4: Screening and Assessment
- Page ID
- 16030
IN THIS CHAPTER
- Screening and Assessment
- Barriers and Challenges to Trauma -Informed Screening and Assessment
- Cross-Cultural Screening and Assessment
- Choosing Instruments
- Trauma-Informed Screening and Assessment
- Concluding Note
Why screen universally for trauma in behavioral health services? Exposure to trauma is common; in many surveys, more than half of respondents report a history of trauma, and the rates are even higher among clients with mental or substance use disorders. Furthermore, behavioral health problems, including substance use and mental disorders, are more difficult to treat if trauma-related symptoms and disorders aren’t detected early and treated effectively (Part 3, Section 1, of this Treatment Improvement Protocol [TIP], available online, summarizes research on the prevalence of trauma and its relationship with other behavioral health problems).
Not addressing traumatic stress symptoms, trauma-specific disorders, and other symptoms/disorders related to trauma can impede successful mental health and substance abuse treatment. Unrecognized, unaddressed trauma symptoms can lead to poor engagement in treatment, premature termination, greater risk for relapse of psychological symptoms or substance use, and worse outcomes. Screening can also prevent misdiagnosis and inappropriate treatment planning. People with histories of trauma often display symptoms that meet criteria for other disorders.
Without screening, clients’ trauma histories and related symptoms often go undetected, leading providers to direct services toward symptoms and disorders that may only partially explain client screening for trauma history and trauma-related symptoms can help behavioral health practitioners identify individuals at risk of developing more pervasive and severe symptoms of traumatic stress. Screening, early identification, and intervention serves as a prevention strategy.
Screening to identify clients who have histories of trauma and experience trauma-related symptoms is a prevention strategy.
The chapter begins with a discussion of screening and assessment concepts, with a particular focus on trauma-informed screening. It then highlights specific factors that influence screening and assessment, including timing and environment. Barriers and challenges in providing trauma-informed screening are discussed, along with culturally specific screening and assessment considerations and guidelines. Instrument selection, trauma-informed screening and assessment tools, and trauma-informed screening and assessment processes are reviewed as well. For a more research-oriented perspective on screening and assessment for traumatic stress disorders, please refer to the literature review provided in Part 3 of this TIP, which is available online.
Screening and Assessment
Screening
The first two steps in screening are to determine whether the person has a history of trauma and whether he or she has trauma-related symptoms. Screening mainly obtains answers to “yes” or “no” questions: “Has this client experienced a trauma in the past?” and “Does this client at this time warrant further assessment regarding trauma-related symptoms?” If someone acknowledges a trauma history, then further screening is necessary to determine whether trauma-related symptoms are present. However, the presence of such symptoms does not necessarily say anything about their severity, nor does a positive screen indicate that a disorder actually exists. Positive screens only indicate that assessment or further evaluation is warranted, and negative screens do not necessarily mean that an individual doesn’t have symptoms that warrant intervention.
Screening is often the first contact between the client and the treatment provider, and the client forms his or her first impression of treatment during this intake process. Thus, how screening is conducted can be as important as the actual information gathered, as it sets the tone of treatment and begins the relationship with the client.
Screening procedures should always define the steps to take after a positive or negative screening. That is, the screening process establishes precisely how to score responses to screening tools or questions and clearly defines what constitutes a positive score (called a “cut-off score”) for a particular potential problem. The screening procedures detail the actions to take after a client scores in the positive range. Clinical supervision is helpful—and sometimes necessary—in judging how to proceed.
Trauma-informed screening is an essential part of the intake evaluation and the treatment planning process, but it is not an end in itself. Screening processes can be developed that allow staff without advanced degrees or graduate-level training to conduct them, whereas assessments for trauma-related disorders require a mental health professional trained in assessment and evaluation processes. The most important domains to screen among individuals with trauma histories include:
-
Trauma-related symptoms.
-
Depressive or dissociative symptoms, sleep disturbances, and intrusive experiences.
-
Past and present mental disorders, including typically trauma-related disorders (e.g., mood disorders).
-
Severity or characteristics of a specific trauma type (e.g., forms of interpersonal violence, adverse childhood events, combat experiences).
-
Substance abuse.
-
Social support and coping styles.
-
Availability of resources.
-
Risks for self-harm, suicide, and violence.
-
Health screenings.
Assessment
When a client screens positive for substance abuse, trauma-related symptoms, or mental disorders, the agency or counselor should follow up with an assessment. A positive screening calls for more action—an assessment that determines and defines presenting struggles to develop an appropriate treatment plan and to make an informed and collaborative decision about treatment placement. Assessment determines the nature and extent of the client’s problems; it might require the client to respond to written questions, or it could involve a clinical interview by a mental health or substance abuse professional qualified to assess the client and arrive at a diagnosis. A clinical assessment delves into a client’s past and cu r-rent experiences, psychosocial and cultural history, and assets and resources.
Assessment protocols can require more than a single session to complete and should also use multiple avenues to obtain the necessary clinical information, including self-assessment tools, past and present clinical and medical records, structured clinical interviews, assessment measures, and collateral information from significant others, other behavioral health professionals, and agencies. Qualifications for conducting assessments and clinical interviews are more rigorous than for screening. Advanced degrees, licensing or certification, and special training in administration, scoring, and interpretation of specific assessment instruments and interviews are often required. Counselors must be familiar with (and obtain) the level of training required for any instruments they consider using.
Advice to Counselors: Screening and Assessing Clients
-
Ask all clients about any possible history of trauma; use a checklist to increase proper identification of such a history (see the online Adverse Childhood Experiences Study Score Calculator [http://acestudy.org/ace_score] for specific questions about adverse childhood experiences).
-
Use only validated instruments for screening and assessment.
-
Early in treatment, screen all clients who have histories of exposure to traumatic events for psychological symptoms and mental disorders related to trauma.
-
When clients screen positive, also screen for suicidal thoughts and behaviors (see TIP 50, Addressing Suicidal Thoughts and Behaviors in Substance Abuse Treatment; Center for Substance Abuse Treatment [CSAT], 2009a).
-
Do not delay screening; do not wait for a period of abstinence or stabilization of symptoms.
-
Be aware that some clients will not make the connection between trauma in their histories and their current patterns of behavior (e.g., alcohol and drug use and/or avoidant behavior).
