal alar cartilage molding achieved after initial repair of the soft palate, prior to repair of the hard palate, anterior nasal floor and lip
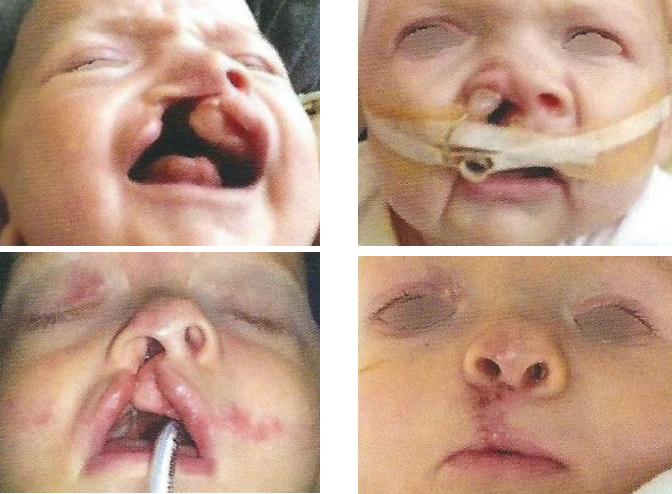
Figure 11: Improvement of cleft alar cartilage architecture following 5 months’ alar cartilage moulding (NAM) and 6 days postoperative (Courtesy Dr Emad Ghabrial)
- Lip bandage (“taping”) to narrow a wide unilateral cleft lip deformity
- Lip bandage (“taping”) both to narrow a wide bilateral cleft lip deformity as well as to reposition a protrusive premaxilla in bilateral cleft lip-alveolus and bilateral cleft lip-alveolus-palate deformities (Figures 1a-c)
- Headgear device to reposition a protrusive premaxilla in bilateral cleft lipalveolus and cleft lip-alveolus-palate deformities (Figures 2, 3)
- Functional jaw-orthognathic suction and drinking plate (FJO) (Figure 4) that further molds the displaced and rotated dentoalveolar arches (Figures 5, 6). Moreover, this device, like an obturator in tumor surgery, separates the nasal from the oral cavity in uni- and bilateral cleft lip-alveolus-palate deformities, allowing sucking, drinking and breathing
- Suction and drinking plate (Bolton plate) for patients with clefts at the hardsoft palate. These plates may be manufactured with or without additional dorsal extension to serve for breathing as an anti-apnoea device as well as an obturator for suction and drinking (Figures 7, 8, 9)
- Nasal alar molding (NAM 1) and nasal alveolar molding (NAM 2) devices
- NAM 1 to improve the deformed alar cartilage pre-surgically that often presents with an anti-convex deformity at the cleft side. Additionally, this device can be used to continuously mold the alar cartilage during the post-surgical healing phase (Figure 10)
- NAM 2 to improve the deformed alar cartilage, to mold displaced and rotated dentoalveolar arches, being further useful as an obturator for suction, drinking and breathing (Figure 11)
Indications
In neonates with any type of cleft lip, alveolus or palatal deformity, primary treatment immediately after birth is of paramount importance to ensure:
- Breathing by separating the oral cavity from the nasal cavity
- Feeding to thrive and gain weight during the pre-surgical period
- Molding displaced-rotated dentoalveolar arches to facilitate planned surgical procedures
- Posterior positioning of a protrusive premaxilla with bilateral cleft lip-alveolus and cleft lip-alveolus-palate, and to ease the tension of reunited muscle and soft tissue during surgery
- Narrowing unilateral and bilateral cleft lip width by presurgical lip bandaging (“taping”) for easier cleft lip reconstruction and a more pleasing outcome
- Nasal alar molding on the cleft side to achieve a more acceptable aesthetic result of the nasal ala and the anterior nasal passage on the cleft side both in the short and long term
Contraindications
Only a few contraindications exist regarding appliances used for primary treatment:
- Skin rash due to taping of lip bandages
- Parents’ compliance: Parents must be committed to clean the devises daily to avoid infection and pressure sores
- Patients with isolated cleft soft palates only very seldom tolerate an obturator plate
- In patients with Pierre Robin sequence who present with a hard-soft cleft palate, the Bolton plate with its dorsal extension may not be tolerated as a breathing (27%) or as a feeding aid (36%)
Timing
- Lip bandaging is commenced shortly after birth with cleft lip and cleft lipalveolus deformities
- In patients with a cleft lip-alveolus palate and cleft hard-soft palate, treatment commences as soon as an impression of the palate with rubber-like material can be made to manufacture the functional jaw-orthognathic suction and drinking plate (FJO), preferably in the 1st week after birth (Figure 4)
Duration
Presurgical treatment of primary cleft lip palates is commenced shortly after birth and continues until the first surgical intervention.
