4.6: Septoplasty
- Page ID
- 15452
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
SEPTOPLASTY FOR DEVIATION OF THE NASAL SEPTUM
Ahmad Sedaghat, Benjamin Bleier
Septoplasty refers to surgical manipulation and/or removal of deviated septal cartilage and/or bone to correct a nasal septal deformity.
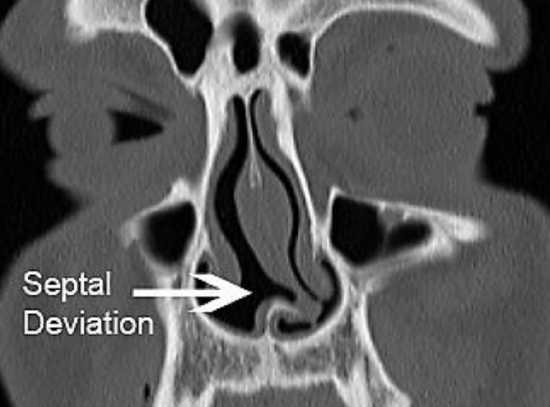
Figure 1: Example of a septal deviation
Up to 90% of people have nasal septal deviations (Figure 1), but the majority is asymptomatic. Septal deviation may cause nasal obstruction only when the nasal mucosa is swollen due to e.g. inflammation, allergic rhinitis, pharmacologic factors such as rhinitis medicamentosa or hormonal changes during pregnancy; in such cases obstruction may resolve either spontaneously or with medical therapy e.g. intranasal or systemic steroids, antihistamines and decongestants.
Indications for septoplasty
Septoplasty may be required to correct a deviated nasal septum for
- Irreversible symptomatic nasal obstruction
- Improving access for endoscopic sinus or skull base surgery
- Septal spurs causing epistaxis
Surgical anatomy
Bone and cartilage
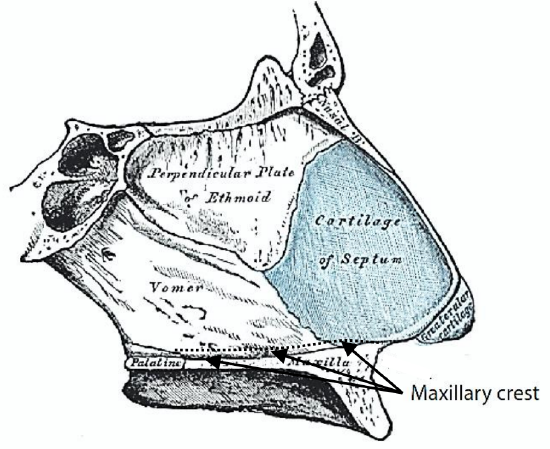
Figure 2: Bony and cartilaginous anatomy
The nasal septum has both bony and cartilaginous components (Figure 2). Anteriorly the septum is composed of the quadrangular cartilage. The posterior septum consists of bone of the perpendicular plate of the ethmoid superiorly and the vomer inferiorly. The most inferior strip of the septum is the maxillary crest, a bony projecttion from the maxilla and palatine bone along the full length of the septum. The maxillary crest articulates with quadrangular cartilage anteriorly and the vomer posteriorly.
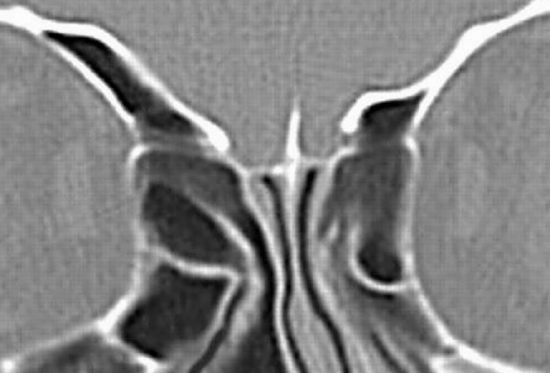
Figure 3: Perpendicular plate of ethmoid attaches to delicate cribriform plate
Superiorly the perpendicular plate of the ethmoid attaches to the delicate cribriform plate (Figure 3). This has clinical relevance as rough handling or twisting of the perpendicular plate can cause a fracture of the skull base, a cerebrospinal fluid leak and meningitis. The bony and cartilaginous septum is covered with periosteum and perichondrium from which it receives its blood supply. Superficially it is lined by respiratory mucosa.
