11.4: Regulation of Water Balance
- Page ID
- 23374
Skills to Develop
- Discuss the physiological events that trigger the thirst mechanism.
- Describe two mechanisms by which the body controls urine output.
As you eat a bite of food, the salivary glands secrete saliva. As the food enters your stomach, gastric juice is secreted. As it enters the small intestine, pancreatic juice is secreted. Each of these fluids contains a great deal of water. How is that water replaced in these organs? What happens to the water now in the intestines? In a day there is an exchange of about 10 liters of water among the body’s organs. The osmoregulation of this exchange involves complex communication between the brain, kidneys, and endocrine system. A homeostatic goal for a cell, a tissue, an organ, and an entire organism is to balance water output with water input.
Osmosis is the passage of solutions across a semi-permeable membrane. Water follows the ions in an attempt to equalize the ionic concentration in the compartments on both sides of the membrane. Osmotic pressure is the pressure excreted by particles in a solution to draw water across a membrane.
Regulation of Daily Water Input
Total water output per day averages 2.5 liters. This must be balanced with water input. Our tissues produce around 300 milliliters of water per day through metabolic processes. The remainder of water output must be balanced by drinking fluids and eating solid foods. The average fluid consumption per day is 1.5 liters, and water gained from solid foods approximates 700 milliliters.
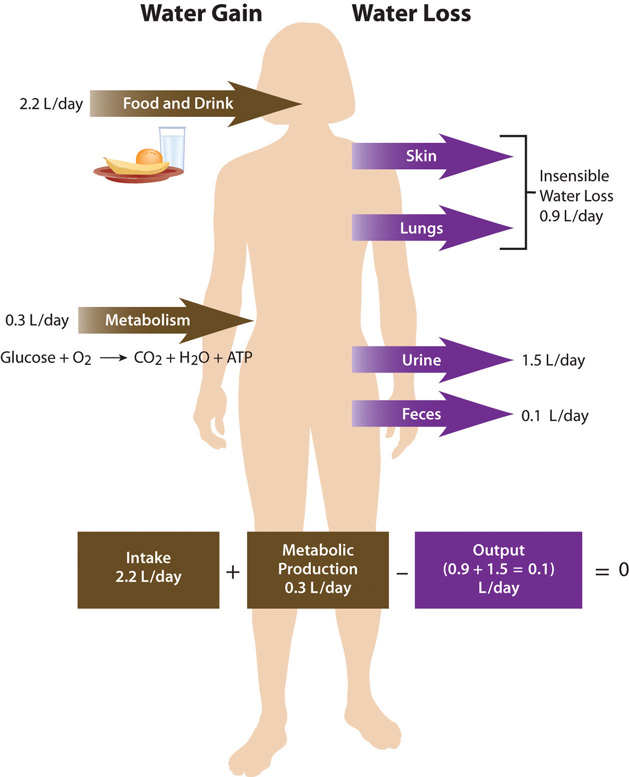
Dietary Gain of Water
The Food and Nutrition Board of the Institute of Medicine (IOM) has set the Adequate Intake (AI) for water for adult males at 3.7 liters (15.6 cups) and at 2.7 liters (11 cups) for adult females.Institute of Medicine Panel on Dietary Reference Intakes for Electrolytes and Water. Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate. (Washington, D.C.: National Academies Press, 2005). http://www.nap.edu/openbook.php?record_id=10925&page=73. These intakes are higher than the average intake of 2.2 liters. It is important to note that the AI for water includes water from all dietary sources; that is, water coming from food as well as beverages. People are not expected to consume 15.6 or 11 cups of pure water per day. In America, approximately 20 percent of dietary water comes from solid foods. See Table 11.4.1 for the range of water contents for selected food items. Beverages include water, tea, coffee, sodas, and juices.