-
Do not require clients to describe emotionally overwhelming traumatic events in detail.
-
Focus assessment on how trauma symptoms affect clients’ current functioning.
-
Consider using paper-and-pencil instruments for screening and assessment as well as self-report measures when appropriate; they are less threatening for some clients than a clinical interview.
-
Talk about how you will use the findings to plan the client’s treatment, and discuss any immediate action necessary, such as arranging for interpersonal support, referrals to community agencies, or moving directly into the active phase of treatment. It is helpful to explore the strategies clients have used in the past that have worked to relieve strong emotions (Fallot & Harris, 2001).
-
At the end of the session, make sure the client is grounded and safe before leaving the interview room (Litz, Miller, Ruef, & McTeague, 2002). Readiness to leave can be assessed by checking on the degree to which the client is conscious of the current environment, what the client’s plan is for maintaining personal safety, and what the client’s plans are for the rest of the day.
For people with histories of traumatic life events who screen positive for possible trauma-related symptoms and disorders, thorough assessment gathers all relevant information necessary to understand the role of the trauma in their lives; appropriate treatment objectives, goals, planning, and placement; and any ongoing diagnostic and treatment considerations, including reevaluation or follow-up.
Overall, assessment may indicate symptoms that meet diagnostic criteria for a substance use or mental disorder or a milder form of symptomatology that doesn’t reach a diagnostic level—or it may reveal that the positive screen was false and that there is no significant cause for concern. Information from an assessment is used to plan the client’s treatment.
The plan can include such domains as level of care, acute safety needs, diagnosis, disability, strengths and skills, support network, and cultural context. Assessments should reoccur throughout treatment. Ongoing assessment during treatment can provide valuable information by revealing further details of trauma history as clients’ trust in staff members grows and by gauging clients’ progress.
Timing of Screening and Assessment
As a trauma-informed counselor, you need to offer psychoeducation and support from the outset of service provision; this begins with explaining screening and assessment and with proper pacing of the initial intake and evaluation process. The client should understand the screening process, why the specific questions are important, and that he or she may choose to delay a response or to not answer a question at all. Discussing the occurrence or consequences of traumatic events can feel as unsafe and dangerous to the client as if the event were reoccurring. It is important not to encourage avoidance of the topic or reinforce the belief that discussing trauma-related material is dangerous, but be sensitive when gathering information in the initial screening. Initial questions about trauma should be general and gradual. Taking the time to prepare and explain the screening and assessment process to the client gives him or her a greater sense of control and safety over the assessment process.
Clients with substance use disorders
No screening or assessment of trauma should occur when the client is under the influence of alcohol or drugs. Clients under the influence are more likely to give inaccurate information. Although it’s likely that clients in an active phase of use (albeit not at the assessment itself ) or undergoing substance withdrawal can provide consistent information to obtain a valid screening and assessment, there is insufficient data to know for sure. Some theorists state that no final assessment of trauma or posttraumatic stress disorder (PTSD) should occur during these early phases (Read, Bollinger, & Sharkansky, 2003), asserting that symptoms of withdrawal can mimic PTSD and thus result in overdiagnosis of PTSD and other trauma-related disorders. Alcohol or drugs can also cause memory impairment that clouds the client’s history of trauma symptoms. However, Najavits (2004) and others note that underdiagnosis, not overdiagnosis, of trauma and PTSD has been a significant issue in the substance abuse field and thus claim that it is essential to obtain an initial assessment early, which can later be modified if needed (e.g., if the client’s symptom pattern changes). Indeed, clinical observations suggest that assessments for both trauma and PTSD— even during active use or withdrawal—appear robust (Coffey, Schumacher, Brady, & Dansky, 2003). Although some PTSD symptoms and trauma memories can be dampened or increased to a degree, their overall presence or absence, as assessed early in treatment, appears accurate (Najavits, 2004).
Conduct Assessments Throughout Treatment
Ongoing assessments let counselors:
-
Track changes in the presence, frequency, and intensity of symptoms.
-
Learn the relationships among the client’s trauma, presenting psychological symptoms, and substance abuse.
-
Adjust diagnoses and treatment plans as needed.
-
Select prevention strategies to avoid more pervasive traumatic stress symptoms.
The Setting for Trauma Screening and Assessment
Advances in the development of simple, brief, and public-domain screening tools mean that at least a basic screening for trauma can be done in almost any setting. Not only can clients be screened and assessed in behavioral health treatment settings; they can also be evaluated in the criminal justice system, educational settings, occupational settings, physicians’ offices, hospital medical and trauma units, and emergency rooms. Wherever they occur, trauma-related screenings and subsequent assessments can reduce or eliminate wasted resources, relapses, and, ultimately, treatment failures among clients who have histories of trauma, mental illness, and/or substance use disorders.
Creating an effective screening and assessment environment
You can greatly enhance the success of treatment by paying careful attention to how you approach the screening and assessment process. Take into account the following points:
-
Clarify for the client what to expect in the screening and assessment process. For example, tell the client that the screening and assessment phase focuses on identifying issues that might benefit from treatment. Inform him or her that during the trauma screening and assessment process, uncomfortable thoughts and feelings can arise. Provide reassurance that, if they do, you’ll assist in dealing with this distress—but also let them know that, even with your assistance, some psychological and physical reactions to the interview may last for a few hours or perhaps as long as a few days after the interview, and be sure to highlight the fact that such reactions are normal (Read et al., 2003).
-
Approach the client in a matter-of-fact, yet supportive, manner. Such an approach helps create an atmosphere of trust, respect, acceptance, and thoughtfulness (Melnick & Bassuk, 2000). Doing so helps to normalize symptoms and experiences generated by the trauma; consider informing clients that such events are common but can cause continued emotional distress if they are not treated. Clients may also find it helpful for you to explain the purpose of certain difficult questions. For example, you could say, “Many people have experienced troubling events as children, so some of my questions are about whether you experienced any such events while growing up.” Demonstrate kindness and directness in equal measure when screening/assessing clients (Najavits, 2004).
-
Respect the client’s personal space. Cultural and ethnic factors vary greatly regarding the appropriate physical distance to maintain during the interview. You should respect the client’s personal space, sitting neither too far from nor too close to the client; let your observations of the client’s comfort level during the screening and assessment process guide the amount of distance. Clients with trauma may have particular sensitivity about their bodies, personal space, and boundaries.