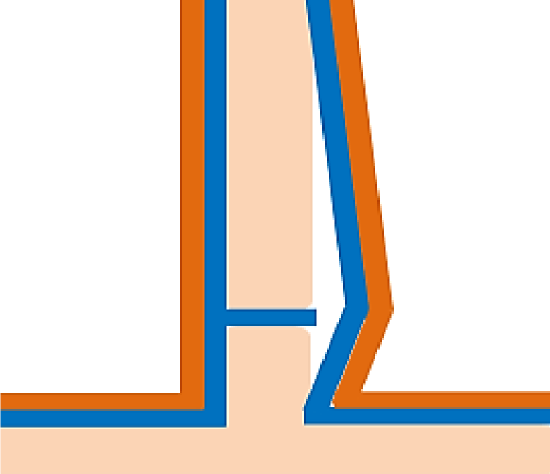
Figure 4: One has to cut across the fibrous attachments to join the superior and inferior subperiosteal tunnels
The perichondrium of the quadrangular cartilage and periosteum of the perpendicular plate of the ethmoid and vomer are in continuity because of their common embryologic origin from the frontonasal prominence. However the periosteum of the maxillary crest is separate from the periosteum of the vomer and perichondrium of the quadrangular cartilage due to its origin from the maxillary processes. This has clinical relevance as one has to cut across these fibrous attachments in order to join subperichondrial and subperiosteal dissection planes over the quadrangular cartilage or vomer with the subperiosteal plane over the maxillary crest (Figure 4).
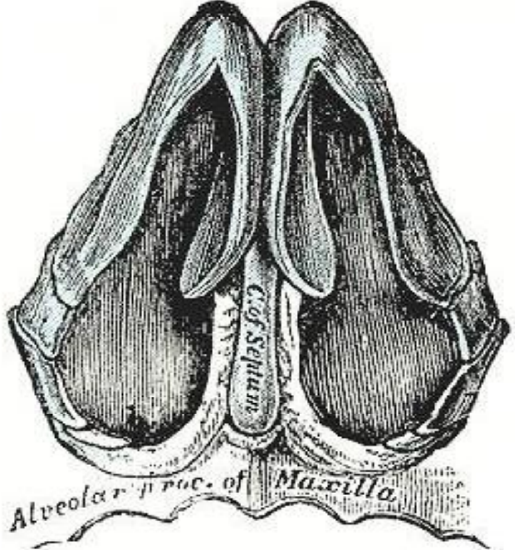
Figure 5: Nasal valve
The internal nasal valve is the narrowest part of the nasal airway and is formed by the septum, the anterior end of the inferior turbinate, the caudal aspect of the upper lateral cartilage and the floor of the piriform aperture (Figure 5). Deviation of the septum at the nasal valve is therefore likely to contribute to symptomatic obstruction. The quadrangular cartilage attaches to the columella by a membranous septum at the anterior and caudal aspect of the septum.
Vascular supply (Figures 6-8)
An understanding of the vascular supply is important if large mucoperiosteal flaps are to be used. Venous outflow generally follows the arterial blood supply.
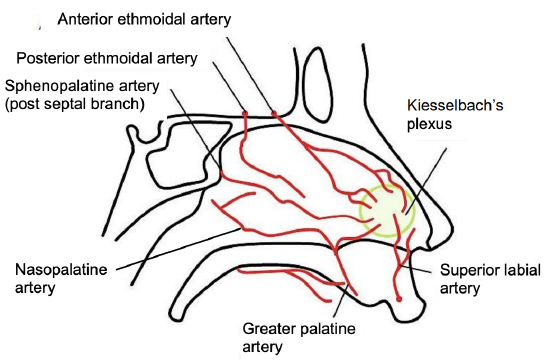
Figure 6: Arterial supply to nasal septum
The nasal septum has both internal (ICA) and external carotid (ECA) artery supply. The anteroinferior septum is supplied by the septal branch of the superior labial artery, and the greater palatine artery (Figure 6). The former arises from the facial artery, a branch of the ECA; the latter is a proximal branch of the internal maxillary artery, also a branch of the ECA.
