8.2: Dietary Guidelines- Foods and Food Components to Reduce
- Page ID
- 39002
The Dietary Guidelines for Americans provides science-based advice to promote health and reduce the risk of major chronic diseases through diet and physical activity. Currently, very few Americans consume diets that meet Dietary Guideline recommendations. This chapter focuses on certain foods and food components that are consumed in excessive amounts and may increase the risk of certain chronic diseases. These include sodium, solid fats (major sources of saturated and trans fatty acids), added sugars, and refined grains. These food components are consumed in excess by children, adolescents, adults, and older adults. In addition, the diets of most men exceed the recommendation for cholesterol. Some people also consume too much alcohol.
This excessive intake replaces nutrient-dense forms of foods in the diet, making it difficult for people to achieve recommended nutrient intake and control calorie intake. Many Americans are overweight or obese, and are at higher risk of chronic diseases, such as cardiovascular disease, diabetes, and certain types of cancer. Even in the absence of overweight or obesity, consuming too much sodium, solid fats, saturated and trans fatty acids, cholesterol, added sugars, and alcohol increases the risk of some of the most common chronic diseases in the United States. Discussing solid fats in addition to saturated and trans fatty acids is important because, apart from the effects of saturated and trans fatty acids on cardiovascular disease risk, solid fats are abundant in the diets of Americans and contribute significantly to excess calorie intake. The recommendations in this chapter are based on evidence that eating less of these foods and food components can help Americans meet their nutritional needs within appropriate calorie levels, as well as help reduce chronic disease risk.
Key Recommendations
- Reduce daily sodium intake to less than 2,300 milligrams (mg) and further reduce intake
to 1,500 mg among persons who are 51 and older and those of any age who are African American or have hypertension, diabetes, or chronic kidney disease. The 1,500 mg recommendation applies to about half of the U.S. population, including children, and the majority of adults. - Consume less than 10 percent of calories from saturated fatty acids by replacing them with monounsaturated and polyunsaturated fatty acids.
- Consume less than 300 mg per day of dietary cholesterol.
- Keep trans fatty acid consumption as low as possible, especially by limiting foods that contain synthetic sources of trans fats, such as partially hydrogenated oils, and by limiting other solid fats.
- Reduce the intake of calories from solid fats and added sugars.
- Limit the consumption of foods that contain refined grains, especially refined grain foods that contain solid fats, added sugars, and sodium.
- If alcohol is consumed, it should be consumed in moderation—up to one drink per day for women and two drinks per day for men—and only by adults of legal drinking age.
Supporting the Recommendations
The following sections expand on the recommendations and review the evidence supporting the health risks associated with greater intake of foods that are high in sodium, solid fats, added sugars, and refined grains, and excessive alcohol consumption. An important underlying principle is the need to control calorie intake to manage body weight and limit the intake of food components that increase the risk of certain chronic diseases. This goal can be achieved by consuming fewer foods that are high in sodium, solid fats, added sugars, and refined grains and, for those who drink, consuming alcohol in moderation.
How is an alcoholic drink defined? One drink is defined as 12 fluid ounces of regular beer (5% alcohol), 5 fluid ounces of wine (12% alcohol), or 1.5 fluid ounces of 80 proof (40% alcohol) distilled spirits. One drink contains 0.6 fluid ounces of alcohol.
Sodium
Sodium is an essential nutrient and is needed by the body in relatively small quantities, provided that substantial sweating does not occur. On average, the higher an individual’s sodium intake, the higher the individual’s blood pressure. A strong body of evidence in adults documents that as sodium intake decreases, so does blood pressure. Moderate evidence in children also has documented that as sodium intake decreases, so does blood pressure. Keeping blood pressure in the normal range reduces an individual’s risk of cardiovascular disease, congestive heart failure, and kidney disease. Therefore, adults and children should limit their intake of sodium.
Virtually all Americans consume more sodium than they need. The estimated average intake of sodium for all Americans ages 2 years and older is approximately 3,400 mg per day (Figure 1).
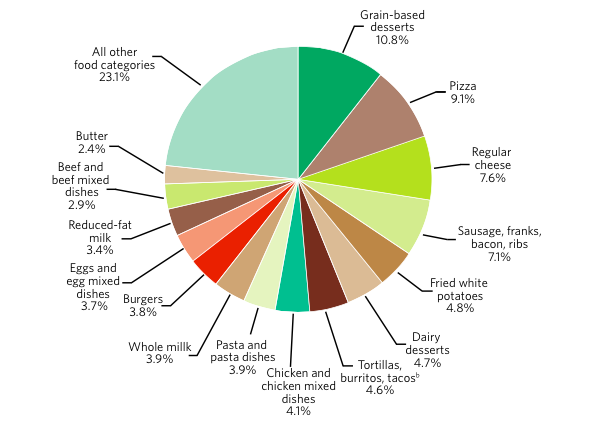
Sodium is primarily consumed as salt (sodium chloride). As a food ingredient, salt has multiple uses, such as in curing meat, baking, masking off- flavors, retaining moisture, and enhancing flavor (including the flavor of other ingredients). Salt added at the table and in cooking provides only a small proportion of the total sodium that Americans consume. Most sodium comes from salt added during food processing. Many types of processed foods contribute to the high intake of sodium (Figure 2).
