2.13: Endoscopic Cholesteatoma, Tympanoplasty, and Middle Ear Surgery
- Page ID
- 17712
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
ENDOSCOPIC CHOLESTEATOMA, TYMPANOPLASTY AND MIDDLE EAR SURGERY
Muaaz Tarabichi
The introduction of the binocular operating microscope was a landmark in modern otology as it changed the scope and character of ear surgery. The endoscope offers a new perspective of cholesteatoma and related surgical procedures; it increases the surgeon’s understanding of the disorder and its extension through the temporal bone and provides a wide field of view of the middle ear compared to the microscope.
Even though it has been two decades since endoscopy was first used to explore mastoid cavities, the endoscope is used infrequently for surgical management of ear disease; most otologists have not felt compelled to master the newer endoscopic techniques.1-6 In addition, there has been a focus on using smaller diameter endoscopes for ear surgery which is counterproductive, as it eliminates the main (and possibly only) advantage of endoscopy i.e. wide field of view compared to that of the microscope.
The rationale, advantages, limitations, technique are discussed in this chapter.
History
The author first used the endoscope for ear surgery in 1993. In recent years, many surgeons have adopted it for middle ear surgery as opposed to the microscope.7-10 Transtympanic middle ear endoscopy was first reported by Nomura and Takahashi.3,4 Poe and Bottrill used transtympanic endoscopy to diagnose perilymphatic fistulae and to identify other middle ear pathology.5 Kakehata used microendoscopy and transtympanic endoscopy to evaluate conductive hearing loss and inspect retraction pockets.11-13 Thomassin reported on the use of operative ear endoscopy for mastoid cavities and designed an instrument for that purpose.1
Badr-el-Dine and El-Messelaty reported on the value of endoscopy as an adjunct in cholesteatoma surgery and documented a reduced risk of recurrence when the endoscope was used.14,15 A reduction in residual disease was confirmed by Yung and Ayache.16,17 Baki used endoscopy to evaluate disease within the sinus tympani.18 Mattox reported on endoscopy-assisted surgery of the petrous apex.19 Magnan20, Bader-el-Dine & El-Garem21-23, and Rosenberg24 reviewed the role of the endoscope in neurotologic procedures. McKennan described 2nd look endoscopic inspection of mastoid cavities through a small postauricular incision.6 Presutti & Marchioni described primary transcanal endoscopic ear surgery in a similar fashion to that reported in this chapter.25,26
Rationale for Endoscopic Ear Surgery
Acquired cholesteatoma is usually a manifestation of advanced tympanic membrane retraction; the sac retracts into the tympanic cavity proper and then extends into areas such as the sinus tympani, facial recess, hypotympanum, and attic.27 Only in advanced cases does cholesteatoma progress further to reach the mastoid cells.
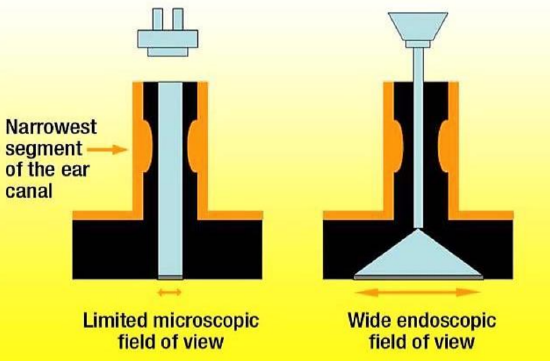
Figure 1: The view through the microscope during transcanal surgery is defined and limited by the narrowest segment of the ear canal; the endoscope bypasses this narrow segment and provides a very wide view that allows the surgeon to “look around corners,” even when the zero-degree scope is used
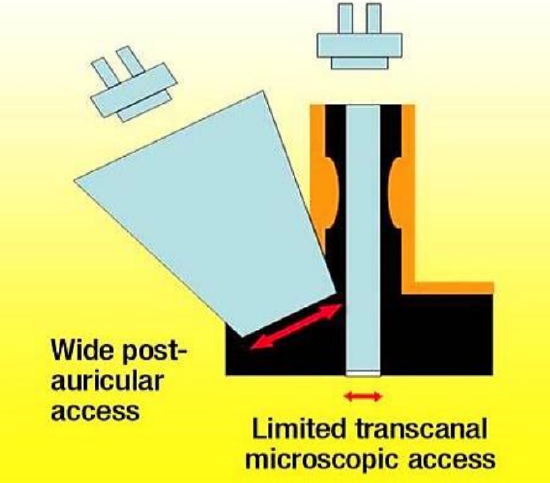
Figure 2: Limited view afforded by the microscope during transcanal procedures requires a postauricular mastoidectomy by which a port is created parallel to the attic after a considerable amount of healthy bone has been removed to enable anterior keyhole access to the attic
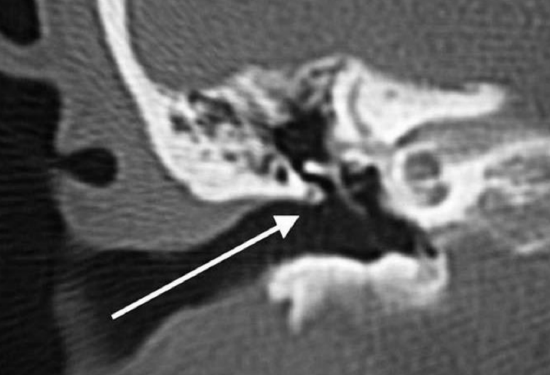
Figure 3: Coronal CT of temporal bone: A line drawn through the ear canal ends in the attic rather than mesotympanum; this almost universal anatomic orientation enables a natural transcanal access to the attic
Most surgical failures following a postauricular approach occur within the tympanic cavity and its hard-to-reach extensions, rather than within the mastoid.28,29 Therefore transcanal access to the tympanic membrane and tympanic cavity to remove cholesteatoma with subsequent step-by-step pursuit of the sac as it extends through the middle ear is the most logical approach. The microscopic view provided by transcanal access is defined and limited by the narrowest segment of the ear canal (Figure 1). This limitation compels surgeons to create a parallel port via a postauricular transmastoid approach to gain keyhole access to the attic, facial recess, and hypotympanum (Figure 3). Transcanal operative endoscopy however bypasses the narrow segment of the ear canal and provides a wide view that enables surgeons to look “around the corner,” even when a zero-degree endoscope is used (Figure 2).
Another anatomic observation that favors transcanal access to the attic, which is the most frequent site of cholesteatoma30, is the orientation of the ear canal in relation to the attic. Figure 3 shows a coronal computed tomographic (CT) section through the temporal bone and illustrates that a line drawn through the ear canal ends in the attic rather than in the mesotympanum. The only structure that is in the way is the scutum; its removal allows wide access to the attic, which is the natural cul de sac of the external auditory canal.
Rediscovering the ear canal as the access port for cholesteatoma surgery has been the main advantage of endoscopic ear surgery. It allows more natural and direct access to pursue cholesteatoma located within the middle ear cleft. In contrast, traditional approaches to the attic and facial recess provide primarily keyhole access through postauricular mastoidectomy; many surgeons use the ear canal to access the anterior part of the attic, even during postauricular tympanomastoidectomy. Other areas, such as the hypotympanum and sinus tympani are minimally accessible even with extensive postauricular mastoidectomy. The wide view provided by the endoscope enables minimally invasive transcanal access to all these areas and facilitates complete extirpation of disease without the need for a postauricular approach.
Instrumentation

Figure 4: Wide-angled telescope
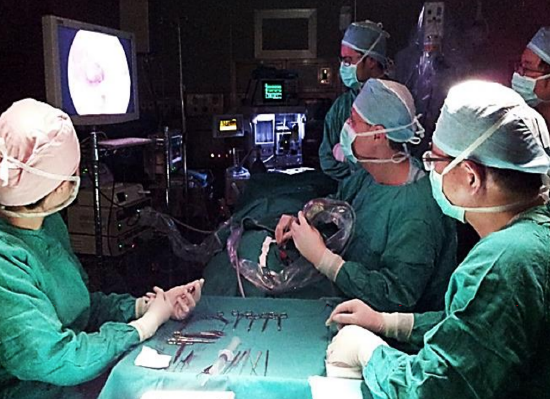
Figure 5: The surgeon operates while watching the monitor which is positioned across the operating room table. The surgical assistant also has a clear view of the monitor
Eighteen-centimeter-long, 4 mm, wide angled, zero-degree and 30-degree Hopkins II telescopes are most often used (Figure 4). Recently a smaller 3 mm endoscope with a very similar field of view to the 4 mm endoscope has been introduced. Smaller diameter scopes are used sparingly. Video equipment consists of a 3-chip video camera and a monitor. Procedures are performed directly off the monitor and recorded. Standard microscopic ear surgery instruments are used (Figure 5).
Important safety issues with endoscopic ear surgery
Thermal injury: This is evident only when a Xenon light source is used. Because of the small size of the cavity, adequate illumination of the middle ear space can be accomplished with a regular light source on lower settings without the need for a Xenon system. While the tip of the endoscope heats up quickly, it cools down quickly too. The tip of the endoscope requires continuous cleaning with antifog solution which probably also helps to cool the endoscope.
Trauma by the tip of the endoscope due to accidental head movement: The relatively large diameter of the endoscope (4 mm) and the anatomical configurations of the ear canal and middle ear space usually preclude introduction of the endoscope beyond the tympanic ring.
Endoscopic anatomy of middle ear cleft
Transcanal endoscopic approaches provide a new way of looking at the anatomy of the tympanic cavity and more specifically at cholesteatoma-bearing areas. The endoscope allows a better understanding of ligaments and folds of the middle ear and how they affect ventilation of the different spaces. This section highlights the endoscopic anatomy of the middle ear cleft and reviews the concept of the epitympanic diaphragm which plays an important role in the pathophysiology of attic cholesteatoma31-32-33.
Facial Recess
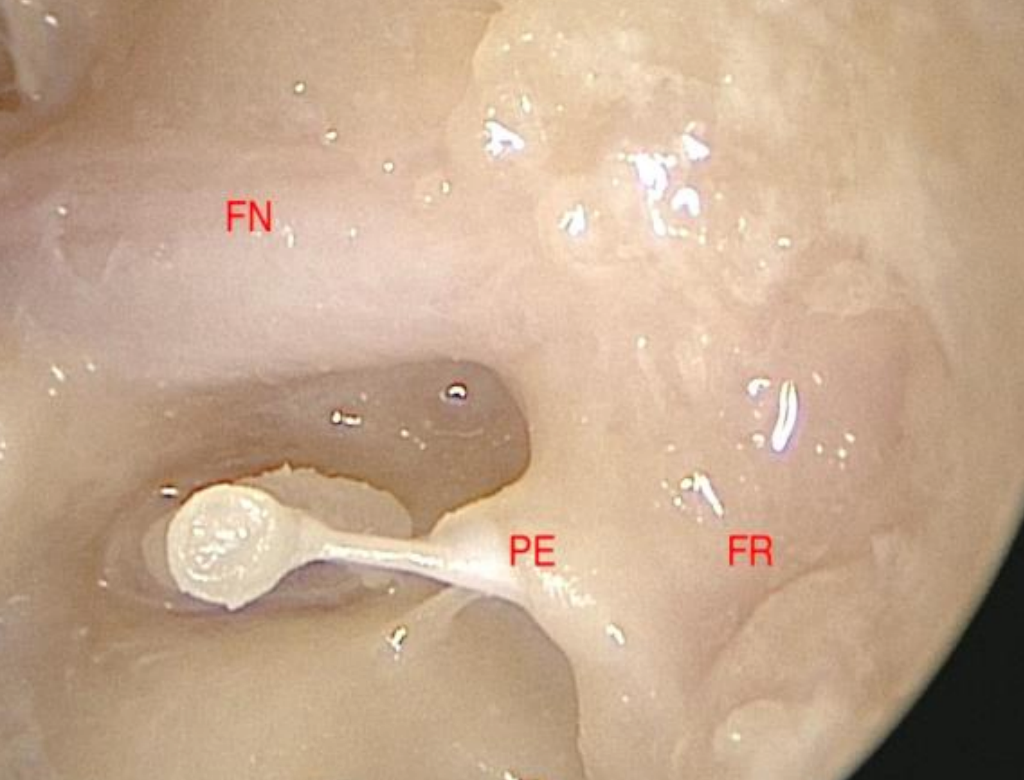
Figure 6: Left ear. Endoscopic view through transcanal endoscopic access after minor removal of bone; the facial recess (FR) is a very shallow and flat depression, more or less at the same level as the pyramidal eminence (PE) and tympanic segment of the facial nerve (FN)
Using a transcanal endoscopic approach, the facial recess is a very accessible, shallow depression on the posterior wall of the tympanic cavity (Figure 6). In contrast, a postauricular posterior tympanotomy gives keyhole access to this important area.
The pyramidal eminence and the vertical segment of the facial nerve form the medial wall of the recess. It marks the depth of the vertical segment of the facial nerve in this area. The bony annulus forms the lateral wall of the recess and can be taken down safely as long as the pyramidal eminence is continuously kept in view. The relationship of the bony annulus to the vertical segment of the facial nerve is very variable as one moves inferiorly beyond the pyramidal eminence; great care should therefore be paid when removing bone from the inferior/posterior aspect of the ear canal and bony annulus.