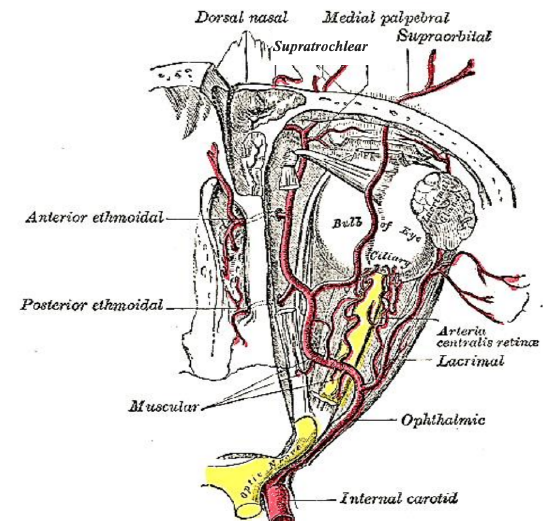
Figure 7: Ophthalmic artery gives rise to anterior and posterior ethmoidal arteries
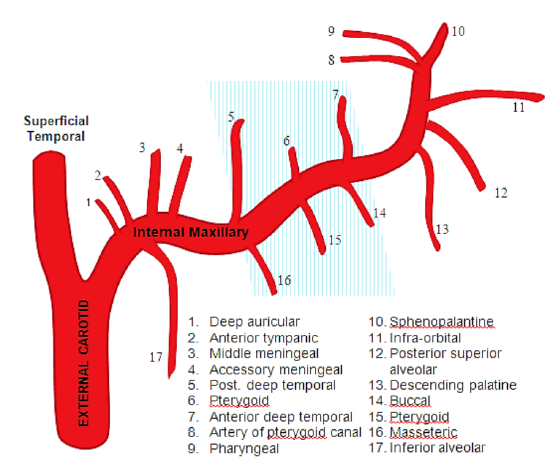
Figure 8: Branches of internal maxillary artery; blue shading denotes 2nd part of internal maxillary artery before it enters pterygopalatine fossa
The anterosuperior septum is supplied by the anterior ethmoidal artery; this arises from the ophthalmic artery, a branch of the ICA (Figure 7). These 3 vessels converge at the anterior septum to form Kiesselbach’s plexus, a common origin of epistaxis. Posterosuperiorly the septum receives its blood supply from the posterior ethmoidal artery, a branch of the ophthalmic artery (ICA) and the posterior septal branch of the sphenopalatine artery, a terminal branch of the internal maxillary artery (ECA) (Figures 6, 8).
Innervation
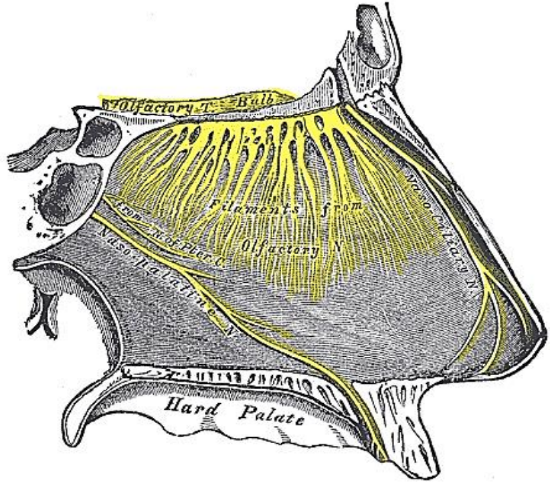
Figure 9: Nasopalatine nerve
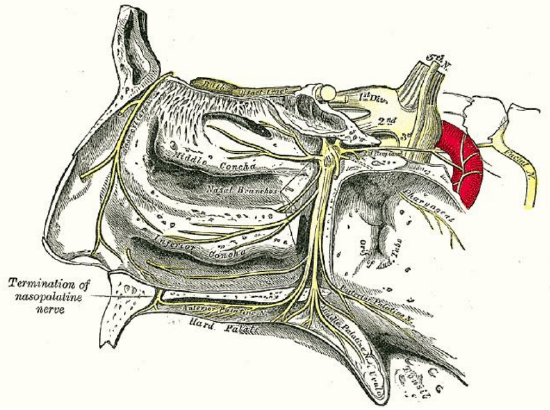
Figure 10: The nasopalatine nerve joins the greater palatine nerve via incisive foramen
The septum is innervated principally by the ophthalmic division (V1) of the trigeminal nerve. The anterior and posterior ethmoid dal nerves (branches of nasociliary nerve) are branches of V1 and provide sensory innervation to most of the septum. Only the nasopalatine nerve has its origin from the maxillary division (V2) of the trigeminal nerve (Figure 9); it arises from the pterygopalatine ganglion and innervates the anterior and caudal septum, primarily in the region of the maxillary crest. It enters the nasal cavity through the sphenopalatine foramen, passes medially below the ostium of the sphenoid sinus to reach the septum, and runs obliquely downward and forward between the periosteum and mucous membrane to reach the inferior septum. It then enters the roof of the mouth through the incisive canal and communicates with the corresponding nerve of the opposite side and with the greater palatine nerve (Figure 10). This has clinical relevance as surgical removal of the maxillary crest during septoplasty may injure the nasopalatine nerve and cause numbness of the maxillary incisors (often transient).