Patients with lip bandages and intra-oral devices need to be reevaluated at least monthly for:
- Plate adjustment due to changes from palatal/oral cavity growth
- Controlling the molding of dentoalveolar arches to achieve the best possible presurgical dentoalveolar arch configuration
- Advice to parents about pressure marks and device tidiness as well as feedback regarding breathing and feeding
Expected results
Primary treatment in cleft lip-palate patients is key to achieving substantially better long term functional (breathing, occlusion, swallowing) as well as aesthetic results of the nose and lip.
Manufacturing of devices
The two important devices for the primary treatment are
- Functional jaw-orthognathic suction and drinking plate (FJO) in cleft lipalveolus-palate patients
- Extended suction and drinking plate, Bolton plate) that can also be dorsally extended in patients with hard-soft palate clefts
Both are essential for breathing and feeding. The FJO is also important to mold the dentoalveolar arches in preparation for surgery.
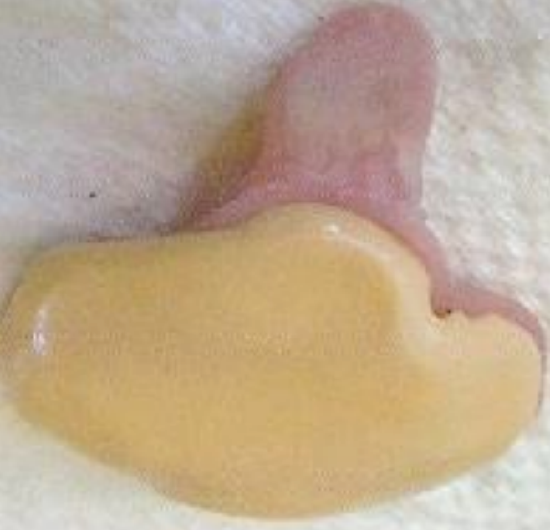
Figure 12: Bolton type device
Jaw impressions are made using a dental ‘rubber’ compound (Figure 12), ± a silicone material, as is normally used to take impressions for dental crowns and bridge reconstruction. Under NO circumstances, should “alginate” material be used to create jaw impressions due to the risk of the alginate being displaced into the nasal and/or pharyngeal/laryngeal spaces. This dental ‘rubber’ component is loaded onto a custom-made infant impression tray or ‘spoon’ (Figure 12), as every infant presents with unique oral anatomical dimensions related to the size and width of the alveolar arches and the depth of the palate.

Figure 13: Jaw impressions are done with a dental ‘rubber’ component of a CLAP
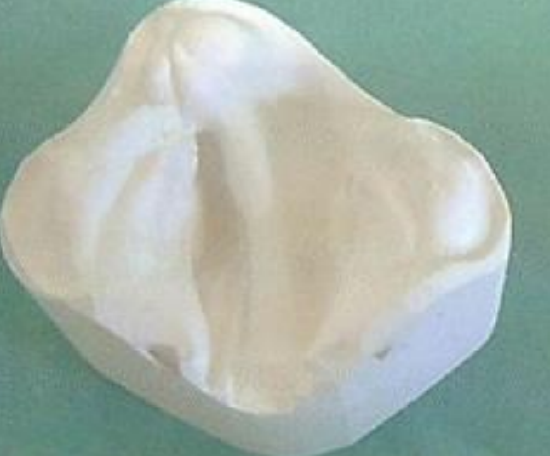
Figure 14: Plaster-of-Paris model on which plates are manufactured
The impression serves as a cast to create a Plaster-of-Paris model (Figures 13, 14) on which the plates are manufactured with Acrylic material of around 0.7–1.0 mm thickness.
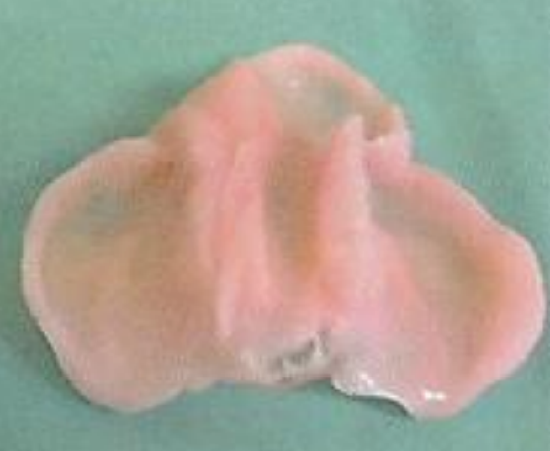
Figure 15: Acrylic material of around 0.7-1.0 mm thickness with soft denture-lining material that has been molded on the Plaster of Paris model for CLAP defect
The plate is equipped with a soft denture lining material that is molded in the oral cavity and the dentoalveolar arches and the palate (Figure 15). The FJO-plate needs to fit well. Should it be loose-fitting, adhesion powders or creams used for dentures may improve its retention.