| Percentage | Food Item |
|---|---|
| 90–99 | Nonfat milk, cantaloupe, strawberries, watermelon, lettuce, cabbage, celery, spinach, squash |
| 80–89 | Fruit juice, yogurt, apples, grapes, oranges, carrots, broccoli, pears, pineapple |
| 70–79 | Bananas, avocados, cottage cheese, ricotta cheese, baked potato, shrimp |
| 60–69 | Pasta, legumes, salmon, chicken breast |
| 50–59 | Ground beef, hot dogs, steak, feta cheese |
| 40–49 | Pizza |
| 30–39 | Cheddar cheese, bagels, bread |
| 20–29 | Pepperoni, cake, biscuits |
| 10–19 | Butter, margarine, raisins |
| 1–9 | Walnuts, dry-roasted peanuts, crackers, cereals, pretzels, peanut butter |
| 0 | Oils, sugars |
Source: US Department of Agriculture, Agricultural Research Service. 2010. National Nutrient Database for Standard Reference, Release 23. Nutrient Data Laboratory Home Page, http://www.ars.usda.gov/ba/bhnrc/ndl.
There is some debate over the amount of water required to maintain health because there is no consistent scientific evidence proving that drinking a particular amount of water improves health or reduces the risk of disease. In fact, kidney stone prevention seems to be the only premise for water consumption recommendations. You may be surprised to find out that the commonly held belief that people need to drink eight 8-ounce glasses of water per day isn’t an official recommendation and isn’t based on any scientific evidence! The amount of water/fluids a person should consume every day is actually variable and should be based on the climate a person lives in, as well as their age, physical activity level, and kidney function. No maximum for water intake has been set.
Thirst Mechanism: Why Do We Drink?
Thirst is an osmoregulatory mechanism to increase water input. The thirst mechanism is activated in response to changes in water volume in the blood but is even more sensitive to changes in blood osmolality. Blood osmolality is primarily driven by the concentration of sodium cations. The urge to drink results from a complex interplay of hormones and neuronal responses that coordinate to increase water input and contribute toward fluid balance and composition in the body. The “thirst center” is contained within the hypothalamus, a portion of the brain that lies just above the brain stem. In older people, the thirst mechanism is not as responsive and as we age there is a higher risk for dehydration. Thirst happens in the following sequence of physiological events:
- Receptor proteins in the kidney, heart, and hypothalamus detect decreased fluid volume or increased sodium concentration in the blood.
- Hormonal and neural messages are relayed to the brain’s thirst center in the hypothalamus.
- The hypothalamus sends neural signals to higher sensory areas in the cortex of the brain, stimulating the conscious thought to drink.
- Fluids are consumed.
- Receptors in the mouth and stomach detect mechanical movements involved with fluid ingestion.
- Neural signals are sent to the brain and the thirst mechanism is shut off.
The physiological control of thirst is the backup mechanism to increase water input. Fluid intake is controlled primarily by conscious eating and drinking habits dependent on social and cultural influences. For example, you might have a habit of drinking a glass of orange juice and eating a bowl of cereal every morning before school or work. Most American adolescents have a daily habit of soft-drink consumption. Soft-drink consumption is influenced by demographics, access to soft drinks, social impacts, and personal behavior.
Regulation of Daily Water Output
As stated, daily water output averages 2.5 liters. There are two types of outputs. The first type is insensible water loss, meaning we are unaware of it. The body loses about 400 milliliters of its daily water output through exhalation. Another 500 milliliters is lost through our skin. The second type of output is sensible water loss, meaning we are aware of it. Urine accounts for about 1,500 milliliters of water output, and feces account for roughly 100 milliliters of water output. Regulating urine output is a primary function of the kidneys, and involves communication with the brain and endocrine system.