Retrotympanum
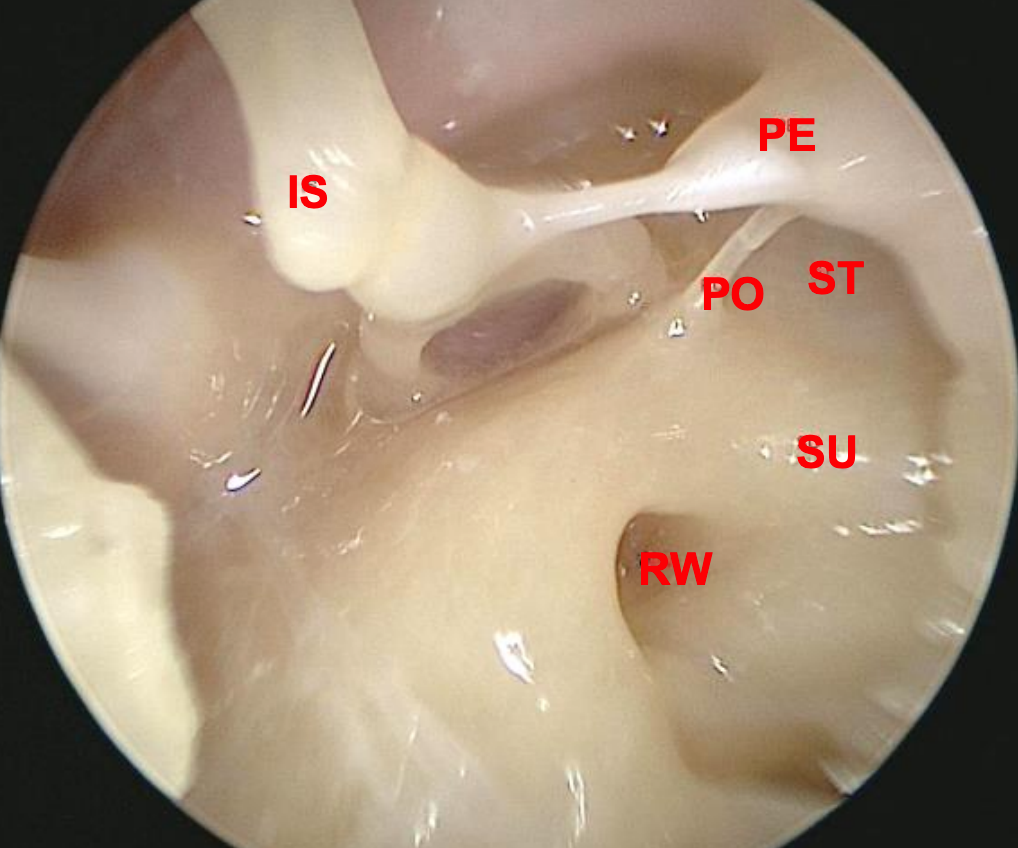
Figure 7: Left ear: View of retrotympanum (IS: incudostapedial joint; PE: pyramidal eminence; PO: ponticulus; ST: sinus tympani; SU: subiculum; RW: round window)
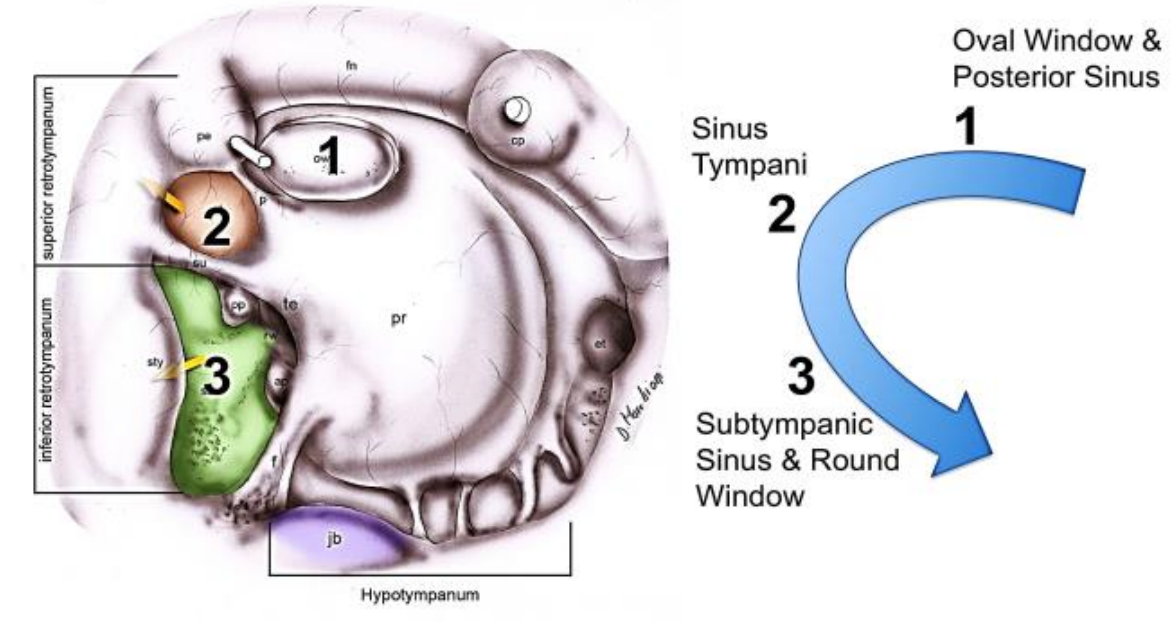
Figure 8: Right ear: Schematic drawing of retrotympanum. It is useful to start superiorly at the oval window and move inferiorly: posterior sinus, then sinus tympani, sinus subtympanicum, and then hypotympanum (Fn: facial nerve; pr: promontory; sty: styloid prominence; te: temen of round window; p: ponticulus; su: subiculum; jb: jugular bulb)
When observing the anatomy of the retrotympanum it is a useful surgical exercise to start superiorly with the posterior sinus and stapes footplate and to move inferiorly identifying the ponticulus, sinus tympani, subiculum, ending up with the sinus subtympanicum where the round window is located (Figures 7, 8). The stapes footplate is located within the posterior sinus that extends around and posterior to it. The round window is located within the sinus subtympanicum that extends posterior and inferior to it. Between these two sinuses lies the sinus tympani.
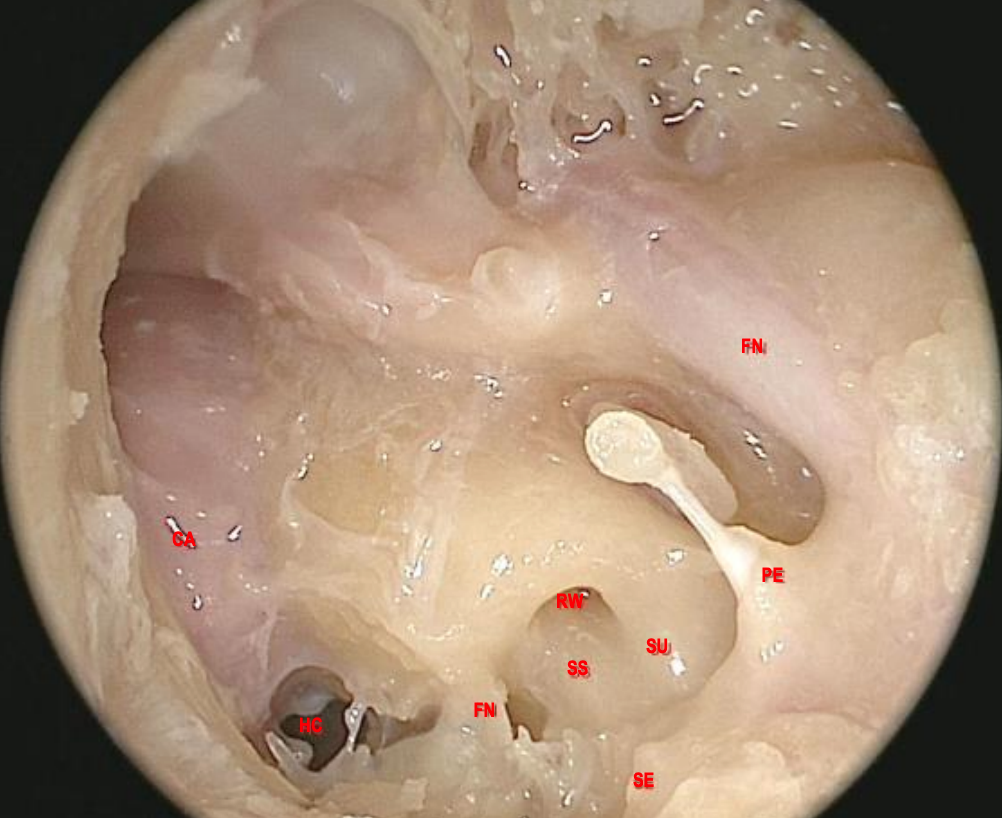
Figure 9: Left ear: Tympanic cavity with special attention to retrotympanum (FN: facial nerve; SU: subiculum; SS: sinus subtympanicus; SE: styloid eminence; RW: round window; FN: finiculus; CA: carotid artery; HC: hypotympanic air cell)
More inferiorly is the hypotympanum; this is separated from the sinus subtympanicum by the finiculus (Figure 9).
Attic
The endoscope permits a much better understanding of the anatomy of the attic and why it is distinct and separate from the mesotympanum both anatomically and in term of ventilation. Attic retraction pockets often present as isolated features with normal ventilation and findings in the mesotympanum. The concept of an epitympanic diaphragm has been advocated by clinicians, temporal bone histologists and pathologists31-33. However, this concept has not made much of an impression clinically because of the difficulty of communicating and understanding the difficult anatomy.
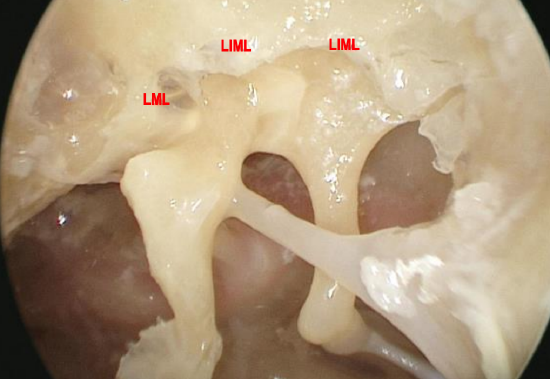
Figure 10: Left ear: Lateral attic is closed off from mesotympanum by lateral incudomallear and mallear ligaments. Note the relatively straight insertion line of the lateral incudomallear ligament (LIML) and the downward sloping insertion line of the lateral mallear ligament (LML)
The attic is a reasonably busy place and contains the bulk of the ossicular chain and many suspensory ligaments and folds. In the lateral attic, the lateral incudomallear and the lateral mallear folds form a lateral wall that does not allow for ventilation of the attic via the mesotympanum laterally (Figure 10). The anterior part of these lateral folds forms the medial wall of Prussak’s space.
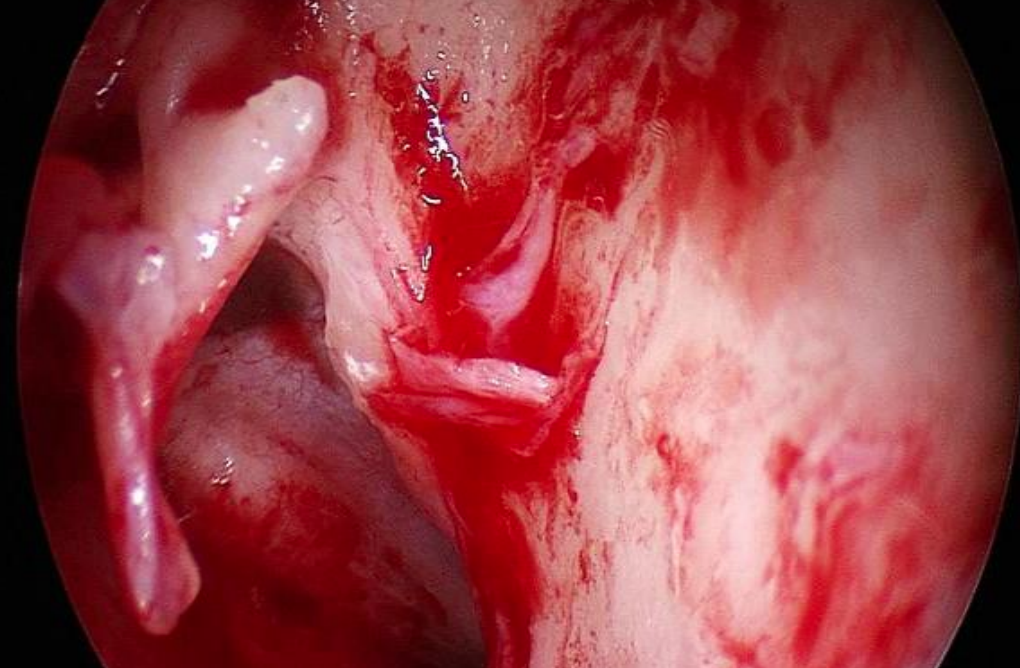
Figure 11: Right ear: Using a 70o endoscope and looking posterosuperiorly one sees a poorly developed supratubal recess. The tensor fold is seen as an almost horizontal structure
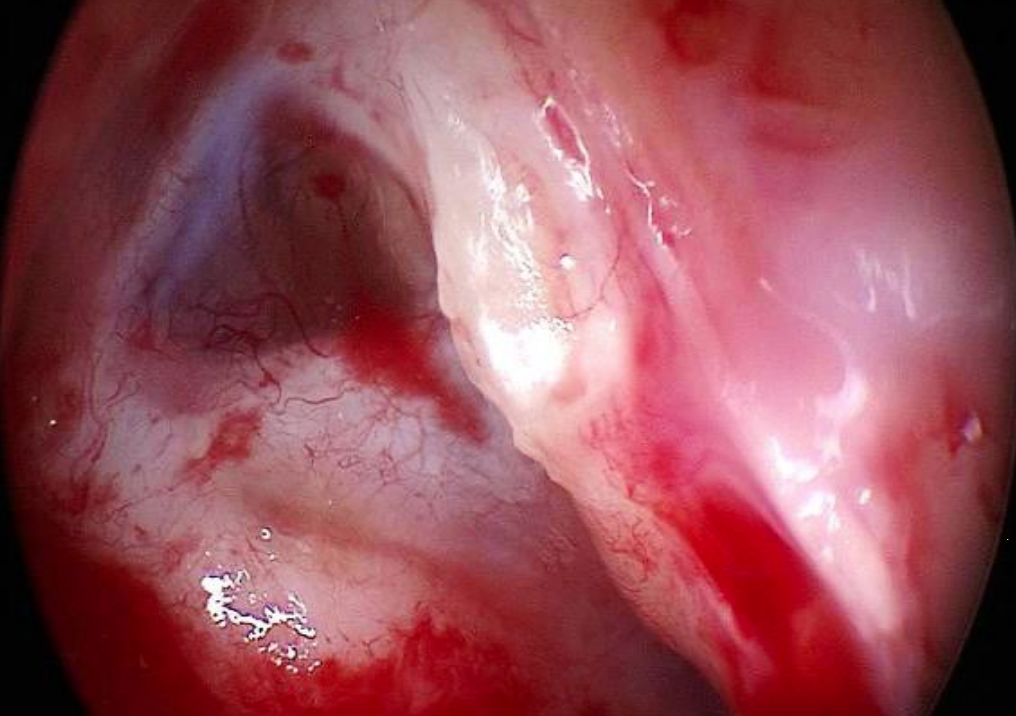
Figure 12: Right ear: Closeup view of the tensor fold seen in Figure 32
Anteriorly the attic is often separated from the mesotympanum and Eustachian tube by the folds of the tensor tympani. There are two main variations of this structure: The first is an almost horizontal orientation where the folds attach to the tensor tendon posteriorly and to the tympanic wall anteriorly very close the anterior tympanic spine (Figures 11 & 12).
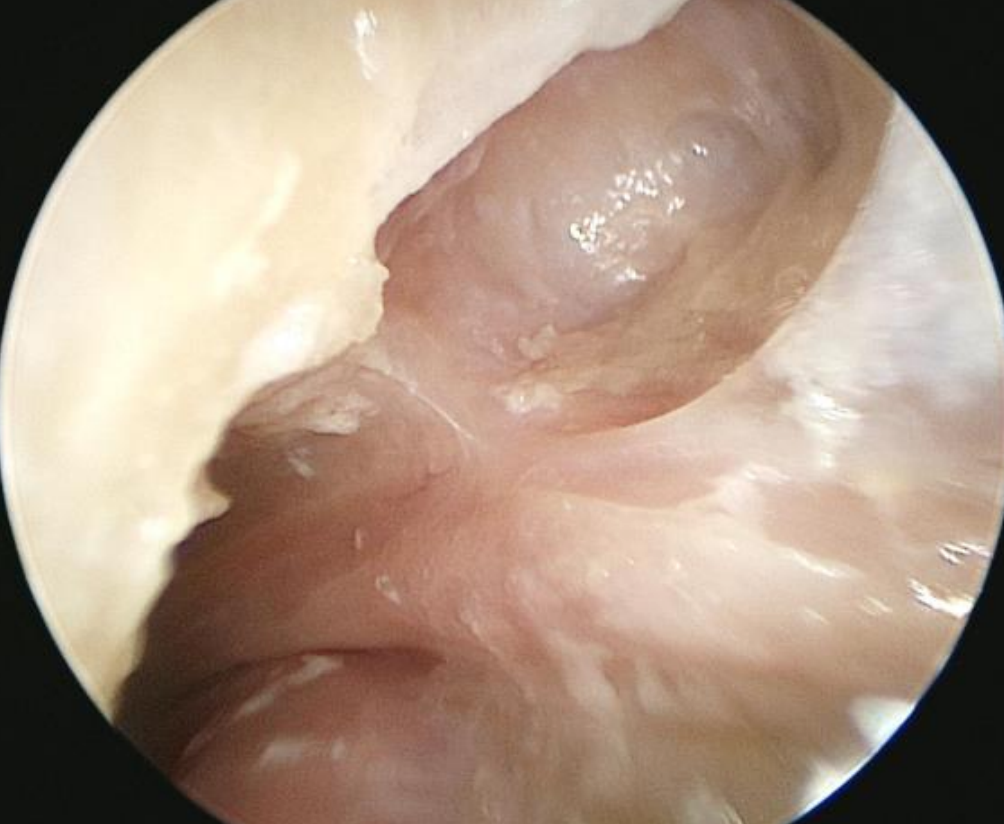
Figure 13: Left ear: Anatomy of tensor fold in a specimen with a well developed supratubal recess. The tensor fold is composed of two segments, a vertical part that attaches to the COG and a horizontal part that forms a partial floor of the supratubal recess
The second is when the supratubal recess is well developed and it pushes the folds to an almost vertical position (Figure 13).