Surgical technique
Septoplasty must achieve separation of the left and right nasal cavities, adequate nasal air flow, as well as preserve dorsal and tip support of the nose. The authors favour submucosal resection of deviated septal cartilage and/or bone as was first reported and popularized by Freer and Killian.
Surgical approaches
It is the authors’ preference to do the surgery endoscopically due to the excellent visibility it affords. Surgery may also be achieved with an operating microscope or with a headlight and nasal speculum. Nonendoscopic surgical approaches may include endonasal (+/-microscope), external rhinoplasty, alar release and midfacial degloving techniques. If an endoscopic technique is not used, access to the nasal septum can be restricted.
Surgical Steps
- Decongest both sides of the nose with pledgets soaked in 1:1000 epinephrine, or alternatively, pseudoephedrine. After several minutes, inject lidocaine with epinephrine in submucoperichondrial planes bilaterally
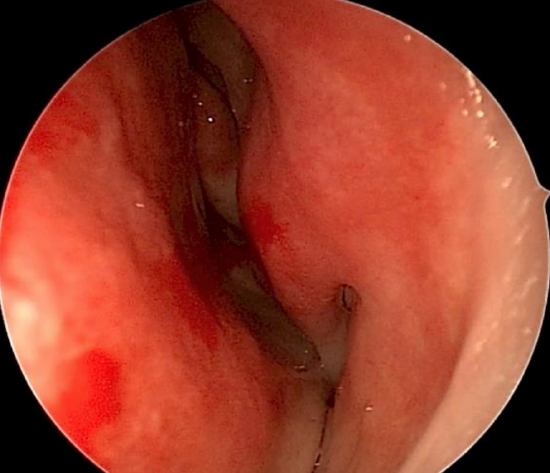
Figure 11: Deviated nasal septum (left nose)
- Examine both sides of the septum (Figure 11)
- Determine the side with a prominent septal convexity for the surgical approach as the mucosa is more likely to tear during elevation of the septal flap
- Incise the mucosa approximately 5 mm anterior to the intended transcartilaginous incision; the authors prefer to make the incision with an angled blade in order to cut perpendicular to the mucosa
- Extend the incision up to the mucoperichondrial junction taking care not to score the underlying cartilage
- Extend the incision as superiorly as possible; if an endoscope is used, use its shaft to retract the upper lateral cartilage to enhance the dorsal exposure
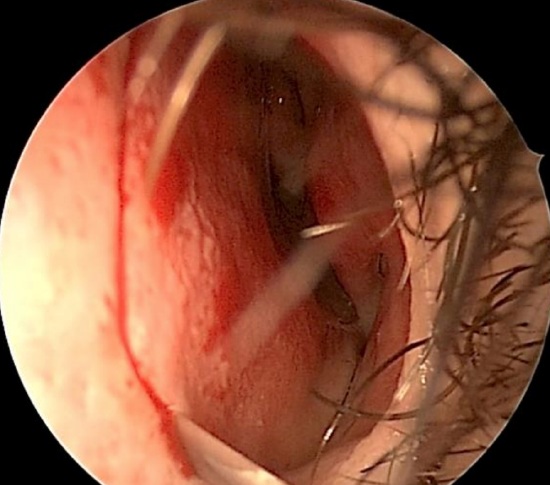
Figure 12: Incision up to the nasal floor where a back cut is added to enhance exposure
- Extend the incision to the nasal floor where a 5 mm back cut may be added to further enhance exposure (Figure 12)