-
Adjust tone and volume of speech to suit the client’s level of engagement and degree of comfort in the interview process. Strive to maintain a soothing, quiet demeanor. Be sensitive to how the client might hear what you have to say in response to personal disclosures. Clients who have been traumatized may be more reactive even to benign or well-intended questions.
-
Provide culturally appropriate symbols of safety in the physical environment. These include paintings, posters, pottery, and other room decorations that symbolize the safety of the surroundings to the client population. Avoid culturally inappropriate or insensitive items in the physical environment.
-
Be aware of one’s own emotional responses to hearing clients’ trauma histories. Hearing about clients’ traumas may be very painful and can elicit strong emotions. The client may interpret your reaction to his or her revelations as disinterest, disgust for the client’s behavior, or some other inaccurate interpretation. It is important for you to monitor your interactions and to check in with the client as necessary. You may also feel emotionally drained to the point that it interferes with your ability to accurately listen to or assess clients. This effect of exposure to traumatic stories, known as secondary traumatization, can result in symptoms similar to those experienced by the client (e.g., nightmares, emotional numbing); if necessary, refer to a colleague for assessment (Valent, 2002). Secondary traumatization is addressed in greater detail in Part 2, Chapter 2, of this TIP.
-
Overcome linguistic barriers via an interpreter. Deciding when to add an interpreter requires careful judgment. The interpreter should be knowledgeable of behavioral health terminology, be familiar with the concepts and purposes of the interview and treatment programming, be unknown to the client, and be part of the treatment team. Avoid asking family members or friends of the client to serve as interpreters.
-
Elicit only the information necessary for determining a history of trauma and the possible existence and extent of traumatic stress symptoms and related disorders. There is no need to probe deeply into the details of a client’s traumatic experiences at this stage in the treatment process. Given the lack of a therapeutic relationship in which to process the information safely, pursuing details of trauma can cause retraumatization or produce a level of response that neither you nor your client is prepared to handle. Even if a client wants to tell his or her trauma story, it’s your job to serve as “gatekeeper” and preserve the client’s safety. Your tone of voice when suggesting postponement of a discussion of trauma is very important. Avoid conveying the message, “I really don’t want to hear about it.” Examples of appropriate statements are:
-
“Your life experiences are very important, but at this early point in our work together, we should start with what’s going on in your life currently rather than discussing past experiences in detail. If you feel that certain past experiences are having a big effect on your life now, it would be helpful for us to discuss them as long as we focus on your safety and recovery right now.”
-
“Talking about your past at this point could arouse intense feelings—even more than you might be aware of right now. Later, if you choose to, you can talk with your counselor about how to work on exploring your past.”
-
“Often, people who have a history of trauma want to move quickly into the details of the trauma to gain relief. I understand this desire, but my concern for you at this moment is to help you establish a sense of safety and support before moving into the traumatic experiences. We want to avoid retraumatization—meaning, we want to establish resources that weren’t available to you at the time of the trauma before delving into more content.”
-
-
Give the client as much personal control as possible during the assessment by:
-
Presenting a rationale for the interview and its stress-inducing potential, making clear that the client has the right to refuse to answer any and all questions.
-
Giving the client (where staffing permits) the option of being interviewed by someone of the gender with which he or she is most comfortable.
-
Postponing the interview if necessary (Fallot & Harris, 2001).
-
-
Use self-administered, written checklists rather than interviews when possible to assess trauma. Traumas can evoke shame, guilt, anger, or other intense feelings that can make it difficult for the client to report them aloud to an interviewer. Clients are more likely to report trauma when they use self-administered screening tools; however, these types of screening instruments only guide the next step. Interviews should coincide with self-administered tools to create a sense of safety for the client (someone is present as he or she completes the screening) and to follow up with more indepth data gathering after a self-administered screening is complete. The Trauma History Questionnaire (THQ) is a self-administered tool (Green, 1996). It has been used successfully with clinical and nonclinical populations, including medical patients, women who have experienced domestic violence, and people with serious mental illness (Hooper, Stockton, Krupnick, & Green, 2011). Screening instruments (including the THQ) are included in Appendix D of this TIP.
-
Interview the client if he or she has trouble reading or writing or is otherwise unable to complete a checklist. Clients who are likely to minimize their trauma when using a checklist (e.g., those who exhibit significant symptoms of dissociation or repression) benefit from a clinical interview. A trained interviewer can elicit information that a self-administered checklist does not capture. Overall, using both a self-administered questionnaire and an interview can help achieve greater clarity and context.
-
Allow time for the client to become calm and oriented to the present if he or she has very intense emotional responses when recalling or acknowledging a trauma. At such times, avoid responding with such exclamations as “I don’t know how you survived that!” (Bernstein, 2000). If the client has difficulty self-soothing, guide him or her through grounding techniques (Exhibit 1.4-1), which are particularly useful—perhaps even critical—to achieving a successful interview when a client has dissociated or is experiencing intense feelings in response to screening and/or interview questions.
-
Avoid phrases that imply judgment about the trauma. For example, don’t say to a client who survived Hurricane Katrina and lost family members, “It was God’s will,” or “It was her time to pass,” or “It was meant to be.” Do not make assumptions about what a person has experienced. Rather, listen supportively without imposing personal views on the client’s experience.
-
Provide feedback about the results of the screening. Keep in mind the client’s vulnerability, ability to access resources, strengths, and coping strategies. Present results in a synthesized manner, avoiding complicated, overly scientific jargon or explanations. Allow time to process client reactions during the feedback session. Answer client questions and concerns in a direct, honest, and compassionate manner. Failure to deliver feedback in this way can negatively affect clients’ psychological status and severely weaken the potential for developing a therapeutic alliance with the client.
-
Be aware of the possible legal implications of assessment. Information you gather during the screening and assessment process can necessitate mandatory reporting to authorities, even when the client does not want such information disclosed (Najavits, 2004). For example, you can be required to report a client’s experience of child abuse even if it happened many years ago or the client doesn’t want the information reported. Other legal issues can be quite complex, such as confidentiality of records, pursuing a case against a trauma perpetrator and divulging information to third parties while still protecting the legal status of information used in prosecution, and child custody issues (Najavits, 2004). It’s essential that you know the laws in your State, have an expert legal consultant available, and access clinical supervision.