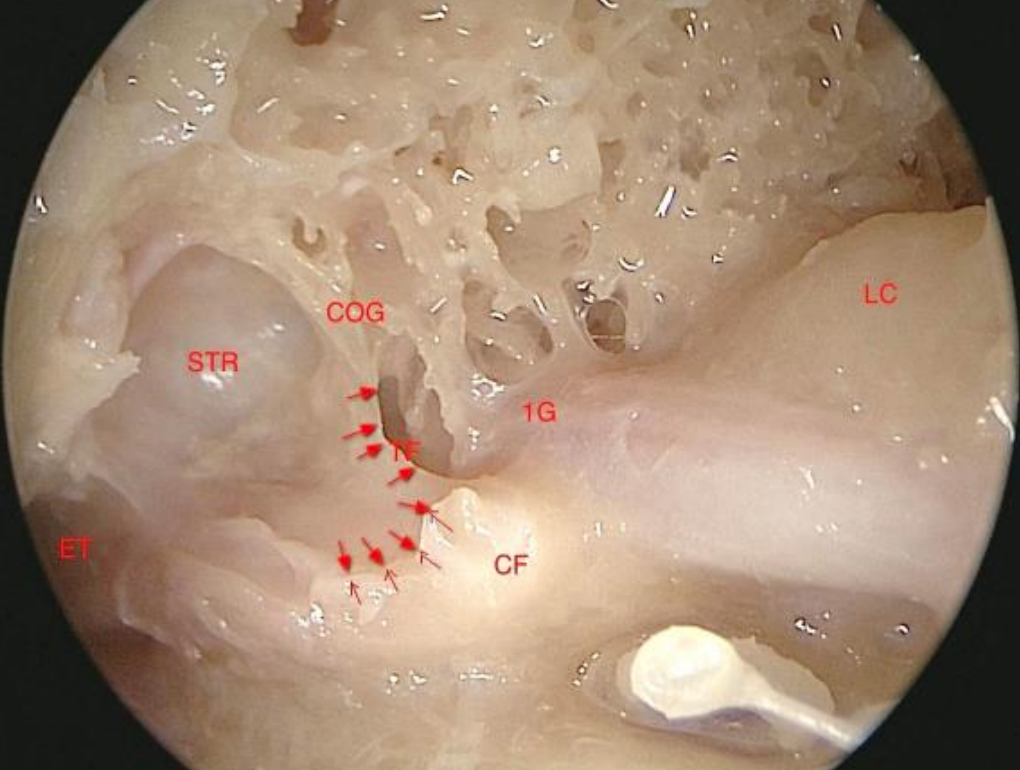
Figure 14: Left ear with tensor tendon transected, handle of malleus, anterior spine, anterior mallear ligament and chorda tympani removed: Note the distinction between the smooth wall of the supratubal recess and the numerous tags and excrescences of the anterior attic. (COG: Sheehy’s COG; TM: remnant of tensor fold; Single arrows: insertion of partially removed vertical segment of the tensor fold; Double arrows: insertion points of completely removed horizontal segment of tensor fold; STR: supratubal recess; ET: Eustachian tube; CG: cochleariform process; 1G: first genu of facial nerve and the geniculate ganglion; LC: lateral semicircular canal)
The attic and the supratubal recess are two distinct areas anatomically and developmentally. The supratubal recess is often a smooth-walled cavity compared to the attic wall that has numerous tags and excrescences. The transverse crest is a semicircular bony ridge that starts at the medial wall of the attic, runs across the roof, and then along the lateral wall of the attic. It marks the boundary between the tags and excrescences in the anterior attic and the smooth-walled supratubal recess (Figure 14).
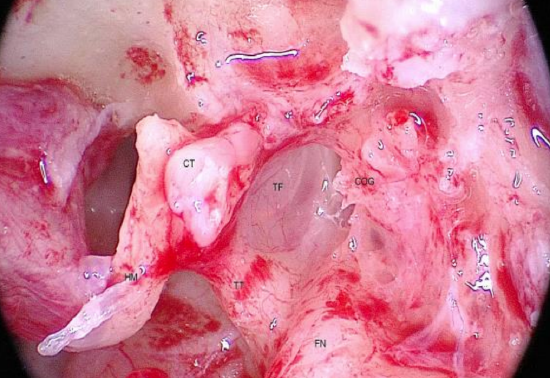
Figure 15: Left ear: Intraoperative view from posterior toward the anterior attic (FN: horizontal segment of facial nerve; HM: handle of malleus; CT: cut edge of chorda tympani; TT: tensor tympani tendon; TF: posterior aspect of tensor fold)
Its medial limb starts from the area of the cochleariform process and forms the COG, a commonly recognized surgical term for a bony protrusion on the medial wall of the anterior attic.34 The tensor fold always inserts more anteriorly than the COG; this leaves space for entrapment of cholesteatoma (Figure 15).
Developmentally the middle ear spaces evolve from four pouches or sacs (saccus anticus, saccus medius, saccus superior, and saccus posticus) that bud from the Eustachian tube35. The attic is formed from the saccus medius, which divides into three saccules i.e. anterior, medial, and posterior. The supratubal recess may be formed by the saccus anticus. The anterior saccule of the saccus medius meets the slower growing saccus anticus at the level of the semicanal of the tensor tympani, thus forming the horizontally aligned tensor tympani fold. The space thus formed above the tensor fold and anterior to the tensor tendon is the anterior attic compartment.36 Alternatively the saccus anticus may occasionally extend upward to the tegmen pushing the tensor fold into an almost vertical position and in the process, forming a well-developed supratubal space36. The expansion from the bony Eustachian tube to form the supratubal recess begins at a late foetal stage and continues throughout childhood37. By contrast, growth of the tympanic cavity, attic and mastoid antrum is virtually complete at birth.38
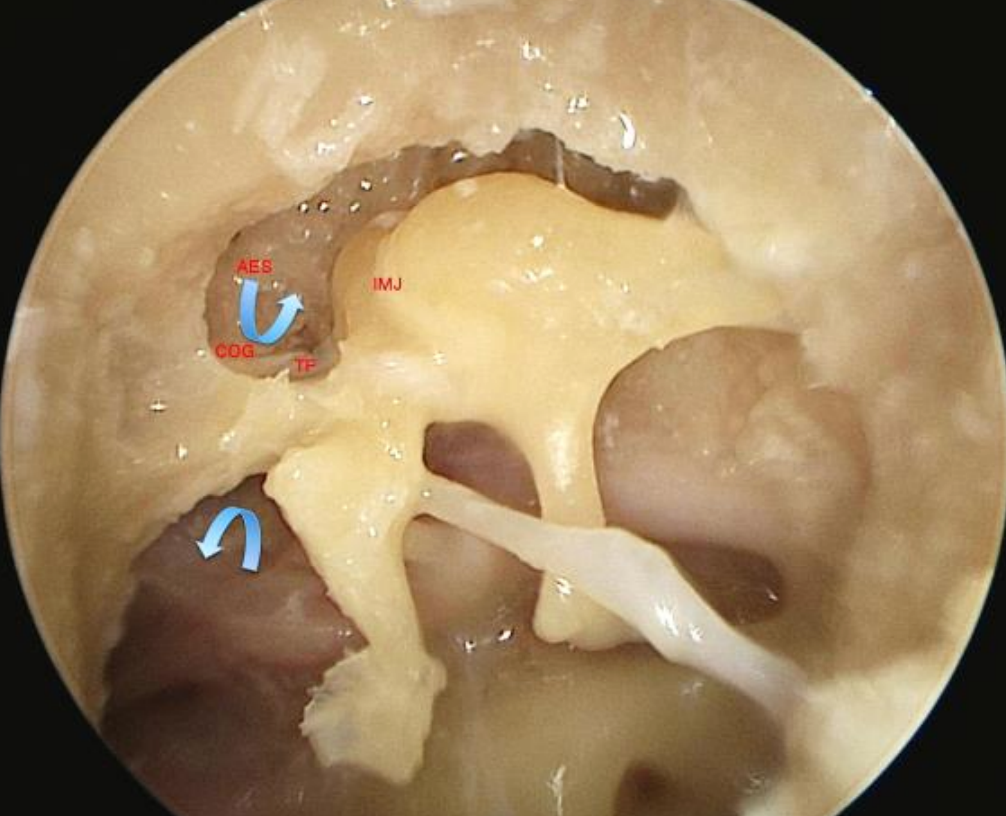
Figure 16: Left ear: Anterior attic separated from supratubal recess and Eustachian tube by tensor fold so that there is no direct communication or ventilation anteriorly between attic and Eustachian tube
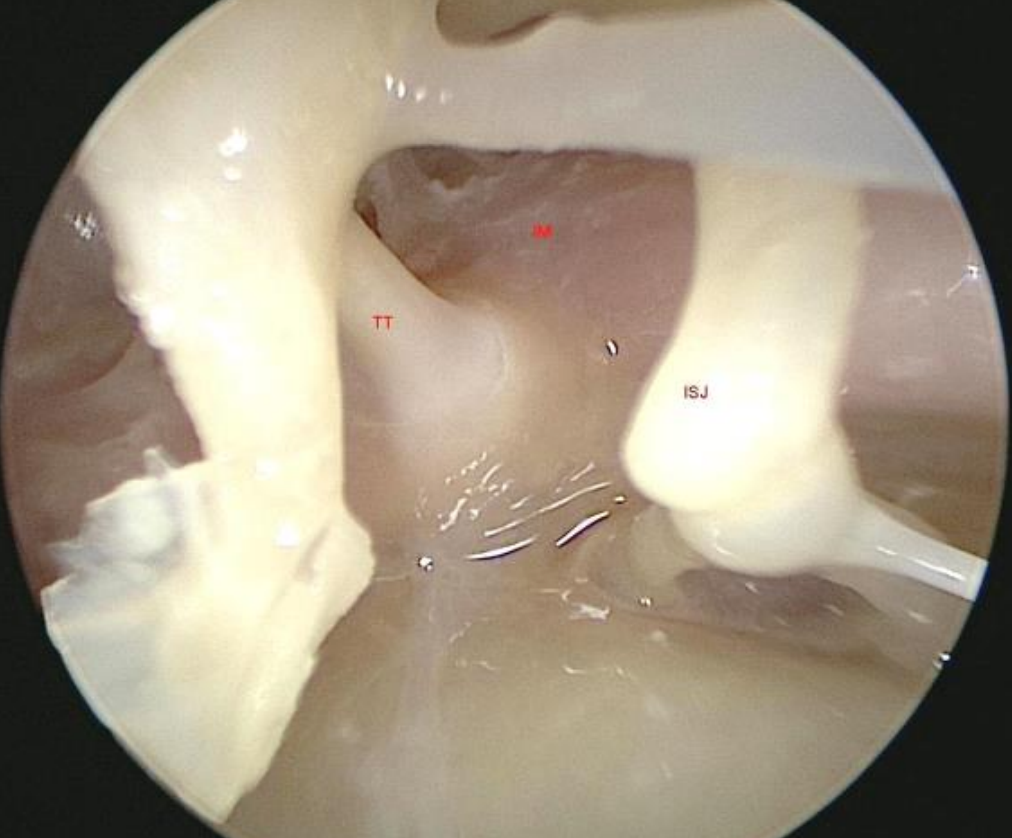
Figure 17: Left ear: IM: isthmus forms the only pathway for attic ventilation in the presence of complete tensor folds (TT: tensor tympani tendon; ISJ: incudostapedial joint)
With an intact tensor fold, a fully formed diaphragm separates the attic from the mesotympanum (Figure 16). This diaphragm is formed by the lateral incudomallear and mallear folds laterally and the tensor folds anteriorly. The only ventilation ports are through the anterior and posterior isthmi. The anterior isthmus extends between the incudostapedial joint and tensor tympani tendon (Figure 17).32
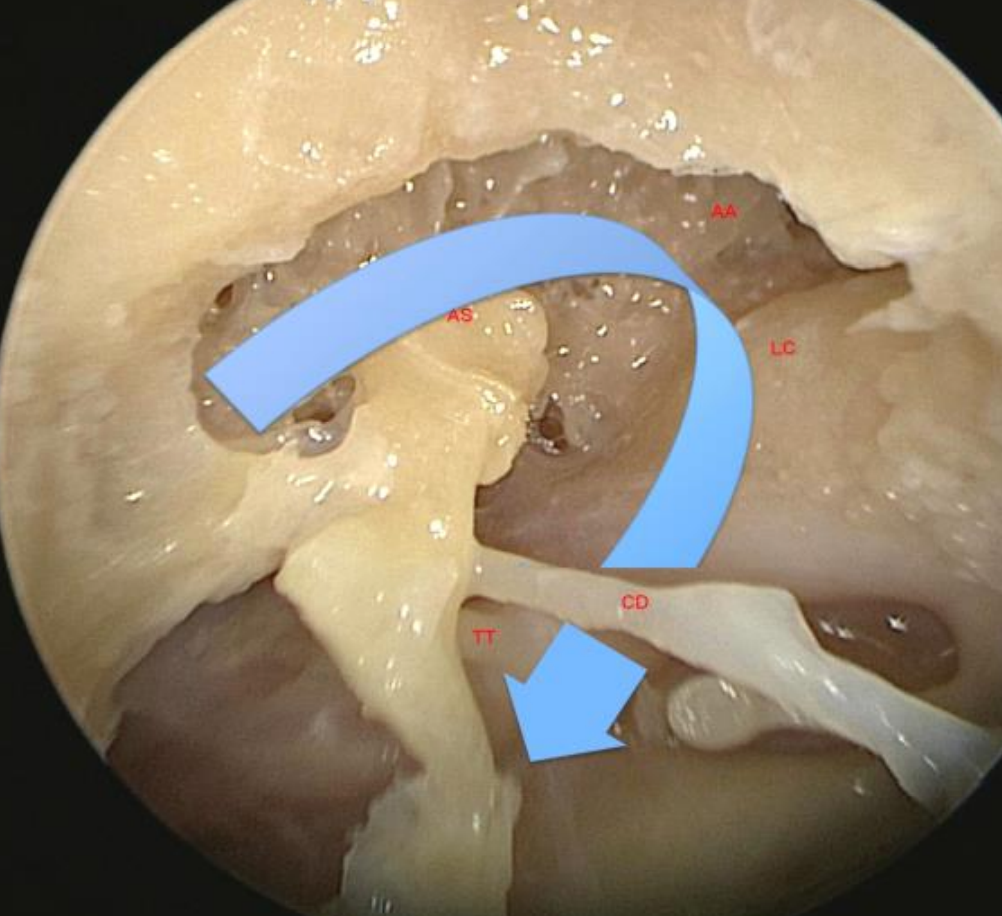
Figure 18: Left ear: Incus has been removed to demonstrate the long narrow channel for ventilation of the attic through the isthmus, medial attic, and upper attic
The posterior isthmus is the area posterior to the incudostapedial joint. It is often extremely narrow and contains the chorda tympani and pyramidal eminence. So the anterior isthmus or “isthmus” is the main path of attic ventilation via a very long channel that extends medial and then superior to the ossicles to ventilate the lateral and anterior attic (Figure 18). This long channel is also populated by other partial folds and suspensory ligaments which provide other opportunities for impaired ventilation.