Some sodium-containing foods are high in sodium, but the problem of excess sodium intake also is due to frequent consumption of foods that contain lower amounts of sodium, such as yeast breads41 (which contribute 7% of the sodium in the U.S. diet). Other sources of sodium include chicken and chicken mixed dishes42 (7% of sodium intake), pizza (6%), and pasta and pasta dishes43 (5%). Some of the sources discussed here and in the following sections contain larger varieties of foods than others (e.g., chicken and chicken mixed dishes). Therefore, some of these sources include foods that can be purchased or prepared to be lower in sodium, as well as lower in other food components recommended to be reduced. For example, chicken naturally contains little sodium. Chicken and chicken mixed dishes can be prepared by purchasing chicken that has not had sodium added to it and by not adding salt or ingredients containing sodium.

a. 2,300 mg/day is the Tolerable Upper Intake Level (UL) for sodium intake in adults set by the Institute of Medicine (IOM). For children younger than age 14 years, the UL is less than 2,300 mg/day.
b. 1,500 mg/day is the Adequate Intake (AI) for individuals ages 9 years and older.
Source: U.S. Department of Agriculture, Agricultural Research Service and U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. What We Eat In America, NHANES 2005–2006. http://www.ars.usda.gov/Services/docs.htm?docid=13793. Accessed August 11, 2010.
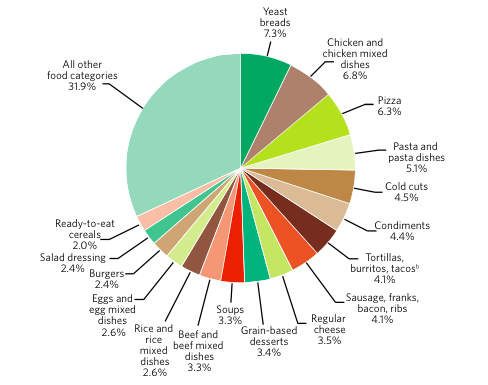
a. Data are drawn from analyses of usual dietary intake conducted by the National Cancer Institute. Foods and beverages consumed were divided into 97 categories and ranked according to sodium contribution to the diet. “All other food categories” represents food categories that each contributes less than 2% of the total intake of sodium from foods.
b. Also includes nachos, quesadillas, and other Mexican mixed dishes.
Source: National Cancer Institute. Sources of Sodium in the Diets of the U.S. Population Ages 2 Years and Older, NHANES 2005–2006. Risk Factor Monitoring and Methods, Cancer Control and Population Sciences. riskfactor.cancer.gov/diet/fo...m/table1a.html. Accessed August 11, 2010.
Americans can reduce their consumption of sodium in a variety of ways:
- Read the Nutrition Facts label for information on the sodium content of foods and purchase foods that are low in sodium.
- Consume more fresh foods and fewer processed foods that are high in sodium.
- Eat more home-prepared foods, where you have more control over sodium, and use little or no salt or salt-containing seasonings when cooking or eating foods.
- When eating at restaurants, ask that salt not be added to your food or order lower sodium options, if available.
Sodium is found in a wide variety of foods, and calorie intake is associated with sodium intake (i.e., the more foods and beverages people consume, the more sodium they tend to consume). Therefore, reducing calorie intake can help reduce sodium intake, thereby contributing to the health benefits that occur with lowering sodium intake.
Because a Recommended Dietary Allowance for sodium could not be determined, the Institute of Medicine (IOM)44 set Adequate Intake (AI) levels for this nutrient. The AI is the recommended daily average intake level of a nutrient, and usual intakes at or above the AI have a low probability of inadequacy. The sodium AI is based on the amount that is needed to meet the sodium needs of healthy and moderately active individuals.45 It covers sodium sweat losses in unacclimatized individuals who are exposed to high temperatures or who become physically active, and ensures that recommended intake levels for other nutrients can be met. The sodium AI for individuals ages 9 to 50 years is 1,500 mg per day. Lower sodium AIs were established for children and older adults (ages 1 to 3 years: 1,000 mg/day; ages 4 to 8 years: 1,200 mg/day; ages 51 to 70 years: 1,300 mg/ day; ages 71 years and older: 1,200 mg/day) because their calorie requirements are lower.