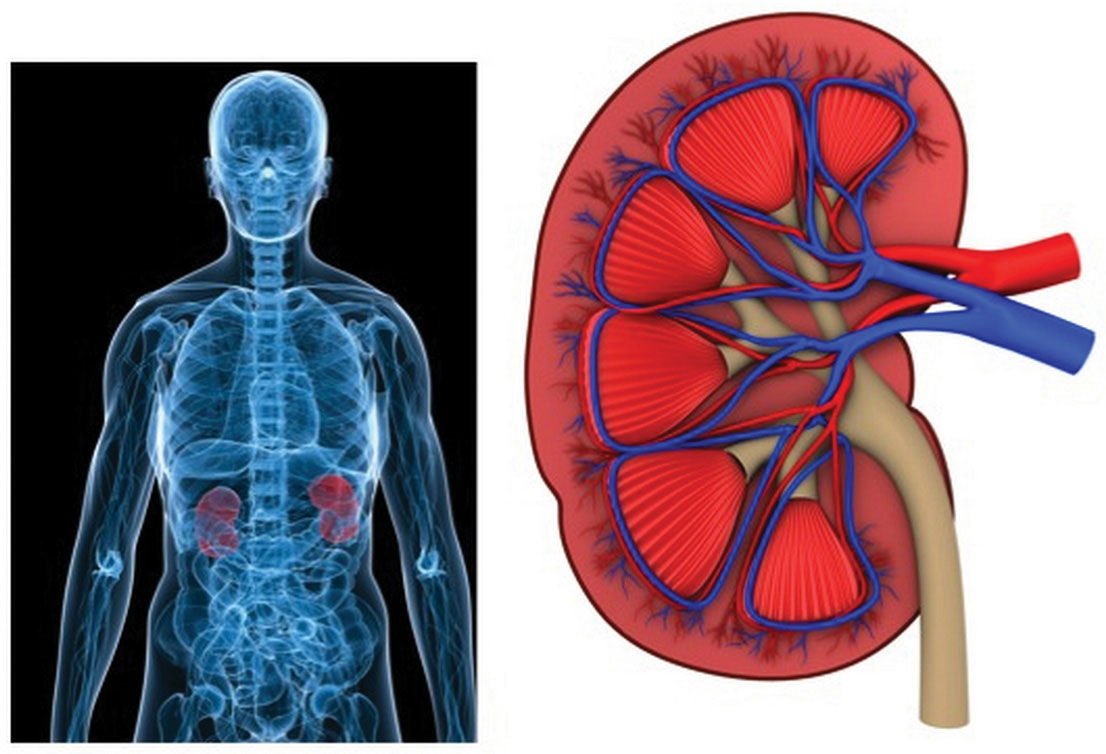
The Kidneys Detect Blood Volume
The kidneys are two bean-shaped organs, each about the size of a fist and located on either side of the spine just below the rib cage (Figure 7.4). The kidneys filter about 190 liters of blood and produce (on average) 1.5 liters of urine per day. Urine is mostly water, but it also contains electrolytes and waste products, such as urea. The amount of water filtered from the blood and excreted as urine is dependent on the amount of water in, and the electrolyte composition of, blood.
Kidneys have protein sensors that detect blood volume from the pressure, or stretch, in the blood vessels of the kidneys. When blood volume is low, kidney cells detect decreased pressure and secrete the enzyme, renin. Renin travels in the blood and cleaves another protein into the active hormone, angiotensin. Angiotensin targets three different organs (the adrenal glands, the hypothalamus, and the muscle tissue surrounding the arteries) to rapidly restore blood volume and, consequently, pressure.
- First, angiotensin travels to the outer perimeter of the adrenal glands and stimulates the release of the hormone aldosterone. Aldosterone travels back to the kidneys and stimulates the sodium-potassium pump. As a result of the pump’s work, the blood reabsorbs the sodium from the liquid that has already been filtered by the kidneys. Water follows sodium into the blood by osmosis, resulting in less water in the urine and restored fluid balance and composition of blood.
- Next, angiotensin travels to the hypothalamus where it stimulates the thirst mechanism and the release of antidiuretic hormone. Antidiuretic hormone travels back to the kidneys where it increases sodium and water reabsorption.
- Lastly, angiotensin targets smooth muscle tissue surrounding arteries, causing them to contract (narrow) the blood vessels, which assists in elevating blood pressure.