Exhibit 1.4-1
Grounding Techniques
Grounding techniques are important skills for assessors and all other behavioral health service providers who interact with traumatized clients (e.g., nurses, security, administrators, clinicians). Even if you do not directly conduct therapy, knowledge of grounding can help you defuse an escalating situation or calm a client who is triggered by the assessment process. Grounding strategies help a person who is overwhelmed by memories or strong emotions or is dissociating; they help the person become aware of the here and now. A useful metaphor is the experience of walking out of a movie theater. When the person dissociates or has a flashback, it’s like watching a mental movie; grounding techniques help him or her step out of the movie theater into the daylight and the present environment. The client’s task is not only to hold on to moments from the past, but also to acknowledge that what he or she was experiencing is from the past. Try the following techniques:
-
Ask the client to state what he or she observes.Guide the client through this exercise by using statements like, “You seem to feel very scared/angry right now. You’re probably feeling things related to what happened in the past. Now, you’re in a safe situation. Let’s try to stay in the present. Take a slow deep breath, relax your shoulders, put your feet on the floor; let’s talk about what day and time it is, notice what’s on the wall, etc. What else can you do to feel okay in your body right now?”
-
Help the client decrease the intensity of affect.
-
“Emotion dial”: A client imagines turning down the volume on his or her emotions.
-
Clenching fists can move the energy of an emotion into fists, which the client can then release.
-
Guided imagery can be used to visualize a safe place.
-
Distraction (see #3 below).
-
Use strengths-based questions (e.g., “How did you survive?” or “What strengths did you possess to survive the trauma?”).
-
-
Distract the client from unbearable emotional states.
-
Have the client focus on the external environment (e.g., name red objects in the room).
-
Ask the client to focus on recent and future events (e.g., “to do” list for the day).
-
Help the client use self-talk to remind himself or herself of current safety.
-
Use distractions, such as counting, to return the focus to current reality.
-
Somatosensory techniques (toe-wiggling, touching a chair) can remind clients of current reality.
-
-
Ask the client to use breathing techniques.
-
Ask the client to inhale through the nose and exhale through the mouth.
-
Have the client place his or her hands on his or her abdomen and then watch the hands go up and down while the belly expands and contracts.
-
Source: Melnick & Bassuk, 2000.
Barriers and Challenges to Trauma-Informed Screening and Assessment
Barriers
It is not necessarily easy or obvious to identify an individual who has survived trauma without screening. Moreover, some clients may deny that they have encountered trauma and its effects even after being screened or asked direct questions aimed at identifying the occurrence of traumatic events. The two main barriers to the evaluation of trauma and its related disorders in behavioral health settings are clients not reporting trauma and providers overlooking trauma and its effects.
Concerning the first main barrier, some events will be experienced as traumatic by one person but considered nontraumatic by another. A history of trauma encompasses not only the experience of a potentially traumatic event, but also the person’s responses to it and the meanings he or she attaches to the event. Certain situations make it more likely that the client will not be forthcoming about traumatic events or his or her responses to those events. Some clients might not have ever thought of a particular event or their response to it as traumatic and thus might not report or even recall the event. Some clients might feel a reluctance to discuss something that they sense might bring up uncomfortable feelings (especially with a counselor whom they’ve only recently met). Clients may avoid openly discussing traumatic events or have difficulty recognizing or articulating their experience of trauma for other reasons, such as feelings of shame, guilt, or fear of retribution by others associated with the event (e.g., in cases of interpersonal or domestic violence). Still others may deny their history because they are tired of being interviewed or asked to fill out forms and may believe it doesn’t matter anyway.
Common Reasons Why Some Providers Avoid Screening Clients for Trauma
Treatment providers may avoid screening for traumatic events and trauma-related symptoms due to:
-
A reluctance to inquire about traumatic events and symptoms because these questions are not a part of the counselor’s or program’s standard intake procedures.
-
Underestimation of the impact of trauma on clients’ physical and mental health.
-
A belief that treatment of substance abuse issues needs to occur first and exclusively, before treating other behavioral health disorders.
-
A belief that treatment should focus solely on presenting symptoms rather than exploring the potential origins or aggravators of symptoms.
-
A lack of training and/or feelings of incompetence in effectively treating trauma-related problems (Salyers, Evans, Bond, & Meyer, 2004).
-
Not knowing how to respond therapeutically to a client’s report of trauma.
-
Fear that a probing trauma inquiry will be too disturbing to clients.
-
Not using common language with clients that will elicit a report of trauma (e.g., asking clients if they were abused as a child without describing what is meant by abuse).
-
Concern that if disorders are identified, clients will require treatment that the counselor or program does not feel capable of providing (Fallot & Harris, 2001).
-
Insufficient time for assessment to explore trauma histories or symptoms.
-
Untreated trauma-related symptoms of the counselor, other staff members, and administrators.
A client may not report past trauma for many reasons, including:
-
Concern for safety (e.g., fearing more abuse by a perpetrator for revealing the trauma).
-
Fear of being judged by service providers.
-
Shame about victimization.
-
Reticence about talking with others in response to trauma.
-
Not recalling past trauma through dissociation, denial, or repression (although genuine blockage of all trauma memory is rare among trauma survivors; McNally, 2003).
-
Lack of trust in others, including behavioral health service providers.
-
Not seeing a significant event as traumatic.
Regarding the second major barrier, counselors and other behavioral health service providers may lack awareness that trauma can significantly affect clients’ presentations in treatment and functioning across major life areas, such as relationships and work. In addition, some counselors may believe that their role is to treat only the presenting psychological and/or substance abuse symptoms, and thus they may not be as sensitive to histories and effects of trauma. Other providers may believe that a client should abstain from alcohol and drugs for an extended period before exploring trauma symptoms. Perhaps you fear that addressing a clients’ trauma history will only exacerbate symptoms and complicate treatment. Behavioral health service providers who hold biases may assume that a client doesn’t have a history of trauma and thus fail to ask the “right” questions, or they may be uncomfortable with emotions that arise from listening to client experiences and, as a result, redirect the screening or counseling focus.