 For adolescents and adults of all ages (14 years and older), the IOM set the Tolerable Upper Intake Level (UL) at 2,300 mg per day. The UL is the highest daily nutrient intake level that is likely to pose no risk of adverse health effects (e.g., for sodium, increased blood pressure) to almost all individuals in the general population. The IOM recognized that the association between sodium intake and blood pressure was continuous and without a threshold (i.e., a level below which the association no longer exists). The UL was based on several trials, including data from the Dietary Approaches to Stop Hypertension (DASH)-Sodium trial. The IOM noted that in the DASH-Sodium trial, blood pressure was lowered when target sodium intake was reduced to 2,300 mg per day, and lowered even further when sodium was targeted to the level of 1,200 mg per day.46 An intake level of 2,300 mg per day was commonly the next level above the AI of 1,500 mg per day that was tested in the sodium trials evaluated by the IOM.
For adolescents and adults of all ages (14 years and older), the IOM set the Tolerable Upper Intake Level (UL) at 2,300 mg per day. The UL is the highest daily nutrient intake level that is likely to pose no risk of adverse health effects (e.g., for sodium, increased blood pressure) to almost all individuals in the general population. The IOM recognized that the association between sodium intake and blood pressure was continuous and without a threshold (i.e., a level below which the association no longer exists). The UL was based on several trials, including data from the Dietary Approaches to Stop Hypertension (DASH)-Sodium trial. The IOM noted that in the DASH-Sodium trial, blood pressure was lowered when target sodium intake was reduced to 2,300 mg per day, and lowered even further when sodium was targeted to the level of 1,200 mg per day.46 An intake level of 2,300 mg per day was commonly the next level above the AI of 1,500 mg per day that was tested in the sodium trials evaluated by the IOM.
The DASH studies demonstrated that the total eating pattern, including sodium and a number of other nutrients and foods, affects blood pressure. In the original DASH trial, the DASH diet47 resulted in a significant reduction in blood pressure compared to the control diet, which was typical of what many Americans consume. In the DASH-Sodium trial, blood pressure levels declined with reduced sodium intake for those who consumed either the DASH or control diet. However, blood pressure declined most for those who both consumed the DASH diet and reduced their sodium intake.
Americans should reduce their sodium intake to less than 2,300 mg or 1,500 mg per day depending on age and other individual characteristics. African Americans, individuals with hypertension, diabetes, or chronic kidney disease and individuals ages 51 and older, comprise about half of the U.S. population ages 2 and older. While nearly everyone benefits from reducing their sodium intake, the blood pressure of these individuals tends to be even more responsive to the blood pressure-raising effects of sodium than others; therefore, they should reduce their intake to 1,500 mg per day. Additional dietary modifications may be needed for people of all ages with hypertension, diabetes, or chronic kidney disease, and they are advised to consult a health care professional. Given the current U.S. marketplace and the resulting excessive high sodium intake, it is challenging to meet even the less than 2,300 mg recommendation—fewer than 15 percent of Americans do so currently. An immediate, deliberate reduction in the sodium content of foods in the marketplace is necessary to allow consumers to reduce sodium intake to less than 2,300 mg or 1,500 mg per day now.
Fats
Dietary fats are found in both plant and animal foods. Fats supply calories and essential fatty acids, and help in the absorption of the fat-soluble vitamins A, D, E, and K. The IOM established acceptable ranges for total fat intake for children and adults (children ages 1 to 3 years: 30–40% of calories; children and adolescents ages 4 to 18 years: 25–35%; adults ages 19 years and older: 20–35%) (see Table 2-4). These ranges are associated with reduced risk of chronic diseases, such as cardiovascular disease, while providing for adequate intake of essential nutrients. Total fat intake should fall within these ranges.
Fatty acids are categorized as being saturated, monounsaturated, or polyunsaturated. Fats contain a mixture of these different kinds of fatty acids. Trans fatty acids are unsaturated fatty acids. However, they are structurally different from the predominant unsaturated fatty acids that occur naturally in plant foods and have dissimilar health effects.
The types of fatty acids consumed are more important in influencing the risk of cardiovascular disease than is the total amount of fat in the diet. Animal fats tend to have a higher proportion of saturated fatty acids (seafood being the major exception), and plant foods tend to have a higher proportion of monounsaturated and/or polyunsaturated fatty acids (coconut oil, palm kernel oil, and palm oil being the exceptions) (Figure 3).
Most fats with a high percentage of saturated or trans fatty acids are solid at room temperature and are referred to as “solid fats,” while those with more unsaturated fatty acids are usually liquid at room temperature and are referred to as “oils.” Solid fats are found in most animal foods but also can be made from vegetable oils through the process of hydrogenation, as described below.
Despite longstanding recommendations on total fat, saturated fatty acids, and cholesterol, intakes of these fats have changed little from 1990 through 2005– 2006, the latest time period for which estimates are available. Total fat intake contributes an average of 34 percent of calories. The following sections provide details on types of fat to limit in the diet.