- Use a Cottle elevator to develop a submucoperichondrial flap via the incision
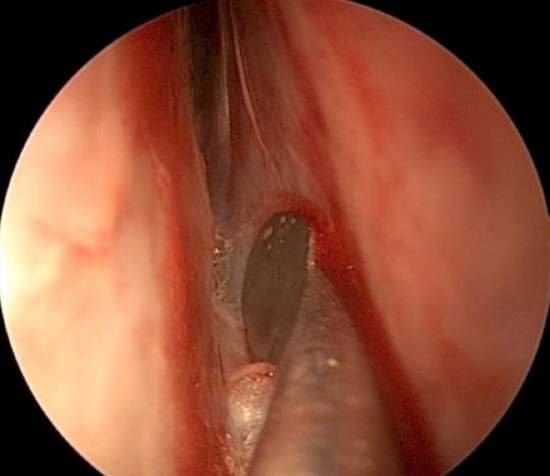
Figure 13: Mucoperichondrial and mucoperiosteal flaps have been elevated down to the maxillary crest
- Elevate a flap while stripping in a semicircular fashion starting in a posterosuperior direction, then down towards the nasal floor and finally sweeping from posterior to anterior inferiorly (Figure 13)
- Take care to remain within the welldefined subperichodrial / subperiosteal plane until you encounter the dense fibrous attachments to the maxillary crest (Figure 4); in order to extend elevation of the flap onto the maxillary crest and nasal floor the surgeon has to divide these fibers sharply using either a Cottle elevator or the belly of a #15 scalpel blade. Scrape along the underlying bone with a sweeping motion from the vertical limb of the maxillary crest inferiorly towards the nasal floor to divide these fibers
- The nasopalatine neurovascular bundle is often seen anteriorly during this step; take care to preserve it (Figures 6, 9)
- Continue to elevate the flap from the convexity of the septal deviation under direct vision until the “horizon” point is reached where one can no longer see the junction between the flap and the underlying cartilage/bone
- If the junction between the flap and the cartilage can no longer be seen, elevation should cease until later in the procedure
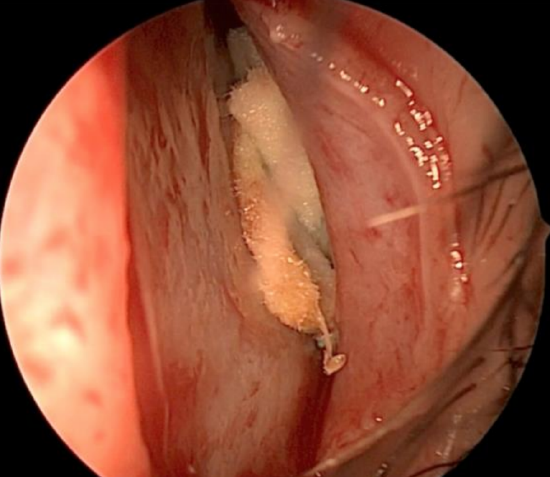
Figure 14: Flap elevated off the septal convexity with an epinephrine soaked pledget used for haemostasis
- Control bleeding with intermittent suction and epinephrine-soaked pledgets (Figure 14)
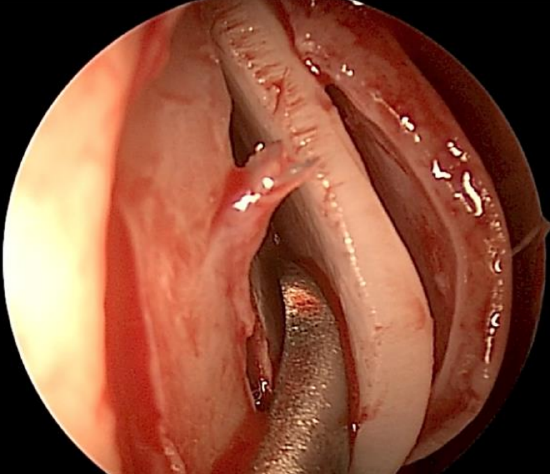
Figure 15: Cottle elevator used to complete the cartilage incision and to create a contralateral submucoperichondrial flap