Cholesteatoma: Technique & management algorithms
Preoperative planning based on high resolution CT and endoscopic examination is important. However definitive management decisions are made in the operating room and patients need to understand the range of possible interventions that may be used.
Three endoscopic approaches may be used for cholesteatoma. These echo principles and lessons borrowed from traditional tympanomastoid surgery.
- Endoscopic transcanal management of limited cholesteatoma
- Endoscopic open cavity management of cholesteatoma
- Expanded transcanal approach to cholesteatoma
The first question to ask whether the ear canal provides an adequate port for complete removal of cholesteatoma?
- If the answer is “yes”, then endoscopic transcanal management of limited cholesteatoma is employed; a wide tympanomeatal flap is elevated, atticotomy performed, the sac is identified and is pursued along with removal of overhanging bone
- If the answer is “no”, then an expanded transcanal approach is used; This entails improving transcanal access by removing skin of the ear canal and enlarging the bony canal
The mastoid then needs to be addressed
- Limited cholesteatoma that extends only to the aditus ad antrum can be completely removed through a transcanal approach
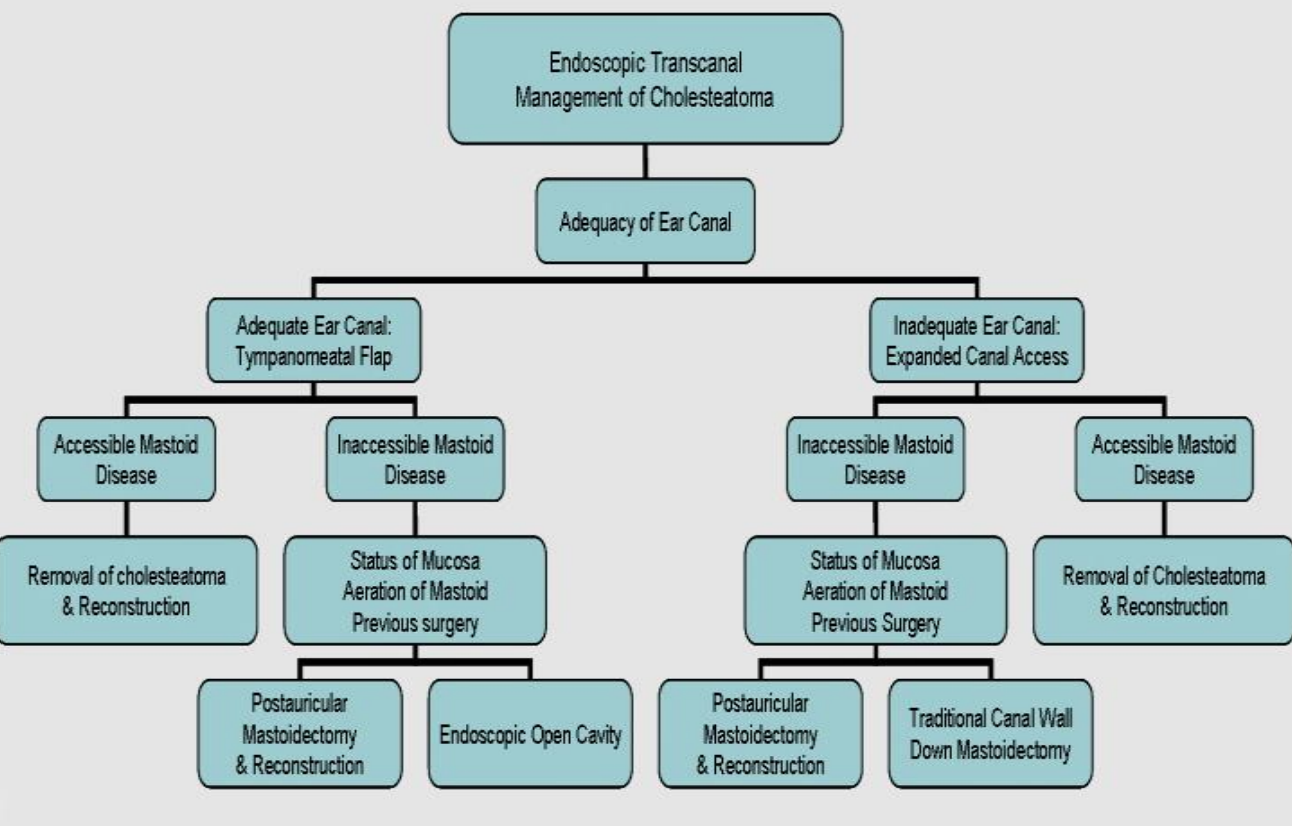
Figure 19: Algorithm: Endoscopic Transcanal Management of Cholesteatoma
- If the mastoid is involved, a decision is made whether to address the disease through a postauricular mastoidectomy or whether to exteriorize it by endoscopic open cavity management of the cholesteatoma; this entails aggressive removal of bone superiorly and posteriorly all the way to the mastoid cavity proper (Figure 19).
Endoscopic transcanal management of limited cholesteatoma
The attic (especially anterior part) is poorly visualized via traditional microscopic approaches. An endoscopic approach however enables a surgeon to start in the mesotympanum and follow the sac along its twists and turns around the ossicles and ligaments. This good access facilitates better preservation of the ossicles while ensuring complete removal of matrix, rather than piecemeal removal via different access ports.
Technique
A wide posterior tympanomeatal flap is elevated. The sac is pursued under direct vision and the bony rim is curetted or drilled just enough to enable dissection to be continued under direct vision. Appropriate ossicular chain work is done, and the attic defect is closed with a composite tragal graft.
Clinical example
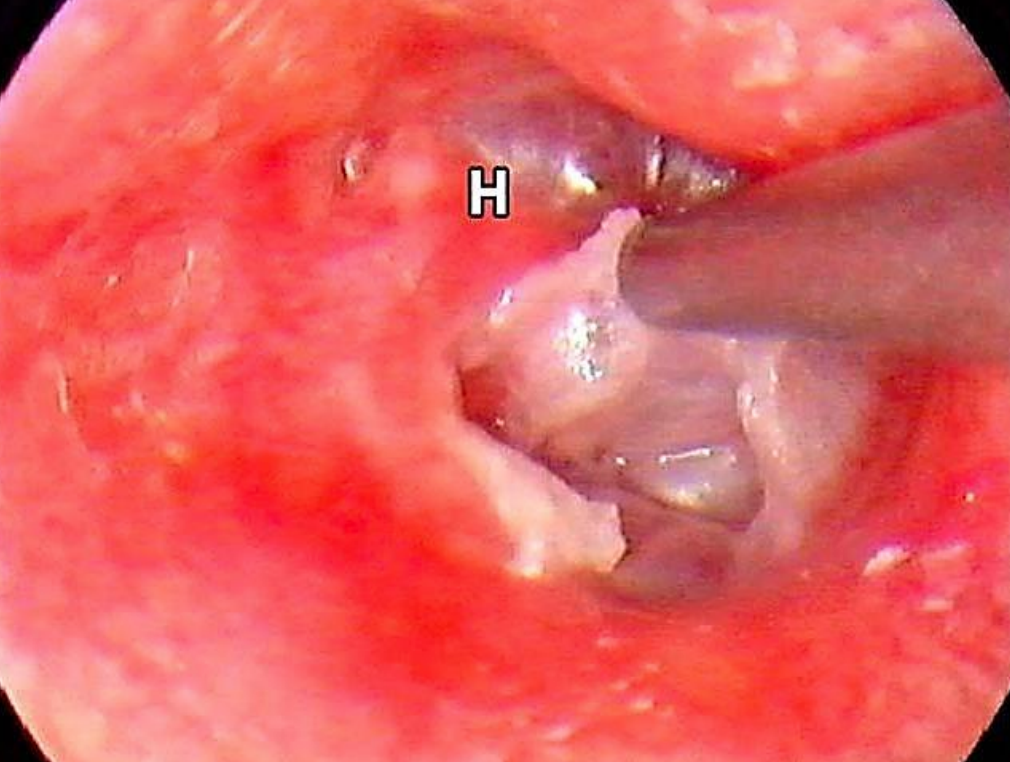
Figure 20: Right ear: Retraction and cholesteatoma (H: handle of malleus)
Figure 20 shows a right ear with evidence of severe retraction and debris in a cholesteatoma sac.
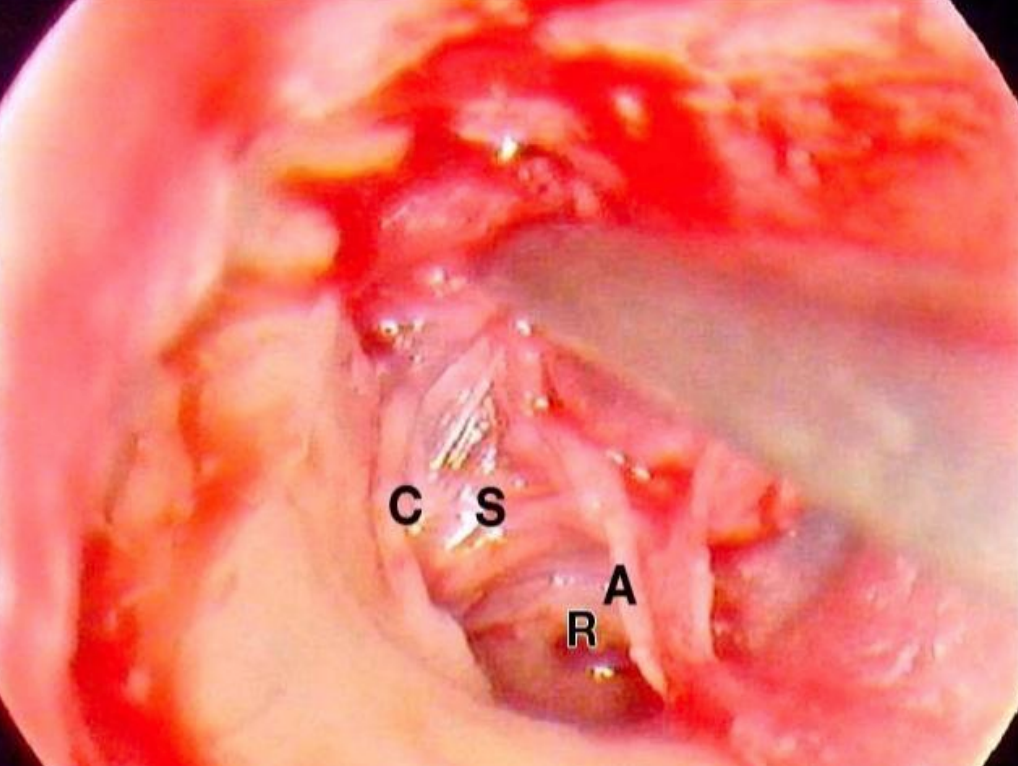
Figure 21: Right ear: Tympanomeatal flap has been elevated, middle ear has been entered, and cholesteatoma sac has been exposed (C: chorda tympani; S: cholesteatoma sac; A: annulus; R: round window)
Endoscopic transcanal approach was undertaken, a wide tympanomeatal flap was elevated, and the middle ear was entered (Figure 21).
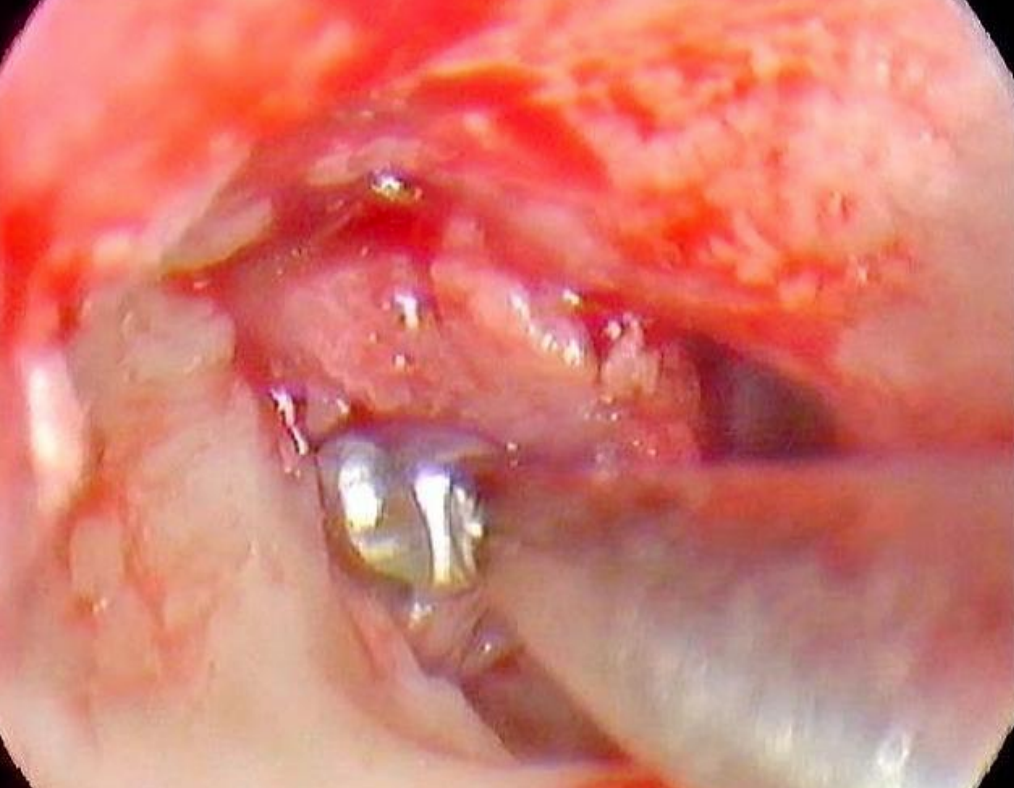
Figure 22: Right ear: wide atticotomy performed with curette
A wide atticotomy was performed with a curette (Figure 22).