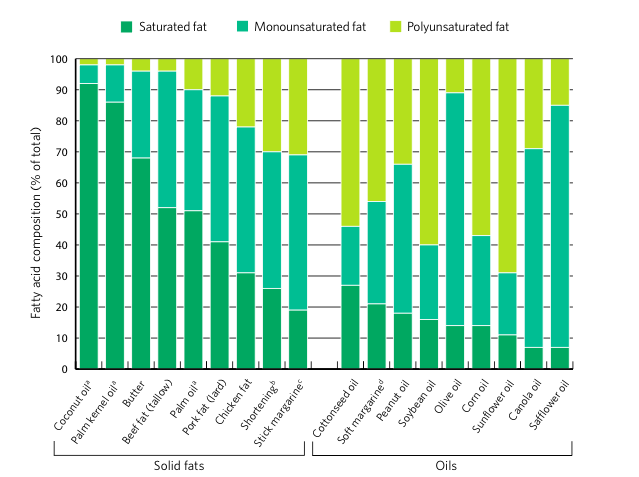
a. Coconut oil, palm kernel oil, and palm oil are called oils because they come from plants. However, they are semi-solid at room temperature due to their high content of short-chain saturated fatty acids. They are considered solid fats for nutritional purposes.
b. Partially hydrogenated vegetable oil shortening, which contains trans fats. c. Most stick margarines contain partially hydrogenated vegetable oil, a source of trans fats.
d. The primary ingredient in soft margarine with no trans fats is liquid vegetable oil.
Source: U.S. Department of Agriculture, Agricultural Research Service, Nutrient Data Laboratory. USDA National Nutrient Database for Standard Reference, Release 22, 2009. Available at www.ars.usda.gov/ba/ bhnrc/ndl. Accessed July 19, 2010.
Saturated fatty acids
The body uses some saturated fatty acids for physiological and structural functions, but it makes more than enough to meet those needs. People therefore have no dietary requirement for saturated fatty acids. A strong body of evidence indicates that higher intake of most dietary saturated fatty acids is associated with higher levels of blood total cholesterol and low-density lipoprotein (LDL) cholesterol. Higher total and LDL cholesterol levels are risk factors for cardiovascular disease.
Consuming less than 10 percent of calories from saturated fatty acids and replacing them with monounsaturated and/or polyunsaturated fatty acids is associated with low blood cholesterol levels, and therefore a lower risk of cardiovascular disease. Lowering the percentage of calories from dietary saturated fatty acids even more, to 7 percent of calories, can further reduce the risk of cardiovascular disease. Saturated fatty acids contribute an average of 11 percent of calories to the diet, which is higher than recommended. Major sources of saturated fatty acids in the American diet include regular (full-fat) cheese (9% of total saturated fat intake); pizza (6%); grain-based desserts48 (6%); dairy-based desserts49 (6%); chicken and chicken mixed dishes (6%); and sausage, franks, bacon, and ribs (5%) (Figure 3).
 To reduce the intake of saturated fatty acids, many Americans should limit their consumption of the major sources that are high in saturated fatty acids and replace them with foods that are rich in mono-unsaturated and polyunsaturated fatty acids. For example, when preparing foods at home, solid fats (e.g., butter and lard) can be replaced with vegetable oils that are rich in monounsaturated and polyunsaturated fatty acids (Figure 3). In addition, many of the major food sources of saturated fatty acids can be purchased or prepared in ways that help reduce the consumption of saturated fatty acids (e.g., purchasing fat-free or low-fat milk, trimming fat from meat). Oils that are rich in monounsaturated fatty acids include canola, olive, and safflower oils. Oils that are good sources of polyunsaturated fatty acids include soybean, corn, and cottonseed oils.
To reduce the intake of saturated fatty acids, many Americans should limit their consumption of the major sources that are high in saturated fatty acids and replace them with foods that are rich in mono-unsaturated and polyunsaturated fatty acids. For example, when preparing foods at home, solid fats (e.g., butter and lard) can be replaced with vegetable oils that are rich in monounsaturated and polyunsaturated fatty acids (Figure 3). In addition, many of the major food sources of saturated fatty acids can be purchased or prepared in ways that help reduce the consumption of saturated fatty acids (e.g., purchasing fat-free or low-fat milk, trimming fat from meat). Oils that are rich in monounsaturated fatty acids include canola, olive, and safflower oils. Oils that are good sources of polyunsaturated fatty acids include soybean, corn, and cottonseed oils.
Trans fatty acids
Trans fatty acids are found naturally in some foods and are formed during food processing; they are not essential in the diet. A number of studies have observed an association between increased trans fatty acid intake and increased risk of cardiovascular disease. This increased risk is due, in part, to its LDL cholesterol-raising effect. Therefore, Americans should keep their intake of trans fatty acids as low as possible.
