4.12: Blood - Components and Functions
- Page ID
- 83994
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
Blood is a complex fluid containing many different types of substances and cellular components. Approximately 55 percent of the blood consists of a pale yellow liquid called plasma; the other 45 percent is made up of the blood cells and platelets, which are suspended in the plasma (Figure 4.14). A person maintains normal numbers of RBCs and platelets by balancing their rapid destruction with rapid production in the red bone marrow.

Plasma
About 90 percent of blood plasma consists of water. The properties of water allow it to dissolve most substances and flow easily through the circulatory system, transporting materials and blood cells. Water also provides an excellent medium for distributing heat from warmer to cooler areas. The water and buffers in the plasma help maintain proper acid/base balance in body cells. Finally, plasma contains substances (e.g., antibodies). Therefore, plasma contributes to all four functions of the circulatory system.
Red Blood Cells
Red blood cells (RBCs) are the most numerous blood cells (Figure 4.14). They contain a great deal of a red material called hemoglobin. Because hemoglobin can bind oxygen and carbon dioxide and can act as a buffer, RBCs can transport much oxygen from the lungs to body cells, transport some carbon dioxide from body cells to the lungs, and help regulate acid/base balance.
Platelets
Platelets are cell fragments that form when small pieces break off from large parent cells in the red bone marrow (Figure 4.14). Platelets start the formation of blood clots.
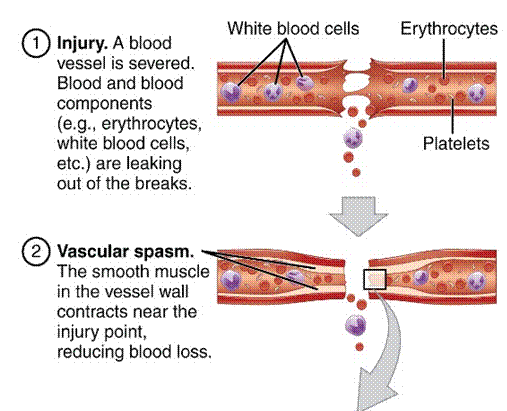
Because platelets are fragments of cells, they are fragile and burst open when they come into contact with rough spots, collagen, or unusual chemicals. This occurs, for example, when blood leaks out of a damaged vessel (Figure 4.15). The bursting platelets release substances that help form a sticky fibrous material called fibrin, which begins to plug the hole in the vessel. As blood cells become trapped in the fibrin mesh, the spaces among the fibrin threads are filled. The resulting blood clot forms a leakproof seal, stopping the bleeding.

Unfortunately, platelets burst open and start the clotting mechanism whenever roughness, collagen, or unusual chemicals are encountered. When this happens on an atherosclerotic plaque, the resulting clot may block the artery and lead to a heart attack or stroke. In addition, since some platelets are bursting at all times, slow blood flow, as occurs in varicose veins, permits the substances released by platelets to accumulate at that location. When enough platelet material builds up, a thrombus forms.
White Blood Cells
The white blood cells (WBCs) are also called leukocytes, which means "white cells." Blood contains only 1 WBC for every 500 RBCs (Figure 4.14).
WBCs can be divided into two main groups. The cells in one group are called polymorphonuclear leukocytes (“many structured nucleus, white blood cell) (PMNs) or granulocytes ("granular cells"). The other main group of WBCs consists of the agranulocytes ("cells without granules").
There are three types of PMNs. The most numerous type by far are neutrophils, which are important defense cells because they phagocytize (ingest) undesirable materials. Because they can move about like amoebas and can travel through capillary walls, they are found not only in the circulating blood but also among body cells. These and other phagocytic WBCs resemble vacuum cleaners as they move into every area of the body, sucking up debris.
Many neutrophils are stored within blood vessels, especially in the bone marrow. Stored neutrophils are mobilized into the circulating blood when there is a need for additional defense activity, as occurs when an infection develops.
The other two types of PMNs are basophils and eosinophils. Basophils produce histamine, which initiates inflammation whenever body cells are injured or killed. Eosinophils seem to help moderate inflammation. Eosinophils seem to be defense cells, too, because their number increases in certain situations, such as during an allergic reaction or when small parasites invade the body. Eosinophils and basophils are thought to have several additional functions.
There are only two types of agranulocytes in the blood. Lymphocytes are the more numerous and function as part of the immune system. Monocytes function like neutrophils and participate in immune responses. Lymphocytes and monocytes are discussed in Chapter 15.
Age Changes in Blood
The total amount of blood per unit of body mass and the relative amounts of plasma and cellular components remain constant regardless of age. Though some of the reserve capacity of the bone marrow to produce blood cells and platelets declines with aging, the marrow always retains enough power to supply as many blood cells and platelets as needed. Information about aging and blood components follows.
Plasma
Negligible changes occur in the chemical composition of plasma, though there is an increase in certain waste products (e.g., urea, creatinine). Increases in these wastes are probably due to the decline in the ability of the kidney to remove them from the blood.
There is an age-related increase in the viscosity or "thickness" of blood. Reasons for the increased viscosity include an increase in clotting factors and broken fibrin strands; elevated norepinephrine, which promotes clot formation; and stiffening of RBCs, especially in blood with high blood cholesterol. Certain clotting factors increase dramatically at menopause, causing a rapid rise in blood viscosity. Other factors that increase blood viscosity include reduced blood oxygen; inadequate exercise; stress; and smoking, including secondhand smoke. These factors can be reduced or eliminated. Effects from higher blood viscosity include slower blood flow, increased risk of clot formation, and more rapid development of atherosclerosis.
Red Blood Cells
No substantial changes occur in RBCs, though there are some indications of a decrease in the concentration of hemoglobin in men over age 65. Overall, however, aging causes no changes in the ability of the RBCs to function.
Platelets
The number of platelets circulating in the blood remains essentially unchanged, and the platelets retain the ability to initiate clot formation. An age‑related increase in the tendency of platelets to clump together may cause a slight increase in the risk of thrombus formation.
White Blood Cells
Age changes in PMNs include decreases in the number and rate of release of stored cells, rate of movement, ability to be chemically attracted to areas, and proportion of cells capable of performing phagocytosis. The number of PMNs capable of performing phagocytosis seems to decline especially rapidly after age 60. The net effect of age changes in PMNs is a decrease in their ability to defend the body against infection, which helps explain the age‑related increase in susceptibility to infections in areas such as the respiratory, urinary, and integumentary systems.
Little has been reported on age changes in monocytes that circulate in the blood. Age changes in lymphocytes are discussed in Chapter 15.