Challenges
Awareness of acculturation and language
Acculturation levels can affect screening and assessment results. Therefore, indepth discussions may be a more appropriate way to gain an understanding of trauma from the client’s point of view. During the intake, prior to trauma screening, determine the client’s history of migration, if applicable, and primary language. Questions about the client’s country of birth, length of time in this country, events or reasons for migration, and ethnic self-identification are also appropriate at intake. Also be aware that even individuals who speak English well might have trouble understanding the subtleties of questions on standard screening and assessment tools. It is not adequate to translate items simply from English into another language; words, idioms, and examples often don’t translate directly into other languages and therefore need to be adapted. Screening and assessment should be conducted in the client’s preferred language by trained staff members who speak the language or by professional translators familiar with treatment jargon.
Common Assessment Myths
Several common myths contribute to underassessment of trauma-related disorders (Najavits, 2004):
-
Myth #1: Substance abuse itself is a trauma. However devastating substance abuse is, it does not meet the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5; American Psychiatric Association [APA], 2013a), criteria for trauma per se. Nevertheless, high-risk behaviors that are more likely to occur during addiction, such as interpersonal violence and self-harm, significantly increase the potential for traumatic injury.
-
Myth #2: Assessment of trauma is enough. Thorough assessment is the best way to identify the existence and extent of trauma-related problems. However, simply identifying trauma-related symptoms and disorders is just the first step. Also needed are individualized treatment protocols and action to implement these protocols.
-
Myth #3: It is best to wait until the client has ended substance use and withdrawal to assess for PTSD. Research does not provide a clear answer to the controversial question of when to assess for PTSD; however, Najavits (2004) and others note that underdiagnosis of trauma and PTSD has been more significant in the substance abuse field than overdiagnosis. Clinical experience shows that the PTSD diagnosis is rather stable during substance use or withdrawal, but symptoms can become more or less intense; memory impairment from alcohol or drugs can also cloud the symptom picture. Thus, it is advisable to establish a tentative diagnosis and then reassess after a period of abstinence, if possible.
Awareness of co-occurring diagnoses
A trauma-informed assessor looks for psychological symptoms that are associated with trauma or simply occur alongside it. Symptom screening involves questions about past or present mental disorder symptoms that may indicate the need for a full mental health assessment. A variety of screening tools are available, including symptom checklists.
However, you should only use symptom checklists when you need information about how your client is currently feeling; don’t use them to screen for specific disorders. Responses will likely change from one administration of the checklist to the next.
Basic mental health screening tools are available. For example, the Mental Health Screening Form-III screens for present or past symptoms of most mental disorders (Carroll & McGinley, 2001); it is available at no charge from Project Return Foundation, Inc. and is also reproduced in TIP 42, Substance Abuse Treatment for Persons With Co-Occurring Disorders (CSAT, 2005c). Other screening tools, such as the Beck Depression Inventory II and the Beck Anxiety Inventory (Beck, Wright, Newman, & Liese, 1993), also screen broadly for mental and substance use disorders, as well as for specific disorders often associated with trauma. For further screening information and resources on depression and suicide, see TIP 48, Managing Depressive Symptoms in Substance Abuse Clients During Early Recovery (CSAT, 2008), and TIP 50, Addressing Suicidal Thoughts and Behaviors in Substance Abuse Treatment (CSAT, 2009a).
For screening substance use disorders, see TIP 11, Simple Screening Instruments for Outreach for Alcohol and Other Drug Abuse and Infectious Diseases (CSAT, 1994); TIP 24, A Guide to Substance Abuse Services for Primary Care Clinicians (CSAT, 1997a); TIP 31, Screening and Assessing Adolescents for Substance Use Disorders (CSAT, 1999c); TIP 42, Substance Abuse Treatment for Persons With Co-Occurring Disorders (CSAT, 2005c); and TIP 51, Substance Abuse Treatment: Addressing the Specific Needs of Women (CSAT, 2009d).
A common dilemma in the assessment of trauma-related disorders is that certain trauma symptoms are also symptoms of other disorders. Clients with histories of trauma typically present a variety of symptoms; thus, it is important to determine the full scope of symptoms and/or disorders present to help improve treatment planning. Clients with trauma-related and substance use symptoms and disorders are at increased risk for additional Axis I and/or Axis II mental disorders (Brady, Killeen, Saladin, Dansky, & Becker, 1994; Cottler, Nishith, & Compton, 2001). These symptoms need to be distinguished so that other presenting subclinical features or disorders do not go unidentified and untreated. To accomplish this, a comprehensive assessment of the client’s mental health is recommended.
Misdiagnosis and underdiagnosis
Many trauma survivors are either misdiagnosed (i.e., given diagnoses that are not accurate) or underdiagnosed (i.e., have one or more diagnoses that have not been identified at all). Such diagnostic errors could result, in part, from the fact that many general instruments to evaluate mental disorders are not sufficiently sensitive to identify posttraumatic symptoms and can misclassify them as other disorders, including personality disorders or psychoses. Intrusive posttraumatic symptoms, for example, can show up on general measures as indicative of hallucinations or obsessions. Dissociative symptoms can be interpreted as indicative of schizophrenia. Trauma-based cognitive symptoms can be scored as evidence for paranoia or other delusional processes (Briere, 1997). Some of the most common misdiagnoses in clients with PTSD and substance abuse are:
-
Mood and anxiety disorders. Overlapping symptoms with such disorders as major depression, generalized anxiety disorder, and bipolar disorder can lead to misdiagnosis.
-
Borderline personality disorder. Historically, this has been more frequently diagnosed than PTSD. Many of the symptoms, including a pattern of intense interpersonal relationships, impulsivity, rapid and unpredictable mood swings, power struggles in the treatment environment, underlying anxiety and depressive symptoms, and transient, stress-related paranoid ideation or severe dissociative symptoms overlap. The effect of this misdiagnosis on treatment can be particularly negative; counselors often view clients with a borderline personality diagnosis as difficult to treat and unresponsive to treatment.
-
Antisocial personality disorder. For men and women who have been traumatized in childhood, “acting out” behaviors, a lack of empathy and conscience, impulsivity, and self-centeredness can be functions of trauma and survival skills rather than true antisocial characteristics.
-
Attention deficit hyperactivity disorder (ADHD). For children and adolescents, impulsive behaviors and concentration problems can be diagnosed as ADHD rather than PTSD.