Some trans fatty acids that Americans consume are produced by a process referred to as hydrogenation. Hydrogenation is used by food manufacturers to make products containing unsaturated fatty acids solid at room temperature (i.e., more saturated)
and therefore more resistant to becoming spoiled or rancid. Partial hydrogenation means that some, but not all, unsaturated fatty acids are converted to saturated fatty acids; some of the unsaturated fatty acids are changed from a cis to trans configuration. Trans fatty acids produced this way are referred to as “synthetic” or “industrial” trans fatty acids. Synthetic trans fatty acids are found in the partially hydrogenated oils used in some margarines, snack foods, and prepared desserts as a replacement for saturated fatty acids. Trans fatty acids also are produced by grazing animals, and small quantities are therefore found in meat and milk products.50 These are called “natural” or “ruminant” trans fatty acids. There is limited evidence to conclude whether synthetic and natural trans fatty acids differ in their metabolic effects and health outcomes. Overall, synthetic trans fatty acid levels in the U.S. food supply have decreased dramatically since 2006 when the declaration of the amount of trans fatty acids on the Nutrition Facts label became mandatory. Consuming fat-free or low-fat milk and milk products and lean meats and poultry will reduce the intake of natural trans fatty acids. Because natural trans fatty acids are present in meat, milk, and milk products,50 their elimination is not recommended because this could have potential implications for nutrient adequacy.
Cholesterol
The body uses cholesterol for physiological and structural functions, but it makes more than enough for these purposes. Therefore, people do not need to eat sources of dietary cholesterol. Cholesterol is found only in animal foods. The major sources of cholesterol in the American diet include eggs and egg mixed dishes (25% of total cholesterol intake),51 chicken and chicken mixed dishes (12%), beef and beef mixed dishes (6%), and all types of beef burgers (5%).52 Cholesterol intake can be reduced by limiting the consumption of the specific foods that are high in cholesterol. Many of these major sources include foods that can be purchased or prepared in ways that limit the intake of cholesterol (e.g., using egg substitutes). Cholesterol intake by men averages about 350 mg per day, which exceeds the recommended level of less than 300 mg per day. Average cholesterol intake by women is 240 mg per day.
Dietary cholesterol has been shown to raise blood LDL cholesterol levels in some individuals. However, this effect is reduced when saturated fatty acid intake is low, and the potential negative effects of dietary cholesterol are relatively small compared to those of saturated and trans fatty acids. Moderate evidence shows a relationship between higher intake of cholesterol and higher risk of cardiovascular disease. Independent of other dietary factors, evidence suggests that one egg (i.e., egg yolk) per day does not result in increased blood cholesterol levels, nor does it increase the risk of cardiovascular disease in healthy people. Consuming less than 300 mg per day of cholesterol can help maintain normal blood cholesterol levels. Consuming less than 200 mg per day can further help individuals at high risk of cardiovascular disease.
a. Data are drawn from analyses of usual dietary intake conducted by the National Cancer Institute. Foods and beverages consumed were divided into 97 categories and ranked according to the saturated fat contribution to the diet. “All other food categories” represents food categories that each contributes less than 2% of the total saturated fat intake.
b. Also includes nachos, quesadillas, and other Mexican mixed dishes.
Source: National Cancer Institute. Sources of saturated fat in the diets of the U.S. population ages 2 years and older, NHANES 2005–2006. Risk Factor Monitoring and Methods. Cancer Control and Population Sciences. riskfactor.cancer.gov/diet/fo...at_fat/sf.html. Accessed August 11, 2010.
Calories from Solid Fats and Added Sugars
Solid fats
As noted previously, fats contain a mixture of different fatty acids, and much research has been conducted on the association between the intake
of saturated and trans fatty acids and the risk of chronic disease, especially cardiovascular disease. Most fats with a high percentage of saturated and/ or trans fatty acids are solid at room temperature and are referred to as “solid fats” (Figure 4). Common solid fats include butter, beef fat (tallow, suet), chicken fat, pork fat (lard), stick margarine, and shortening. The fat in fluid milk also is considered to be solid fat; milk fat (butter) is solid at room temperature but is suspended in fluid milk by the process of homogenization.
Although saturated and trans fatty acids are components of many foods, solid fats are foods themselves or ingredients (e.g., shortening in a cake or hydrogenated oils in fried foods). The purpose for discussing solid fats in addition to saturated and trans fatty acids is that, apart from the effects of saturated and trans fatty acids on cardiovascular disease risk, solid fats are abundant in the diets of Americans and contribute significantly to excess calorie intake.
Solid fats contribute an average of 19 percent of the total calories in American diets, but few essential nutrients and no dietary fiber. Some major food sources of solid fats in the American diet are grain-based desserts (11% of all solid fat intake); pizza (9%); regular (full-fat) cheese (8%); sausage, franks, bacon, and ribs (7%); and fried white potatoes (5%) (Figure 5).
In addition to being a major contributor of solid fats, moderate evidence suggests an association between the increased intake of processed meats (e.g., franks, sausage, and bacon) and increased risk of colorectal cancer and cardiovascular disease.53 To reduce the intake of solid fats, most Americans should limit their intake of those sources that are high in solid fats and/ or replace them with alternatives that are low in solid fats (e.g., fat-free milk). Reducing these sources of excess solid fats in the diet will result in reduced intake of saturated fatty acids, trans fatty acids, and calories.