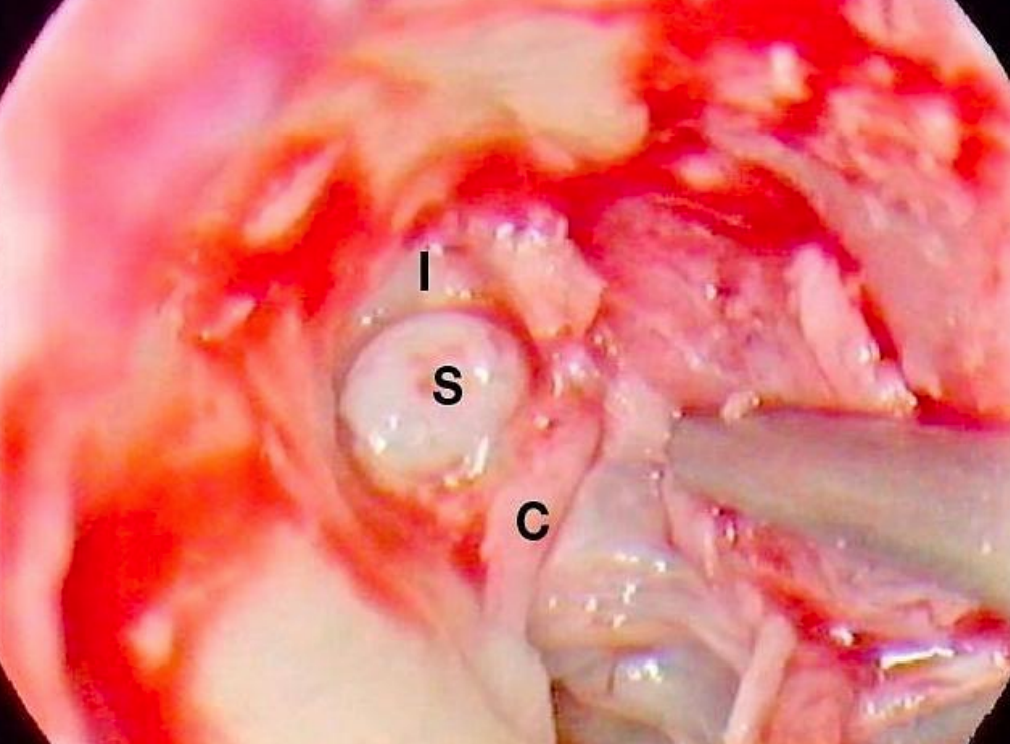
Figure 23: Right ear: Sac (S) has been pulled down from attic, lateral to body of incus and medial to scutum. Body of incus (I) can be seen. Chorda (C) forms a collar around the neck of the sac
The cholesteatoma sac was identified; it extended to the lateral attic and was pulled downward lateral to the body of the incus and medial to the removed scutum (Figure 23).
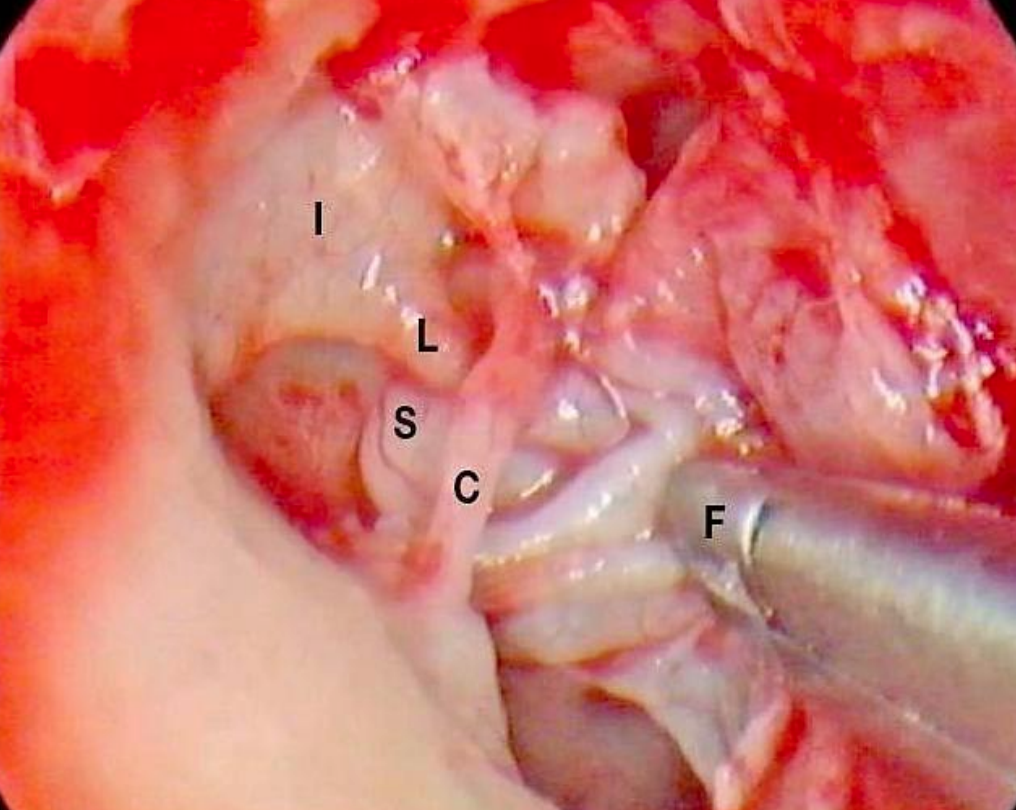
Figure 24: Right ear: Sac has been completely delivered from area lateral to body of incus (I), but another process of the sac (S) has rotated posteriorly and medially around the incudostapedial joint, medial to long process of the incus (L). Cupped forceps (F) are used to pull the sac from underneath the chorda (C)
Another extension of the sac had rotated posteriorly and medially around the incudostapedial joint and the superstructure of the stapes and had advanced medial to the long process of the incus (Figure 24).
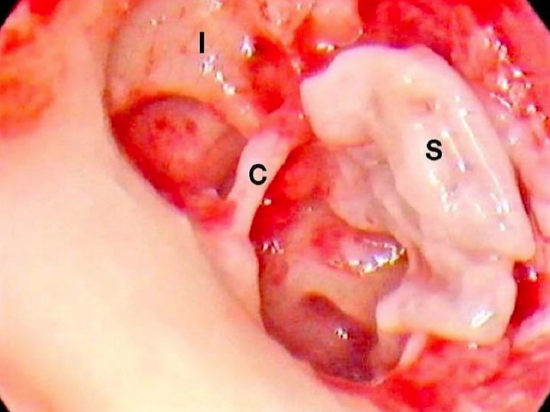
Figure 25: Right ear: Sac (S) has been completely delivered and deflected over the tympanomeatal flap with incus (I) and chorda (C) in view
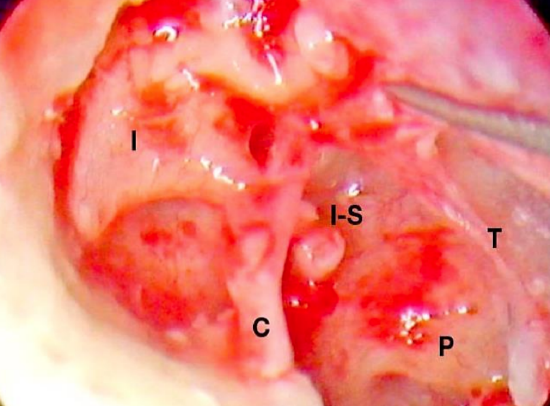
Figure 26: Right ear: Sac is removed. Cholesteatoma has eroded incudostapedial joint (I-S). The incus (I), chorda (C), and promontory (P) are clearly seen. The anterior edge of the tympanic membrane retraction (T), now a perforation, is also visible
The sac is delivered (Figure 25). It was evident that the sac had eroded the incudostapedial joint (Figure 26).
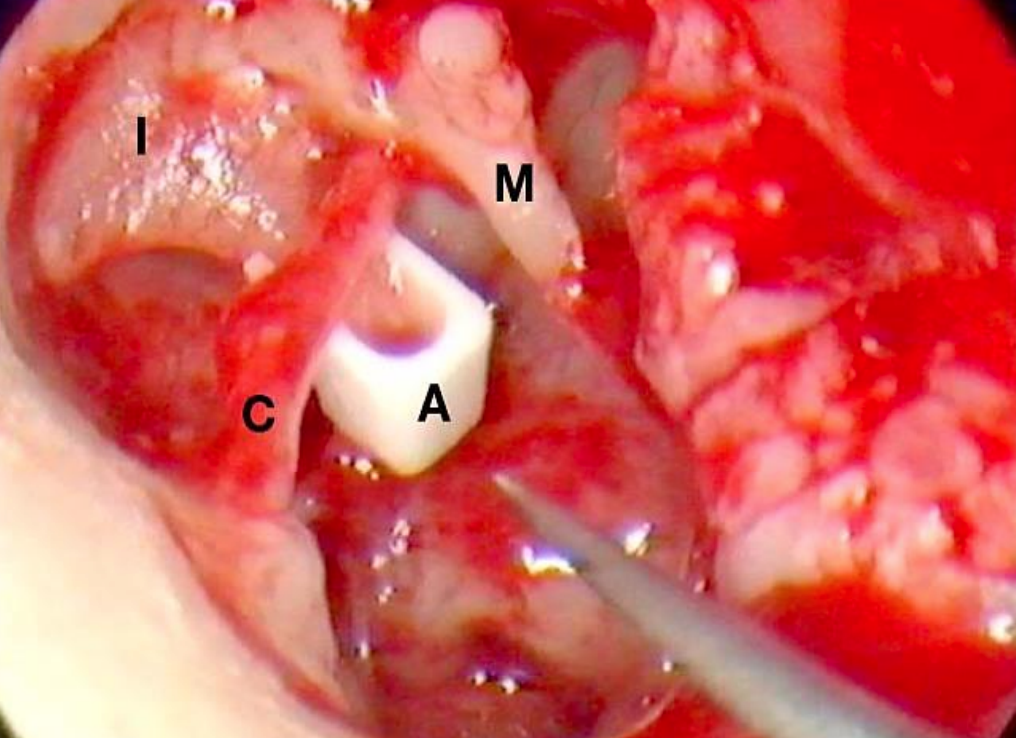
Figure 27: Right ear: A prosthesis (A) is used to reconstruct the incudostapedial joint. Handle of malleus (M) and incus (I) and chorda (C) are seen
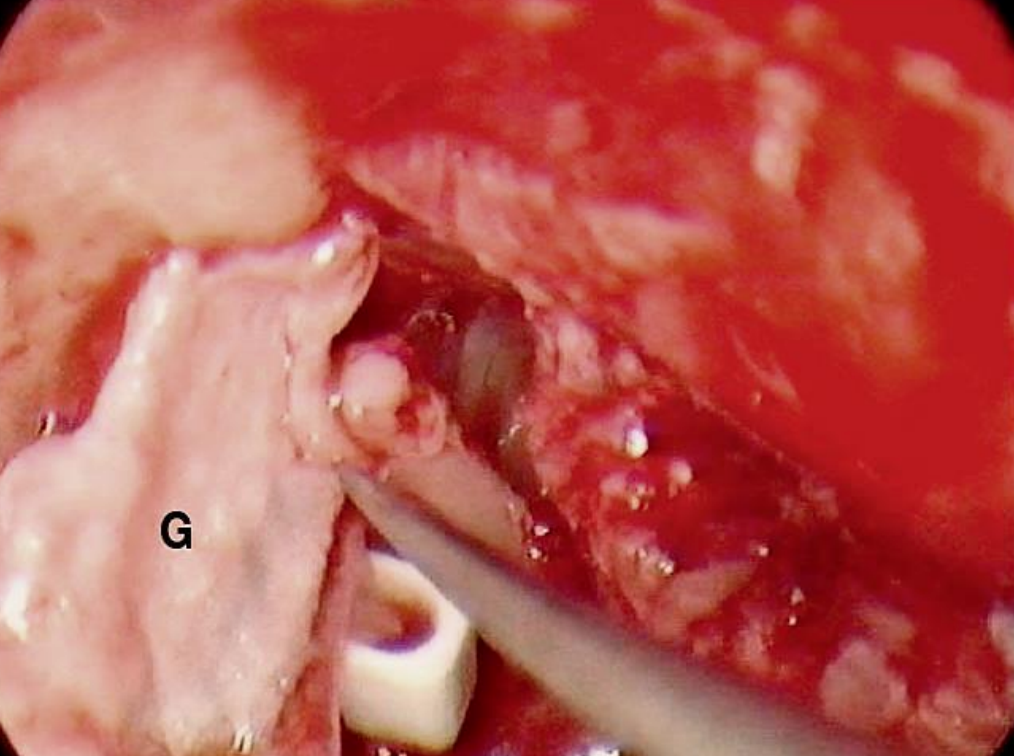
Figure 28: Right ear: Attic defect being reconstructed with a composite tragal cartilage graft (G)
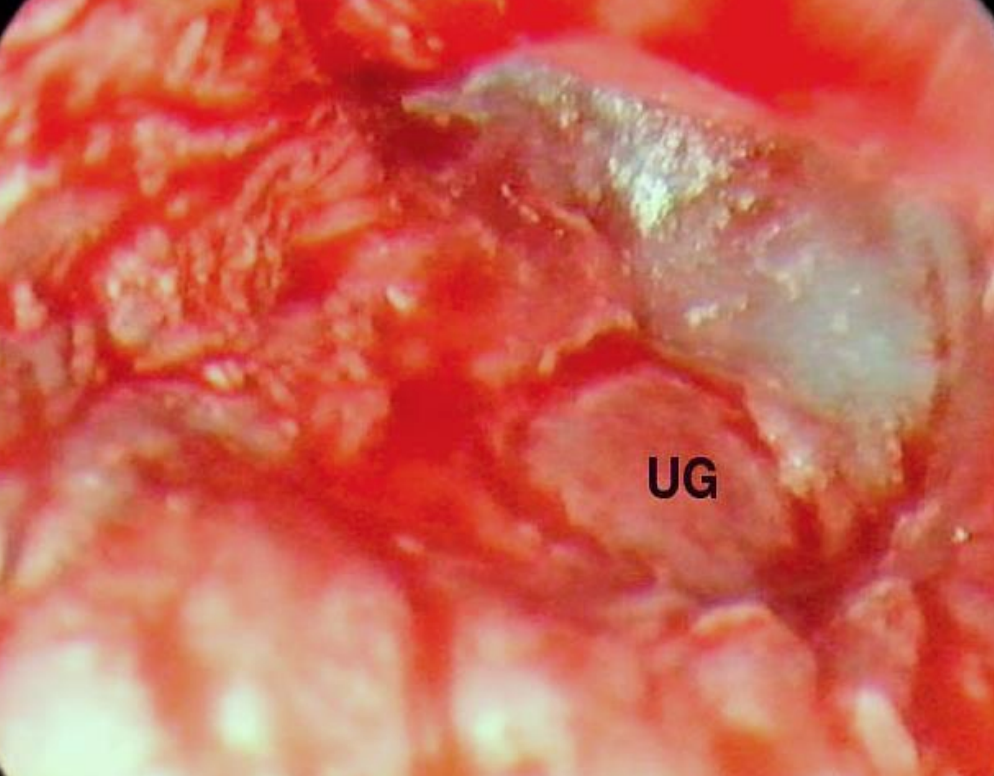
Figure 29: Right ear: Tympanomeatal flap is repositioned over underlay graft (UG)
A prosthesis was used to reconstruct the ossicular chain (Figure 27). A tragal composite graft with perichondrium was used to reconstruct the attic defect (Figure 28). The defect in the tympanic membrane was reconstructed with a perichondrial underlay graft, and the tympanomeatal flap was repositioned (Figure 29).
Endoscopic open cavity management of cholesteatoma
In canal wall down procedures all disease containing cavities are exteriorized to provide aeration and direct access to the disease in an ambulatory (clinic) setting. However, during the process of accessing the disease, large cavities that may require lifelong maintenance are created. In addition, unpredictable healing, fibrosis, and meatal stenosis, which are associated with postauricular canal wall down procedures, may prevent later ossicular reconstruction.