- With the ipsilateral flap elevated beyond the septal deviation, make a transcartilaginous incision 1-2 mm posterior to the original mucosal incision with an angled blade or by scoring the cartilage with the blade and then using a Cottle elevator to complete the cartilage incision (Figure 15)
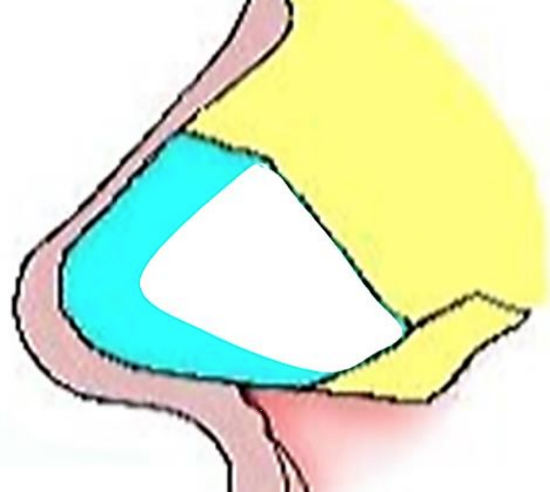
Figure 16: Dorsal and caudal cartilage struts of >1 cm are preserved for support
- Preserve dorsal and caudal cartilage struts of >1 cm for nasal and tip support (Figure 16)
- Elevate a contralateral flap (Figure 15); stop elevating the flap when the junction between the flap and cartilage cannot be seen
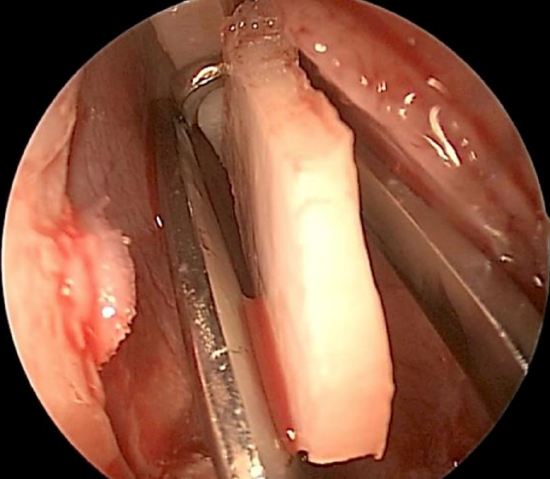
Figure 17: A swivel knife is being used to excise the deviated cartilage
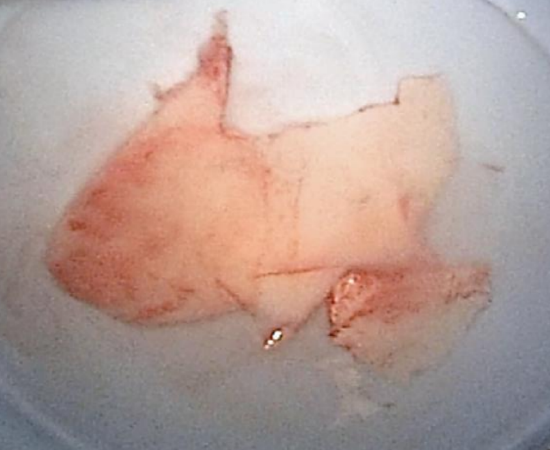
Figure 18: Cartilage is preserved to be replaced at later in the procedure
- Once both flaps have been fully elevated, use a swivel knife or scissors to remove part of the quadrangular cartilage (Figure 17); save the cartilage to later replace it (Figure 18)
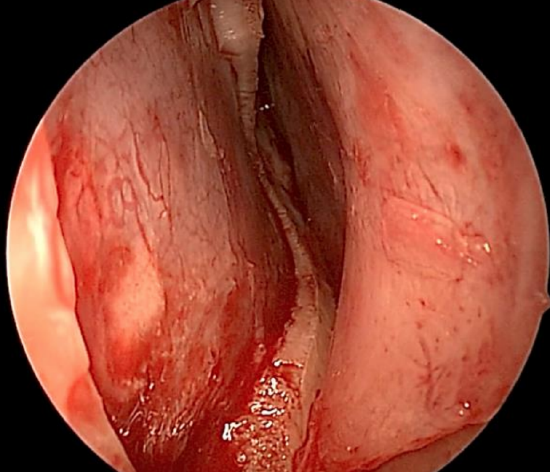
Figure 19: Improved access after removal of cartilage
- Removing cartilage improves the view of remaining septal deflections and affords better access to the “horizon points” which previously limited elevating the flaps (Figure 19)
- Further elevate the flaps to fully expose the septal deflections
- Use a through-biting punch to remove bone above the deflection to separate the deflection from its attachment to the skull base taking care not to twist the vertical plate of the ethmoid to avoid inadvertently fracturing of the cribriform plate
- Once the deflection has been separated from the skull base, reflect remaining mucosal attachments around the deflection and carefully fracture and re-move remaining bony deflections with grasping forceps
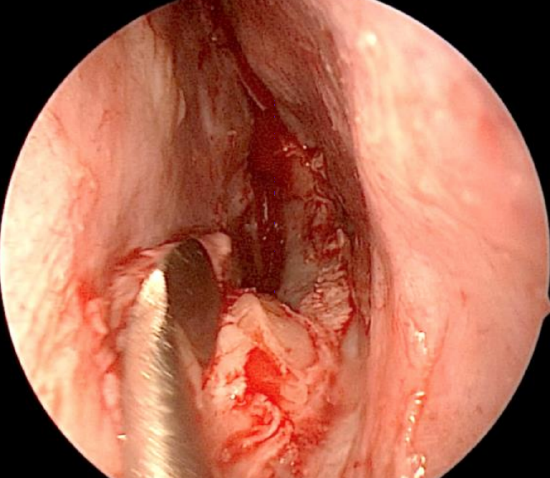
Figure 20: Exposing the maxillary crest
- If a deflection involves the maxillary crest, elevate the mucosa along the floor of the nose in a posterior to anterior direction (Figures 1, 20)