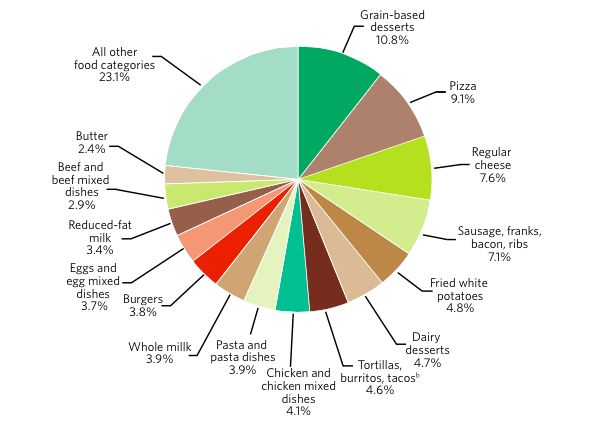
a. Data are drawn from analyses of usual dietary intake conducted by the National Cancer Institute. Foods and beverages consumed were divided into 97 categories and ranked according to solid fat contribution to the diet. “All other food categories” represents food categories that each contributes less than 2% of the total solid fat intake.
b. Also includes nachos, quesadillas, and other Mexican mixed dishes.
Source: National Cancer Institute. Sources of solid fats in the diets of U.S. population ages 2 years and older, NHANES 2003-2004. Risk Factor Monitoring and Methods. Cancer Control and Population Sciences. riskfactor.cancer.gov/diet/fo...ps/table3.html. Accessed August 11, 2010.
Added sugars
Sugars are found naturally in fruits (fructose) and fluid milk and milk products (lactose). The majority of sugars in typical American diets are sugars added to foods during processing, preparation, or at the table. These “added sugars” sweeten the flavor of foods and beverages and improve their palatability. They also are added to foods for preservation purposes and to provide functional attributes, such as viscosity, texture, body, and browning capacity.
Although the body’s response to sugars does not depend on whether they are naturally present in food or added to foods, sugars found naturally in foods are part of the food’s total package of nutrients and other healthful components. In contrast, many foods that contain added sugars often supply calories, but few or no essential nutrients and no dietary fiber. Both naturally occurring sugars and added sugars increase the risk of dental caries.
Added sugars contribute an average of 16 percent of the total calories in American diets. Added sugars include high fructose corn syrup, white sugar, brown sugar, corn syrup, corn syrup solids, raw sugar, malt syrup, maple syrup, pancake syrup, fructose sweetener, liquid fructose, honey, molasses, anhydrous dextrose, and crystal dextrose.
As a percent of calories from total added sugars, the major sources of added sugars in the diets of Americans are soda, energy drinks, and sports drinks (36% of added sugar intake), grain-based desserts (13%), sugar-sweetened fruit drinks54 (10%), dairy-based desserts (6%), and candy (6%) (Figure 6).
Reducing the consumption of these sources of added sugars will lower the calorie content of the diet, without compromising its nutrient adequacy. Sweetened foods and beverages can be replaced with those that have no or are low in added sugars. For example, sweetened beverages can be replaced with water and unsweetened beverages.
Why calories from solid fats and added sugars are a particular concern
Solid fats and added sugars are consumed in excessive amounts, and their intake should be limited. Together, they contribute a substantial portion of the calories consumed by Americans—35 percent on average, or nearly 800 calories per day—without contributing importantly to overall nutrient adequacy of the diet. Moreover, they have implications for weight management. Foods containing solid fats and added sugars are no more likely to contribute to weight gain than any other source of calories in an eating pattern that is within calorie limits. However, as the amount of solid fats and/or added sugars increases in the diet, it becomes more difficult to also eat foods with sufficient dietary fiber and essential vitamins and minerals, and still stay within calorie limits. For most people, no more than about 5 to 15 percent of calories from solid fats and added sugars can be reasonably accommodated in the USDA Food Patterns, which are designed to meet nutrient needs within calorie limits.
Reducing the consumption of solid fats and added sugars allows for increased intake of nutrient-dense foods without exceeding overall calorie needs. Because solid fats and added sugars are added to foods and beverages by manufacturers and by consumers at home, Americans can reduce their consumption of these food components in a variety of ways:
- Focus on eating the most nutrient-dense forms of foods from all food groups.
- Limit the amount of solid fats and added sugars when cooking or eating (e.g., trimming fat from meat, using less butter and stick margarine, and using less table sugar).
- Consume fewer and smaller portions of foods and beverages that contain solid fats and/or added sugars, such as grain-based desserts, sodas, and other sugar-sweetened beverages.
a. Data are drawn from analyses of usual dietary intake conducted by the National Cancer Institute. Foods and beverages consumed were divided into 97 categories and ranked according to added sugars contribution to the diet. “All other food categories” represents food categories that each contributes less than 2% of the total added sugar intake.