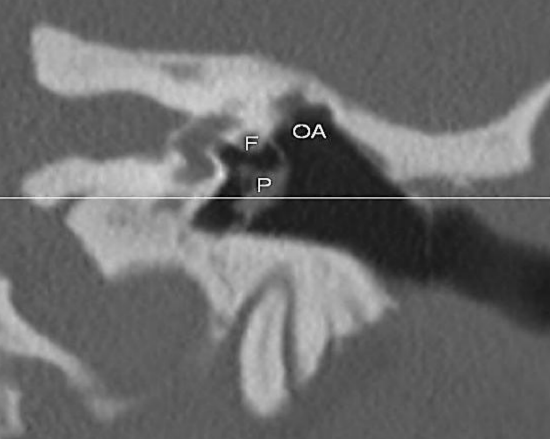
Figure 30: Left ear: Coronal CT following endoscopic open cavity management of cholesteatoma. Neotympanic membrane is reconstructed up to level of horizontal segment of facial nerve (FN); attic is left open (OA)
Endoscopic techniques permit transcanal exploration of disease-containing area without opening areas that are not involved by cholesteatoma. The transcanal endoscopic approach opens only diseased areas, preserves many healthy air cells, and leaves the cortical bone intact. It also allows one to create two separate cavities; a small reconstructed tympanic cavity that conducts sound through the middle ear and is small enough to be serviced by the (usually dysfunctional) eustachian tube, and a larger attic, antrum, and mastoid cavity, which is joined to the ear canal and exteriorized (Figure 30).
Such an approach was described by Tos in 1982.27 It enables one to reconstruct the middle ear in a highly predictable fashion, and in turn creates a better foundation for ossicular and tympanic membrane reconstruction.
A major concern for many surgeons is the possibility of closing off an open attic. This concern is based on results of traditional open mastoid surgery in which damage to the cartilaginous ear canal produces a vicious circle: trauma to the ear canal causes fibrosis and narrowing of the meatus which forces the surgeon to design a more aggressive meatoplasty which in turn causes more trauma, secondary fibrosis, and narrowing. A large meatus is created to compensate for fibrosis and narrowing. In contrast, the very limited trauma to the cartilaginous ear canal caused with endoscopic surgery allows surgeons to avoid such complications and produces a small, shallow, benign, problem-free cavity.
Technique
With endoscopic open cavity management of cholesteatoma, a wide posterior tympanomeatal flap is elevated as described above. A transcanal atticotomy is performed. The incus and head of malleus are removed from the attic. Aggressive bone removal is then performed to provide open endoscopic access to the attic and all the way into the antrum posteriorly. Tympanic membrane defects inferior to the horizontal segment of the facial nerve (including atelectatic areas) are reconstructed with perichondrial grafts which are placed directly onto the horizontal segment of the facial nerve superiorly and on a bed of Gelfoam packed in the middle ear inferiorly. The ear canal and opened attic are then packed with Gelfoam. This technique should result in a small, closed, reconstructed tympanic cavity and membrane anteriorly and inferiorly (to service the impedance-matching function of the middle ear) and an open attic and antrum superiorly and posteriorly (Figure 30).
Clinical example
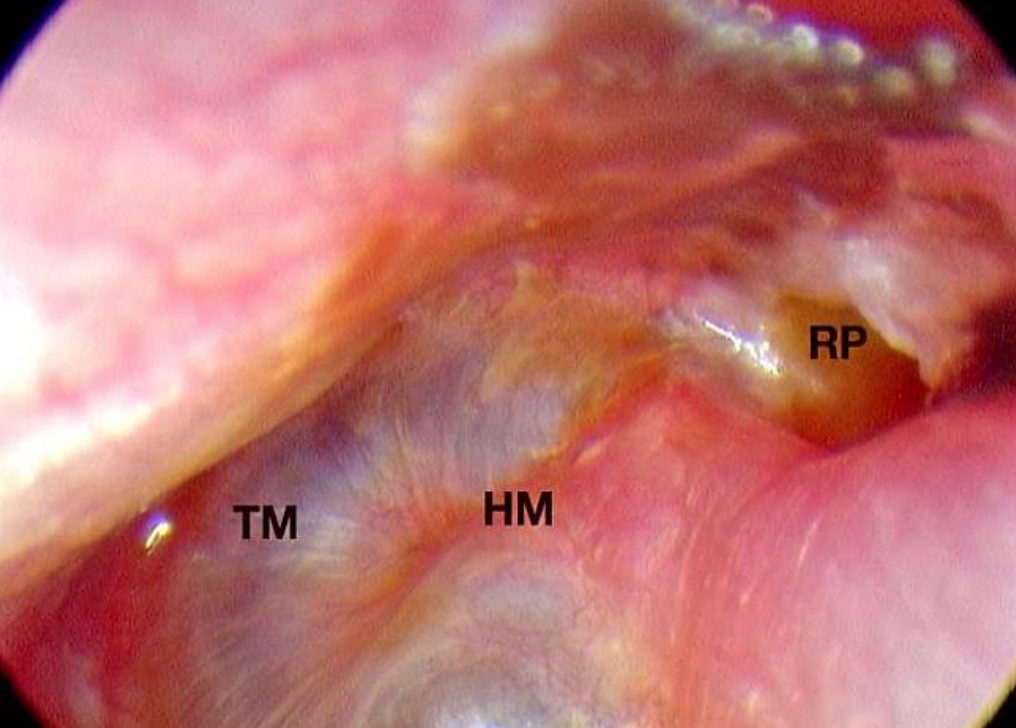
Figure 31: Left ear: Large retraction pocket (RP) with recurrent infections and granulation tissue (HM, handle of malleus; TM, tympanic membrane)
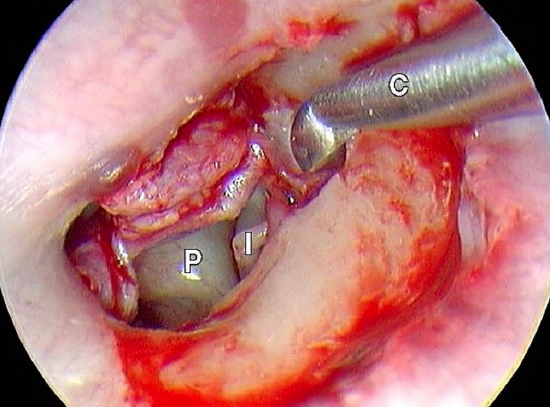
Figure 32: Left ear: Wide tympanomeatal flap is elevated. Promontory (P) and incudostapedial joint (I) are seen. A curette (C) is used to create an extended atticotomy
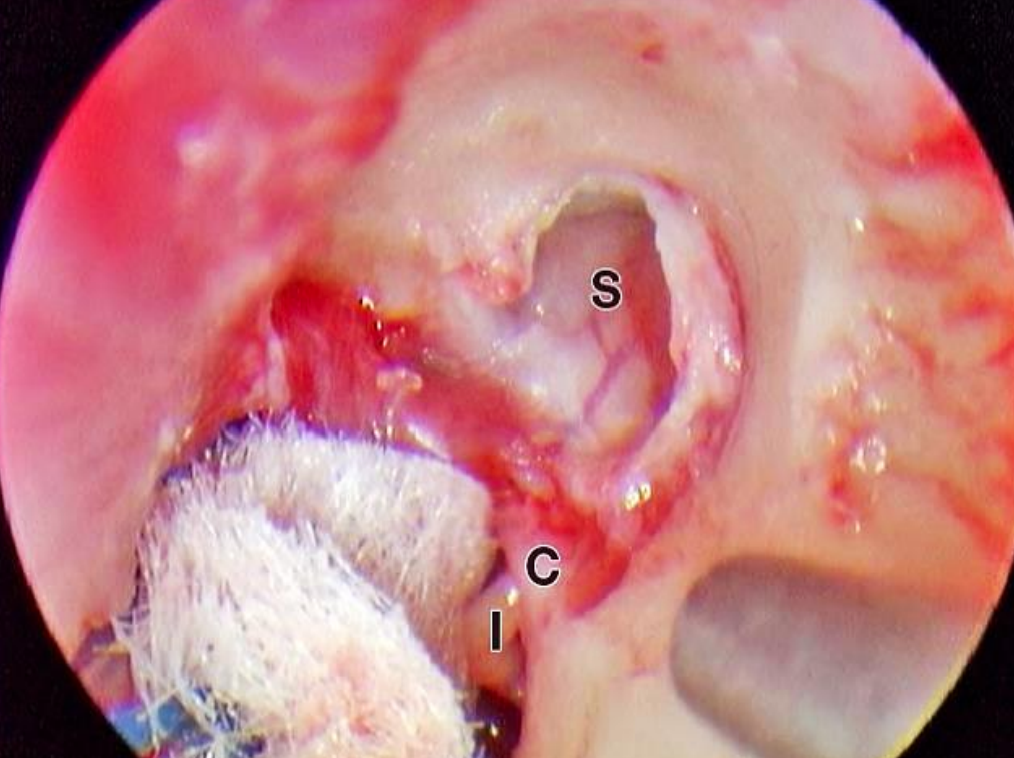
Figure 33: Left ear: Extended atticotomy and thick sac (S); (C, chorda tympani; I, incudostapedial joint)
Figure 31 shows a large attic retraction pocket after it was emptied of dermal debris. A wide tympanomeatal flap has been elevated and a thick vascularized sac can be seen after the atticotomy was extended (Figures 32 & 33).
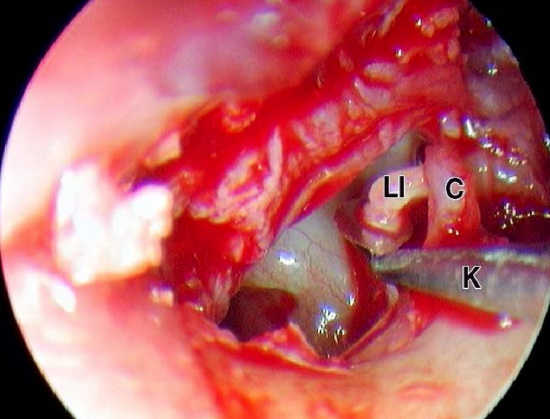
Figure 34: Left ear: Incudostapedial joint (LI) is dislocated with a small round knife. (C, chorda tympani)
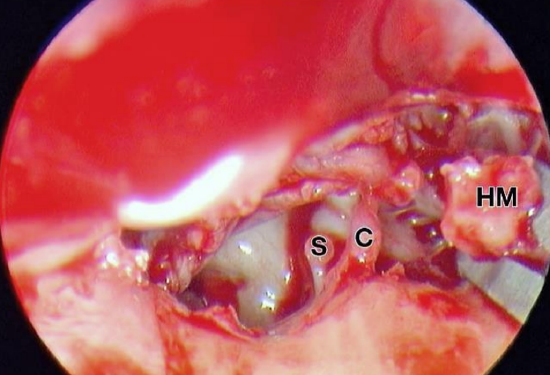
Figure 35: Left ear: Incus has been removed and head of malleus (HM) is being extracted. Note that head of malleus is separated from handle with malleus nipper proximally to preserve ligaments stabilizing handle of malleus. S, stapes; C, chorda tympani
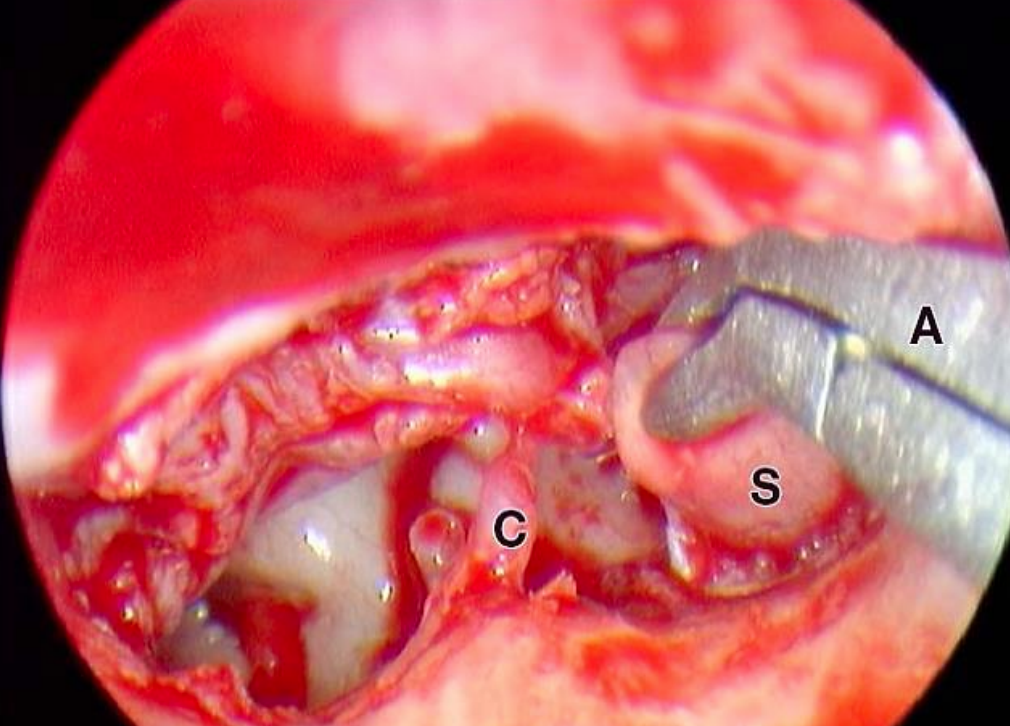
Figure 36: Left ear: Sac (S) being delivered (C, chorda tympani)
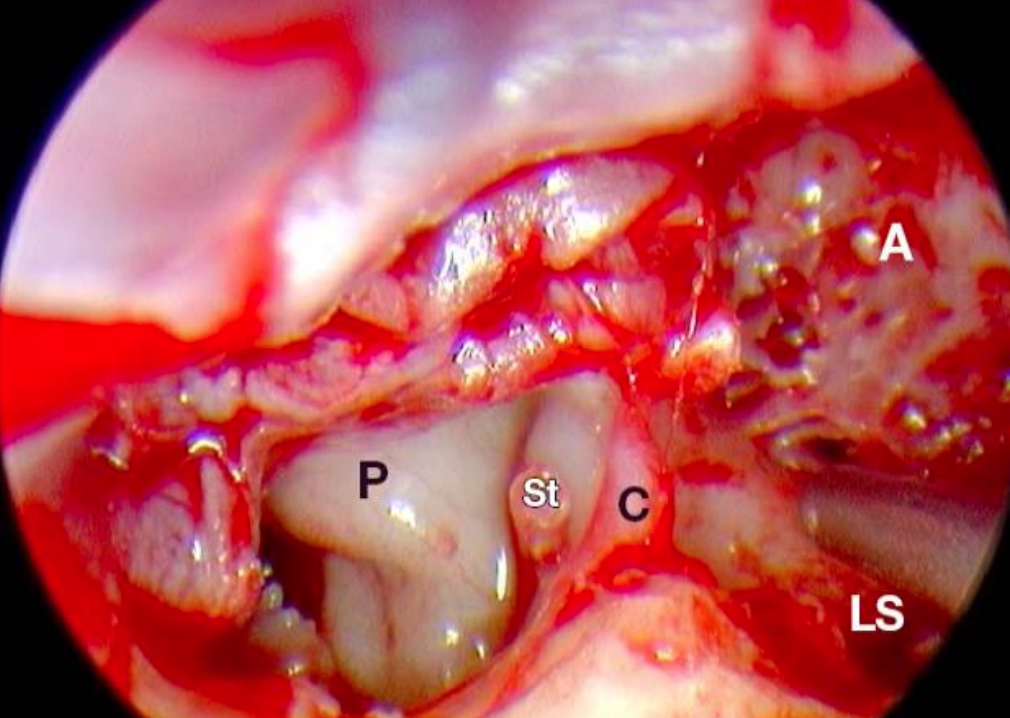
Figure 37: Left ear: Sac has been completely removed. (A, Attic; P, promontory; C, chorda tympani; S, stapes; LS, lateral semicircular canal)
The incus and the head of malleus were removed after dislocating the incudo-stapedial joint (Figures 34, 35). The anterior epitympanum was cleared of disease. The remainder of the sac deep to the removed ossicles was removed after further widening the atticotomy (Figure 36). All disease was excised and specific attention was paid to the attic and the tympanic cavity (Figure 37).