The Hypothalamus Detects Blood Osmolality
Osmoreceptors (specialized protein receptors) in the hypothalamus detect sodium concentration in the blood. In response to a high sodium level, the hypothalamus activates the thirst mechanism and concurrently stimulates the release of antidiuretic hormone. Thus, it is not only kidneys that stimulate antidiuretic- hormone release, but also the hypothalamus. This dual control of antidiuretic hormone release allows for the body to respond to both decreased blood volume and increased blood osmolality.
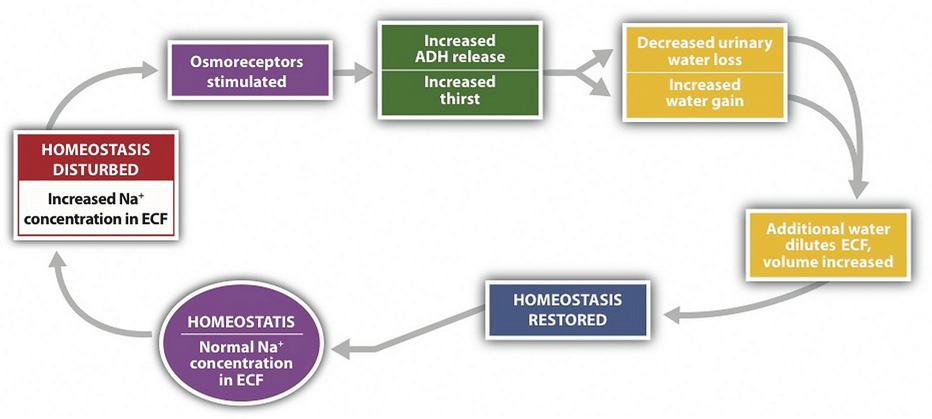
The Adrenal Glands Detect Blood Osmolality
Cells in the adrenal glands sense when sodium levels are low, and when potassium levels are high, in the blood. In response to either stimulus, they release aldosterone. Therefore, aldosterone is released in response to angiotensin stimulation and is also controlled by blood electrolyte concentrations. In either case, aldosterone communicates the same message, which is to increase sodium reabsorption and consequently water reabsorption. In exchange, potassium is excreted.
The mechanisms involved in regulating water input and output are intertwined with those controlling electrolyte balance. In a healthy individual, this multilevel coordinated control of fluid and electrolyte levels in the body ensures homeostasis. However, in a person with heart failure, the crosstalk between organs can have dire consequences. Heart failure results in a decrease in blood output from the heart, which lowers blood pressure. In response to the lower blood pressure, the kidneys release renin leading to the release of antidiuretic hormone. Antidiuretic hormone acts on the kidneys and increases water reabsorption, thereby increasing blood volume and pressure. This makes the heart work harder and exacerbates the heart condition. To block this response, people with heart failure are treated with drugs that block the kidneys’ compensatory response. Diuretics are drugs that act either by inhibiting the actions of antidiuretic hormone or by promoting sodium excretion in the urine. This increases water output and blood pressure is reduced. Diuretics, along with other drugs, are useful in treating heart failure and in decreasing blood pressure in people with hypertension.
Key Takeaways
- A homeostatic goal for a cell, tissue, organ, and entire organism is to balance water output with water input. The amount of water a person should consume every day is variable and should be based on the climate a person lives in, as well as their age, physical activity level, and kidney function.
- Thirst results from a complex interaction of hormones and neuronal responses that coordinate to achieve fluid balance and composition in the body. Thirst is triggered by either a decrease in blood volume or an increase in blood osmolality.
- Other mechanisms by which body water balance is maintained are aimed at controlling the water volume of urine. The amount of water filtered from the blood and excreted as urine is dependent upon the amount of water in blood and the electrolyte composition of blood.
- The regulation of water output involves complex communication between the kidneys, hypothalamus, and endocrine glands.
Discussion Starters
- Why do people urinate more often when it is cold outside?
- Discuss the signs you first detect when you are thirsty.