Source: National Cancer Institute. Sources of added sugars in the diets
of the U.S. population ages 2 years and older, NHANES 2005–2006. Risk Factor Monitoring and Methods. Cancer Control and Population Sciences. riskfactor.cancer.gov/diet/fo...sugars/table5a. html. Accessed August 11, 2010.
refined grains
The Food Label: A Useful Tool
The Nutrition Facts label provides information on the amount of calories; beneficial nutrients, such as dietary fiber and calcium; as well as the amount of certain food components that should be limited in the diet, including saturated fat, trans fat, cholesterol, and sodium.
The ingredients list can be used to find out whether a food or beverage contains solid fats, added sugars, whole grains, and refined grains.
The refining of whole grains involves a process that results in the loss of vitamins, minerals, and dietary fiber. Most refined grains are enriched with iron, thiamin, riboflavin, niacin, and folic acid before being further used as ingredients in foods. This returns some, but not all, of the vitamins and minerals that were removed during the refining process.55 Dietary fiber and some vitamins and minerals that are present in whole grains are not routinely added back to refined grains. Unlike solid fats and added sugars, enriched refined grain products have a positive role in providing some vitamins and minerals. However, when consumed beyond recommended levels, they commonly provide excess calories, especially because many refined grain products also are high in solid fats and added sugars (e.g., cookies and cakes).
On average, Americans consume 6.3 ounce-equivalents of refined grains per day.56 At the 2,000-calorie level of the USDA Food Patterns, the recommended amount of refined grains is no more than 3 ounce- equivalents per day. Refined grains should be replaced with whole grains, such that at least half of all grains eaten are whole grains. Consumption of refined grain products that also are high in solid fats and/or added sugars, such as cakes, cookies, donuts, and other desserts, should be reduced. Major sources of refined grains in the diets of Americans are yeast breads (26% of total refined grain intake); pizza (11%); grain-based desserts (10%); and tortillas, burritos, and tacos (8%) (Figure 7).
Alcohol
In the United States, approximately 50 percent of adults are current regular drinkers and 14 percent are current infrequent drinkers. An estimated
9 percent of men consume an average of more than two drinks per day and 4 percent of women consume an average of more than one drink per day. Of those who drink, about 29 percent of U.S. adult drinkers report binge drinking within the past month, usually on multiple occasions. This results in about 1.5 billion episodes of binge drinking in the United States each year.
The consumption of alcohol can have beneficial or harmful effects, depending on the amount consumed, age, and other characteristics of the person consuming the alcohol. Alcohol consumption may have beneficial effects when consumed in moderation. Strong evidence from observational studies has shown that moderate alcohol consumption is associated with a lower risk of cardiovascular disease. Moderate alcohol consumption also is associated with reduced risk of all-cause mortality among middle-aged and older adults and may help to keep cognitive function intact with age. However, it is not recommended that anyone begin drinking or drink more frequently on the basis of potential health benefits because moderate alcohol intake also is associated with increased risk of breast cancer, violence, drowning, and injuries from falls and motor vehicle crashes.
Because of the substantial evidence clearly demonstrating the health benefits of breastfeeding, occasionally consuming an alcoholic drink does not warrant stopping breastfeeding. However, breastfeeding women should be very cautious about drinking alcohol, if they choose to drink at all. If the infant’s breastfeeding behavior is well established, consistent, and predictable (no earlier than at 3 months of age), a mother may consume a single alcoholic drink if she then waits at least 4 hours before breastfeeding. Alternatively, she may express breast milk before consuming the drink and feed the expressed milk to her infant later.
Excessive (i.e., heavy, high-risk, or binge) drinking has no benefits, and the hazards of heavy alcohol intake are well known. Excessive drinking increases the risk of cirrhosis of the liver, hypertension, stroke, type 2 diabetes, cancer of the upper gastrointestinal tract and colon, injury, and violence. Excessive drinking over time is associated with increased body weight and can impair short- and long-term cognitive function. For the growing percentage of the population with elevated blood pressure, reducing alcohol intake can effectively lower blood pressure, although this is most effective when paired with changes in diet and physical activity patterns. Excessive alcohol consumption is responsible for an average of 79,000 deaths in the United States each year. More than half of these deaths are due to binge drinking. Binge drinking also is associated with a wide range of other health and social problems, including sexually transmitted diseases, unintended pregnancy, and violent crime.
Key Definitions for Alcohol
What is moderate alcohol consumption?
Moderate alcohol consumption is defined as up to 1 drink per day for women and up to 2 drinks per day for men.
What is heavy or high-risk drinking?
Heavy or high-risk drinking is the consumption of more than 3 drinks on any day or more than 7 per week for women and more than 4 drinks on any day or more than 14 per week for men.
What is binge drinking?
Binge drinking is the consumption within 2 hours of 4 or more drinks for women and 5 or more drinks for men.
There are many circumstances in which people should not drink alcohol:
- Individuals who cannot restrict their drinking to moderate levels.