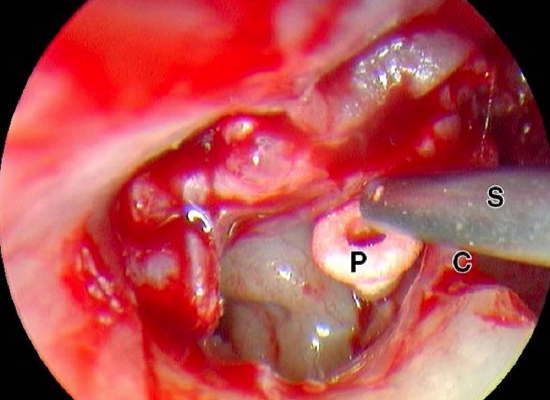
Figure 38: Left ear: Ossicular chain reconstructed with a prosthesis (P). C, chorda tympani; S, suction
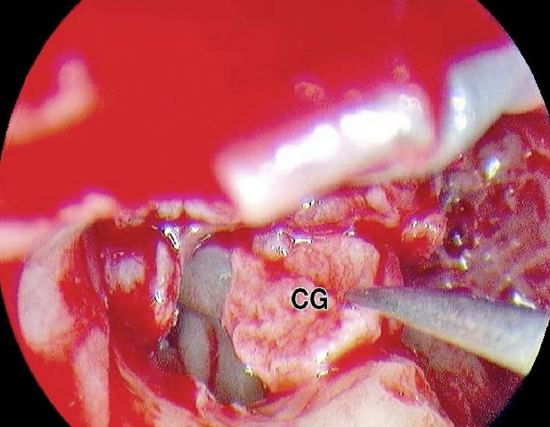
Figure 39: Left ear: Composite tragal cartilage (CG) is used on top of prosthesis
A prosthesis is used to reconstruct the ossicular chain (Figure 38) and a composite cartilage graft is positioned on top of the prosthesis (Figure 39).
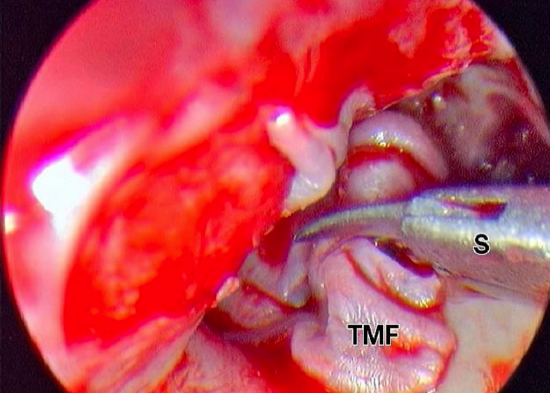
Figure 40: Left ear: Tympanomeatal flap is cut longitudinally with middle ear scissors
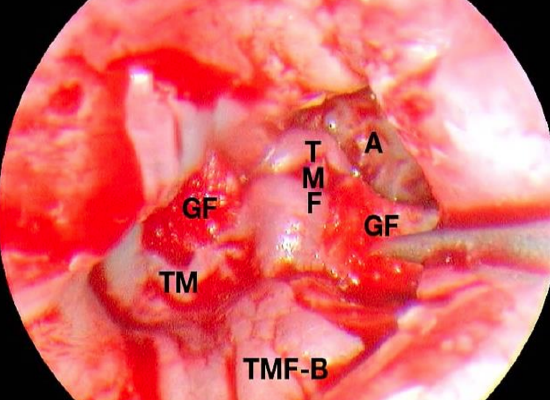
Figure 41: Left ear: Inferior part of tympanomeatal flap (TMF-B) is repositioned over ear canal while superior part of tympanomeatal flap (TMF) is reflected over horizontal segment of facial nerve into open attic (A). Small pieces of gelfoam (GF) are used to pack open the attic and ear canal. (TM, tympanic membrane)
The tympanomeatal flap is divided longitudinally (Figure 40); the inferior part is positioned over the ear canal, the superior part is draped over the horizontal segment of the facial nerve (Figure 41), and the attic is packed open with small pieces of gelfoam.
Expanded transcanal access to middle ear and petrous apex
Although the endoscope allows a more expanded transcanal access to the middle ear compared to the microscope, a small, angulated ear canal can sometimes be very limiting and preclude adequate exposure. In order to perform adequate and safe endoscopic surgery, as well as to provide wide access to disease in the anterior part of the middle ear, eustachian tube and petrous bone, it is essential to overcome limitations that may hamper access prior to addressing the disease.
Technique
The extent of the disease is determined by endoscopic examination and review of CTs of the temporal bone. The anterior part of the middle ear, eustachian tube, and significant disease within the hypotympanum often require an expanded transcanal approach. After defining factors in the ear canal that restrict access one has to decide whether to address such factors.
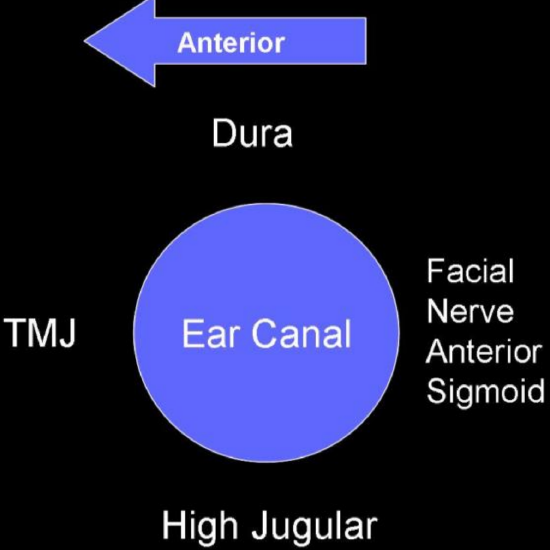
Figure 42: Structures to be considered when enlarging the ear canal
When enlarging the ear canal the surgeon needs to be keenly aware of important structures that lie in close proximity (Figure 42). One should also think of all the structures that border the tympanic cavity when enlarging the ear canal. The bony annulus has wide anatomical variations.39 Posteriorly are the facial nerve and sigmoid sinus.40 Inferiorly, a high jugular bulb may be laterally located and abut the ear canal.41 Breaching the glenoid fossa anteriorly is usually a non-event, but can be a limiting factor.
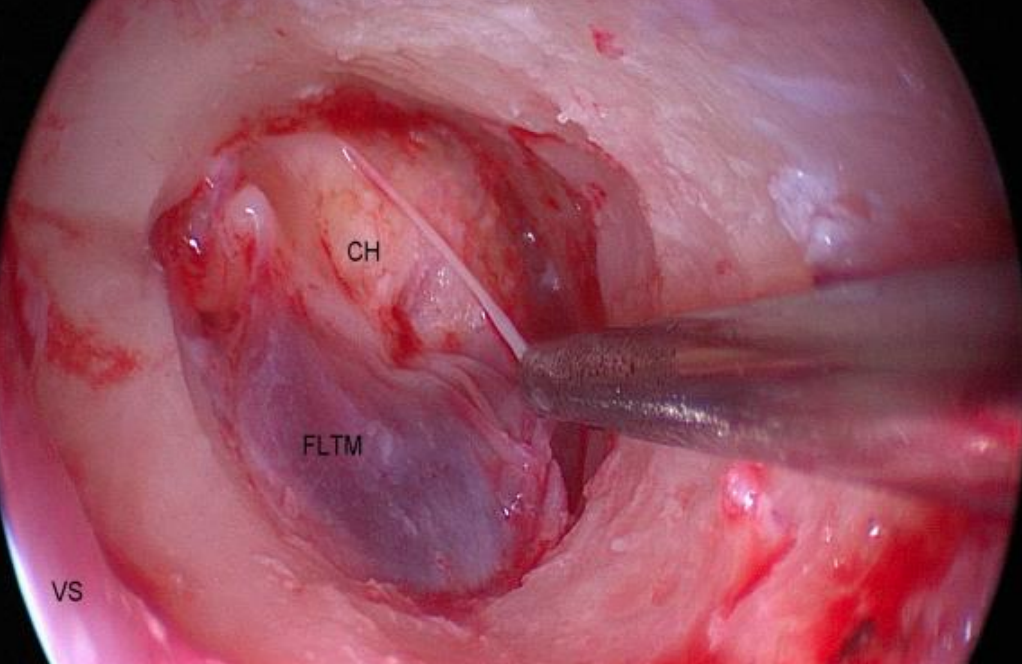
Figure 45: Right ear: Skin of ear canal is elevated in continuity with the epithelial layer of tympanic membrane with preservation of vascular strip, followed by enlargement of ear canal. VS: vascular strip; FLTM: fibrous layer of tympanic membrane; CH: cholesteatoma
The expanded transcanal approach is similar to Sheehy's lateral graft tympanoplasty. The skin of the ear canal is removed along with the epithelial outer layer of the tympanic membrane. A vascular strip is preserved (Figure 45). The ear canal is enlarged with a drill as needed. The annulus and fibrous layer of the tympanic membrane are elevated either partially or completely to provide access. The entire overhanging bony annulus is curetted to provide wide access to the middle ear. After the necessary ossicular chain work has been completed the remaining tympanic membrane is repositioned, a lateral graft is applied, and the skin of the ear canal is repositioned and held in place with packing.
Clinical example
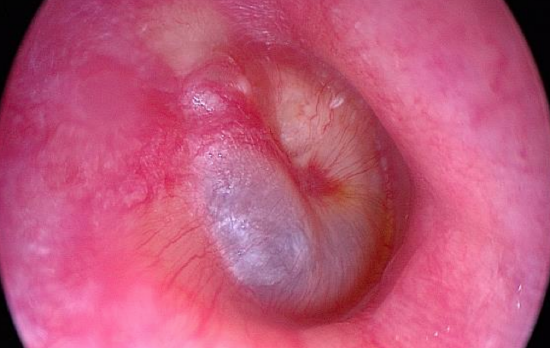
Figure 43: Right ear: Anterior whitish lesion behind intact tympanic membrane
A patient with longstanding right-sided hearing loss and dizziness had an anteriorly located whitish lesion behind an intact tympanic membrane (Figure 43).
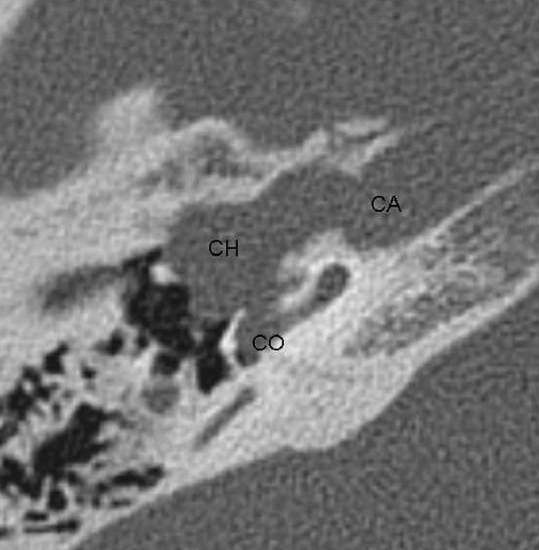
Figure 44: Right ear: Axial CT of temporal bone. CO: basal turn of cochlea; CA: carotid artery; CH: cholesteatoma
Audiometry indicated a “dead” right ear. CT scan showed extensive cholesteatoma of the petrous bone eroding cochlea and carotid artery (Figure 44). Using an "expanded transcanal access" technique, the vascular strip is preserved, the ear canal skin is removed, the fibrous layer of the tympanic membrane is preserved, and the ear canal is enlarged (Figure 45).
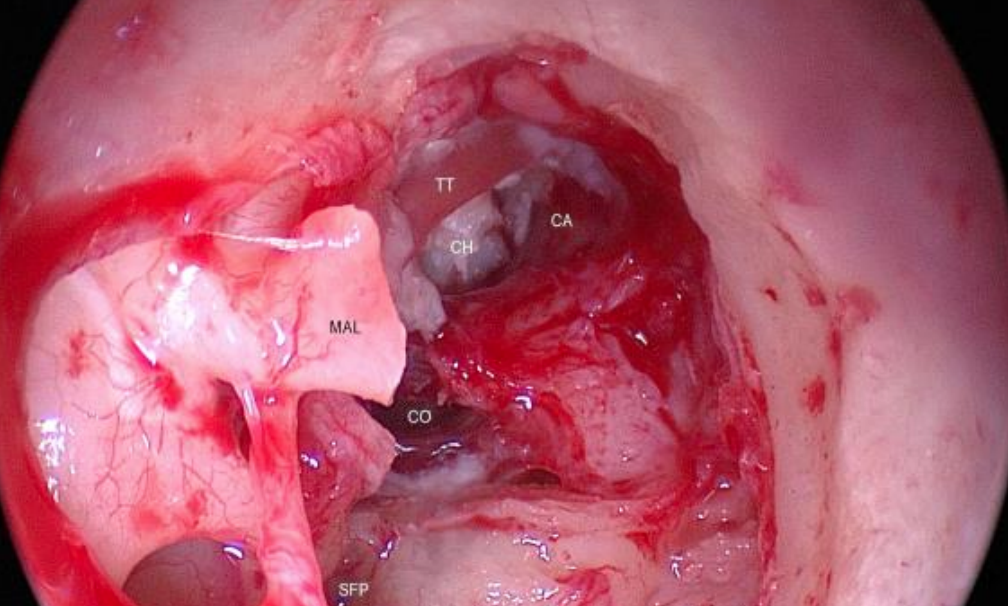
Figure 46: Right ear: Much of the cholesteatoma eroding the cochlea has been removed (MAL: malleus with handle transected; SFP: stapes footplate; CO: eroded middle turn of the cochlea; CA: eroded carotid artery canal; CH: cholesteatoma in petrous apex surrounding TT: tensor tympani muscle)
An extensive cholesteatoma had eroded the bony covering of the tensor tympani muscle and carotid and middle and apical turns of the cochlea (Figure 45). The cholesteatoma was completely removed from the petrous apex (Figure 46).