Examples
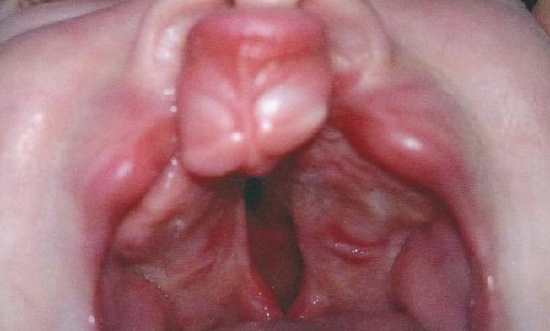
Figure 16: A bilateral cleft palate and lip (CLAP)
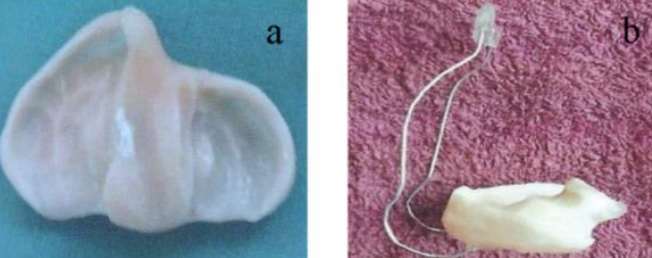
Figure 17a: Orthopedic device (drinking plate); 17b: Suction and drinking plate (SDP) with external facial stabilizer for hPsP cleft
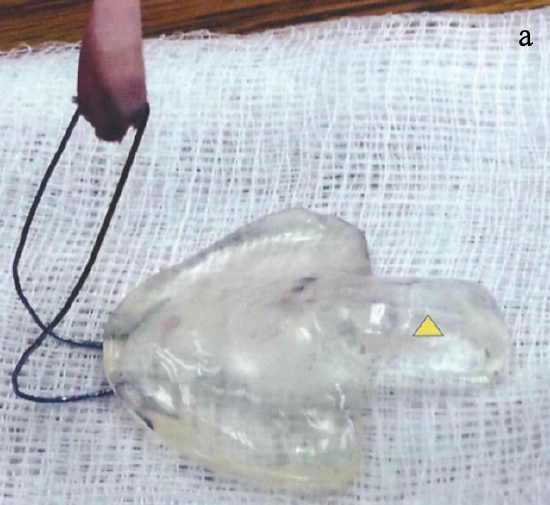
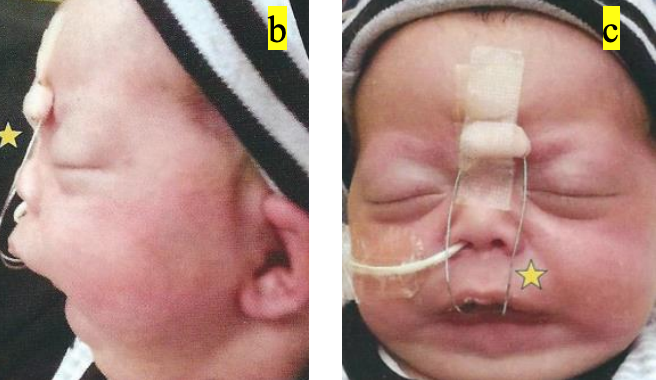
Figure 18a-c: To avoid glossoptosis in a patient with hPsP and Pierre Robin syndrome, a special suction plate (Bolton plate) is used with an additional posterior extension and external facial retention
Other cleft palate and lip chapters
Cleft lip & palate surgical techniques: introduction and philosophy
Recommended online text
Authors
Professor Kurt-W Bütow MChD (MFO Surg), DrMedDent, PhD, DSc, FCMFOS, Maxillo-Facial Surgery; Fellowship in Cleft Facial Deformities
University of Pretoria Cleft Palate Deformities Clinic
Pretoria, South Africa
kurt@butow.co.za
Roger Zwahlen DipMedDent, DipMed, DrMed, DrMedDent, Private Docent
FMHMKG, FEBOMFS, FIBCSOMS
Specialist in Oral and Maxillofacial Surgery
Practice Verdeja
Fribourg, Switzerland
rozwahlen@gmail.com
Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