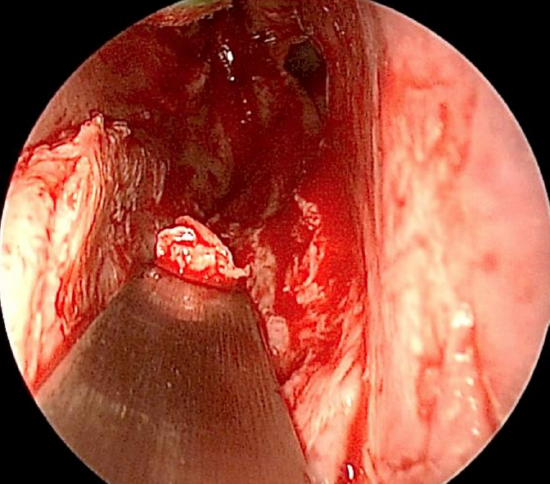
Figure 21: A 4 mm chisel is used to remove crest projecting into the airway
- Remove the crest which projects into the airway with a 4 mm chisel (Figure 21); do not completely transect the crest if possible as this may injure the nasopalatine nerve and precipitate troublesome bleeding from the greater palatine artery Once the entire deflection has been removed it is recommended that the cartilage that had been removed is replaced, particularly if a large portion of the quadrangular cartilage was excised; curved areas of the cartilage are first flattened with a mallet
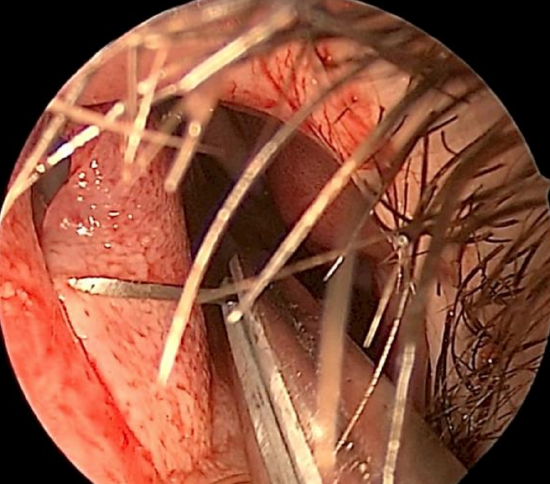
Figure 22: Coapting the mucoperichondrial flaps
- The mucoperichondrial flaps are closed; use a 4-0 plain catgut suture on a a Keith needle to close both the incision and to coapt the mucoperichondrial flaps with a quilting stitch
- Pass the needle posterior and then anterior to the incision; tie the 2 knots to tack down the mucosa (Figure 22) Take care with this initial stitch to fully approximate the mucosal edges leaving a long tail
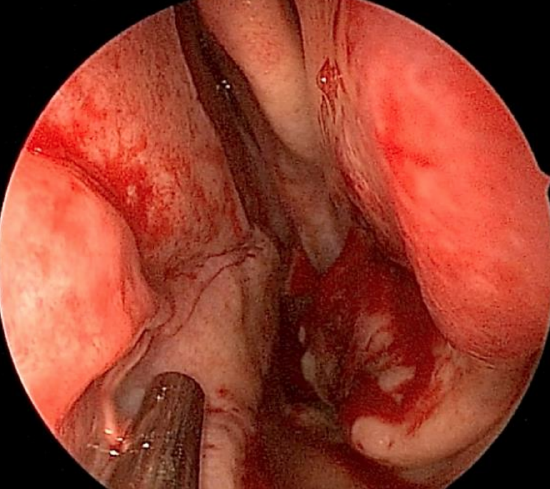
Figure 23: Coapting the mucoperichondrial flaps
- Use the same stitch to close the incision using a similar back-and-forth technique. It may be carried posteriorly to coapt the mucoperichondrial flaps using 3 to 4 passes (Figure 23). Finally the stitch may be brought anteriorly and tied to the long tail of the initial tacking stitch
- Splints are optional following quilting although it may promote healing and reduce the risk of a septal hematoma; the senior author uses Doyle splints which are sutured through the membranous septum and left in place for approximately 1 week
Complications
- Septal hematoma
- Epistaxis from raw mucosal edges
- Septal perforation
- Bilateral, opposing mucosal tears
- Excessive packing
- Septal hematoma
- Nasal obstruction
- Inadequate correction of septal deformity