- Anyone younger than the legal drinking age. Besides being illegal, alcohol consumption increases the risk of drowning, car accidents, and traumatic injury, which are common causes of death in children and adolescents.
- Women who are pregnant or who may be pregnant. Drinking during pregnancy, especially in the first few months of pregnancy, may result in negative behavioral or neurological consequences in the offspring. No safe level of alcohol consumption during pregnancy has been established.
- Individuals taking prescription or over-the-counter medications that can interact with alcohol.
- Individuals with certain specific medical conditions (e.g., liver disease, hypertriglyceridemia, pancreatitis).
- Individuals who plan to drive, operate machinery, or take part in other activities that require attention, skill, or coordination or in situations where impaired judgment could cause injury or death (e.g., swimming).
Chapter Summary
On average, American men, women, and children consume too much sodium, solid fats (the major source of saturated and trans fatty acids), added sugars, and refined grains. Men consume too much cholesterol, which also is found in some solid fats. In addition, some people consume too much alcohol.
Americans should follow the recommendations provided in this chapter to help achieve a dietary pattern that will meet their nutrient needs, control calorie intake, and help reduce the risk of certain chronic diseases. This goal can be achieved by consuming fewer foods high in sodium, solid fats, added sugars, and refined grains. For people who drink, alcohol should be consumed in moderation. It is not recommended that anyone begin drinking alcohol or drink more frequently on the basis of potential health benefits. The dietary patterns outlined in Chapter 5 can help Americans reduce their consumption of these foods, thereby meeting their nutrient needs within appropriate calorie levels. Appendix 4 discusses how food labels can help consumers evaluate and compare the nutritional content and/or ingredients of products, and assist them in purchasing foods that contain relatively lower amounts of certain undesirable nutrients and ingredients, such as sodium, saturated and trans fats, and added sugars.
[reveal-answer q=”891017″]Show References[/reveal-answer]
[hidden-answer a=”891017″]
41. Includes white bread or rolls, mixed-grain bread, flavored bread, whole-wheat bread or rolls, bagels, flat breads, croissants, and English muffins.
42. Includes fried or baked chicken parts and chicken strips/patties, chicken stir-fries, chicken casseroles, chicken sandwiches, chicken salads, stewed chicken, and other chicken mixed dishes.
43. Includes macaroni and cheese, spaghetti and other pasta with or without sauces, filled pastas (e.g., lasagna and ravioli), and noodles.
44. Institute of Medicine. Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate. Washington (DC): The National Academies Press; 2005.
45. Because of increased loss of sodium from sweat, the AI does not apply to highly active individuals and workers exposed to extreme heat stress.
46. The average achieved levels of sodium intake, as reflected by urinary sodium excretion, was 2,500 and 1,500 mg/day.
47. The DASH diet emphasized fruits, vegetables, and low-fat milk and milk products; included whole grains, poultry, fish, and nuts; and contained only small amounts of red meat, sweets, sugar-containing beverages, and decreased amounts of total and saturated fat and cholesterol.
48. Includes cakes, cookies, pies, cobblers, sweet rolls, pastries, and donuts.
49. Includes ice cream, frozen yogurt, sherbet, milk shakes, and pudding.
50. Milk and milk products also can be referred to as dairy products.
51. Includes scrambled eggs, omelets, fried eggs, egg breakfast sandwiches/biscuits, boiled and poached eggs, egg salad, deviled eggs, quiche, and egg substitutes.
52. Beef and beef mixed dishes and all types of beef burgers would collectively contribute 11% of total cholesterol intake.
53. The DGAC did not evaluate the components of processed meats that are associated with increased risk of colorectal cancer and cardiovascular disease.
54. Includes fruit-flavored drinks, fruit juice drinks, and fruit punch.
55. Folic acid is added to enriched refined grains to a level that doubles the amount lost during the refining process.
56. One ounce-equivalent of grain is 1 one-ounce slice bread; 1 ounce uncooked pasta or rice; 1⁄2 cup cooked rice, pasta, or cereal; 1 tortilla (6″ diameter); 1 pancake (5″ diameter); 1 ounce ready-to-eat cereal (about 1 cup cereal flakes).
[/hidden-answer]
- Image of salt and pepper shaker. Authored by: Matthias Ripp. Located at: https://flic.kr/p/ocvEBs. License: CC BY: Attribution
- Image of cooking oil. Authored by: Martin Cooper. Located at: https://flic.kr/p/qupHwL. License: CC BY: Attribution
- Lifetime Fitness and Wellness. Provided by: Extended Learning Institute of Northern Virginia Community College. Located at: https://eli.nvcc.edu/. License: CC BY: Attribution
- Chapter 3 Dietary Guidelines for Americans, 2010. Provided by: U.S. Department of Agriculture, U.S. Department of Health and Human Services. Located at: http://www.dietaryguidelines.gov. License: Public Domain: No Known Copyright