It is possible, however, for clients to legitimately have any of these disorders in addition to trauma-related disorders. Given the overlap of posttraumatic symptoms with those of other disorders, a wide variety of diagnoses often needs to be considered to avoid misidentifying other disorders as PTSD and vice versa. A trained and experienced mental health professional will be required to weigh differential diagnoses. TIP 42 (CSAT, 2005c) explores issues related to differential diagnosis.
Cross-Cultural Screening and Assessment
Many trauma-related symptoms and disorders are culture specific, and a client’s cultural background must be considered in screening and assessment (for review of assessment and cultural considerations when working with trauma, see Wilson & Tang, 2007). Behavioral health service providers must approach screening and assessment processes with the influences of culture, ethnicity, and race firmly in mind. Cultural factors, such as norms for expressing psychological distress, defining trauma, and seeking help in dealing with trauma, can affect:
-
How traumas are experienced.
-
The meaning assigned to the event(s).
-
How trauma-related symptoms are expressed (e.g., as somatic expressions of distress, level of emotionality, types of avoidant behavior).
-
Willingness to express distress or identify trauma with a behavioral health service provider and sense of safety in doing so.
-
Whether a specific pattern of behavior, emotional expression, or cognitive process is considered abnormal.
-
Willingness to seek treatment inside and outside of one’s own culture.
-
Response to treatment.
-
Treatment outcome.
When selecting assessment instruments, counselors and administrators need to choose, whenever possible, instruments that are culturally appropriate for the client. Instruments that have been normed for, adapted to, and tested on specific cultural and linguistic groups should be used. Instruments that are not normed for the population are likely to contain cultural biases and produce misleading results. Subsequently, this can lead to misdiagnosis, overdiagnosis, inappropriate treatment plans, and ineffective interventions. Thus, it is important to interpret all test results cautiously and to discuss the limitations of instruments with clients from diverse ethnic populations and cultures. For a review of cross-cultural screening and assessment considerations, refer to the planned TIP, Improving Cultural Competence (Substance Abuse and Mental Health Services Administration, planned c).
Culture-Specific Stress Responses
Culture-bound concepts of distress exist that don’t necessarily match diagnostic criteria. Culture-specific symptoms and syndromes can involve physical complaints, broad emotional reactions, or specific cognitive features. Many such syndromes are unique to a specific culture but can broaden to cultures that have similar beliefs or characteristics. Culture-bound syndromes are typically treated by traditional medicine and are known throughout the culture. Cultural concepts of distress include:
-
Ataques de nervios. Recognized in Latin America and among individuals of Latino descent, the primary features of this syndrome include intense emotional upset (e.g., shouting, crying, trembling, dissociative or seizure-like episodes). It frequently occurs in response to a traumatic or stressful event in the family.
-
Nervios. This is considered a common idiom of distress among Latinos; it includes a wide range of emotional distress symptoms including headaches, nervousness, tearfulness, stomach discomfort, difficulty sleeping, and dizziness. Symptoms can vary widely in intensity, as can impairment from them. This often occurs in response to stressful or difficult life events.
-
Susto. This term, meaning “fright,” refers to a concept found in Latin American cultures, but it is not recognized among Latinos from the Caribbean. Susto is attributed to a traumatic or frightening event that causes the soul to leave the body, thus resulting in illness and unhappiness; extreme cases may result in death. Symptoms include appetite or sleep disturbances, sadness, lack of motivation, low self-esteem, and somatic symptoms.
-
Taijin kyofusho. Recognized in Japan and among some American Japanese, this “interpersonal fear” syndrome is characterized by anxiety about and avoidance of interpersonal circumstances. The individual presents worry or a conviction that his or her appearance or social interactions are inadequate or offensive. Other cultures have similar cultural descriptions or syndromes associated with social anxiety.
Sources: APA, 2013, pp. 833–837; Briere & Scott, 2006b.
Choosing Instruments
Numerous instruments screen for trauma history, indicate symptoms, assess trauma-related and other mental disorders, and identify related clinical phenomena, such as dissociation. One instrument is unlikely to meet all screening or assessment needs or to determine the existence and full extent of trauma symptoms and traumatic experiences. The following sections present general considerations in selecting standardized instruments.
Purpose
Define your assessment needs. Do you need a standardized screening or assessment instrument for clinical purposes? Do you need information on a specific aspect of trauma, such as history, PTSD, or dissociation? Do you wish to make a formal diagnosis, such as PTSD? Do you need to determine quickly whether a client has experienced a trauma? Do you want an assessment that requires a clinician to administer it, or can the client complete the instrument himself or herself? Does the instrument match the current and specific diagnostic criteria established in the DSM-5?
Population
Consider the population to be assessed (e.g., women, children, adolescents, refugees, disaster survivors, survivors of physical or sexual violence, survivors of combat-related trauma, people whose native language is not English); some tools are appropriate only for certain populations. Is the assessment process developmentally and culturally appropriate for your client? Exhibit 1.4-2 lists considerations in choosing a screening or assessment instrument for trauma and/or PTSD.
Exhibit 1.4-2
Key Areas of Trauma Screening and Assessment
Trauma
Key question: Did the client experience a trauma?
Examples of measures: Life Stressor Checklist-Revised (Wolfe & Kimerling, 1997); Trauma History Questionnaire (Green, 1996); Traumatic Life Events Questionnaire (Kubany et al., 2000).
Note: A good trauma measure identifies events a person experienced (e.g., rape, assault, accident) and also evaluates other trauma-related symptoms (e.g., presence of fear, helplessness, or horror).
Acute Stress Disorder (ASD) and PTSD
Key question: Does the client meet criteria for ASD or PTSD?
Examples of measures: Clinician-Administered PTSD Scale (CAPS; Blake et al., 1990); Modified PTSD Symptom Scale (Falsetti, Resnick, Resnick, & Kilpatrick, 1993); PTSD Checklist (Weathers, Litz, Herman, Huska, & Keane, 1993); Stanford Acute Stress Reaction Questionnaire (Cardena, Koopman, Classen, Waelde, & Spiegel, 2000).
Note: A PTSD diagnosis requires the person to meet criteria for having experienced a trauma; some measures include this, but others do not and require use of a separate trauma measure. The CAPS is an interview; the others listed are self-report questionnaires and take less time.