- Synechiae from opposing, traumatized septal and inferior turbinate mucosal surfaces
- Nasal deformity from excessive removal of cartilage and preserving too little dorsal or caudal cartilage struts
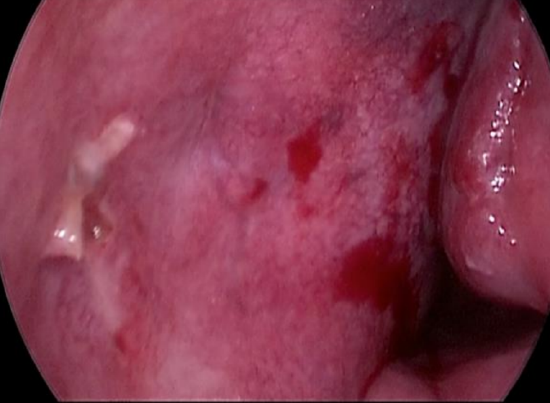
Figure 24: Septal hematoma
Septal hematomas (Figure 24) are rare, particularly with the use of quilting stitches and splints. The surgeon should be vigilant for this complication as it requires immediate intervention. Many hematomas may be managed in a clinic setting by incising the mucosa under local anesthesia and evacuating the clot. Bilateral packing to exert pressure on the site of the hematoma is recommended to avoid reaccumulation. If an obvious cause is not evident, the surgeon should rule out a coagulopathy.
Septal perforations may be very symptomtic and should be avoided at all costs. The key to avoiding perforations is to avoid opposing mucosal perforations. While a perforation ipsilateral to the deviation may be unavoidable and generally does not have consequence, great care should be taken to preserve the integrity of the contralateral mucosal flap. If opposing perforations are noted, then an interposition graft should be placed between the flaps such as autologous cartilage/fascia or an alloplastic graft. The authors do not recommend attempting to primarily approximate the edges of a perforation as tension on the mucosa from the suture may cause further tears, compromise blood supply, and enlarge the mucosal defect.
Authors
Ahmad R. Sedaghat, MD, PhD
Chief Resident
Department of Otolaryngology - Head and Neck Surgery
Massachusetts Eye and Ear Infirmary
Harvard Medical School
Boston, USA
ahmad_sedaghat@meei.harvard.edu
Benjamin S. Bleier, MD
Assistant Professor
Department of Otology and Laryngology
Massachusetts Eye and Ear Infirmary
Harvard Medical School
Boston, USA
benjamin_bleier@meei.harvard.edu
Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


