3.3: Patient Risk Assessment
- Page ID
- 9997
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)To prevent and minimize MSI injuries related to patient handling activities, a risk assessment must be done to determine a patient’s ability to move, the need for assistance, and the most appropriate means of assistance (Provincial Health Services Authority [PHSA], 2010). There are four important areas to assess:
- The patient
- The environment
- The health care provider
- The organization of the work
Checklist 24 outlines what to assess and how to assess a patient prior to positioning, ambulation, and transfers.
Checklist 24: Risk AssessmentDisclaimer: Always review and follow your hospital policy regarding this specific skill. |
|||
Safety considerations:
|
|||
Steps |
Additional Considerations |
||
| 1. Assess your patient. | There are three areas to assess:
1. Is the patient cooperative and able to follow directions? Ask patient to squeeze your hands. Is the behaviour predictable (non-aggressive, fearful, or fatigued)? Is the patient able to follow directions with cues? If yes, proceed to next question. If no, use a mechanical lift for transfers and/or assistive devices for repositioning in bed if patient has some abilities. 2. Can the patient bear weight? Ask patient to lift buttocks off the bed (also known as “bridging”) and hold the position for 5 seconds. The health care provider may give cues on how to lift buttocks off the bed. 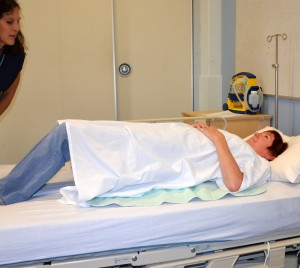
Bridging hips strength test After bridging, ask the patient to perform a straight leg raise by lifting one leg up off the bed and holding it for 5 seconds while the other leg is kept bent. Repeat with the opposite leg. 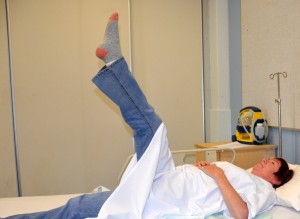
Leg lift strength test If yes, proceed to next question. If no, use an appropriate moving technique, such as a mechanical lift and/or assistive device, to transfer a non-weight-bearing patient. 3. Can the patient sit up on the side of the bed without support? Can the patient sit forward on a chair or the edge of the bed without support? 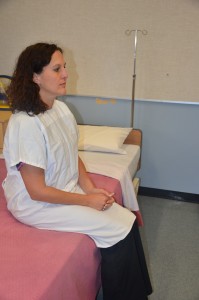
Sit unassisted on the bed If yes, decide on the amount of assist required (minimum, moderate, or maximum) according to your agency policy. If no, use a mechanical lift for transfers and/or an assistive device for repositioning if patient has some movement abilities. |
||
| 2. Assess your environment. | Is there adequate space?
Is available equipment in proper working order? Have all hazards been removed? |
||
| 3. Assess yourself and readiness to perform procedures. | Complete all required training according to health agency regulations.
Wear non-slip footwear. Maintain a neutral spine; do not twist or side bend, and use proper body mechanics when moving or positioning patients. Designate a leader if working in a team to mobilize or position a patient. Always use proper weight-shift techniques (side to side, front to back, and up and down). |
||
| 4. Assess your work organization. | Ensure adequate number of caregivers.
Ensure there is enough time to perform the procedure. Take rest breaks and vary activities to promote optimal back health. If patient is complex or bariatric, consult additional resources, seek assistance, and use assistive devices. |
||
| Data source: Interior Health, 2012; National Institute of Occupational Safety and Health, 2010; PHSA, 2010; WorkSafeBC, 2010 | |||
To help you assess and make decisions about moving a patient, refer to these two useful tools.
Critical Thinking Exercises
- A patient requires repositioning in bed. After your assessment, you determine the patient is cooperative and predictable, able to weight bear, but unable to sit up unassisted. What are your two options to reposition the patient?
- When assessing your abilities to perform a patient-handling procedure, what five things must you consider?
- Vision and hearing impairments, along with language barriers, are risk factors when performing patient-handling procedures. What additional risk factors should be considered?