Other Trauma-Related Symptoms
Key question: Does the client have other symptoms related to trauma? These include depressive symptoms, self-harm, dissociation, sexuality problems, and relationship issues, such as distrust.
Examples of measures: Beck Depression Inventory II (Beck, 1993; Beck et al., 1993); Dissociative Experiences Scale (Bernstein & Putnam, 1986; Carlson & Putnam, 1993); Impact of Event Scale (measures intrusion and avoidance due to exposure to traumatic events; Horowitz, Wilner, & Alvarez, 1979; Weiss & Marmar, 1997); Trauma Symptom Inventory (Briere, 1995); Trauma Symptom Checklist for Children (Briere, 1996b); Modified PTSD Symptom Scale (Falsetti et al., 1993).
Note: These measures can be helpful for clinical purposes and for outcome assessment because they gauge levels of symptoms. Trauma-related symptoms are broader than diagnostic criteria and thus useful to measure, even if the patient doesn’t meet criteria for any specific diagnoses.
Other Trauma-Related Diagnoses
Key question: Does the client have other disorders related to trauma? These include mood disorders, anxiety disorders besides traumatic stress disorders, and dissociative disorders.
Examples of measures: Mental Health Screening Form III (Carroll & McGinley, 2001); The Mini-International Neuropsychiatric Interview (M.I.N.I.) Structured Clinical Interview for DSM-IV-TR, Patient Edition (First, Spitzer, Gibbon, & Williams, revised 2011); Structured Clinical Interview for DSM-IV-TR, Non-Patient Edition (First, Spitzer, Gibbon, & Williams, revised 2011a).
Note: For complex symptoms and diagnoses such as dissociation and dissociative disorders, interviews are recommended. Look for measures that incorporate DSM-5 criteria.
Sources: Antony et al., 2001; Najavits, 2004.
Instrument Quality
An instrument should be psychometrically adequate in terms of sensitivity and specificity or reliability and validity as measured in several ways under varying conditions. Published research offers information on an instrument’s psychometric properties as well as its utility in both research and clinical settings. For further information on a number of widely used trauma evaluation tools, see Appendix D and Antony, Orsillo, and Roemer’s paper (2001).
The DSM-5 and Updates to Screening and Assessment Instruments
The recent publication of the DSM-5 (APA, 2013a) reflects changes to certain diagnostic criteria, which will affect screening tools and criteria for trauma-related disorders. Criterion A2 (specific to traumatic stress disorders, acute stress, and posttraumatic stress disorders), included in the fourth edition (text revision) of the DSM (DSM-IV-TR; APA, 2000a), has been eliminated; this criterion stated that the individual’s response to the trauma needs to involve intense fear, helplessness, or horror. There are now four cluster symptoms, not three: reexperiencing, avoidance, arousal, and persistent negative alterations in cognitions and mood. Changes to the DSM-5 were made to symptoms within each cluster. Thus, screening will need modification to adjust to this change (APA, 2012b).
Practical Issues
Is the instrument freely and readily available, or is there a fee? Is costly and extensive training required to administer it? Is the instrument too lengthy to be used in the clinical setting? Is it easily administered and scored with accompanying manuals and/or other training materials? How will results be presented to or used with the client? Is technical support available for difficulties in administration, scoring, or interpretation of results? Is special equipment required such as a microphone, a video camera, or a touch-screen computer with audio?
Trauma-Informed Screening and Assessment
The following sections focus on initial screening. For more information on screening and assessment tools, including structured interviews, see Exhibit 1.4-2. Screening is only as good as the actions taken afterward to address a positive screen (when clients acknowledge that they experience symptoms or have encountered events highlighted within the screening). Once a screening is complete and a positive screen is acquired, the client then needs referral for a more indepth assessment to ensure development of an appropriate treatment plan that matches his or her presenting problems.
Establish a History of Trauma
A person cannot have ASD, PTSD, or any trauma-related symptoms without experiencing trauma; therefore, it is necessary to inquire about painful, difficult, or overwhelming past experiences. Initial information should be gathered in a way that is minimally intrusive yet clear. Brief questionnaires can be less threatening to a client than face-to-face interviews, but interviews should be an integral part of any screening and assessment process.
If the client initially denies a history of trauma (or minimizes it), administer the questionnaire later or delay additional trauma-related questions until the client has perhaps developed more trust in the treatment setting and feels safer with the thoughts and emotions that might arise in discussing his or her trauma experiences.
The Stressful Life Experiences (SLE) screen (Exhibit 1.4-3) is a checklist of traumas that also considers the client’s view of the impact of those events on life functioning. Using the SLE can foster the client–counselor relationship. By going over the answers with the client, you can gain a deep understanding of your client, and the client receives a demonstration of your sensitivity and concern for what the client has experienced. The National Center for PTSD Web site offers similar instruments.
In addition to broad screening tools that capture various traumatic experiences and symptoms, other screening tools, such as the Combat Exposure Scale (Keane et al., 1989) and the Intimate Partner Violence Screening Tool (Exhibit 1.4-4), focus on acknowledging a specific type of traumatic event.
Exhibit 1.4-4
STaT Intimate Partner Violence Screening Tool
-
Have you ever been in a relationship where your partner has pushed or Slapped you?
-
Have you ever been in a relationship where your partner Threatened you with violence?
-
Have you ever been in a relationship where your partner has thrown, broken, or punched Things?
Source: Paranjape & Liebschutz, 2003. Used with permission
Screen for Trauma-Related Symptoms and Disorders in Clients With Histories of Trauma
This step evaluates whether the client’s trauma resulted in subclinical or diagnosable disorders. The counselor can ask such questions as, “Have you received any counseling or therapy? Have you ever been diagnosed or treated for a psychological disorder in the past? Have you ever been prescribed medications for your emotions in the past?” Screening is typically conducted by a wide variety of behavioral health service providers with different levels of training and education; however, all individuals who administer screenings, regardless of education level and experience, should be aware of trauma-related symptoms, grounding techniques, ways of creating safety for the client, proper methods for introducing screening tools, and the protocol to follow when a positive screen is obtained. (See Appendix D for information on specific instruments.) Exhibit 1.4-5 is an example of a screening instrument for trauma symptoms, the Primary Care PTSD (PC-PTSD) Screen. Current research (Prins et al., 2004) suggests that the optimal cutoff score for the PC-PTSD is 3. If sensitivity is of greater concern than efficiency, a cutoff score of 2 is recommended.