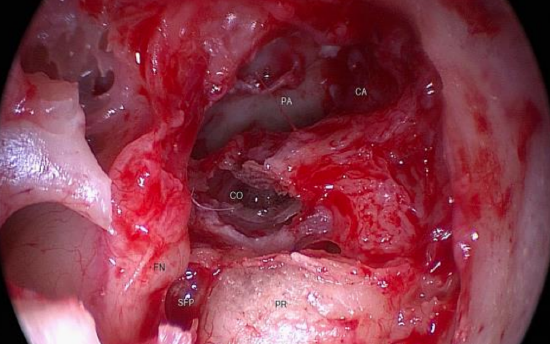
Figure 47: Right ear: View after complete removal of cholesteatoma (PA: petrous apex; CA: carotid artery; CO: eroded middle turn of cochlea; FN: dehiscent facial nerve; SFP: stapes footplate; PR: promontory)
Endoscopic tympanoplasty
Depending on the anatomy of the ear canal and the size and location of the perforation, the author uses either of two approaches to graft the tympanic membrane:
- Endoscopic transcanal medial graft tympanoplasty: Small and well exposed perforations
- Endoscopic Sheehy's lateral graft tympanoplasty: Total perforations, surgical failures and for ear canals that limit access
Endoscopic transcanal medial graft tympanoplasty
Medial graft tympanoplasty is commonly practiced. Adequate exposure of the whole tympanic perforation is key to its success. When using a microscope, unfavorable ear canal anatomy and/or anterior perforations make for technically challenging transcanal procedures and a postauricular approach may be needed to provide adequate access. The endoscope allows for a wide transcanal, all-encompassing view of all the elements of this surgery i.e. the ear canal, tympanic ring, and tympanic membrane, without needing to continuously reposition the microscope, even in the presence of an anterior overhang.
Technique
All surgical steps are performed with an endoscope. This includes injection of the ear canal, debridement of the edges of the perforation, elevation of a tympanomeatal flap, inspection of the middle ear for disease and ossicular integrity, positioning of a medially placed graft on a bed of gelfoam, repositioning of the tympanomeatal graft and packing the ear canal with gelfoam.
Clinical example
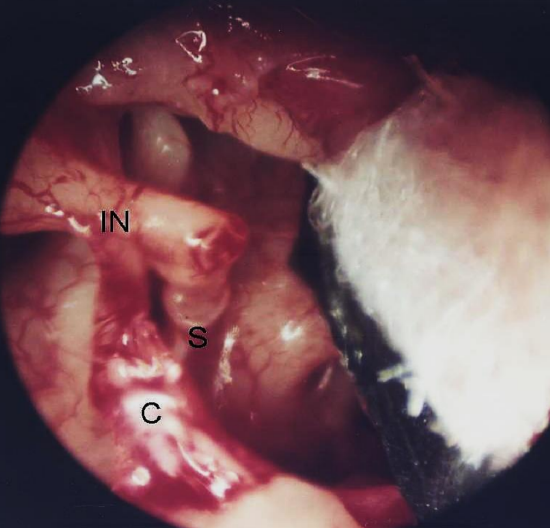
Figure 48: A tympanomeatal flap is reflected anteriorly to reveal the incus (IN), stapes (S) and chorda (C)
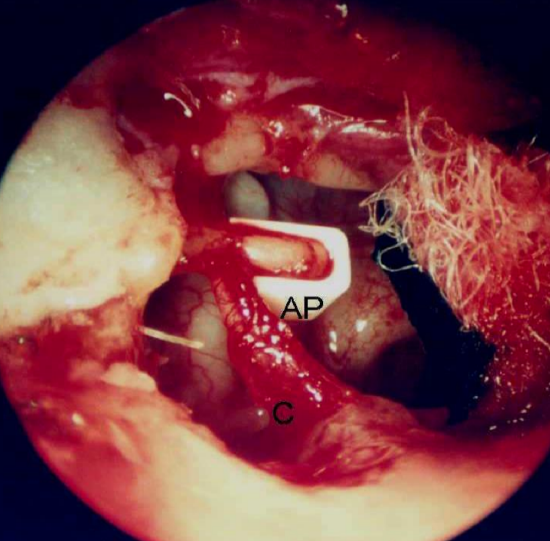
Figure 49: Applebaum prosthesis (AP) is used to bridge the incudostapedial joint
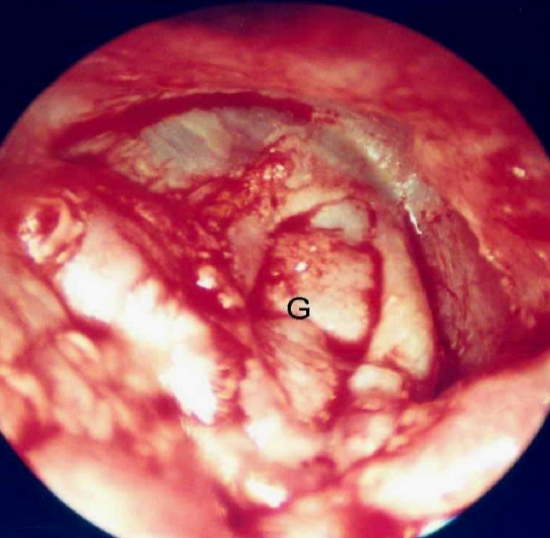
Figure 50: Graft (G) in place
Figures 48 - 50 illustrate a case of central tympanic membrane perforation with moderate conductive hearing loss. Transcanal endoscopic medial graft tympanoplasty is performed and the incudo-stapedial joint dislocation is addressed with an Applebaum prosthesis.
Endoscopic Sheehy lateral graft tympanoplasty
Lateral graft tympanoplasty has stood the test of time as an effective surgical approach for large perforations. It involves more extensive surgery than transcanal medial graft technique, but usually produces a higher success rates. Critical to it's success is a wide exposure of the ear canal which classically involves a postauricular approach. The endoscope offers a wide transcanal access and view of the ear canal and tympanic membrane without the need for a postauricular approach.
Technique
Using transcanal endoscopy, the skin of the ear canal is elevated along with the epithelial layer of the remaining tympanic membrane with the preservation of vascular strip. The ear canal is then enlarged as needed with a drill. The middle ear is packed with gelfoam. The graft is positioned lateral to the fibrous layer of the membrane and is tucked under the handle of malleus. The skin of the canal is then repositioned and the canal is packed with gelfoam.
Endoscopic stapedectomy
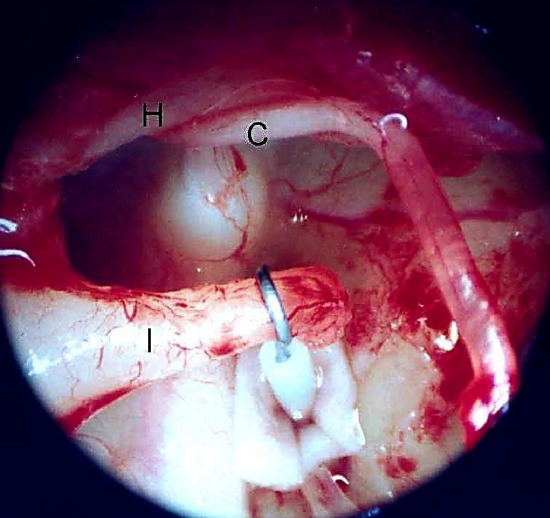
Figure 51: Stapes prosthesis in place
Although experienced endoscopic surgeons probably prefer the using the endoscope, there are no compelling reasons to use the endoscope instead of the microscope in stapes surgery as the microscope offers a good view of the region of the stapes (Figure 51).
A few issues need to be taken into consideration when using the endoscope for stapes surgery. The first is that the endoscope’s wide angle allows a better view of the footplate without much curetting of bone. However, the improved view does not translate into improved access when using traditional straight picks and drill bits. One needs to overexpose these areas endoscopically in order to allow work to be done using existing straight instruments. The second issue relates to crimping of the wire over the the incus. If the surgeon spends too much time with the light of the endoscope directed at the piston wire prosthesis, the wire is heated and “uncrimps” because of the memory of the metal used and its tendency to return to its original shape when heated. The third issue is that the endoscope deprives the surgeon from using a two-handed technique to placement a bucket handle type prosthesis.
Concluding comments
The story of endoscopic management of cholesteatoma is that of rediscovering the ear canal as the most direct and natural access to cholesteatoma which is limited to the mesotympanum, attic, facial recess, sinus tympani, hypotympanum, and eustachian tube. It offers a fresh outlook on this disease and changes the surgical treatment paradigm of such cholesteatoma.
Editor’s comment
Endoscopic otologic surgery presents a cheaper and more transportable option than operating microscopes for surgeons working in resource constrained developing world countries to perform myringotomies, insert ventilation tubes (grommets) and do tympanoplasties.
References
- Thomassin JM, Korchia D, Doris JM. Endoscopic-guided otosurgery in the prevention of residual cholesteatomas. Laryngoscope 1993;103:939-43
- Hawke M. Telescopic otoscopy and photography of the tympanic membrane. J Otolaryngol 1982;11:35-9
- Nomura Y. Effective photography in otolaryngology-head and neck surgery: endoscopic photography of the middle ear. Otolaryngol Head Neck Surg 1982;90:395-8
- Takahashi H, Honjo I, Fujita A, Kurata K. Transtympanic endoscopic findings in patients with otitis media with effusion. Arch Otolaryngol Head Neck Surg 1990;116:1186-9
- Poe DS, Bottrill ID. Comparison of endoscopic and surgical explorations for perilymphatic fistulas. Am J Otol 1994;15:735-8
- McKennan KX. Endoscopic 'second look' mastoidoscopy to rule out residual epitympanic/mastoid cholesteatoma. Laryngoscope 1993;103:810-4
- Tarabichi M. Endoscopic management of acquired cholesteatoma. Am J Otol 1997;18:544-9
- Tarabichi M. Endoscopic middle ear surgery. Ann Otol Rhinol Laryngol 1999;108:39-46
- Tarabichi M. Endoscopic management of cholesteatoma: long-term results. Otolaryngol Head Neck Surg 2000; 122:874-81
- Tarabichi M. Endoscopic management of limited attic cholesteatoma. Laryngoscope 2004;114:1157-62
- Kakehata S, Futai K, Sasaki A, Shinkawa H. Endoscopic transtympanic tympanoplasty in the treatment of conductive hearing loss: early results. Otol Neurotol. 2006 Jan;27(1):14-9
- Kakehata S, Hozawa K, Futai K, Shinkawa H. Evaluation of attic retraction pockets by microendoscopy. Otol Neurotol. 2005 Sep;26(5):834-7
- Kakehata S, Futai K, Kuroda R, Shinkawa H. Office-based endoscopic procedure for diagnosis in conductive hearing loss cases using OtoScan Laser-Assisted Myringotomy. Laryngoscope. 2004 Jul;114(7):1285-9
- Badr-el-Dine M. Value of ear endoscopy in cholesteatoma surgery. Otol Neurotol 2002;23:631-5
- El-Meselaty K, Badr-El-Dine M, Mandour M, Mourad M, Darweesh R. Endoscope affects decision making in cholesteatoma surgery. Otolaryngol Head Neck Surg 2003; 129: 490-6
- Yung MW. The use of middle ear endoscopy: has residual cholesteatoma been eliminated? J Laryngol Otol 2001;115:958-61
- Ayache S, Tramier B, Strunski V. Otoendoscopy in cholesteatoma surgery of the middle ear. What benefits can be expected? Otol Neurotol. 2008 Dec;29(8):1085-90
- Abdel Baki F, Badr-El-Dine M, El Saiid I, Bakry M. Sinus tympani endoscopic anatomy. Otolaryngol Head Neck Surg. 2002; 127: 158-62
- Mattox DE. Endoscopy-assisted surgery of the petrous apex. Otolaryngol Head Neck Surg. 2004;130:229-41
- Magnan J, Sanna M. Endoscopy in neuro-otology. Stuttgart: Georg Thieme Verlag; 2003
- Badr-El-Dine M, El-Garem HF, Talaat AM, Magnan J. Endoscopically Assisted Minimally Invasive Microvascular Decompression of Hemifacial Spasm. Otol Neurotol 2002; 122-8
- El-Garem HF, Badr-El-Dine M, Talaat AM, Magnan J. Endoscopy as a Tool in Minimally Invasive Trigeminal Neuralgia Surgery. Otol Neurotol 2002 132-5
- Badr-El-Dine M, El-Garem HF, ElAshram Y, Talaat AM, Magnan J. Endoscope Assisted Minimal Invasive Microvascular Decompression of Hemifacial spasm. Abstracts of the 9th International Facial Nerve Symposium. Otol Neurotol Suppl. 2002; 23 (3): 68- 72
- Rosenberg SI, Silverstein H, Willcox TO, Gordon MA. Endoscopy in otology and neurotology. Am J Otol 1994;15:168-72
- Presutti L, Marchioni D, Mattioli F, et al. Endoscopic Management of Acquired Cholesteatoma: Our Experience. Otolaryngol Head Neck Surg, 2008: 37, (4), 1-7
- Marchioni D, Mattioli F, Ciufelli MA, Presutti L. Endoscopic approach to tensor fold in patients with attic cholesteatoma. Acta Otolaryngol 2008,19:1-9
- Tos M. Modification of combinedapproach tympanoplasty in attic cholesteatoma. Arch Otolaryngol 1982;108:772-8
- Sheehy JL, Brackmann DE, Graham MD. Cholesteatoma surgery: residual and recurrent disease. A review of 1,024 cases. Ann Otol Rhinol Laryngol 1977;86:451-62
- Glasscock ME, Miller GW. Intact canal wall tympanoplasty in the management of cholesteatoma. Laryngoscope 1976;86:1639-57
- Kinney SE. Five years experience using the intact canal wall tympanoplasty with mastoidectomy for cholesteatoma: preliminary report. Laryngoscope 1982;92:1395-400
- Chatellier HP, Lemoine J. Le diaphragme interattico-tympanique du 612 nouveau-né. Description de sa morphologie considérations sur son role 613 pathogénique dans les otomastoidites cloisonnées du nourisson. Ann Otolaryngol Chir Cervicofac (Paris) 1945;13:534-66
- Aimi K. The tympanic isthmus: its anatomy and clinical significance. Laryngoscope 1978;88(7 Pt 1):1067-81
- Palva T, Ramsay H. Incudal folds and epitympanic aeration. Am J Otol 1996; 17:700-8
- Palva T, Ramsay H, Böhling T. Tensor fold and anterior epitympanum Am J Otol 1997;18:307-16.
- Hammar JA. Studien Uper Die Entwicklung Des Vorderdarms und Einiger Angrenzenden Organe. Arch Mikroskop Anat 1902;59: 471-628
- Proctor B. The development of the middle ear spaces and their surgical significance. J Laryngol Otol 1964;78: 631-48
- Tono T, Schachern PA, Morizono T, Paparella MM, Morimitsu T. Developmental anatomy of the supratubal recess in temporal bones from fetuses and children. Am J Otol 1996;17:99-07
- Schuknecht HF, Gulya AJ. Anatomy of the Temporal Bone with Surgical Implications. Philadelphia, Pa: Lea & Febiger; 1986:89-90
- Adad B, Rasgon BM, Ackerson L. Relationship of the facial nerve to the tympanic annulus: a direct anatomic examination. Laryngoscope 1999;109: 1189-92
- Gangopadhyay KP, McArthur D, Larsson SG. Unusual anterior course of the sigmoid sinus: report of a case and review of the literature. J Laryngol Otol 1996;110:984-6
- Philip J. Moore.The high jugular bulb in ear surgery: three case reports and a review of the literature. J Laryngol Otol 1994;108:772-5
Author
Muaaz Tarabichi MD
Center for Ear Endoscopy
Kenosha, Wisconsin, USA
& American Hospital Dubai, Dubai UAE
mtarabichi@ahdubai.com
Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