Exhibit 1.4-5
PC-PTSD Screen
In your life, have you ever had any experience that was so frightening, horrible, or upsetting that, in the past month, you…
-
Have had nightmares about it or thought about it when you did not want to?YES NO
-
Tried hard not to think about it or went out of your way to avoid situations that reminded you of it?YES NO
-
Were constantly on guard, watchful, or easily startled?YES NO
-
Felt numb or detached from others, activities, or your surroundings?YES NO
Source: Prins et al., 2004. Material used is in the public domain.
Another instrument that can screen for traumatic stress symptoms is the four-item self-report SPAN, summarized in Exhibit 1.4-6, which is derived from the 17-item Davidson Trauma Scale (DTS). SPAN is an acronym for the four items the screening addresses: startle, physiological arousal, anger, and numbness. It was developed using a small, diverse sample of adult patients (N=243; 72 percent women; 17.4 percent African American; average age = 37 years) participating in several clinical studies, including a family study of rape trauma, combat veterans, and Hurricane Andrew survivors, among others.
Exhibit 1.4-6
The SPAN
The SPAN instrument is a brief screening tool that asks clients to identify the trauma in their past that is most disturbing to them currently. It then poses four questions that ask clients to rate the frequency and severity with which they have experienced, in the past week, different types of trauma-related symptoms (startle, physiological arousal, anger, and numbness).
To order this screening instrument, use the following contact information:
-
Multi-Health Systems, Inc.P.O. Box 950North Tonawanda, NY14120-0950Phone: 800-456-3003
Source: Meltzer-Brody et al., 1999.
The SPAN has a high diagnostic accuracy of 0.80 to 0.88, with sensitivity (percentage of true positive instances) of 0.84 and specificity (percentage of true negative instances) of 0.91 (Meltzer-Brody, Churchill, & Davidson, 1999). SPAN scores correlated highly with the full DTS (r = 0.96) and other measures, such as the Impact of Events Scale (r = 0.85) and the Sheehan Disability Scale (r = 0.87).
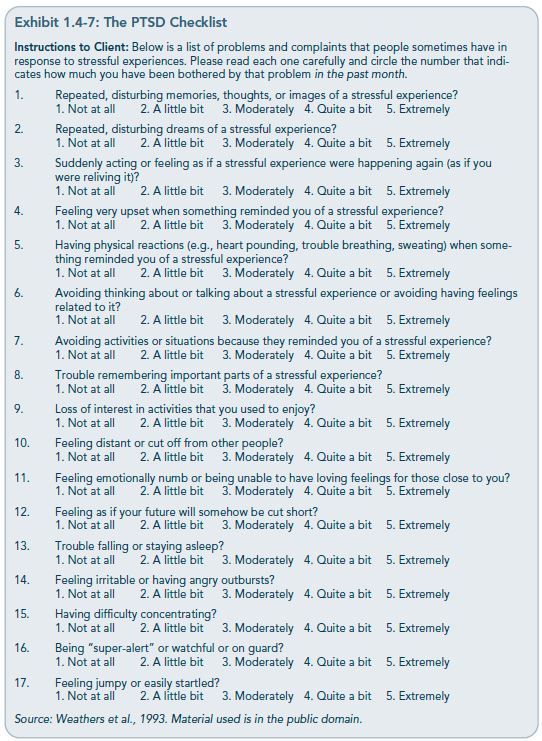
The PTSD Checklist (Exhibit 1.4-7), developed by the National Center for PTSD, is in the public domain. Originally developed for combat veterans of the Vietnam and Persian Gulf Wars, it has since been validated on a variety of noncombat traumas (Keane, Brief, Pratt, & Miller, 2007). When using the checklist, identify a specific trauma first and then have the client answer questions in relation to that one specific trauma.

Other Screening and Resilience Measures
Along with identifying the presence of trauma-related symptoms that warrant assessment to determine the severity of symptoms as well as whether or not the individual possesses subclinical symptoms or has met criteria for a trauma-related disorder, clients should receive other screenings for symptoms associated with trauma (e.g., depression, suicidality). It is important that screenings address both external and internal resources (e.g., support systems, strengths, coping styles). Knowing the client’s strengths can significantly shape the treatment planning process by allowing you to use strategies that have already worked for the client and incorporating strategies to build resilience (Exhibit 1.4-8).
Exhibit 1.4-8
Resilience Scales
A number of scales with good psychometric properties measure resilience:
-
Resilience Scale (Wagnild & Young, 1993)
-
Resilience Scale for Adults (Friborg, Hjemdal, Rosenvinge, & Martinussen, 2003)
-
Connor Davidson Resilience Scale, 25-,10-, and 2-Item (Connor & Davidson, 2003; Campbell-Sills & Stein, 2007; Vaishnavi, Connor, & Davidson, 2007, respectively)
-
Dispositional Resilience Scale, 45-,30-, 15-item forms (Bartone, Roland, Picano, & Williams, 2008)
Preliminary research shows improvement of individual resilience through treatment interventions in other populations (Lavretsky, Siddarth, & Irwin, 2010).
Screen for suicidality
All clients—particularly those who have experienced trauma—should be screened for suicidality by asking, “In the past, have you ever had suicidal thoughts, had intention to commit suicide, or made a suicide attempt? Do you have any of those feelings now? Have you had any such feelings recently?” Behavioral health service providers should receive training to screen for suicide. Additionally, clients with substance use disorders and a history of psychological trauma are at heightened risk for suicidal thoughts and behaviors; thus, screening for suicidality is indicated. See TIP 50, Addressing Suicidal Thoughts and Behaviors in Substance Abuse Treatment (CSAT, 2009a). For additional descriptions of screening processes for suicidality, see TIP 42 (CSAT, 2005c).
Concluding Note
Screenings are only beneficial if there are follow-up procedures and resources for handling positive screens, such as the ability to review results with and provide feedback to the individual after the screening, sufficient resources to complete a thorough assessment or to make an appropriate referral for an assessment, treatment planning processes that can easily incorporate additional trauma-informed care objectives and goals, and availability and access to trauma-specific services that match the client’s needs. Screening is only the first step!

